Abstract
Inborn errors of metabolism (IEMs) are a group of diseases involving a genetic defect that alters a metabolic pathway and that presents usually during infancy. The tyrosine degradation pathway contains five enzymes, four of which being associated with IEMs. The most severe metabolic disorder associated with this catabolic pathway is hereditary tyrosinemia type 1 (HT1; OMIM 276700). HT1 is an autosomal recessive disease caused by a deficiency of fumarylacetoacetate hydrolase (FAH), the last enzyme of the tyrosine catabolic pathway. Although a rare disease worldwide, HT1 shows higher incidence in certain populations due to founder effects. The acute form of the disease is characterized by an early onset and severe liver failure while the chronic form appears later and also involves renal dysfunctions. Until 1992 the only treatment for this disease was liver transplantation. Since then, NTBC/Nitisone (a drug blocking the pathway upstream of FAH) is successfully used in combination with a diet low in tyrosine and phenylalanine, but patients are still at risk of developing hepatocellular carcinoma. This chapter summarizes the biochemical and clinical features of HT1.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Hereditary tyrosinemia type 1 (HT1)
- Fumarylacetoacetate hydrolase (FAH)
- Liver
- Kidney
- Hepatocellular carcinoma
1 Introduction
Inborn errors of metabolism (IEMs) are a group of diseases (more than 400) in which a single gene defect causes a block in a metabolic pathway resulting either in the accumulation of unwanted metabolites or in product deficiency. Most IEMs disorders present early in life although milder forms may remain undetected until adulthood. Individually they are rare, but collectively they are common. In Canada, the incidence of IEMs is estimated at 40/100,000 live births (Applegarth et al. 2000).
IEMs are classified according to their clinical features, the type of enzyme involved and their pattern of inheritance. They include genetic defects that alter amino acids, lipid and carbohydrate metabolisms in addition to mucopolysaccharidoses, purine and pyrimidine disorders and porphyrias.
Amino acids are the building blocs of proteins and are a source of nitrogen for biologically important compounds such as hormones and neurotransmitters. Many IEMs alter amino acid metabolism such as alkaptonuria, maple syrup urine disease and homocystinuria. This chapter focusses on the most severe metabolic disorder of the tyrosine catabolic pathway, hereditary tyrosinemia type 1 (HT1; OMIM 276700) (Mitchell et al. 2001; Sniderman King et al. 2006) and is aimed at describing the general biochemical and clinical aspects of this disease.
2 Phenylalanine and Tyrosine
Phenylalanine and tyrosine only differ by the presence of an – OH group attached to the benzene ring (Fig. 2.1). Hence, tyrosine is also known as 4-hydroxyphenylalanine. Phenylalanine normally has two fates in cells: incorporation into polypeptide chains and hydroxylation to tyrosine via phenylalanine hydroxylase (PAH). Therefore phenylalanine degradation follows the tyrosine catabolic pathway.
Tyrosine is involved in protein biosynthesis and is also a precursor for neurotransmitters and hormones. Indeed, tyrosine is involved in epinephrine, melanin and thyroxine synthesis among others. Together with phenylalanine, they are considered glucogenic and ketogenic amino acids due to the products yield by their degradation.
2.1 Tyrosine Catabolism
The tyrosine degradation pathway involves five enzymes that ultimately lead to the conversion of tyrosine into fumarate and acetoacetate (Fig. 2.2). The first step is catalyzed by tyrosine aminotransferase (TAT) and consists in the transformation of tyrosine in 4-hydroxyphenylpyruvic acid. TAT uses α-ketoglutarate as the amino acceptor, which leads to the generation of glutamate. The second step is performed by p-hydroxyphenylpyruvate dioxygenase (HPD), which catalyzes the oxidation of 4-hydroxyphenylpyruvic acid to homogentisic acid (HGA). This product is then oxidized by the homogentisate oxidase (HGO) into 4-maleylacetoacetate (MAA). The fourth enzyme of the pathway is the maleylacetoacetate isomerase (MAAI, also known as glutathione S-transferase zeta (ζ) 1 (GSTZ1)), which converts MAA in 4-fumarylacetoacetate (FAA). The final step consists in the cleavage of FAA in fumarate and acetoacetate by fumarylacetoacetate hydrolase (FAH). The fumarate end product of tyrosine catabolism feeds directly the tricarboxylic acid (TCA) cycle while the acetoacetate is activated to acetoacetyl-CoA via succinyl-CoA:3-oxoacid-CoA transferase (mitochondria) or acetoacetyl-CoA synthetase (cytosol). Acetoacetyl-CoA is involved in the mevalonate pathway and has a role in cholesterol biosynthesis as well as in ketogenesis.
Tyrosine degradation pathway. Enzymatic steps of the tyrosine catabolic pathway. Each enzyme is abbreviated and the corresponding IEM is written near the “no” symbol. The conversion of 4-maleylacetoacetate (MAA) and 4-fumarylacetoacetate (FAA) into succinylacetoacetate (SAA) and then succinylacetone (SA) is depicted as well as the inhibitory effect of SA on ALAD. The site of action of NTBC is also indicated. TAT tyrosine aminotransferase, HPD p-hydroxyphenylpyruvate dioxygenase, HGO homogentisate oxidase, MAAI maleylacetoacetate isomerase, FAH fumarylacetoacetate hydrolase, TCA cycle tricarboxylic acid cycle, ALAD δ-aminolevulic acid dehydratase
2.2 Diseases Associated with Enzymes of the Tyrosine Catabolic Pathway
Of the five enzymes involved in tyrosine catabolism, four are implicated in autosomal recessive metabolic disorders (IEMs) and seven diseases have been reported to be associated with this catabolic pathway (Table 2.1).
