Abstract
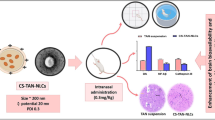
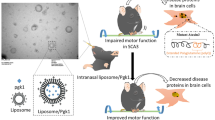
Parkinson’s disease (PD) is the second most common neurodegenerative disorder (ND), characterized by the loss of dopaminergic neurons, microglial activation, and neuroinflammation. Current available treatments in clinical practice cannot halt the progression of the disease. During the last few years, growth factors (GFs) have been raised as a promising therapeutic approach to address the underlying neurodegenerative process. Among others, glial cell-derived neurotrophic factor (GDNF) is a widely studied GF for PD. However, its clinical use is limited due to its short half life, rapid degradation rate, and difficulties in crossing the blood-brain barrier (BBB). Lately, intranasal administration has appeared as an alternative non-invasive way to bypass the BBB and target drugs directly to the central nervous system (CNS). Thus, the aim of this work was to develop a novel nanoformulation to enhance brain targeting in PD through nasal administration. For that purpose, GDNF was encapsulated into chitosan (CS)-coated nanostructured lipid carriers, with the surface modified with transactivator of transcription (TAT) peptide (CS-nanostructured lipid carrier (NLC)-TAT-GDNF). After the physiochemical characterization of nanoparticles, the in vivo study was performed by intranasal administration to a 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) mouse model of PD. The CS-NLC-TAT-GDNF-treated group revealed motor recovery which was confirmed with immunohistochemistry studies, showing the highest number of tyrosine hydroxylase (TH+) fibers in the striatum and TH+ neuron levels in the substantia nigra. Moreover, ionizing calcium-binding adaptor molecule 1 immunohistochemistry was performed, revealing that CS-NLC-TAT-GDNF acts as a modulator on microglia activation, obtaining values similar to control. Therefore, it may be concluded that the intranasal administration of CS-NLC-TAT-GDNF may represent a promising therapy for PD treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is the second most common neurodegenerative disease, affecting five million patients worldwide. Clinically it is characterized by resting tremor, bradykinesia, rigidity, and postural instability. Non-motor features such as olfactory dysfunction, cognitive impairment, pain, and sleep disorders are also common in early PD and are associated with reduced health related quality of life. Moreover, the pathological hallmarks of PD are progressive loss of dopaminergic neurons in the substantia nigra pars compacta (SNc) followed by decrease of dopamine (DA) and the presence of intraneuronal aggregations of abnormal protein alpha-synuclein (α-syn), called Lewy bodies [1,2,3]. Neuroinflammation is another well-known feature of PD. Numerous studies have demonstrated the presence of an active inflammatory response in the brain mediated primarily by microglia and astrocytes. Microgliosis resulting from microglial activation occurs within the area of neurodegeneration, highlighting the link between neuroinflammation, PD, and neuronal loss. Although the underlying mechanisms are not clear, it can be implied that reducing microglia activation is a reasonable target for neuroprotective therapies in PD [4,5,6].
Currently, the available treatments for PD focus on DA replacement to control motor symptoms. Although this approach can be initially effective in managing movement disorder symptoms, as the disease advances, it is not useful in treating non-movement disorder symptoms. Moreover, side effects in long-term treatment (motor and non-motor fluctuations, dyskinesia, and psychosis) are crucial challenges in the clinical management of PD [3, 7]. This is why there is an urgent need of a disease modifying treatment capable of slowing down the progression of the disease. In an attempt to address neuronal degeneration, the use of growth factors (GFs) has been raised as a promising alternative treatment. Among GFs, glial derived neurotrophic factor (GDNF) is known to be one of the most important for dopaminergic and motor neuronal survival due to its neuroprotective and neuroregenerative properties. However, GDNF’s rapid degradation rate, structure, and molecular weight limit its ability to cross the blood-brain barrier (BBB), making the search for alternative ways of bypassing the BBB necessary [8]. In an attempt to deliver GDNF directly to the brain, intraventricular and intraparenchymal administrations have been proposed in both animals and human clinical trials, pointing out the therapeutic properties of this GF for PD [9,10,11,12,13,14]. Lastly, due to the risks associated with these clinically less accepted administration routes, safer non-invasive ways have been proposed to reach the brain [15]. Recent studies have described intranasal administration (i.n.) as a method to transport drugs directly to the central nervous system (CNS) through the olfactory and trigeminal pathways [16]. Nevertheless, the disadvantages of this route of administration are the limited absorption across the nasal epithelium and the short residence time in the nasal cavity due to the mucociliary clearance, which leads to uncompleted drug absorption [17]. In order to enhance the residence time in the nasal cavity, as well as protect these therapeutic proteins from being degraded, biodegradable nanocarriers have been used [18, 19]. Moreover, the co-administration of nanoparticles (NP) with mucoadhesive polymers has shown to increase the contact time with nasal mucosa, hence, increasing brain concentrations. In fact, different experimental studies have confirmed the suitability of nanotechnology devices for target drug delivery to the CNS after i.n. administration [20,21,22,23,24,25,26]. In this regard, our research group developed chitosan (CS)-coated nanostructured lipid carriers (NLCs) for the delivery of therapeutic proteins by i.n. administration. The NLCs are improved second-generation lipid carriers, derived from solid lipid nanoparticles (SLN), with higher entrapment efficiencies and a better safety profile. In this experimental research, CS-NLC was shown to be an effective nanocarrier for i.n. administration, obtaining brain targeting. However, less than expected concentrations of drug were obtained in the brain [27]. Thus, further modifications with this nanoformulation are needed in order to enhance CNS drug targeting after i.n. administration.
