Abstract
This paper presents the use of discrete-event simulation to support process improvements at an outpatient internal medicine department. This department is significantly effective upon treating patients; however, patient waiting times tend to be longer and consequently patient satisfaction rates continue to decrease. With the aid of this technique, 3 improvement scenarios proposed by medical and administrative staff from this department were designed and simulated including changes related to installed capacity and an emphasis on physicians keeping to the schedule. Statistical analysis of output data evidenced which scenarios resulted in poor performance (statistically equal or higher waiting times) and which strategies caused lower waiting times. In this case, Scenario 3 was selected as the best improvement choice with 71.28 % and 19.28 % reduction in average waiting time and standard deviation respectively. With this approach, inefficient strategies can be avoided and real improvement alternatives can be identified.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
A substantial waiting time for patients who request for outpatient services is represented by the interval between patient´s need for special treatment, well known as referral date and actual date of treatment or outpatient clinic date. This delay - appointment lead time - results in more patient dissatisfaction than generated when patients arrive to the outpatient department and wait until physicians call them for treatment [1, 2]. This may represent a weighty number of patients who decline to attend their appointment because of the expectation of long appointment lead times [3].
Specifically, outpatient internal medicine departments are in charge of identifying risk individual factors related to those diseases that affect diverse organs or systems simultaneously; and also treating patients with pluripathology. Both situations tend to be more frequent due to the progressive aging of population. In this way, delayed diagnosis or interventions related to internal medicine could bring about the development of more severe complications in patient´s health and more complex healthcare services such as hospitalization, surgery, intensive care and emergency care could be required [4]. Nonetheless, outpatient internal medicine departments are composed by complex structures; reason why the day-to-day planning of these departments become in a challenging task and should be supported in computational intelligence techniques [5].
In an effort to address this problem, this paper presents a computer discrete-event simulation (DES) approach whose primary aim is to define and evaluate improvement alternatives for the reduction of appointment lead times in outpatient internal medicine departments. This paper also aims to demonstrate how inefficient strategies can be discarded without implementing them on real healthcare systems; in this way, extra charges and negative operational effects can be avoided for both patients and healthcare providers [6].
The remainder of this paper is organized as follows: in Sect. 2 a brief literature review is presented; Sect. 3 presents a case study in an outpatient internal department from hospital sector. Analysis and discussion on results are also described in this section. Finally, Sect. 4 presents concluding remarks and future work.
2 Related Work
There is clear evidence that the research community has focused on using computational simulation techniques to reduce patient waiting times in outpatient departments. Wijewickrama used simulation analysis to reduce queues in mixed-patient´s outpatient department. During this process, Wijewickrama explored bottlenecks in consultation rooms and evaluated four appointment scheduling rules and their possible combinations [7]. This author also applied DES simulation in an outpatient department of Internal Medicine in Japan to reduce patient waiting times before doctor’s calling for treatment. In the simulation model, doctor schedule mixes (DSMs) and diverse appointment schedules (Ass) were examined. Conclusions of this work evidenced meaningful reduction of patient waiting time by combining one DSM found via an optimization program with some ASs [5].
Harper & Gamlin presented a specific simulation model of an ENT clinic that was created in Simul8. In this study, different appointment schedules were tested and it was concluded that waiting times may be meaningfully reduced in that clinic by improved appointment schedules and better management of the schedule [6]. Similar work was developed by Giachetti et al. who described a simulation model to design the appointment system of a dermatology clinic. In this clinic, patients arrive at the same time in a day to reduce physician´s idle time, which is suitable when the clinic cannot predict no-shows. Recommendations of this work express that it would be better to implement a policy in which patients can ask for an appointment in the morning and be seen the same day [8].
Several case studies were designed for specific hospitals and clinics as exposed by Takakuwa & Katagiri where simulation models represented outpatient departments with all patient pathways, human resources and service times [9]; meanwhile, other authors like Kuljis et al. focused on generic methodologies to model outpatient departments. In their work, they proposed CLINSIM approach with successful implementation in 20 clinics located in UK [10].
