Abstract
Natural killer (NK) cells are lymphocytes of the innate immune system that have the ability to recognize malignant cells through detection of a variety of cell-surface indicators of stress and danger. Once activated through such recognition, NK cells release cytokines and induce target cell lysis through a variety of mechanisms. NK cells are increasingly recognized as important mediators of other immunotherapeutic modalities, including cytokines, antibodies, immunomodulators, and stem cell transplantation. Adoptive immunotherapies with NK cells are being tested in early-stage clinical trials, and recent advances in manipulating their number and function have caused a renewed emphasis on this cancer-fighting cell. In this chapter we address the evidence for NK cell recognition of osteosarcoma in vitro and in vivo, discuss new therapies that are directly or indirectly dependent on NK cell function, and describe potential approaches for manipulating NK cell number and function to enhance therapy against osteosarcoma.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Brief Overview of NK Cell Biology
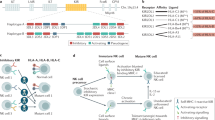
NK cells are lymphocytes of the innate immune system with cytotoxic and regulatory functions, which are critical mediators of immune responses against infections and malignancies [1]. Unlike adaptive T and B lymphocytes, NK cells are characterized by their ability to recognize such targets without prior sensitization. Human NK cells comprise approximately 10–15 % of all peripheral blood lymphocytes and are identified by the lack of CD3 and the presence of CD56 and/or CD16. NK cells express several classes of activating receptors that recognize proteins which are upregulated by cell stress or are of nonself origin, and are negatively regulated by inhibitory receptors that primarily bind human leukocyte antigens (HLA) as a mechanism of self-recognition. NK-cell effector function, including target cytotoxicity, is triggered when the balance of activating and inhibiting signals is tipped towards activation.
Activating and Inhibitory Receptors
Several families of activating receptors have been characterized, including CD16 (FcRγIIIa), natural cytotoxicity receptors (NCR), and NK Group 2 (NKG2)-family lectin-like receptors. CD16 is the low-affinity Fc receptor which binds the Fc portion of human IgG1 and IgG3, mediating antibody-dependent cell cytotoxicity (ADCC) of antibody-labeled cells [2]. The NCRs (NKp30, NKp44, and NKp46) are activating receptors that bind virus- and stress-related proteins, with expression mostly restricted to NK cells [3]. The receptors of the NKG2 family are expressed as heterodimers with CD94, except for NKG2D which is expressed as homodimer [4]. NKG2D, the major activating receptor in this family, recognizes MHC-class-I-related Chain A or B (MICA/B) and members of the UL-16 binding protein (ULBP)-family, which are increased in response to cellular stress.
Killer Immunoglobulin-like Receptors (KIR) have cytoplasmic domains comprised of a short immunoreceptor tyrosine-based activating motif (ITAM) or a long immunoreceptor tyrosine-based inhibition motif (ITIM) [4]. The primary inhibitory receptors in NK cells are the long-tailed KIRs and NKG2A, which serve to recognize self by binding to HLA class I molecules, preventing NK-mediated lysis of cells with normal HLA expression.
Fifteen closely related KIR genes are located on chromosome 19q13.4 and are present or absent in many haplotype combinations such that most individuals lack one or more KIR genes. In addition to their haplotype variability, KIR genes are highly polymorphic, are variably expressed between NK cells, and functional reactivity is educated by interaction with the host HLA haplotypes. Thus, the NK-cell repertoire varies greatly between individuals. The allelic variations in KIR have been grouped into A and B haplotypes [5], with B haplotypes having greater numbers of activating KIR genes. Allogeneic transplants from donors with the “B” haplotype are predicted to have superior NK cell-mediated antitumor effects [6].
Inhibitory KIRs are specific for HLA isotypes on the basis of conserved amino acid residues at position 80. Approximately half of HLA-C alleles have the amino acid asparagine (N) at residue 80—referred to as Group C1—which confers binding to KIR2DL2 and KIR2DL3. The other half of the C alleles codes for lysine (K) at residue 80 (Group C2), which confers binding to KIR2DL1. Similarly, about 40 % of HLA-B alleles carry the supertypic serologic epitope HLA-Bw4 (defined primarily by threonine (T) at residue 80), which confers binding to KIR3DL1. The presence of the HLA ligand regulates the activity of these KIRs during NK cell development through a process called licensing. Thus, given both parental alleles it is possible for the HLA type of an individual to restrict NK cell licensing to as few as one (e.g., C2/C2 homozygous and Bw4–) or as many as three (C1/C2 heterozygous and Bw4+) inhibitory KIR.
This HLA-biased education without HLA-restricted antigen recognition (as for T cells), gave rise to the “missing-self hypothesis,” which postulates that NK cells recognize and destroy autologous cells with lost or altered self-HLA class I molecules [7]. However, classical HLA class I is not always required to protect from NK-cell mediated cytotoxicity, nor is it always sufficient to prevent NK-cell cytotoxicity [8].
