Purpose:
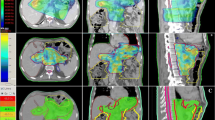
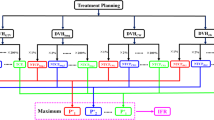
Dose-volume histograms (DVHs) were reviewed to determine if there is an advantage of the two modalities when treating patients with non-small cell lung cancer (NSCLC).
Patients and Methods:
24 stage I NSCLC patients who underwent proton-beam therapy (PBT) from June 2003 to May 2007 were included in this study. Based on the same clinical target volumes (CTVs), treatment planning was made to cover CTV within 90% isodose lines. Each patient was evaluated by two sets of DVHs, one for PBT and the other for three-dimensional conformal X-ray therapy (3D-CRT).
Results:
For all patients, the 95% isodose line covered 86.4% of the CTV for PBT, and 43.2% for 3D-CRT. PBT was associated with significantly lower mean doses to the ipsilateral lung, total lung, heart, esophagus, and spinal cord than 3D-CRT. PBT offered reduced radiation doses to the lung when evaluated in terms of percentage lung volumes receiving ≥ 5 Gy (V5), ≥ 10 Gy (V10), and ≥ 20 Gy (V20) when compared to 3D-CRT.
Conclusion:
PBT is advantageous over 3D-CRT in reducing doses to the lung, heart, esophagus, and spinal cord in treating stage I NSCLC.
Ziel:
Dosis-Volumen-Histogramme (DVHs) wurden untersucht, um die Vorteile der beiden Modalitäten bei der Behandlung von Patienten mit nichtkleinzelligem Lungenkarzinom (NSCLC) im Stadium I zu ermitteln.
Patienten und Methodik:
Die Studie umfasste 24 Patienten mit NSCLC Stadium I, die im Zeitraum von Juni 2003 bis Mai 2007 mit Protonenstrahltherapie („proton beam therapy“ [PBT]) behandelt wurden. Auf der Basis gleicher klinischer Zielvolumina (CTVs) wurde jeder Patient mit zwei Gruppen von DVHs beurteilt: einer für die PBT und einer für dreidimensionale konforme Röntgenstrahltherapie (3D-CRT).
Ergebnisse:
Bei allen Patienten wurden die CTVs von 90% der Isodosislinien sowohl bei PBT als auch bei 3D-CRT abgedeckt, während 95% der Isodosislinien bei PBT 86,4% und bei 3D-CRT 43,2% der CTVs abdeckten. Die PBT war mit einer signifikant niedrigeren mittleren Strahlendosis für die ipsilaterale Lunge, die gesamte Lunge, das Herz, die Speiseröhre und das Rückenmark assoziiert als die 3D-CRT. Die PBT bot reduzierte Strahlenbelastungen der Lunge, wenn der Prozentsatz des Lungenvolumens bewertet wurde, welches im Vergleich zur 3D-CRT einer Strahlenbelastung von ≥ 5 Gy (V5), ≥ 10 Gy (V10) und ≥ 20 Gy (V20) ausgesetzt war.
Schlussfolgerung:
Die PBT bietet gegenüber der 3D-CRT Vorteile bei der Reduktion der Strahlendosis für die umliegenden Organe und ist die Behandlung der Wahl insbesondere bei in der Nähe des Mediastinums liegenden Tumoren.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Auberger T, Seydl K, Futschek T, et al. Photons or protons: precision radiotherapy of lung cancer. Strahlenther Onkol 2007;183:Special Issue 2:3–6.
Bischof M, Debus J, Herfarth K, et al. Surgery and chemotherapy for small cell lung cancer in stages I-II with or without radiotherapy. Strahlenther Onkol 2007;183:679–84.
Chang JY, Zhang X, Wang X, et al. Significant reduction of normal tissue dose by proton radiotherapy compared with three-dimensional conformal or intensity-modulated radiation therapy in stage I or stage III non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 2006;65:1087–96.
Endo C, Sagawa M, Sakurada A, et al. Surgical treatment of stage I non-small cell lung carcinoma. Ann Thorac Cardiovasc Surg 2003;9:283–9.
Ernst-Stecken A, Lambrecht U, Mueller R, et al. Hypofractionated stereotactic radiotherapy for primary and secondary intrapulmonary tumors: first results of a phase I/II study. Strahlenther Onkol 2006;182:696–702.
Gauden S, Ramsay J, Tripcony L. The curative treatment by radiotherapy alone of stage I non-small cell carcinoma of the lung. Chest 1995;108:1278–82.
Georg D, Hillbrand M, Stock M, et al. Can protons improve SBRT for lung lesions? Dosimetric considerations. Radiother Oncol 2008;88:368–75.
Graham MV, Purdy JA, Emami B, et al. Clinical dose-volume histogram analysis for pneumonitis after 3D treatment for non-small cell lung cancer (NSCLC). Int J Radiat Oncol Biol Phys 1999;45:323–9.
Harpole DH Jr, Herndon JE 2nd, Young WG Jr, et al. Stage I nonsmall cell lung cancer. A multivariate analysis of treatment methods and patterns of recurrence. Cancer 1995;76:787–96.
