Abstract
Background
This study aims to illustrate the results of percutaneous forefoot surgery (PFS) for correction of hallux valgus.
Materials and methods
A prospective study of 108 patients, with hallux valgus deformity, who underwent PFS was conducted. The minimum clinical and radiological follow-up was two years (mean 57.3 months, range 22–112).
Results
Preoperative mean visual analog scale was 6.3 ± 1.5 points, and AOFAS scores were 50.6 ± 11 points. At the last follow-up, both scores improved to 1.9 ± 2.4 points and 85.9 ± 1.83 points, respectively. Mean hallux valgus angle changed from 34.3° ± 9.3° preoperatively to 22.5° ± 11.1° at follow-up. At follow-up, 76.5% of the subjects were satisfied or very satisfied. Recurrence of medial 1st MT head pain happened in 22 cases (16.7%).
Conclusions
PFS, in our study, does not improve the radiological and patient satisfaction rate results compared with conventional procedures. The main advantage is a low postoperative pain level, but with an insufficient HVA correction.
Level of evidence
II, prospective study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Percutaneous forefoot surgery (PFS) has been developed by Stephen Isham, Mariano de Prado and Pau Golano. They have produced valuable knowledge and built an anatomic and technical foundation for PFS [1, 2]. It is theorized that 50% of forefoot cases are surgically repaired in the USA by means of PFS and minimum incision surgery (MIS) [3]. However, PFS has not been given a great deal of attention in the surgical literature [4].
PFS is performed through 1–3 mm incisions, using a mini-blade for soft tissue and power rotary bur for osseous procedures under image intensification. Theoretical advantages are a potential faster recovery with immediate weight bearing, reduced surgical time, a less painful postoperative period and less stress to the patient. Besides, PFS is performed as an outpatient procedure. The main disadvantages are the requirement for specific equipment and lengthy learning curve.
The purpose of the present study is to evaluate the clinical and radiographic results of PFS for hallux valgus (HV) deformity.
Materials and methods
This is a single forefoot non-specialized center, with a single-surgeon prospective study. The surgeon had a previous surgical experience in PFS technique of 20 cases. All the patients were treated in an outpatient surgery unit.
Between April 2006 and December 2013, 126 patients were included in the study, 108 of them completed the minimum two-year follow-up period (57.3 months, range 24–112), 24 patients with a one-step bilateral surgery. Therefore, a total of 132 feet were studied, with previous informed consent.
The indication was a painful HV with or without metatarsalgia, with less than 60° of HV angle (HVA) and less than 20° of 1–2 intermetatarsal angle (IMA). All patients had adequate ROM of the first metatarsophalangeal (MTP) joint. All patients reported having pain and difficulty wearing shoes, with no improvement from conservative treatments. Patients were excluded if they had rheumatoid arthritis or other inflammatory diseases, previously failed HV surgery or isolated interphalangeal HV.
A clinical and radiological weight-bearing examination, by an independent review, was performed preoperatively and postoperatively at two months, one year and at final follow-up (December 2015). It included visual analog scale (VAS), American Orthopaedic Foot and Ankle Society hallux score (AOFAS) [5, 6], HVA, IMA, distal metatarsal articular angle (DMAA), the metatarsal index (M1 > M2, M1 = M2, M1 < M2) and joint congruency of MTF joint. Besides, VAS was collected one and three weeks postoperative, to assess pain level at immediate postoperative period. The subjective satisfaction with the outcome (very satisfied, satisfied, dissatisfied, or disappointed) was also recorded. Anteroposterior weight-bearing radiographic angles were measured by the Couglin et al. method [7]. Joint congruency of the first MTP was assessed using the criteria defined by Pigott [8]. All the measurements were taken digitally (Ykonos, Sescam©).
Surgical technique
All of the procedures were performed under spinal anesthesia with bupivacaine (0.25%) ankle block for postoperative pain control. At home, patients were recommended to use acetaminophen and/or dipyrone and/or nonsteroidal anti-inflammatory agents according to demand.