Even though these studies have exposed different solutions to reduce waiting times in different outpatient departments, a little effort has been reported considering the need of minimizing appointment lead times. Therefore, this paper aims to contribute to this research field by supporting healthcare decision making in these departments with the aid of computational simulation techniques. In this way, guidance is provided for both practitioners and researchers who work in this area.
3 A Case Study: Outpatient Department of Internal Medicine
A case study of an outpatient department of internal medicine from hospital sector is presented to explore the validity and effectiveness of the proposed approach. This department operates from 8.0 to 17.0 during weekdays with two different types of patient appointments: first-time and control.
First-time appointments are assigned for patients who request outpatient internal medicine services for first time. In these appointments, internists spend time getting to know the patients and checking out their medical history to establish suitable treatments. Furthermore, control appointments are scheduled to monitor the progression of patient´s health and effectiveness of prescribed treatments.
Medical consultation in internal medicine are in charge of 3 internists who have different working hours. Internist 1 attends patients on Monday, Tuesday and Thursday from 10.30 to 14.0; while Internist 2 treats them on Tuesday and Wednesday in the same time as Internist 1. Finally, Internist 3 is available for consultation on Friday at the same period as the rest of internists. In this process, - appointment lead time – is a critical to satisfaction and is regulated by the Government. The upper specification limit for this indicator has been established as 8 days/appointment on average.
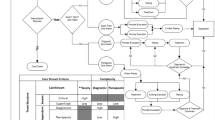
A simulation model was designed with the support of Arena 14.0 ® software to improve the current performance of the outpatient department. With a p-value equal to 0.3957 (higher than 0.05), it was validated that simulation model is statistically equivalent to the real system. After this, current appointment lead time was measured. On average, a patient has to wait 6.2 days with a standard deviation of 1.78 (refer to Fig. 1b). This means there is a probability of 15.6 % that a patient waits for more than 8 days before being treated by an internist of this department. In an effort to address this problem, 3 improvements scenarios were designed by medical staff from the department and assessed through the simulation model without implementing them on the real system (Figs. 2a, b, c). This is to avoid possible negative affectations of poor-performance strategies and their related extra charges.
Scenario 1 proposes eliminating the cancellations of medical agenda through a sanctions policy where each cancelled appointment represents financial penalties for the internist. Meanwhile, Scenario 2 suggests increasing the installed capacity of Internist 2 through an extension of his opening hours (from 8.0 to 14.0) on Tuesdays and Wednesdays. Finally, Scenario 3 recommends setting Tuesdays, Wednesdays and Fridays for Internist 3 in the same time proposed in Scenario 2. After simulating these scenarios, results evidence that appointment lead times of Scenarios 1 and 3 are statistically different compared to those in current system with a p-value = 0 in both cases. Specifically, appointment lead times in Scenario 1 are statistically higher than those in real-world system; nonetheless, these waiting times in Scenario 3 are statistically lower compared to those in current outpatient department of internal medicine (Average appointment lead time = 1.15 days, standard deviation = 1.37 days and probability of overpassing upper specification limit = 0 %) reason by which it can be considered as the best improvement choice. In addition, it was concluded that Scenario 2 is statistically equal to real-world system with a p-value = 0.388.
With regard to the maximum appointment lead time, Scenario 1 and Scenario 2 are both statistically equal to the current system with P-values of 0.305 and 0.509 respectively. Nevertheless, with a p-value = 0, it was proved that Scenario 3 is statistically lower compared with the initial situation of the system.
4 Conclusions and Future Work
In this paper we have proved the effectiveness of computational simulation techniques to reduce appointment lead times in an outpatient internal medicine department. Results evidenced that, under the existing system, 15 % of the appointments scheduled in this department will have an appointment lead time higher than 8 days. Thus, 3 improvement scenarios were simulated and evaluated with the support of medical staff from the hospital; nonetheless, 2 of the scenarios were identified as inefficient and consequently discarded as potential solutions. This is relevant upon considering the negative operational and financial effects if implemented in real-world system for both patients and healthcare providers. This was further evidenced through the application of statistical analysis.