The defect of TAT, the first enzyme of the tyrosine degradation pathway, leads to hereditary tyrosinemia type 2 (HT2, OMIM 276600) (also called Richner-Hanhart syndrome) (Table 2.1). HT2 is associated with elevated tyrosine levels in both blood and urine. The clinical phenotype of HT2 includes mental retardation, painful corneal eruptions, photophobia, keratitis, and painful palmoplantar hyperkeratosis (Natt et al. 1992).
Mutations abolishing HPD function, the second enzyme of the pathway, can result in Hawkinsinuria (OMIM 140350) or hereditary tyrosinemia type 3 (HT3, OMIM 276710) (Table 2.1). Hawkinsinuria develops when only one HPD allele is mutated (dominant IEM) while HT3 occurs when both HPD alleles are affected (recessive IEM) (Tomoeda et al. 2000). Hawkinsinuria is associated with transient metabolic acidosis and hypertyrosinemia. The symptoms improve within the first year of life but patients excrete hawkinsin in their urine throughout life (Niederwieser et al. 1977; Wilcken et al. 1981). HT3 is a very rare disease with clinical phenotype including mild mental retardation and/or convulsions, and noteworthy, the absence of liver damage (Tomoeda et al. 2000). Of note, a delay in HPD maturation results in transient tyrosinemia of the newborn. This condition is benign and disappears spontaneously with no sequelae (Mitchell et al. 2001; Russo et al. 2001).
A defect of HGO, the third enzyme of the pathway, leads to the first IEM ever recognized, alkaptonuria (AKU, OMIM 203500) (Garrod 1902). This disease is not life-threatening and the usual consequences are ochronosis (bluish-black discoloration of the tissues) and arthritis (reviewed in (Vilboux et al. 2009)). The accumulation of HGA also causes the urine to darken on exposure to air.
Up to now, a deficiency in MAAI has been suggested twice in literature but it has not been clearly confirmed (Karnik et al. 2004; Fernandez-Canon et al. 2002) (OMIM gene ID: 603758). In both cases, patient developed liver failure and kidney dysfunction similar to hereditary tyrosinemia type 1 (HT1, see below) but with absence of SA accumulation and the corresponding disease was therefore called HT1 type b (HT1b). It remains unclear if MAAI deficiency actually exists in human patients, especially since there is an enzyme-independent bypass that allows the isomerization of MAA in FAA (Fernandez-Canon et al. 2002).
Finally, the defect of the last enzyme of the pathway (FAH) causes HT1 (OMIM 276700), which is a severe progressive liver disease coupled with renal tubular dysfunction (Lindblad et al. 1977; Mitchell et al. 2001; Russo et al. 2001). HT1 is the most severe disease associated to the tyrosine catabolism pathway.
3 HT1 Incidence
The incidence of HT1 is around 1/100,000 births worldwide but can be much higher in certain regions due to founder effects (reviewed in (Angileri et al. 2015)). The highest incidence of HT1 is found in the region of Saguenay-Lac-St-Jean (SLSJ) (Quebec Province, Canada), where 1:1846 children has HT1 and 1:22 individual is a carrier of a disease allele (De Braekeleer and Larochelle 1990; Grompe et al. 1994; Poudrier et al. 1996) (See Larochelle, Chap. 1). The splice mutation c.1062 + 5G>A (IVS12 + 5G→A) is the most frequently found mutation within this population (~90% of the HT1 reported allele) and accounts for approximately one third of all HT1 reported alleles worldwide (Grompe et al. 1994; Poudrier et al. 1996; St-Louis and Tanguay 1997; Angileri et al. 2015).
A second mutation cluster of HT1 is found in Scandinavia, most precisely in the Finnish population of Pohjanmaa where 1/5000 individual is affected by HT1 while the overall incidence of HT1 in Finland is 1/60,000 (Kvittingen et al. 1981; Mustonen et al. 1997; St-Louis et al. 1994). The most frequent HT1 reported allele in Finland is c.786G>A (p.W262X) which represents ~88% of the reported alleles in nine out of ten alleles in this country (St-Louis et al. 1994). A third cluster of HT1 occurs in an immigrant population from Pakistan living predominantly in Birmingham (United Kingdom) (Hutchesson et al. 1998). HT1 alleles have been reported all over the world except in Central America and on the Oceania continent (Angileri et al. 2015) (See Morrow et al. Chap. 3).
4 FAH, the Deficient Enzyme in HT1
The FAH gene is located on the long arm of chromosome 15 at position 25.1 (15q25.1; base pairs 80,152,890 to 80,186,581) (Phaneuf et al. 1991). The corresponding protein (FAH, E.C. 3.7.1.2) is a metalloenzyme for which the structure has been determined by crystallography (Timm et al. 1999; Tanguay 2002; Bateman et al. 2007; Bateman et al. 2001). FAH is a cytosolic homodimeric enzyme of two 46 kDa subunits, which is mainly expressed in liver and kidneys. It is also expressed in other tissues, such as fibroblasts, amniocytes, chorionic villi, erythrocytes and oligodendrocytes, albeit at a lower level. As the last enzyme of the tyrosine catabolic pathway, FAH catalyzes the conversion of FAA into fumarate and acetoacetate (Phaneuf et al. 1992; Tanguay et al. 1990) (Fig. 2.2).
