Abstract
The accumulation of tau filaments in neurons is a pathological hallmark of various neurodegenerative diseases, including Alzheimer’s disease. However, it is not the filamentous aggregates themselves, but non-filamentous tau species, tau oligomer, that is thought to be the culprit in tau-mediated neurodegeneration. The definition of and methodology for isolating tau oligomers vary among researchers. Here we describe how tau oligomers are identified, summarize the differences of tau oligomers among research groups, and discuss their hypothesized functions.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Prediction of Non-fibrillar Aggregates of Tau Protein
Neurofibrillary tangles (NFTs), a pathological hallmark of Alzheimer’s disease (AD), are composed of filamentous polymers of tau protein [1]. NFTs are insoluble and resistant to proteases. Thus, even after neurons are lost, NFTs remain as “tombstones” of the NFT-bearing neurons and are called ghost tangles. In AD, the number of neurons lost and the number of NFT/ghost tangles should be the same if all of the neurons were lost after NFT formation. But they aren’t. More neurons are lost than ghost tangles remain [2, 3]. Although the number of NFTs, neurons lost, and the severity of the disease all correlate well with each other [3], several findings point to a missing element. NFT formation and neuronal loss have been reported to be distinct events. Suppression of human tau (hTau) expression in an hTau transgenic mouse model did not block tau filament formation but reduced neuronal loss [4], and NFT-bearing neurons were functionally intact in hTau transgenic mice [5]. In an hTau Drosophila model, hTau over-expression induced neuronal loss without NFT formation [6]. Therefore, overexpression of tau, at least, induces neuronal toxicity in an animal model, but the toxic species of tau was not the tau filament itself, but something produced in the process of tau aggregation. In that sense, granular tau oligomers, the intermediate form of tau filament, meet this criterion for the toxic tau species.
Tau Oligomer as an Intermediate Species of Tau Filament
Tau is highly hydrophilic and does not aggregate by itself. The core of the tau filament, the microtubule binding domain (MBD), is positively charged, and that charge prevents intermolecular interactions of tau. Under physiological conditions, the positively charged residues of tau interact with negatively charged residues of tubulin [1]. Under pathological conditions, tau is highly phosphorylated, and the negative charge of phosphor residues is thought to neutralize the positive change of the MBD, induce detachment of tau from tubulin, and allow tau-tau interactions [1].
Polyanionic compounds, such as RNA or heparin, induce aggregation of recombinant tau probably by neutralizing the positive charges of tau [7,8,9]. Lipids, such as arachidonic acid, also induce tau aggregation above the critical micelle concentration because the surfaces of lipid micelles are negatively charged [10]. In an in vitro tau aggregation assay, non-filamentous tau aggregates called granular tau oligomers were found [11]. The non-filamentous tau aggregates could be separated from tau monomers and filaments by sucrose gradient centrifugation (Fig. 27.1). Tau filaments do not form in vitro without aggregation inducers. However, simply concentrating tau oligomers induces tau filament formation without additional heparin, and under atomic force microscopy (AFM), filaments formed in vitro or purified and AD brain degraded to granular tau structures [11] (Fig. 27.2). This suggested that the tau oligomer is an intermediate species of the tau filament. In addition, tau oligomers were found in animal models and human brains [12,13,14] (Fig. 27.3). The amino acid sequences critical for tau filament formation, PHF6 and PHF6∗ [15], are also reported to be key for tau oligomerization by western blots (WBs) and nuclear magnetic resonance analysis [16, 17]. In human brains, the number of tau oligomers was increased in the frontal cortex of Braak stage I patients, when NFTs have yet to form. Thus, tau oligomers form before NFTs [12,13,14].