Hata M, Tokuuye K, Kagei K, et al. Hypofractionated high-dose proton beam therapy for stage I non-small-cell lung cancer: preliminary results of a phase I/II clinical study. Int J Radiat Oncol Biol Phys 2007;68:786–93.
Kong FM, Ten Haken RK, Schipper MJ, et al. High-dose radiation improved local tumor control and overall survival in patients with inoperable/unresectable non-small-cell lung cancer: long-term results of a radiation dose escalation study. Int J Radiat Oncol Biol Phys 2005;63:324–33.
Marino P, Preatoni A, Cantoni A. Randomized trials of radiotherapy alone versus combined chemotherapy and radiotherapy in stages IIIa and IIIb nonsmall cell lung cancer. A meta-analysis. Cancer 1995;76:593–601.
McGarry RC, Papiez L, Williams M, et al. Stereotactic body radiation therapy of early-stage non-small-cell lung carcinoma: phase I study. Int J Radiat Oncol Biol Phys 2005;63:1010–5.
Morita K, Fuwa N, Suzuki Y, et al. Radical radiotherapy for medically inoperable non-small cell lung cancer in clinical stage I: a retrospective analysis of 149 patients. Radiother Oncol 1997;42:31–6.
Nagata Y, Takayama K, Matsuo Y, et al. Clinical outcomes of a phase I/II study of 48 Gy of stereotactic body radiotherapy in 4 fractions for primary lung cancer using a stereotactic body frame. Int J Radiat Oncol Biol Phys 2005;63:1427–31.
National Cancer Center. Cancer statistics in Japan - 2005. Tokyo, Japan: National Cancer Center, 2005 (http://www.ncc.go.jp/jp/statistics/2005/index.html, accessed September 20, 2008).
Nieder C, Bremnes RM. Effects of smoking cessation on hypoxia and its potential impact on radiation treatment effects in lung cancer patients. Strahlenther Onkol 2008;184:605–9.
Onimaru R, Shirato H, Shimizu S, et al. Tolerance of organs at risk in small-volume, hypofractionated, image-guided radiotherapy for primary and metastatic lung cancers. Int J Radiat Oncol Biol Phys 2003;56:126–35.
Onishi H, Araki T, Shirato H, et al. Stereotactic hypofractionated high-dose irradiation for stage I nonsmall cell lung carcinoma: clinical outcomes in 245 subjects in a Japanese multiinstitutional study. Cancer 2004;101:1623–31.
Peters N, Wieners G, Pech M, et al. CT-guided interstitial brachytherapy of primary and secondary lung malignancies. Results of a prospective phase II trial. Strahlenther Onkol 2008;184:296–301.
Pritchard RS, Anthony SP. Chemotherapy plus radiotherapy compared with radiotherapy alone in the treatment of locally advanced, unresectable, non-small-cell lung cancer. A meta-analysis. Ann Intern Med 1996;125:723–9.
Qiao X, Tullgren O, Lax I, et al. The role of radiotherapy in treatment of stage I non-small cell lung cancer. Lung Cancer 2003;41:1–11.
Saitoh H, Fujisaki T, Sakai R, et al. Dose distribution of narrow beam irradiation for small lung tumor. Int J Radiat Oncol Biol Phys 2002;53:1380–7.
Segawa Y, Takigawa N, Kataoka M, et al. Risk factors for development of radiation pneumonitis following radiation therapy with or without chemotherapy for lung cancer. Int J Radiat Oncol Biol Phys 1997;39:91–8.
Semrau S, Bier A, Thierbach U, et al. 6-year experience of concurrent radiochemotherapy with vinorelbine plus a platinum compound in multimorbid or aged patients with inoperable non-small cell lung cancer. Strahlenther Onkol 2007;183:30–5.
Shioyama Y, Tokuuye K, Okumura T, et al. Clinical evaluation of proton radiotherapy for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 2003;56:7–13.
Timmerman R, Papiez L, McGarry R, et al. Extracranial stereotactic radioablation: results of a phase I study in medically inoperable stage I non-small cell lung cancer. Chest 2003;124:1946–55.
Wang S, Liao Z, Wei X, et al. Analysis of clinical and dosimetric factors associated with treatment-related pneumonitis (TRP) in patients with non-small-cell lung cancer (NSCLC) treated with concurrent chemotherapy and three-dimensional conformal radiotherapy (3D-CRT). Int J Radiat Oncol Biol Phys 2006;66:1399–407.
Yamada M, Kudoh S, Hirata K, et al. Risk factors of pneumonitis following chemoradiotherapy for lung cancer. Eur J Cancer 1998;34:71–5.
Yendamuri S, Komaki RR, Correa AM, et al. Comparison of limited surgery and three-dimensional conformal radiation in high-risk patients with stage I non-small cell lung cancer. J Thorac Oncol 2007;2:1022–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, C., Nakayama, H., Sugahara, S. et al. Comparisons of Dose-Volume Histograms for Proton-Beam versus 3-D Conformal X-Ray Therapy in Patients with Stage I Non-Small Cell Lung Cancer. Strahlenther Onkol 185, 231–234 (2009). https://doi.org/10.1007/s00066-009-1923-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-009-1923-x
Key Words:
- Dose-volume histograms
- Proton-beam therapy
- Three-dimensional conformal radiotherapy
- Stage I non-small cell lung cancer