Abstract
The femoral trochlea is important for controlling the patellofemoral gliding mechanism [4,19]. The normal articular shape of the trochlea and patella allow for undisturbed patellar tracking. The normal cartilaginous surface of the trochlea consists of the lateral and medial facets of the femoral sulcus and is defined by different criteria in the proximal-distal, medio-lateral, and antero-posterior direction [9, 10, 27]. The normal trochlea deepens from proximal to distal [9, 27]. In the proximal-distal direction, it is longest laterally and shortest on the medial side (Fig. 26.1). The deepened trochlear groove separates the lateral facet from the medial part. In the antero-posterior measurements, the most anterior aspect of the lateral condyle is normally higher than the medial condyle and the deepest point is represented by the center of the trochlear groove [10].
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Trochlear Groove
- Antero-posterior Measurement
- Femoral Sulcus
- Lateral Articular Facet
- Trochlear Dysplasia
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
26.1 Introduction
The femoral trochlea is important for controlling the patellofemoral gliding mechanism [4,19]. The normal articular shape of the trochlea and patella allow for undisturbed patellar tracking. The normal cartilaginous surface of the trochlea consists of the lateral and medial facets of the femoral sulcus and is defined by different criteria in the proximal-distal, medio-lateral, and antero-posterior direction [9, 10, 27]. The normal trochlea deepens from proximal to distal [9, 27]. In the proximal-distal direction, it is longest laterally and shortest on the medial side (Fig. 26.1). The deepened trochlear groove separates the lateral facet from the medial part. In the antero-posterior measurements, the most anterior aspect of the lateral condyle is normally higher than the medial condyle and the deepest point is represented by the center of the trochlear groove [10].
Trochlear dysplasia is an abnormality of shape and depth of the trochlear groove, mainly in its proximal extent [17,28]. It represents an important pathologic articular morphology that is a strong risk factor for permanent patellar instability [3, 4, 9, 12–15, 17, 18, 22, 23, 25, 29, 30]. Dejour et al. [15] described several types of trochlear dysplasia with increasing severity. The trochlear depth may be decreased, the trochlea may be flat, or a trochlear bump is present. According to this, different classifications are described in the literature [12, 16].
Additionally we have noticed that there exists a wide spread variability of combinations of trochlear dysplasia [9]. Seen from this angle we documented a different and unknown type of trochlear dysplasia, which to our present knowledge not described before: the too short lateral articular trochlea (Fig. 26.2) [5, 6]. We believe that this short lateral trochlea is another relevant factor for lateral patellar instability. Accordingly, surgical treatment should aim to correct this specific type of dysplastic trochlea.
26.2 Physical Examination
The patients with a too short lateral trochlea facet suffer from patellar instability. The patella is well centred in the trochlea under relaxed conditions. But when the patient contracts the quadriceps muscle with the leg in extension, the patella is pulled to proximal out of the short trochlea because it is not sufficiently guided and stabilized by the too short lateral facet of the trochlea. In most cases, the contraction also causes subluxation to the lateral side (Fig. 26.3a and b). We call this abnormal gliding mechanism dynamic supero-lateral patellar subluxation. This clinical finding is often only mild, but significant. In severe cases, this can also cause complete dynamic lateral patellar dislocation. In contrast to the lateral pull sign described by Kolowich et al. [21], this type of patellofemoral instability is primarily due not to soft tissue abnormalities (atrophy of the vastus medialis obliquus and hypertrophy of the vastus lateralis and lateral structures), but caused by a pathologic proximal patellar tracking due to the missing osteochondral opposing force of the lateral trochlea facet. This type of patella instability can also be depicted by manual examination in complete extension of the knee. Only minimal manual pressure laterally causes subluxation and discomfort to the patient. In most cases the patient feels pain and tries to resist this manoeuvre. This test in full extension must be differentiated from the patellar apprehension test which is performed in 20°–30° of knee flexion [4, 24]. With increasing knee flexion, the patella enters into the more distal and normal part of the trochlear groove and becomes more and more stable. This confirms the clinical suspicion of proximal patellar instability to the lateral side.
26.3 Imaging
26.3.1 Radiographs
The radiologic examination of patients with a too short lateral facet of the trochlea do not normally show the typical findings of trochlear dysplasia in the true lateral view such as the crossing sign, supratrochlear spur, double contour [12, 14, 15, 17] or lateral trochlear sign [20]. Radiographs can only show signs of dysplasia in combined trochlear abnormalities. The different indices used for patellar height measurements are normal.