Mechanisms of NK Cell-Mediated Killing
Upon receiving a predominance of activating signals, NK cells release granules containing perforin and granzymes directed towards the target cell. The perforins form a pore in the cell membrane, allowing entry of the granzymes to the cytoplasm to induce apoptosis by direct activation of caspase-3 [9]. NK cell activation also results in increased expression of death receptor ligands on the NK cell, such as Fas ligand (FasL) and tumor necrosis factor (TNF)-related apoptosis-inducing ligand (TRAIL) [10], which induce apoptosis via associated death receptors on target cells [11–13]. In addition to these pathways, NK cells also produce several cytokines such as IFN-γ, which are important in mediating the adaptive immune response against cancer [14].
Evidence for NK Cell Activity in Osteosarcoma
NK Cell Function in Osteosarcoma Patients
NK cells play a critical role in tumor surveillance and low NK cell cytotoxicity in older adults is associated with increased risk of developing cancer [15]. Clinical data show that NK cells may play an important role in osteosarcoma (OS) prevention and treatment response. In patients with OS, a lower number of circulating NK cells was observed in peripheral blood compared to normal controls [16] suggesting that NK cells play a preventive role in OS tumor development. Furthermore, patients undergoing treatment for OS demonstrate better survival outcome with faster absolute lymphocyte recovery compared to patient with slow lymphocyte recovery [17], denoting the antitumor role of the immune system in treatment response. Finally, patients with OS treated with Il-2 in addition to polychemotherapy and surgery showed augmentation in the number and activity of NK cells, the magnitude of which correlated with an improved clinical outcome [18]. Whereas NK cells in patients with several types of cancer have been shown to have poor function, NK cells isolated from patients with OS were shown to be functionally and phenotypically unimpaired, have intact IFN signaling, and demonstrated cytolytic activity against autologous and allogeneic OS cells and other target cells [19, 20].
Expression of NK Ligands
The susceptibility of tumor cells to NK cell lysis is regulated by the proportion of inhibiting and activating signals perceived upon interaction of NK cells with the target cell. It correlates negatively with expression of HLA class I antigens and positively with intercellular adhesion molecules and activating ligands on the surface of tumor cells.
Downregulation of HLA class I antigens on the cell surface can be induced by stress conditions and is correlated with increased susceptibility to NK cell killing through decreased signaling by inhibitory KIRs, a phenomenon described as “missing-self.” In vitro experiments with OS cell lines of varying levels of HLA class I antigen expression show that OS cells with surface expression of HLA are less susceptible to killing by NK cells compared to cells lacking cell surface HLA; moreover, downregulation of cell-surface HLA enhances the sensitivity of NK-resistant OS cells to NK killing. Similarly, OS target cell killing correlates with their degree of KIR-HLA incompatibility with the NK cells [21]. In vivo, OS primary and metastatic tumors have been shown to lose or downregulate HLA class I expression, thus becoming more susceptible to NK cell killing [22].
Expression of cell adhesion molecules renders tumor cells more susceptibility to NK-mediated lysis; these molecules fortify cell-to-cell interactions and provide co-stimulatory signals that enhance the cytotoxic activity of NK cells [23, 24]. Expression of the adhesion molecules CD54 and CD58 increases the bond between target and effector cells and correlates positively with the susceptibility of OS cells to NK lysis [25–27]. In vivo, lack of CD54 expression allows the circulation of tumor cells, avoids establishing stable cytolytic conjugates, and provides means of evading NK spontaneous lysis [28].
Several activating receptor–ligand interactions have been implicated in the interaction of NK cells with OS cells. Ligands for NKG2D and DNAM-1 activating receptors (MICA/B, ULBP, PVR, and nectin-2) are widely expressed on OS cell lines and OS tumor samples [19, 29], rendering them more sensitive to NK recognition and killing. Cytolysis of OS cells is dependent on NKG2D and DNAM-1 pathways and blockade of both pathways is required for optimal inhibition of activated NK cells; activation through NKG2D and DNAM-1 pathways also overcomes inhibition of NK cells mediated by KIR–HLA interaction [19]. In vivo, the level of MICA expression on OS cells has been correlated with staging; expression of MICA is higher in patients with early stage disease compared to late stage, suggesting a role for MICA-NKG2D mediated NK control of OS [29], and downregulation of MICA appears to be a common immune escape mechanism [30]. Unlike other tumor types, MICA expression on OS tumor cells is unaltered by exposure to chemotherapy [19]. NK cell recognition of OS tumor cell has also been described via the NCR receptors, although the ligands on OS cells for these receptors is unknown.
Mechanisms of Killing
NK cells exert direct and indirect antitumor activity and kill target tumor cells via release of perforin and granzyme containing granules, secretion of cytokines and effector molecules, ligation of death receptors, and ADCC through the CD16 receptor.
