Abstract
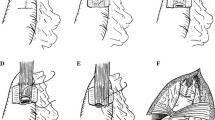
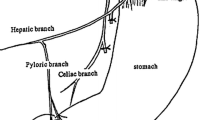
This is a report of our new method of valvuloplastic esophagogastrostomy for the prevention of postoperative reflux esophagitis, and the clinical results in 10 patients. After proximal resection of the stomach, the medial side of the cut end of the gastric remnant is closed in the usual fashion. The mucosal layer of the lateral side of the gastric remnant is partially closed, but the seromuscular layers are left open. The esophagus is anastomosed to the gastric remnant mucosa, which is inverted so as to form a mucosal valve. The seromuscular layers of the gastric remnant are then wrapped around the distal esophagus, similar to a Nissen fundoplication, so as to create an artificial fundus. The intragastric esophageal wall facing the fundus acts as a long oneway flap valve to prevent reflux. The 10 patients who have undergone valvuloplastic esophagogastrostomy have remained free of postoperative complications due to reflux. X-ray fluoroscopy and esophagoscopy done at the time of discharge from the hospital revealed no evidence of reflux or esophagitis. Withdrawal pH studies performed in 5 of the patients showed a sharp rise in pH starting at the site of the anastomosis. Withdrawal intraluminal pressure studies performed in 7 patients showed a high pressure zone with a mean pressure of 11.3 mm Hg and a mean length of 4.0 cm. These results indicate that the new method of esophagogastrostomy effectively prevented postoperative reflux esophagitis after conventional methods of proximal gastric resection.
Résumé
Nous présentons les résultats obtenus, chez 10 malades, par notre nouvelle technique d'oesogastrostomie avec valvuloplastie pur la prévention de l'oesophagite par reflux postopératoire. Après résection de la partie proximale de l'estomac, la partie interne de la tranche de section gastrique est suturée de la manière habituelle. La muqueuse de la partie externe est partiellement fermée, mais la séromusculeuse est laissée ouverte. L'oesophage est anastomosé à la muqueuse du moignon gastrique, et cette suture est invaginée pour former la valve muqueuse. La couche séromusculaire vient ensuite entourer l'oesophage distal, comme dans une fundoplicature à la Nissen, pour former une nouvelle poche à air. La paroi oesophagienne, en position intragastrique dans la nouvelle poche à air, forme une longue valve unidirectionnelle qui s'oppose au reflux. Les 10 malades qui ont subi cette oesogastrostomie avec valvuloplastie n'ont présenté aucune complication attribuable au reflux. Les examens radiologiques et endoscopiques au moment de la sortie n'ont montré ni reflux, ni oesophagite. Chez 5 malades, des mesures de pH faites de long de l'anastomose et de la valve révèlent une brusque élévation de pH au moment où l'électrode atteint le niveau de la suture. Chez 7 malades, des mesures de pression au même endroit montrent une zone de pression élevée (en moyenne 11.3 mm Hg sur une hauteur moyenne de 4.0 cm). Ces résultats indiquent que cette nouvelle technique d'oesogastrostomie est efficace dans la prévention de l'oesophagite par reflux après gastrectomie proximale conventionnelle.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Hatafuku, T., Higuchi, T., Kusaka, Y., Kato, S., Ohtsu, S., Kono, K., Yashima, Y., Seta, K.: [Review of the methods of proximal gastrectomy for a high gastric ulcer]. Operation29:143, 1975
Hatafuku, T., Higuchi, T., Ohtsu, S., Watanabe, M., Seta, K.: [Operative technique of valvuloplastic esophagogastrostomy]. Operation30:891, 1976
Hatafuku, T., Higuchi, T., Seta, K.: Introduction of a method of valvuloplastic esophagogastrostomy in proximal gastrectomy. Tohoku J. Exp. Med.124:129, 1978
Thal, A.P., Hatafuku, T., Kurtzman, R.: A new method for reconstruction of the esophagogastric junction. Surg. Gynecol. Obstet.120:1225, 1965
Hatafuku, T., Maki, T., Thal, A.P.: Fundic patch operation in the treatment of advanced achalasia of the esophagus. Surg. Gynecol. Obstet.134:611, 1972
Skinner, D.B., Booth, D.J.: Assessment of distal esophageal function in patients with hiatal hernia and/or gastroesophageal reflux. Ann. Surg.112:627, 1970
Fyke, F.E., Code, C.F., Schlegel, J.F.: The gastroesophageal sphincter in healthy human beings. Gastroenterologia86:135, 1956
Franke, H.: Erfahrungen mit einer Klappenbildung aus Magenwand nach Kardia-Resektion zur Vermeidung einer Reflux-esophagitis. Langenbecks Arch. Klin. Chir.322:406, 1968
Tocornal, J.A., Snow, H.D., Fonkalsrud, E.W.: A mucosal flap valve mechanism to prevent gastroesophageal reflux and esophagitis. Surgery64:519, 1968
Watkins, D.H., Prevedel, A.E., Munro, G.A.: Valvular esophagogastrostomy. A method of preventing peptic esophagitis following esophagogastric anastomosis. Surg. Forum5:328, 1954
Dillard, D.H., Griffith, C.A., Merendino, K.A.: Surgical construction of esophageal valve to replace “cardiac sphincter”. Surg. Forum5:306, 1954
Henderson, R.D., Feaver, B.: Invagination for control of reflux after esophagogastric anastomosis. Can. J. Surg.14:195, 1971
Merendino, K.A., Dillard, D.H.: The concept of sphincter substitution by an interposed jejunal segment for anatomic and physiologic abnormalities at the esophagogastric junction, with special reference to reflux esophagitis, cardiospasm and esophageal varices. Ann. Surg.142:486, 1955
Dillard, D.H., Merendino, K.A.: Experiences with the interposed jejunal segment operation combined with adjunct procedure in the prevention of esophagitis. An experimental study. Surg. Forum5:323, 1954
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Seta, K., Higuchi, T., Watanabe, M. et al. A method of valvuloplastic esophagogastrostomy to prevent reflux after proximal gastrectomy. World J. Surg. 2, 851–857 (1978). https://doi.org/10.1007/BF01556538
Issue Date:
DOI: https://doi.org/10.1007/BF01556538