Abstract
Background: The routine use of drainage after axillary node dissection in patients undergoing breast-conserving therapy (BCT) is being questioned. To determine the value of routine drainage, we evaluated the postoperative course of patients with primary breast carcinoma who underwent axillary dissection with or without axillary drainage.
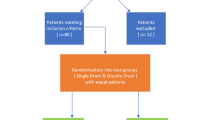
Methods: A retrospective review of 69 patients prompted a prospective randomized trial of 46 patients undergoing BCT at our tertiary cancer center. Variables studied were age, treatment (drain or no drain), number and tumor status of excised lymph nodes, size of primary tumor, duration of drainage or aspiration, number and volume of aspirations, number of office visits, incidence of complications and degree of pain, change in arm or forearm circumference, and body mass index (BMI). Data from prospective and retrospective studies were pooled for analysis.
Results: Of 115 patients, 72 were treated with a drain (Drain group) and 43 were not (No-drain group). Overall there was no difference in the number or tumor status of excised nodes, the size of the primary tumor, or the incidence of complications between the two groups. Aspiration was required in 50% of the No-drain patients and 8.3% of the Drain patients. The incidence of drain placement or replacement postoperatively was 9.3% for the No-drain patients and 4.2% for the Drain patients. The No-drain patients had more office visits (5.1±0.4 vs. 3.6±0.1;P=.0002) and a longer interval between operation and last aspiration or drain removal (16.2±1.4 days vs. 11.3±0.6 days;P=.0040). Findings were similar in the subgroup of 46 prospectively studied patients, who included 24 Drain patients and 22 No-drain patients. In this group, pain evaluation using a scale of 0 to 10 showed a mean rating of 4.2±2.6 in Drain patients and 2.7±0.4 in No-drain patients (P=.0062).
Conclusions: Axillary node dissection can be managed with or without a drain. More office visits but less pain can be expected if a drain is not used.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Fisher B, Anderson S, Redmond CK, Wolmark N, Wickerham DL, Cronin WM. Reanalysis and results after 12 years of follow-up in a randomized clinical trial comparing total mastectomy with lumpectomy with or without irradiation in the treatment of breast cancer.N Engl J Med 1995;333:1456–61.
Vinton AL, Traverso LW, Jolly PC. Wound complications after modified radical mastectomy compared with tylectomy with axillary lymph node dissection.Am J Surg 1991;161:584–8.
Tadych K, Donegan WL. Postmastectomy seromas and wound drainage.Surg Gynecol Obstet 1987;165:483–7.
Jeffrey SS, Goodson WH, Ikeda DM, Birdwell RL, Bogetz MS. Axillary lymphadenectomy for breast cancer without axillary drainage.Arch Surg 1995;130:909–13.
Siegel BM, Mayzel KA, Love SM. Level I and II axillary dissection in the treatment of early-stage breast cancer.Arch Surg 1990;125:1144–7.
Petrek JA, Peters MM, Nori S, Knauer C, Kinne DW, Rogatko A. Axillary lymphadenectomy.Arch Surg 1990;125:378–82.
Somers RG, Jablon LK, Kaplan MJ, Sanders GL, Rosenblatt NK. The use of closed suction drainage after lumpectomy and node dissection for breast cancer.Ann Surg 1992;21:146–9.
Petrek JA, Peters MM, Cirrincione C, Thaler HT. A prospective randomized trial of single versus multiple drains in the axilla after lymphadenectomy.Surg Gynecol Obstet 1992;175:405–9.
Jansen RFM, Van Geel AN, De Groot HGW, Rottier AB, Olthuis GAA, Van Putten WLJ. Immediate versus delayed shoulder exercises after axillary lymph node dissection.Am J Surg 1990;160:481–4.
Author information
Authors and Affiliations
Additional information
The views expressed herein are those of the authors and do not necessarily reflect the views of the United States Army, United States Navy, Uniformed Services University of the Health Sciences, or the Department of Defense.
Rights and permissions
About this article
Cite this article
Zavotsky, J., Jones, R.C., Brennan, M.B. et al. Evaluation of axillary lymphadenectomy without axillary drainage for patients undergoing breast-conserving therapy. Annals of Surgical Oncology 5, 227–231 (1998). https://doi.org/10.1007/BF02303777
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02303777