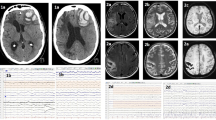
Abstract
Management of seizures and epilepsy in persons who have had a cerebrovascular accident is a complex process involving a number of decisions. Was the event in question an epileptic seizure? If so, should treatment be initiated after a single seizure? If treatment is considered necessary, which antiepileptic drug (AED) should be used to prevent seizure recurrence?
Seizures may present in different settings. Some seizures present in the acute phase of a cerebrovascular accident, often when the patient is in the intensive care unit. Others present weeks or months after a stroke, in which case the recurrence rate is high if untreated, often leading to the diagnosis of epilepsy, rather than single seizures. The pathophysiology, treatment modalities, and consequences of acute poststroke events differ greatly from late seizures and are discussed separately in this chapter. In addition, we discuss the challenges associated with management of seizures and epilepsy in the elderly (Leppik, Walczak, Birnbaum, Lancet, 380:1128–1130, 2012).
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Comorbidity of Epilepsy and Stroke
Cerebrovascular disorders are one of the most common identifiable causes of epilepsy, especially in the elderly [1]. Seizures after a stroke can occur early, within 7–14 days [2–6], or late, after 14 days [7–10]. Early seizures do not necessarily progress to epilepsy, but may result in increased morbidity and mortality. Reports vary considerably regarding the incidence of single seizures and epilepsy after a stroke. In adults younger than 50 years of age, 12.7 % with ischemic strokes and 25.6 % with intracranial hemorrhage developed epilepsy. This study used the more recent definition of epilepsy, which is the occurrence of a single seizure associated with an enduring condition associated with epilepsy. Another large study reported the occurrence of seizures in 168 (8.9 %) of 1897 persons following an ischemic stroke and 28 (10.6 %) of 265 after a hemorrhagic stroke [4]. Most seizures occurred within 2 years of the stroke.
A critical question addressing the issue of treatment is the occurrence of a second seizure after a single seizure. Unfortunately, this is a difficult question to answer from the literature. Many physicians initiate treatment with antiepileptic drugs (AEDs) following a single seizure because of the perception that there is a high risk of additional seizures in the context of stroke and seizure. Thus, reports of recurrent seizures are confounded with treatment, and it is difficult to establish the risk of epilepsy as defined by two or more unprovoked seizures. In one study by Arntz, 75 % of persons with an ischemic stroke and 80 % with a hemorrhagic stroke were prescribed AEDs. Nevertheless, nine with ischemic and four with hemorrhagic had additional seizures during AED treatment.
There is a paucity of data regarding morbidity and mortality resulting from seizures after a stroke; however, at least one study, the Canadian Registry, has shown a higher mortality rate at 30 days (36.2 %) and 1 year (48.6 %). The presence of seizures may also lead to longer hospital stay and disability [11].
Management
Clear evidence to support the role of prophylactic seizure medications in patients with ischemic and hemorrhagic stroke is lacking. The Cochrane review published in 2010 (covering a period of almost 60 years) did not find any randomized controlled trials evaluating the role of AEDs in either primary or secondary prevention of seizures post stroke and highlighted that there was not enough evidence for the use of AEDs in either primary or secondary prevention of seizures post stroke [12]. A more recent Cochrane review for primary or secondary prevention of seizures after subarachnoid hemorrhage (SAH) did not show any evidence to support or oppose the use of these as prophylaxis [13].
Based on currently available evidence, most neurologists support not initiating an AED for prevention of poststroke seizures. However, if a seizure occurs in the setting of a stroke, an AED is often started due to high risk of recurrence due to the underlying structural lesion. The duration of treatment depends on many variables. The risk–benefit ratio must be evaluated carefully, particularly in the elderly patients. A careful review of all the other medications that may interact with the AED chosen (including lowering of seizure threshold) has to be done to avoid poor outcomes. In most cases, a single AED is sufficient to control poststroke seizures when treatment was required [8].
The choice of an AED depends on many variables as well. No randomized clinical trials have explored the evaluation of older versus newer AEDs in stroke-related epilepsy. However, the newer agents offer the advantage of fewer side effects, which makes them appropriate to use particularly in the elderly [14, 15, 35]. A few studies have shown gabapentin and lamotrigine to be effective in the treatment of late-onset poststroke seizures [16, 17].