OS cell lines and freshly isolated OS tumor cells are susceptible to the cytolytic activity of activated NK cells [31]. The release of granules containing granzyme B (GrB) into the target cell cytoplasm is a predominant pathway involved in NK cell killing of OS cells; blocking GrB results in complete abrogation of NK-mediated OS lysis [19]. NK cytotoxicity to OS cells is enhanced by Fc–FcγR interaction; epidermal growth factor receptor (EGFR)-expressing OS cells are more susceptible to NK killing in the presence anti-EGFR monoclonal antibody (MoAb) compared to EGFR-negative OS cells [32]. The Fas-Fas ligand mediated apoptosis, an important process of target killing by NK cells, appears at least in vitro to play only a minor role in the interaction between NK cells and OS cells [19].
Mechanisms of Immune Escape
Tumor cells may acquire diverse mechanisms to evade NK cell recognition [33]. No or low expression of adhesion molecules or ligands for activating receptors and/or increased expression of ligands for inhibitory receptors are described mechanisms adapted by tumor cells to evade NK cell surveillance. In addition, shedding of NKG2D ligands (soluble sMICA) from the membrane of tumor cells can impair NKG2D-mediated cytotoxicity by blocking the NKG2D receptors on NK cells. Furthermore, secretion of immunosuppressive cytokines and transforming growth factor-β has been associated with defective NK cell function, restricting tumor cell recognition and killing.
Both classical and nonclassical HLA class I molecules, which are ligands for inhibitory KIR and CD94/NKG2A receptors, are expressed on some OS naïve tumors and may be increased in OS cells when exposed to chemotherapy [19].
OS cell lines and tumor sample show higher expression of surface MICA compared to normal bone tissue and benign bone tumors making them theoretically more susceptible to NK cells killing. However, soluble MICA was detected in the serum of some patient with OS resulting in diminished NKG2D expression on NK cells and decreased tumor cell killing. Clinical correlation showed that in patients with OS, elevated MICA expression combined with increased soluble MICA was associated with decreased NKG2D expression on PBMC, and this combination correlated significantly with advanced and metastatic disease [29, 34]. With progression of OS, expression of MICA decreases, soluble MICA increases, and expression of NKG2D on NK cells decreases [29].
Indirect Activation of NK Cell Function
In patients with OS, NK cell abnormalities have been described including lower numbers of circulating cells and decreased expression of activating receptors; these NK cells, however, have normal cytolytic activity following stimulation in vitro. The antitumor activity of NK cells can be modulated and enhanced by monoclonal antibodies, cytokines, or immunomodulators.
Monoclonal Antibodies
ADCC by NK cells requires interaction between the Fc receptor (CD16) on NK cells and the Fc region of an antibody binding to an antigen on the tumor cell surface, resulting in NK cell activation and degranulation toward the target cell.
EGFR is expressed on 90 % of OS tumor samples [35]. Cetuximab, a MoAb targeting EGFR, increases NK-dependent lysis of EGFR-expressing sarcomas. Importantly, the sensitivity to cetuximab-enhanced lysis by resting NK cells is comparable among most EGFR-expressing cell lines, including chemotherapy-resistant OS cells [32]. Although prolonged OS/NK cell cocultures and excess of tumor cells in culture results in diminished NK cell cytotoxicity secondary to downregulation of activating receptors on NK cell surface, ADCC killing of OS by NK cells is unaltered by this suppressive mechanism [36].
Cytokines
Cytokines may act directly on tumor cells as anti-proliferative agents and indirectly via activation of cellular immune agents such as NK cells leading to increased lysis of tumor cells.
Interleukin (IL)-15 potentiates the cytolytic activity of NK cells by increasing NKG2D expression on cell surface and enhancing GrB release upon activation. IL-15 activation reverses impaired expression of NKG2D and DNAM-1 and impaired NK cell cytotoxicity induced by prolonged cocultures of NK cells with OS cells, and NK cells activated with IL-15 prior to coculture with OS cells do not downregulate activating receptors and preserve functional activity despite prolonged exposure to target cells [36]. IL-2 and IL-12 increase cytotoxicity of NK cells to NK-sensitive and NK-resistant OS cell lines by increasing the density of CD18 and CD2 receptors on the NK cell surface, enhancing the conjugate-forming capacity of NK cells to OS targets [37]. Importantly, targeted application of IL-2 to the lung by aerosolized delivery markedly improves the migration of adoptively transferred NK cells into lung metastasis, resulting in enhanced control of metastatic disease [38].
IL-12 increases expression of ICAM-1 (a ligand for CD18) on OS cell lines cocultured with PBMCs in cell-to-cell contact [39]. In a mouse model of metastatic osteosarcoma, mice bearing pulmonary metastasis treated with IL-12 showed decreased number and size of pulmonary metastasis mediated by NK cells [40]. IFN potentiates NK-mediated lysis of OS cell lines, IFN-conjugated antibodies specifically localize tumor cells in a mouse xenograft tumor model and further increase NK cell activation and tumor cell lysis [41, 42]. IL-17 augments expression of fibronectin on OS cell lines that express the IL-17 receptor, mediating increased adhesion of NK cells to OS cells and thus enhancing NK cytotoxicity. IL-17 has no direct effect on NK cells function [43].