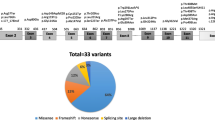
Ninety-eight mutations have been reported to cause HT1 and their occurrence worldwide has been recently compiled (Angileri et al. 2015). The most common FAH mutation causing HT1 are c.1062 + 5G>A (IVS12 + 5G>A) followed by c.554-1G>T (IVS6-1G > T) and c.786G > A (p.W262X) (See Morrow et al. Chap. 3).
5 Biochemical Features of HT1
The deficiency of FAH was originally associated with increased levels of hepatic transaminases, as well as increased plasma levels of tyrosine, methionine and phenylalanine and with urinary elevated concentrations of tyrosine metabolites (p-hydroxyphenylpyruvate, p-hydroxyphenyllactate and p-hydroxyphenylacetate) (Table 2.2). Hypertyrosinemia can be caused by numerous other conditions affecting the liver and is also a feature of transient tyrosinemia of the newborn, a condition that resolves spontaneously without significant damages (Mitchell et al. 2001; Russo et al. 2001) (Table 2.1).
HT1 patients usually present with high levels of plasma α-fetoprotein (AFP) and most importantly with high levels of succinylacetone in plasma and urine (SA) the only valid prognosis marker of HT1. The latter metabolite is widely used for HT1 screening and its presence can be directly linked to the lack of FAH activity. Indeed, the absence of FAH results in the accumulation of FAA and MAA, which are then reduced in succinylacetoacetate (SAA) (Fig. 2.2). The subsequent decarboxylation of SAA is responsible of the observed succinylacetone (SA).
FAA and SA are the most damaging metabolites resulting from FAH deficiency and considerable efforts have been made to find by which molecular mechanisms these compounds act to produce the severe phenotype seen in HT1 (See Tanguay et al. Chap. 4).
5.1 Overview of FAA Toxicity
FAA is an electrophilic compound that has been suggested to damage DNA. While a direct effect on DNA remains to be demonstrated, it was shown to be mutagenic in a cell assay, albeit at a much lower level than classical mutagens (Tanguay et al. 1996). FAA induces genome instability through activation of the ERK pathway (Jorquera and Tanguay 2001). Moreover, it induces cell cycle arrest and apoptosis through glutathione (GSH) depletion (Jorquera and Tanguay 1997, 2001). Hence, GSH, a major actor of redox homeostasis, was shown to reduce FAA mutagenicity in cultured cells (Jorquera and Tanguay 1997, 2001) and to rescue neonatal death in the fah knockout model of HT1 (Langlois et al. 2008). At the cellular level, the stress caused by FAA accumulation was also shown to induce the unfolding protein response (UPR) in the endoplasmic reticulum (Bergeron et al. 2006).
In an interesting study, FAA was shown to inhibit 6 of the 7 human DNA glycosylases involved in DNA base removal during base excision repair (BER) (Bliksrud et al. 2013). This is in agreement with a previous report showing that the expression of DNA glycosylase OGG1 and the nucleotide excision repair protein ERCC1, was reduced in lymphocytes of two HT1 patients (van Dyk et al. 2010). Preventing DNA repair by the BER pathway, would favor accumulation of oxidative damage to DNA resulting in increased potent mutagenic lesions. Noteworthy, GSH depletion due to FAA accumulation is likely to affect DNA repair indirectly as redox homeostasis is also important for this process (Langie et al. 2007; Storr et al. 2012).
5.2 Overview of SA Toxicity
Contrary to FAA, SA has no mutagenic effect on DNA (Tanguay et al. 1996) nor was it shown to have any inhibiting effect on human DNA glycosylases (Bliksrud et al. 2013).
The toxicity of SA mostly relies on its ability to be a competitive inhibitor of δ-aminolevulinic acid dehydratase (ALAD), the enzyme responsible of the conversion of δ-aminolevulinic acid (ALA) in porphobilinogen, which is precursor of heme synthesis (Fig. 2.2). This inhibition results in the accumulation of ALA and its excretion in urine. ALA has been associated with mitochondrial toxicity, liver toxicity, liver cancer, and neuropshychiatric problems. Indeed, it lowers heme levels for cytochrome/hemoproteins synthesis and increases mitochondrial iron levels, resulting in heme deficiency, down regulation of mitochondrial cytochrome oxidase and overall mitochondrial toxicity (reviewed in (Lee and O’Brien 2010)). Accordingly, SA is widely used as a heme synthesis inhibitor to create a mitochondrial iron-loading model that is similar to the mitochondrial iron loading found in Friedreich’s ataxia (Lee and O’Brien 2010; Richardson et al. 2001).
At the tissue level, SA causes dysfunction of kidney membrane transport by altering membrane fluidity and possibly disrupting normal structure. Indeed, it was shown to cause renal tubular dysfunction in normal rat kidneys, mimicking human Fanconi syndrome (Roth et al. 1991; Wyss et al. 1992; Tanguay et al. 2009).
6 Clinical Features of HT1
HT1 is characterized by progressive liver disease and renal tubular dysfunction leading to hypophosphatemic rickets. Moreover, it is the IEM with the highest incidence of hepatocellular carcinoma (HCC) (Schady et al. 2015) (Table 2.3). HT1 is categorized into three main clinical types (acute, subacute and chronic) based on the age of onset and the clinical manifestations (Tanguay et al. 1990; Mitchell et al. 2001; van Spronsen et al. 1994).
