Abstract
Objective and design
Mesenchymal stem cells (MSCs) are potent modulators of immune responses. Sepsis is the association of a systemic inflammatory response with an infection. The aim of this study was to test the ability of MSCs derived from adipose tissue, which have immunomodulatory effects, and to inhibit the septic process in an experimental model of mice.
Methods
Three experimental groups (male C57BL/6 mice) were formed for the test: control group, untreated septic group and septic group treated with MSCs (1 × 106 cells/animal).
Results
In the control group, there were no deaths; in the untreated septic group, the mortality rate was 100 % within 26 h; in the septic group treated with MSCs, the mortality rate reached 40 % within 26 h. The group treated with MSCs was able to reduce the markers of tissue damage in the liver and pancreas. The treated group had a reduction of inflammatory markers. Furthermore, the MSCs-treated group was able to inhibit the increase of apoptosis in splenocytes observed in the untreated septic group.
Conclusions
Our data showed that MSCs ameliorated the immune response with decrease of inflammatory cytokines and increase anti-inflammatory IL-10; moreover, inhibited splenocytes apoptosis and, consequently, inhibited tissue damage during sepsis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Severe sepsis is currently a major cause of death in critically ill patients, with 750,000 new cases every year, and more than 200,000 fatalities [1]. With the increased use of invasive surgical procedures and immunosuppression, the incidence is likely to increase in the next few years. Furthermore, sepsis incurs a staggering $16.7 billion cost in the US health economy [1, 2].
Septic syndromes (sepsis, severe sepsis and septic shock, ranked by increased severity) are defined as the presence of infection associated with a systemic inflammatory response. The initial phase of the disease is dominated by an exacerbated inflammatory response (also called ‘cytokine storm’) responsible for successive organ failures and ultimately refractory hypotension leading to shock [3, 4]. Apoptosis is a major contributor to the pathophysiology of sepsis that leads to a striking loss of lymphocytes and dendritic cells. It also causes a decrease in the number of immune effector cells, combined with the immunosuppressive effect of apoptotic cells, and contributes to immunoparalysis, a major cause of morbidity and mortality in this disorder [5, 6]. Even with appropriate antibiotic and resuscitative therapies, sepsis carries a 30 % mortality rate and is significantly associated with organ failure. Thus, new therapeutic strategies are necessary to improve the outcome of septic patients [7].
Mesenchymal stem cells (MSCs) are multi-potent progenitor cells and can be cultured from adult and fatal tissues. They can regenerate different types of cell lines such as tendon, cartilage, bone and adipose cells. In the last decade, MSCs have been found to be potent modulators of immune responses [8–11]. The protective role of MSCs has also been tested in early clinical trials in cardiac disease, inflammatory bowel disease, stroke and several other clinical disorders [12–16]. More importantly, there is evidence that MSCs have a beneficial effect on preclinical models of polymicrobial sepsis. These studies showed that MSC injections into septic mice have reduced the septic inflammatory response and mortality by decreasing proinflammatory cytokine expression while increasing anti-inflammatory IL-10 [17, 18]. However, these studies did not address the response of MSCs derived from adipose tissue on cellular apoptosis associated with immune dysfunction during sepsis. Consequently, the purpose of this study was to investigate the role of murine MSCs derived from adipose tissue as a possible protection against the effects of the septic process. We conducted a survival curve comparing MSC-injected animals to a control septic. Furthermore, we analyzed the mechanisms involved in this protective effect such as the levels of tissue injury markers and the levels of pro and anti-inflammatory cytokines, and evaluated the apoptosis of splenocytes.
Materials and methods
Animals
Male C57BL/6 mice (8–12 weeks old) were kept on shelves with ventilated cages that provide 60 air cycles per hour, relative humidity ranging between 55 and 65 %, a 12-h light–dark cycle, temperature of 22 ± 2 °C with free access to food and water. The animals were maintained in accordance with the Guiding Principles in the Care and Use of Animals approved by the Council of the American Physiological Society. The experimental protocol was approved by the Ethics Research Committee of Pontifícia Universidade Católica do Rio Grande do Sul (protocol number 11/00252).
Cell culture
Murine MSCs were isolated, expanded, and characterized as previously described [19, 20]. Prior to the collection of the adipose tissue, mice were killed by cervical dislocation. Adipose tissue was obtained from the epididymal adipose tissue, cut into small pieces, collagenase digested, filtered and then cultured using DMEM Dulbecco’s Modified Eagle Medium (Invitrogen Corporation, California, USA) without ribonucleosides or deoxyribonucleosides containing 2 mM l-glutamine and 10 % fetal bovine serum (FBS) (Invitrogen, USA), with 1 % penicillin–streptomycin. Cells were passaged every 3–4 days by trypsinization when they reached 70–80 % confluence and were used for the experiments between passages 3 and 4. Between each passage, cell viability was measured using the trypan blue exclusion test. MSCs were cultured in a humidified incubator at 5 % CO2 and 37 °C under sterile conditions. Before each experiment, cells were trypsinized, counted, washed twice with PBS and resuspended in phosphate-buffered saline (PBS) (Gibco, USA). In all in vivo experiments, MSCs were used between passages 3 and 4.