Chemotherapy
As mentioned above, chemotherapy appears to increase expression of inhibitory ligands, but does not increase MICA [19]. Chemotherapy does increase sensitivity to ADCC by NK cells [36], and both gemcitabine [44] and cisplatin [45] may increase sensitivity of OS to direct NK cell lysis by upregulation of Fas or downregulation of anti-apoptotoic proteins.
Immunomodulators
In addition to MoAbs and cytokines, a variety immunomodulatory drugs have been successfully combined with NK cells to potentiate their antitumor activity and treat human malignancies [46–48].
In the setting of OS, the activity of NK cells may be weakened or enhanced by immune-modulating agents. Sodium valproate (an HDAC inhibitor) and hydralazine (a DNA-methylation inhibitor) increase the expression of MICA and MICB on OS cells, but not sMICA in serum, and therefore increase the susceptibility of tumor cells to NK cell lysis [49, 50]. Moreover, hydralazine increases cell surface expression of Fas and augments Fas-induced OS cell death, whereas valproic acid sensitizes OS cells to Fas-mediated cell death and decreases production of soluble Fas [49, 50], thus further potentiating OS sensitivity to NK cell killing. However, both HDAC inhibition [51] and DNA hypomethylation [52] can have an adverse direct effect on NK cell function, necessitating approaches that sequence drug therapy and cell therapy. A narrow-spectrum HDAC inhibitor, SNDX-275, has been shown to increase osteosarcoma killing through upregulation of Fas [53], c-FLIP [54], and MICA [52], and also augments NK cell function through upregulation of NKG2D [30].
Lenalidomide is an immunomodulatory thalidomide derivative with activity against a wide variety of cancers. Lenalidomide may enhance NK cell number and maturation through increased IL-15 levels [55]. Lenalidomide augments the activity of NK cells by enhancing ADCC of MoAbs against solid tumors [56], including trastuzumab and cetuximab activity against bone sarcomas [57]. Mifamurtide (MTP-PE), discussed extensively in chapter “IL-11Rα: A Novel Target for the Treatment of Osteosarcoma,” may exert some of its anticancer effect by enhancing NK cell activity [58].
Heat treatment of OS cell lines increases their susceptibility to NK-cell-mediated lysis through upregulation heat-shock-protein 72 (HSP72) expression [59]. Hypoxia decreases the expression of MICA on OS cell lines in a hypoxia-inducible factor 1α (HIF-1α)-dependent manner and consequently decreases the susceptibility of tumor cells to NK cell lysis [60]. However, hypoxia does not interfere with MoAb-mediated target cell killing by ADCC [61].
NK Cell Adoptive Immunotherapy
Clinical NK Cell Sources and Trials
NK cells may be obtained in numbers sufficient for clinical use in adoptive immunotherapy by apheresis and CD3 depletion, or by ex vivo expansion. NK cells have been successfully expanded from peripheral blood, cord blood, and pluripotent or embryonic stem cells. Expansion methods have included various combinations of cytokines, cytokine fusion proteins, cytokines and OKT3, cytokines and stromal support, antibody-coated beads, and feeder cells obtained from peripheral blood or derived from EBV-lymphoblastoid cell lines or K562 (reviewed in [62]).
NK cells have been delivered by adoptive transfer to very few patients with osteosarcoma. Expanded NK cells were given as adjuvant immunotherapy after matched allogeneic transplant (C. Mackall, personal communication—ClinicalTrials.gov Identifier NCT01287104). As mentioned above, KIR-ligand incompatibility is associated with increased NK cell activity against osteosarcoma cell lines [21]. Thus, similar to the observed benefit in AML, it is likely that approaches using mismatched allogeneic donors for NK cell therapy of osteosarcoma will have greater antitumor effect than matched or autologous NK cells. NK92 is a cell line derived from a patient with NK cell leukemia and has NK cell-like activity against tumor cell lines. Clinical grade irradiated NK92 cells have been infused in a patient with advanced osteosarcoma, though no response to treatment was observed [63].
Future Approaches
The recent availability of clinically viable approaches for obtaining large number of NK cells now enables the clinical testing of combination therapies to enhance NK cell function and osteosarcoma sensitivity. Genetic modification of NK cells may further enhance their activity against osteosarcoma. The antigen-binding domains of all of the MoAbs mentioned above have been identified and genetically manipulated to generate chimeric antigen receptors (CAR) that mediate enhanced killing by T cells, as described in chapter “Using Canine Osteosarcoma as a Model to Assess Efficacy of Novel Therapies: Can Old Dogs Teach Us New Tricks?” These CAR also have potential application for clinical development in NK cells, and CAR with NKG2D-like specificity can further improve the NK cell immunotherapy of osteosarcoma in murine models [64]. The ability to deliver large cell doses, combination with sensitizing chemotherapy, radiation, or immunomodulatory drugs, and genetic modifications will be the subjects of cutting edge trials in the decade to come.