The purification of granular tau oligomers using sucrose step gradient centrifugation. (a) Tau proteins were aggregated in vitro and layered onto 20–50% sucrose step gradients and centrifuged at 200,000 × G for 2 h to separate non-aggregated tau, granular tau oligomers, and tau filaments. (b, c) Staining with Coomassie brilliant blue (CBB) (b) and AFM images of all fractions (c) are shown. Granular tau oligomers could be recovered in fraction 3 as indicated (b, c). In fraction 1, tau monomers and multimers were collected (b), but no aggregated structure were observed under AFM (c). The amount of tau in fraction 3 was less than that in fraction 1 (b), but granular structures were detected under AFM (c). Longer filaments were collected in fractions 4–6 (c) [11]
The formation and degradation of tau filaments. (a) Granular tau oligomers in fraction 3 and non-aggregated tau in fraction 1 were concentrated without adding heparin. Filaments were observed by AFM in concentrated fraction 3 (C3) but not in the concentrated fraction 1 (C1). Blue arrows indicate the generated filaments in C3. (b, c) Structures were exposed to mechanical damage by AFM tips. Continuous AFM observation revealed that mechanical damage degraded tau filaments formed in vitro (b) or purified from an AD brain (c) to granular tau structures. The numbers at the top right indicate the order of the images. It took about 9 min to take an image [11]. Blue arrows indicate the breaking points of the tau filament
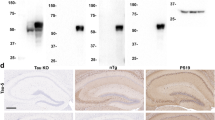
Purification of granular tau oligomers from human brains. (a) Granular tau oligomers in human brains were purified in a combination of immune-affinity column chromatography with a pan-tau antibody and sucrose step gradient centrifugation [12]. (b) AD brains (Braak stage V) contained more granular tau oligomers than control brains (Braak stage 0) [12]. Inserts show the magnified images of granular tau oligomers purified from AD or control brains
Various Types of Non-filamentous Tau Aggregates
Definition and preparation of tau oligomers vary among researchers. For example, Maeda et al. induced tau aggregation by mixing recombinant tau with heparin and defined tau oligomers as granular structures under AFM [11]. The Davies group reported non-filamentous tau species that were extracted by a conformation-dependent antibody, MC1 [18]. The non-filamentous tau species formed filaments after concentration, indicating that the oligomers extracted here are identical with the oligomers described above. Berger et al. reported a correlation of tau multimers and behavioral scores in an hTau transgenic mouse model [19]. Multimers were defined by the molecular mass by WB (140- and 170-kDa bands). The multimer can be a component of higher order aggregates, such as globular oligomers or tau filaments, but it degrades to a multimeric form under WB denaturing conditions. Thus, one component of tau oligomers may be the 140-/170-kDa multimers. Multimers might also be complexes of tau and other molecules, but another group reported that similar multimers may form only from recombinant tau [16]. Mandelkow’s group induced tau oligomers using recombinant protein produced in insect cells (i.e., Sf9 cells) because highly phosphorylated tau proteins can be extracted, whereas recombinant tau protein produced in E. coli had no post-translational modifications [20]. They confirmed that phosphorylation enhanced tau aggregation [20, 21]. The Kayed group generated tau oligomers by cross-seeding with amyloid beta (Aβ) oligomers [22]. Those oligomers induced cell death when added exogenously to cells [22, 23]. Anti-tau oligomer antibodies were generated using the cross-seeded tau oligomers, and the antibodies blocked tau-induced neurodegeneration in hTau transgenic mouse models that lack Aβ aggregates and could not form Aβ seeds [24, 25]. Thus, tau aggregates, like tau oligomers seeded by Aβ aggregates, can be induced in the absence of Aβ aggregates. Binder’s group [26] stabilized tau aggregates with a chemical cross linker and found that, by WB, the tau dimer is a component of tau aggregates and that cross-linked tau dimers form short filaments and oligomeric globular structures but not long filaments.
Tau Oligomer Detection Methods EM and Oligomer Antibodies
Granular tau oligomers can be detected by AFM and electron microscopy (EM) [11, 22, 26], but not by other methods. To expand their ability to study tau, researchers generated antibodies specific for tau oligomers.