Experimental sepsis induction and treatment
The animals were weighed and then anesthetized with a mixture of ketamine (80 mg/kg) and xylazine (20 mg/kg) intraperitoneally (i.p.). The abdomen of each animal was shaved and cleansed with povidone–iodine solution. A 1 cm midline abdominal incision was made to expose the linea alba. The peritoneum was opened by blunt dissection. All procedures were performed using sterile surgical instruments.
Sepsis was induced by introducing a sterile gelatin capsule size “1” in the peritoneal cavity containing another sterile capsule size “2” with the Escherichia coli (3 µL, ATCC 25922) suspension and a non-sterile fecal content (20 mg). E. coli was stored in autoclaved skimmed milk on glass beads at −70 °C. Each week, a bead was inoculated into trypticase soy agar and incubated overnight at 37 °C. The culture was passed daily for use the next day. Each day, a representative colony was transferred into a tube containing 10 mL of nutrient broth, incubated at 37 °C, and shaken for 2 h, until the optical density at 650 nm was between 0.280 and 0.300. The culture was diluted in pyrogen-free phosphate-buffered saline to yield 4 × 108 colony forming U/mL. This experimental model was adapted from technique developed in our laboratory [21].
The animals were then divided into three groups: (i) sham (mice were implanted with an empty capsule and received retro-orbital injection of 200 μL PBS), (ii) septic (sepsis-induced and received retro-orbital injection of 200 μL PBS), (iii) septic + MSCs (sepsis-induced and treated with 1 × 106 MSCs in retro-orbital injection of 200 μL PBS at the time of induction). Blood samples were collected using cardiac puncture 12 h after sepsis induction. This time was determined in previous studies in our laboratory [21] and previous works with sepsis and stem cells that collected samples for evaluation 12 h after induction of sepsis [17, 18]. The sepsis induction was evaluated by blood culture. All septic animals had positive blood culture for E. coli.
Survival curve
A survival curve for different experimental groups was performed. After 7 days, animals that were still alive were anesthetized with an i.p. solution of ketamine (100 mg/kg) and xylazine (50 mg/kg) and decapitated.
Body temperature
Body temperature was measured in animals using a rectal thermometer 12 h after sepsis induction.
Biochemical analysis
Biochemical analysis was performed on whole blood samples collected (12 h after sepsis induction) in tubes without anticoagulant and centrifuged (1,000×g for 5 min) after the clot retraction. The separated serum was then frozen at −70 °C until the time for analysis. Serum levels of aspartate aminotransferase (AST), alanine aminotransferase (ALT), glucose and amylase were measured using the commercial kits (Labtest Diagnóstica, Brazil) in a semi-automatic spectrophotometer (Spectronic/Genesis 8).
TGF-β1 quantification
Serum TGF-β1 concentration was measured in samples collected from mice 12 h after sepsis induction, using commercially available ELISA kit (R&D Systems, USA). The kit contained a specific monoclonal antibody immobilized on 96-well microtiter plate that bound TGF-β1 in the aliquot, and a second enzyme-conjugated specific polyclonal antibody. After washing away any unbound substances and antibodies, a substrate solution was added to the wells. Color development was stopped by sulfuric acid, and optical density was determined at 540 nm with the correction wavelength set at 570 nm in an ELISA plate reader. Results were calculated according to a standard curve concentration and multiplied by the dilution factor. TGF-β1 levels were expressed as pg/mL.
Cytokines quantification
To determine cytokine levels, serum samples were collected from mice 12 h after sepsis induction. Multiple soluble cytokines: interleukin-6 (IL-6), interleukin-12 p70 (IL-12 p70), interferon-γ (IFN-γ), tumor necrosis factor-α (TNF-α), interleukin-10 (IL-10) and monocyte chemotactic protein-1 (MCP-1) were simultaneously measured by flow cytometry using the cytometric bead array (CBA) Mouse Inflammation Kit (BD Biosciences, USA). Acquisition was performed with a FACSCanto II flow cytometer (BD Biosciences, USA). Quantitative results were generated using FCAP Array v1.0.1 software (Soft Flow Inc., Pecs, Hungary). The detection limit ranged between 20 and 5,000 pg/mL.
