Abstract
Objective
The present study evaluates the anti-inflammatory effect of the quinoline alkaloid skimmianine (SKM), isolated from Ruta graveolens L., against carrageenan-induced acute inflammation.
Methods
SKM at a dose of 5.0 mg/kg body weight was found to be the minimal concentration for maximal edema inhibition. Carrageenan suspension was administered into the sub-plantar tissue of the right hind paw 1 h after SKM and diclofenac (20 mg/kg) administration (i.p.). Paw edema was determined 3 h after carrageenan administration. The rats were then killed and mRNA expressions of TNF-α and IL-6, levels of PGE2 and TBARS, activities of COX-2, 5-LOX, SOD, catalase, glutathione peroxidase (GPx) and myeloperoxidase (MPO) and the level of nitrite were measured.
Results
SKM treatment resulted in a decrease in the mRNA levels of TNF-α and IL-6, which are upstream events of the inflammatory cascade. The levels of PGE2 and NO and the activities of COX-2 and 5-LOX were also significantly reduced after SKM treatment. Neutrophil infiltration, lipid peroxidation and associated oxidative stress in the paw tissue were reduced following SKM treatment.
Conclusion
These results support the anti-inflammatory properties of skimmianine and its multi-targeted mechanism of action, suggesting its potential therapeutic efficacy in various inflammatory diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammation is essentially a defensive response aimed at protecting organisms against physical, chemical and infective insults. Frequently, however, dysregulation of this response leads to damage of normal tissues. Prostaglandin E2 (PGE2), a key mediator of inflammatory response, is generated at sites of inflammation in substantial amounts from arachidonic acid by the enzyme cyclooxygenase (COX) and mediates many of the associated pathological features [1]. One of the early cellular events in inflammation is the infiltration/localization of polymorphonuclear leukocytes (PMN). The enzyme myeloperoxidase (MPO), present in the azurophilic granules of PMN, is unique to neutrophils and monocytes/macrophages. However, monocytes contain only one third of the MPO found in PMN’s. MPO activity can be used as an indicator of neutrophil accumulation [2]. Nitric oxide (NO) plays an important role in inflammation and inhibitors of NO synthase (NOS) have been shown to reverse several classic inflammatory symptoms [3].
The pro-inflammatory cytokine, tumor necrosis factor-α (TNF-α) was observed to stimulate neutrophils to synthesize and release several cytokines and chemokines [4]. Although conventional therapeutic approaches with non-steroidal anti-inflammatory drugs (NSAIDs) have been very successful in managing pain and inflammatory conditions [5], the rather discouraging profile of side effects has emerged as a constraint [6]. Even newer anti-inflammatory drugs like COX-2 inhibitors are not devoid of adverse effects [7]. Some studies have revealed the role played by oxidative stress in the origin of inflammation, which has led to investigation of the use of antioxidants as a countermeasure [8]. Natural antioxidants, which are ubiquitous in fruits, vegetables and medicinal plants, have received great attention and have been studied extensively, since they are effective free-radical scavengers and are assumed to be less toxic than synthetic antioxidants [9]. Through years of ingenious syntheses and structural modifications that usually follow the design and development of new drugs, many NSAIDS have been prepared and marketed [10]. However, these drugs are known to provoke adverse effects. Hence, a search for alternative anti-inflammatory drugs, mainly from natural herbs, is required.
Ruta graveolens L. (Rutaceae), commonly known as rue, has been reported to have medicinal properties against aching pain, eye problems, rheumatism and dermatitis since ancient times [11]. R. graveolens is native to the Mediterranean region but is also cultivated throughout Europe and many Asian countries, including China, India and Japan. The plant contains more than 120 compounds belonging to different classes of natural products such as alkaloids, coumarins, essential oils, flavonoids and furoquinolines [12]. These compounds are of great interest to medicinal chemistry due to their broad range of biological activity. The anti-inflammatory effects of the total alkaloid fraction isolated from R. graveolens against adjuvant-induced arthritis was reported by our group [13]. Further analysis of this total alkaloid fraction yielded seven active fractions, designated F1–F7. Of the seven fractions, the F2 fraction demonstrated significant paw edema inhibition in the carrageenan-induced acute paw edema model. Structural analysis of this F2 fraction identified the active component to be skimmianine. Previous studies with skimmianine also demonstrated anti-inflammatory effect in an ear edema model [14]. In this study, skimmianine was demonstrated to inhibit the release of histamine, intracellular Ca2+ signaling and protein kinase C signaling. These effects play a role in granule exocytosis [15]. In a separate study, skimmianine was found to inhibit formyl-l-methionyl-l-leucyl-l-phenylalanine/cytochalasin B (FMLP/CB)-induced elastase release [16]. The present study was designed to investigate the efficacy of skimmianine in the prevention of carrageenan-induced paw edema and in understanding the biochemical mechanism involved.
