Abstract
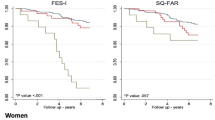
Background and aims: Falls efficacy has been shown to predict functional decline, but whether it is independently associated with frailty is still unclear. This study investigated the cross-sectional association between falls efficacy and the frailty pheno-type in high-functioning older persons. Methods: Subjects (n=861) were a sub-sample of community-dwelling persons aged 65 to 70 years enrolled in the “Lc65+” cohort, who had gait assessment. Data included demographics, functional, cognitive, affective and health status, as well as measures of physical performance. Falls efficacy was measured with the Falls Efficacy Scale-International (FES-I) and frailty with Fried’s criteria. Participants were categorized into robust (no frailty criterion) and vulnerable (1 or more criteria). Low falls efficacy was defined as a FES-I score in the lowest quartile. Results: Overall, 23.9% of participants were vulnerable. Compared with robust participants, they were more likely to report low falls efficacy (43.3% vs 19.1%, p<0.001) and had poorer health and functional and mental status. They had slower gait speed (1.07±0.18 vs 1.15±0.15 m/s, p<0.001) and increased gait speed variability (coefficient of variation 4.10±4.03 vs 3.33±1.45%, p<0.001), although only 6 participants (0.7%) fulfilled Fried’s slow walking criterion. In multivariate analysis, low falls efficacy remained associated with being vulnerable (adjusted OR 1.80, 95%, CI 1.19–2.74, p=0.006), independent of comorbidity, functional status, falls history and gait performance. Conclusion: In high-functioning older persons, low falls efficacy was associated with vulnerability, even after controlling for gait performance and falls history. Whether low falls efficacy is a potential target on the pathway leading to frailty should be further examined prospectively.
Similar content being viewed by others
References
Delbaere K, Crombez G, Vanderstraeten G, Willems T, Cambier D. Fear-related avoidance of activities, falls and physical frailty. A prospective community-based cohort study. Age Ageing 2004; 33: 368–73.
Zijlstra GA, van Haastregt JC, van Eijk JT, van RE, Stalenhoef PA, Kempen GI. Prevalence and correlates of fear of falling, and associated avoidance of activity in the general population of community-living older people. Age Ageing 2007; 36: 304–9.
Bandura A. Self-efficacy mechanism in human agency. Am Psychol 1982; 37: 122–47.
Tinetti ME, Richman D, Powell L. Falls efficacy as a measure of fear of falling. J Gerontol 1990; 45: 239–43.
Deshpande N, Metter EJ, Lauretani F, Bandinelli S, Guralnik J, Ferrucci L. Activity restriction induced by fear of falling and objective and subjective measures of physical function: a prospective cohort study. J Am Geriatr Soc 2008; 56: 615–20.
Carriere I, Colvez A, Favier F, Jeandel C, Blain H. Hierarchical components of physical frailty predicted incidence of dependency in a cohort of elderly women. J Clin Epidemiol 2005; 58: 1180–7.
Fried LP, Tangen CM, Walston J et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 2001; 56: M146–56.
Woods NF, LaCroix AZ, Gray SL et al. Frailty: emergence and consequences in women aged 65 and older in the Women’s Health Initiative Observational Study. J Am Geriatr Soc 2005; 53: 1321–30.
Bandeen-Roche K, Xue QL, Ferrucci L et al. Phenotype of frailty: characterization in the women’s health and aging studies. J Gerontol A Biol Sci Med Sci 2006; 61: 262–6.
Maki BE. Gait changes in older adults: predictors of falls or indicators of fear? J Am Geriatr Soc 1997; 45: 313–20.
Kressig RW, Gregor RJ, Oliver A et al. Temporal and spatial features of gait in older adults transitioning to frailty. Gait Posture 2004; 1: 30–5.
Rochat S, Martin E, Piot-Ziegler C, Najafi B, Aminian K, Bula CJ. Falls self-efficacy and gait performance after gait and balance training in older people. J Am Geriatr Soc 2008; 56: 1154–6.
Cumming RG, Salkeld G, Thomas M, Szonyi G. Prospective study of the impact of fear of falling on activities of daily living, SF-36 scores, and nursing home admission. J Gerontol A Biol Sci Med Sci 2000; 55: M299–305.
Santos-Eggimann B, Karmaniola A, Seematter-Bagnoud L et al. The Lausanne cohort Lc65+: a population-based prospective study of the manifestations, determinants and outcomes of frailty. BMC Geriatr 2008; 8: 20.
Aminian K, Najafi B, Bula C, Leyvraz PF, Robert P. Spatio-temporal parameters of gait measured by an ambulatory system using miniature gyroscopes. J Biomech 2002; 35: 689–99.
Hausdorff JM, Rios DA, Edelberg HK. Gait variability and fall risk in community-living older adults: a 1-year prospective study. Arch Phys Med Rehabil 2001; 82: 1050–6.
Yardley L, Todd C, Beyer N, Hauer K, Kempen R, Piot-Ziegler C. Development and initial validation of the Falls Efficacy Scale International (FES-I). Age Ageing 2005; 34: 614–9.
Barnett A, Smith B, Lord SR, Williams M, Baumand A. Community-based group exercise improves balance and reduces falls in at-risk older people: a randomised controlled trial. Age Ageing 2003; 32: 407–14.
Zijlstra G, van Haastregt JC, van Eijk JT, Kempen GI. Evaluating an intervention to reduce fear of falling and associated activity restriction in elderly persons: design of a randomised controlled trial [ISRCTN43792817]. BMC Public Health 2005; 5: 26.
Perera S, Mody SH, Woodman RC, Studenski SA. Meaningful change and responsiveness in common physical performance measures in older adults. J Am Geriatr Soc 2006; 54: 743–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Seematter-Bagnoud, L., Santos-Eggimann, B., Rochat, S. et al. Vulnerability in high-functioning persons aged 65 to 70 years: the importance of the fear factor. Aging Clin Exp Res 22, 212–218 (2010). https://doi.org/10.1007/BF03324799
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03324799