Another strategy to enhance NP target delivery into the brain is the use of cell-penetrating peptides (CPP). CPP are short amphipathic and cationic peptides which are rapidly internalized across cell membranes. They can be attached to the nanocarrier’s surface in order to increase drug permeating efficiency and tissue targeting. Regarding nose-to-brain delivery, TAT and penetratin are well-known CPP for enhancing CNS targeting [28, 29]. Indeed, Gartziandia et al. confirmed the suitability of TAT-modified lipid nanocarriers for nose-to-brain delivery in in vitro cell monolayers. Among the different studied formulations, TAT surface-modified CS-NLC (CS-NLC-TAT) formulation exhibited the highest transport rate, confirming the appropriateness of this approach [30].
On the basis of the above mentioned results, the aim of this study was to assess the neuroprotective and neurorestorative potential of CS-NLC-TAT loading GDNF nanoformulation (CS-NLC-TAT-GDNF) intranasally administered to a MPTP (1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine) mouse model of PD. Moreover, the ability of CS-NLC-TAT-GDNF to act as a regulator of the microglia activation process was studied due to the possible implication of this process in the pathogenesis of brain disorders associated with inflammation, such as PD.
Materials and Methods
Materials
Precirol ATO®5 (glyceryl distearate) and Mygliol ® (caprylic/capric triglyceride) were a kind of gift from Gattefosé (France) and Sasol Germany GmbH, respectively. Tween 80 and Lutrol ® F-68 (Poloxamer 188) were purchased from Panreac (Spain). Chitosan (CS) was obtained from NovaMatrix (Norway). Trehalose dihydrate, Triton X-110, MPTP, 3,3′diaminobenzide (DAB), bovine serum albumin (BSA), and primary antibody anti-tyrosine hydroxylase (TH) were acquired from Millipore Sigma Life Sciences (Germany). rhGDNF was purchased from Peprotech (UK), Depex mounting medium from BDH Gum ® (UK), avidin-biotin-peroxidase complex (ABC kit), and DAPI mounting medium from Palex (Spain). Anti-rabbit Alexa fluor IgG 488 was purchased from Invitrogen® and Isoflurane Esteve from Maipe Comercial (Spain). Finally, TAT was obtained from ChinaPeptides.
CS-NLC-TAT-GDNF Preparation
NLCs were prepared using a previously described melt-emulsification technique [27]. Firstly, a mixture of solid and liquid lipids (Precirol ATO ®5 2.5%, w/v and Mygliol ® 0.25% w/v) with GDNF (0.15%, w/v) was melted 5 °C above their melting point (56 °C). Then, an aqueous solution containing the surfactant combination of Tween 80 (3%, w/v) and Poloxamer 188 (2%, w/v) was heated at the same temperature to be added to the lipid phase under continuous stirring, for 60 s and at 50 W (Bradson® Sonifier 250). The resulting emulsion was maintained with magnetic stirring for 15 min at room temperature (RT) and immediately cooled at 4–8 °C overnight to obtain the NLCs formation due to lipid solidification.
Prior to the NLC coating process, TAT was covalently linked to CS by a surface activation method previously described by our research group [30, 31]. Briefly, 250 μl EDC (1-ethyl-3-(3-dimethylaminopropyl)carbodiimide hydrochloride) in solution (1 mg/ml) and 250 μl of sulfo-NHS (N-hydroxysulfosuccinimide) in 0.02 M phosphate buffered saline (PBS) were added dropwise to a 4 ml CS solution (0.5% w/v, in PBS 0.02 M), under magnetic stirring (2 h at RT). For the coupling of TAT, 250 μl TAT solution (1 mg/ml) in PBS (0.02 M; pH 7.4) was added dropwise to the activated CS, under gentle agitation. The TAT-CS solution was maintained under agitation for another 4 h at RT and then incubated 4 °C overnight. The next day, the NLC were coated with TAT-CS; NLC dispersion previously prepared was added dropwise to the TAT-CS solution under continuous agitation for 20 min at RT. After the coating process, CS-NLC-TAT nanoformulation was centrifuged in Amicon filters (Amicon, “Ultracel-100 k”, Millipore, USA) at 908 G (MIXTASEL, P Selecta, Spain) for 15 min, washed three times with Milli-Q water. Finally the nanoformulation was freeze-dried with the cryoprotectant trehalose at a final concentration of 15% (w/w) of the weighed lipid, and then it was lyophilized for 42 h (LyoBeta 15, Telstar, Spain).
NLC Characterization: Particle Size, Zeta Potential, Morphology, and Encapsulation Efficiency
The mean particle size (Z-average diameter) and the polydispersity index (PDI) were measured by Dynamic Light Scattering (DLS), and the zeta potential was determined through Laser Doppler microelectrophoresis (Malvern® Zetasizer Nano ZS, Model Zen 3600; Malvern Instruments Ltd., UK). Three replicate analyses were performed for each formulation. The data are represented as the mean ± SEM. Nanoparticle surface characteristics and morphology were examined by transmission electron microscopy (JEOL JEM 1400 Plus).
The encapsulation efficiency (EE) of the NLC was determined by an indirect method, in which we measured the non-encapsulated GDNF presented in the supernatant obtained after the filtration/centrifugation process described in the “Materials” section. The EE (%) was determined by GDNF Emax® ImmunoAssay System (Promega Corporation, Madison, USA) and calculated using the following equation
Animal Model and Treatments
Nine-week-old male C57BL/6J mice supplied from Charles River Laboratory (Charles River, L’Arbresle, France) were used to produce the MPTP parkinsonian model. Mice were housed in standard conditions with a constant temperature of 22 °C, a 12-h dark/light cycle and ad libitum access to water and food. All experimental procedures were performed in compliance with the Ethical Committee of Animal Welfare (CEBA) at the PROEX 343/14.
