Abstract
Objective
Revision of unicompartmental knee arthroplasty (UKA) to total knee arthroplasty (TKA) with the in situ referencing technique aiming to preserve as much ligament function and epi-metaphyseal bone stock as possible.
Indications
Aseptic loosening, progression of osteoarthritis, periprosthetic fracture, periprosthetic infection, arthrofibrosis, polyethylene wear, malalignment, instability, femoro-tibial impingement.
Contraindications
Unexplained pain, localized or systemic active infection (anywhere).
Surgical technique
Referencing for the tibia and the femur cuts is performed prior to implant removal. The tibial cutting jig and the initial tibial resection level is set in a way that the sawblade just fits under the tibial implant. In case too much bone needs to be removed to achieve flush implant sitting on both the medial and lateral tibia, a step cut needs to be performed to build up the medial defect with an augment. Prior to femoral component removal, rotational alignment is determined and intramedullary referencing for the distal femur osteotomy is performed. Level of constraint and additional tibial stem fixation is chosen according to the amount of bone resected and according to ligament stability.
Postoperative management
Sterile dressings and elastic compression bandaging. No limitation of active/passive range of motion. Full weight-bearing or partial weight-bearing for 2 weeks postoperatively in the presence of bone or soft tissue defects.
Results
Between 2008 and 2019, 84 patients underwent revision of unicompartmental knee arthroplasty. The mean follow-up was 64 months (range 3–132 months). Implant survival after revision of UKA to TKA was 92% (95% CI = 82–97%) at 5 years of follow-up and 86% (95% CI = 69–93%) at 10 years of follow-up. The mean Oxford knee score was 20.1 (6–39, SD ± 6.5) preoperatively and 30.2 (3–48, SD ± 11.3) postoperatively. The mean visual analogue scale was 6.9 (range 1–10, SD ± 1.8) preoperatively and 3.9 (range 0–9, SD ± 2.6) postoperatively.
Zusammenfassung
Operationsziel
Wechsel eines unikompartimentellen Kniegelenkersatzes (UNI) auf eine totale Kniegelenkendoprothes (TEP) in In-situ-Referenzierungstechnik unter bestmöglichem Erhalt der artikulären Bandfunktion und des epi-metaphysären Knochens.
Indikationen
Aseptische Lockerung, Progression der Arthrose, periprothetische Fraktur, periprothetische Infektion, Arthrofibrose, Polyethylenabrieb, Malalignement, Instabilität, femorotibiales Impingement.
Kontraindikationen
Unerklärbarer Schmerz, lokale oder systemische aktive Infektion (unabhängig von der Lokalisation).
Operationstechnik
Die Referenzierung für die Tibia- und Femurschnitte findet bei noch liegendem Implantat statt. Die tibiale Resektion erfolgt direkt unterhalb des Tibiaimplantats. Wenn für einen bündigen Implantatsitz sowohl auf der medialen als auch auf der lateralen Tibia zu viel Knochen entfernt werden muss, muss eine stufenförmige Osteotomie erfolgen, um den medialen Defekt mit einem Augment behandeln zu können. Die Entfernung der Femurkomponente erfolgt erst nach Einstellung der Femurrotation und intramedullärer Referenzierung für die Osteotomie des distalen Femurs. Der Kopplungsgrad der Prothese wird vom Ausmaß des Knochendefekts und der bestehenden Bandstabilität bestimmt. Gegebenenfalls muss auf eine stielgeführte Prothese zurückgegriffen werden.
Weiterbehandlung
Steriler Verband und elastokompressive Wickelung. Keine Limitation des aktiven bzw. passiven Bewegungsumfangs. Vollbelastung bzw. Teilbelastung für 2 Wochen postoperativ bei größeren Knochen- bzw. Weichteildefekten.