26.3.2 MR Measurements
MR images allow complete and precise visualization of the patellofemoral joint by clearly delineating the proximal portion of the trochlea and for assessing femoral trochlear dysplasia [12, 26]. MR imaging is therefore the best modality to assess the proximal part of the trochlea in patients with suspected too short lateral facet of the trochlea.
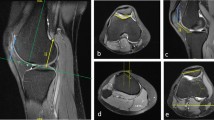
MR measurements are performed with the knee in 0° of flexion, the foot in 15° external rotation, and the quadriceps muscle consciously relaxed. Measurements on sagittal images include different parameters (Fig. 26.4) [5, 6, 11]. The parameters are measured on the most lateral section of the lateral condyle with visible articular cartilage in the trochlea (Fig. 26.5). The length of the anterior articular cartilage of the lateral trochlea (a) is calculated using as a reference the length of the posterior articular cartilage of the lateral condyle (p). For each individual subject p is always considered to be 100%. The variable length of a is calculated in percentages with regard to p. The lateral condyle index compares the length a with the length p and is expressed in percentages.
MR measurements (31). C1 Proximal circle in the femoral shaft. C2 Distal circle in the femoral shaft. Ca Central axis. d Baseline distal condyle (perpendicular to Ca). 1 Superior most aspect of anterior cartilage of the lateral condyle. 2 Superior most aspect of posterior cartilage of the lateral condyle. a Length of the anterior articular cartilage of the lateral condyle (red line). p Length of the posterior articular cartilage of the lateral condyle (blue line)
The values of the lateral condyle index found in a normal control population without any patellofemoral complaints were on average 93% [11]. Therefore we consider an anterior length of the lateral articular facet of the trochlea with index values of 93% or more of the length of the posterior articular cartilage as normal (Fig. 26.5). Lateral condyle index values of 84% (on average) were found in patients with chronic lateral patellar subluxation and instability documenting a too short lateral articular facet of the trochlea (Fig. 26.6). Index values of less than 93% must therefore be considered as pathologic and values of 86% or less confirm the presence of a too short lateral facet. Index values between 86% and 93% need additional assessment such as the patellotrochlear index or radiologic patellar height measurements (Insall-Salvati, Blackburne-Peel,Caton-Dechamps ratios) to document or exclude Patella Alta [7]. In cases with normal patellar height measurements, lengthening of the anterior lateral articular facet of the trochlea is recommended. In cases with Patella Alta, other surgical interventions, such as distalization of the tibial tubercle or shortening of the patellar tendon, may be needed.
26.4 Surgery
Surgical techniques have been developed to correct the pathologic morphology, though they differ in the site of surgical correction [1–3, 13–15, 17, 22, 25, 29, 30]. The therapeutic procedure which aims at correcting the abnormalities is selected according to the documented type of trochlear dysplasia [9,17]. Elevation of the lateral trochlea facet of a flat dysplastic trochlea, lowering the floor of the sulcus, and removing a prominent trochlear bump are described in numerous variations as reasonable well known surgical procedures to treat patellar instability [1, 3, 4, 9, 12–15, 17, 23, 29, 30].
26.4.1 Lengthening
Lengthening of the lateral facet is another, mostly unknown technique of trochleoplasty. It is indicated when a too short lateral trochlea is documented (clinically and with MRI) and the patient remains symptomatic after conservative therapy. A clear indication is given when the lateral condyle index is 86% or less. Lengthening is designed to create a longer proximal part of the lateral trochlear sulcus to improve the contact within the patellofemoral joint and to optimize the patellofemoral gliding mechanism. A longer lateral trochlea facet is the feature that must “capture” the patella in extension before the knee starts to flex, to ensure that it is guided into the more distal trochlear groove. Normally, the contact between the articular surface of the trochlea and the articular cartilage behind the patella is about one third of the length of the patellar cartilage (measured using the patellotrochlear index) [7]. This value is very helpful both in planning (using MRI) and during surgery to determine how much lengthening to the proximal should be performed.