The MPTP lesion was carried out as described in previous reports [32, 33]. Fifty-three mice were used, of which five were treated with the saline solution as negative control. The other 48 were treated with the neurotoxin MPTP (30 mg/kg) intraperitoneally (i.p.) administered at 24 h intervals for five consecutive days in order to obtain a PD animal model for testing the different formulations. At the same time, the lesion protocol was initiated the animals were divided into seven groups (n = 6). They got the following treatments on alternate days during 3 weeks, through nasal administration: negative control saline solution (saline i.p + saline i.n.), positive control saline solution (MPTP i.p + saline i.n.), GDNF (MPTP i.p + GDNF i.n.),empty CS-NLC (MPTP i.p + empty CS-NLC i.n.), CS-NLC-GDNF (MPTP i.p + CS-NLC-GDNF i.n.), and CS-NLC-TAT-GDNF (MPTP i.p + CS-NLC-TAT-GDNF i.n.) (Table 1). Mice were anesthetized with isoflurane and maintained in a supine position before the intranasal administration was realized. The corresponding treatments were suspended in 20 μl of PBS for being administered to alternating nostrils (four administrations of 2.5 μl per nostril, leaving 3 min between administrations) using an automatic micropipette. The final dose of GDNF after the 3 weeks treatment was 2.5 μg per each animal group.
Locomotor Activity: Rotarod Test
Locomotor activity of mice was assessed in a Rotarod apparatus (Ugo Basile, Italy) with increasing acceleration. The apparatus consisted of a horizontal motor-driven rotating rod in which the animals were placed perpendicular to the long axis of the rod. The mouse head was directed against the direction of rotation, so that the mouse has to progress forward to avoid falling. Once the animal has been positioned in the axis, the test ends when the animal fell or after a maximum of 5 min. The time spent on the rotating rod was recorded for each animal and trial. On the test day, each mouse is submitted to five consecutive trials with an interval of 30 min between each trial. However, the first four trials are discarded since they are pre-training sessions to familiarize mice with the procedure. Only the results from the fifth trial for each animal were used for statistical comparisons. The animals were tested in the locomotor activity assay before they were lesioned with MPTP, in the second and third week during the treatment and before they were sacrificed (Fig. 1).
TH Immunohistochemistry
Mice were transcardially perfused with 0.9% (w/v) and 4% (v/v) paraformaldehyde in 0.1 M PBS, pH 7.4. The brains were removed and post-fixed for 72 h in paraformaldehyde and then transferred to a PBS solution (0.1 M) for conservation and subsequent analysis. Hereafter, the fixed brains were coronally cut on a vibratome (Leica Microsystem) at 30 μm, and batches of six tissue sections were collected in cold PBS with azide at 0.1% for further examination.
After selecting the brain areas of striatum (ST) and substantia nigra (SN), the TH+ (tyrosine hydroxylase positive) immunohistochemistry assay was performed. Fixed brain sections were washed with 0.1 M PBS. Endogenous peroxidases were quenched using 1% H2O2 (v/v) and 1% (v/v) ethanol in PBS for 15 min at RT. After rinsing, the brain sections were blocked with 2% BSA and 0.5% Triton-X in PBS. Then, they were incubated with primary antibody rabbit anti-tyrosine hydroxylase (1:2000) overnight under constant agitation at 4 °C. The following day, the brain slices were incubated with secondary biotinylated antibody (1:250) for 1 h. All the brain sections were processed with an ABC kit for 90 min, and the reaction was visualized using DAB as the chromogen. Finally, slices were mounted on gelatin-coated slides, dehydrated, and mounted with fixed DPX medium.
Iba-1 Immunohistochemistry
After selecting the brain areas of ST and SN, Iba-1 (ionizing calcium-binding adaptor molecule 1) immunohistochemistry was performed. Fixed brain sections were blocked with 2% (w/v) BSA solution and 0.5% (w/v) Triton-X in PBS. After rinsing, they were incubated in primary antibody Iba-1 (1:1000, Wako) overnight at 4 °C. The following day brain slices were incubated with the secondary antibody: anti-rabbit Alexa Fluor IgG 488 (1:1000) in PBS with 0.1% BSA and 0.1% Triton-X for 2 h. Then, the slices were washed and mounted on gelatin-coated slides and coverslipped with mounting medium with DAPI.
IOD of ST
The optical density of ST TH+ immunoreactive dopaminergic fibers was measured using a computerized analysis system (ImageJ), reading optical densities as gray levels. Images from sections including ST were taken at a 3200-ppp resolution digital scan (HP Photosmart C7200). The IOD reading was corrected for background staining by subtracting the values of an area outside of the ST. Every sixth striatal section was immunolabeled for TH and a total of six sections were analyzed per animal.
Number of TH+ Neurons in SN
The total number of TH+ neurons in SN was estimated by an unbiased stereology method. Images were taken using an inverted microscopy (Eclipse model TE2000-S, Nikon) at × 20 magnification. Uniform, randomly chosen slices through the SN/every sixth section were analyzed for the total TH+ neurons in each mouse. TH+ neurons were scored as positive if their cell-body image included well defined nuclear counterstaining.
Iba-1 Immunohistochemistry Evaluation in ST and SN
The analysis of activated microglia cells was performed by an unbiased stereology method similar to that described in the paragraph above. Images were taken using light microscopy (Leica TCS SP2 AOBS Spectral Confocal Scanner mounted on a Leica DM IRE2 inverted fluorescent microscope) at × 20 magnification. Uniform, randomly chosen slices through the SN and ST/every sixth section were analyzed for the total of activated microglia cells in each mouse. Microglia cells were scored as positive if their cell-body image included well-defined nuclear counterstaining. The images were processed with ImageJ win-64 Fiji.
Statistical Analysis
Results are expressed as mean ± SEM. Experimental data were analyzed using GraphPad Prism (v. 6.01, GraphPad Software, Inc.). One-way ANOVA was used for TH+ histological analysis evaluation. Student’s t test was applied for behavioral data and Iba-1 immunohistochemistry results, in both ST and SN. P values < 0.05 were considered significant.
Results
Nanoparticle Characterization
As shown in Fig. 2, all formulations had a similar mean size. Moreover, they all exhibited positive zeta values, which indicated that the CS-coating process was successful. Regarding encapsulation efficiency, there were no statistically significant differences between both formulations, being about 87% for both of them. In the external morphological study made by TEM, the nanoparticles showed uniform size without abnormalities.