Ergebnisse
Zwischen 2008 und 2019 wurde bei 84 Patienten die Revision eines unikompartimentellen Kniegelenkersatzes durchgeführt. Das durchschnittliche Follow-up betrug 64 Monate (3–132 Monate). Das Implantatüberleben nach Wechsel von UNI auf TEP betrug 92 % (95 %-Konfidenzintervall [KI] 82–97 %) nach 5 Jahren Follow-up und 86 % (95 %-KI 69–93 %) nach 10 Jahren Follow-up. Der mittlere Oxford Knee Score betrug präoperativ 20,1 (6–39, Standardabweichung [SD] ± 6,5) und postoperativ 30,2 (3–48, SD ± 11,3), der mittlere Wert auf der visuellen Analogskala lag präoperativ bei 6,9 (1–10, SD ± 1,8) und postoperativ bei 3,9 (0–9, SD ± 2,6).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introductory remarks
Unicompartmental knee arthroplasty (UKA) is a less invasive bone-sparing surgical alternative to total knee arthroplasty (TKA) for patients with unicompartmental knee osteoarthritis [1,2,3,4]. The implantation of a primary UKA seems to have some important advantages for the patient compared to TKA such as shorter hospitals stays, higher postoperative range of motion, better overall knee function and fewer short-term complications [5,6,7,8,9]. However, international knee arthroplasty registries have demonstrated that UKAs are not only revised earlier, but also more often than TKAs [10, 11]. This might be due to technical errors made by low-volume surgeons, incorrect indications or the obvious belief that UKA to TKA revision is a technically simple and easy procedure comparable to the implantation of a primary TKA, which might per se decrease the threshold for UKA revision [9, 12].
Prima facie, the obvious belief that UKA to TKA revision is an easy and simple procedure might be true in some cases, as some smaller studies indeed described the need for revision implants or augments to be negligible [13]. However, caution is advised, since UKA to TKA revision due to significant bone loss, infection or ligament instability might require the same technical toolbox and surgical skill set as those needed for TKA to TKA revision. Moreover, studies analysing data from large referral centres and national joint registries have demonstrated that overall clinical outcomes and revision rates of UKA to TKA revision are by no means comparable to those after primary TKA implantation [14,15,16]. In fact, it has been shown that revision components are needed in up to one third of UKA to TKA revisions [12] and that functional scores and quality of life measurements are more comparable to those after TKA to TKA revision [17]. In this context, Hang and co-workers reported results from 1948 UKA to TKA revisions and demonstrated cumulative re-revision rates of 15% after 5 years similar to those after TKA to TKA revisions, which were 18% after 5 years [15].
It is of utmost importance that surgeons know these data not only to properly guide and counsel patients prior to UKA revision, but also to be able to per se appreciate that UKA to TKA revision is not always a straightforward procedure. In order to achieve good functional results and good survival rates, surgeons need to be well-trained in knee revision arthroplasty techniques rather to expect another primary TKA-like procedure and they have to hold revision implants available when performing UKA to TKA revisions.
Keeping this rationale in mind, the aim of this article is therefore to describe in detail the authors’ surgical technique of UKA to TKA revision, including the preoperative planning process and postoperative aftercare. Furthermore, data are provided from a retrospective study performed at the authors’ university level 1 department, including functional outcomes and implant survival after UKA to TKA revision.
Surgical principle and objective
Safe and reliable revision of UKA to TKA with the in situ referencing technique aiming to preserve as much ligament function and epi-metaphyseal bone stock as possible. With this technique, the femoral component is not removed until the valgus angle and the amount of distal femoral bone to be resected is determined as well as anatomical landmarks of femoral rotational alignment are assessed.
Advantages
-
Preservation of bone stock and ligament function
-
Reliable joint line reconstruction and rotational alignment
-
Reproducible implantation technique
-
No expensive navigation software/tools required
Disadvantages
-
A certain degree of experience in revision knee arthroplasty is needed for the distinct identification of anatomical landmarks and correct axial/rotational alignment of the implants.
-
The in situ referencing technique cannot be applied in the presence of significant femoral implant migration or tibial collapse.
-
In some cases, modular knee revision systems are necessary with the possibility to augment bone defects, increase the level of constraint or add femoral and/or tibial stems.
Indications
-
Aseptic loosening
-
Progression of osteoarthritis
-
Periprosthetic fracture
-
Periprosthetic infection
-
Arthrofibrosis
-
Dislocation of the insert, polyethylene wear
-
Malalignment
-
Instability
-
Femoro-tibial impingement
Contraindications
-
Unexplained pain
-
Localized or systemic active infection
-
Poor therapeutic compliance
Patient information
-
General risks of surgery (infection, hematoma, wound healing complications, thrombosis, embolism, iatrogenic nerve palsy or lesions of vascular structures, inter alia).