6.1 Acute, Subacute and Chronic Forms of HT1
The acute form of HT1 has an onset before 2 months of age and is mainly characterized by severe liver failure associated with cirrhosis, hepato- and spleno-megaly, abnormal blood coagulation and hypoglycemia leading to death in the first months of life (Table 2.3). Renal tubular dysfunctions such as Fanconi syndrome and rickets have also been considered hallmarks of HT1 (Mitchell et al. 2001; Russo et al. 2001). The subacute form is similar to the acute form but symptoms appear between 2 and 6 months (van Spronsen et al. 1994) (Table 2.3).
The chronic form is initially less aggressive and presents after 6 months of age. While its onset is insidious and progressive, renal manifestations, such as proximal tubulopathy, are prominent and may even be the presenting problem (Table 2.3). Patients show impaired renal tubular reabsorption functions leading to Fanconi syndrome, renal tubular acidosis, generalized aminoaciduria, hypophosphatemic vitamin D-resistant rickets and growth retardation (Paradis et al. 1990; Russo and O’Regan 1990; Fernandez-Lainez et al. 2014; Forget et al. 1999).
6.2 High Incidence of HCC in HT1
HT1 is characterized by gradual liver alterations leading to cirrhosis and HCC development. In fact, the risk of developing HCC in HT1 is considered the highest among all metabolic disorders (Russo et al. 2001; Schady et al. 2015). In an early study, HCC was reported in 37% of HT1 patients over 2 years of age (Weinberg et al. 1976) but subsequent studies in Scandinavia (van Spronsen et al. 1989) and in Quebec (Russo et al. 2001) showed a lower frequency of HCC (~15%) likely due to the advent of transplantation and improved treatment. In addition to be at high risk of developing HCC, HT1 patients develop them earlier then patients having other diseases (often before 5 years of age) (Schady et al. 2015) (See van Ginkel et al. Chap. 9).
7 Diagnosis of HT1
As mentioned above, the deficiency of FAH gives rise to elevated plasma concentrations of amino acids such as tyrosine and methionine as well as excretion of unusual tyrosine metabolites like SA (Mitchell et al. 2001; Russo et al. 2001) (Table 2.2). Although elevated levels of tyrosine and plasma AFP are indicative of HT1, the most reliable biochemical diagnostic marker consists in the presence of SA in urine, blood and amniotic fluid (Grenier et al. 1976; Grenier et al. 1982). In Quebec, where a high incidence of HT1 is observed, a neonatal screening program for the disease has been established in 1970 and consists of measuring SA levels in dried blood spots. Tandem mass spectrometry (MS/MS) is now used as a sensitive and rapid method, for screening HT1 by measuring the level of SA (Allard et al. 2004). Prenatal biochemical diagnosis can also be done by measuring the level of SA in amniotic fluid sampled between the 14th and 16th weeks of pregnancy (Grenier et al. 1996; Jakobs et al. 1990). However, some false-positives have been reported using this method.
An enzymatic assay based on FAH activity measurements on cultured fibroblasts, blood, or liver specimen has also been used for diagnosis (Kvittingen et al. 1981, 1983). However, this method is less reliable on liver specimen as some HT1 patients have mosaic expression of FAH in their liver due to reversion of the mutation (Demers et al. 2003; Kvittingen et al. 1993, 1994; Poudrier et al. 1998).
Genetic diagnosis tests are also performed when the family history or the origin of the patient suggests that one parent may be a carrier of the disorder. This kind of test has been facilitated by the technological progress achieved in the past decade and the identification of predominant mutations in certain ethnic groups (Angileri et al. 2015). The best example of this is the genetic screening test that was designed to detect the most common mutation found in HT1 (c.1062 + 5G>A, IVS12 + 5G→A) (Grompe and al-Dhalimy 1995). The method is based on the amplification of the genomic DNA region containing the mutation by PCR followed by enzymatic cleavage of the amplified sequence in order to distinguish the mutated allele from the wild-type sequence. Similar molecular tests have since been developed for most mutations and can be performed on blood, chorionic villi or cultured amniocytes. However, with the improvement of new sequencing technologies, it is becoming very simple to perform the FAH gene sequencing.
8 Treatment of HT1
8.1 Restrictive Diet
Before 1990s, there was no treatment available for HT1 except liver transplantation. Patients were following a restrictive diet with low phenylalanine and tyrosine intake. While this was beneficial at the beginning, it was not fully preventing ulterior liver damage and renal dysfunction.
8.2 Orthotopic Liver Transplantation
Orthotopic liver transplantation (OLT) is performed in the most severe HT1 cases due to the risks associated to the surgery. OLT is essentially curative but does not fully correct metabolic perturbations in HT1 since kidneys continue to excrete SAA, SA and ALA in urine (Fernandez-Lainez et al. 2014; Tuchman et al. 1987; Pierik et al. 2005; Bartlett et al. 2013). Only half of liver transplanted patients show partial improvement of renal function but still, altered kidney size and architecture persists (Paradis et al. 1990; Fernandez-Lainez et al. 2014; Forget et al. 1999) (See Alvarez and Mitchell Chap. 5 and McKiernan Chap. 7 on liver transplantation).
8.3 NTBC
NTBC (2-(2-nitro-4-trifluoro-methylbenzyol)-1,3 cyclohexanedione, Nitisinone) was first used in 1992 (Lindstedt et al. 1992). It acts by inhibiting the second enzyme of the tyrosine catabolic pathway, HPD (Fig. 2.2). The advantage of blocking the pathway at this step is that there is no accumulation of FAA and MAA and therefore no accumulation of SA either. Moreover, as mentioned in Sect. 2.2 no liver damages are associated with inhibition of HPD in HT3.