Study of Locomotor Activity in MPTP-Treated Mice
In order to assess the capability of CS-NLC-TAT-GDNF to restore MPTP-induced locomotor impairment, the Rotarod test was performed (Fig. 3). Moreover, this test confirmed the suitability of the MPTP animal model, given that the administration of this toxin led to a statistically significant impairment on motor performance from the second week until the end of the study: MPTP (week 2 37.17 ± 6.1; week 3 34.2 ± 5.7; week 4 44.8 ± 6.7) vs Control (week 2 93.8 ± 26.3; week 3 118.4 ± 59.9; week 4 107.3 ± 21.84).
Graphical representation of the data obtained from Rotarod test before and after MPTP administration and treated with different formulations. The Rotarod test was performed before the MPTP lesion, at the second and third week after the lesion, and before sacrifice. The data are shown as the mean ± SEM. (*p < 0.05 Control vs MPTP; &&&& p < 0.0001 CS-NLC-TAT-GDNF vs MPTP; & p < 0.05 CS-NLC-TAT-GDNF vs CS-NLC-blank, CS-NLC-GDNF; ## p < 0.05 CS-NLC-TAT-GDNF vs MPTP; # p < 0.05 CS-NLC-TAT-GDNF vs CS-NLC-blank; ++ p < 0.01 CS-NLC-TAT-GDNF vs MPTP, CS-NLC-blank; + p < 0.05 CS-NLC-TAT-GDNF vs CS-NLC-GDNF)
On the other hand, as shown in Fig. 3, the administration of CS-NLC-TAT-GDNF led to a significant improvement of the locomotor activity since this lipid nanoparticle administration was initiated. Whereas other groups exhibited a more attenuated recovery, mice treated with CS-NLC-TAT-GDNF displayed a statistically significant increase in motor performance since the beginning of the study at week 2 (191.8 ± 21.9; *p < 0.05). This recovery was constant for the duration of the test: week 3 (175.3 ± 35.9; *p < 0.05) and week 4 (176.4 ± 38.8; *p < 0.05). The values of this group are comparable to the Control group. Although GDNF and CS-NLC-GDNF produce an improvement in locomotor activity, these were not statistically significant in any of the 3 weeks.
Histological Evaluation
In addition to behavioral studies, immunohistochemical techniques were also used to analyze the efficacy of the treatments in a PD mouse model. For this purpose, 3 weeks after the treatment started, the animals were sacrificed in order to examine the presence of dopaminergic structures in both ST and SN. Figure 4a–g shows representative photomicrographs of TH immunostain in ST of the different treatment groups. It is remarkable the degeneration of TH+ fibers in the ST after MPTP administration (MPTP 93.22 ± 4.1 vs Control 136.1 ± 8.8; %%%% p < 0.05), confirming the success of the lesion. The administration of GDNF did not statistically increase the density of TH fibers (108.6 ± 5.03; p > 0.05) nor did the administration of CS-NLC-GDNF (88.64 ± 3.1; p > 0.05). In contrast, the administration of CS-NLC-TAT-GDNF resulted in the highest regeneration of TH+ fibers (141. 18 ± 5.68;****p < 0.05). On the other hand, the percentage of recovery of TH+ positive neurons was analyzed in the SN (Fig. 5). As in the ST, the percentage of TH+ neurons decreased after MPTP administration (25.02 ± 2.26; ****p < 0.05) compared to control, ratifying the lesion made by the parkinsonizing agent. The exogenous administration of GDNF did not statically increase the percentage of TH+ neurons. However, the encapsulation of this GF statically increased the percentage of TH+ neurons in both formulations (CS-NLC-GDNF and CS-NLC-TAT-GDNF). Moreover, the highest recovery of TH+ neurons was observed in the group of animals treated with CS-NLC-TAT-GDNF (91.46 ± 7.54; #### p < 0.05), which is in accordance with the results obtained in the ST.
Histological evaluation of the striatum. Representative photomicrographs of TH immunostain in ST in all mice groups: MPTP (a), Control (b), GDNF (c), CS-NLC-blank (d), CS-NLC-GDNF (e), and CS-NLC-TAT-GDNF (f). The integrated optical density (IOD) of TH+ fibers in the ST of all groups (g). The data are shown as the mean ± SEM. (%%%% p < 0.05 Control vs MPTP; ****p < 0.05 CS-NLC-TAT-GDNF vs MPTP, CS-NLC-GDNF; &&& p < 0.05 CS-NLS-TAT-GDNF vs CS-NLC-blank; ## p < 0.05 CS-NLC-TAT GDNF vs GDNF, one-way ANOVA)
Histological evaluation of the SN. Representative photomicrographs of TH immunostain in SN in all groups (a): MPTP, Control, GDNF, CS-NLC-blank, CS-NLC-GDNF, and CS-NLC-TAT-GDNF. b TH+ neurons in SN (%). The data are shown as the mean ± SEM. (****p < 0.05 Control vs MPTP; #### p < 0.05 CS-NLC-TAT-GDNF vs MPTP, GDNF and CS-NLC-blank; && p < 0.05 CS-NLC-TAT-GDNF vs CS-NLC-GDNF, one-way ANOVA)
Microglial Activation Evaluation
Iba1 immunohistochemistry was performed in order to check the ability of our novel nanoformulation to decrease the number of activated microglia in both ST and SN (Fig. 6). First, the potential microglial toxicity of MPTP was confirmed in both ST and SN. Indeed, the number of activated microglia was markedly increased in ST (144.8 ± 3.2; ****p < 0.0001) and in the SN it was almost duplicate (188.1 ± 4.1; ****p < 0.0001).