-
Intraoperative fracture, ligament or tendon lesion.
-
Arthrofibrosis, instability or malalignment.
-
Aseptic or septic loosening.
-
Postoperative partial weight-bearing in case of significant bone or soft tissue defects.
-
Patient expectations should be taken into consideration to improve satisfaction after surgery. Survival rates after UKA to TKA conversion and expected outcomes need to be discussed.
Preoperative work up
-
Standard preoperative work up in consultation with an anesthesiologist to assess the current medical status and risk profile of the patient. Optimization of co-morbidities.
-
Preoperative patient education program and enrolment into standard clinical pathways including prehabilitation programs, fast track concepts, patient blood management and multi-modal pain management programs.
-
Preoperative joint aspiration (with subsequent cell count, gram staining, microbiological culture for at least 2 weeks) in cases of unexplained pain or clinical signs of infection/elevated levels of inflammatory serum markers [18, 19].
-
The type of the implanted unicondylar prosthesis should be known. At best, the surgical protocol should be made available [20].
-
Radiographic analyses (antero-posterior in standing position, true lateral radiograph with the knee in 30° of flexion, antero-posterior orthoroentgenogram in standing position and Merchant view is mandatory). In some cases, MRI and CT analyses might be necessary for further diagnostic evaluation.
-
Digital templating within a picture archiving and communication system (PACS) to determine implant type, size, level of constraint and need for augments or stems (Fig. 1).
Preoperative digital templating and postoperative radiographs in a patient with aseptic loosening of the tibial tray. Templating makes it possible to anticipate the intraoperative levels of osteotomy, the tibial slope and the need for augments or stems. In this context, surgeons should not hesitate to repeat radiographic examinations in cases where the knee is malrotated. Proper planning of implant size and posterior condylar offset is only possible on true lateral radiographs
Instruments and implants
-
Commonly used implantation kit and instruments for total knee replacement including straight and curved chisels.
-
High-pressure irrigation (jet lavage).
-
Standard modular knee revision systems should be available especially in cases with significant femoral implant migration or tibial tray collapse.
Anesthesia and positioning
-
Multimodal analgesic protocol including preoperative pain and anti-inflammatory medication as well as intraoperative local infiltration analgesia (LIA).
-
General or spinal anesthesia.
-
Adductor canal block for fast-track surgery patients. Femoral nerve block as single shot or via continuous infusion systems in situations in which fast-track concepts are not applicable.
-
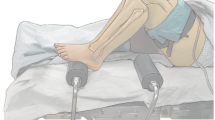
Supine positioning of the patient without pressure points.
-
Positioning of the leg within a leg holder or footrest.
-
A pneumatic tourniquet is applied but it is only inflated during the cementation process. The authors do not use suction drains in patients who are eligible to enter fast-track pathways.
-
Preoperative administration of intravenous tranexamic acid and postoperative application of low-molecular-weight heparins until full weight-bearing.
-
Preoperative single-dose administration of i.v. antibiotics (e.g. Cefazolin 2 g).