The use of NTBC combined to the low tyrosine/phenylalanine diet has proven to be very efficient in preventing HT1 progression, by curing both liver and kidney dysfunctions (Larochelle et al. 2012; Bartlett et al. 2014). It is very efficient particularly when introduced early in life (Larochelle et al. 2012), but it is still unsure if it will be sufficient to prevent problems on a long-term basis. For instance, failure to respond to NTBC has been reported in one child (Mohan et al. 1999) and high risks of HCC have been reported when NTBC is introduced after 2 years of age (McKiernan 2006; van Spronsen et al. 2005) (for more information on NTBC see Maiorana and Dionisi-Vici Chap. 8 and Lock Chap. 16).
9 Concluding Remarks
HT1 is a severe liver disease that should be detected at the earliest to be treated effectively. The management of this disease has been revolutionised by the introduction of NTBC (de Laet et al. 2013), but the venue of alternative/complementary treatments will be of upmost importance due to difficulties to fully comply to the restrictive diet for some patients and the high cost of NTBC. It is also important to favor newborn screening programs for the early detection of HT1 patients whenever possible. Such screening is inexpensive and should prevent late intervention when liver damage has already been done. Finally additional basic research is still needed to unveil the pathogenic mechanisms involved in HT1.
Abbreviations
- ALA:
-
δ-aminolevulinic acid
- ALAD:
-
δ-aminolevulinic acid dehydratase
- BER:
-
Base excision repair
- FAA:
-
Fumaryl acetoacetate
- FAH:
-
Fumarylacetoacetate hydrolase
- GSH:
-
Glutathione
- HCC:
-
Hepatocellular carcinoma
- HGA:
-
Homogentisic acid
- HGO:
-
Homogentisic acid oxidase
- HPD:
-
p-hydroxyphenylpyruvate dioxygenase
- HT1:
-
Hereditary tyrosinemia
- IEM:
-
Inborn errors of metabolism
- MAA:
-
Maleyl acetoacetate
- MAAI:
-
Maleyl acetoacetate isomerase also known as (ζ) 1 GSTZ1
- OLT:
-
Orthotopic liver transplantation
- PAH:
-
Phenylalanine hydroxylase
- SAA:
-
Succinylacetone
- TAT:
-
Tyrosine aminotransferase
- TCA:
-
Trichloroacetic acid cycle
References
Allard P, Grenier A, Korson MS, Zytkovicz TH (2004) Newborn screening for hepatorenal tyrosinemia by tandem mass spectrometry: analysis of succinylacetone extracted from dried blood spots. Clin Biochem 37(11):1010–1015. doi:S0009-9120(04)00202-4
Angileri F, Bergeron A, Morrow G, Lettre F, Gray G, Hutchin T, Ball S (2015) Geographical and ethnic distribution of mutations of the fumarylacetoacetate hydrolase gene in hereditary tyrosinemia type 1. JIMD Rep 19:45–58. doi:10.1007/8904_2014_363
Applegarth DA, Toone JR, Lowry RB (2000) Incidence of inborn errors of metabolism in British Columbia, 1969–1996. Pediatrics 105(1):e10
Bartlett DC, Preece MA, Holme E, Lloyd C, Newsome PN, McKiernan PJ (2013) Plasma succinylacetone is persistently raised after liver transplantation in tyrosinaemia type 1. J Inherit Metab Dis 36(1):15–20. doi:10.1007/s10545-012-9482-1
Bartlett DC, Lloyd C, McKiernan PJ, Newsome PN (2014) Early nitisinone treatment reduces the need for liver transplantation in children with tyrosinaemia type 1 and improves post-transplant renal function. J Inherit Metab Dis 37(5):745–752. doi:10.1007/s10545-014-9683-x
Bateman RL, Bhanumoorthy P, Witte JF, McClard RW, Grompe M, Timm DE (2001) Mechanistic inferences from the crystal structure of fumarylacetoacetate hydrolase with a bound phosphorus-based inhibitor. J Biol Chem 276(18):15284–15291. doi:10.1074/jbc.M007621200
Bateman RL, Ashworth J, Witte JF, Baker LJ, Bhanumoorthy P, Timm DE, Hurley TD, Grompe M, McClard RW (2007) Slow-onset inhibition of fumarylacetoacetate hydrolase by phosphinate mimics of the tetrahedral intermediate: kinetics, crystal structure and pharmacokinetics. Biochem J 402(2):251–260. doi:10.1042/BJ20060961
Bergeron A, Jorquera R, Orejuela D, Tanguay RM (2006) Involvement of endoplasmic reticulum stress in hereditary tyrosinemia type I. J Biol Chem 281(9):5329–5334. doi:M506804200
Bliksrud YT, Ellingsen A, Bjoras M (2013) Fumarylacetoacetate inhibits the initial step of the base excision repair pathway: implication for the pathogenesis of tyrosinemia type I. J Inherit Metab Dis 36(5):773–778. doi:10.1007/s10545-012-9556-0
De Braekeleer M, Larochelle J (1990) Genetic epidemiology of hereditary tyrosinemia in Quebec and in Saguenay-Lac-St-Jean. Am J Hum Genet 47(2):302–307
