Background In spite of recent advances in the diagnosis and treatment of iNPH, favorable outcomes following CSF diversion continue to be limited by complications, both valve dependent and valve independent, as well as by a reduction, over time, in the response to shunting.
Materials and methods Between September 1997 and December 2006, 148 patients underwent ventriculo-peritoneal shunt surgery in our department. All patients underwent the implantation of gravitational valves. These patients were followed-up 3, 6 and 12 months after surgery and then at annual intervals.
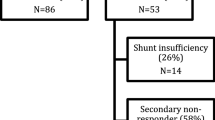
Findings The mean age of the 94 men and 54 women in our study was 68 years. The perioperative mortality was 0.7% (one patient died from a pulmonary embolism). A further 23 patients died during the follow-up period from causes unrelated to iNPH or the surgery. This study reports on groups of patients followed-up for 2 years (n=92), 3 years (n=62), 4 years (n=38) and 5 years (n=21) postoperatively. Valve independent complications occurred postoperatively in 6% of patients (n=10). Of these, five patients (3=of the total) had an infection and catheter displacement was recorded in a further five. Valve dependent complications occurred in 24 patients (16=), with overdrainage found in seven patients (5=) and underdrainage apparent in 17 (11=). Responder rates were 79= at 2 years, 79= at 3 years, 64= at 4 years and 60= at 5 years. The optimal valve opening pressure in programmable valves with a gravitational unit was between 30 and 70 mmHg.
Conclusions Sixty percent of patients with iNPH who underwent a ventriculo-peritoneal shunt using a gravitational valve continue to benefit from surgery 5 years postoperatively.
Access provided by Autonomous University of Puebla. Download to read the full chapter text
Chapter PDF
Similar content being viewed by others
Keywords
References
Boon AJ, Tans JT, Delwel EJ, Egeler-Peerdeman SM, Hanlo PW, Wurzer HA, Hermans J (1999) Dutch normal-pressure hydro-cephalus study: the role of cerebrovascular disease. J Neurosurg 90(2):221–2226
Børgesen SE (1984) Conductance to outflow of CSF in normal pressure Hydrocephalus. Acta Neurochir (Wien) 71:1–15
Decq P, Barat JL, Duplessis E, Leguerinel C, Gendrault P, Keravel Y (1995) Shunt failure in adult hydrocephalus: flow-controlled shunt versus differential pressure shunts—a cooperative study in 289 patients. Surg Neurol 43:333–339
Drake JM, Kestle JRW, Milner R (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43:294–305
Hebb AO, Cusimano MD (2002) Idiopathic normal pressure hydrocephalus: a systematic review of diagnosis and outcome. Neurosurgery 49:1166–1184
Kiefer M, Eymann R, Meier U (2002) Five years experience with gravitational shunts in chronic hydrocephalus of adults. Acta Neurochir (Wien) 144:755–767
Kiefer M, Eymann R, Komenda Y, Steudel WI (2003) A grading system for chronic hydrocephalus. Zentralbl Neurochir 64:109–115
Meier U (2004) Outcome of idiopathic normal pressure hydroceph-alus after surgery with gravity valves. Neurosurg Q 14:119–126
Mori K (2001) Management of idiopathic normal-pressure hydrocephalus: a multiinstitutional study conducted in Japan. J Neurosurg 95:970–973
Pollack IF, Albright AL, Adelson PD (1999) A randomized, controlled study of a programmable shunt valve versus a conventional valve for patients with hydrocephalus. Hakim-Medos Investigator Group. Neurosurgery 45:1399–1408
Sprung C, Miethke C, Shakeri K, Lanksch WR (1998) Pitfalls in shunting of hydrocephalus—clinical reality and improvement by the hydrostatic dual-switch valve. Eur J Pediatr Surg 8(Suppl 1):26–30
Zemack G, Romner B (2002) Adjustable valves in normal-pressure hydrocephalus: a retrospective study of 218 patients. Neurosurgery 51:1392–1400
Author information
Authors and Affiliations
Editor information
Rights and permissions
Copyright information
© 2008 Springer-Verlag/Wien
About this paper
Cite this paper
Meier, U., Lemcke, J., Al-Zain, F. (2008). Course of disease in patients with idiopathic normal pressure hydrocephalus (iNPH): a follow-up study 3, 4 and 5 years following shunt implantation. In: Steiger, H.J. (eds) Acta Neurochirurgica Supplements. Acta Neurochirurgica Supplementum, vol 102. Springer, Vienna. https://doi.org/10.1007/978-3-211-85578-2_25
Download citation
DOI: https://doi.org/10.1007/978-3-211-85578-2_25
Publisher Name: Springer, Vienna
Print ISBN: 978-3-211-85577-5
Online ISBN: 978-3-211-85578-2
eBook Packages: MedicineMedicine (R0)