Surgical technique
Implant exposure. Standard approach extending the previously used skin incision. Prior to arthrotomy synovial fluid is aspirated for microbiological analyses and white-blood-cell count (a). After synovectomy, multiple soft tissue samples are collected and further processed to exclude infection or synovitis due to wear debris. The authors’ preference is to perform a subperiosteal release of the soft tissues at the medial tibia plateau and to excise the Hoffa fat pad. Osteophytes at the patella rim are removed, a lateral patella-facetectomy is performed and the anterior cruciate ligament is excised (b)
Assessment of implant failure. Preoperative diagnoses such as arthritic progression (a), tibial collapse (b), polyethylene wear causing osteolyses (c) or femoro-tibial impingement (d) should be intraoperatively confirmed and documented. In the case of infection, thorough debridement, lavage and meticulous removal of the entire articular cartilage is indicated, followed by implantation of an antibiotic-loaded dual-compartment cement spacer. The authors do not advocate the use of single-compartment spacers as the bradytrophic osteo-chondral surface of the joint needs to be completely removed in order to adequately treat the infection
Tibial in situ referencing. After exposure of the tibial plateau, an intramedullary alignment rod is used to secure and position the 0° posterior slope tibial cutting jig (a). In rare cases, the intramedullary rod is not able to pass the tibial implant and an extramedullary jig system needs to be applied. The cutting jig and the initial resection level is set in a way that the sawblade just fits under the tibial implant (b). The authors recommend using the saw even in obviously loose tibial implants to minimize the defect created by the removal of the tray and the subjacent cement. If too much bone needs to be removed to achieve flush implant sitting on both the medial and the lateral tibia, a step cut should be performed to build up the medial defect with an augment. Prior to this step, it is essential to determine correct rotational tibial alignment and anticipate tibial implant size in order not to perform an incorrect sagittal tibia cut, which could negatively impact tibial implant rotation/positioning or result in excessive bone resection. Several modular revision systems offer tibial resection jigs with sagittal and horizontal slots that take the later medial augment width and height into consideration (c). If specific resection jigs of this kind are unavailable, the trial medial augment alone is positioned onto the medial resection surface. An angel wing can now be put through the resection jig to be positioned flush with the surface of the trial medial augment. The resection jig is pinned and the resection of the lateral plateau is performed (d). The trial tibial tray is now used to determine correct tibial implant rotation and size. In some cases, an additional freehand sagittal cut is necessary to adjust for correct tibial rotational alignment and medial augment width. Eventually, the trial tibia tray is pinned after assembly with the trial tibial augment and the keel or the stem extension is prepared (e)
Femoral in situ referencing. Prior to femoral component removal, rotational alignment is determined and intramedullary referencing for the distal femoral osteotomy is performed (a). The authors first use the femoral sizer set at 3° of external rotation to mark the transepicondylar line by sliding its paddles under the native and the resurfaced posterior condyle. An intramedullary alignment rod is then used and the distal femoral cutting jig positioned flush with the femoral implant and set according to the preoperatively determined valgus angle. The distal resection is performed while avoiding the femoral peg. Prior to definitive femoral implant removal, a fine osteotome is used to separate the implant from the bone of the posterior condyle. The symmetry of the extension gap can now be controlled with spacer blocks (b). Some modular revision systems offer the option to place hemi-augments on the medial side of the spacer block to account for the medial tibial defect. Whiteside’s line is marked. Rotational alignment must comply with the previously marked transepicondylar line (Insall line; c). At this stage, femoral size and definitive implant rotation needs to be determined by using the femoral sizer, which is provisionally pinned (d). With the 4‑in‑1 block pinned at the same place as the sizer, the knee joint is flexed to 90° and the symmetry of the flexion gap controlled with spacer blocks (e). At the same time, this step serves as a control step for correct femoral rotational alignment. The first chamfer cut is made through the slotted guide at the anterior femoral cortex to check for the “grand piano sign”, giving the surgeon another opportunity to ex post control rotational alignment (f) [21, 22]. If any of the aforementioned methods reveals malrotation of the unicondylar implant or previous posterior femoral over-resection, the use of a modular femoral implant is mandatory to account for the defect of the medial posterior femoral condyle. After the chamfer cuts are completed, remaining cement particles are carefully removed and trial implants are tested. The tourniquet is then inflated, smaller drill holes are placed at the cut surface to facilitate cement interdigitation and the bony surfaces are meticulously cleaned of debris and membranes by pulsed lavage. The bone obtained from the femoral box cut should be carefully preserved as this bone is ideal to fill smaller cavitary bone defects, especially at the tibia. After final implant bed preparation, the prosthesis is implanted applying cement to the implant and the previously dried bony surfaces
Postoperative management
-
Sterile wound dressing, elastic compression bandaging and local cryotherapy.
-
Deep vein thrombosis prophylaxis with low-molecular-weight heparins until full weight-bearing is achieved (regular monitoring of thrombocyte counts and/or anti-Xa activity).
-
If an intra-articular drain is applied, this should be removed after 24 h to allow for autonomy of the patient.
