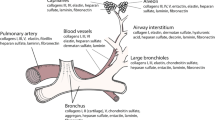
Abstract
The limited available treatment options for patients with chronic lung diseases, such as fibrosis, lead to poor prognosis after diagnosis and short survival rates. An exciting new bioengineering approach utilizes de- and recellularization of lung tissue to potentially overcome donor organ shortage and immune reactions toward the received transplant. The goal of decellularization is to create a scaffold which contains the necessary framework for stability and functionality for regenerating lung tissue while removing immunomodulatory factors by removal of cells. After decellularization, the scaffold could be re-functionalized by repopulation with the patient’s own stem/progenitor cells to create a fully functional organ or can be used as ex vivo models of disease. In this chapter the decellularization of lung tissue from multiple species (i.e., rodents, pigs, and humans) as well as disease states such as fibrosis is described. We discuss and describe the various quality control measures which should be used to characterize decellularized scaffolds, methods for protein analysis of the remaining scaffold, and methods for recellularization of scaffolds.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Moore BB, Hogaboam CM (2008) Murine models of pulmonary fibrosis. Am J Physiol Lung Cell Mol Physiol 294(2):L152–L160. doi:10.1152/ajplung.00313.2007
Mouratis MA, Aidinis V (2011) Modeling pulmonary fibrosis with bleomycin. Curr Opin Pulm Med 17(5):355–361. doi:10.1097/MCP.0b013e328349ac2b
Sokocevic D, Bonenfant NR, Wagner DE et al (2013) The effect of age and emphysematous and fibrotic injury on the re-cellularization of de-cellularized lungs. Biomaterials 34(13):3256–3269. doi:10.1016/j.biomaterials.2013.01.028
Schiller HB, Fernandez IE, Burgstaller G et al (2015) Time- and compartment-resolved proteome profiling of the extracellular niche in lung injury and repair. Mol Syst Biol 11(7):819. doi:10.15252/msb.20156123
Sun H, Zhu Y, Pan H et al (2016) Netrin-1 regulates fibrocyte accumulation in the decellularized fibrotic sclerodermatous lung microenvironment and in bleomycin-induced pulmonary fibrosis. Arthritis Rheumatol 68(5):1251–1261. doi:10.1002/art.39575
Price AP, England KA, Matson AM et al (2010) Development of a decellularized lung bioreactor system for bioengineering the lung: the matrix reloaded. Tissue Eng Part A 16(8):2581–2591. doi:10.1089/ten.TEA.2009.0659
Petersen TH, Calle EA, Zhao L et al (2010) Tissue-engineered lungs for in vivo implantation. Science 329(5991):538–541. doi:10.1126/science.1189345
Booth AJ, Hadley R, Cornett AM et al (2012) Acellular normal and fibrotic human lung matrices as a culture system for in vitro investigation. Am J Respir Crit Care Med 186(9):866–876. doi:10.1164/rccm.201204-0754OC
Gilpin SE, Guyette JP, Ren X et al (2013) Up-scaling decellularization and whole organ culture for human lung regeneration. J Heart Lung Transpl 32(4):S69–S70. doi:10.1016/j.healun.2013.01.172
Wagner DE, Bonenfant NR, Parsons CS et al (2014) Comparative decellularization and recellularization of normal versus emphysematous human lungs. Biomaterials 35(10):3281–3297. doi:10.1016/j.biomaterials.2013.12.103
Gilpin SE, Guyette JP, Gonzalez G et al (2014) Perfusion decellularization of human and porcine lungs: bringing the matrix to clinical scale. J Heart Lung Transplant 33(3):298–308. doi:10.1016/j.healun.2013.10.030
Wagner DE, Bonenfant NR, Sokocevic D et al (2014) Three-dimensional scaffolds of acellular human and porcine lungs for high throughput studies of lung disease and regeneration. Biomaterials 35(9):2664–2679. doi:10.1016/j.biomaterials.2013.11.078
Balestrini JL, Gard AL, Liu A et al (2015) Production of decellularized porcine lung scaffolds for use in tissue engineering. Integr Biol (Camb) 7(12):1598–1610. doi:10.1039/c5ib00063g