Materials and methods
All biochemicals used in this study were purchased from Sigma Chemical Company, St Louis, MO, USA. Commercially available diclofenac (Novartis, Hyderabad, India) was used as the standard anti-inflammatory drug for the study. Deuterated solvents for NMR were bought from Merck, and other chemicals and solvents used were of analytical grade from SRL Chemicals, Mumbai, India. IR spectroscopy was performed and was recorded using a Spectrum One FT-IR spectrometer (Perkin-Elmer). 1H-NMR (500 MHz) and 13C-NMR (125 MHz) were recorded in CDCl3 using a Bruker AMX 500 spectrometer (Bruker Avance II 500) with TMS as the internal standard. Mass spectra were recorded under FAB/LRMS at 5000 resolution using a JMS 600H (JEOL) mass spectrometer.
Plant material
Fresh plant material was collected from Kannur district in Kerala, India, and was authenticated by a botanist (Dr. G. Valsaladevi, Department of Botany, University of Kerala, India).
Extraction and isolation of skimmianine
The dried and powdered aerial part of Ruta graveolens (5 kg) was extracted with hexane and methanol (MeOH). The MeOH extract obtained was fractionated over silica gel 60 (70–230 mesh) into three fractions: dichloromethane (CH2Cl2), ethyl acetate (EtOAc) and MeOH. The methanol fraction (82 g) was dissolved in H2O:MeOH (3:7) and successively partitioned using solvents of increasing polarity (hexane and CH2Cl2). The CH2Cl2 subfraction (2 g) was chromatographed over silica gel (230–400 mesh) with a step gradient (10 % steps) of ethyl acetate in CH2Cl2. Skimmianine (20 mg) was obtained from the F2 fraction [CH2Cl2:EtOAc (90:10)]. The identity was confirmed by TLC, mass spectrum and NMR analysis. The spectral data presented are in agreement with previous literature reports [17, 18].
Skimmianine was isolated as colourless prisms (20 mg): R
f = 0.81 (20 % ethyl acetate:chloroform). mp: 178–179 °C; 1H-NMR (500 MHz, CD3Cl3): δ 8.017 (d, J = 9 Hz, 1H), δ 7.58 (d, J = 2.5 Hz, 1H), δ 7.24 (d, J = 9.5 Hz, 1H), δ 7.04 (d, J = 2.5 Hz, 1H), δ 4.43(s, 3H), δ 4.12 (s, 3H), δ 4.03(s, 3H); 13C-NMR (125 MHz, CD3Cl3): δ 56.8, 59.0, 61.7, 102.0, 104.6, 112.1, 114.9, 118.2, 141.5, 142.0, 143.0, 152.1, 157.2, 164.3 ppm; IR (KBr): \( \bar{\nu } \) = 3117, 2980, 2835, 1616, 1577, 1504, 1390, 1365, 1269, 1105, 997 cm−1; UV/VIS (CH3OH): λ
max (ε) = 248(0.7), 327(0.08). HRMS-FAB m/z [M + H]+ calcd for C14H13NO4: 259.26, found: 259.08. 
Animal experiments
Adult male Wistar rats (weighing 150 ± 10 g) bred in the host department animal facility were used for this study. They were kept in a environment controlled for temperature (24–26 °C), humidity (55–60 %) and photoperiod (12:12 h light–dark cycle). A commercial balanced laboratory diet (Amrut Laboratory Animal Feeds, Maharashtra, India) and tap water were provided ad libitum. The animals received humane care, in compliance with the host institutional animal ethics guidelines. All experiments were conducted according to the guidelines of the animal ethics committee CPCSEA (Registration no. 218/CPCSEA) according to the Government of India accepted principles for laboratory animal use and care.
Dose–response and toxicity studies
A dose–response study on the anti-inflammatory activity of skimmianine against carrageenan-induced paw edema model was carried out in the range of 1–10 mg/kg body weight (bw). From this, a dose of 5 mg/kg bw was found to be the minimal concentration for maximal edema inhibition.
A toxicity curve for skimmianine was carried out in the dose range 1–100 mg/kg bw and toxicity parameters like GOT, GPT and LDH were analyzed. Skimmianine was found to exhibit no toxicity effect up to 100 mg/kg bw (data not shown). Hence the minimal effective dose of 5 mg/kg bw was selected for further evaluation of the anti-inflammatory effect of skimmianine.
Treatment protocol and experimental design for acute inflammation
Anti-inflammatory activity was measured using the carrageenan-induced rat paw edema assay [19]. The male Wistar rats were randomly divided into five groups with six rats in each.