-
Patient mobilization with crutches under physiotherapist supervision ideally on the day of surgery.
-
Full weight-bearing or partial weight-bearing for 2 weeks postoperatively in the presence of bone or soft tissue defects.
-
Pharmacological pain management according to World Health Organization guidelines.
-
Continuous passive motion therapy. No limitation of active or passive range of motion.
-
Physiotherapy with gait training focusing on isometric and functional quadriceps control.
-
Regular clinical and radiographic follow-ups (directly postoperatively and at 6 and 12 months).
Errors, hazards and complications
-
Do not revise a UKA unless there is a diagnosis. Revision for unexplained pain results in poorer outcomes compared to situations in which the diagnosis is known [23].
-
Do not evoke wrong patient expectations: not every UKA is easy to revise. UKA revision is not always comparable to a primary TKA procedure.
-
Patients need to be informed that complications, complication rate and implant survivorship after UKA to TKA revision are similar to those after TKA to TKA revision [17].
-
In the case of significant femoral implant migration or tibial tray collapse, the in situ referencing technique is no longer applicable and the use of a modular revision system is mandatory. In this case, the referencing needs to be performed at the non-resurfaced compartments. At the femoral side, the distal femoral cutting jig is positioned at least 2 mm distal to the lateral condyle to account for the physiological distal femoral valgus angle. In such cases, the use of a modular revision system is mandatory as modular 4‑in‑1 blocks with augments are necessary to account for the medial femoral defect. At the tibial side, the position of the tibial cutting jig is determined by referencing at the non-resurfaced lateral compartment. During this step, the surgeon needs to take the later implant height into consideration. If a modular implant system is available, then the cuts are performed the other way round, as described in Fig. 4c. If no resection jig with sagittal and multiple horizontal slots—that take the later medial augment width and height into consideration—is available, then a correct step cut is difficult to perform, since most tibial resection jigs can be distalized only in 2‑mm increments and most augments measure 5 or 10 mm in height.
Results
Between January 2008 and January 2019, 84 consecutive patients (62 female, 22 male) underwent UKA to TKA revision at the Department of Orthopaedic Surgery of the Julius Maximilians University of Wuerzburg, Germany. Reasons for revision included aseptic loosening and/or polyethylene wear (n = 45), instability/malalignment (n = 12), progression of osteoarthritis (n = 18), infection (n = 2), recurrent dislocation of the insert (n = 4) and unexplained pain (n = 3). In 15 cases, the UKA had been performed at the authors’ clinic, while all others were referrals. The average time between the index operation and UKA to TKA revision was 3.8 years (45.2 months). Mean patient age at the time of UKA to TKA revision was 63.6 years (39–85 years). Operation and implant details as well as patient-reported outcomes were prospectively collected in the authors’ in-house arthroplasty database. Approval for retrospective data analysis was obtained from the University’s institutional review board (approval no. 2018122001). Mean follow-up after UKA to TKA revision was 5.3 years (64.0 months; 3–132).
In 73 patients (88.1%), a standard bicondylar implant was used for revision (seven cruciate-retaining, one condylar-stabilizing and 65 posterior-stabilized inserts). In 18 of these patients a tibial stem extension was utilized. Nine patients (10.7%) received a condylar-constrained implant. In five of these, a tibial and femoral stem extension was used, in four a tibial extension only. Tibial augments were used in seven of these patients, while one patient required tibial and femoral augmentation. Two patients (2.4%) were revised with a rotating hinge revision implant. Patella resurfacing was performed in 42 patients (50%). Two intraoperative complications were recorded during UKA to TKA revision. These were two intraoperative fractures of the medial tibial plateau during final implantation of the original component. Both cases were successfully treated by open reduction and internal screw fixation.
The Oxford knee score (OKS) and the visual analog scale (VAS) for pain were used to measure functional outcome after UKA to TKA revision. Complete pre- and postoperative data sets were available for 62 patients (73.8%). Implant status was available for all patients. Statistical analysis was performed using Sigma-Plot®13.0-Software. Values were recorded as mean, range and standard deviation (SD). The Saphiro-Wilk test was used to test whether the data was normally distributed. Statistically significant differences between the pre- and postoperative patient status were tested using the paired t‑test in the case of normally distributed data or the Wilcoxon test for non-normally distributed data. Implant survival was evaluated using Kaplan-Meier analysis (Fig. 6).