Splenocytes isolation
Single-cell suspensions of the removed spleens were prepared by passing the tissue through a 100-μm-pore size mesh Cellstrainer (Falcon, BD Biosciences, Heidelberg, Germany). The suspension was cleared from erythrocytes by treatment with Gey’s solution for 5 min, washed twice with PBS and resuspended in ISCOVE’s medium (PAA Laboratories GmbH, Germany) supplemented with 10 % heat-inactivated fetal calf serum, 100 U/mL penicillin and 100 μg/mL streptomycin (Invitrogen, USA). After counting splenocytes for each individual mouse, the cells of each group were pooled by taking equal number of cells from each mouse and adjusted to a concentration of 107 cells/mL [22]. Trypan blue exclusion assay was used as a means of determining cell viability.
Apoptosis quantification
Apoptosis was assessed using the FITC Annexin V Apoptosis Detection Kit I (BD Bioscience, USA). Briefly, 12 h after sepsis induction, the spleens were removed and the splenocytes isolated [21]. Cells were washed twice with PBS and resuspended in binding buffer before addition of FITC Annexin V and propidium iodide (PI). Cells were vortexed and incubated for 15 min, in the dark, at room temperature. A total of 10,000 events were acquired for each assayed sample. All data were acquired using a FACSCanto II flow cytometer (BD Biosciences). Data were analyzed using the FlowJo 7.2.5 software (Tree Star Inc., USA). Results are displayed as scatter dots allowing discrimination between viable cells, apoptotic cells with an intact membrane, and cells undergoing secondary necrosis.
Analysis of mitochondrial membrane potential (ΔΨm)
Breakdown of ΔΨm was determined by FACS analysis using the MitoScreen Kit (BD Biosciences, Germany). JC-1 dye (5,5,6,6-tetra-chloro-1,1,3,3-tetraethylbenzimidazol-carbocyanine iodide), which is selectively incorporated into mitochondria, is a sensitive and reliable method for the detection of changes in mitochondrial membrane potential (ΔΨm). Twelve hours after sepsis induction, the spleens were removed and the splenocytes isolated [22]. Cells were stained with 0.5 mL JC-1 solution for 15 min at 37 °C. Stained splenocytes were washed twice in JC-1 MitoScreen wash buffer. A total of 10,000 events were acquired for each assayed sample. All data were obtained immediately after staining on a FACSCanto II flow cytometer with CellQuest PRO v4.0.2 software (BD Biosciences, Germany). The results were displayed as scatter dots allowing discrimination between polarized and depolarized cells.
Statistical analysis
All data were expressed as mean ± standard error of the mean (SEM). The analysis of variance (ANOVA) followed by the post hoc Bonferroni test was used. Survival data were presented as Kaplan–Meier curves and the statistical significance was assessed by Mantel-Cox test. A level of p < 0.05 was considered statistically significant in all analyses. The statistical analysis was performed using Statistical Package for the Social Sciences (SPSS, USA), version 18.0.
Results
MSCs treatment improves survival and organ injury function in experimental model of sepsis
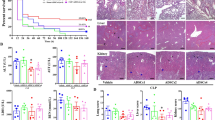
MSCs-treated mice had a reduction in mortality compared to the untreated group. The survival rate at 26 h was nearly 54.5 % in the sepsis + MSCs group, while in the sepsis group survival was 0 % (p < 0.001) (Fig. 1). Mice from both sepsis and sepsis + MSCs groups showed a decrease in their mean body temperature after 12 h of septic induction. MSCs administration did not attenuate the decline in temperature compared to sham group (p < 0.05) (Fig. 2).
Because the lethality of sepsis is associated with organ failure, we evaluated if treatment with MSCs was able to reduce tissue damage. The concentrations of liver enzymes (aspartate aminotransferase and alanine aminotransferase) were measured in serum. The sepsis induction showed an increase of AST and ALT in both sepsis and sepsis + MSCs groups, when compared to sham group; however, ALT levels in the sepsis + MSCs group were reduced when compared to the sepsis group (p < 0.05). This demonstrates that there was a reduction of liver damage (Fig. 3a, b).
The concentration of serum amylase was also measured, revealing a possible pancreatic damage. The sepsis group showed a significant increase compared to the sham group; however, the sepsis + MSCs group did not show a significant increase compared to the sham group (p < 0.05), demonstrating again the ability to prevent tissue damage exerted by MSCs (Fig. 4).
During sepsis, there is an increase in insulin resistance, generating hyperglycemia that leads to a decrease in energy intake. Therefore, we evaluated the glucose concentration 12 h after induction of septic in all groups. When compared to the sham group, both sepsis and sepsis + MSCs groups showed a significant increase (p < 0.05). This result showed that a treatment with MSCs did not prevent the increase of glycaemia (Fig. 5).