Platz J, Bonenfant NR, Uhl FE et al (2016) Comparative study to the use of decellularized alpha-Gal KO pig lungs for xenogeneic lung transplantation. Tissue Eng Part C Methods. doi:10.1089/ten.TEC.2016.0109
Godin LM, Sandri BJ, Wagner DE et al (2016) Decreased laminin expression by human lung epithelial cells and fibroblasts cultured in acellular lung scaffolds from aged mice. PLoS One 11(3):e0150966. doi:10.1371/journal.pone.0150966
Parker MW, Rossi D, Peterson M et al (2014) Fibrotic extracellular matrix activates a profibrotic positive feedback loop. J Clin Invest 124(4):1622–1635. doi:10.1172/jci71386
Zhou Y, Peng H, Sun H et al (2014) Chitinase 3-like 1 suppresses injury and promotes fibroproliferative responses in mammalian lung fibrosis. Sci Transl Med 6(240):240ra276. doi:10.1126/scitranslmed.3007096
Wallis JM, Borg ZD, Daly AB et al (2012) Comparative assessment of detergent-based protocols for mouse lung de-cellularization and re-cellularization. Tissue Eng Part C Methods 18(6):420–432. doi:10.1089/ten.TEC.2011.0567
Daly AB, Wallis JM, Borg ZD et al (2012) Initial binding and recellularization of decellularized mouse lung scaffolds with bone marrow-derived mesenchymal stromal cells. Tissue Eng Part A 18(1–2):1–16. doi:10.1089/ten.TEA.2011.0301
Bonvillain RW, Danchuk S, Sullivan DE et al (2012) A nonhuman primate model of lung regeneration: detergent-mediated decellularization and initial in vitro recellularization with mesenchymal stem cells. Tissue Eng Part A 18(23–24):2437–2452. doi:10.1089/ten.TEA.2011.0594
Lluri G, Langlois GD, McClellan B et al (2006) Tissue inhibitor of metalloproteinase-2 (TIMP-2) regulates neuromuscular junction development via a beta1 integrin-mediated mechanism. J Neurobiol 66(12):1365–1377. doi:10.1002/neu.20315
Zvarova B, Uhl FE, Uriarte JJ et al (2016) Residual detergent detection method for nondestructive cytocompatibility evaluation of decellularized whole lung scaffolds. Tissue Eng Part C Methods 22(5):418–428. doi:10.1089/ten.TEC.2015.0439
Reed W, Noga SJ, Gee AP et al (2009) Production Assistance for Cellular Therapies (PACT): four-year experience from the United States National Heart, Lung, and Blood Institute (NHLBI) contract research program in cell and tissue therapies. Transfusion 49(4):786–796. doi:10.1111/j.1537-2995.2008.02027.x
Yankaskas JR, Haizlip JE, Conrad M et al (1993) Papilloma virus immortalized tracheal epithelial cells retain a well-differentiated phenotype. Am J Phys 264(5 Pt 1):C1219–C1230
Bonenfant NR, Sokocevic D, Wagner DE et al (2013) The effects of storage and sterilization on de-cellularized and re-cellularized whole lung. Biomaterials 34(13):3231–3245. doi:10.1016/j.biomaterials.2013.01.031
Melo E, Cardenes N, Garreta E et al (2014) Inhomogeneity of local stiffness in the extracellular matrix scaffold of fibrotic mouse lungs. J Mech Behav Biomed Mater 37:186–195. doi:10.1016/j.jmbbm.2014.05.019
Moeller A, Ask K, Warburton D et al (2008) The bleomycin animal model: a useful tool to investigate treatment options for idiopathic pulmonary fibrosis? Int J Biochem Cell Biol 40(3):362–382. doi:10.1016/j.biocel.2007.08.011
Fernandez IE, Amarie OV, Mutze K et al (2016) Systematic phenotyping and correlation of biomarkers with lung function and histology in lung fibrosis. Am J Physiol Lung Cell Mol Physiol 310(10):L919–L927. doi:10.1152/ajplung.00183.2015
Crapo PM, Gilbert TW, Badylak SF (2011) An overview of tissue and whole organ decellularization processes. Biomaterials 32(12):3233–3243. doi:10.1016/j.biomaterials.2011.01.057
Griffin WC (1954) Calculation of HLB values of non-ionic surfactants. J Soc Cosmet Chem 5:249–256