Group 1: Control (0.5 % DMSO in normal saline), Con.
Group 2: Skimmianine (5 mg/kg bw), Con + SKM.
Group 3: Carrageenan, Carr.
Group 4: Carrageenan + Skimmianine (5 mg/kg bw), Carr + SKM.
Group 5: Carrageenan + Diclofenac (20 mg/kg bw), Carr + Dic.
The diclofenac dose (20 mg/kg bw) used for the current study has been previously used in our laboratory as a standard anti-inflammatory drug; 20 mg/kg bw of diclofenac was found to significantly induce paw edema inhibition, with very little toxic effects in rats [13, 20]. Skimmianine was dissolved in DMSO and carried over into normal saline (0.5 % DMSO). The skimmianine and standard drug diclofenac were given intraperitoneally, followed after 1 h by injection of 1 % carrageenan suspension in 0.9 % NaCl solution into the sub-plantar tissue of the right hind paw. Paw volume was measured at hourly intervals for 3 h by a paw edema meter (Marsap Pvt. Ltd., USA). Anti-inflammatory activity was measured as the percentage reduction in edema level when treated with extract as compared to control. Activity = 100 − (100 × average for drug-treated/average for control). At the end of their third hour, animals were killed by euthanasia. Blood and paw tissue was collected for various biochemical analyses.
Paw sample preparation
After death, paws from experimental rats were amputated above the ankle, degloved, and snap-frozen in liquid nitrogen. Frozen paws were pulverized in a liquid nitrogen bath and divided into aliquots for extraction and analysis of COX-2, MPO, thiobarbituric acid reactive substance (TBARS) and cytokine mRNAs. Samples were processed immediately or stored at −70 °C for use within 24 h.
Myeloperoxidase activity assay
The neutrophil marker enzyme, myeloperoxidase (MPO), was measured using the method of Bradley et al. [21]. The paw tissue was homogenized in 50 mM K2HPO4 buffer (pH 6.0) containing 0.5 % hexadecyl trimethylammonium bromide (HTBA) using a homogenizer. After freeze-thawing three times, the samples were centrifuged at 2,500g for 30 min at 4 °C to obtain the supernatant. MPO activity was measured by mixing 40 μL of supernatant with 960 μL of 50 mM phosphate buffer, pH 6, containing 0.167 mg/mL O-dianisidine dihydrochloride and 0.0005 % hydrogen peroxide. The change in absorbance at 460 nm was measured spectrophotometrically. One unit of MPO activity was defined as that amount of enzyme degrading 1 μmol of peroxide per minute at 25 °C, and the activity is expressed as units per mg of tissue.
Superoxide dismutase activity assay
SOD activity was measured according to the method of Kakkar et al. [22]. The assay mixture contained 0.1 mL of supernatant, 1.2 mL of sodium pyrophosphate buffer (pH 8.3; 0.052 M), 0.1 mL of phenazine methosulphate (186 μM), 0.3 mL of nitroblue tetrazolium (NBT; 300 μM) and 0.2 mL of NADH (750 μM). The reaction was started by addition of NADH. After incubation at 30 °C for 90 s, the reaction was stopped by addition of 0.1 mL of glacial acetic acid. The reaction mixture was stirred vigorously with 4.0 mL of n-butanol. The colour intensity of the chromogen in the butanol layer was measured spectrophotometrically at 560 nm. One unit of enzyme activity was defined as that amount of enzyme which caused 50 % inhibition of NBT reduction/mg protein.
Catalase activity assay
Catalase activity (CAT) was measured by the method of Aebi [23]. An aliquot (5 μL) of each tissue supernatant was added to a cuvette containing 1.995 mL of 50 mM phosphate buffer (pH 7.0). The reaction was started by the addition of 1.0 mL of freshly prepared 30 mM H2O2. The rate of decomposition of H2O2 was measured spectrophotometrically at 240 nm.
Glutathione peroxidase assay
Paw tissue glutathione peroxidase (GPx) was assayed in a 1 mL cuvette containing 0.890 mL of 100 mM potassium phosphate buffer (pH 7.0), 1 mM EDTA, 1 mM NaN3, 0.2 mM NADPH, 1 U/mL GSH reductase and 1 mM GSH. 10 μL of each paw tissue homogenate was added to make a total volume of 0.9 mL. The reaction was initiated by the addition of 100 μL of 2.5 mM H2O2, and the conversion of NADPH to NADP+ was monitored spectrophotometrically at 340 nm for 3 min. GPx activity was expressed as nmoles of NADPH oxidized to NADP+/min/mg protein, using a molar extinction coefficient of 6.22 × 106 (cm−1 M−1) for NADPH [24].