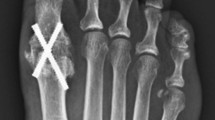
The PFS procedures were based on the description of Isham and De Prado [1, 2]. Exostosectomy, lateral metatarsophalangeal arthrolysis and percutaneous Akin osteotomy of the first phalanx were done in all cases [9]. Patients with moderate to severe lateral metatarsalgia underwent distal metatarsal mini-invasive osteotomy (DMMO), without fixation, of 2nd, 3rd and 4th metatarsals. Patients with IMA ≥ 15° underwent proximal closing wedge osteotomy of the first metatarsal with minimally invasive surgery (MIS), and fixed with a superolateral compression staple. Treatment of lesser toes was determined on a case-by-case basis, with a combination of procedures on the soft tissues (flexor and extensor tendon tenotomies) and bones (phalangeal osteotomies) (Fig. 1).
In every case, a specific dressing is fashioned at the end of the procedure to maintain the correction. Monitoring of this dressing was done at first and third weeks and removed at third week.
Immediate full weight bearing was allowed with a rigid, flat-soled postoperative shoe for 5 weeks, and no deep venous thrombosis prophylaxis was used. Only cases with compression staple osteosynthesis received one antibiotic prophylaxis dose with cefazolin.
Statistical analysis
Continuous data were described as means and standard deviations. Categorical data were described as absolute and relative frequencies. The Wilcoxon signed-rank test was used to compare values before and after surgery and during follow-up. A 0.05 level of significance was used throughout. Statistical analyses were performed with the aid of PASW 18.0 statistical analysis software (SPSS Inc, Chicago, IL, USA).
Results
The demographics of age, sex and operated side are shown in Table 1. The associated pathologies to HV and surgical procedures performed are listed in Table 2. It is essential to highlight a greater number of cases with metatarsalgia treated with DMMO in the group. Also in the 27.3% of patients have been performed a proximal closing wedge osteotomy of the first metatarsal with MIS. Both facts affect the clinical and radiological results.
Mean average preoperative AOFAS hallux score was 50.6 ± 11.2 points, and at follow-up, it improved to 85.9 ± 13.8 points (Table 3). The vast majority of patients had a preoperative pain level moderate or severe (96.2%) (VAS 4–9). One week after the procedure, patients with none or mild pain (VAS 0–3) were 59%. At the third week, that percentage increased to 74.6%. Final follow-up, 76.5% had none or mild pain. Mean preoperative pain score (6.3 ± 1.5 points) decreased progressively at first (3.2 ± 2 points) and third week (2.4 ± 1.8 points) (p < 0.001), but without changes between third week and second month (2.4 ± 2.2 points) (p = 0.792). A further improvement in pain occurred between the second month and the first year (1.8 ± 2.5 points) (p = 0.007). No changes in the level of pain until the final follow-up (1.9 ± 2.4 points) (p = 0.588).
The mean average HVA improved from 34.3° ± 9.3° before the operation to 16° ± 8.2° at second month, a correction of 53.3%. During the first year, there was a loss of postoperative correction of 6.5°, implying a loss of 18.9%, but stabilizing angulation after the first year. Preoperative IMA was 13.1° ± 3.5°, decreasing 2.4° (18.3%), at final follow-up. The DMAA suffered a slight, but progressive worsening with a mean of 18.5° ± 7.3° preoperative and 23.6° ± 9.7° at final follow-up (Table 4).
The number of cases with preoperative metatarsal index M1 < M2 was 47.7% and M1 > M2 was 23.5%. At final follow-up, they were 43.5% and 29%, respectively. Preoperative joint congruency of the first MTP was 47% cases, improving at second month to 95% (p < 0.001), but decreasing at fist year (80.3%, p < 0.001). Without changes between fist-year and final follow-ups (73.3%, p = 0.150).
At final follow-up, 76.5% of the subjects were satisfied or very satisfied. Only 6.8% of cases were disappointed. Recurrence of medial 1st MT head pain happened in 22 cases (16.7%). Complications registered are shown in Table 5.
Discussion
The VAS is validated for various orthopedic outcomes and has shown to be reliable [10–12]. In our study, PFS has shown a low immediate postoperative pain level, with mean VAS score of 3.2 ± 2 points at first week. Pain level continued improving until third week (2.4 ± 1.8 points), lower than Nikolau et al. (3.84 ± 1.3 points) [13] with Mitchell’s osteotomy, and at first year (1.8 ± 2.5 points) (p = 0.007), without worsening at final follow-up. Our final VAS score was lower than that reported by Deveci et al. [14] with Scarf osteotomy (2.4 ± 1). This shows us a rapid recovery of pain. The final follow-up AOFAS hallux score in our study was 85.9 ± 1.8 points, previous reports with different procedures presented similar outcomes [14–18], although in our study we have treated also patients with metatarsalgia, increasing pain level and delaying recovery.