Effect of MSCs on serum cytokine concentrations
Recent evidence shows that MSCs may also exhibit immunosuppressive or immunomodulatory properties. Therefore, we studied multiple inflammatory cytokines (TNF-α, IL-12 p70, IFN-γ, IL-6 and MCP-1) and anti-inflammatory cytokines (IL-10 and TGF-β1). All cytokines were analyzed in serum 12 h after sepsis induction and MSC injection.
When the concentration of TNF-α was measured, an increase was observed in the sepsis group compared to the sham group (p < 0.05). In contrast, the septic + MSCs group did not show a significant increase compared to the sham group (Fig. 6a). IL-12, which is known to trigger other cytokines, did not have its bioactive form (p70) altered in both sepsis and sepsis + MSCs groups, compared to the sham group (Fig. 6b). Consequently, no significant alterations were observed in the concentration of IFN-γ (Fig. 6c). However, IL-6 and MCP-1 concentrations had a significant increase in the sepsis group compared to the sham group and the sepsis + MSCs group (p < 0.05) (Fig. 6d, e).
The concentration of IL-10 was measured showing a significant increase in the sepsis + MSCs group, when compared to both septic and the sham groups (p < 0.05) (Fig. 6f). In contrast, when we administered a dose of TGF-β1, another agent with an important role in the anti-inflammatory profile of MSCs, no significant differences were found between both sepsis + MSCs and the sham groups, but a significant increase was observed in the sepsis group compared to the sham group (p < 0.05). The MSCs treatment prevents the increase of TGF-β1 (Fig. 7).
MSCs prevents the increase of apoptosis in splenocytes during sepsis
During sepsis, there is extensive apoptotic death of lymphocytes and gastrointestinal epithelial cells. The extensive apoptotic death of lymphocytes is likely to be an important cause of the profound immunosuppression that is a hallmark of patients with sepsis. The potential importance of apoptosis in the pathophysiology of sepsis is illustrated by results from animal models, which demonstrate that blocking lymphocyte apoptosis by using caspase inhibitors improves survival in sepsis. The potential effect of MSCs on apoptosis was analyzed in splenocytes (isolates of the three experimental groups 12 h after starting the experiment) with two different method: the first method was used to detect the apoptotic cells by measuring the translocation of phosphatidylserine to the outer cell membrane surface, and the second, to measure the effect on mitochondrial transmembrane potential (ΔΨm).
Flow cytometric analysis of the Annexin V labeling assay detected an increase of apoptotic cells in the sepsis group compared to the sham group (p < 0.05). The treatment with MSCs (sepsis + MSCs group) significantly inhibited the increase of apoptosis (p < 0.05 vs. sepsis group) (Fig. 8).
Apoptotic cells were assessed using the FITC Annexin V (a) in different experimental groups. n = 10 for each group. *p < 0.05 vs. sham group. $ p < 0.05 vs. septic group. Thereunder, flow cytometric scatter plot of FITC annexin V/PI-stained sham group cells (b), septic group cells (c) and MSCs-treated group (d). Figures (b–d) represent one out of 10 experiments that were conducted
To assess the effects of treatment with MSCs on mitochondrial injury, we analyzed the ΔΨm in splenocytes. Changes of ΔΨm were determined by JC-1 staining of different experimental groups. The treatment did not cause significant changes in ΔΨm between the groups (Fig. 9).
Mitochondrial apoptotic cells were assessed using the FACS analysis (a) in different experimental groups. n = 11 for each group. Thereunder, flow cytometric scatter plot of the MSCs impact on ΔΨm: sham group (b), septic group (c) or MSCs-treated group (d). Figures (b–d) represent one out of ten experiments that were conducted
Discussion
The results showed that the mortality rate of the untreated septic group reached 100 % in 26 h. For the septic animals treated with MSCs, it was only 54.5 %. Our results corroborate previous studies that described the ability of mesenchymal stem cells to increase survival time in different animal models of sepsis [13, 17, 18]. These data revealed that, by some mechanism, the mesenquimal stem cells affected the septic process, reducing the mortality rate of the animals. Therefore, we have evaluated several mechanisms in order to elucidate the MSC function during sepsis, and how it can improve the survival of mice.
The material for biochemical and immunological analysis was collected 12 h after the experiment started. Before that, the body temperature of the animals was measured. Hypothermia was found in both sepsis and sepsis + MSCs groups. These data are not consistent with those found in the study by Krasnodembskaya et al. [18], where stem cells were able to prevent hypothermia. In this study, Krasnodembskaya used stem cells derived from bone marrow of humans as a treatment for peritoneal sepsis model in mice using P. aeruginosa. These differences in study design may have been critical to find a different result in our experiment.
