Abstract
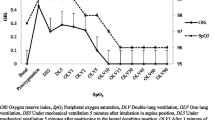
Eighty patients undergoing elective thoracotomy were studied to assess the possibility of predicting arterial oxygenation (PaO2) during one-lung anaesthesia (OLA). The first 50 patients were studied retrospectively. The method of multiple linear regression was used to construct a predictive equation for PaO2 during OLA. Potential predictors of PaO2 during OLA which were considered were: age, side of operation, preoperative pulmonary flow rates, preoperative and intraoperative PaO2 during twolung ventilation. The three most significant predictors for PaO2 during OLA were: side right of operation (P < 0.05), preoperative FEV1% (P < 0.01) and intraoperative PaO2 during two-lung ventilation (P = 0.0001). The predictive equation for PaO2 after ten minutes of OLA was: PaO2 = 100 − 72 (side) − 1.86 (FEV1%) + 0.75 (two-lung) PaO2; (for side insert 0 for left-sided thoracotomy and 1 for right-sided thoracotomy). The remaining 30 patients were studied prospectively and the predicted PaO2 correlated with the observed PaO2 after ten minutes of OLA (r = 0.73,P < 0.01). Four of 30 patients had a predicted PaO2 at ten minutes of OLA < 150 mmHg. Of these, 2/4 subsequently required abandonment of OLA for pulse oximetric saturation <85%. We conclude that although it is not possible to predict an individual patient’s PaO2 during OLA with a high degree of accuracy, it is possible, before the initiation of OLA, to identify those patients whose arterial oxygenation is likely to decrease to low levels during OLA.
Résumé
L’étude regroupant quatre-vingts patients au programme pour thoracotomie a pour objectif de déterminer la possibilité de prédire l’oxygénation artérielle (PaO2) pendant l’anesthésie monopulmonaire. Pour les 50 premiers patients l’étude est rétrospective. La méthode de régression linéaire multiple est utilisée pour construire une équation prédictive pour ta PaO2 pendant l’anesthésie monopulmonaire. Les critères retenus sont: l’âge, le côté opéré, les débits pulmonaires préopératoires, la PaO2 pré- et peropératoire pendant la ventilation bipulmonaire. Les trois paramètres les plus significatifs pour prévoir la PaO2 sous anesthésie monopulmonaire sont: les interventions sur le côté droit (P < 0,05), le VEMS préopératoire (P < 0,01) et la PaO2 peropératoire pendant l’anesthésie bipulmonaire (P = 0,0001). L’équation prédictive obtenue après dix minutes de ventilation à un poumon est exprimée ainsi: PaO2 = 100 − 72 (côté)-1,86 (VEMS) + 0,75 PaO2 (deux poumons) [pour le côté, on accorde 0 pour la thoracotomie gauche et 1 pour la thoracotomie droite]. Les trente autres patients sont étudiés de façon prospective et la PaO2 prédite correspond à la PaO2 observée après dix minutes de ventilation monopulmonaire (r = 0,73, P < 0,01). Après dix minutes de ventilation monopulmonaire, quatre des 30 patients ont une valeur prédite de PaO2 intérieure à 150 mmHg. Deceux-ci, chéz deux sur quatre, la ventilation monopulmonaire est abandonnée à cause d’une saturation puisée inférieure à 85%. Nous concluons que bien qu ’il soit impossible de prédire avec précision la PaO2 d’un patient donné pendant la ventilation à un poumon, on peut avant d’initier la ventilation monopulmonaire, identifier ceux parmi les patients dont l’oxygénation artérielle est susceptible de s’abaisser de façon importante.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Benumof J. Anesthesia for Thoracic Surgery. Philadelphia, PA, WB Saunders, 1987: 273.
Marshall B. Anesthesia for one-lung ventilation. Anesthesiology 1988; 69: 630–1.
Slinger P.Suissa S, Adam J, Triolet W. Predicting arterial oxygenation during one-lung ventilation with continuous positive airway pressure to the non-ventilated lung. Journal of Cardiothoracic Anesthesia 1990; 4: 436–40.
