Abstract
Purpose
Dexamethasone may have potential advantages in the prevention of postoperative sore throat. We therefore undertook a study to evaluate the efficacy of intravenously administered dexamethasone in reducing the incidence and severity of postoperative sore throat in patients receiving general anesthesia with endotracheal intubation.
Methods
In a randomized, double-blind and placebo-controlled study, 120 patients receiving general anesthesia with endotracheal intubation were randomly assigned to two groups. Group 1 (control) patients received normal saline 2 mL iv and group 2 (D) patients received dexamethasone 8 mg iv. After surgery, visual analogue scale (VAS) scores at rest and with effort (swallowing movement) for postoperative sore throat were recorded by a blinded observer.
Results
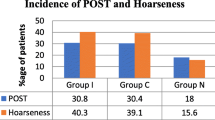
The overall incidence of postoperative sore throat during the first 24 hr following surgery was lower in dexamethasone group (D) compared to the control group (C). Eleven (20%) patients in the dexamethasone group had postoperative sore throat, compared to 31 (56.3%) patients in the control group (P < 0.01). Postoperatively at one hour, three hours, six hours, 12 hr and 24 hr, the VAS scores for postoperative sore throat at rest and during effort were lower in the dexamethasone group (D) compared to the control group (P < 0.01) at corresponding time intervals.
Conclusion
Preoperative administration of dexamethasone 8 mg iv reduces the incidence and severity of postoperative sore throat in patients receiving general anesthesia with endotracheal intubation.
Résumé
Objectif
La dexaméthasone pourrait avoir des avantages potentiels pour la prévention des maux de gorge postopératoires. C’est pourquoi nous avons entrepris une étude afin d’évaluer l’efficacité de la dexaméthasone administrée en iv dans la réduction de l’incidence et de la sévérité des maux de gorge postopératoires chez les patients recevant une anesthésie générale avec intubation endotrachéale.
Méthode
Dans une étude randomisée, en double aveugle et contrôlée par placebo, 120 patients recevant une anesthésie générale avec intubation endotrachéale ont été randomisés en deux groupes. Les patients du groupe 1 (témoin) ont reçu du sérum physiologique 2 mL iv et les patients du groupe 2 (D) ont reçu de la dexaméthasone 8 mg iv. Après la chirurgie, les scores de l’échelle visuelle analogue (EVA) au repos et à l’effort (mouvement de déglutition) pour les maux de gorge postopératoires ont été enregistrés par un observateur en aveugle.
Résultats
L’incidence globale de mal de gorge postopératoire durant les premières 24 h suivant la chirurgie était plus basse dans le groupe dexaméthasone (D) comparé au groupe témoin (C). Onze (20 %) patients du groupe dexaméthasone ont souffert de mal de gorge postopératoire, comparé à 31 (56,3 %) patients dans le groupe témoin (P < 0,01). A une heure, trois heures, six, douze et 24 heures postopératoires, les scores EVA pour le mal de gorge postopératoire au repos et à l’effort étaient plus bas dans le groupe dexaméthasone (D) que dans le groupe témoin (P < 0,01) aux intervalles de temps correspondants.
Conclusion
L’administration préopératoire de dexaméthasone 8 mg iv réduit l’incidence et la sévérité des maux de gorge postopératoires chez les patients recevant une anesthésie générale avec intubation endotrachéale.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Lev R, Rosen P. Prophylactic lidocaine use preintubation: a review. J Emerg Med 1994; 12:499–506.
Monroe MC, Gravenstein N, Saga-Rumley S. Postoperative sore throat: effect of oropharyngeal airway in orotracheally intubated patients. Anesth Analg 1990; 70:512–6.
Seegobin RD, van Hasselt GL. Endotracheal cuff pressure and tracheal mucosal blood flow: endoscopic study of effects of four large volume cuffs. Br Med J (Clin Res Ed) 1984; 288:965–8.
Loeser EA, Bennett GM, Orr DL, Stanley TH. Reduction of postoperative sore throat with new endotracheal tube cuffs. Anesthesiology 1980; 52:257–9.
Thomas DV. Hoarseness and sore throat after tracheal intubation. Small tubes prevent (Letter). Anaesthesia 1993; 48:355–6.