Mean of final HVA correction was 12° in our study. A similar correction was shown in several reports with Scarf [19–21], Chevron [17, 22], Kramer [18] and Reverdin–Isham osteotomy [23, 24] (12°–16°), with similar follow-up. Our correction was lower compared to those reported by Lee et al. [25], Deveci et al. [14], Jones et al. [26] and Bonnel et al. [27] (22°–25°, with Scarf and Chevron osteotomies), but with lower mean follow-up (7–26 months). Lee et al. [16], with Chevron proximal and distal osteotomy, reported 24° of HVA correction with similar follow-up. Mean IMA correction in several reports was between 6° and 9° (Scarf, proximal and distal Chevron and Kramer osteotomies) [14, 16, 18, 21, 25, 26], which is better than 3° of our study. But, Bauer et al. [23, 24], with Reverdin–Isham osteotomy, obtained a correction equal to ours. The proximal closing wedge osteotomy of the first metatarsal performance (27.3% of patients) has affected the clinical and radiological results. But we have considered it a necessary associated procedure to decrease the pathologic IMA. We have to take into account that intraobserver and interobserver reliability rates are high for measuring the HVA and IMA (<5°, 95% confidence interval) [28].
76.5% of patients were “satisfied” or “very satisfied,” and this percentage is significantly lower than those reported with Scarf, proximal or distal Chevron and Reverdin–Isham osteotomies (85–95%) [16, 19, 20, 23, 29]. Recurrence of medial 1st MT head pain happend in 16.7% of patients, of which, only 5.3% request revision surgery. A total of 10.6% of patients needed revision surgery. Rates of HV recurrence vary in the literature from 2.7 to 20% [30–34], and therefore, recurrence is common in HV surgery, with a multifactorial cause including patient-related and surgical factors [35]. In PFS, recurrence of medial 1st MT head pain may be in relation to insufficient resection with peripheral bony prominence. Moreover, an inadequate lateral MTP release can cause lack of HVA correction. Both mistakes are more frequent at the beginning of the learning curve.
There was no case of HV deformity or deep venous thrombosis. The most numerous complications were metatarsalgia after DMMO (11.4%) (without relationship with HV deformity), with a lower rate than that reported by García-Fernández et al. (40%) [36] and similar to Henry et al. (14%) [37] reports. Although Bauer [38] considers DMMO an easily reproducible procedure with a short learning curve, we consider it a technically demanding procedure with a prolonged forefoot edema and high complications rate (22.9%, in our study). Therefore, we do not recommend its systematic realization.
PFS could be an option for surgical HV deformity treatment, but without improving the patient satisfaction rate results published with conventional procedures. The main advantage is a low postoperative pain level, but with an insufficient HVA correction. Despite the worse radiographic results in our study, compared with previous reports using different procedures, we present similar clinical outcomes. Which is in line with what was published by Thordarson et al. [39].
The major limitation of the present study is the difficulty to standardize treatment in HV surgery, with several additional procedures, that have some influence on outcomes (metatarsalgia, proximal closing wedge osteotomy of the first metatarsal and lesser toes deformities). Also we have not studied how this might impact outcomes. Nevertheless, this study presents our results with this surgical strategy. The surgeon who participated in the study only had twenty cases of surgical experience previous to the study. As a consequence, the results may apply to surgeons with little experience. The study’s strengths are the prospective study, the cohort number and the mean final follow-up.
Conclusion
PFS, in our study, does not improve the radiological and patient satisfaction rate results compared with conventional procedures. The main advantage is a low postoperative pain level, but with an insufficient HVA correction. The technique requires a learning curve before being able to produce reliably acceptable results.
