Summary
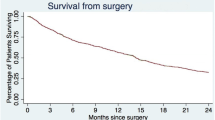
The efficacy of ‘limited posterior surgery’ for metastases in the thoracic and lumbar spine was studied prospectively in 51 patients (32 men and 19 women, mean age 64 years). The most common primary tumors were prostate, breast, and renal carcinoma, 37 patients had metastases in the thoracic spine and 14 in the lumbar spine. Indications for surgery were severe pain or neurologic deficit. Of the 46 patients with neurologic symptoms, 25 were unable to walk. Surgery was confined to direct or indirect decompression and stabilization with a pedicle screw fixator over few segments as possible. Pain, as well as a variety of functional performance parameters and residential status were registered preoperatively and after surgery at 3, 6, 9, and 12 months, and at 6-monthly intervals thereafter. Pain was rated by the patient on a Visual Analog Scale, and functional performance was assessed with the Eastern Co-operative Oncology Group (ECOG) Performance Status Scale. We had no perioperative neurologic deterioration or death. Nineteen of the 25 nonambulatory patients regained their walking ability. Postoperative pain relief was significant and lasting over time. Nearly half of the patients attained improvement in functional performance. The median survival was 8 months. Older age and intact postoperative walking ability were positive factors for survival.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Allen BL, Tencer AF, Ferguson RL (1987) The biomechanics of decompressive laminectomy. Spine 12: 803–808
Arseni CN, Simonescu MD, Horwath L (1959) Tumors of the spine. Acta Psychiatr Neurol Scand 34: 398–410
Barnat IL, Greenberg ER, Barret J (1983) Suspected epidural compression of the spinal cord and cauda equina by metastatic carcinoma. Cancer 51: 1953–1957
Barron KD, Hirano A, Araki A, Terry RD (1959) Experiences with metastatic neoplasms involving the spinal cord. Neurology 9: 91–106
Benson H, Scharff J, Todd ID (1979) Spinal cord compression in myeloma. Br Med J 1: 1541–1544
Berrettoni BA, Carter JR (1986) Mechanisms of cancer metastasis to bone. J Bone Joint Surg [Am] 68: 308–311
Black P (1979) Spinal metastasis. Current status and recommended guidelines for management. J Neurosurg 5: 726–746
Boland PJ, Lane JM, Sundaresan N (1982) Metastatic disease of the spine. Clin Orthop 169: 95–102
Boxer D I, Todd CEC, Coleman R, Fogelman I (1989) Bone secondaries in breast cancer: the solitary metastasis. J Nucl Med 30: 1318–1320
Brice J, McKissock W (1965) Surgical treatment of malignant extradural spinal tumours. Br Med J 1: 1341–1344
Bridwell KH, Jenny AB, Saul T, Rich K, Grubb RL (1988) Posterior segmental spinal instrumentation (PSSI) with posterolateral decompression and debulking for metastatic thoracic and lumbar spine disease. Limitations of the technique. Spine 13: 1383–1394
Brolund C (1982) Pain relief through radiotherapy and chemotherapy. Acta Anaesthesiol Scand 74: 114–116
Constans JP, Divitiis E, Donzelli R, Spaziante R, Meder JF, Haye C (1983) Spinal metastases with neurological manifestations. Review of 600 cases. J Neurosurg 59: 111–118
Cox DR (1972) Regression models for life tables. J R Stat Soc 34: 187–220
Dorey F, Nasser S, Amstutz H (1993) The need for confidence intervals in the presentation of orthopaedic data. Current concepts review. J Bone Joint Surg [Am] 1844–1852
Dunn RC, Kelly WA, Wohns RNW, Howe JF (1980) Spinal epidural neoplasia. J Neurosurg 52: 47–51
Fidler M (1986) Anterior decompression and stabilisation of metastatic spinal fractures. J Bone Joint Surg [Br] 68: 83–90
Findlay G (1987) The role of vertebral body collapse in the management of malignant spinal cord compression. J Neurol Neurosurg Psychiatry 50: 151–154
Fornasier MD, Czitrom AA (1978) Collapsed vertebrae. A Review of 659 autopsies. Clin Orthop 131: 261–265
Fosså S, Aaronson NK, van Cangh PJ, Denis L, Kurth KH, de Pauw M (1990) Quality of life and treatment of hormone resistant metastatic prostatic cancer. Eur J Cancer 26: 1133–1136
Freyd M (1923) The graphic rating scale. J Educat Psych 14: 83–102
Galasko C (1978) Mechanism of lytic and blastic metastatic disease in bone. Clin Orthop 4: 273–283
Gilbert RW, Kim JH, Posner JB (1978) Epidural spinal cord compresslon from metastatic tumor: diagnosis and treatment. Ann Neurol 3: 40–51
Goutallier DL, Lwertowski JM (1992) Treatment of thoracic, thoracolumbar and lumbar metastases with predominant involvement of the vertebral body by corporectomy and anterior fixation using cement and plate and screws applied to the vertebral bodies. J Orthop Surg 6: 324–327
Hall AJ, Mackay NN (1973) The results of laminectomy for compression of the cord or cauda equina by extradural malignant tumour. J Bone Joint Surg [Br] 55: 497–505
Hammerberg KW (1992) Surgical treatment of metastatic spine disease. Spine 17: 1148–1153
Harrington K (1986) Metastatic disease of the spine. J Bone Joint Surg [Am] 68: 1110–1115
Hays R, Shapiro M (1992) An overview of general health-related quality of life measures for HIV research. Qual Life Res 1: 91–97
