Abstract
Purpose: To compare postoperative gastrointestinal recovery between continuous epidural bupivacaine-fentanyl and bupivacaine-morphine.
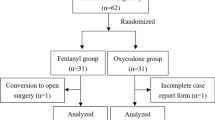
Methods: In a blinded, randomized, prospective trial, 60 women undergoing surgery for gynecologic cancer were studied. Anesthesia was provided by a combined general/epidural (L2–3 catheter) technique without epidural opioids. Postoperative epidural analgesia was by continuous infusion of bupivacaine 0.1% with either morphine 0.05 mg·ml−1 (BM) or fentanyl 5 µg·ml−1 (BF). Visual Analogue Scale (VAS) scores for pain at rest and during movement, and the return of bowel function were collected for three days and the duration of hospitalization were noted.
Results: On POD-1, 18.5% of patients in the BM group had emesis compared with none in the BF group (P=0.038) and fewer patients in the BM group tolerated clear oral fluids (11.1% BM vs 40.6% BF,P=0.025). These differences became insignificant on POD-2 and 3. Median pain scores were comparable at rest and ranged from 10–20 in the BM group vs 0–20 in the BF group over the three days. Similarly, median pain scores with movement respectively ranged from 20–25 and 20–30 in the BF and BM groups. The mean duration of hospitalization was longer in the BM group (5.7±2.4) vs BF (4.5±1.2 days),P=0.017.
Conclusion: Epidural BM and BF provided equally effective postoperative analgesia at rest and during movement. Compared with BM, epidural BF is associated with less emesis and an increased ability to tolerate oral fluids on POD-I and an overall shorter hospital stay.
Résumé
Objectif: Comparer la récupération gastro-intestinale postopératoire à la suite d’une perfusion péridurale continue avec bupivacaïne et, fentanyl ou morphine.
Méthode: L’étude à l’insu, randomisée et prospective a porté sur 60 femmes qui ont subi l’opération d’un cancer gynécologique. Une technique générale/péridurale combinée (cathéter dans l’espace L2–3) sans opioïdes périduraux a permis l’anesthésie. L’analgésie péridurale postopératoire comprenait une perfusion continue de bupivacaïne à 0,1 % avec, soit 0,05mg·ml−1 de morphine (BM), soit 5µg·ml−1 de fentanyl (BF). On a enregistré pendant 3 jrs les scores de douleur au repos et pendant le mouvement à l’échelle visuelle analogique (EVA), et le retour de la fonction intestinale. La durée de l’hospitalisation a été notée.
Résultats: Au jour I postopératoire, 18,5 % des patientes du groupe BM avaient des vomissements mais aucune du groupe BF (P=0,038) et peu de patientes du groupe BM ont toléré les liquides oraux clairs (11,1 % BM vs 40,6 % BF,P=0,025). Ces différences n’étaient plus significatives aux jours 2 et 3. Les scores moyens de douleur ont été comparables au repos et allaient de 10–20 pour le groupe BMvs 0–20 pour le groupe BF au cours des trois jours. De même, les scores moyens de douleur au mouvement se retrouvaient respectivement de 20–25 et de 20–30 pour les groupes BF et BM. La durée moyenne d’hospitalisation a été plus longue dans le groupe BM (5,7±2,4) vs le groupe BF (4,5±1,2 jours),P=0,017.
Conclusion: L’analgésie péridurale BM et l’analgésie BF ont fourni un soulagement équivalent de la douleur postopératoire au repos et lors de mouvements. L’analgésie avec BF, comparée à l’analgésie avec BM, est associée à moins de vomissement et à une capacité accrue de tolérance aux liquides oraux le premier jour postopératoire ainsi qu’à un séjour hospitalier plus court.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Liu SS, Carpenter RL, Mackey DC, et al. Effects of perioperative analgesic technique on rate of recovery after colon surgery. Anesthesiology 1995; 83: 757–65.
Thorén T, Sundberg A, Wattwil M, Garvill J-E, Jürgensen U. Effects of epidural bupivacaine and epidural morphine on bowel function and pain after hysterectomy. Acta Anaesthesiol Scand 1989; 33: 181–5.
Thorén T, Tanghöj H, Wattwill M, Järnerot G Epidural morphine delays gastric emptying and small intestinal transit in volunteers. Acta Anaesthesiol Scand 1989; 33: 174–80.
Cousins MJ, Mather LE. Intrathecal and epidural administration of opioids. Anesthesiology 1984; 61: 276–310.
Glantz SA. Primer of Biostatistics, 4th ed. New York: McGraw-Hill, 1997.
Berti M, Fanelli G, Casati A, Lugani D, Aldegheri G, Torri G. Comparison between epidural infusion of fentanyl/bupivacaine and morphine/bupivacaine after orthopaedic surgery. Can J Anaesth 1998; 45: 545–50.
Saito Y, Uchida H, Kaneko M, Nakatani M, Kosaka Y. Comparison of continuous epidural infusion of morphine/bupivacaine with fentanyl/bupivacaine for post-operative pain relief. Acta Anaesthesiol Scand 1994; 38: 398–401.
Fischer RL, Lubenow TR, Liceaga A, McCarthy RJ, Ivankovich AD. Comparison of continuous epidural infusion of fentanyl-bupivaciane and morphine bupivacaine in management of postoperative pain. Anesth Analg 1988; 67: 559–63.
Steinbrook RA. Epidural anesthesia and gastrointestinal motility. Anesth Analg 1998; 86: 837–44.
Scott AM, Starling JR, Ruscher AE, DeLessio ST, Harms BA. Thoracic versus lumbar epidural anesthesia’s effect on pain control and ileus resolution after restorative proctocolectomy. Surgery 1996; 120: 688–97.
Mc Fadden DW, Zinner MJ. Manifestations of gastrointestinal disease.In: Schwartz SS (Ed.). Principles of Surgery, 6th ed. New York: McGraw-Hill, 1994: 1031.
Shihata Y, Nimura Y, Yasui A, Miyachi M, Shimada Y. The effect of epidural morphine on human intestinal motility in the early postoperative period. Hepato-Gastroenterol 1994; 41: 559–63.
Jaffe JH, Martin WR. Opioid analgesics and antagonistsIn: Gilman AG, Rall TW, Nies AS, Taylor P (Eds.). Goodman and Gilman’s, The Pharmacological Basis of Therapeutics, 8th ed. Elmsford, NY: Pergamon Press, 1990: 485–508.
Massi P, Giagnoni G, Basilico L, Gori E, Rubino T, Parolaro D Intestinal effect of morphine 6-glucuronide: in vivo and in vitro characterization. Eur J Pharmacol 1994; 253: 269–74.
Thörn S-E, Wattwil M, Lindberg G, Säwe J. Systemic and central effects of morphine on gastroduodenal motility. Acta Anaesthesiol Scand 1996; 40: 177–186.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vallejo, M.C., Edwards, R.P., Shannon, K.T. et al. Improved bowel function after gynecological surgery with epidural bupivacaine-fentanyl than bupivacaine-morphine infusion. Can J Anaesth 47, 406–411 (2000). https://doi.org/10.1007/BF03018968
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03018968