References
De Prado M, Ripio PL, Golano P (2003) Hallux valgus. In: Cirugía percutánea del antepie. Barcelona: Masson SA, pp 57–94
Isham SA (1991) The Reverdin-Isham procedure for the correction of hallux abducto valgus. A distal metatarsal osteotomy procedure. Clin Podiatr Med Surg 8(1):81–94
De Lavigne C, de Prado M, Sugar G, Determe P (2007) Hallux valgus and forefoot surgery: mini-invasive or open? In: Symposium 41. 8th EFORT congress, May 13, 2007, Florence Italy. http://www.efort.org/_documents%5CJunior%20Reports%5C3.rapor.pdf. Accessed 10 Oct 2008
Roukis TS (2009) Percutaneous and minimum incisión metatarsal osteotomies: a systematic review. J Foot Ankle Surg 48(3):380–387
Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Meyerson MS, Sanders M (1999) Clinical rating systems for the ankle-hindfoot, midfoot, hallux and lesser toes. Foot Ankle Int 15(7):349–353
Ibrahim T, Beiri A, Azzabi M, Best AJ, Taylos GJ, Menon DK (2007) Reliability and validity of the subjective component of the American Orthopaedic Foot and Ankle Society clinical rating scales. J Foot Ankle Surg 46(2):65–74
Coughlin MJ, Saltzman CL, Nunley JAI (2002) Angular measurements in the evaluation of hallux valgus deformities: a report of the ad hoc committee of the American Orthopaedic Foot and Ankle Society on angular measurements. Foot Ankle Int 23:68–74
Pigott H (1960) The natural history of hallux valgus in adolescent and early adult life. J Bone Joint Surg Am 42:749–760
Kadakia AR, Smerek JP, Myerson MS (2007) Radiographic results after percutaneous distal metatarsal osteotomy for correction of hallux valgus deformity. Foot Ankle Int 28:355–360
Price DD, McGrath PA, Rafii A, Buckingham B (1983) The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 17(1):45–56
Jensen MP, Karoly P, Braver S (1986) The measurement of clinical pain intensity: a comparison of six methods. Pain 27(1):117–126
Lee JS, Hobden E, Stiell IG, Wells GA (2003) Clinically important change in the visual analog scale after adequate pain control. Acad Emerg Med 10(10):1128–1130
Nikolaou VS, Korres D, Xypnitos F, Lazarettos J, Lallos S, Sapkas G, Efstathopoulos N (2009) Fixation of Mitchell’s osteotomy with bioabsorbable pins for treatment of hallux valgus deformity. Int Orthop 33(3):701–706
Deveci A, Firat A, Yilmaz S, Oken OF, Yildirim AO, Ucaner A, Bozkurt M (2013) Short-term clinical and radiologic results of the scarf osteotomy: what factors contribute to recurrence? J Foot Ankle Surg 52(6):771–775
Aminian A, Kelikian A, Moen T (2006) Scarf osteotomy for hallux valgus deformity: an intermediate follow-up of clinical and radiographic outcomes. Foot Ankle Int 27:883–886
Lee KB, Cho NY, Park HW, Seon JK, Lee SH (2015) A comparison of proximal and distal Chevron osteotomy, both with lateral soft-tissue release, for moderate to severe hallux valgus in patients undergoing simultaneous bilateral correction. Bone Jt J 97B:202–207
Schneider W, Aigner N, Pinggera O, Knahr K (2004) Chevron osteotomy in hallux valgus: ten-year results of 112 cases. J Bone Jt Surg Br 86:1016–1020
Giannini S, Cavallo M, Faldini C, Luciani D, Vannini F (2013) The SERI distal metatarsal osteotomy and Scarf osteotomy provide similar correction of hallux valgus. Clin Orthop Relat Res 471:2305–2311
Frelson M, Gayet LE, Bouche G, Hamcha H, Nebout J, Pries P (2005) Ostetomie Scarf dans le traitement de l’hallux valgus. A propos de 123 cas avec un recul moyen de 4,8 ans. Rev Chir Orthop 91:257–266
Crevoiser X, Mouhsine E, Ortolano V, Udin B, Dutoit M (2001) The Scarf osteotomy for the treatment of hallux valgus deformity: a review of 84 cases. Foot Ankle Int 22:970–976