de Laet C, Dionisi-Vici C, Leonard JV, McKiernan P, Mitchell G, Monti L, de Baulny HO, Pintos-Morell G, Spiekerkotter U (2013) Recommendations for the management of tyrosinaemia type 1. Orphanet J Rare Dis 8:8. doi:1750-1172-8-8
Demers SI, Russo P, Lettre F, Tanguay RM (2003) Frequent mutation reversion inversely correlates with clinical severity in a genetic liver disease, hereditary tyrosinemia. Hum Pathol 34(12):1313–1320. doi:S0046817703004064
Fernandez-Canon JM, Baetscher MW, Finegold M, Burlingame T, Gibson KM, Grompe M (2002) Maleylacetoacetate isomerase (MAAI/GSTZ)-deficient mice reveal a glutathione-dependent nonenzymatic bypass in tyrosine catabolism. Mol Cell Biol 22(13):4943–4951
Fernandez-Lainez C, Ibarra-Gonzalez I, Belmont-Martinez L, Monroy-Santoyo S, Guillen-Lopez S, Vela-Amieva M (2014) Tyrosinemia type I: clinical and biochemical analysis of patients in Mexico. Ann Hepatol 13(2):265–272. doi:1090941
Forget S, Patriquin HB, Dubois J, Lafortune M, Merouani A, Paradis K, Russo P (1999) The kidney in children with tyrosinemia: sonographic, CT and biochemical findings. Pediatr Radiol 29(2):104–108
Garrod AE (1902) About alkaptonuria. Med-Chir Trans 85:69–78
Grenier A, Belanger L, Laberge C (1976) alpha1-Fetoprotein measurement in blood spotted on paper: discriminating test for hereditary tyrosinemia in neonatal mass screening. Clin Chem 22(7):1001–1004
Grenier A, Lescault A, Laberge C, Gagne R, Mamer O (1982) Detection of succinylacetone and the use of its measurement in mass screening for hereditary tyrosinemia. Clin Chim Acta 123(1–2):93–99
Grenier A, Cederbaum S, Laberge C, Gagne R, Jakobs C, Tanguay RM (1996) A case of tyrosinaemia type I with normal level of succinylacetone in the amniotic fluid. Prenat Diagn 16(3):239–242. doi:10.1002/(SICI)1097-0223(199603)16:3<239::AID-PD829>3.0.CO;2-W
Grompe M, Al-Dhalimy M (1995) Rapid nonradioactive assay for the detection of the common French Canadian tyrosinemia type I mutation. Hum Mutat 5(1):105. doi:10.1002/humu.1380050117
Grompe M, St-Louis M, Demers SI, al-Dhalimy M, Leclerc B, Tanguay RM (1994) A single mutation of the fumarylacetoacetate hydrolase gene in French Canadians with hereditary tyrosinemia type I. N Engl J Med 331(6):353–357. doi:10.1056/NEJM199408113310603
Hutchesson AC, Bundey S, Preece MA, Hall SK, Green A (1998) A comparison of disease and gene frequencies of inborn errors of metabolism among different ethnic groups in the West Midlands, UK. J Med Genet 35(5):366–370
Jakobs C, Stellaard F, Kvittingen EA, Henderson M, Lilford R (1990) First-trimester prenatal diagnosis of tyrosinemia type I by amniotic fluid succinylacetone determination. Prenat Diagn 10(2):133–134
Jorquera R, Tanguay RM (1997) The mutagenicity of the tyrosine metabolite, fumarylacetoacetate, is enhanced by glutathione depletion. Biochem Biophys Res Commun 232(1):42–48. (47). doi:http://dx.doi.org/10.1006/bbrc.1997.6220
Jorquera R, Tanguay RM (2001) Fumarylacetoacetate, the metabolite accumulating in hereditary tyrosinemia, activates the ERK pathway and induces mitotic abnormalities and genomic instability. Hum Mol Genet 10(17):1741–1752
Karnik D, Thomas N, Eapen CE, Jana AK, Oommen A (2004) Tyrosinemia type I: a clinico-laboratory case report. Indian J Pediatr 71(10):929–932
Kvittingen EA, Jellum E, Stokke O (1981) Assay of fumarylacetoacetate fumarylhydrolase in human liver-deficient activity in a case of hereditary tyrosinemia. Clin Chim Acta 115(3):311–319
Kvittingen EA, Halvorsen S, Jellum E (1983) Deficient fumarylacetoacetate fumarylhydrolase activity in lymphocytes and fibroblasts from patients with hereditary tyrosinemia. Pediatr Res 17(7):541–544. doi:10.1203/00006450-198307000-00005
Kvittingen EA, Rootwelt H, Brandtzaeg P, Bergan A, Berger R (1993) Hereditary tyrosinemia type I. Self-induced correction of the fumarylacetoacetase defect. J Clin Invest 91(4):1816–1821. doi:10.1172/JCI116393
Kvittingen EA, Rootwelt H, Berger R, Brandtzaeg P (1994) Self-induced correction of the genetic defect in tyrosinemia type I. J Clin Invest 94(4):1657–1661. doi:10.1172/JCI117509
Langie SA, Knaapen AM, Houben JM, van Kempen FC, de Hoon JP, Gottschalk RW, Godschalk RW, van Schooten FJ (2007) The role of glutathione in the regulation of nucleotide excision repair during oxidative stress. Toxicol Lett 168(3):302–309. doi:S0378-4274(06)01335-X
Langlois C, Jorquera R, Orejuela D, Bergeron A, Finegold MJ, Rhead WJ, Tanguay RM (2008) Rescue from neonatal death in the murine model of hereditary tyrosinemia by glutathione monoethylester and vitamin C treatment. Mol Genet Metab 93(3):306–313. doi:S1096-7192(07)00441-6