The Davies group generated two conformation-dependent antibodies, Alz50 and MC1 [27], that react with tau filaments purified from AD brains. Alz50 recognizes discontinuous sequences at the N-terminus and MBD. During abnormal conformation changes, inter- or intramolecular attachment of the N-terminus to the MBD may generate the Alz50 epitope [28]. MC1 is a second-generation conformation-dependent antibody that was raised against tau aggregates purified with an Alz50 immunoaffinity column. MC1 reacts with aggregated tau species more specifically than Alz50 [27, 29] and detects both tau filaments and oligomers [2]. With a combination of sucrose step gradients and the MC1 antibody, oligomeric species can be detected even in mouse tissue lysates [14]. However, the requirement for sucrose step gradient centrifugation limits the ability to do mechanistic studies of tau oligomer-dependent pathogenesis.
Researchers next sought to distinguish tau oligomers from tau filaments without gradient centrifugation. They generated more specific antibodies against tau oligomers than Alz50 and MC1 antibodies. Binder’s group found the 180-kDa tau species in AD brain lysates [26]. To examine the pathogenesis of this tau species, they cross-linked tau dimers to obtain stable lower-order tau aggregates. When incubated with arachidonic acid, cross-linked tau dimers formed granular tau oligomer but not long fibrils. The researchers immunized tau-knockout mice with the cross-linked tau dimers and obtained the Tau Oligomeric Component-1 (TOC1) antibody [26]. TOC1 preferentially labels granular tau oligomers and the end of tau filaments, supporting the idea that tau oligomers are an intermediate species of tau filament and the attachment of tau oligomer to tau filament will elongate the filament [11]. Unlike another tau-conformation dependent antibody, Alz50 that recognizes discontinuous tau sequences, amino acids 2–10 and 312–342, TOC1 recognizes amino acids 209–224 of tau.
TNT1 is another conformation-dependent antibody generated by the Binder group [30]. Its epitope is the tau phosphatase-activating domain (PAD) in the N-terminal domain. The N-terminus attaches to the MBD under physiological conditions. It is detached by aggregation or phosphorylation and impairs axonal transport via phosphatase activation, GSK-3β activation, and kinesin light chain phosphorylation [30, 31]. As with all other tau oligomer antibodies, reactivity depends on conformation. Notably, the PAD sequence lacks the endogenous mouse tau sequence, and thus, TNT1 cannot detect mouse tau even though mouse tau aggregates like human tau [32]. Both TOC1 and TNT1 are pan-tau antibodies in WB because their epitopes are freely accessible even under denatured conditions [33].
The Kayed group raised antibodies against the cross-seeding oligomeric species of tau and obtained the T22 (rabbit polyclonal) and TOMA (mouse monoclonal) antibodies [25, 34]. For unknown reasons, the epitopes of these antibodies are preserved even in WB, whereas other conformation-dependent antibodies function as pan-tau antibodies in WB because all sequences of tau protein are accessible to the antibodies. Normal tau immunization induced neurologic deficits in normal mice [35]. However, immunization with these antibodies blocked tau-induced neuronal dysfunction in hTau transgenic mice as mentioned above, suggesting that granular tau oligomers, not tau monomers, should be explored as therapeutic targets for tauopathies [24, 25].
Tau Oligomerization Enhancers, Blockers, and the Toxic Mechanism
Not all FTDP-17 mutations increase tau filament formation [36, 37]. However, all FTDP-17 tau mutations examined so far for tau oligomerization enhanced tau oligomerization. Notably, the P301L mutation decreases the size and increases the number of tau oligomers [14].
Tau aggregates (mainly filaments) have been suggested to spread from one brain region to another trans-synaptically [38]. The spreading may be mediated by the tau aggregates themselves, which are called prion-like tau species, but not by the dysfunction of projecting neurons [38]. Although it is not clear that the soluble fraction has prion-like activity [39, 40], tau oligomers may mediate the propagation [41]. They may function as a template for newly formed tau oligomers that can be amplified by adding non-aggregated tau [22]. Thus, the tau oligomer itself may increase tau oligomer numbers.