Histological evaluation of activated microglia cells in both ST and SN. a Representative Iba-1 immunophotographs of all mice groups in the SN. (Control, MPTP, GDNF, CS-NLC-blank, CS-NLC-GDNF and CS-NLC-TAT-GDNF). b Iba-1 cells in ST of all mice groups (%). The data are shown as the mean ± SEM. (****p < 0.0001 MPTP vs Control; #### p < 0.0001CS-NLC-TAT-GDNF vs MPTP and GDNF, Student’s t test). c Iba-1 cells in SN of all mice groups (%). The data are shown as the mean ± SEM. (****p < 0.001 MPTP vs Control, #### p < 0.0001 CS-NLC-TAT-GDNF vs MPTP, GDNF and CS-NLC-blank; & p < 0.05 CS-NLC-TAT-GDNF vs CS-NLC-GDNF, Student’s t test)
Moreover, as seen in Fig. 6, the number of activated microglia after GDNF treatment (148.2 ± 3.2) is similar to that obtained after MPTP administration; therefore, the free GDNF administration did not produce a therapeutic effect as it did not decrease the level of activated microglia. However, when this GF was encapsulated into CS-NLC (CS-NLC-GDNF), the number of activated microglia was significantly decreased (105.6 ± 5.2; #### p < 0.0001). In addition, in the group treated with CS-NLC-TAT-GDNF, activated microglia levels were still lower (99.43.0 ± 4.25; #### p < 0.0001). Although no significant differences were seen between these two formulations (CS-NLC-GDNF vs CS-NLC-TAT-GDNF), a downward trend was observed.
Regarding the results obtained in SN, the tendency seen in the number of activated microglia is similar to the outcome achieved in ST. GDNF did not decrease the number of activated microglia (172.4 ± 6.4), but as we have previously pointed out in ST, the encapsulation into CS-NLC (CS-NLC-GDNF) led to a decrease of activated microglia levels (124.3 ± 3.2; #### p < 0.0001). Contrary to the results obtained in ST, the CS-NLC-TAT-GDNF group exhibited a statistically significant decrease vs the CS-NLC-GDNF treated group (& p < 0.05), with the lowest levels of activated microglia (107.0 ± 6.2; #### p < 0.0001).
Discussion
Despite all the efforts made by the scientific community to obtain an effective therapy for PD, current available treatments cannot halt the progression of this disorder. In an attempt to address the neurodegenerative process, different disease-modifying treatments are under investigation [34]. Among others, GFs and specially the use of GDNF are particularly promising since these exhibit efficacy in the upregulation of the neurological mechanism involved in neurogenic processes and, therefore, modulates the progression of the disease [8]. However, the hydrophilic nature of GDNF makes it difficult to cross the BBB, and for that reason, in the past few years, numerous researchers have developed different nano- and microformulations loading GDNF as an approach for PD treatment [35,36,37,38,39]. However, the invasive routes of administration used involve some risk which makes its translation to clinical practice difficult. In order to avoid them, new administration routes are under investigation, such as i.n. administration. In an attempt to increase the mucosal contact time and extend the residence time in the nasal cavity, nanoparticles can be coated with mucoadhesive substances, such as chitosan. Many studies published in the past few years have developed CS-coated nanoparticles for the brain delivery of different drugs. Although in all these studies the obtained brain concentrations of drugs were less than desired, they were enough to obtain a significant pharmacodynamic effect [22, 26, 27, 40]. In light of these encouraging results, further modifications of nanoparticle surface should enhance brain concentrations, maximizing the therapeutic effect of this drug. Accordingly, in the present study, a previously developed CS-NLC was coated with TAT peptide in light of our previous studies in in vitro cell monolayers, which confirmed the suitability of CS-NLC-TAT for nose-to-brain drug delivery [30]. Thus, in the present work, GNDF was encapsulated into TAT-modified lipid nanocarriers (CS-NLC-TAT-GDNF) in order to enhance brain targeting.
Nanoparticle physicochemical characterization revealed values similar to those reported by us in previous work [30, 40]. Hereafter, the in vivo study was performed to prove the efficacy of our novel formulation by i.n. administration. For that main purpose, a MPTP animal model of PD was used. This model includes apoptotic cell death of DA neurons located in SNc and loss of striatal TH+ fibers. Moreover, this MPTP animal model mimics the clinical cardinal symptoms of PD in humans. For all these reasons, it is considered the gold standard animal model to screen neuroprotective and neurorestorative treatments for PD [33, 41, 42].
The Rotarod test evidenced motor recovery soon after CS-NLC-TAT-GDNF i.n. administration and exhibited the best levels until the end of the study. In contrast, GDNF did not statistically improve the behavioral activity and neither did CS-NLC-GDNF, although a slight recovery can be seen. This finding was unexpected, since in our previous work, the administration of CS-NLC-GDNF has been shown to reach the brain and improve locomotor activity [40]. However, it should be noted that both the animal model and the administration frequency is different in this study. Indeed, in this research, we used an MPTP mouse model with treatment on alternate days. In contrast, in the previous work, 6-hydroxydopamine partially lesioned rats with daily administration of CS-NLC-GDNF were used to assess the neuroprotective activity of the treatment.
In addition, the histological evaluation of the brains was performed. The injection of MPTP is directly related with degeneration of dopaminergic neurons, which means low density of TH+ structures in ST and SN, as seen in the results (Figs. 4 and 5). The exogenous administration of GDNF did not lead to a statistically significant increase in either in the ST or SN. Indeed, it is a known fact that GDNF is a peptide which has difficulty crossing the BBB so it needs to be directly administered into the CNS [43]. This is probably why the i.n. administration of this GF did not exhibit any therapeutic effect in this study. However, the CS-NLC-TAT-GDNF-treated group increased the level of TH+ structures in both ST and SN, highlighting the improvement with GDNF brain targeting obtained after the lipid nanoparticle coated process with CS and TAT. Furthermore, the group treated with CS-NLC-GDNF did not increase TH+ fibers as expected, especially in ST, in light of Gartziandia et al. findings [40]. As noted before, not only the animal model but also the administration frequency were different in this new in vivo assay, so it is difficult to extrapolate these results and make a reliable comparison. In any case, in the present study, we determined that the surface modification with TAT maximized the therapeutic benefits of GDNF, inducing histological recovery not only in the SN but also in ST [28, 29].