The mean OKS was 20.1 (6–39, SD ± 6.5) preoperatively and 30.2 (3–48, SD ± 11.3) postoperatively. The mean VAS was 6.9 (range 1–10, SD ± 1.8) preoperatively and 3.9 (range 0–9, SD ± 2.6) postoperatively. For both the OKS (p < 0.001) and the VAS (p < 0.001) there was a statistically significant difference between the pre- and postoperative status. Implant survival after UKA to TKA revision was 92% (95% CI = 82–97%) at 5 years of follow-up and 86% (95% CI = 69–93%) at 10 years of follow-up (Fig. 6). Seven patients underwent re-revision. The mean time to failure was 23.9 months (5–40; SD ± 12.1). Reasons for re-revision were aseptic loosening (n = 3), instability (n = 3) and infection (n = 1).
This study demonstrates that the described in situ referencing technique for UKA to TKA revision is reliable and safe and that the application of this technique can result in good mid-term and long-term outcomes. Of note, overall outcomes in the present study were not comparable to outcomes after primary TKA and are more comparable to the ones after TKA to TKA revision as previously described by other groups [14, 16]. Under certain circumstances, UKA to TKA revision can be a challenging and complex procedure—even after careful preoperative planning (Fig. 7). In the authors’ view, this procedure should therefore be performed by high-volume knee surgeons that are familiar with modular revision implants.
A 69-year-old female patient with malalignment and instability after unicompartmental knee arthroplasty (UKA). Good functional result 3 years after UKA to total knee arthroplasty (TKA) revision using a standard bicondylar implant with tibial stem extension and posterior-stabilized insert (a). A 66-year-old female patient suffering from aseptic loosening and osteolysis of the medial tibia plateau and lateral femoral condyle due to wear debris 8 years after UKA (for the corresponding intraoperative finding please see Fig. 3c). Status 12 months post revision surgery using a condylar-constrained implant with hybrid stem extensions and medial tibial 5‑mm augment. The contained defect of the lateral femoral condyle was filled with autologous bone obtained from the box cut (b)
References
Arnholdt J, Holzapfel BM, Sefrin L, Rudert M, Beckmann J, Steinert AF (2017) Individualized unicondylar knee replacement: use of patient-specific implants and instruments. Oper Orthop Traumatol 29(1):31–39
Arno S, Maffei D, Walker PS, Schwarzkopf R, Desai P, Steiner GC (2011) Retrospective analysis of total knee arthroplasty cases for visual, histological, and clinical eligibility of unicompartmental knee arthroplasties. J Arthroplasty 26(8):1396–1403
Bergeson AG, Berend KR, Lombardi AV Jr., Hurst JM, Morris MJ, Sneller MA (2013) Medial mobile bearing unicompartmental knee arthroplasty: early survivorship and analysis of failures in 1000 consecutive cases. J Arthroplasty 28(9 Suppl):172–175
Campi S, Tibrewal S, Cuthbert R, Tibrewal SB (2018) Unicompartmental knee replacement—Current perspectives. J Clin Orthop Trauma 9(1):17–23
Brown NM, Sheth NP, Davis K, Berend ME, Lombardi AV, Berend KR, Valle DCJ (2012) Total knee arthroplasty has higher postoperative morbidity than unicompartmental knee arthroplasty: a multicenter analysis. J Arthroplasty 27(8 Suppl):86–90
Fisher N, Agarwal M, Reuben SF, Johnson DS, Turner PG (2006) Sporting and physical activity following Oxford medial unicompartmental knee arthroplasty. Knee 13(4):296–300
Laurencin CT, Zelicof SB, Scott RD, Ewald FC (1991) Unicompartmental versus total knee arthroplasty in the same patient. A comparative study. Clin Orthop Relat Res (273):151–156. (PMID: 1959264)
Liddle AD, Judge A, Pandit H, Murray DW (2014) Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients: a study of data from the National Joint Registry for England and Wales. Lancet 384(9952):1437–1445