Heat shock proteins (HSPs) are involved in tau oligomerization [42]. HSPs, including Hsp90 and 27 that block tau aggregation, are inversely correlated with tau oligomer levels in human brains [16]. Thus, HSPs are an intriguing target for therapies to prevent tau pathogenesis [43, 44]. Other small molecules also block tau oligomerization. A screen of a library of natural compound derivatives for tau-binding compounds revealed several positives. For example, 1,2-dihydroxybenzene blocked tau oligomerization, and DL-isoproterenol reduced tau aggregation and neuronal cell loss in human tau transgenic mice [45]. These findings also support the idea that tau oligomer is a culprit of tau-mediated pathogenesis.
Tau aggregates accumulate inside of neurons. Thus, to assess their toxicity, tau oligomers must be introduced into neurons. However, tau oligomers are thought to be incorporated into cells [46] and to induce synaptotoxicity and Ca dysregulation [20, 47]. Surprisingly, the synaptotoxicity may be separate from cell viability, even though neuronal cell loss correlates well with the NFT formation as mentioned above. Ca dysregulation by tau oligomers may be mediated by M1 and M3 muscarinic receptors [48], even though aggregated tau species showed less toxicity than monomeric non-aggregated tau in that system.
The mechanism of tau toxicity is unknown, but a hint might be provided by its conformation. Tau is reported to have a paper-clip conformation: the N-terminus is bent over to MBD in native state [49]. Tau aggregation disrupt that conformation and exposes the N-terminus. The exposure allows the PAD domain to induce the impairment of axonal trafficking [30].
Conclusion
Tau aggregation is toxic to cells. Thus, many researchers have visualized tau aggregation in their experimental models to search for a common feature between AD patients and the models. The exact mechanism of tau aggregation and toxicity and the targets of tau aggregates are still open issues. The discrepancy of tau filaments from neuronal cell loss implicates tau oligomers as the culprit of tau-mediated pathogenesis. Researchers have characterized tau oligomers by various methods. However, to directly examine their toxicity mechanisms, we will need methods to enhance or block tau oligomerization inside neurons. Also, to develop drugs that target tau oligomers, we will need tau oligomer probes that can be used for the target engagement in human live imaging. Antibodies specific for tau oligomers were used to show that tau oligomers have a structure distinct from other tau species. Thus, it might be possible to develop tau oligomer–specific probes for positron emission tomography. Those probes would be a powerful tool in combination with similar probes for tau filaments [50].
References
Morris M, Maeda S, Vossel K, Mucke L. The many faces of tau. Neuron. 2011;70:410–26.
Ihara Y. PHF and PHF-like fibrils--cause or consequence? Neurobiol Aging [Internet]. 2001;22(1):123–6. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11164285
Gómez-Isla T, Hollister R, West H, Mui S, Growdon JH, Petersen RC, et al. Neuronal loss correlates with but exceeds neurofibrillary tangles in Alzheimer’s disease. Ann Neurol. 1997;41(1):17–24.
Santacruz K, Lewis J, Spires T, Paulson J, Kotilinek L, Ingelsson M, et al. Tau suppression in a neurodegenerative mouse model improves memory function. Science [Internet]. 2005;309(5733):476–81. Available from: http://www.ncbi.nlm.nih.gov/pubmed/16020737%5Cn, http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=PMC1574647
Kuchibhotla KV, Wegmann S, Kopeikina KJ, Hawkes J, Rudinskiy N, Andermann ML, et al. Neurofibrillary tangle-bearing neurons are functionally integrated in cortical circuits in vivo. Proc Natl Acad Sci. 2014;111:510–4.
Wittmann CW, Wszolek MF, Shulman JM, Salvaterra PM, Lewis J, Hutton M, et al. Tauopathy in Drosophila: neurodegeneration without neurofibrillary tangles. Science. 2001;293(5530):711–4.