To date, investigations with GDNF for PD treatment have focused on the neuroprotective and neurorestorative potential of this GF. However, recently, it has been highlighted the therapeutic effect of GDNF modulating microglial activation process in the disease. Indeed, microglia-mediated neuroinflammation has gained much attention in the development of PD and its treatment seems to be a key therapeutic option to prevent the progression of the neurodegenerative process. In the last few years, research studies with primary rat microglia cultures and mouse microglial cell lines have demonstrated that GDNF decreases the synthesis and release of proinflammatory and neurotoxic molecules [44,45,46]. Therefore, the exogenous administration of GDNF may not only have a protective effect on neurons but may also modulate microglial activities to exert its therapeutic effect.
That is why in the present study, Iba-1 immunostaining was performed to assess the potential of the CS-NLC-TAT-GDNF formulation to decrease microglial activation in a MPTP mouse model of PD. Among different neurotoxic molecules, MPTP is known to produce an increase in microglial activation, which has been confirmed in monkeys, mice, and even in humans [47,48,49]. The data obtained in this study are in accordance with these results, since the subchronic administration of MPTP led to a statistically significant increase in the number of activated microglial cells. Moreover, microscopic photographs (Fig. 6) also illustrated the MPTP induced microglia activation.
The administration of GDNF did not decrease the activation of microglial cells. However, when encapsulated into surface modified lipid nanocarriers, the number of microglial activated cells decreased almost to control levels. These results were observed in both ST and SN. Moreover, the administration of CS-NLC-TAT-GDNF in SN was statistically significant when compared with CS-NLC-GDNF, which confirmed not only the suitability of the CS coating process but also the surface modification with TAT to bypass the BBB. Additionally, microglia is more numerous in the SN than in adjacent structures of the brain, resulting in an increase in apoptotic biomarkers and cytokines levels. These findings are supported by studies in both PD animal models and Parkinson’s patients [50, 51]. Therefore, our results are encouraging since the exogenous administration of GDNF, encapsulated into our novel nanoformulation, targets microglia activation, modulating the neuroinflammatory component of PD.
Conclusion
Taking all these results into account, we can conclude that the in vivo administration of CS-NLC-TAT-GDNF improves the nose-to-brain delivery of GDNF. Both the behavioral studies and the immunohistochemistry data have confirmed that i.n. administration of our novel nanoformulation may be a promising treatment for PD. In addition, the exogenous administration of GDNF in these biodegradable nanocarriers has demonstrated to reduce microgliosis in a MPTP mouse model of the disease. Although further studies are needed to ensure these findings, all in all, it can be concluded that this nanoformulation approach is a step forward in PD therapy.
References
Lees AJ, Hardy J, Revesz T (2009) Parkinson’s disease. Lancet 373:2055–2066. doi:10.1016/S0140-6736(09)60492-X
Nussbaum RL, Ellis CE (2003) Alzheimer’s disease and Parkinson’s disease. N Engl J Med 348:1356–1364. doi:10.1056/NEJM2003ra020003
Kalia LV, Lang AE (2015) Parkinson’s disease. Lancet 386:896–912. doi:10.1016/S0140-6736(14)61393-3
Hirsch EC, Hunot S (2009) Neuroinflammation in Parkinson’s disease: a target for neuroprotection? Lancet Neurol 8:382–397. doi:10.1016/S1474-4422(09)70062-6
Joers V, Tansey MG, Mulas G, Carta AR (2016) Microglial phenotypes in Parkinson’s disease and animal models of the disease. Prog Neurobiol. doi:10.1016/j.pneurobio.2016.04.006
Long-Smith CM, Sullivan AM, Nolan YM (2009) The influence of microglia on the pathogenesis of Parkinson’s disease. Prog Neurobiol 89:277–287. doi:10.1016/j.pneurobio.2009.08.001
Oertel W, Schulz JB (2016) Current and experimental treatments of Parkinson disease: a guide for neuroscientists. J Neurochem 139(Suppl 1):325–337. doi:10.1111/jnc.13750
Allen SJ, Watson JJ, Shoemark DK, Barua NU, Patel NK (2013) GDNF, NGF and BDNF as therapeutic options for neurodegeneration. Pharmacol Ther 138:155–175. doi:10.1016/j.pharmthera.2013.01.004
Sullivan AM, Toulouse A (2011) Neurotrophic factors for the treatment of Parkinson’s disease. Cytokine Growth Factor Rev 22:157–165. doi:10.1016/j.cytogfr.2011.05.001
Lapchak PA, Gash DM, Jiao S, Miller PJ, Hilt D (1997) Glial cell line-derived neurotrophic factor: a novel therapeutic approach to treat motor dysfunction in Parkinson’s disease. Exp Neurol 144:29–34. doi:10.1006/exnr.1996.6384
Gill SS, Patel NK, Hotton GR, O’Sullivan K, McCarter R, Bunnage M, Brooks DJ, Svendsen CN et al (2003) Direct brain infusion of glial cell line-derived neurotrophic factor in Parkinson disease. Nat Med 9:589–595. doi:10.1038/nm850
