Abstract
The objective of this work was to establish a novel and robust technology, based on electron paramagnetic resonance (EPR) oximetry, as a practical tool for measurement of tumor oxygen. Previously, we have reported on the development of oxygen-sensing paramagnetic crystals (LiNc-BuO) encapsulated in a biocompatible polymer, called OxyChip. In this report we present our recent data on the use of OxyChip for pO2 measurements in the tumor of a pre-clinical, large-animal rabbit model. The results establish that OxyChip is capable of noninvasive and repeated measurement of pO2 in a large animal model.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Despite the clinical significance and importance of tissue oxygen levels in the diagnosis, prognosis, and treatment of several pathologies [1], there is clearly an unmet need for devices to measure oxygen levels with a reasonable degree of accuracy, reliability, and robustness. Our laboratory is interested in bringing the accuracy and reliability of electron paramagnetic resonance (EPR) oximetry [2] to the clinical realm for useful measurements in cardiovascular, cancer, and cutaneous applications. Previously, we have discovered unique solid-state implants (probes) and procedures that enable unsurpassed accuracy and repeated interrogation of tissue oxygen level at specific sites over a period of time, extending to months or longer [3]. However, these developments are limited primarily to laboratory research involving cells and small animals. Therefore, we plan to translate this promising technology to the clinical realm, by developing probes and procedures specifically intended for pO2 measurements in transcutaneous, subcutaneous, and deep tissue/organs and validate them in pre-clinical animal models . Here we report our first studies in the tumor of a large animal model, namely rabbit. The results demonstrate the feasibility and reliability of making repeated measurements of pO2 in a pre-clinical model.
2 Methods
2.1 Fabrication and Calibration of OxyChips
Microcrystals of LiNc-BuO were prepared as described previously [4]. Medical grade polydimethylsiloxane (PDMS) base, namely MED-4210 Platinum Silicone Elastomer, was obtained from Factor II, Inc. (Lakeside, AZ). OxyChips containing 40% LiNc-BuO (w/w) in PDMS were prepared in the form of a wire (diameter, 0.6 mm; length 5 cm) using a modification of a previously reported procedure [5]. Briefly, the PDMS base and catalyst/crosslinker (supplied with the PDMS elastomer) were mixed in a 10:1 ratio, after which the LiNc-BuO crystals were added. The heterogeneous dispersion/mixture was outgassed using a vacuum desiccator. One end of a 20-G PTFE (polytetrafluoroethylene) tube was dipped into the PDMS mixture and negative pressure was applied from the other end with a 10-ml syringe to draw the mixture into the tubing to about 5 cm. The PTFE tubing with PDMS mixture was cured in an oven for at least 8 h at 70 °C, followed by withdrawing (by gentle pulling) of the cured PDMS chip out from the tubing. The chip (wire) was further cured at 70 °C overnight. The cured chip (referred to as OxyChip) was in the form of a wire (0.6-mm diameter) that is cut into small segments of 1.0–5.0-mm length for use. In order to verify that mechanical stress or tearing of PDMS coating does not occur resulting in leaching of LiNc-BuO crystals, the OxyChips were suspended in water and subjected to continuous stirring for 72 h at room temperature, after which the chips were removed and dried. Prior to implantation, the chips were sterilized by autoclaving at 121 °C for 30 min. The present study used OxyChips of 5.0-mm length and 0.6-mm diameter. This OxyChip provides an average pO2 in a volume of about 1.4 mm3, and therefore samples a region that may include many capillary segments at the implant site. There are several advantages in using OxyChip than other raw (un-encapsulated) paramagnetic crystals. Encapsulation in PDMS effectively shields the LiNc-BuO crystals from interaction with the biological milieu and thus limits the probability of local and/or systemic toxicity from interactions with the tissue. Further, the encapsulation will hold the crystals together and prevent any migration of them from the site of implant. The OxyChip can be left in the tissue or removed when no longer needed using biopsy procedures. Simultaneous measurements of pO2 from multiple sites can be made by implanting 2–4 OxyChips. We have obtained an Investigational Device Exemption from FDA to test the safety and feasibility of oximetry using OxyChips (5.0 mm × 0.6 mm) in cancer patients.