The simulation model created for this case study provided quick insight into the extra capacity needed for this department and influence of sanctions policy. In this case, the proposed penalty policy did not cause a positive effect on waiting time; while the impact of increased installed capacity was proved as statistically significant in Scenario 3. With this scenario, the probability of overpassing upper specification limit established by the Government (8 days) can be reduced to 0 %; which represents a significant contribution to healthcare upon preventing the development of more severe complications in patient´s health. This approach can be implemented in any outpatient department of internal medicine; although it can be also extended to other specialties. Future work will include financial analysis on each improvement scenario with the purpose of strongly supporting healthcare decision making and developing optimal combinatorial approaches with significant results [11].
References
Günal, M.M., Pidd, M.: Discrete event simulation for performance modelling in health care: a review of the literature. J. Simul. 4(1), 42–51 (2010)
McCarthy, K., McGee, H.M., O’Boyle, C.A.: Outpatient clinic waiting times and non-attendance as indicators of quality. Psychol. Health Med. 5(3), 287–293 (2000)
Blizzard, R.: Patient satisfaction starts in the waiting room. Gallup Poll News Service (2009)
Barrios, M.A.O., Caballero, J.E., Sánchez, F.S.: A methodology for the creation of integrated service networks in outpatient internal medicine. In: Bravo, J., Hervás, R., Villarreal, V. (eds.) AmIHEALTH 2015. LNCS, vol. 9456, pp. 247–257. Springer, Heidelberg (2015)
Wijewickrama, A., Takakuwa, S.: Simulation analysis of appointment scheduling in an outpatient department of internal medicine. In: Proceedings of the Winter Simulation Conference, pp. 2264–2273. IEEE (2005)
Harper, P.R., Gamlin, H.M.: Reduced outpatient waiting times with improved appointment scheduling: a simulation modelling approach. OR Spectr. 25(2), 207–222 (2003)
Wijewickrama, A.K.: Simulation analysis for reducing queues in mixed-patients’ outpatient department. Int. J. Simul. Model. 5(2), 56–68 (2006)
Giachetti, R.E., Centeno, E.A., Centeno, M.A., Sundaram, R.: Assessing the viability of an open access policy in an outpatient clinic: a discrete-event and continuous simulation modeling approach. In: Proceedings of the 37th Conference on Winter Simulation, pp. 2246–2255. Winter Simulation Conference (2005)
Takakuwa, S., Katagiri, D.: Modeling of patient flows in a large-scale outpatient hospital ward by making use of electronic medical records. In: 2007 Winter Simulation Conference, pp. 1523–1531. IEEE (2007)
Kuljis, J., Paul, R.J., Chen, C.: Visualization and simulation: two sides of the same coin? Simulation 77(3–4), 141–152 (2001)
Herazo-Padilla, N., Montoya-Torres, J.R., Munoz-Villamizar, A., Nieto Isaza, S., Ramirez Polo, L.: Coupling ant colony optimization and discrete-event simulation to solve a stochastic location-routing problem. In: 2013 Simulations Conference (WSC), pp. 3352–3362. IEEE (2013)
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing AG
About this paper
Cite this paper
Ortiz, M.A., López-Meza, P. (2016). Using Computer Simulation to Improve Patient Flow at an Outpatient Internal Medicine Department. In: García, C., Caballero-Gil, P., Burmester, M., Quesada-Arencibia, A. (eds) Ubiquitous Computing and Ambient Intelligence. UCAmI 2016. Lecture Notes in Computer Science(), vol 10069. Springer, Cham. https://doi.org/10.1007/978-3-319-48746-5_30
Download citation
DOI: https://doi.org/10.1007/978-3-319-48746-5_30
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-48745-8
Online ISBN: 978-3-319-48746-5
eBook Packages: Computer ScienceComputer Science (R0)