Larochelle J, Alvarez F, Bussieres JF, Chevalier I, Dallaire L, Dubois J, Faucher F, Fenyves D, Goodyer P, Grenier A, Holme E, Laframboise R, Lambert M, Lindstedt S, Maranda B, Melancon S, Merouani A, Mitchell J, Parizeault G, Pelletier L, Phan V, Rinaldo P, Scott CR, Scriver C, Mitchell GA (2012) Effect of nitisinone (NTBC) treatment on the clinical course of hepatorenal tyrosinemia in Quebec. Mol Genet Metab 107(1–2):49–54. doi:S1096-7192(12)00211-9
Lee O, O’Brien PJ (2010) Modifications of mitochondrial function by toxicants. In: CA MQ (ed) Comprehensive toxicology. Elsevier, Oxford, pp 411–445
Lindblad B, Lindstedt S, Steen G (1977) On the enzymic defects in hereditary tyrosinemia. Proc Natl Acad Sci U S A 74(10):4641–4645
Lindstedt S, Holme E, Lock EA, Hjalmarson O, Strandvik B (1992) Treatment of hereditary tyrosinaemia type I by inhibition of 4-hydroxyphenylpyruvate dioxygenase. Lancet 340(8823):813–817. doi:0140-6736(92)92685-9
McKiernan PJ (2006) Nitisinone in the treatment of hereditary tyrosinaemia type 1. Drugs 66(6):743–750. doi:6662
Mitchell GA, Grompe M, Lambert H, Tanguay RM (2001) Hypertyrosinemia. In: Scriver C, Beaudet A, Sly WSJ, Valle D (eds) The metabolic and molecular bases of inherited diseases, vol II, 8th edn. McGrawHill, New York, pp 1777–1805
Mohan N, McKiernan P, Preece MA, Green A, Buckels J, Mayer AD, Kelly DA (1999) Indications and outcome of liver transplantation in tyrosinaemia type 1. Eur J Pediatr 158(Suppl 2):S49–S54. doi:9158S049.431
Mustonen A, Ploos van Amstel HK, Berger R, Salo MK, Viinikka L, Simola KO (1997) Mutation analysis for prenatal diagnosis of hereditary tyrosinaemia type 1. Prenat Diagn 17(10):964–966. doi:10.1002/(SICI)1097-0223(199710)17:10<964::AID-PD164>3.0.CO;2-6
Natt E, Kida K, Odievre M, Di Rocco M, Scherer G (1992) Point mutations in the tyrosine aminotransferase gene in tyrosinemia type II. Proc Natl Acad Sci U S A 89(19):9297–9301
Niederwieser A, Matasovic A, Tippett P, Danks DM (1977) A new sulfur amino acid, named hawkinsin, identified in a baby with transient tyrosinemia and her mother. Clin Chim Acta 76(3):345–356
Paradis K, Weber A, Seidman EG, Larochelle J, Garel L, Lenaerts C, Roy CC (1990) Liver transplantation for hereditary tyrosinemia: the Quebec experience. Am J Hum Genet 47(2):338–342
Phaneuf D, Labelle Y, Berube D, Arden K, Cavenee W, Gagne R, Tanguay RM (1991) Cloning and expression of the cDNA encoding human fumarylacetoacetate hydrolase, the enzyme deficient in hereditary tyrosinemia: assignment of the gene to chromosome 15. Am J Hum Genet 48(3):525–535
Phaneuf D, Lambert M, Laframboise R, Mitchell G, Lettre F, Tanguay RM (1992) Type 1 hereditary tyrosinemia. Evidence for molecular heterogeneity and identification of a causal mutation in a French Canadian patient. J Clin Invest 90(4):1185–1192. doi:10.1172/JCI115979
Pierik LJ, van Spronsen FJ, Bijleveld CM, van Dael CM (2005) Renal function in tyrosinaemia type I after liver transplantation: a long-term follow-up. J Inherit Metab Dis 28(6):871–876. doi:10.1007/s10545-005-0059-0
Poudrier J, St-Louis M, Lettre F, Gibson K, Prevost C, Larochelle J, Tanguay RM (1996) Frequency of the IVS12 + 5G-->A splice mutation of the fumarylacetoacetate hydrolase gene in carriers of hereditary tyrosinaemia in the French Canadian population of Saguenay-Lac-St-Jean. Prenat Diagn 16(1):59–64. doi:10.1002/(SICI)1097-0223(199601)16:1<59::AID-PD810>3.0.CO;2-D
Poudrier J, Lettre F, Scriver CR, Larochelle J, Tanguay RM (1998) Different clinical forms of hereditary tyrosinemia (type I) in patients with identical genotypes. Mol Genet Metab 64(2):119–125. doi:S1096-7192(98)92695-6
Richardson DR, Mouralian C, Ponka P, Becker E (2001) Development of potential iron chelators for the treatment of Friedreich’s ataxia: ligands that mobilize mitochondrial iron. Biochim Biophys Acta 1536(2–3):133–140
Roth KS, Carter BE, Higgins ES (1991) Succinylacetone effects on renal tubular phosphate metabolism: a model for experimental renal Fanconi syndrome. Proc Soc Exp Biol Med 196(4):428–431
Russo P, O’Regan S (1990) Visceral pathology of hereditary tyrosinemia type I. Am J Hum Genet 47(2):317–324
Russo PA, Mitchell GA, Tanguay RM (2001) Tyrosinemia: a review. Pediatr Dev Pathol 4(3):212–221
Schady DA, Roy A, Finegold MJ (2015) Liver tumors in children with metabolic disorders. Transl Pediatr 4(4):290–303. doi:10.3978/j.issn.2224-4336.2015.10.08
Sniderman King L, Trahms C, Scott CR (2006 ) Tyrosinemia type 1. In: Pagon RA, Adam MP, Bird TD, Dolan CR, Fong CT, Stephens K (eds). doi:http://www.ncbi.nlm.nih.gov/books/NBK1515/