Kampers T, Friedhoff P, Biernat J, Mandelkow EM, Mandelkow E. RNA stimulates aggregation of microtubule-associated protein tau into Alzheimer-like paired helical filaments. FEBS Lett [Internet]. 1996;399(3):344–9. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=8985176
Goedert M, Jakes R, Spillantini MG, Hasegawa M, Smith MJ, Crowther RA. Assembly of microtubule-associated protein tau into Alzheimer-like filaments induced by sulphated glycosaminoglycans. Nature [Internet]. 1996;383(6600):550–3. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=8849730
Perez M, Valpuesta JM, Medina M, Montejo de Garcini E, Avila J. Polymerization of tau into filaments in the presence of heparin: the minimal sequence required for tau-tau interaction. J Neurochem [Internet]. 1996;67(3):1183–90. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=8752125
Chirita CN, Necula M, Kuret J. Anionic micelles and vesicles induce tau fibrillization in vitro. J Biol Chem. 2003;278(28):25644–50. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=12730214
Maeda S, Sahara N, Saito Y, Murayama M, Yoshiike Y, Kim H, et al. Granular tau oligomers as intermediates of tau filaments. Biochemistry. 2007;46(12):3856–61.
Maeda S, Sahara N, Saito Y, Murayama S, Ikai A, Takashima A. Increased levels of granular tau oligomers: an early sign of brain aging and Alzheimer’s disease. Neurosci Res. 2006;54(3):197–201.
Lasagna-Reeves CA, Castillo-Carranza DL, Sengupta U, Guerrero-Munoz MJ, Kiritoshi T, Neugebauer V, et al. Alzheimer brain-derived tau oligomers propagate pathology from endogenous tau. Sci Rep [Internet]. 2012;2:700. Available from: http://www.nature.com/srep/2012/121003/srep00700/full/srep00700.html
Maeda S, Sato Y, Takashima A. Frontotemporal dementia with Parkinsonism linked to chromosome-17 mutations enhance tau oligomer formation. Neurobiol Aging. 2018;69:26–32.
Von Bergen M, Barghorn S, Li L, Marx A, Biernat J, Mandelkow EM, et al. Mutations of tau protein in frontotemporal dementia promote aggregation of paired helical filaments by enhancing local beta-structure. J Biol Chem. 2001;276(51):48165–74.
Sahara N, Maeda S, Murayama M, Suzuki T, Dohmae N, Yen SH, et al. Assembly of two distinct dimers and higher-order oligomers from full-length tau. Eur J Neurosci. 2007;25(10):3020–9.
Peterson DW, Zhou H, Dahlquist FW, Lew J. A soluble oligomer of tau associated with fiber formation analyzed by NMR. Biochemistry [Internet]. 2008;47(28):7393–404. Available from: https://www.ncbi.nlm.nih.gov/pubmed/18558718
Weaver CL, Espinoza M, Kress Y, Davies P. Conformational change as one of the earliest alterations of tau in Alzheimer’s disease. Neurobiol Aging [Internet]. 2000;21(5):719–27. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11016541
Berger Z, Roder H, Hanna A, Carlson A, Rangachari V, Yue M, et al. Accumulation of pathological tau species and memory loss in a conditional model of tauopathy. J Neurosci. 2007;27(14):3650–62.
Tepper K, Biernat J, Kumar S, Wegmann S, Timm T, Hübschmann S, et al. Oligomer formation of tau protein hyperphosphorylated in cells. J Biol Chem. 2014;289(49):34389–407.
Alonso A, Zaidi T, Novak M, Grundke-Iqbal I, Iqbal K. Hyperphosphorylation induces self-assembly of tau into tangles of paired helical filaments/straight filaments. Proc Natl Acad Sci U S A [Internet]. 2001;98(12):6923–8. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11381127
Lasagna-Reeves CA, Castillo-Carranza DL, Guerrero-Muñoz MJ, Jackson GR, Kayed R. Preparation and characterization of neurotoxic tau oligomers. Biochemistry. 2010;49(47):10039–41.
Lasagna-Reeves CA, Castillo-Carranza DL, Sengupta U, Clos AL, Jackson GR, Kayed R. Tau oligomers impair memory and induce synaptic and mitochondrial dysfunction in wild-type mice. Mol Neurodegener. 2011;6(1):39.