Knudson RJ, Lebovitz MD, Holberg CJ, Burrows L. Changes in the normal maximal expiratory flow-volume curve with growth and aging. Am Rev Respir Dis 1983: 127: 725–34.
S.A.S. Users’ Guide: Statistics Version 5. Cary, Ind, Statistical Analysis System Institute, 1985: 433.
Kerlinger FN, Pedhazure EJ. Multiple regression in behavioural research. New York, NY, Holt, 1973: 282–5.
Weinreich AI, Silvay G, Lumb PD. Continuous ketamine infusion for one-lung anaesthesia. Can Anaesth Soc J 1980; 27: 485–90.
Read RC, Friday CD, Eason CN. Prospective study of the Robertshaw endobronchial catheter in thoracic surgery. Ann Thorac Surg 1977; 24: 156–61.
Tarhan S, Lungborg RO. Effects of increased expiratory pressure on blood gas tensions and pulmonary shunting during thoracotomy with the use of the Carlens catheter. Can Anaesth Soc J 1970; 17: 4–11.
Kerr JH, Crampton Smith A, Prys-Roberts C, Meloche R, Foex P. Observations during endobronchial anaesthesia II: oxygenation. Br J Anaesth 1974; 46: 84–92.
Severinghaus JW, Naifeh KH. Accuracy of response of six pulse oximeters to profound hypoxia. Anesthesiology 1987; 67: 551–8.
Desiderio DP, Wong C, Shah NK. A clinical evaluation of pulse oximetry during thoracic surgery. Journal of Cardiothoracic Anesthesia 1990; 4: 30–4.
Katz JA, Lavern RG, Fairley HB, Thomas AN. Pulmonary oxygen exchange during endobronchial anesthesia: effects of tidal volume and PEEP. Anesthesiology 1982; 56: 164–70.
Flacke JW, Thompson DS, Read RC. Influence of tidal volume and pulmonary artery occlusion on arterial oxygenation during endobronchial anesthesia. South Med J 1976; 69: 619–26.
Larsson A, Malmkvist G, Werner O. Variations in lung volume and compliance during pulmonary surgery. Br J Anaesth 1987; 59: 585–91.
Pepe PE, Marini JJ. Occult positive end-expiratory pressure in mechanically ventilated patients with airflow obstruction. Am Rev Resp Dis 1982; 126: 166–70.
Slinger PD, Hickey DR, Lenis SG, Gottfried S. Intrinsic PEEP during one-lung ventilation. Anesth Analg 1989; 68: S269.
Benumof JL, Augustine SD, Gibbons JA. Halothane and isoflurane only slightly impair arterial oxygenation during one-lung ventilation in patients undergoing thoracotomy. Anesthesiology 1987; 67: 910–5.
Eisenkraft JB. Effects of anaesthetics on the pulmonary circulation. Br J Anaesth 1990; 65: 63–78.
Chen L, Williams JJ, Alexander CM, Ray RJ, Marshall C, Marshall BE. The effect of pleural pressure on the hypoxic pulmonary vasoconstrictor response in closed chest dogs. Anesth Analg 1988; 67: 763–9.
Hurford WE, Kolker AC, Strauss HW. The use of ventilation/perfusion scans to predict oxygenation during onelung anesthesia. Anesthesiology 1987; 67: 841–4.
Capan LM, Turndorf H, Patel C, Ramanthan S, Acinapura A, Chaton J. Optimization of arterial oxygenation during one-lung anesthesia. Anesth Analg 1980; 59: 847–51.
Speis C, Zanne U, Boden G. Different anesthetic regimens in pulmonary surgery. Anesth Analg 1991; 72: S270.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Slinger, P., Suissa, S. & Triolet, W. Predicting arterial oxygenation during one-lung anaesthesia. Can J Anaesth 39, 1030–1035 (1992). https://doi.org/10.1007/BF03008370
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03008370