Abstract
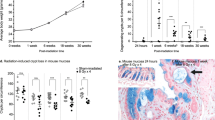
PURPOSE: Irradiation inflicts acute injuries to the intestinal mucosa with rapid apoptosis induction and subsequent reduction in epithelial surface area. It may therefore be assumed that the intestinal barrier function is affected. The aim of this study was to compare the mucosal permeability in irradiated rectum and nonirradiated sigmoid colon from patients subjected to radiation therapy before surgical treatment for rectal cancer. METHODS: Segments from sigmoid colon and rectum obtained from irradiated and nonirradiated patients were stripped from the serosa-muscle layer and mounted in Ussing diffusion chambers. The mucosa-to-serosa passage of the marker molecules14C-mannitol, fluorescein isothiocyanate-dextran 4,400, and ovalbumin was followed for 120 minutes. RESULTS: The permeability to the markers was size-dependent and increased linearly across time in all specimens. The passage of all markers was increased in irradiated rectum compared with nonirradiated sigmoid colon, whereas in specimens from nonirradiated patients there were no differences between rectum and sigmoid colon. Histologic signs of crypt and mucosal atrophy were found in the irradiated rectal specimens. CONCLUSIONS: Early gastrointestinal complications after radiation therapy may be the result of mucosal atrophy in addition to mucosal damage, with a loss of barrier integrity.
Similar content being viewed by others
References
Tobias JS. Clinical practice of radiotherapy. Lancet 1992;339:159–63.
Lichter AS, Lawrence TS. Recent advances in radiation oncology. N Engl J Med 1995;332:371–9.
Påhlman L, Glimelius B. The value of adjuvant radio(chemo)therapy for rectal cancer. Eur J Cancer 1995;31A:1347–50.
Lise M, Gerard A, Nitti D,et al. Adjuvant therapy for colorectal cancer: the EORTC experience and a review of the literature. Dis Colon Rectum 1987;30:847–54.
Swedish Rectal Cancer Trial. Improved survival with preoperative radiotherapy in resectable rectal cancer. N Engl J Med 1997;336:980–7.
Bloomer WD, Hellman S. Normal tissue responses to radiation therapy. N Engl J Med 1975;293:80–3.
Galland RB, Spencer J. The natural history of clinically established radiation enteritis. Lancet 1985;1:1257–8.
Galland RB, Spencer J. Surgical aspects of radiation injury to the intestine. Br J Surg 1979;66:135–8.
DeCosse JJ, Rhodes RS, Wentz WB, Reagan JW, Dworken HJ, Holden WD. The natural history and management of radiation induced injury of the gastrointestinal tract. Ann Surg 1969;170:369–84.
Nussbaum ML, Campana TJ, Weese JL. Radiation-induced intestinal injury. Clin Plast Surg 1993;20:573–80.
Potten CS, Booth C. The role of radiation-induced and spontaneous apoptosis in the homeostasis of the gastrointestinal epithelium: a brief review. Comp Biochem Physiol 1997;118B:473–8.
Porvaznik M. Tight junction disruption and recovery after sublethal γ irradiation. Radiat Res 1979;78:233–50.
Buell MG, Harding RK. Proinflammatory effects of local abdominal irradiation on rat gastrointestinal tract. Dig Dis Sci 1989;34:390–9.
Followill DS, Kester D, Travis EL. Histological changes in mouse colon after single- and split-dose irradiation. Radiat Res 1993;136:280–8.
Herrera JL, Vigneulle RM, Gage T, MacVittie TJ, Nold JB, Dubois A. Effect of radiation and radioprotection on small intestinal function in canines. Dig Dis Sci 1995;40:211–8.
Dublineau I, Ksas B, Aigueperse J, Gourmelon P, Griffiths NM. In vivo alterations of fluid and electrolyte fluxes in rat colon by gamma irradiation. Dig Dis Sci 1998;43:652–62.
Brady ME, Hayton WL. GI drug absorption in rats exposed to cobalt-60 γ-radiation II: in vivo rate of absorption. J Pharm Sci 1977;66:366–70.
Baer AR, Cheeseman CI, Thomson AB. The assessment of recovery of the intestine after acute radiation injury. Radiat Res 1987;109:319–29.
Coltart RS, Howard GC, Wraight EP, Bleehen NM. The effect of hyperthermia and radiation on small bowel permeability using51Cr-EDTA and14C mannitol in man. Int J Hyperthermia 1998;5:467–77.
Carratu R, Secondulfo M, de Magistris L,et al. Assessment of small intestinal damage in patients treated with pelvic radiotherapy. Oncol Rep 1998;3:635–9.
Jörgensen LN, Kallehave F, Karlsmark T, Gottrup F. Reduced collagen accumulation after major surgery. Br J Surg 1996;83:1591–94.
Pantzar N, Ekström GM, Wang Q, Weström BR. Mechanisms of increased intestinal51Cr-EDTA absorption during experimental colitis in the rat. Dig Dis Sci 1994;39:2327–33.
Grass GM, Sweetana SA. In vitro measurement of gastrointestinal tissue permeability using a new diffusion cell. Pharm Res 1988;5:372–6.
Laurell CB. Electroimmunoassay. Scand J Clin Lab Invest 1972;29:21–37.
Hopewell JW, Calvo W, Jaenke R, Reinhold HS, Robbins ME, Whitehouse EM. Microvasculature and radiation damage. Recent results. Cancer Res 1993;130:1–16.
Langberg CW, Waldron JA, Baker ML, Hauser-Jensen M. Significance of overall treatment time for the development of radiation-induced intestinal complications. Cancer 1994;73:2663–8.
Earnest DL, Trier JS. Radiation enteritis and colitis. In: Sleisenger MH, Fordtran JS, eds. Gastrointestinal disease. Philadelphia: WB Saunders, 1989:1369–82.
Pantzar N. Characteristics of intestinal permeability to different-sized molecules in the rat. Thesis: Department of Animal Physiology, Lund University. 1995.
Nejdfors P, Wang Q, Ekelund M,et al. Increased colonic permeability in patients with ulcerative colitis: an in vitro study. Scand J Gastroenterol 1998;33:749–53.
Walker RI, Ledney GD, Galley CB. Aseptic endotoxemia in radiation injury and graft-vs-host disease. Radiat Res 1975;62:242–9.
Author information
Authors and Affiliations
Additional information
Supported by grants from the Anna-Greta Crafoord Foundation, Lund; Lisa and Johan Grönberg's Foundation, Stockholm; the Swedish Cancer Research Foundation (3966-B97-01XAB); and the Dir Albert Påhlsson Foundation, Malmö, Sweden.
About this article
Cite this article
Nejdfors, P., Ekelund, M., Weström, B.R. et al. Intestinal permeability in humans is increased after radiation therapy. Dis Colon Rectum 43, 1582–1587 (2000). https://doi.org/10.1007/BF02236743
Issue Date:
DOI: https://doi.org/10.1007/BF02236743