Measurement of thiobarbituric acid reactive substance
TBARS levels were measured by the double heating method [25], which is based on spectrophotometric measurement of the purple colour generated by the reaction of thiobarbituric acid (TBA) with malondialdehyde. Briefly, 0.5 mL of paw tissue homogenate was mixed with 2.5 mL of trichloroacetic acid (TCA, 10 %, w/v) solution followed by boiling in a water bath for 15 min. After cooling to room temperature, the samples were centrifuged at 3,000 rpm for 10 min and 2 mL of each sample supernatant was transferred to a test tube containing 1 mL of TBA solution (0.67 %, w/v). Each tube was then placed in a boiling water bath for 15 min. After cooling to room temperature, the absorbance with respect to the blank solution was measured at 532 nm.
Determination of cycloxygenase-2 activity in paw tissue
COX-2 activity was checked using a colorimetric assay kit purchased from Cayman Chemicals, USA. The COX-2 activity assay utilizes the peroxidase component of cyclooxygenases. The peroxidase activity is assayed colorimetrically by monitoring the appearance of oxidized N,N,N′,N′-tetramethyl-p-phenylenediamine (TMPD) at 590 nm. Briefly, the paw tissue after experimental period was dissected and rinsed with Tris buffer (pH 7.4) to remove any red blood cells and clots. Tissue was homogenized in cold 0.1 M Tris–HCl (pH 7.8) containing 1 mM EDTA and spun at 10,000g for 15 min at 4 °C. The supernatant obtained was used for the COX assay. A COX-1 specific inhibitor, SC560, was used in the assay to eliminate non-COX-2 activity.
Activity of 5-lipoxygenase in peripheral blood mononuclear cells
Peripheral blood mononuclear cells (PBMC) were prepared as described by Radhika et al. [26]. A 3 ml volume of Histopaque 1083-solution was placed in a 15 ml tube and 3 ml blood was layered on top of this density gradient. After centrifugation (400g for 30 min at room temperature) and discarding the plasma layer, the buffy coat layer containing PBMC was carefully taken off by aspiration and washed twice with phosphate-buffered saline (PBS). The resultant pellet was resuspended in PBS-Tween and subjected to a freeze–thaw cycle three times. The resulting lysate was used as the enzyme source. 5-Lipoxygenase (5-LOX) activity was measured by the method of Axelrod et al. [27].
Reverse transcription–polymerase chain reaction
The levels of TNF-α and IL-6 mRNA were measured by semi-quantitative reverse transcription–polymerase chain reaction (RT-PCR). Total RNA was isolated from paw tissues using a RNA isolation mini kit (Sigma Aldrich, USA) according to the manufacturer’s instructions. The sequences of the primers used are shown in Table 1. GAPDH primers were used as an internal control for RNA loading. RT-PCR was performed in an Eppendorf thermocycler using a two step RT-PCR kit where reverse transcription and DNA amplification was done separately. 2 μg of total RNA was used as template in the first reaction that included dNTPs, oligo (dT) and reverse transcriptase enzyme. The second reaction included appropriate primers, PCR enzyme, cDNA formed in the first step and dNTPs. The PCR conditions were as follows: denaturation at 94 °C for 4 min; 35 cycles of 94 °C for 30 s, primer annealing for 30 s, and 72 °C for 1 min; and then a final extension at 72 °C for 3 min. The PCR products were separated by electrophoresis on 1.5 % agarose gel containing ethidium bromide, visualized under a UV-transilluminator, and the relative intensities of bands of interest were measured on a GelDoc 2000 scanner (Bio-Rad, CA, USA) with scan analysis software.
Determination of PGE2 level
Paw tissues were added to 4 ml/g tissue of lysis solution containing 80 % methanol, 20 % saline and 1 mM indomethacin. Tissues were homogenized on ice with a Polytron and centrifuged at 5,000g for 15 min. The supernatants were stored at −70 °C until analyzed. The PGE2 levels were determined using a PGE2 EIA kit (Cayman Chemicals, Ann Arbor, MI, USA). The sensitivity of the PGE2 assay was 15 pg/ml as per the manufacturer’s instructions.
Determination of NO concentrations in serum
NO was measured as its breakdown product of nitrite by using the Griess method [28]. In the presence of H2O, NO is rapidly converted into nitrite and nitrate. Total production of NO may therefore be determined by measuring the stable NO metabolite nitrite (NO2 −). Equal volumes of paw tissue supernatant and Griess reagent (1 % sulphanilamide and 0.1 % N-[naphthyl]ethylenediamine dihydrochloride, 1:1) were mixed and the absorbance measured at 550 nm. The amount of nitrite was calculated from a NaNO2 standard curve.