St-Louis M, Tanguay RM (1997) Mutations in the fumarylacetoacetate hydrolase gene causing hereditary tyrosinemia type I: overview. Hum Mutat 9(4):291–299. doi:10.1002/(SICI)1098-1004(1997)9:4<291::AID-HUMU1>3.0.CO;2-9
St-Louis M, Leclerc B, Laine J, Salo MK, Holmberg C, Tanguay RM (1994) Identification of a stop mutation in five Finnish patients suffering from hereditary tyrosinemia type I. Hum Mol Genet 3(1):69–72
Storr SJ, Woolston CM, Martin SG (2012) Base excision repair, the redox environment and therapeutic implications. Curr Mol Pharmacol 5(1):88–101. doi:EPub-Abstract-CMP-60
Tanguay R (2002) Fumarylacetoacetate hydrolase. Wiley encyclopedia of molecular medicine. Wiley, New York
Tanguay RM, Valet JP, Lescault A, Duband JL, Laberge C, Lettre F, Plante M (1990) Different molecular basis for fumarylacetoacetate hydrolase deficiency in the two clinical forms of hereditary tyrosinemia (type I). Am J Hum Genet 47(2):308–316
Tanguay RM, Jorquera R, Poudrier J, St-Louis M (1996) Tyrosine and its catabolites: from disease to cancer. Acta Biochim Pol 43(1):209–216
Tanguay RM, Bergeron A, Jorquera R (2009) Hepatorenal tyrosinemia. In: Lifton RP, Somlo S, Giebsih D, Seldin DW (eds) Genetic diseases of the kidney, vol Chap 40. Elsevier, Amsterdam, pp 681–691
Timm DE, Mueller HA, Bhanumoorthy P, Harp JM, Bunick GJ (1999) Crystal structure and mechanism of a carbon-carbon bond hydrolase. Structure 7(9):1023–1033. doi:st7915
Tomoeda K, Awata H, Matsuura T, Matsuda I, Ploechl E, Milovac T, Boneh A, Scott CR, Danks DM, Endo F (2000) Mutations in the 4-hydroxyphenylpyruvic acid dioxygenase gene are responsible for tyrosinemia type III and hawkinsinuria. Mol Genet Metab 71(3):506–510. doi:10.1006/mgme.2000.3085
Tuchman M, Freese DK, Sharp HL, Ramnaraine ML, Ascher N, Bloomer JR (1987) Contribution of extrahepatic tissues to biochemical abnormalities in hereditary tyrosinemia type I: study of three patients after liver transplantation. J Pediatr 110(3):399–403
van Dyk E, Steenkamp A, Koekemoer G, Pretorius PJ (2010) Hereditary tyrosinemia type 1 metabolites impair DNA excision repair pathways. Biochem Biophys Res Commun 401(1):32–36. doi:S0006-291X(10)01677-3
van Spronsen FJ, Berger R, Smit GP, de Klerk JB, Duran M, Bijleveld CM, van Faassen H, Slooff MJ, Heymans HS (1989) Tyrosinaemia type I: orthotopic liver transplantation as the only definitive answer to a metabolic as well as an oncological problem. J Inherit Metab Dis 12(Suppl 2):339–342
van Spronsen FJ, Thomasse Y, Smit GP, Leonard JV, Clayton PT, Fidler V, Berger R, Heymans HS (1994) Hereditary tyrosinemia type I: a new clinical classification with difference in prognosis on dietary treatment. Hepatology 20(5):1187–1191. doi:S027091399400340X
van Spronsen FJ, Bijleveld CM, van Maldegem BT, Wijburg FA (2005) Hepatocellular carcinoma in hereditary tyrosinemia type I despite 2-(2 nitro-4-3 trifluoro- methylbenzoyl)-1, 3-cyclohexanedione treatment. J Pediatr Gastroenterol Nutr 40(1):90–93. doi:00005176-200501000-00017
Vilboux T, Kayser M, Introne W, Suwannarat P, Bernardini I, Fischer R, O’Brien K, Kleta R, Huizing M, Gahl WA (2009) Mutation spectrum of homogentisic acid oxidase (HGD) in alkaptonuria. Hum Mutat 30(12):1611–1619. doi:10.1002/humu.21120
Weinberg AG, Mize CE, Worthen HG (1976) The occurrence of hepatoma in the chronic form of hereditary tyrosinemia. J Pediatr 88(3):434–438
Wilcken B, Hammond JW, Howard N, Bohane T, Hocart C, Halpern B (1981) Hawkinsinuria: a dominantly inherited defect of tyrosine metabolism with severe effects in infancy. N Engl J Med 305(15):865–868. doi:10.1056/NEJM198110083051505
Wyss PA, Boynton SB, Chu J, Spencer RF, Roth KS (1992) Physiological basis for an animal model of the renal Fanconi syndrome: use of succinylacetone in the rat. Clin Sci 83(1):81–87
Acknowledgements
The work on HT1 in the RMT’s lab was supported by grants from the Canadian Institutes of Health Research (CIHR) and Fondation du Grand Défi Pierre Lavoie.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Morrow, G., Tanguay, R.M. (2017). Biochemical and Clinical Aspects of Hereditary Tyrosinemia Type 1. In: Tanguay, R. (eds) Hereditary Tyrosinemia. Advances in Experimental Medicine and Biology, vol 959. Springer, Cham. https://doi.org/10.1007/978-3-319-55780-9_2
Download citation
DOI: https://doi.org/10.1007/978-3-319-55780-9_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-55779-3
Online ISBN: 978-3-319-55780-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)