References
Raulet DH, Guerra N (2009) Oncogenic stress sensed by the immune system: role of natural killer cell receptors. Nat Rev Immunol 9(8):568–580. doi:10.1038/nri2604
Trinchieri G (1989) Biology of natural killer cells. Adv Immunol 47:187–376
Moretta A, Bottino C, Vitale M, Pende D, Cantoni C, Mingari MC, Biassoni R, Moretta L (2001) Activating receptors and coreceptors involved in human natural killer cell-mediated cytolysis. Annu Rev Immunol 19:197–223. doi:10.1146/annurev.immunol.19.1.197, 19/1/197 [pii]
Pegram HJ, Andrews DM, Smyth MJ, Darcy PK, Kershaw MH (2011) Activating and inhibitory receptors of natural killer cells. Immunol Cell Biol 89(2):216–224. doi:10.1038/icb.2010.78
Uhrberg M, Valiante NM, Shum BP, Shilling HG, Lienert-Weidenbach K, Corliss B, Tyan D, Lanier LL, Parham P (1997) Human diversity in killer cell inhibitory receptor genes. Immunity 7(6):753–763
McQueen KL, Dorighi KM, Guethlein LA, Wong R, Sanjanwala B, Parham P (2007) Donor-recipient combinations of group A and B KIR haplotypes and HLA class I ligand affect the outcome of HLA-matched, sibling donor hematopoietic cell transplantation. Hum Immunol 68(5):309–323. doi:10.1016/j.humimm.2007.01.019
Ljunggren HG, Karre K (1990) In search of the ‘missing self’: MHC molecules and NK cell recognition. Immunol Today 11(7):237–244
Farag SS, Caligiuri MA (2006) Human natural killer cell development and biology. Blood Rev 20(3):123–137. doi:10.1016/j.blre.2005.10.001, S0268-960X(05)00055-X [pii]
Browne KA, Blink E, Sutton VR, Froelich CJ, Jans DA, Trapani JA (1999) Cytosolic delivery of granzyme B by bacterial toxins: evidence that endosomal disruption, in addition to transmembrane pore formation, is an important function of perforin. Mol Cell Biol 19(12):8604–8615
Zamai L, Ahmad M, Bennett IM, Azzoni L, Alnemri ES, Perussia B (1998) Natural killer (NK) cell-mediated cytotoxicity: differential use of TRAIL and Fas ligand by immature and mature primary human NK cells. J Exp Med 188(12):2375–2380
Kayagaki N, Yamaguchi N, Nakayama M, Takeda K, Akiba H, Tsutsui H, Okamura H, Nakanishi K, Okumura K, Yagita H (1999) Expression and function of TNF-related apoptosis-inducing ligand on murine activated NK cells. J Immunol 163(4):1906–1913
Smyth MJ, Cretney E, Takeda K, Wiltrout RH, Sedger LM, Kayagaki N, Yagita H, Okumura K (2001) Tumor necrosis factor-related apoptosis-inducing ligand (TRAIL) contributes to interferon gamma-dependent natural killer cell protection from tumor metastasis. J Exp Med 193(6):661–670
Takeda K, Smyth MJ, Cretney E, Hayakawa Y, Yamaguchi N, Yagita H, Okumura K (2001) Involvement of tumor necrosis factor-related apoptosis-inducing ligand in NK cell-mediated and IFN-gamma-dependent suppression of subcutaneous tumor growth. Cell Immunol 214(2):194–200. doi:10.1006/cimm.2001.1896
Smyth MJ, Hayakawa Y, Takeda K, Yagita H (2002) New aspects of natural-killer-cell surveillance and therapy of cancer. Nat Rev Cancer 2(11):850–861. doi:10.1038/nrc928
Imai K, Matsuyama S, Miyake S, Suga K, Nakachi K (2000) Natural cytotoxic activity of peripheral-blood lymphocytes and cancer incidence: an 11-year follow-up study of a general population. Lancet 356(9244):1795–1799. doi:10.1016/S0140-6736(00)03231-1, S0140-6736(00)03231-1 [pii]
Markiewicz K, Zeman K, Kozar A, Golebiowska-Wawrzyniak M, Wozniak W (2012) Evaluation of selected parameters of cellular immunity in children with osteosarcoma at diagnosis. Med Wieku Rozwoj 16(3):212–221
Moore C, Eslin D, Levy A, Roberson J, Giusti V, Sutphin R (2010) Prognostic significance of early lymphocyte recovery in pediatric osteosarcoma. Pediatr Blood Cancer 55(6):1096–1102. doi:10.1002/pbc.22673
Luksch R, Perotti D, Cefalo G, Gambacorti Passerini C, Massimino M, Spreafico F, Casanova M, Ferrari A, Terenziani M, Polastri D, Gambirasio F, Podda M, Bozzi F, Ravagnani F, Parmiani G, Fossati Bellani F (2003) Immunomodulation in a treatment program including pre- and post-operative interleukin-2 and chemotherapy for childhood osteosarcoma. Tumori 89(3):263–268
