Summary
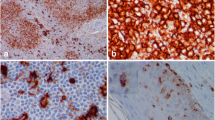
The morphological, ultrastructural and immunophenotypic properties of Histiocytosis-X (H-X) cells were investigated in a lymph node involved by Letterer-Siwe (L-S) disease. H-X cells were T6+ (CD1a), S-100+, T4+ (CD4) and HLA-DR+; in addition they were consistently T11+ (CD2) and were stained by antibodies directed against receptors for transferrin (T9), C3bi (OKM-1/CD11b), IgG-Fc (Leu-11/CD16) and Interleukin-2 (IL-2R/CD25). On immunostained cytosmears, T6+ cells were highly polymorphic and a prominent fraction (45%) showed immature morphology, characterized by lymphoid appearance. Cells expressing macrophage markers (ANAE, AACT, Leu-M3/CD14, PAM-1) were 10-fold fewer than T6+ cells and did not show a lymphoid morphology. At TEM level, H-X cells were characterized by poor content of LC granules and by the presence of myelin-like laminated bodies and of lysosome-like dense bodies. The immunophenotypic properties of H-X cells were compared to those of epidermal Langerhans cells (LCs) and of LCs present in lymph nodes of three cases of dermatopathic lymphadenitis. Epidermal LCs were T6+/HLA-DR+, and sometimes faintly T4+. Lymph node LCs were T6+, S-100+, T4+, HLA-DR+, and showed the same variety of surface receptors detected in H-X cells; furthermore, in a case with massive infiltration of the paracortex by T6+ cells, lymph node LCs were faintly T11+ and some of the T6+ cells had lymphoid aspect. Our findings suggest that the H-X cell population of L-S disease is not homogeneous, but is composed of discrete cell subsets with distinctive antigenic and morphological traits closely resembling those of cells of LC lineage at different maturational stages.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Alcover A, Ramarli D, Richardson NE, Chang H-C, Reinherz EL (1987) Functional and molecular aspects of human T lymphocyte activation via T3-Ti and T11 pathways. Immunol Rev 95:5–36
Beckstead JH, Wood GS, Turner RR (1984) Histiocytosis X cells and Langerhans cells: enzyme histochemical and immunologic similarities. Hum Pathol 15:826–833
Bieber T, Hanau D, Heid E, Kazatchkine MD (1985) Histiocytosis-X cells express C3b, C3d and C3bi receptor (CR1, CR2 and CR3) antigens. Arch Dermathol Res 277:496–498
Biondi A, Rossig TH, Bennett J, Todd RF (1984) Surface membrane heterogeneity among human mononuclear phagocytes. J Immunol 132:1237–1243
Buckley RH, Wray BB, Belmaker EZ (1972) Extreme hyperimmunoglobulinemia E and undue susceptibility to infections. Pediatrics 49:59–70
Chollet S, Dournovo P, Richard MS, Soler P, Basset F (1982) Reactivity of Histiocytosis X cells with monoclonal anti-T6 antibody. N E J Med 307:685
Goldberg NS, Bauer K, Rosen ST, Caro WA, Marder RJ, Zugerman C, Rao S, Variakojis D (1986) Histiocytosis X. Flow cytometric DNA-content and immunohistochemical and ultrastructural analysis. Arch Dermathol 122:446–450
Goordyal P, Isaacson PG (1985) Immunocytochemistry of monocytes growing in human bone marrow culture. A clue to the origin of Langerhans and Interdigitating reticulum cells. J Pathol 146:189–195
Harrist TJ, Bhan AK, Murphy GF, Sato S, Berman RS, Gellis SE, Freedman S, Mihm MC (1983) Histiocytosis X: in situ characterization of cutaneous infiltrates with monoclonal antibodies. Am J Clin Pathol 79:294–300
Hashimoto K, Pritzker MS (1973) Electron microscopic study of reticulohistiocytoma. An unusual case of congenital, self-healing reticulohistiocytosis. Arch Dermathol 107:263–270
Kahn HJ, Marks A, Thom H, Baumal R (1983) Role of antibody to S-100 protein in diagnostic pathology. Am J Clin Pathol 79:341–347
Lanier LL, Le AM, Cwirla S, Federspiel N, Phillips JH (1986) Antigenic, functional and molecular genetic studies of human natural killer cells and cytotoxic T lymphocytes not restricted by the major histocompatibility complex. Federation Proc 45:2823–2828
Lichtenstein L (1953) histiocytosis X: Integration of eosinophilic granuloma of bone. “Letterer-Siwe disease” and “Schuller-Christian disease”, as related manifestations of a single nosologic entity. Arch Pathol 56:84–102
Mirro J, Antoun GR, Zipf TF, Melvin S, Stass S (1985) The E rosette-associated antigen of T cells can be identified on blasts from patients with acute myeloblastic leukemia. Blood 65:363–367
Murphy GF (1985) Cell membrane glycoproteins and Langerhans cells. Hum Pathol 16:103–112
Murphy GF, Harrist TJ, Bahn AK, Mihm MC (1983) Distribution of cell surface antigens in Histiocytosis X cells. Quantitative immunoelectronmicroscopy using monoclonal antibodies. Lab Invest 48:90–97
Murphy GF, Massadi D, Fonferko E, Hancock WW (1986) Phenotypic transformation of macrophages to Langerhans cells in the skin. Am J Pathol 123:401–406
Nezelof C, Diebold N, Rousseau-Merck MF (1977) IgG surface receptors and erythrophagocytic activity of histiocytosis X cells in vitro. J Pathol 122:105–113
Nezelof C, Frileux-Herbert F, Cronier-Sachot J (1979) Disseminated histiocytos X. Analysis of prognostic factors based on a retrospective study of 50 cases. Cancer 44:1824–1838
Scarpelli D (1986) Histiocytosis X. Arch Dermathol 122:402–403
Steiner G, Tschachler E, Tani M, Malek TR, Shevach EM, Holter W, Knapp W, Wolff K, Stingl G (1986) Interleukin-2 receptor on cultured murine epidermal Langerhans cells. J Immunol 137:155–159
Stingl G, Wolff-Schreiner EC, Pichler WJ, Gschnait F, Wolff K (1977) Epidermal Langerhans cells bear Fc and C3 receptors. Nature 268:245–246
Thomas JA, Janossy G, Chilosi M, Pritchard J, Pincott JR (1982) Combined immunological and histochemical analysis of skin and lymph node lesions in Histiocytosis X. J Clin Pathol 35:327–337
Uccini S, Vitolo D, Stoppacciaro A, Paliotta D, Cassano AM, Barsotti P, Ruco LP, Baroni CD (1986) Immunoreactivity for S-100 protein in dendritic and in lymphocyte-like cells in human lymphoid tissues. Virchows Arch B (Cell Pathol) 52:129–141
Williams AF, Barclay AN, Clark SJ, Paterson DJ, Willis AC (1987) Similarities in sequences and cellular expression between rat CD2 and CD4 antigens. J Exp Med 165:368–380
Author information
Authors and Affiliations
Additional information
Supported by CNR contract N. 86.00303.44, Progetto Finalizzato Oncologia, and by Fondazione Cenci-Bolognetti Istituto Pasteur
Rights and permissions
About this article
Cite this article
Ruco, L.P., Remotti, D., Monardo, F. et al. Letterer-Siwe disease: Immunohistochemical evidence for a proliferative disorder involving immature cells of Langerhans lineage. Vichows Archiv A Pathol Anat 413, 239–247 (1988). https://doi.org/10.1007/BF00718616
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00718616