Statistical analysis
All statistical calculations were carried out with Statistical Package for Social Sciences (SPSS) software (version 11.0 for Windows). The values are expressed as the mean ± SEM. Statistical evaluation was done using one-way ANOVA and significant differences were determined using Duncan’s test at the level of p ≤ 0.05.
Results
Effect of skimmianine on percentage edema inhibition
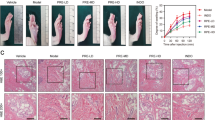
The percentage edema inhibition by different doses of skimmianine isolated from R. graveolens in the carrageenan-induced acute model is shown in Fig. 1. Skimmianine at a dose of 5 mg/kg bw showed 82 % edema inhibition, significantly higher than that of the standard drug diclofenac. Skimmianine at a dose of 5.0 mg/kg bw was found to be the minimal concentration for maximal edema inhibition. Hence the dose 5 mg/kg bw dosage was selected for further evaluation of the anti-inflammatory effects of skimmianine.
Effect of skimmianine on the paw edema (dose–response). Skimmianine at a dose of 5.0 mg/kg bw was found to be the minimal concentration for maximal edema inhibition. Values are expressed as mean ± SEM (n = 6 per group). *p ≤ 0.05 compared to Dic, # p ≤ 0.05 compared to SKM (1.0 mg/kg), ¥ p ≤ 0.05 compared to SKM (2.5 mg/kg). Dic represents animals administered an i.p. injection of 20 mg/kg diclofenac. SKM represents animals administered an i.p. injection of skimmianine (1.0, 2.5, 5.0, 7.5 and 10.0 mg/kg bw). Dic and SKM were administered as a pre-treatment, 1 h after which animals in all the groups received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema. Paw volume was measured using a paw edema meter
Effect of skimmianine on the concentration of PGE2
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in PGE2 levels compared to the control (Con) group. PGE2 levels significantly increased in carrageenan-treated rats (Carr) compared to the Con group. Diclofenac administration (Carr + Dic) significantly reduced the concentration of PGE2 compared to the Carr group. However, animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the concentration of PGE2 compared to the carrageenan (Carr) and a non-significant decrease compared to the diclofenac (Carr + Dic) administered groups (Fig. 2).
Effect of skimmianine on the concentration of PGE2 in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the concentration of PGE2 when compared to the carrageenan group (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on COX-2 and 5-LOX activities
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in the activities of COX-2 in paw tissue and 5-LOX in PBMC compared to the control (Con) group. COX-2 activity in paw tissue and 5-LOX activity in PBMC was significantly increased in carrageenan-treated rats (Carr) compared to the control group (Con). Diclofenac administration (Carr + Dic) significantly reduced the activity of COX-2 and 5-LOX compared to the Carr group. However, animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the activity of COX-2 compared to the Carr group. The activity of 5-LOX showed a significant decrease in animals pre-treated with skimmianine compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups (Figs. 3, 4).
Effect of skimmianine on the activity of COX-2 in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the activity of COX-2 compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the activity of 5-LOX in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the activity of 5-LOX compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents the animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents the animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the activity of MPO
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in MPO activity in paw tissue compared to control (Con) group. MPO activity in paw tissue was significantly increased in carrageenan-treated rats (Carr) compared with the control group (Con). Diclofenac administration (Carr + Dic) significantly reduced the activity of MPO compared to the Carr group. However, animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the activity of MPO compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups (Fig. 5).
Effect of skimmianine on the activity of MPO in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the activity of MPO compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the activity of antioxidant enzymes
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) slightly increased their antioxidant status through an increase in the activities of SOD, catalase and GPx in paw tissue compared to the control (Con) group. Carrageenan treatment (Carr) resulted in a significant reduction in activities of SOD, catalase and GPx in paw tissue compared with the control group (Con). Diclofenac administration (Carr + Dic) significantly increased the activity of catalase and GPx compared to the Carr group. However, animals pre-treated with skimmianine (Carr + SKM) showed a significant increase in the activities of all the anti-oxidant enzymes compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups (Fig. 6).
Effect of skimmianine on the activity of anti-oxidant enzymes in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant increase in the activity of SOD, catalase and GPx compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents the animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents the animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the level of lipid peroxidation product, TBARS
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in the levels of TBARs compared to the control (Con) group. The TBARS level was significantly increased in tissue homogenates in carrageenan-treated rats (Carr) in comparison with the control group (Con). Diclofenac administration (Carr + Dic) significantly reduced the levels of TBARS compared to the Carr group. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the level of TBARS compared to the carrageenan (Carr) and a non-significant decrease compared to the diclofenac (Carr + Dic) administered groups (Fig. 7).
