Abstract
Objectives: To develop and test a scaled program evaluation questionnaire focusing on resident satisfaction with workload, learning environment, and stress.
Design/participants: Phase 1: A cross-section of 92 residents from five programs completed questionnaires for factor analysis and descriptive statistics. Phase 2: A three-year prospective study of questionnaire responses in a single program.
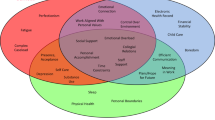
Questionnaire development: After extensive literature review, 33 Likert-scaled statements were written, dealing with situational, personal, and professional issues. After pilot testing, the 92 questionnaires obtained in Phase 1 were factor analyzed, resulting in three distinct scales: workload, faculty/learning environment, and stress.
Interventions: Program changes in Phase 2 included the introduction of a night float between 1989 and 1990, and an increase in senior resident call between 1990 and 1991.
Results: Phase 1: The first-year residents reported significantly less stress and generally greater satisfaction with workload and learning environment than did the second- or third-year residents. Marked differences between programs were also present in the mean scores on all three scales. Phase 2: The introduction of a night float did not significantly affect response to the questionnaire, but the increase in nights on call significantly increased stress and dissatisfaction with the faculty/learning environment.
Conclusions: This study demonstrates the techniques needed to develop and use scaled program evaluation questionnaires. It is hoped that widespread use and validation of such instruments may result in greater responsiveness to the needs of trainees and more facilitative environments in which to acquire medical knowledge.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Swanson AG. Medical students’ specialty choices. In: Harris DL. Reform in Medical Education and Medical Education in the Ambulatory Setting. Washington, DC: US Dept of Health and Human Services, 1991;35–9.
Schwartz MD, Linzer M, Babbott D, et al. Medical Student Interest in Internal Medicine. Initial Report of the Society of General Internal Medicine Interest Group Survey on Factors Influencing Career Choice in Internal Medicine. Ann Intern Med. 1991;114:6–15.
Babbott D, Levey GS, Weaver SO, Killian CD. Medical student attitudes about internal medicine: a study of U.S. medical school seniors in 1988. Ann Intern Med. 1991;114:16–22.
Reitemeier RJ. The leadership crisis in internal medicine: what can be done? Ann Intern Med. 1991;114:69–75.
Lewis CE, Prout DM, Chalmers EP, Leake B: How satisfying is the practice of internal medicine? A national survey. Ann Intern Med. 1991;114:1–5.
Lipkin M, Levinson W, Barker R, et al. Primary care internal medicine: a challenging career choice for the 1990’s. Ann Intern Med. 1990;112:371–8.
Uliana RL, Hubbell FA, Wyle FA, Gordon GH. Mood changes during the internship. J Med Educ. 1984;59:118–23.
Gordon GH, Hubbell FA, Wyle FA, Charter RA. Stress during internship: a prospective study of mood states. J Gen Intern Med. 1986;1:228–31.
Girard DE, Elliot DL, Hickam DH, et al. The internship—a prospective investigation of emotions and attitudes. West J Med. 1986;144:93–8.
Girard DE, Sack RL, Reuler JB, Chang MK, Nardone DA. Survival of the medical internship. Forum Med. 1980;3:460–3.
Zeigler JL, Strull WM, Larsen RC, et al. Stress and medical training. West J Med. 1985;142:814–9.
Rudner HL. Stress and coping mechanisms in a group of family practice residents. J Med Educ. 1985;60:564–6.
Alexander D, Monk JS, Jonas AP. Occupational stress, personal strain, and coping among residents and faculty members. J Med Educ. 1985;60:830–9.
Smith JW, Denny WF, Witzke DB. Emotional impairment in internal medicine house staff. JAMA. 1096;255:1155–8.
Reuben DB. Psychologic effects of residency. South Med J. 1983;76:380–3.
Reuben DB. Depressive symptoms in medical house officers. Arch Intern Med. 1985;145:286–8.
Samuel SE, Lawrence JS, Schwartz HJ, Weiss JC, Setzer JL. Investigating stress levels of residents: a pilot study. Med Teacher. 1991;13:89–92.
Badger LW, Chesebro MJ, Hartman JA. First year residency stress: sources and mediators. Fam Pract Res J. 1987;7:104–13.
Walerstein SJ, Rosner F, Wallace EZ. House staff stress. N Y State J Med. 1989;89:454–7.
Schwartz AJ, Black ER, Goldstein MG, Jozefowicz RF, Emmings FG. Levels and causes of stress among residents. J Med Educ. 1987;62:744–53.
Whitley TW, Gallery ME, Allison EJ Jr, Revicki DA. Factors associated with stress among emergency medicine residents. Ann Emerg Med. 198;18:1157–61.
Ditts PV Jr, Dilts SL. Stress in residency: proposals for solution. Am J Obstet Gynecol. 1987;157:1093–6.
McCue JD. The distress of internship, causes and prevention. N Engl J Med. 1985;312:449–52.
Matheson KH. Stress and stress counselling. Postgrad Med J. 1990;66:738–42.
Levin R. Beyond “The Men of Steel”: the origins and significance of house staff training stress. Gen Hosp Psychiatry. 1988;10:114–21.
Resident Services Committee, Association of Program Directors in Internal Medicine. Stress and impairment during residency training: strategies for reduction, identification, and management. Ann Intern Med. 1988;109:154–61.
Colford JM Jr, McPhee SJ: The ravelled sleeve of care: managing the stresses of residency training. JAMA. 1989;261:889–93.
Butterfield PS. The stress of residency: a review of the literature. Arch Intern Med. 1988;148:1428–35.
Martin AR: Stress in residency: a challenge to personal growth. J Gen Intern Med. 1986;1:252–7.
McCue JD, Sachs CL. A stress management workshop improves residents’ coping skills. Arch Intern Med. 1991;151:2273–7.
McCall TB. The impact of long working hours on resident physicians. N Engl J Med. 1988;318:775–8.
Alpert JS, Coles R. Residency reform: an urgent necessity. Arch Intern Med. 1988;148:1507–8.
Giardino AP, Giardino ER. Medical education and resident work hours. JAMA. 1990;263:620.
Resident Physician Section: American Medical Association Board acts to limit resident work hours. JAMA. 1989;262:2970.
Trontell MC, Carson JL, Taragin MI, Duff A. The impact of the night float system on internal medicine residency programs. J Gen Intern Med. 1991;6:445–9.
Accreditation Council for Graduate Medical Education. Directory of Graduate Medical Education Programs. Chicago, IL: American Medical Association, 199;9–47.
DeVellis RF. Guidelines in scale development. In: Scale Development: Theory and Applications. Newbury Park, CA: Sage Publications, 1991;51–90.
Comrey AL. Common methodological problems in factor analytic studies. J Consult Clin Psychol 1978;46:648–59.
SAS 6.04. Cary, NC: SAS Institute, Inc., 1987.
Author information
Authors and Affiliations
Additional information
Received from the University of North Carolina, Chapel Hill, and the Internal Medicine Residency Training Program, New Hanover Regional Medical Center, Wilmington, North Carolina.
Rights and permissions
About this article
Cite this article
Seel1C, C.B. Quantitating qualitative issues in residency training. J Gen Intern Med 8, 610–613 (1993). https://doi.org/10.1007/BF02599716
Issue Date:
DOI: https://doi.org/10.1007/BF02599716