An important marker of sepsis severity is hyperglycemia. Several studies in animals and septic patients are joining efforts to show that glycemic control can be effective as an adjuvant during the treatment of sepsis. Certain neuroendocrine and inflammatory mediators such as interleukin-1 (IL-1), interleukin-6 and tumor necrosis factor alpha (TNF-α) are involved in this hyperglycemia process [23–25]. This profile of blood glucose increase was observed in the sepsis group and also in the group treated with mesenchymal stem cells, demonstrating that MSCs had no influence on energy intake during the septic process.
The therapeutic benefits of MSCs transplantation have been observed in acute tissue injuries of the lung, heart, kidney and liver. The MSCs have been observed to migrate to injured sites following systemic administration. Tissue-specific engraftment is referred to as homing, and this aspect of MSCs therapy in disease may be essential for their medicinal effects [26]. The homing ability of MSCs has been demonstrated in the settings of wound healing, and tissue regeneration [7, 27]. It is likely that increased inflammatory chemokine concentration at the site of inflammation is a major factor causing MSCs to preferentially migrate to these sites. Chemokines are released after tissue damage, and MSCs express the receptors for several chemokines [7, 28, 29].
In our experiment, we have observed that stem cells derived from adipose tissue had also a positive response in preventing tissue injury through the analysis of serological markers of liver (ALT and AST) and pancreas (amylase) injury. The results obtained were effective in increasing the survival rate of animals treated with stem cells.
Multiple studies have demonstrated that MSCs can exert potent immunosuppressive effects by inhibiting the activity of both innate and adaptive immune system. This immunosuppression has been shown to be mediated by cell-contact-dependent and independent mechanisms through the release of soluble factors. In this study, the immunomodulatory ability of stem cells to respond to imbalance of inflammation was investigated.
The profile of the inflammatory cytokines was evaluated between the groups. The sepsis + MSCs group had a significant reduction in the concentration of TNF-α, IL-6 and MCP-1 when compared to the sepsis group. Several studies have demonstrated the effective participation of these cytokines in inflammatory response during sepsis [14, 30, 31]. TNF-α has several functions in the human immunopathology, as it produces inflammation, cell proliferation and differentiation, tumorigenesis, viral replication and inducing cell death by apoptosis through activation of caspase 8—known as the extrinsic apoptosis pathway in sepsis [3]. In clinical models of sepsis, the administration of TNF-α causes hypotension, activation of the coagulation cascade and organ dysfunction, confirming its role as a mediator for the acute phase response [32, 33].
The role of IL-6 in sepsis resolution is uncertain, although most evidence points towards more rapid declines in serum IL-6 being associated with sepsis resolution and improved outcome [34]. In the cecal ligation/perforation (CLP) sepsis model, mice genetically deficient in MCP-1 showed lower IL-10 production in peritoneal macrophages and increased mortality [35]. High serum levels of MCP-1 have been demonstrated in animal models of sepsis or systemic inflammatory response syndrome (SIRS), as well as in sepsis patients [36–38]. In a recent study profiling a large number of cytokines in the plasma of patients with severe sepsis, MCP-1 levels showed the best correlation with organ dysfunction and mortality [39]. MCP-1 is primarily a chemo attractant for monocytes, memory T lymphocytes, and natural killer cells, with some recent studies also pointing to a potential role in attracting neutrophils [40].
All the results showed that the reduction of inflammatory markers such as TNF-alpha, IL-6 and MCP-1 could be beneficial in sepsis. A reduction of these markers was found in our study, showing the positive impact of MSC treatment.
Nemeth et al. [17] reported that bone marrow-derived MSCs, activated by LPS or TNF-α, secreted PGE2, which reprogrammed alveolar macrophages to secrete IL-10. The beneficial effect of MSCs on mortality and improved organ function following sepsis (CLP) was eliminated by macrophage depletion or pretreatment with antibodies specific for interleukin-10 (IL-10) or IL-10 receptor, suggesting an essential role for IL-10. A dose of IL-10 was administered in all experimental groups and a significant increase of IL-10 was found in the septic group treated with stem cells, which corroborates previous studies, demonstrating that the role of this anti-inflammatory cytokine is very important in increasing survival of the animals and also in our experimental model. Previous studies on septic mice treated with MSCs showed that increased IL-10 is one of the key factors for reduced mortality and inflammatory response [17, 41].
Interestingly, when the concentration of TGF-β1 was evaluated (another important anti-inflammatory mediator during sepsis) an increase was observed in the septic group, compared to the sham group, and a significant decreased concentration in the septic + MSCs group, compared to the septic group. It occurred because we used an experimental model of severe sepsis and the material was collected 12 h after the experiment started. The animals were probably in a transition from an initial hyperinflammatory phase to a late sepsis, with an anti-inflammatory immune response that disables most immune functions by altering cytokine production, reducing lymphocyte proliferation and increasing apoptosis [42].