Heller M, McBroom RJ, Macnab T, Perrin RM (1986) Treatment of metastatic disease of the spine with posterolateral decompression and Luque instrumentation. Neuro Orthopedics 2: 70–74
Joyce C, Zutshi D, Hrubes V, Mason R (1975) Comparison of fixed interval and visual analogue scales for rating chronic pain. Eur J Clin Pharmacol 8: 415–420
Jónsson B, Jónsson H Jr., Petrén-Mallmin M, Andréasson I, Sjöström L. Rauschning W (1995) Pathoanatomical findings in pedicle screw fixated thoracolumbar breast cancer metastases. Spine (submitted)
Jónsson B, Petrén-Mallmin M, Jónsson H Jr, Andréasson I, Rauschning W (1994) Pathoanatomical and radiographic findings in spinal breast cancer metastases. J Spinal Disord 8: 26–38
Jónsson B, Sjöström L, Jónsson H Jr., Karlström G (1992) Surgery for multiple myeloma of the spine. Acta Orthop Scand 63: 192–194
Jónsson B, Sjöström L, Olerud C, Jónsson H Jr, Andersén S, Karlström G (1994) Surgical treatment of spinal metastases. Cost-benefit analysis. A prospective study. J Bone Joint Surg [Br] 76: 7
Kaplan EL, Meier P (1958) Non-parametric estimation from incomplete observations. J Am Stat Assoc 53: 457–481
Karlström G, Andersén S, Sjöström L, Olerud C, Jónsson H Jr, Jónsson B (1992) Surgical stabilization in metastatic disease of the spine. Acta Orthop Scand; 63 [Suppl 248]: 15
Kleiman WB, Kiernan HA, Michelsen WJ (1978) Metastatic cancer of the spinal column. Clin Orthop 136: 166–172
Kostuik JP (1983) Anterior spinal cord decompression for lesions of the thoracic and lumbar spine: techniques, new methods of internal fixation results. Spine 8: 512–533
Kostuik JP, Errico TJ, Gleason TF, Errico CC (1988) Spinal stabilization of vertebral column tumors. Spine 13: 250–256
Kuban DA, Mahdi AM, Sigfred SV, Schellhammer PF, Babb TJ (1986) Characteristics of spinal cord compression in adenocarcinoma of prostate. Urology 28: 364–369
Livingstone KE, Perrin RG (1978) Neurological management of spinal metastases. J Neurosurg 49: 839–843
McAfee PC, Zdeblick TA (1989) Tumors of the thoracic and lumbar spine: Surgical treatment via the anterior approach. J Spinal Disord 2: 145–154
Moore AJ, Uttley D (1989) Anterior decompression and stabilization of the spine in malignant disease. J Neurosurg 24: 713–717
O'Neil JG, Gardner V, Armstrong G (1988) Treatment of tumors of the thoracic and lumbar spinal column. Clin Orthop 227: 103–112
Ohnhaus E, Alder R (1975) Methodological problems in the measurement of pain: a comparison between the verbal rating scale and the visual analogue scale. Pain 1: 379–384
Olerud C, Sjöström L, Jónsson H Jr (1992) Posterior reduction of a pathologic spinal fracture. A case of indirect anterior dural decompression. Acta Orthop Scand 63: 345–346
Olerud S, Karlström G, Sjöström L (1988) Transpedicular fixation of thoracolumbar vertebral fractures. Clin Orthop 227: 44–51
Onimus M, Schraub S, Bertin D, Bosset JF, Guidet M (1986) Surgical treatment of vertebral metastases. Spine 11: 883–891
Perrin RG, Livingstone LK (1980) Neurosurgical treatment of pathological fracture-dislocation of the spine. J Neurosurg 52: 330–334
Robinson R, McHugh P, Folstein M (1975) Measurement of appetite disturbances in psychiatric disorders. Pain 2: 175–184
SAS Institute (1989) SAS/STAT User's guide, version 6, 4th edn. SAS Institute, Cary, NC
Schaberg JGB (1985) A profile of metastatic carcinoma of the spine. Spine 10: 19–20
Scott J, Huskisson E (1976) Graphic representation of pain. Pain 2: 175–184
Siegal T, Siegal T (1985) Surgical decompression of anterior and posterior malignant epidural tumors compressing the spinal cord: a prospective study. J Neurosurg 17: 424–432
Siegal T, Siegal T (1985) Vertebral body resection for epidural compression by malignant tumors. Results of forty-seven consecutive operative procedures. J Bone Joint Surg [Am] 67: 375–382
Sjöström L, Jónsson H Jr, Karlström G, Ordeberg G (1993) Surgical treatment of vertebral metastases. Contemp Orthop 26: 247–255
Sundaresan N, Galichich JH (1984) Treatment of spinal metastases by vertebral body resection. Cancer Invest 2:383–397
Sörensen PS, et al (1990) Metastatic epidural spinal cord compression. Results of treatment and survival. Cancer 65: 1502–1508
Tokuhashi Y, Matsuzaki H, Toriyama S, Kawano H, Oshaka S (1990) Scoring system for the preoperative evaluation of metastatic spine tumor prognosis. Spine 11: 1110–1113
Tomita T, Galichich JH, Sundaresan NG (1983) Radiation therapy for spinal epidural metastases with complete block. Acta Radiol Oncol 22: 135–143
Turner PL, Prince HG, Webb JK, Sokal MP (1988) Surgery for malignant extradural tumours of the spine. J Bone Joint Surg [Br] 70: 51–56
Verger E, Salamero M, Conill C (1990) Can Karnofsky performance status be transformed to the Eastern Cooperative Oncology Group Scoring Scale and vice versa? Eur J Cancer 28: 1328–1330
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Jónsson, B., Sjöström, L., Olerud, C. et al. Outcome after limited posterior surgery for thoracic and lumbar spine metastases. Eur Spine J 5, 36–44 (1996). https://doi.org/10.1007/BF00307825
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00307825