Effect of skimmianine on the concentration of TBARS in paw tissue. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the level of TBARs compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents the animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the level of nitrite
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in the concentration of nitrite in the serum compared to the control (Con) group. The concentration of nitrite was significantly increased in serum in carrageenan-treated rats (Carr) in comparison with the control group (Con). Diclofenac administration (Carr + Dic) significantly reduced the concentration of nitrite compared to the Carr group. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the concentration of nitrite compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups (Fig. 8).
Effect of skimmianine on the concentration of nitrite in serum. Animals pre-treated with skimmianine (Carr + SKM) showed a significant decrease in the concentration of nitrite compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Values are expressed as mean ± SEM (n = 6 per group). a p ≤ 0.05 compared to Con, b p ≤ 0.05 compared to Carr. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents the animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents the animals pre-treated with 20 mg/kg of diclofenac (i.p.) and then treated with carrageenan
Effect of skimmianine on the mRNA expression of TNF-α and IL-6
Control animals that were given an i.p. injection of 5 mg/kg bw of skimmianine (Con + SKM) showed no significant change in their TNF-α and IL-6 mRNA levels compared to the control (Con) group. The mRNA expressions of TNF-α and IL-6 were upregulated in carrageenan-treated (Carr) paw tissue compared to control (Con) group. Diclofenac administration (Carr + Dic) reduced the TNF-α and IL-6 mRNA levels compared to the Carr group. Animals pre-treated with skimmianine (Carr + SKM) showed a reduction in TNF-α and IL-6 mRNA levels compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups (Fig. 9).
Effect of skimmianine on mRNA levels of TNF-α and IL-6. Animals pre-treated with skimmianine (Carr + SKM) showed a reduction in TNF-α and IL-6 mRNA levels compared to the carrageenan (Carr) and diclofenac (Carr + Dic) administered groups. Con represents animals that were treated with 0.5 % DMSO (vehicle) in saline, Con + SKM represents control animals that were administered an i.p. injection of 5 mg/kg bw of skimmianine, Carr represents animals that received an injection of 0.1 ml of 1 % carrageenan into the sub-plantar tissue of the right hind paw to induce edema, Carr + SKM represents animals pre-treated with 5 mg/kg of skimmianine (i.p.) and then treated with carrageenan, and Carr + Dic represents animals pre-treated with 20 mg/kg of diclofenac (i.p) and then treated with carrageenan
Discussion
The inflammatory process is characterized by the production of PGs, leukotrienes, histamine, bradykinin, platelet-activating factor and the release of chemicals from tissues and migrating cells [29, 30]. Carrageenan-induced local inflammation (paw edema or pleurisy) is a commonly used method for evaluating the efficacy of NSAIDs and also for determining the role of mediators involved in vascular changes associated with acute inflammation [31]. The initial phase of inflammation (edema, 0–1 h) has been attributed to the release of histamine, 5-hydroxytryptamine and bradykinin, followed by a late phase (1–6 h) mainly sustained by PG production by COX activation in the tissue [32].
Tissue MPO activity is used as an index to assess the extent of neutrophil infiltration. The carrageenan-induced inflammatory response is linked to neutrophil infiltration and production of neutrophil-derived free radicals such as hydrogen peroxide, superoxide and hydroxyl radicals [33]. Free-radical-mediated peroxidation of plasma membrane lipids is indicated by the production of TBARS, which is found to accumulate in inflammatory conditions [34]. Skimmianine treatment significantly decreased the elevated MPO activity, indicating reduced neutrophil infiltration. While the activities of SOD, catalase and GPx were significantly increased following skimmianine treatment, a corresponding significant decrease in TBARS level was observed. This decrease in TBARS indicates a favorable antioxidant environment, presumably due to the increased activity of antioxidant enzymes or reduced neutrophil infiltration.
The l-arginine-NO pathway is an important mediator of carrageenan-induced inflammatory response. Pharmacological inhibition of NOS is reported to reduce the development of the carrageenan-induced inflammatory response [35]. The formation of peroxynitrite in the carrageenan-induced paw edema model and its relationship to NO production has also been reported [36]. In the present study, skimmianine treatment inhibited NO production.
PGs and leukotrienes, mediators of the inflammatory response, are produced from arachidonic acid by COX and 5-LOX, respectively. COX-mediated PG synthesis exhibits two regulatory characteristics. While COX-1 mediates PG production for normal homeostasis, COX-2-mediated PG production is involved in the inflammatory response [27]. We observed an upregulation in COX-2 and 5-LOX activity and the overproduction of PGE2 in carrageenan-induced rats, which is supportive of the inflammatory response. In the current study, edema inhibition by skimmianine was more pronounced in the second phase, suggesting the possible inhibition of prostaglandin production as a major mechanism of skimmianine action. Skimmianine’s inhibitory effect on COX-2 and 5-LOX activity in paw tissue is supportive of this assumption.