Apoptosis is a major cause of death in lymphocytes and gastrointestinal epithelial cells in patients with sepsis and trauma [43]. We performed the dissection of the spleens of mice and isolated splenocytes to check if there were more apoptotic cells in the septic group compared to the septic group treated with MSCs. Two different sets of flow cytometry were used; one to evaluate apoptosis through changes in the mitochondrial membrane potential; and the other to detect phosphatidylserine in cell membrane.
Immunohistochemical studies of spleens from patients dying of sepsis demonstrated focal regions, in which 25–50 % of cells were positive for apoptosis markers [43]. A study of circulating white blood cells from patients with sepsis showed that 15–20 % of circulating T and B cells were undergoing apoptosis [44]. Studies by Hotchkiss et al. showed that adoptive transfer of apoptotic splenocytes worsens survival when CLP is used as an experimental model of sepsis [45].
Stem cells possess anti-apoptotic mechanisms, which consist of upregulating DNA-repair, down-regulating mitochondrial death pathways, increasing antioxidant activity, and altering anti- and pro-apoptotic protein expression. These mechanisms can be especially important in sepsis, where mitochondrial dysfunction, oxidative stress, and apoptosis have clearly been implicated in pathological conditions [7]. Mei et al. [13] revealed the capacity of MSCs to prevent apoptotic cell death in the lung and kidneys of mice after CLP.
After completion of the analysis, it was possible to observe a significant increase in the number of apoptotic cells in the septic group compared to the group treated with stem cells. In contrast, the kit used to determine the mitochondrial potential exhibited an increase in the number of apoptotic cells; however, the results were not statistically significant. These findings corroborate several previous studies and show that MSC treatment can prevent the increase of apoptotic cells during sepsis by “delaying” the onset of immunosuppression, thereby help increase the survival time of animals.
In conclusion, the treatment with mesenchymal stem cells derived from adipose tissue was able to increase the survival time of septic-induced animals. Our data showed that MSCs modulate the immune system, inhibit cell apoptosis and, consequently, inhibit tissue damage during sepsis. These results corroborate other studies published and show the great potential that these cells have for treating sepsis. However, more efforts are needed to better understand the routes by which these cells operate. Considering their regenerative potential and immunoregulatory effect, MSC therapy is a promising tool to be used in clinical settings.
References
Angus DC, Linde-Zwirble WT, Lidicker JMA, Clermont G, Carcillo J, Pinsky MR. Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med. 2001;29:1303–10.
Nguyen HB, Rivers EP, Abrahamian FM, Moran GJ, Abraham E, Trzeciak S, Huang DT, Osborn T, Stevens D, Talan DA. Severe sepsis and septic shock: review of the literature and emergency department management guidelines. Ann Emerg Med. 2006;48:28–54.
Hotchkiss RS, Nicholson DW. Apoptosis and caspases regulate death and inflammation in sepsis. Nature. 2006;6:813–22.
Oberholzer A, Oberholzer C, Moldawer LL. Sepsis syndromes: understanding the role of innate and acquired immunity. Shock. 2001;16:83–96.
Huttunen R, Aittoniemi J. New concepts in the pathogenesis, diagnosis and treatment of bacteremia and sepsis. J Infect. 2011;63:407–19.
Rimmelé T, Kellum JA. Clinical review: blood purification for sepsis. Crit Care. 2011;15(1):205.
Wannemuehler TJ, Manukyan MC, Brewster BD, Rouch J, Poynter JA, Wang Y, Meldrum DR. Advances in mesenchymal stem cell research in sepsis. J Surg Res. 2011;173:113–26.
Gerlach H, Toussaint S. Managing septic shock. F1000 Medicine Reports 2010;2:40.
Barry FP, Murphy JM. Mesenchymal stem cells: clinical applications and biological characterization. Int J Biochem Cell Biol. 2004;36:568–84.
Baksh D, Song L, Tuan RS. Adult mesenchymal stem cells: characterization, differentiation, and application in cell and gene therapy. J Cell Mol Med. 2004;8:301–16.
Wang M, Crisostomo PR, Herring C, Meldrum KK, Meldrum DR. Human progenitor cells from bone marrow or adipose tissue produce VEGF, HGF and IGF-1 in response to TNF by a p38 mitogen activated protein kinase dependent mechanism. Am J Physiol Regul Integr Comp Physiol. 2006;291:880–4.
Weil BR, Manukyan MC, Herrmann JL, Wang Y, Abarbanell AM, Poynter JA, Meldrum DR. Mesenchymal stem cells attenuate myocardial functional depression and reduce systemic and myocardial inflammation during endotoxemia. Surgery. 2010;148:444–52.