Murray DW, Liddle AD, Dodd CA, Pandit H (2015) Unicompartmental knee arthroplasty: is the glass half full or half empty? Bone Joint J 97-B(10 Suppl A):3–8
Furnes O, Espehaug B, Lie SA, Vollset SE, Engesaeter LB, Havelin LI (2007) Failure mechanisms after unicompartmental and tricompartmental primary knee replacement with cement. J Bone Joint Surg Am 89(3):519–525
Koskinen E, Paavolainen P, Eskelinen A, Pulkkinen P, Remes V (2007) Unicondylar knee replacement for primary osteoarthritis: a prospective follow-up study of 1,819 patients from the Finnish Arthroplasty Register. Acta Orthop 78(1):128–135
Thienpont E (2017) Conversion of a unicompartmental knee arthroplasty to a total knee arthroplasty: can we achieve a primary result? Bone Joint J 99-B(1 Supple A):65–69
Robb CA, Matharu GS, Baloch K, Pynsent PB (2013) Revision surgery for failed unicompartmental knee replacement: technical aspects and clinical outcome. Acta Orthop Belg 79(3):312–317
Jarvenpaa J, Kettunen J, Miettinen H, Kroger H (2010) The clinical outcome of revision knee replacement after unicompartmental knee arthroplasty versus primary total knee arthroplasty: 8–17 years follow-up study of 49 patients. Int Orthop 34(5):649–653
Hang JR, Stanford TE, Graves SE, Davidson DC, de Steiger RN, Miller LN (2010) Outcome of revision of unicompartmental knee replacement. Acta Orthop 81(1):95–98
Pearse AJ, Hooper GJ, Rothwell A, Frampton C (2010) Survival and functional outcome after revision of a unicompartmental to a total knee replacement: the New Zealand National Joint Registry. J Bone Joint Surg Br 92(4):508–512
Lunebourg A, Parratte S, Ollivier M, Abdel MP, Argenson JN (2015) Are revisions of unicompartmental knee arthroplasties more like a primary or revision TKA? J Arthroplasty 30(11):1985–1989
Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Valle DCJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection: from the Workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res 469(11):2992–2994
Della Valle C, Parvizi J, Bauer TW, DiCesare PE, Evans RP, Segreti J, Spangehl M, Watters WC 3rd, Keith M, Turkelson CM, Wies JL, Sluka P, Hitchcock K, American Academy of Orthopaedic S (2011) American Academy of Orthopaedic Surgeons clinical practice guideline on: the diagnosis of periprosthetic joint infections of the hip and knee. J Bone Joint Surg Am 93(14):1355–1357
Horas K, Arnholdt J, Steinert AF, Hoberg M, Rudert M, Holzapfel BM (2017) Acetabular defect classification in times of 3D imaging and patient-specific treatment protocols. Orthopäde 46(2):168–178
Cui WQ, Won YY, Baek MH, Kim KK, Cho JH (2006) Variations of the ‘grand-piano sign’ during total knee replacement. A computer-simulation study. J Bone Joint Surg Br 88(11):1441–1447
Ohmori T, Kabata T, Kajino Y, Taga T, Inoue D, Yamamoto T, Takagi T, Yoshitani J, Ueno T, Tsuchiya H (2018) Usefulness of the “grand-piano sign” for determining femoral rotational alignment in total knee arthroplasty. Knee 25(1):15–24
Jonas SC, Jermin P, Howells N, Porteous A, Murray J, Robinson J (2019) Outcome of revision UKR to TKR when compared to a matched group of TKR of same total arthroplasty lifespan. Knee 26(2):400–404
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Weißenberger, N. Petersen, S. Bölch, D. Rak, J. Arnholdt, M. Rudert and B.M. Holzapfel state that there are no conflicts of interest.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Additional information
Redaktion
D.C. Wirtz, Bonn
Zeichnungen
R. Himmelhan, Mannheim
Rights and permissions
About this article
Cite this article
Weißenberger, M., Petersen, N., Bölch, S. et al. Revision of unicompartmental knee arthroplasty using the in situ referencing technique. Oper Orthop Traumatol 32, 273–283 (2020). https://doi.org/10.1007/s00064-020-00656-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00064-020-00656-w