Buddingh EP, Schilham MW, Ruslan SE, Berghuis D, Szuhai K, Suurmond J, Taminiau AH, Gelderblom H, Egeler RM, Serra M, Hogendoorn PC, Lankester AC (2011) Chemotherapy-resistant osteosarcoma is highly susceptible to IL-15-activated allogeneic and autologous NK cells. Cancer Immunol Immunother 60(4):575–586. doi:10.1007/s00262-010-0965-3
Buddingh EP, Ruslan SE, Berghuis D, Gelderblom H, Anninga JK, Hogendoorn PC, Egeler RM, Schilham MW, Lankester AC (2012) Intact interferon signaling in peripheral blood leukocytes of high-grade osteosarcoma patients. Cancer Immunol Immunother 61(6):941–947. doi:10.1007/s00262-012-1232-6
Delgado D, Webster DE, DeSantes KB, Durkin ET, Shaaban AF (2010) KIR receptor-ligand incompatibility predicts killing of osteosarcoma cell lines by allogeneic NK cells. Pediatr Blood Cancer 55(7):1300–1305. doi:10.1002/pbc.22665
Tsukahara T, Kawaguchi S, Torigoe T, Asanuma H, Nakazawa E, Shimozawa K, Nabeta Y, Kimura S, Kaya M, Nagoya S, Wada T, Yamashita T, Sato N (2006) Prognostic significance of HLA class I expression in osteosarcoma defined by anti-pan HLA class I monoclonal antibody, EMR8-5. Cancer Sci 97(12):1374–1380. doi:10.1111/j.1349-7006.2006.00317.x, CAS317 [pii]
Chong AS, Boussy IA, Jiang XL, Lamas M, Graf LH Jr (1994) CD54/ICAM-1 is a costimulator of NK cell-mediated cytotoxicity. Cell Immunol 157(1):92–105. doi:10.1006/cimm.1994.1208, S0008-8749(84)71208-1 [pii]
Tarozzi A, Mariani E, Facchini A (1995) In vitro cytolytic activity of human NK cells against osteosarcoma cell lines. Boll Soc Ital Biol Sper 71(7–8):221–226
Mariani E, Tarozzi A, Meneghetti A, Cattini L, Facchini A (1998) TNF-alpha but not IL-1 and IL-6 modifies the susceptibility of human osteosarcoma cells to NK lysis. Int J Oncol 13(2):349–353
Mariani E, Tarozzi A, Meneghetti A, Cattini L, Facchini A (1997) Human osteosarcoma cell susceptibility to natural killer cell lysis depends on CD54 and increases after TNF alpha incubation. FEBS Lett 406(1–2):83–88
Meneghetti A, Mariani E, Santi S, Riccio M, Cattini L, Paoletti S, Facchini A (1999) NK binding capacity and lytic activity depend on the expression of ICAM-1 on target bone tumours. Int J Oncol 15(5):909–914
Zamai L, Zauli G, Bavelloni A, Marmiroli S, Cataldi A, Weber G, Vitale M (1995) Tiazofurin induces a down-modulation of ICAM-1 expression on K562 target cells impairing NK adhesion and killing. Cell Immunol 164(1):100–104. doi:10.1006/cimm.1995.1147, S0008-8749(85)71147-1 [pii]
Xiao P, Xue L, Che LH, Peng JJ, Wu HX, Li Y, Qiao H (2008) Expression and roles of MICA in human osteosarcoma. Histopathology 52(5):640–642. doi:10.1111/j.1365-2559.2008.02989.x, HIS2989 [pii]
Zhu S, Denman CJ, Cobanoglu ZS, Kiany S, Lau CC, Gottschalk SM, Hughes DPM, Kleinerman ES, Lee DA (2013) The narrow-spectum HDAC inhibitor entinostat enhances NKG2D expression without NK cell toxicity, leading to enhanced recognition of sarcoma. Pharmacol Res (In Press)
Cho D, Shook DR, Shimasaki N, Chang YH, Fujisaki H, Campana D (2010) Cytotoxicity of activated natural killer cells against pediatric solid tumors. Clin Cancer Res 16(15):3901–3909. doi:10.1158/1078-0432.CCR-10-0735, 1078-0432.CCR-10-0735 [pii]
Pahl JH, Ruslan SE, Buddingh EP, Santos SJ, Szuhai K, Serra M, Gelderblom H, Hogendoorn PC, Egeler RM, Schilham MW, Lankester AC (2012) Anti-EGFR antibody cetuximab enhances the cytolytic activity of natural killer cells toward osteosarcoma. Clin Cancer Res 18(2):432–441. doi:10.1158/1078-0432.CCR-11-2277
Waldhauer I, Steinle A (2008) NK cells and cancer immunosurveillance. Oncogene 27(45):5932–5943. doi:10.1038/onc.2008.267
Lu SM, Xiao P, Xue L, Che LH, Yang P, Li Y, Qiao H (2008) Prevalent expression of MHC class I chain-related molecule A in human osteosarcoma. Neoplasma 55(3):266–272
Lee JA, Ko Y, Kim DH, Lim JS, Kong CB, Cho WH, Jeon DG, Lee SY, Koh JS (2012) Epidermal growth factor receptor: is it a feasible target for the treatment of osteosarcoma? Cancer Res Treat 44(3):202–209. doi:10.4143/crt.2012.44.3.202
