Abstract
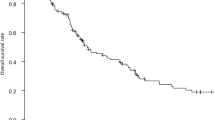
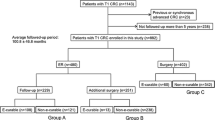
PURPOSE: The aim of this study was to determine the long-term outcome after curative resection of colorectal cancers that extend only into the submucosa (“minimally invasive”) and to evaluate potential histologic predictors of lymph node metastases. METHODS: Seventy-nine patients who underwent curative resection of minimally invasive colorectal cancer and were followed for at least five years were studied retrospectively. RESULTS: The series was comprised of 53 men and 26 women, with a mean age of 61 years. The lesion was in the colon in 47 patients and the rectosigmoid or rectum in 32 patients. Open surgery followed attempted endoscopic tumor removal in 25 patients. Lymph node metastasis, found in 11/79 patients (13.9 percent), was associated with worse outcome: 36.4 percent of node(+) patients developed recurrence,vs.only 5.9 percent of node(−) patients (P<0.005). The cumulative survival rate was also worse in node(+)vs.node(−) patients: 72.7 percentvs.91.1 percent at five years (P<0.05) and 45.5 percentvs.65.3 percent at ten years (P<0.05). Five histopathologic characteristics were identified as risk factors for lymph node metastasis: 1) small clusters of undifferentiated cancer cells ahead of the invasive front of the lesion (“tumor budding”); 2) a poorly demarcated invasive front; 3) moderately or poorly differentiated cancer cells in the invasive front; 4) extension of the tumor to the middle or deep submucosal layer; 5) cancer cells in lymphatics. Whereas patients with three or fewer risk factors had no nodal spread, the rate of lymph node involvement with four or more risk factors was 33.3 percent and 66.7 percent, respectively. CONCLUSIONS: Metastasis is not infrequent in “minimally invasive” colorectal cancer. Appropriate bowel resection with lymph node dissection is indicated if such a lesion exhibits more than three histologie risk factors for metastasis.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Hermanek P, Gall FP. Early (microinvasive) colorectal carcinoma-pathology, diagnosis, surgical treatment. Int J Colorectal Dis 1986;1:79–84.
Richard WO, Webb WA, Morris SJ,et al. Patient management after endoscopic removal of the cancerous colon adenoma. Ann Surg 1987;205:665–72.
Cranley JP, Petras RE, Carey WD,et al. When is endoscopic polypectomy adequate therapy for colonic polyps containing invasive carcinoma? Gastroenterology 1986;91:419–27.
Coverlizza S, Risio M, Ferrari A,et al. Colorectal adenomas containing invasive carcinoma: pathologic assessment of lymph node metastatic potential. Cancer 1989;64:1937–47.
Haggitt RC, Glotzbach RE, Soffer EE, Wruble LD. Prognostic factors in colorectal carcinomas arising in adenomas; implications for lesions removed by endoscopic polypectomy. Gastroenterology 1985;89:328–36.
Colacchio TA, Forde KA, Scantlebury VP. Endoscopic polypectomy: inadequate treatment for invasive colorectal carcinoma. Ann Surg 1981;194:704–7.
Morson BC, Whiteway JE, Jones EA,et al. Histopathology and prognosis of malignant colorectal polyps treated by endoscopic polypectomy. Gut 1984;25:437–44.
Shatney CH, Lober PH, Gilbertsen VA, Sosin H. The treatment of pedunculated adenomatous colorectal polyps with focal cancer. Surg Gynecol Obstet 1974; 139:845–50.
Wolff WI, Shinya H. Definitive treatment of “malignant” polyps of the colon. Ann Surg 1975;182:516–25.
Nivatvongs S, Rojanasakul A, Reiman HM,et al. The risk of lymph node metastasis in colorectal polyps with invasive adenocarcinoma. Dis Colon Rectum 1991;34:323–8.
Wilcox GM, Anderson PB, Colacchio TA. Early invasive carcinoma in colonie polyps: a review of the literature with emphasis on the assessment of the risk of metastasis. Cancer 1986;57:160–71.
Kodaira S, Teramoto T, Ono S,et al. Lymph node metastases from carcinomas developing in pedunculated and semipedunculated colorectal adenomas. Aust N Z J Surg 1981;51:429–33.
Cooper HS. Surgical pathology of endoscopically removed malignant polyps of the colon and rectum. Am J Surg Pathol 1983;7:613–23.
Rossini FP, Ferrari A, Coverlizza S,et al. Large bowel adenomas containing carcinoma: a diagnostic and therapeutic approach. Int J Colorectal Dis 1988;3:47–52.
Hase K, Shatney CH, Johnson D,et al. Prognostic value of tumor “budding” in patients with colorectal cancer. Dis Colon Rectum 1993;36:627–35.
Muto T, Sawada T, Sugihara K. Treatment of carcinoma in adenomas. World J Surg 1991;15:35–40.
Nivatvongs S, Goldberg SM. Management of patients who have polyps containing invasive carcinoma removedvia colonoscope. Dis Colon Rectum 1978;21:8–11.
Sugihara K, Muto T, Morikawa Y. Management of patients with invasive carcinoma removed by colonoscopic polypectomy. Dis Colon Rectum 1989;32:829–34.
Webb WA, McDaniel L, Jones L. Experience with 1000 colonoscopic polypectomies. Ann Surg 1988;201:626–32.
Furusawa M. Prognosis of patients with colon cancer limited to submucosal layer, who had undergone endoscopic polypectomy. I to Cho 1985;20:1087–94.
Christie JP. Malignant colon polyps: cure by colonoscopy or colectomy? Am J Gastroenterol 1984;79:543–7.
Masuda T, Matsumoto K, Sugihira N,et al. A case report of colon cancer with submucosal invasion and lymph node metastasis with special reference to flow cytometric DNA analysis. Nippon Shokakigeka Gakkai Zasshi 1987;20:2666–8.
Ishii K, Okabe S, Nakajima K,et al. A study on early cancer of the colon and rectum. Nippon Shokakigeka Gakkai Zasshi 1986;19:2050–6.
Maruoka Y, Maetani S, Tobe T. Statistical analysis of pathologic factors influencing prognosis of colorectal carcinoma. Nippon Geka Gakkai Zasshi 1988;89:181–91.
Hayashida K, Isomoto H, Shirouzu K,et al. A study of invasive colorectal carcinoma with reference mainly to vessel invasion and budding. Nippon Daichokomonbyo Gakkai Zasshi 1987;40:119–26.
Author information
Authors and Affiliations
About this article
Cite this article
Hase, K., Shatney, C.H., Mochizuki, H. et al. Long-term results of curative resection of “minimally invasive” colorectal cancer. Dis Colon Rectum 38, 19–26 (1995). https://doi.org/10.1007/BF02053852
Issue Date:
DOI: https://doi.org/10.1007/BF02053852