Lang AE, Gill S, Patel NK et al (2006) Randomized controlled trial of intraputamenal glial cell line-derived neurotrophic factor infusion in Parkinson disease. Ann Neurol 59:459–466. doi:10.1002/ana.20737
Nutt JG, Burchiel KJ, Comella CL, Jankovic J, Lang AE, Laws ER Jr, Lozano AM, Penn RD et al, ICV GDNF Study Group. Implanted intracerebroventricular. Glial cell line-derived neurotrophic factor (2003) Randomized, double-blind trial of glial cell line-derived neurotrophic factor (GDNF) in PD. Neurology 60:69–73
Salvatore MF, Ai Y, Fischer B, Zhang AM, Grondin RC, Zhang Z, Gerhardt GA, Gash DM (2006) Point source concentration of GDNF may explain failure of phase II clinical trial. Exp Neurol 202:497–505
Tajes M, Ramos-Fernandez E, Weng-Jiang X, Bosch-Morato M, Guivernau B, Eraso-Pichot A, Salvador B, Fernandez-Busquets X et al (2014) The blood-brain barrier: structure, function and therapeutic approaches to cross it. Mol Membr Biol 31:152–167. doi:10.3109/09687688.2014.937468
Djupesland PG, Messina JC, Mahmoud RA (2014) The nasal approach to delivering treatment for brain diseases: an anatomic, physiologic, and delivery technology overview. Ther Deliv 5:709–733. doi:10.4155/tde.14.41
Costantino HR, Illum L, Brandt G, Johnson PH, Quay SC (2007) Intranasal delivery: physicochemical and therapeutic aspects. Int J Pharm 337:1–24. doi:10.1016/j.ijpharm.2007.03.025
Re F, Gregori M, Masserini M (2012) Nanotechnology for neurodegenerative disorders. Maturitas 73:45–51. doi:10.1016/j.maturitas.2011.12.015
Shah B, Khunt D, Bhatt H, Misra M, Padh H (2015) Application of quality by design approach for intranasal delivery of rivastigmine loaded solid lipid nanoparticles: effect on formulation and characterization parameters. Eur J Pharm Sci 78:54–66. doi:10.1016/j.ejps.2015.07.002
Sharma S, Lohan S, Murthy RSR (2013) Formulation and characterization of intranasal mucoadhesive nanoparticulates and thermo-reversible gel of levodopa for brain delivery. Drug Dev Ind Pharm 40:869–878. doi:10.3109/03639045.2013.789051
Zhang C, Chen J, Feng C, Shao X, Liu Q, Zhang Q, Pang Z, Jiang X (2014) Intranasal nanoparticles of basic fibroblast growth factor for brain delivery to treat Alzheimer’s disease. Int J Pharm 461:192–202. doi:10.1016/j.ijpharm.2013.11.049
Md S, Khan RA, Mustafa G, Chuttani K, Baboota S, Sahni JK, Ali J (2013) Bromocriptine loaded chitosan nanoparticles intended for direct nose to brain delivery: pharmacodynamic, pharmacokinetic and scintigraphy study in mice model. Eur J Pharm Sci 48:393–405. doi:10.1016/j.ejps.2012.12.007
Mistry A, Glud SZ, Kjems J, Randel J, Howard KA, Stolnik S, Illum L (2009) Effect of physicochemical properties on intranasal nanoparticle transit into murine olfactory epithelium. J Drug Target 17:543–552. doi:10.1080/10611860903055470
Fazil M, Md S, Haque S, Kumar M, Baboota S, Jk S, Ali J (2012) Development and evaluation of rivastigmine loaded chitosan nanoparticles for brain targeting. Eur J Pharm Sci 47:6–15. doi:10.1016/j.ejps.2012.04.013
Zhao Y, Li X, Lu C, Lin M, Chen L, Xiang Q, Zhang M, Jin R et al (2014) Gelatin nanostructured lipid carriers-mediated intranasal delivery of basic fibroblast growth factor enhances functional recovery in hemiparkinsonian rats. Nanomedicine 10:755–764. doi:10.1016/j.nano.2013.10.009
Jafarieh O, Md S, Ali M, Baboota S, Sahni JK, Kumari B, Bhatnagar A, Ali J (2015) Design, characterization, and evaluation of intranasal delivery of ropinirole-loaded mucoadhesive nanoparticles for brain targeting. Drug Dev Ind Pharm 41:1674–1681. doi:10.3109/03639045.2014.991400
Gartziandia O, Herran E, Pedraz JL, Carro E, Igartua M, Hernandez RM (2015) Chitosan coated nanostructured lipid carriers for brain delivery of proteins by intranasal administration. Colloids Surf B Biointerfaces 134:304–313. doi:10.1016/j.colsurfb.2015.06.054
Qin Y, Chen H, Zhang Q, Wang X, Yuan W, Kuai R, Tang J, Zhang L et al (2011) Liposome formulated with TAT-modified cholesterol for improving brain delivery and therapeutic efficacy on brain glioma in animals. Int J Pharm 420:304–312. doi:10.1016/j.ijpharm.2011.09.008
Kanazawa T, Akiyama F, Kakizaki S, Takashima Y, Seta Y (2013) Delivery of siRNA to the brain using a combination of nose-to-brain delivery and cell-penetrating peptide-modified nano-micelles. Biomaterials 34:9220–9226. doi:10.1016/j.biomaterials.2013.08.036
Gartziandia O, Egusquiaguirre SP, Bianco J, Pedraz JL, Igartua M, Hernandez RM, Préat V, Beloqui A (2016) Nanoparticle transport across in vitro olfactory cell monolayers. Int J Pharm 499:81–89. doi:10.1016/j.ijpharm.2015.12.046
Egusquiaguirre SP, Manguán-García C, Pintado-Berninches L et al (2015) Development of surface modified biodegradable polymeric nanoparticles to deliver GSE24.2 peptide to cells: a promising approach for the treatment of defective telomerase disorders. Eur J Pharm Biopharm 91:91–102. doi:10.1016/j.ejpb.2015.01.028
Anitua E, Pascual C, Pérez-Gonzalez R, Orive G, Carro E (2015) Intranasal PRGF-Endoret enhances neuronal survival and attenuates NF-κB-dependent inflammation process in a mouse model of Parkinson’s disease. J Control Release 203:170–180. doi:10.1016/j.jconrel.2015.02.030