Castillo-Carranza DL, Sengupta U, Guerrero-Muñoz MJ, Lasagna-Reeves CA, Gerson JE, Singh G, et al. Passive immunization with Tau oligomer monoclonal antibody reverses tauopathy phenotypes without affecting hyperphosphorylated neurofibrillary tangles. J Neurosci [Internet]. 2014;34(12):4260–72. Available from: http://www.ncbi.nlm.nih.gov/pubmed/24647946
Castillo-Carranza DL, Gerson JE, Sengupta U, Guerrero-Muñoz MJ, Lasagna-Reeves CA, Kayed R. Specific targeting of tau oligomers in Htau mice prevents cognitive impairment and tau toxicity following injection with brain-derived tau oligomeric seeds. J Alzheimers Dis. 2014;40(Suppl 1):S97–S111.
Patterson KR, Remmers C, Fu Y, Brooker S, Kanaan NM, Vana L, et al. Characterization of prefibrillar tau oligomers in vitro and in Alzheimer disease. J Biol Chem. 2011;286(26):23063–76.
Jicha GA, Bowser R, Kazam IG, Davies P. Alz-50 and MC-1, a new monoclonal antibody raised to paired helical filaments, recognize conformational epitopes on recombinant tau. J Neurosci Res [Internet]. 1997;48(2):128–32. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=9130141
Carmel G, Mager EM, Binder LI, Kuret J. The structural basis of monoclonal antibody Alz50’s selectivity for Alzheimer’s disease pathology. J Biol Chem [Internet]. 1996;271(51):32789–95. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=8955115
Jeganathan S, Hascher A, Chinnathambi S, Biernat J, Mandelkow EM, Mandelkow E. Proline-directed pseudo-phosphorylation at AT8 and PHF1 epitopes induces a compaction of the paperclip folding of tau and generates a pathological (MC-1) conformation. J Biol Chem. 2008;283:32066–76.
Kanaan NM, Morfini GA, LaPointe NE, Pigino GF, Patterson KR, Song Y, et al. Pathogenic forms of tau inhibit kinesin-dependent axonal transport through a mechanism involving activation of axonal phosphotransferases. J Neurosci. 2011;31(27):9858–68.
LaPointe NE, Morfini G, Pigino G, Gaisina IN, Kozikowski AP, Binder LI, et al. The amino terminus of tau inhibits kinesin-dependent axonal transport: implications for filament toxicity. J Neurosci Res. 2009;87:440–51.
Kampers T, Pangalos M, Geerts H, Wiech H, Mandelkow E. Assembly of paired helical filaments from mouse tau: implications for the neurofibrillary pathology in transgenic mouse models for Alzheimer’s disease. FEBS Lett [Internet]. 1999;451(1):39–44. Available from: http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=10356980
Cox K, Combs B, Abdelmesih B, Morfini G, Brady ST, Kanaan NM. Analysis of isoform-specific tau aggregates suggests a common toxic mechanism involving similar pathological conformations and axonal transport inhibition. Neurobiol Aging. 2016;47:113–26.
Lasagna-Reeves CA, Castillo-Carranza DL, Sengupta U, Sarmiento J, Troncoso J, Jackson GR, et al. Identification of oligomers at early stages of tau aggregation in Alzheimer’s disease. FASEB J. 2012;26:1946–59.
Rosenmann H, Grigoriadis N, Karussis D, Boimel M, Touloumi O, Ovadia H, et al. Tauopathy-like abnormalities and neurologic deficits in mice immunized with neuronal tau protein. Arch Neurol. 2006;63(10):1459–67.
Nacharaju P, Lewis J, Easson C, Yen S, Hackett J, Hutton M, Yen S-H. Accelerated filament formation from tau protein with specific FTDP-17 missense mutations. FEBS Lett. 1999;447 (2–3):195–9.
