Abstract
Purpose: The standard laryngeal mask airway LMA-Classic was designed as an alternative to the endotracheal tube (ETT) or the face mask for use with either spontaneous or positive pressure ventilation. Positive pressure ventilation may exploit leaks around the LMA cuff, leading to gastric distension and/or inadequate ventilation. We compared gastric distension and ventilation parameters with LMAvs ETT during laparoscopic cholecystectomy.
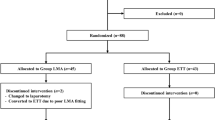
Methods: One hundred and one, ASA 1–11 adults scheduled for elective laparoscopic cholecystectomy were randomly assigned to LMA-Classic or ETT. Patients with BMI >30 kg·m−2, hiatus hernia or gastroesophageal reflux were excluded. Following induction of anesthesia, an in-and-out orogastric tube was passed to decompress the stomach before insertion of the LMA (women size #4, men size #5) or ETT (women 7 mm, men 8 mm). Anesthesia was maintained with isoflurane in nitrous oxide and oxygen (FIO2 0.3–0.5), rocuronium and fentanyl. The surgeon, blinded to the type of airway, scored gastric distention 0–10 at insertion of the laparoscope and immediately before removal at the end of the surgical procedure.
Results: Incidence and degree of change in gastric distension were similar in both groups. Ventilation parameters during insufflation (mean±Sd) for LMA and ETT were: SpO2 98±1vs 98±1, PETCO2 38±4vs 36±4 mm Hg and airway pressure 21±4vs 23±3 cm water.
Conclusion: Positive pressure ventilation with a correctly placed LMA-Classic of appropriate size permits adequate pulmonary ventilation. Gastric distension occurs with equal frequency with either airway device.
Résumé
Objectif: Le masque laryngé classique (ML) a été conçu comme une solution de remplacement au tube endotrachéal (TET) ou au masque lors de ventilation à pression positive ou de ventilation spontanée. La ventilation à pression positive accentue les fuites autour du ballonnet du ML. Nous avons comparé la distension gastrique et les paramètres de la ventilation avec le MLvs le TET pendant la cholécystectomie laparoscopique.
Méthode: Cent un patients d’état physique ASA 1–11, dont la cholécystectomie laparoscopique avait été planifiée, ont été répartis au hasard en deux groupes: ML et TET. Les patients dont l’IMC était >30kg·m−2, ou qui présentaient une hernie hiatale ou du reflux gastro-œsophagien ont été exclus de l’étude. Après l’induction de l’anesthésie, un cathéter orogastrique (placé et enlevé) a été introduit pour décompresser l’estomac avant l’insertion du ML (modèle 4 pour les femmes, 5 pour les hommes) ou un TET (7 mm pour les femmes, 8 mm pour les hommes). L’anesthésie a été maintenue avec de l’isoflurane dans un mélange de protoxyde l’azote et d’oxygène (FIO2 0,3–0,5), du rocuronium et du fentanyl. Le chirurgien, qui ne connaît pas le type de canule utilisée, a coté la distension gastrique de 0 à 10 à l’insertion du laparoscope et immédiatement avant son retrait à la fin de l’intervention chirurgicale.
Résultats: L’incidence et le degré de changement de distension gastrique ont été similaires dans les deux groupes. Les paramètres de ventilation notés pendant l’insufflation (moyenne±écart type) pour le ML et le TET ont été de: SpO2 98±1vs 98±1, PETCO238±4vs 36±4 mm Hg et la pression des voies aériennes de 21 ±4vs 23±3 cm d’eau.
Conclusion: La ventilation à pression positive avec un ML bien placé et de grandeur appropriée permet une ventilation pulmonaire adéquate. La distension gastrique survient selon la même fréquence avec le ML ou le TET.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Freedman B. Equipoise and the ethics of clinical research. N Eng J Med 1987; 317: 141–5.
Brain AIJ. The laryngeal mask — a new concept in airway management. Br J Anaesth 1983; 55: 801–5.