Bock P, Kluger R, Kirsten K, Mittlbock M, Schuh R, Trnka H (2015) The Scarf osteotomy with minimally invasive lateral release for treatment of hallux valgus deformity. J Bone Jt Surg Am 97:1238–1245
Fakoor M, Sarafan N, Mohammadhoseini P, Khorami M, Arti H, Mosavi S, Aghaeeaghdam A (2014) Comparison of clinical outcomes of Scarf and Chevron osteotomies and the McBride procedure in the treatment of hallux valgus deformity. Arch Bone Jt Surg 2(1):31–36
Bauer T, Lavigne C, Biau D, De Prado M, Isham S, Laffenetre O (2009) Percutaneous hallux valgus surgery: a prospective multicenter study of 189 cases. Orthop Clin N Am 40:505–514
Bauer T, Biau D, Lortat-Jacob A, Ardí P (2010) Percutaneous hallux valgus correction using the Reverdin-Isham osteotomy. Orthop Traumatol Surg Res 96(4):407–416
Lee KB, Hur CI, Chung JY, Juns ST (2009) Outcome of unilateral versus simultaneous correction for hallux valgus. Foot Ankle Int 30(2):120–123
Jones S, Al Hussainy HA, Ali F, Betts RP, Flowers MJ (2004) Scarf osteotomy for hallux valgus. A prospective clinical and pedobarographic study. J Bone Joint Surg Br 86:830–836
Bonnel F, Canovas F, Poiree G, Dusserre F, Vergnes C (1999) Èvaluation de l’ostéotomie Scarf pour hallux valgus en function de l’angle articulaire distal métarsien: etude prospective sur 79 cas operas. Rev Chir Orthop 85:381–386
Easley ME, Trnka HJ (2007) Current concepts review: hallux valgus part II: operative treatment. Foot Ankle Int 28(6):748–758
Trnka HJ, Zembsch A, Easeley ME, Salzer M, Ritschl P, Myerson MS (2000) The chevron osteotomy for correction of hallux valgus. Comparison of findings after two and five years of follow-up. J Bone Jt Surg Am 82:1373–1378
Kilmartin TE, O’Kane C (2010) Combined rotation scarf and Akin osteotomies for hallux valgus: a patient focussed 9 year follow up for 50 patients. J Foot Ankle Res 3:2. doi:10.1186/1757-1146-3-2
Okuda R, Kinoshita M, Yasuda T, Jotoku T, Shima H, Takamura M (2011) Hallux valgus angle as a predictor of recurrence following proximal metatarsal ostoeotomy. J Orthop Sci 16(6):760–764
Lehman DE (2003) Salvage of complications of hallux valgus surgery. Foot Ankle Clin 8(1):15–35
Robison AH, Limbers JP (2005) Modern concepts in the treatment of hallux valgus. J Bone Jt Surg Br 87(8):1038–1045
Torkki M, Seitsalo S, Paavolainen P (2001) Chevron osteotomy for correction of hallux valgus: a long-term follow-up study. Foot 11:91–93
Raikin SM, Miller AG, Daniel J (2014) Recurrence of hallux valgus. A review. Foot Ankle Clin N Am 19:259–274
García-Fernández D, Gil-Garay E, Lora-Pablos D, De la Cruz Bértolo J, Llanos-Alcázar LF (2011) Comparative study of the Weil osteotomy with and without fixation. Foot Ankle Surg 17:103–107
Henry J, Besse JL, Fessy AFCP (2011) Distal osteotomy of the lateral metatarsals: a series of 72 cases comparing the Weil osteotomy and the DMMO percutaneous osteotomy. Orthop Traumatol Surg Res 97S:S57–S65
Bauer T (2014) Percutaneous forefoot surgery. Orthop Traumatol Surg Res 100:S191–S204
Thordason D, Ebramzadeh E, Moorthy M, Lee J, Rudicel S (2005) Correlation of hallux valgus surgical outcome with AOFAS forefoot score and radiological parameters. Foot Ankle Int 26(2):122–127
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declared no potential conflicts of interests with respect to the research, authorship and/or publication of this article.
Human and animal rights statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Crespo Romero, E., Peñuela Candel, R., Gómez Gómez, S. et al. Percutaneous forefoot surgery for treatment of hallux valgus deformity: an intermediate prospective study. Musculoskelet Surg 101, 167–172 (2017). https://doi.org/10.1007/s12306-017-0464-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-017-0464-1