Arrasate M, Mitra S, Schweitzer ES, Segal MR, Finkbeiner S. Inclusion body formation reduces levels of mutant huntingtin and the risk of neuronal death. Nature. 2004;431(7010):805–10.
Mudher A, Colin M, Dujardin S, Medina M, Dewachter I, Alavi Naini SM, et al. What is the evidence that tau pathology spreads through prion-like propagation? Acta Neuropathol Commun. 2017;5(1):99.
Clavaguera F, Bolmont T, Crowther RA, Abramowski D, Frank S, Probst A, et al. Transmission and spreading of tauopathy in transgenic mouse brain. Nat Cell Biol. 2009;11(7):909–13.
Sanders DW, Kaufman SK, DeVos SL, Sharma AM, Mirbaha H, Li A, et al. Distinct tau prion strains propagate in cells and mice and define different tauopathies. Neuron. 2014;82(6):1271–88.
Gerson JE, Kayed R. Formation and propagation of tau oligomeric seeds. Front Neurol. 2013;4:93.
Pratt WB, Gestwicki JE, Osawa Y, Lieberman AP. Targeting Hsp90/Hsp70-based protein quality control for treatment of adult onset neurodegenerative diseases. Annu Rev Pharmacol Toxicol. 2015;55:353–71.
Fontaine SN, Martin MD, Akoury E, Assimon VA, Borysov S, Nordhues BA, et al. The active Hsc70/tau complex can be exploited to enhance tau turnover without damaging microtubule dynamics. Hum Mol Genet. 2015;24:3971–81.
Abisambra J, Jinwal UK, Miyata Y, Rogers J, Blair L, Li X, et al. Allosteric heat shock protein 70 inhibitors rapidly rescue synaptic plasticity deficits by reducing aberrant tau. Biol Psychiatry. 2013;74:367–74.
Soeda Y, Yoshikawa M, Almeida OFX, Sumioka A, Maeda S, Osada H, et al. Toxic tau oligomer formation blocked by capping of cysteine residues with 1,2-dihydroxybenzene groups. Nat Commun [Internet]. 2015;6:1–12. https://doi.org/10.1038/ncomms10216.
Shafiei SS, Guerrero-Muñoz MJ, Castillo-Carranza DL. Tau oligomers: cytotoxicity, propagation, and mitochondrial damage. Front Aging Neurosci. 2017;9:83.
Kaniyappan S, Chandupatla RR, Mandelkow EM, Mandelkow E. Extracellular low-n oligomers of tau cause selective synaptotoxicity without affecting cell viability. Alzheimers Dement. 2017;13(11):1270–91.
Gómez-Ramos A, Díaz-Hernández M, Rubio A, Miras-Portugal MT, Avila J. Extracellular tau promotes intracellular calcium increase through M1 and M3 muscarinic receptors in neuronal cells. Mol Cell Neurosci. 2008;37:673–81.
Jeganathan S, Von Bergen M, Brutlach H, Steinhoff HJ, Mandelkow E. Global hairpin folding of tau in solution. Biochemistry. 2006;45(7):2283–93.
Sahara N, Shimojo M, Ono M, Takuwa H, Febo M, Higuchi M, et al. In vivo tau imaging for a diagnostic platform of tauopathy using the rTg4510 mouse line. Front Neurol. 2017;8:663.
Acknowledgement
The authors thank Dr. Gary Howard for editorial review. This research was partially supported by grants from the Cyclic Innovation for Clinical Empowerment (CiCLE) and the Acceleration Program for Intractable Diseases Research Utilizing Disease-specific iPS Cells from the Japan Agency for Medical Research and Development (AMED) and JSPS to SM.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Maeda, S., Takashima, A. (2019). Tau Oligomers. In: Takashima, A., Wolozin, B., Buee, L. (eds) Tau Biology. Advances in Experimental Medicine and Biology, vol 1184. Springer, Singapore. https://doi.org/10.1007/978-981-32-9358-8_27
Download citation
DOI: https://doi.org/10.1007/978-981-32-9358-8_27
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-32-9357-1
Online ISBN: 978-981-32-9358-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)