Malins AF, Cooper GM. Laparoscopy and the laryngeal mask airway (Letter). Br J Anaesth 1994; 73: 121.
Verghese C, Brimacombe JR. Survey of laryngeal mask airway usage in 11,910 patients: safety and efficacy for conventional and nonconventional usage. Anesth Analg 1996; 82: 129–33.
Bapat PP, Verghese C. Laryngeal mask airway and the incidence of regurgitation during gynecological laparoscopies. Anesth Analg 1997; 85: 139–43.
Swann DG, Spens H, Edwards SA, Chestnut RJ. Anaesthesia for gynaecological laparoscopy — a comparison between the laryngeal mask airway and tracheal intubation. Anaesthesia 1993; 48: 431–4.
Buniatian AA, Dolbneva EL. Laryngeal mask under total myoplegia and artificial pulmonary ventilation during laparoscopic cholecystectomies. (Russian) Vestn Ross Akad Med Nauk 1997; 9: 33–8.
Weiler N, Latorre F, Eberle B, Goedecke R, Heinrichs W. Respiratory mechanics, gastric insufflation pressure, and air leakage of the laryngeal mask airway. Anesth Analg 1997; 84: 1025–8.
Latorre F, Eberle B, Weiler N, et al. Laryngeal mask airway position and the risk of gastric insufflation. Anesth Analg 1998; 86: 867–71.
Ho-Tai LM, Devitt JH, Noel AG, P’Donnell, MP. Gas leak and gastric insufflation during controlled ventilation: face maskversus laryngeal mask airway. Can J Anaesth 1998, 45: 206–11.
Devitt JH, Wenstone R, Noel AG, O’Donnell MP. The laryngeal mask airway and positive-pressure ventilation. Anesthesiology 1994; 80: 550–5.
Brain AIJ. The Laryngeal Mask Airway (LMA) Instruction Manual. Intavent Research Limited 1995: 39.
Joshi S, Sciacca RR, Solanki DR, Young WL, Mathru MM. A prospective evaluation of clinical tests for placement of laryngeal mask airways. Anesthesiology 1998; 89: 1141–6.
Brimacombe JR, Brain AIJ, Berry AM, Verghese C, Ferson D. Gastric insufflation and the laryngeal mask (Letter). Anesth Analg 1998; 86: 914–20.
Brimacombe JR Positive pressure ventilation with the size 5 laryngeal mask. J Clin Anesth 1997; 9: 113–7.
Doyle MT, Twomey CF, Owens TM, McShane AJ. Gastroesophageal reflux and tracheal contamination during laparoscopic cholecystectomy and diagnostic gynecological laparoscopy. Anesth Analg 1998; 86: 624–8.
Lind JF, Warrian WG, Wankling WJ. Responses of the gastroesophageal junctional zone to increases in abdominal pressure. Can J Surg 1966; 9: 32–8.
Jones MJ, Mitchell RW, Hindocha N. Effect of increased intra-abdominal pressure during laparoscopy on the lower esophageal sphincter. Anesth Analg 1989; 68: 63–5.
Brimacombe JR, Berry A. The incidence of aspiration associated with the laryngeal mask airway: a meta-analysis of published literature. J Clin Anesth 1995; 7: 297–305.
Warner MA, Warner ME, Weber JG. Clinical significance of pulmonary aspiration during the perioperative period. Anesthesiology 1993; 78: 56–62.
Benumof J. Laryngeal mask airway. Indications and contraindications (Editorial). Anesthesiology 1992; 77: 843–6.
Crosby ET, Cooper RM, Douglas MJ, et al. The unanticipated difficult airway with recommendations for management. Can J Anaesth 1998; 45: 757–76.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maltby, J.R., Beriault, M.T., Watson, N.C. et al. Gastric distension and ventilation during laparoscopic cholecystectomy: LMA-classic vs. tracheal intubation. Can J Anaesth 47, 622–626 (2000). https://doi.org/10.1007/BF03018993
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018993