Pahl JH, Ruslan SE, Kwappenberg KM, van Ostaijen-Ten Dam MM, van Tol MJ, Lankester AC, Schilham MW (2013) Antibody-dependent cell lysis by NK cells is preserved after sarcoma-induced inhibition of NK cell cytotoxicity. Cancer Immunol Immunother 62(7):1235–1247. doi:10.1007/s00262-013-1406-x
Mariani E, Meneghetti A, Tarozzi A, Cattini L, Facchini A (2000) Interleukin-12 induces efficient lysis of natural killer-sensitive and natural killer-resistant human osteosarcoma cells: the synergistic effect of interleukin-2. Scand J Immunol 51(6):618–625, sji737 [pii]
Guma SR, Lee DA, Yu L, Gordon N, Hughes D, Stewart J, Wang WL, Kleinerman ES (2013) Natural killer cell therapy and aerosol interleukin-2 for the treatment of osteosarcoma lung metastasis. Pediatr Blood Cancer. doi:10.1002/pbc.24801
Liebau C, Merk H, Schmidt S, Roesel C, Karreman C, Prisack JB, Bojar H, Baltzer AW (2002) Interleukin-12 and interleukin-18 change ICAM-I expression, and enhance natural killer cell mediated cytolysis of human osteosarcoma cells. Cytokines Cell Mol Ther 7(4):135–142
Mills L, Huang G, Worth LL (2005) The role of interferon gamma and NK cells in the eradication of pulmonary osteosarcoma metastases by IL-12. AACR Meeting Abstracts 2005(1):1413c
Pelham JM, Gray JD, Flannery GR, Pimm MV, Baldwin RW (1983) Interferon-alpha conjugation to human osteogenic sarcoma monoclonal antibody 791 T/36. Cancer Immunol Immunother 15(3):210–216
Flannery GR, Pelham JM, Gray JD, Baldwin RW (1984) Immunomodulation: NK cells activated by interferon-conjugated monoclonal antibody against human osteosarcoma. Eur J Cancer Clin Oncol 20(6):791–798
Honorati MC, Neri S, Cattini L, Facchini A (2003) IL-17 enhances the susceptibility of U-2 OS osteosarcoma cells to NK cell lysis. Clin Exp Immunol 133(3):344–349
Gordon N, Koshkina NV, Jia SF, Khanna C, Mendoza A, Worth LL, Kleinerman ES (2007) Corruption of the Fas pathway delays the pulmonary clearance of murine osteosarcoma cells, enhances their metastatic potential, and reduces the effect of aerosol gemcitabine. Clin Cancer Res 13(15 Pt 1):4503–4510. doi:10.1158/1078-0432.CCR-07-0313
Kinoshita H, Yoshikawa H, Shiiki K, Hamada Y, Nakajima Y, Tasaka K (2000) Cisplatin (CDDP) sensitizes human osteosarcoma cell to Fas/CD95-mediated apoptosis by down-regulating FLIP-L expression. Int J Cancer 88(6):986–991
Hayashi T, Hideshima T, Akiyama M, Podar K, Yasui H, Raje N, Kumar S, Chauhan D, Treon SP, Richardson P, Anderson KC (2005) Molecular mechanisms whereby immunomodulatory drugs activate natural killer cells: clinical application. Br J Haematol 128(2):192–203. doi:10.1111/j.1365-2141.2004.05286.x, BJH5286 [pii]
Fujii H, Trudeau JD, Teachey DT, Fish JD, Grupp SA, Schultz KR, Reid GS (2007) In vivo control of acute lymphoblastic leukemia by immunostimulatory CpG oligonucleotides. Blood 109(5):2008–2013. doi:10.1182/blood-2006-02-002055, blood-2006-02-002055 [pii]
Brandau S, Riemensberger J, Jacobsen M, Kemp D, Zhao W, Zhao X, Jocham D, Ratliff TL, Bohle A (2001) NK cells are essential for effective BCG immunotherapy. Int J Cancer 92(5):697–702. doi:10.1002/1097-0215(20010601)92:5, <697::AID-IJC1245>3.0.CO;2-Z [pii]
Yamanegi K, Yamane J, Kobayashi K, Kato-Kogoe N, Ohyama H, Nakasho K, Yamada N, Hata M, Nishioka T, Fukunaga S, Futani H, Okamura H, Terada N (2010) Sodium valproate, a histone deacetylase inhibitor, augments the expression of cell-surface NKG2D ligands, MICA/B, without increasing their soluble forms to enhance susceptibility of human osteosarcoma cells to NK cell-mediated cytotoxicity. Oncol Rep 24(6):1621–1627
Yamanegi K, Yamane J, Kobayashi K, Kato-Kogoe N, Ohyama H, Nakasho K, Yamada N, Hata M, Fukunaga S, Futani H, Okamura H, Terada N (2012) Valproic acid cooperates with hydralazine to augment the susceptibility of human osteosarcoma cells to Fas- and NK cell-mediated cell death. Int J Oncol 41(1):83–91. doi:10.3892/ijo.2012.1438
Ogbomo H, Michaelis M, Kreuter J, Doerr HW, Cinatl J Jr (2007) Histone deacetylase inhibitors suppress natural killer cell cytolytic activity. FEBS Lett 581(7):1317–1322