Cytokines, such as TNF-α, IL-1β, IL-6, PGs and adhesion molecules, are important for the genesis of inflammatory signals [37, 38]. PGE2 production is enhanced by stimulation of macrophages/monocytes, fibroblasts and epithelial cells by cytokines such as TNF-α [39]. In the present study, skimmianine treatment suppressed the transcription of TNF-α and IL-6 genes, highlighting the downregulation of cytokine production and subsequent production of PGE2, indicating its anti-inflammatory effect.
In summary, this study provides evidence for the mechanisms by which skimmianine exerts its anti-inflammatory activity in the carrageenan-induced paw edema model. The suggested mechanism of this action is the suppression of pro-inflammatory cytokine production and their upstream events, inhibition of neutrophil infiltration and neutralization of oxidative stress by stimulation of antioxidant enzyme activity. Due to its ability to modulate multiple cytokines, skimmianine has potential therapeutic efficacy in various types of inflammatory diseases.
References
Serhan CN, Levy B. Success of prostaglandin E2 in structure-function is a challenge for structure-based therapeutics. Proc Natl Acad Sci USA. 2003;100:8609–11.
Goulet JL, Snouwaert JN, Latour AM, Coffman TM, Koller BH. Altered inflammatory responses in leukotriene-deficient mice. Proc Natl Acad Sci USA. 1994;91:12852–6.
Amin AR, Vyas P, Attur M, Leszczynska-Piziak J, Patel IR, Weissmann G, et al. The mode of action of aspirin-like drugs: effect on inducible nitric oxide synthase. Proc Natl Acad Sci USA. 1995;92:7926–30.
Marucha PT, Zeff RA, Kreutzer DL. Cytokine-induced IL-1 beta gene expression in the human polymorphonuclear leukocyte: transcriptional and post-transcriptional regulation by tumor necrosis factor and IL-1. J Immunol. 1991;147:2603–8.
Davies NM, Saleh JY, Skjodt NM. Detection and prevention of NSAID-induced enteropathy. J Pharm Pharm Sci. 2000;3:137–55.
James MW, Hawkey CJ. Assessment of non-steroidal anti-inflammatory drug (NSAID) damage in the human gastrointestinal tract. Br J Clin Pharmacol. 2003;56:146–55.
Wallace JL. Selective cyclooxygenase-2 inhibitors: after the smoke has cleared. Dig Liver Dis. 2002;34:89–94.
Bermond P. Analgesic and antiinflammatory properties of vitamins. Int J Vitam Nutr Res Suppl. 1989;30:153–60.
Ratnam DV, Ankola DD, Bhardwaj V, Sahana DK, Kumar MN. Role of antioxidants in prophylaxis and therapy: a pharmaceutical perspective. J Control Release. 2006;113:189–207.
Osadebe PO, Okoye FBC. Anti-inflammatory effects of crude methanolic extract and fractions of Alchornea cordifolia leaves. J Ethnopharmacol. 2003;89:19–24.
Conway GA, Slocumb JC. Plants used as abortifacients and emmenagogues by Spanish New Mexicans. J Ethnopharmacol. 1979;1:241–61.
Kuzovkina I, Al’terman I, Schneider B. Specific accumulation and revised structures of acridone alkaloid glucosides in the tips of transformed roots of Ruta graveolens. Phytochemistry. 2004;65:1095–100.
Ratheesh M, Shyni GL, Sindhu G, Helen A. Protective effects of isolated polyphenolic and alkaloid fractions of Ruta graveolens L. on acute and chronic models of inflammation. Inflammation. 2010;33:18–24.
Garcia-Argaez AN, Ramirez Apan TO, Parra Delgado H, Velazquez G, Martinez-Vazquez M. Anti-inflammatory activity of coumarins from Decatropis bicolor on TPA ear mice model. Planta Med. 2000;66:279–81.
Nugroho AE, Riyanto S, Sukari MA, Maeyama K. Effects of skimmianine, a quinoline alkaloid of Aegle marmelos correa roots, on the histamine release from rat mast cells. J Basic Appl Sci. 2010;6:141–8.
Chen JJ, Wang TY, Hwang TL. Neolignans, a coumarinolignan, lignan derivatives, and a chromene: anti-inflammatory constituents from Zanthoxylum avicennae. J Nat Prod. 2008;71:212–7.
Robertson AV. The proton magnetic resonance of furoquinoline alkaloids and related compounds. Aust J Chem Soc. 1963;16:451–8.