Hjelmeland LM (1980) A nondenaturing zwitterionic detergent for membrane biochemistry: design and synthesis. Proc Natl Acad Sci U S A 77(11):6368–6370. doi:10.1073/pnas.77.11.6368
Ren X, Moser PT, Gilpin SE et al (2015) Engineering pulmonary vasculature in decellularized rat and human lungs. Nat Biotechnol 33(10):1097–1102. doi:10.1038/nbt.3354
Calle EA, Mendez JJ, Ghaedi M et al (2015) Fate of distal lung epithelium cultured in a decellularized lung extracellular matrix. Tissue Eng Part A 21(11–12):1916–1928. doi:10.1089/ten.TEA.2014.0511
Ghaedi M, Calle EA, Mendez JJ et al (2013) Human iPS cell-derived alveolar epithelium repopulates lung extracellular matrix. J Clin Invest 123(11):4950–4962. doi:10.1172/JCI68793
Gilpin SE, Ren X, Okamoto T et al (2014) Enhanced lung epithelial specification of human induced pluripotent stem cells on decellularized lung matrix. Ann Thorac Surg 98(5):1721–1729. doi:10.1016/j.athoracsur.2014.05.080
Sun H, Calle E, Chen X et al (2014) Fibroblast engraftment in the decellularized mouse lung occurs via a beta1-integrin-dependent, FAK-dependent pathway that is mediated by ERK and opposed by AKT. Am J Physiol Lung Cell Mol Physiol 306(6):L463–L475. doi:10.1152/ajplung.00100.2013
Sun Z, Gong X, Zhu H et al (2014) Inhibition of Wnt/beta-catenin signaling promotes engraftment of mesenchymal stem cells to repair lung injury. J Cell Physiol 229(2):213–224. doi:10.1002/jcp.24436
Ott HC, Clippinger B, Conrad C et al (2010) Regeneration and orthotopic transplantation of a bioartificial lung. Nat Med 16(8):927–933. doi:10.1038/nm.2193
Nichols JE, Niles J, Riddle M et al (2013) Production and assessment of decellularized pig and human lung scaffolds. Tissue Eng Part A 19(17–18):2045–2062. doi:10.1089/ten.TEA.2012.0250
Price AP, Godin LM, Domek A et al (2015) Automated decellularization of intact, human-sized lungs for tissue engineering. Tissue Eng Part C Methods 21(1):94–103. doi:10.1089/ten.TEC.2013.0756
Wagner DE, Uhl FE, Weiss DJ (2015) Acellular lung scaffolds in lung bioengineering. In: Bertoncello I (ed) Stem cells in the lung: development. Repair and Regeneration. Springer International Publishing, Cham, pp 309–347. doi:10.1007/978-3-319-21082-7_18
Huleihel L, Hussey GS, Naranjo JD et al (2016) Matrix-bound nanovesicles within ECM bioscaffolds. Sci Adv 2(6):e1600502. doi:10.1126/sciadv.1600502
Acknowledgments
The authors are grateful to Douglas Taatjes Ph.D. and Nicole Bishop of the UVM Microscopy and Imaging Center for assistance with IHC staining, transmission electron microscopy imaging, and image interpretations. We would like to thank Caroline Andrews, Nicholas Bonenfant, Zachary Borg, Amy Coffey, Amanda Daly, Jacob Dearborn, Nathan Gasek, Ethan Griswold, Zachary Phillips, Joseph Platz, Alexander Riveron, Dino Sokocevic, John Wallis, Sean Wrenn, and Basa Zvorova for the assistance with lung decellularizations, microscopy, and analysis of the detergent effluents. Studies were supported by the NIH RO1 HL127144-01 (DJW), Vermont Lung Center CoBRE grant (P20RR15557), NIH PACT program (contract HHSN268201000008C), NHBLI Lung Biology Training grant T32 HL076122, NIH Institutional Development Award (IDeA) NIGMS grant P20GM103449, and NCRR grant P40RR017447.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer Science+Business Media LLC
About this protocol
Cite this protocol
Uhl, F.E., Wagner, D.E., Weiss, D.J. (2017). Preparation of Decellularized Lung Matrices for Cell Culture and Protein Analysis. In: Rittié, L. (eds) Fibrosis. Methods in Molecular Biology, vol 1627. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4939-7113-8_18
Download citation
DOI: https://doi.org/10.1007/978-1-4939-7113-8_18
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4939-7112-1
Online ISBN: 978-1-4939-7113-8
eBook Packages: Springer Protocols