Abstract
Purpose
To assess the ease of insertion of laryngeal mask airway (LMA) comparing propofol with lidocaine or midazolam followed by thiopentone and compare the costs with each technique.
Methods
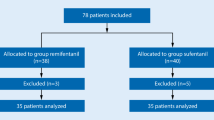
One hundred and fifty ASA 1 or 2 patients equally divided into three groups scheduled for elective surgery were recruited into this prospective, single blind, randomized, parallel groups study. Anaesthetic induction was achieved with 1 μg · kg−1 fentanyl iv followed by either 2.5 mg · kg−1 propofol (group P), or a sequence of 1.5 mg · kg−1 lidocaine and 5 mg· kg−1 thiopentone (group LT), or midazolam 0.1 mg· kg−1 and, three minutes later, 5 mg· kg−1 thiopentone (group MT). The LMA was inserted by the blinded anaesthetist who assessed and graded the conditions for LMA insertion and noted any adverse responses (i.e., inadequate jaw relaxation, gagging, coughing, limb or head movement, hiccough and laryngospasm). Conditions were considered “excellent” if there were no adverse responses, and “satisfactory” if such a response was mild and transient.
Results
Excellent or satisfactory conditions were observed in 48 (96%) patients in the midazolam-thiopentone group, 46 (92%) in the propofol group, and 34 (68%) in the lidocaine-thiopentone group (P = 0.0001). The incidence of gagging (P = 0.042), limb movement (P = 0.031), and laryngospasm (P = 0.0001) was higher in the lidocaine-thiopentone group.
Conclusions
With the above doses, a fentanyl-midazolam-thiopentone combination which is about 35% less expensive than fentanyl-propofol, provides equally good conditions for the insertion of LMA.
Résumé
Objectif
Évaluer la facilité d’insertion du masque laryngé (ML) en comparant le propofol avec l’association lidocaïne ou midazolam-thiopentone et les coûts entraînés par chacune des techniques.
Méthodes
Cent cinquante patients ASA 1 et 2 répartis également en trois groupes, programmés pour une chirurgie non urgente étaient admis dans cette étude prospective, à l’aveugle, aléatoire et en groupes parallèles. L’induction était réalisée avec fentanyl 1 μg · kg−1 iv suivi soit par du propofol 2,5 mg· kg−1 (groupe P), ou une séquence de lidocaïne 1,5 mg · kg−1 et thiopentone 5 mg kg−1 (groupe LT), ou midazolam 0,1 mg· kg−1 (groupe MT) suivis trois minutes plus tard de thiopentone 5 mg · kg−1. Le ML était inséré par un anesthésiste neutre qui évaluait et classait les conditions d’insertion du ML, et notait toute condition défavorable (c. à d., relaxation de la mâchoire insuffisante, réflexe nauséeux, toux, mouvement de la tête ou des membres, hoquet ou spasme laryngé). Les conditions étaient considérées comme excellentes si aucune réaction défavorable n ’était constatée, et satisfaisante, si la réaction n’était que légère ou transitoire.
Résultats
On a constaté des conditions excellentes ou satisfaisante chez 48 (96%) des patients du groupe midazolamthiopentone, chez 46 (92%) du groupe propofol et 34 (68%) du groupe lidocaine-thiopentone (P = 0,0001). L’incidence de réflexes nauséeux (P = 0,042), mouvements des membres (P = 0,031) et de spasme laryngé (P= 0,0001) était plus élevée dans le groupe lidocaïne-thiopentone.
Conclusions
Aux doses mentionnées, la combinaison fentanyl-thiopentone procure d’aussi bonnes conditions pour l’insertion du ML que la combinaison fentanyl-propofol et coûte environ 35% moins cher.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Brain AIJ. The laryngeal mask — a new concept in airway management. Br J Anaesth 1983; 55: 801–5.
Brain AIJ. The Intavent Laryngeal Mask Instruction Manual, 2nd ed. Henley on Thames: Intavent, 1993; 7.
Brown GW, Patel N, Ellis FR. Comparison of propofol and thiopentone for laryngeal mask insertion. Anaesthesia 1991; 46: 771–2.
Scanlon P, Carey M, Power M, Kirby F. Patient response to laryngeal mask insertion after induction of anaesthesia with propofol or thiopentone. Can J Anaesth 1993; 40: 816–8.
Brimacombe J, Berry A. Insertion of LMA — an indication for propofol? Anaesth Intensive Care 1992; 20: 394–5.
McKeating K, Bali IM, Dundee JW. The effects of thiopentone and propofol on upper airway integrity. Anaesthesia 1988; 43: 638–40.
Wilson IG, Fell D, Robinson SL, Smith G. Cardiovascular responses to insertion of the laryngeal mask. Anaesthesia 1992; 47: 300–2.
Poulton TJ, James FM III. Cough suppression by lidocaine. Anesthesiology 1979; 50: 470–2.
Steinhaus JE, Gaskin L. A study of intravenous lidocaine as a suppressant of cough reflex. Anesthesiology 1963, 24; 285–90.
Abou-Madi MN, Keszler H, Yacoub JM. Cardiovascular reactions to laryngoscopy and tracheal intubation following small and large intravenous doses of lidocaine. Can Anaesth Soc J 1977; 24: 12–9.
Hamill JF, Bedford RF, Weaver DC, Colohon AR. Lidocaine before endotracheal intubation: intravenous or laryngotracheal? Anesthesiology 1981; 55: 578–81.
Stoneham MD, Bree SE, Sneyd JR. Facilitation of laryngeal mask insertion. Effects of lignocaine given intravenously before induction with propofol. Anaesthesia 1995; 50: 464–6.
Short TG, Galletly DC, Plummer JL. Hypnotic and anaesthetic action of thiopentone and midazolam alone and in combination. Br J Anaesth 1991; 66: 13–9.
Reves JG, Fragen RJ, Vinilc HR, Greenblatt DJ. Midazolam: pharmacology and uses. Anesthesiology 1985; 62: 310–24.
Harrison GA. The influence of different anaesthetic agents on the response to respiratory tract irritation. Br J Anaesth 1962; 34: 804–11.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bapat, P., Joshi, R.N., Young, E. et al. Comparison of propofol versus thiopentone with midazolam or lidocaine to facilitate laryngeal mask insertion. Can J Anaesth 43, 564–568 (1996). https://doi.org/10.1007/BF03011767
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03011767