Linewidth versus pO2 calibration and oxygen response-time curves of OxyChip were constructed by measuring EPR linewidth while the equilibrating gas content was changed from 0–21% oxygen. The EPR measurements were carried out using a custom-built L-band (1.2 GHz) spectrometer with a surface-loop resonator. Gases with known compositions of oxygen (0%, 5% and 21%; balance nitrogen) equilibrated at 37 °C, were flushed over the OxyChip, while the spectra were recorded every minute until a steady linewidth , indicative of equilibration, was achieved.
2.2 Animal Preparation
All the animal procedures were approved by the Institutional Animal Care and Use Committee of Geisel School of Medicine at Dartmouth College (USA). Three New Zealand female rabbits (2.0–2.5 kg body weight) obtained from Charles River Laboratories (Wilmington, MA) were used for all experiments. The animals were separately maintained in a clean 12-h light-dark cycle with free access to food and water. For all experimental procedures, 3.0–3.5% isoflurane mixed with 30% O2 was used for anesthesia induction, 2.5–3.0% isoflurane in 30% O2 for surgery procedure including the implantation of tumor and OxyChips, and 2.0–2.5% in 30% O2 for maintenance of anesthesia during EPR measurements. The core temperature of the animal was measured using a rectal probe and maintained at 37 ± 1 °C using a heating pad.
2.3 Propagation and Inoculation of VX2 Carcinoma in Rabbit, OxyChip Placement, and pO2 Measurements
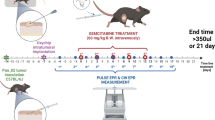
Small (4 × 10 mm) pieces of VX2 carcinoma, which were originally obtained from Dr. Hoopes (Geisel School of Medicine, Dartmouth College), were used for inoculation in rabbit mammary pad as described previously [6, 7]. Briefly, under isoflurane anesthesia, pieces of 2 × 2 mm VX2 carcinoma were implanted and grown subcutaneously in the posterior flank of a rabbit. When the tumors reached a size of 20–30 mm, in approximately 12–14 days after implantation, they were surgically removed and sliced into 2 × 2-mm pieces and then implanted subcutaneously in the left mammary pad in the other rabbits. When the tumor in the mammary pad reached a size of 6–10 mm, a single piece of OxyChip was implanted in the center of the tumor at a depth of 3–5 mm from the surface of the tumor. A second piece of OxyChip was implanted in the right mammary pad at a depth of 1 mm from the surface. Measurements of normal (mammary pad) and tumor pO2 values were performed under 30% O2 breathing for 20 min (baseline) and hyperoxia challenge induced by 100% oxygen inhalation for 15–18 min every 2 days for up to 3 weeks after OxyChip implantation.
3 Results and Discussion
The stability of OxyChip calibration in VX2 tumor and mammary fat pad (normal tissue) in rabbits was evaluated. Figure 41.1 shows a comparison of EPR linewidth versus pO2 calibration of an OxyChip before implantation and after removal from the tumor 3 weeks later. The data showed a linear variation of EPR linewidth with pO2 in the measured range of 0–21% oxygen. Further, there was no change in the linearity or oxygen sensitivity of the chip after 3 weeks of residency in the tumor establishing the stability of calibration. Calibration of chips implanted in the mammary fat pad also showed similar stability (data not shown). The results agree with the calibration data of OxyChip and LiNc-BuO crystals measured in mice and rats [4, 8].
Calibration curve of OxyChip used for pO2 measurement in rabbit VX2 tumor. OxyChips of dimension 0.6-mm diameter and 5.0-mm length (shown in the inset) were calibrated before implantation (pre) and after explanation (post) from the tumor 3 weeks later. The data show a stable and linear calibration of OxyChip
We next evaluated changes in tumor and normal tissue pO2 values as a function of tumor growth. Figure 41.2 shows the pO2 values measured in a VX2 tumor and mammary fat pad of a rabbit over 3 weeks of tumor growth. The pO2 in the tumor remained hypoxic throughout the period while the mammary pad showed substantially higher values (3.9 ± 1.0 mmHg vs. 25.5 ± 2.4 mmHg). The values, in general, appeared to be lower and increasing during the first 7–10 days, apparently due to surgical trauma and inflammation associated with the implantation of OxyChip [4, 8]. The pO2 value in the VX2 tumor measured by OxyChip EPR oximetry appears to be more reliable when compared to values reported by other methods, for example 16.0 ± 14.8 mmHg [9] or 52.4 ± 18.3 mmHg [10] using fiber optic fluorescence method.