Mei SHJ, McCarter SD, Deng Y, Parker CH, Liles WC, Stewart DJ. Prevention of LPS-induced acute lung injury in mice by mesenchymal stem cells overexpressing Angiopoietin 1. PLoS Med. 2007;4:1525–37.
Soleymaninejadia E, Pramanik K, Samadian E. Immunomodulatory properties of mesenchymal stem cells: cytokines and factors. Am J Reprod Immunol. 2012;67:1–8.
Lee JW, Gupta N, Serikov V, Matthay MA. Potential application of mesenchymal stem cells in acute lung injury. Expert Opin Biol Ther. 2009;9:1259–70.
van Poll D, Parekkadan B, Cho CH, Berthiaume F, Nahmias Y, Tilles AW, Yarmush ML. Mesenchymal stem cell-derived molecules directly modulate hepatocellular death and regeneration in vitro and in vivo. Hepatology. 2008;47:1634–43.
Németh K, Leelahavanichkul A, Yuen PST, Mayer B, Parmelee A, Doi K, Robey PG, Leelahavanichkul K, Koller BH, Brown JM, Hu X, Jelinek I, Star RA, Mezey E. Bone marrow stromal cells attenuate sepsis via prostaglandin E2-dependent reprogramming of host macrophages to increase their interleukin-10 production. Nat Med. 2009;15:42–9.
Krasnodembskaya A, Samarani G, Song Y, Zhuo H, Su X, Lee JW, Gupta N, Petrini M, Matthay MA. Human mesenchymal stem cells reduce mortality and bacteremia in gram negative sepsis in mice in part by enhancing the phagocytic activity of blood monocytes. Am J Physiol Lung Cell Mol Physiol. 2012;302:1003–13.
Mosna F, Sensebé L, Krampera M. Human bone marrow and adipose tissue mesenchymal stem cells: a user’s guide. Stem Cells Dev. 2010;19(10):1449–70.
Zuk PA, Zhu M, Mizuno H, Huang J, Futrell JW, Katz AJ, Benhaim P, Lorenz HP, Hedrick MH. Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng. 2001;7:211–28.
Nunes FB, Pires MGS, Filho JCFA, Wächter PH, Oliveira JR. Physiopathological studies in septic rats and the use of fructose-1,6-bisphosphate as cellular protection. Crit Care Med. 2002;30(9):2069–74.
Schulz SM, Köhler G, Holscher C, Iwakura Y, Alber G. IL-17A is produced by Th17, gammadelta T cells and other CD42 lymphocytes during infection with Salmonella enterica serovar Enteritidis and has a mild effect in bacterial clearance. Int Immunol. 2008;20:1129–38.
Ellger B, Debaveye Y, Vanhorebeek I, Langouche L, Giulietti A, Van Etten E, Herijgers P, Mathieu C, Van den Berghe G. Survival benefits of intensive insulin therapy in critical illness: impact of maintaining normoglycemia versus glycemia-independent actions of insulin. Diabetes. 2006;55:1096–105.
Branco RG, Tasker RC, Ramos Garcia PC, Piva JP, Dias Xavier L. Glycemic control and insulin therapy in sepsis and critical illness. J Pediatr. 2007;83:128–36.
Mizock BA. Alterations in fuel metabolism in critical illness: hyperglycaemia. Best Pract Res Clin Endocrinol Metab. 2001;15:533–51.
Yagi H, Soto-Gutierrez A, Parekkadan B, Kitagawa Y, Tompkins RG, Kobayashi N, Yarmush ML. Mesenchymal stem cells: mechanisms of immunomodulation and homing. Cell Transpl. 2010;19:667–79.
Mizuno H. Adipose-derived stem cells for tissue repair and regeneration: ten years of research and a literature review. J Nippon Med Sch. 2009;76:56–66.
Askari AT, Unzek S, Popovic ZB, Goldman CK, Forudi F, Kiedrowski M, Rovner A, Ellis SG, Thomas JD, DiCorleto PE, Topol EJ, Penn MS. Effect of stromal-cell-derived factor 1 on stem-cell homing and tissue regeneration in ischaemic cardiomyopathy. Lancet. 2003;362:697–703.
Rojas M, Xu J, Woods CR, Mora AL, Spears W, Roman J, Brigham KL. Bone marrow-derived mesenchymal stem cells in repair of the injured lung. Am J Respir Cell Mol Biol. 2005;33:145–52.
Hoogduijn MJ, Popp F, Verbeek R, Masoodi M, Nicolaou A, Baan C, Dahlke MH. The immunomodulatory properties of mesenchymal stem cells and their use for immunotherapy. Int Immunopharmacol. 2010;10:1496–500.