Stenqvist O, Nilsson K. Postoperative sore throat related to tracheal tube cuff design. Can Anaesth Soc J 1982; 29:384–6.
Fuller PB. The relationship between preintubation lidocaine and postanesthesia sore throat. AANAJ 1992; 60:374–8.
Ayoub CM, Ghobashy A, Koch ME, et al. Widespread application of topical steroids to decrease sore throat, hoarseness, and cough after tracheal intubation. Anesth Analg 1998; 87:714–6.
el-Hakim M. Beclomethasone prevents postoperative sore throat. Acta Anaesthesiol Scand 1993; 37:250–2.
Baxendale BR, Vater M, Lavery KM. Dexamethasone reduces pain and swelling following extraction of third molar teeth. Anaesthesia 1993; 48:961–4.
Elhakim M, Ali NM, Rashed I, Riad MK, Refat M. Dexamethasone reduces postoperative vomiting and pain after pediatric tonsillectomy. Can J Anesth 2003; 50:392–7.
Schmelzeisen R, Frolich JC. Prevention of postoperative swelling and pain by dexamethasone after operative removal of impacted third molar teeth. Eur J Clin Pharmacol 1993; 44:275–7.
Wang JJ, Ho ST, Lee SC, Liu YC, Liu YH, Liao YC. The prophylactic effect of dexamethasone on postoperative nausea and vomiting in women undergoing thyroidectomy: a comparison of droperidol with saline. Anesth Analg 1999; 89:200–3.
Jensen PJ, Hommelgaard P, Sondergaard P, Eriksen S. Sore throat after operation: influence of tracheal intubation, intracuff pressure and type of cuff. Br J Anaesth 1982; 54:453–7.
Biro P, Seifert B, Pasch T. Complaints of sore throat after tracheal intubation: a prospective evaluation. Eur J Anaesthesiol 2005; 22:307–11.
Hamelberg W, Welch CM, Siddall J, Jacoby J. Complication of endotracheal intubation. J Am Med Assoc 1958; 168:1959–62.
Harding CJ, McVey FK. Interview method affects incidence of postoperative sore throat. Anaesthesia 1987; 42:1104–7.
Stride PC. Postoperative sore throat: topical hydrocortisone. Anaesthesia 1990; 45:968–71.
Yao XL, Cowan MJ, Gladwin MT, Lawrence MM, Angus CW, Shelhamer JH. Dexamethasone alters arachi-donate release from human epithelial cells by induction of p11 protein synthesis and inhibiting phospholipase A2 activity. J Biol Chem 1999; 274:17202–8.
Lubenow TR, Ivankovich AD, McCarthy RJ. Management of acute postoperative pain. In:Barash PG, Cullen BF, Stoelting RK (Eds). Clinical Anesthesia. Philadelphia: Lippincott Williams & Wilkins Inc; 2001: 1403–34.
Agarwal A, Bose N, Gaur A, Singh U, Gupta MK, Singh D. Acupressure and ondansetron for postoperative nausea and vomiting after laparoscopic cholecystectomy. Can J Anesth 2002; 49:554–60.
Lee Y, Lin YS, Chen YH. The effect of dexamethasone upon patient-controlled analgesia-related nausea and vomiting. Anaesthesia 2002; 57:705–9.
Rajeeva V, Bhardwaj N, Batra YK, Dhaliwal LK. Comparison of ondansetron with ondansetron and dexamethasone in prevention of PONV in diagnostic laparoscopy. Can J Anesth 1999; 46:40–4.
Wu CL, Naqibuddin M, Rowlingson AJ, Lietman SA, Jermyn RM, Fleisher LA. The effect of pain on health- related quality of life in the immediate postoperative period. Anesth Analg 2003; 97:1078–85.
Apfel CC, Laara E, Koivuranta M, Greim CA, Roewer N. A simplified risk score for predicting postoperative nausea and vomiting: conclusions from cross-validations between two centers. Anesthesiology 1999; 91:693–700.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thomas, S., Beevi, S. Dexamethasone reduces the severity of postoperative sore throat. Can J Anesth 54, 897–901 (2007). https://doi.org/10.1007/BF03026793
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03026793