Through a short parapatellar lateral incision (maximum 5 cm), the superficial retinaculum is localized. About 1 cm from the border of the patella it is longitudinally incised and carefully separated from the oblique part of the retinaculum in the posterior direction to allow lengthening of the lateral retinaculum at the end of surgery if needed [4]. The oblique part is cut, together with the synovial membrane. The patellofemoral joint is opened and the intraarticular inspection possible. Other pathologies can be identified and treated if necessary. The proximal shape of the lateral facet of the trochlea and the length of the articular cartilage are assessed with regards to the length of the sulcus and the medial facet of the trochlea (Fig. 26.7). The presence of a too short lateral articular facet is reconfirmed. In such a case, the patellotrochlear overlap is less than one third. The overlap present allows one to determine the amount of lengthening of the lateral facet and should be about one third at the end, measured in extension (0° of flexion) [4,7]. The incomplete lateral osteotomy is made at least 5 mm from the cartilage of the sulcus to prevent necrosis of the trochlea or breaking of the lateral facet. The osteotomy starts at the end of the cartilage (arrow) and is continued approximately 1–1.5cm distal into the femoral condyle and proximal into the femoral shaft, always according to the aimed patellofemoral overlapping (Fig. 26.10). The osteotomy is opened carefully with the use of a chisel. Fracture of the distal cartilage may occur and has no consequences; sharp edges must be smoothed. Cancellous bone (obtained through a small cortical opening of the lateral condyle more posterior) is inserted and impacted (Fig. 26.8). Additional fixation is possible using resorbable sutures. To finish, the lateral retinaculum is reconstructed in about 60° of knee flexion.
26.4.2 Elevation
Combined pathologies with a too short, but also a flat lateral facet of the trochlea can occur (Fig. 26.9). The surgical steps consist then of a lengthening osteotomy with additional elevation of the lateral facet. The approach is the same. The osteotomy is opened carefully and the lateral facet lifted up to the desired height (Fig. 26.10). The amount of elevation depends on the present pathomorphology. The lateral facet of the sulcus should be higher than the medial facet (Fig. 26.11). The anterior cortex of the femoral shaft serves as an orientation of the necessary elevation. In most cases 5–6 mm elevation are sufficient. Overcorrection (with hypercompression) must be strictly avoided. It also has to be considered that in five out of six cases the lateral condyle is not too flat, but the floor of the trochlea too high (8, 10). This would be visible on preoperative axial MR images.
Too short and flat lateral articular trochlea (arrow) (same patient as Fig. 26.6)
26.5 Postoperative Care
Partial weight bearing (10–20kg) is recommended for 3–4 weeks to avoid hypercompression of the osteotomy. Range of motion is limited (0°–90°) in the very beginning for some days to decrease swelling and pain. Continuous passive motion starts immediately to optimize the patellofemoral gliding mechanism and to form the reconstructed trochlea. Bicycling and swimming are the first sport activities allowed after 2–3 weeks. Sports activities without any restriction are permitted after 3 months.
26.6 Conclusions
The described too short lateral articular facet of the trochlea represents another type of trochlear dysplasia causing lateral patellar instability. Physical examination and MRI help to document this type of pathomorphology. The lateral condyle index is the most reliable measurement for the diagnosis. Index values 93% or more are normal, values of 86% or less pathologic and confirm the presence of a too short lateral facet. Surgical correction must address also in such cases the underlying abnormality. Lengthening is the surgical treatment of choice to improve the patellotrochlear overlapping and with this the stability. In cases with additional flat lateral facet, moderate elevation of the lateral trochlea may be necessary.