Ren G, Zhang L, Zhao X, Xu G, Zhang Y, Roberts AI, Zhao RC, Shi Y. Mesenchymal stem cell-mediated immunosuppression occurs via concerted action of chemokines and nitric oxide. Cell Stem Cell. 2008;2:141–50.
Muenzer JT, Davis CG, Chang K, Schmidt RE, Dunne WM, Coopersmith CM, Hotchkiss RS. Characterization and modulation of the immunosuppressive phase of sepsis. Infect Immun. 2010;78:1582–92.
Qiu P, Cui X, Barochia A, Li Y, Natanson C, Eichacker PQ. The evolving experience with therapeutic TNF inhibition in sepsis: considering the potential influence of risk of death. Expert Opin Investig Drugs. 2011;20:1555–64.
Webb S. The role of mediators in sepsis resolution. Adv Sepsis. 2002;2:8–14.
Gomes RN, Figueiredo RT, Bozza FA, Pacheco P, Amâncio RT, Laranjeira AP, Castro-Faria-Neto HC, Bozza PT, Bozza MT. Increased susceptibility to septic and endotoxic shock in monocyte chemoattractant protein 1/CC chemokine ligand 2-deficient mice correlates with reduced interleukin 10 and enhanced macrophage migration inhibitory factor production. Shock. 2006;26:457–63.
Matsukawa A, Hogaboam CM, Lukacs NW, Lincoln PM, Strieter RM, Kunkel SL. Endogenous monocyte chemoattractant protein-1 (MCP-1) protects mice in a model of acute septic peritonitis: cross-talk between MCP-1 and leukotriene B4. J Immunol. 1999;163:6148–54.
Matsukawa A, Hogaboam CM, Lukacs NW, Lincoln PM, Strieter RM, Kunkel SL. Endogenous MCP-1 influences systemic cytokine balance in a murine model of acute septic peritonitis. Exp Mol Pathol. 2000;68:77–84.
Bossink AWJ, Paemen L, Jansen PM, Hack CE, Thijs LG, Van Damme J. Plasma levels of the chemokines monocyte chemotactic proteins-1 and -2 are elevated in human sepsis. Blood. 1995;86:3841–7.
Bozza FA, Salluh JI, Japiassu AM, Soares M, Assis EF, Gomes RN, Bozza MT, Castro-Faria-Neto HC, Bozza PT. Cytokine profiles as markers of disease severity in sepsis: a multiplex analysis. Crit Care. 2007;11:R49.
Speyer CL, Gao H, Rancilio NJ, Neff TA, Huffnagle GB, Sarma JV, Ward PA. Novel chemokine responsiveness and mobilization of neutrophils during sepsis. Am J Pathol. 2004;165:2187–96.
Gonzalez-Rey E, Anderson P, González MA, Rico L, Büscher D, Delgado M. Human adult stem cells derived from adipose tissue protect against experimental colitis and sepsis. Gut. 2009;58:929–39.
Monneret G. How to identify systemic sepsis-induced immunoparalysis. Adv Sepsis. 2005;4:42–9.
Hotchkiss RS, Tinsley KW, Swanson PE, Schmieg RE Jr, Hui JJ, Chang KC, Osborne DF, Freeman BD, Cobb JP, Buchman TG, Karl IE. Sepsis-induced apoptosis causes progressive profound depletion of B and CD4 + T lymphocytes in humans. J Immunol. 2001;166:6952–63.
Le Tulzo Y, Pangault C, Gacouin A, Guilloux V, Tribut O, Amiot L, Tattevin P, Thomas R, Fauchet R, Drénou B. Early circulating lymphocyte apoptosis in human septic shock is associated with poor outcome. Shock. 2002;18:487–94.
Hotchkiss RS, Chang KC, Grayson MH, Tinsley KW, Dunne BS, Davis CG, Osborne DF, Karl IE. Adoptive transfer of apoptotic splenocytes worsens survival, whereas adoptive transfer of necrotic splenocytes improves survival in sepsis. PNAS. 2003;100:6724–9.
Acknowledgments
This work was supported by CAPES (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior). The authors thank Msc Stéphanie Gallo and Lucas Bortolotto Rizzo for their technical support. The authors also thank Dr Eduardo Pedrazza for his assistance.
Conflict of interest
The authors declare that there was no conflict of interest in this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: Kumar Visvanathan.
Rights and permissions
About this article
Cite this article
Pedrazza, L., Lunardelli, A., Luft, C. et al. Mesenchymal stem cells decrease splenocytes apoptosis in a sepsis experimental model. Inflamm. Res. 63, 719–728 (2014). https://doi.org/10.1007/s00011-014-0745-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-014-0745-1