Representative data showing the growth of an ectopic VX2 tumor and changes in pO2 values measured in rabbit mammary pad over 3 weeks. The pO2 values were measured in the tumor and normal mammary fat pad using implanted OxyChip. (A) Tumor growth curve. (B) pO2 values measured in the tumor and normal tissue over 3 weeks. The pO2 data shown are Mean ± SEM representing the measurement error. Mean ± SEM values over the 3-week period for tumor and mammary pad were 3.9 ± 1.0 mmHg and 25.5 ± 2.4 mmHg, respectively
Figure 41.3 shows the effect of hyperoxygenation on VX2 tumor and mammary pad tissue . The baseline pO2 measured during the first 20-min administration of 30% O2 with 2–2.5% isoflurane via nose-cone breathing was 6.5 ± 0.5 mmHg. When the oxygen composition in the breathing mask was switched to 100%, the pO2 showed a rapid increase reaching a maximum of 21.2 ± 0.4 mmHg in about 10 min. The corresponding values for mammary pad was 23.9 ± 0.8 mmHg and 49.0 ± 1.3 mmHg, respectively.
4 Conclusion
The study demonstrated for the first time that OxyChip was capable of monitoring pO2 values in a large animal model of tumor as a function of tumor growth and hyperoxic intervention. The VX2 tumor in the mammary pad was hypoxic and responsive to hyperoxygenation intervention.
References
Kulkarni A, Kuppusamy P, Parinandi NL (2007) Oxygen, the lead actor in the pathophysiologic drama: enactment of the trinity of normoxia, hypoxia, and hyperoxia in disease and therapy. Antiox Redox Signal 9:1717–1730
Ahmad R, Kuppusamy P (2010) Theory, instrumentation, and applications of electron paramagnetic resonance oximetry. Chem Rev 110:3212–3236
Swartz HM, Hou H, Khan N et al (2014) Advances in probes and methods for clinical EPR oximetry. Adv Exp Med Biol 812:73–79
Pandian RP, Parinandi NL, Ilangovan G et al (2003) Novel particulate spin probe for targeted determination of oxygen in cells and tissues. Free Radic Biol Med 35:1138–1148
Meenakshisundaram G, Eteshola E, Pandian RP et al (2009) Fabrication and physical evaluation of a polymer-encapsulated paramagnetic probe for biomedical oximetry. Biomed Microdevices 11:773–782
Chen JH, Chen JH, Lin YC et al (2004) Induction of VX2 carcinoma in rabbit liver: comparison of two inoculation methods. Lab Anim 38:79–84
Zhu M, Lin XA, Zha XM et al (2015) Evaluation of the therapeutic efficacy of sequential therapy involving percutaneous microwave ablation in combination with 131I-Hypericin using the VX2 rabbit breast solid tumor model. PLoS One 10:1–16
Hou H, Khan N, Nagane M et al (2016) Skeletal muscle oxygenation measured by EPR oximetry using a highly sensitive polymer-encapsulated paramagnetic sensor. Adv Exp Med Biol 923:351–357
Sun CJ, Li C, Lv HB et al (2014) Comparing CT perfusion with oxygen partial pressure in a rabbit VX2 soft-tissue tumor model. J Radiat Res 55:183–190
Levy EB, Johnson CG, Jacobs G et al (2015) Direct quantification and comparison of intratumoral hypoxia following transcatheter arterial embolization of VX2 liver tumors with different diameter microspheres. J Vasc Interv Radiol 26:1567–1573
Acknowledgment
This work was supported by National Institutes of Health grant EB004031.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Hou, H., Khan, N., Kuppusamy, P. (2017). Measurement of pO2 in a Pre-clinical Model of Rabbit Tumor Using OxyChip, a Paramagnetic Oxygen Sensor. In: Halpern, H., LaManna, J., Harrison, D., Epel, B. (eds) Oxygen Transport to Tissue XXXIX. Advances in Experimental Medicine and Biology, vol 977. Springer, Cham. https://doi.org/10.1007/978-3-319-55231-6_41
Download citation
DOI: https://doi.org/10.1007/978-3-319-55231-6_41
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-55229-3
Online ISBN: 978-3-319-55231-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)