Abstract
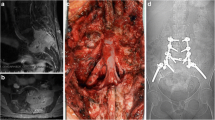
INTRODUCTION: The efficacy of Gamma Knife surgery (GKS) in local tumor control of non-secreting paragangliomas (PGLs) has been fully described by previous studies. However, with regard to secreting PGL, only one previous case report exists advocating its efficacy at a biological level. CASE REPORT: The aims of this study were: 1) to evaluate the safety/efficacy of GKS in a dopamine-secreting PGL; 2) to investigate whether the biological concentrations of free methoxytyramine could be used as a marker of treatment efficacy during the follow-up. We describe the case of a 62-year-old man diagnosed with left PGL. He initially underwent complete surgical excision. Thirty months after, he developed recurrent biological and neuroradiological disease; the most sensitive biomarker for monitoring the disease, concentration of plasma free methoxytyramine, started to increase. GKS was performed at a maximal marginal dose of 16 Gy. During the following 30 months, concentration of free methoxytyramine gradually decreased from 0.14 nmol/l (2*URL) before GKS to 0.09 nmol/l, 6 months after GKS and 0.07 nmol/l at the last follow-up after GKS (1.1*URL), confirming the efficacy of the treatment. Additionally, at 30 months there was approximately 36.6% shrinkage from the initial target volume. CONCLUSION: The GKS treatment was safe and effective, this being confirmed clinically, neuroradiologically and biologically. The case illustrates the importance of laboratory tests taking into account methoxytyramine when analyzing biological samples to assess the biochemical activity of a PGL. In addition, the identification of methoxytyramine as a unique positive biomarker could designate it for the monitoring of tumor relapse after treatments, including Gamma Knife surgery.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Kuhweide R, Lanser MJ, Fisch U, 1996 Catecholamine-secreting paragangliomas at the skull base. Skull Base Surg 6: 35–45.
Manolidis S, Shohet JA, Jackson CG, Glasscock ME 3rd, 1999 Malignant glomus tumors. Laryngoscope 109: 30–34.
Castrucci WA, Chiang VL, Hulinsky I, Knisely JP, 2010 Biochemical and clinical responses after treatment of a catecholamine-secreting glomus jugulare tumor with gamma knife radiosurgery. Head Neck 32: 1720–1727.
Chen PG, Nguyen JH, Payne SC, Sheehan JP, Hashisaki GT, 2010 Treatment of glomus jugulare tumors with gamma knife radiosurgery. Laryngoscope 120: 1856–1862.
Lieberson RE, Adler JR, Soltys SG, Choi C, Gibbs IC, Chang SD, 2012 Stereotactic radiosurgery as the primary treatment for new and recurrent paragangliomas: is open surgical resection still the treatment of choice? World Neurosurg 77: 745–761.
Miller JP, Semaan M, Einstein D, Megerian CA, Maciunas RJ, 2009 Staged Gamma Knife radiosurgery after tailored surgical resection: a novel treatment paradigm for glomus jugulare tumors. Stereotact Funct Neurosurg 87: 31–36.
Schwaber MK, Glasscock ME, Nissen AJ, Jackson CG, Smith PG, 1984 Diagnosis and management of catecholamine secreting glomus tumors. Laryngoscope 94: 1008–1015.
Erickson D, Kudva YC, Ebersold MJ, et al, 2001 Benign paragangliomas: clinical presentation and treatment outcomes in 236 patients. J Clin Endocrinol Metab 86: 5210–5216.
Puder J, Stadelmann R, Schoettker P, Buclin T, Grouzmann E, 2013 A pain in the neck. Clin Chem 59: 1280–1281.
Woods CI, Strasnick B, Jackson CG, 1993 Surgery for glomus tumors: the Otology Group experience. Laryngoscope 103: 11 Pt 2 Suppl 60: 65–70.
Jansen JC, van den Berg R, Kuiper A, van der Mey AG, Zwinderman AH, Cornelisse CJ, 2000 Estimation of growth rate in patients with head and neck paragangliomas influences the treatment proposal. Cancer 88: 2811–2816.
Jackson CG, Kaylie DM, Coppit G, Gardner EK, 2004 Glomus jugulare tumors with intracranial extension. Neurosurg Focus 17: E7.
Rosenwasser H, 1952 Glomus jugularis tumor of the middle ear; carotid body tumor, tympanic body tumor, nonchromaffin paraganglioma. Trans Am Laryngol Rhinol Otol Soc 3(56th Meeting): 94–106.
Al-Mefty O, Teixeira A, 2002 Complex tumors of the glomus jugulare: criteria, treatment, and outcome. J Neurosurg 97: 1356–1366.
Green JD Jr, Brackmann DE, Nguyen CD, Arriaga MA, Telischi FF, De la Cruz A, 1994 Surgical management of previously untreated glomus jugulare tumors. Laryngoscope. 104: 8 Pt 1: 917–921.
Tasar M, Yetiser S, 2004 Glomus tumors: therapeutic role of selective embolization. J Craniofac Surg 15: 497–505.
Li G, Chang S, Adler JR Jr, Lim M, 2007 Irradiation of glomus jugulare tumors: a historical perspective. Neurosurg Focus 23: E13.
Genc A, Bicer A, Abacioglu U, Peker S, Pamir MN, Kilic T, 2010 Gamma knife radiosurgery for the treatment of glomus jugulare tumors. J Neurooncol 97: 101–108.
Duke WM, Phillips MW, Donald JM Jr, Boshell BR, 1965 A Norepinephrine-Secreting Glomic Tissue Tumor (Chemodectoma). JAMA 193: 20–22.
Pluta RM, Ram Z, Patronas NJ, Keiser H, 1994 Long-term effects of radiation therapy for a catecholamine-producing glomus jugulare tumor. Case report. J Neurosurg 80: 1091–1094.
Osorio JE, Powell TD, Frank RS, et al, 2003 Recombinant raccoon pox vaccine protects mice against lethal plague. Vaccine 21: 1232–1238.
Brown JS, 1985 Glomus jugulare tumors revisited: a ten-year statistical follow-up of 231 cases. Laryngoscope 95: 284–288.
van Duinen N, Steenvoorden D, Kema IP, et al, 2010 Increased urinary excretion of 3-methoxytyramine in patients with head and neck paragangliomas. J Clin Endocrinol Metab 95: 209–214.
Eisenhofer G, Goldstein DS, Sullivan P, et al, 2005 Biochemical and clinical manifestations of dopamine-producing paragangliomas: utility of plasma methoxytyramine. J Clin Endocrinol Metab 90: 2068–2075.
Zendron L, Fehrenbach J, Taverna C, Krause M, 2004 Pitfalls in the diagnosis of phaeochromocytoma. BMJ 328: 629–630.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tuleasca, C., Jaquet, Y., Schweizer, V. et al. Clinical and biochemical responses after Gamma Knife surgery for a dopamine-secreting paraganglioma: case report. Hormones 15, 106–112 (2016). https://doi.org/10.1007/BF03401409
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03401409