Blandini F, Armentero MT (2012) Animal models of Parkinson’s disease. FEBS J 279:1156–1166. doi:10.1111/j.1742-4658.2012.08491.x
Kalia LV, Kalia SK, Lang AE (2015) Disease-modifying strategies for Parkinson’s disease. Mov Disord 30:1442–1450. doi:10.1002/mds.26354
Herran E, Requejo C, Ruiz-Ortega JA et al (2014) Increased antiparkinson efficacy of the combined administration of VEGF- and GDNF-loaded nanospheres in a partial lesion model of Parkinson’s disease. Int J Nanomedicine 9:2677–2687
Herrán E, Ruiz-Ortega JÁ, Aristieta A, Igartua M, Requejo C, Lafuente JV, Ugedo L, Pedraz JL et al (2013) In vivo administration of VEGF- and GDNF-releasing biodegradable polymeric microspheres in a severe lesion model of Parkinson’s disease. Eur J Pharm Biopharm 85:1183–1190. doi:10.1016/j.ejpb.2013.03.034
Garbayo E, Montero-Menei CN, Ansorena E, Lanciego JL, Aymerich MS, Blanco-Prieto MJ (2009) Effective GDNF brain delivery using microspheres—a promising strategy for Parkinson’s disease. J Control Release 135:119–126. doi:10.1016/j.jconrel.2008.12.010
Garbayo E, Ansorena E, Lanciego JL, Blanco-Prieto MJ, Aymerich MS (2011) Long-term neuroprotection and neurorestoration by glial cell-derived neurotrophic factor microspheres for the treatment of Parkinson’s disease. Mov Disord 26:1943–1947. doi:10.1002/mds.23793
Jollivet C, Aubert-Pouessel A, Clavreul A, Venier-Julienne M, Remy S, Montero-Menei CN, Benoit J, Menei P (2004) Striatal implantation of GDNF releasing biodegradable microspheres promotes recovery of motor function in a partial model of Parkinson’s disease. Biomaterials 25:933–942. doi:10.1016/S0142-9612(03)00601-X
Gartziandia O, Herrán E, Ruiz-Ortega JA, Miguelez C, Igartua M, Lafuente JV, Pedraz JL, Ugedo L et al (2016) Intranasal administration of chitosan-coated nanostructured lipid carriers loaded with GDNF improves behavioral and histological recovery in a partial lesion model of Parkinson’s disease. J Biomed Nanotechnol 12:1–11. doi:10.1166/jbn.2016.2313
Schober A (2004) Classic toxin-induced animal models of Parkinson’s disease: 6-OHDA and MPTP. Cell Tissue Res 318:215–224. doi:10.1007/s00441-004-0938-y
Blesa J, Przedborski S (2014) Parkinso’s disease: animal models and dopaminergic cell vulnerability. Front Neuroanat 8:155. doi:10.3389/fnana.2014.00155
Barker RA (2009) Parkinson’s disease and growth factors—are they the answer? Parkinsonism Relat Disord 15(Supplement 3):S181–S184. doi:10.1016/S1353-8020(09)70810-7
Chang YP, Fang KM, Lee TI, Tzeng SF (2006) Regulation of microglial activities by glial cell line derived neurotrophic factor. J Cell Biochem 97:501–511. doi:10.1002/jcb.20646
Rocha SM, Cristovão AC, Campos FL, Fonseca CP, Baltazar G (2012) Astrocyte-derived GDNF is a potent inhibitor of microglial activation. Neurobiol Dis 47:407–415. doi:10.1016/j.nbd.2012.04.014
Rickert U, Grampp S, Wilms H, Spreu J, Knerlich-Lukoschus F, Held-Feindt J, Lucius R (2014) Glial cell line-derived neurotrophic factor family members reduce microglial activation via inhibiting p38MAPKs-mediated inflammatory responses. J Neurodegener Dis 2014:369468. doi:10.1155/2014/369468
Liberatore GT, Jackson-Lewis V, Vukosavic S, Mandir AS, Vila M, McAuliffe WG, Dawson VL, Dawson TM et al (1999) Inducible nitric oxide synthase stimulates dopaminergic neurodegeneration in the MPTP model of Parkinson disease. Nat Med 5:1403–1409. doi:10.1038/70978
Langston JW, Forno LS, Tetrud J, Reeves AG, Kaplan JA, Karluk D (1999) Evidence of active nerve cell degeneration in the substantia nigra of humans years after 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine exposure. Ann Neurol 46:598–605
McGeer PL, Schwab C, Parent A, Doudet D (2003) Presence of reactive microglia in monkey substantia nigra years after 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine administration. Ann Neurol 54:599–604. doi:10.1002/ana.10728
Lawson LJ, Perry VH, Dri P, Gordon S (1990) Heterogeneity in the distribution and morphology of microglia in the normal adult mouse brain. Neuroscience 39:151–170. doi:10.1016/0306-4522(90)90229-W
Mogi M, Kondo T, Mizuno Y, Nagatsu T (2007) p53 protein, interferon-γ, and NF-κB levels are elevated in the parkinsonian brain. Neurosci Lett 414:94–97. doi:10.1016/j.neulet.2006.12.003
Acknowledgements
This project was partially supported by the “Ministerio de Economía y Competitividad” (SAF2013-42347-R), the University of the Basque Country (UPV/EHU) (UFI 11/32), and the FEDER funds. The authors thank SGIker of UPV/EHU and European funding (ERDF and ESF) for technical and human support. The authors also wish to thank the intellectual and technical assistance from the ICTS “NANBIOSIS”, more specifically by the Drug Formulation Unit (U10) of the CIBER-BBN at the UPV/EHU.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hernando, S., Herran, E., Figueiro-Silva, J. et al. Intranasal Administration of TAT-Conjugated Lipid Nanocarriers Loading GDNF for Parkinson’s Disease. Mol Neurobiol 55, 145–155 (2018). https://doi.org/10.1007/s12035-017-0728-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-017-0728-7