Kopp LM, Ray A, Denman CJ, Senyukov VS, Somanchi SS, Zhu S, Lee DA (2013) Decitabine has a biphasic effect on natural killer cell viability, phenotype, and function under proliferative conditions. Mol Immunol 54(3–4):296–301. doi:10.1016/j.molimm.2012.12.012
Rao-Bindal K, Zhou Z, Kleinerman ES (2012) MS-275 sensitizes osteosarcoma cells to Fas ligand-induced cell death by increasing the localization of Fas in membrane lipid rafts. Cell Death Dis 3:e369. doi:10.1038/cddis.2012.101
Rao-Bindal K, Koshkina NV, Stewart J, Kleinerman ES (2013) The histone deacetylase inhibitor, MS-275 (Entinostat), downregulates c-FLIP, sensitizes osteosarcoma cells to FasL, and induces the regression of osteosarcoma lung metastases. Curr Cancer Drug Targets 13(4):411–422
Berg SL, Cairo MS, Russell H, Ayello J, Ingle AM, Lau H, Chen N, Adamson PC, Blaney SM (2011) Safety, pharmacokinetics, and immunomodulatory effects of lenalidomide in children and adolescents with relapsed/refractory solid tumors or myelodysplastic syndrome: a Children’s Oncology Group Phase I Consortium report. J Clin Oncol 29(3):316–323. doi:10.1200/JCO.2010.30.8387
Liu Y, Wu HW, Sheard MA, Sposto R, Somanchi SS, Cooper LJ, Lee DA, Seeger RC (2013) Growth and activation of natural killer cells ex vivo from children with neuroblastoma for adoptive cell therapy. Clin Cancer Res 19(8):2132–2143. doi:10.1158/1078-0432.CCR-12-1243
Wu L, Parton A, Lu L, Adams M, Schafer P, Bartlett JB (2011) Lenalidomide enhances antibody-dependent cellular cytotoxicity of solid tumor cells in vitro: influence of host immune and tumor markers. Cancer Immunol Immunother 60(1):61–73. doi:10.1007/s00262-010-0919-9
Talmadge JE, Schneider M, Collins M, Phillips H, Herberman RB, Wiltrout RH (1985) Augmentation of NK cell activity in tissue specific sites by liposomes incorporating MTP-PE. J Immunol 135(2):1477–1483
Kubista B, Trieb K, Blahovec H, Kotz R, Micksche M (2002) Hyperthermia increases the susceptibility of chondro- and osteosarcoma cells to natural killer cell-mediated lysis. Anticancer Res 22(2A):789–792
Yamada N, Yamanegi K, Ohyama H, Hata M, Nakasho K, Futani H, Okamura H, Terada N (2012) Hypoxia downregulates the expression of cell surface MICA without increasing soluble MICA in osteosarcoma cells in a HIF-1alpha-dependent manner. Int J Oncol 41(6):2005–2012. doi:10.3892/ijo.2012.1630
Balsamo M, Manzini C, Pietra G, Raggi F, Blengio F, Mingari MC, Varesio L, Moretta L, Bosco MC, Vitale M (2013) Hypoxia downregulates the expression of activating receptors involved in NK-cell-mediated target cell killing without affecting ADCC. Eur J Immunol 43(10):2756–2764. doi:10.1002/eji.201343448
Denman CJ, Senyukov VV, Somanchi SS, Phatarpekar PV, Kopp LM, Johnson JL, Singh H, Hurton L, Maiti SN, Huls MH, Champlin RE, Cooper LJ, Lee DA (2012) Membrane-bound IL-21 promotes sustained ex vivo proliferation of human natural killer cells. PLoS One 7(1):e30264. doi:10.1371/journal.pone.0030264
Tonn T, Schwabe D, Klingemann HG, Becker S, Esser R, Koehl U, Suttorp M, Seifried E, Ottmann OG, Bug G (2013) Treatment of patients with advanced cancer with the natural killer cell line NK-92. Cytotherapy. doi:10.1016/j.jcyt.2013.06.017
Chang YH, Connolly J, Shimasaki N, Mimura K, Kono K, Campana D (2013) A chimeric receptor with NKG2D specificity enhances natural killer cell activation and killing of tumor cells. Cancer Res 73(6):1777–1786. doi:10.1158/0008-5472.CAN-12-3558
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Tarek, N., Lee, D.A. (2014). Natural Killer Cells for Osteosarcoma. In: Kleinerman, M.D., E. (eds) Current Advances in Osteosarcoma. Advances in Experimental Medicine and Biology, vol 804. Springer, Cham. https://doi.org/10.1007/978-3-319-04843-7_19
Download citation
DOI: https://doi.org/10.1007/978-3-319-04843-7_19
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-04842-0
Online ISBN: 978-3-319-04843-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)