Riyanto S, Sukari MA, Rahmani M, Ee GCL, Yap YHT, Aimi N, et al. Alkaloids from Aegle marmelos (Rutaceae). Malays J Anal Sci. 2001;7:463–5.
Winter CA, Risley EA, Nuss GW. Carrageenin-induced edema in hind paw of the rat as an assay for antiinflammatory drugs. Proc Soc Exp Biol Med. 1962;111:544–7.
Shyni GL, Ratheesh M, Sindhu G, Helen A. Anti-inflammatory and antioxidant effects of Jeevaneeya Rasayana: an ayurvedic polyherbal formulation on acute and chronic models of inflammation. Immunopharmacol Immunotoxicol. 2010;32:569–75.
Bradley PP, Priebat DA, Chrisrensen RD, Rothstein G. Measurement of cutaneous inflammation: estimation of neutrophil content with an enzyme marker. J Invest Dermatol. 1982;78:206–9.
Kakkar P, Das B, Viswanathan PN. A modified spectrophotometric assay of superoxide dismutase. Indian J Biochem Biophys. 1984;21:130–2.
Aebi H. Catalase in vitro. Methods Enzymol. 1984;105:121–6.
Paglia DE, Valentine WN. Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. J Lab Clin Med. 1967;70:158–69.
Draper HH, Hadley M. Malondialdehyde determination as index of lipid peroxidation. Methods Enzymol. 1990;186:421–31.
Radhika A, Jacob SS, Sudhakaran PR. Influence of oxidatively modified LDL on monocyte-macrophage differentiation. Mol Cell Biochem. 2007;305:133–43.
Axelrod B, Cheesebrough TM, Laakso S, Axelrod B, Cheesebrough TM, Laakso S. Lipoxygenase from soybean. Methods Enzymol. 1981;71:441–5.
Grisham MB, Johnson GG, Lancaster JR Jr. Quantitation of nitrate and nitrite in extracellular fluids. Methods Enzymol. 1996;268:237–46.
Vane J, Botting R. Inflammation and the mechanism of action of anti-inflammatory drugs. FASEB J. 1987;1:89–96.
Tomlinson A, Appleton I, Moore AR, Gilroy DW, Willis D, Mitchell JA, et al. Cyclooxygenase and nitric oxide synthase isoforms in rat carrageenin-induced pleurisy. Br J Pharmacol. 1994;113:693–8.
Cuzzocrea S, Nocentini G, Di Paola R, Agostini M, Mazzon E, Ronchetti S, et al. Proinflammatory role of glucocorticoid-induced TNF receptor-related gene in acute lung inflammation. J Immunol. 2006;177:631–41.
Mazzon E, Esposito E, Di Paola R, Muia C, Crisafulli C, Genovese T, et al. Effect of tumour necrosis factor-alpha receptor 1 genetic deletion on carrageenan-induced acute inflammation: a comparison with etanercept. Clin Exp Immunol. 2008;153:136–49.
Dawson J, Sedgwick AD, Edwards JC, Lees P. A comparative study of the cellular, exudative and histological responses to carrageenan, dextran and zymosan in the mouse. Int J Tissue React. 1991;13:171–85.
Janero DR. Malondialdehyde and thiobarbituric acid-reactivity as diagnostic indices of lipid peroxidation and peroxidative tissue injury. Free Radic Biol Med. 1990;9:515–40.
Tracey WR, Nakane M, Kuk J, Budzik G, Klinghofer V, Harris R, et al. The nitric oxide synthase inhibitor, l-NG-monomethylarginine, reduces carrageenan-induced pleurisy in the rat. J Pharmacol Exp Ther. 1995;273:1295–9.
Salvemini D, Wang ZQ, Bourdon DM, Stern MK, Currie MG, Manning PT. Evidence of peroxynitrite involvement in the carrageenan-induced rat paw edema. Eur J Pharmacol. 1996;303:217–20.
Baeuerle PA, Baltimore D. NF-kappa B: ten years after. Cell. 1996;87:13–20.
Baeuerle PA, Henkel T. Function and activation of NF-kappa B in the immune system. Annu Rev Immunol. 1994;12:141–79.
Dayer JM, Beutler B, Cerami A. Cachectin/tumor necrosis factor stimulates collagenase and prostaglandin E2 production by human synovial cells and dermal fibroblasts. J Exp Med. 1985;162:2163–8.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible Editor: Jerauld Skotnicki.
Rights and permissions
About this article
Cite this article
Ratheesh, M., Sindhu, G. & Helen, A. Anti-inflammatory effect of quinoline alkaloid skimmianine isolated from Ruta graveolens L.. Inflamm. Res. 62, 367–376 (2013). https://doi.org/10.1007/s00011-013-0588-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-013-0588-1