References
Albee FH (1915) The bone graft wedge in the treatment of habitual dislocation of the patella. Med Rec 88:257–259
Arendt E (2005) Anatomy and malalignment of the patellofemoral joint: its relation to patellofemoral arthrosis. Clin Orthop 436:71–75
Bereiter H, Gautier E (1994) Die Trochleaplastik als chirurgische Therapie der rezidivierenden Patellaluxation bei Trochleadysplasie des Femurs. Arthroskopie 7:281–286
Biedert RM (2004) Patellofemoral disorders: diagnosis and treatment. Wiley, New York
Biedert RM (2005) Measurements of the length of the proximal and distal trochlea and the trochlear depth on sagittal MRI in patients with lateral patellar subluxation. Proceedings of the International Patellofemoral Study Group meeting, Lausanne, Switzerland
Biedert RM (2006) Trochlea dysplasia: indications for trochleoplasty (deepening) and raising/shortening/lengthening of flat/short lateral trochlea. Proceedings of the International Patellofemoral Study Group meeting, Boston, MA, USA
Biedert RM, Albrecht S (2006) The patellotrochlear index: a new index for assessing patellar height. Knee Surg Sports Traumatol Arthrosc 14:707–712
Biedert RM, Bachmann M (2008) Trochlea dysplasia: too much or not enough? Proceedings of the International Patellofemoral Study Group meeting, Stellenbosch, South Africa
Biedert RM (2008) Osteotomien. Der Orthopäde 37: 872–883
Biedert RM, Bachmann M (2009) Anterior-posterior trochlear measurements of normal and dysplastic trochlea by axial magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc 17:1225–1230
Biedert RM, Netzer P, Gal I, Sigg A, Tscholl Ph (2009) The lateral condyle index: a new index for assessing the length of the lateral articular trochlea. Knee Surg Sports Traumatol Arthrosc (submitted)
Carrillon Y, Abidi H, Dejour D, Fantino O, Moyen B, Tran-Minh VA (2000) Patellar instability: assessment on MR images by measuring the lateral trochlear inclination – initial experience. Radiology 216:582–585
Dejour H, Walch G, Neyret P, Adeleine P (1990) Dysplasia of the femoral trochlea. Rev Chir Orthop Reparatrice Appar Mot 76:45–54
Dejour H, Walch G, Nove-Josserand L, Guier Ch (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2: 19–26
Dejour H, Walch G, Nove-Josserand L, Guier Ch (1994) Factors of patellar instability: an anatomoradiographic analysis. In: Feagin JA Jr (ed) The crucial ligaments. Diagnosis and treatment of ligament injuries about the knee. Churchill Livingstone, New York, pp 361–367
Dejour D, Locatelli E (2001) Patellar instability in adults. Surg Tech Orthop Traumatol 55:1–6
Dejour D, Le Coultre B (2007) Osteotomies in patellofemoral instabilities. Sports Med Arthrosc Rev 15:39–46
Donell ST, Joseph G, Hing CB, Marshall TJ (2006) Modified Dejour trochleoplasty for severe dysplasia: operative technique and early clinical results. Knee 13:266–273
Feinstein WK, Noble PC, Kamaric E, Tullos HS (1996) Anatomic alignment of the patellar groove. Clin Orthop 331: 64–73
Grelsamer RP, Tedder JL (1992) The lateral trochlear sign: femoral trochlear dysplasia as seen on a lateral view roentgenograph. Clin Othop 281:159–163
Kolowich PA, Paulos LE, Rosenberg TD, Farnsworth S (1990) Lateral release of the patella: indications and contraindications. Am J Sports Med 18:359–365
Malaghem J, Maldague B (1989) Depth insufficiency of the proximal trochlear groove on lateral radiographs of the knee: relation to patellar dislocation. Radiology 170: 507–510
Masse Y (1978) Trochleoplasty: restoration of the intercondylar groove in subluxations and dislocations of the patella. Rev Chir Orthop Reparatrice Appar Mot 64:3–17
Percy EC, Strother RT (1985) Patellalgia. Physician Sportsmed 13:43–59
Servien E, Neyret P, Si Selmi TA, Biedert RM (2004) Radiographs. In: Biedert RM (ed) Patellofemoral disorders: diagnosis and treatment. Wiley, New York, pp 87–100
Tavernier T, Dejour D (2001) Knee imaging: what is the best modality? J Radiol 82(387–405):407–408
Tecklenburg K, Dejour D, Hoser C, Fink C (2006) Bony and cartilaginous anatomy of the patellofemoral joint. Knee Surg Sports Traumatol Arthrosc 14:235–240
Van Huyssteen AL, Hendrix MRG, Barnett AJ, Wakeley CJ, Eldrige JDJ (2006) Cartilage-bone mismatch in the dysplastic trochlea. J Bone Joint Surg 88-B:688–691
Verdonk R, Jansegers E, Stuyts B (2005) Trochleoplasty in dysplastic knee trochlea. Knee Surg Sports Traumatol Arthrosc 13:529–533
Von Knoch E, Böhm T, Bürgi ML, Von Knoch M, Bereiter H (2006) Trochleoplasty for recurrent patellar dislocation in association with trochlear dysplasia. J Bone Joint Surg 88B:1331–1335
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2010 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Biedert, R.M. (2010). Trochlear Lengthening Osteotomy with or Without Elevation of the Lateral Trochlear Facet. In: Zaffagnini, S., Dejour, D., Arendt, E. (eds) Patellofemoral Pain, Instability, and Arthritis. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-05424-2_26
Download citation
DOI: https://doi.org/10.1007/978-3-642-05424-2_26
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-05423-5
Online ISBN: 978-3-642-05424-2
eBook Packages: MedicineMedicine (R0)