Several studies have tried to review early versus late onset of seizures and the role of AEDs. In poststroke seizures, there has been no evidence that AEDs affect the course of recurrent seizures after treatment is discontinued. Some studies suggest that AED treatment can be discontinued in early seizures after a month if there are no further seizures noted [18, 19].
The effects of poststroke seizures on the outcome of stroke are unclear, with conflicting reports from different studies [20]. However, the factor with the most impact on stroke outcome is the underlying cause of stroke itself.
Choosing the Right AED
Stroke incidence rises with every age decade, and the bulk of stroke patients are over 60 years of age. Age-related physiologic changes directly impact the blood levels of AEDs by influencing protein binding and reduction in liver volume and blood flow. Because of the complexity of confounding variables and the lack of correlation between simple measures of liver function and drug metabolism, the effect of age on hepatic drug metabolism remains largely unknown [21]. Interestingly, genetic determinants of hepatic isoenzymes may be more important than age in determining a person’s clearance [22].
Renal clearance is the major route of elimination for a number of newer AEDs. It is well known that an elderly person’s renal capacity decreases by approximately 10 % per decade [23]. However, there exists a substantial amount of individual variability because clearance is also highly dependent upon the patient’s general state of health [24]. Thus, purely age-based dose recommendations may not be appropriate. Measurements of serum creatinine and estimations of creatinine clearance may be more helpful in determining the dose. Measurement of the actual AED concentration at steady state is the most accurate means to determine that the dose is appropriate. Despite the known effects of age-related physiologic changes on drug disposition and the widespread use of AEDs in the elderly, few studies on AED pharmacokinetics in the elderly have been published.
Variability of AED Levels over Time
Studies have shown that in compliant patients, the variability of AED concentrations over time is relatively small. Compliant clinic patients experienced variability of approximately 20–25 % [25, 26]. Approximately 5–10 % of this variability may be due to inter-laboratory variability in measurement of drug concentrations, although laboratories not following rigid quality control standards may experience even larger amounts of variability. The remainder of noted variability arises from day-to-day alterations in absorption, metabolism, or differences in AED manufacturing processes between brand and generic drugs. In nursing homes, however, some patients experienced a difference in concentration of two- to threefold from the lowest to the highest level [27].
Clinical Trials of AEDs in the Elderly
All major AEDs have a Food and Drug Administration (FDA) indication for use for the seizure types most likely to be encountered in the elderly. However, there are little data relating specifically to these drugs in the elderly, and those that are available have been limited to the community-dwelling elderly. One post hoc Veterans Administration (VA) cooperative study of carbamazepine and valproate found that elderly patients often had seizure control associated with lower AED levels than those seen in younger subjects. Notably, these elderly patients also experienced side effects at lower levels compared with those seen in younger subjects [28].
A multicenter, double-blind, randomized comparison between lamotrigine and carbamazepine in newly diagnosed epileptic elderly patients (mean = 77 years of age) in the UK showed that the main difference between the two groups was the rate of drop out due to adverse events, with lamotrigine incurring an 18 % dropout rate compared to that of carbamazepine which incurred a 42 % dropout rate [29]. The VA Cooperative Study #428, an 18-center, parallel, double-blind trial on the use of gabapentin, lamotrigine, and carbamazepine in patients ≥ 60 years of age found that drug efficacy did not differ, but the main finding favoring the two newer AEDs was better tolerability than carbamazepine [30].
Choosing AEDs for the Elderly
At the present time, there are little data regarding the clinical use of AEDs in the elderly. The paucity of information makes it very difficult to recommend specific AEDs with any confidence that outcomes will be optimal. A drug that is optimal for the elderly healthy with only epilepsy may not be appropriate for elderly with multiple medical problems or the frail elderly.
Phenytoin
Phenytoin is effective for localization-related epilepsies, and thus has an efficacy profile appropriate for the elderly. Evidence for this can be gathered from a VA cooperative study that included elderly patients that found phenytoin to be as effective as carbamazepine, phenobarbital, and primidone, but that phenytoin and carbamazepine were better tolerated [31]. Phenytoin has a narrow therapeutic range, is approximately 90 % bound to serum albumin, and undergoes saturable metabolism, which has the effect of producing nonlinear changes in serum concentrations when the dose is changed or absorption is altered. Clinical studies in elderly patients have shown decrease in phenytoin binding to albumin and increase in free fraction. A recent study suggested that metabolism does not decrease greatly with age in healthy elderly. Using stable-labeled (nonradioactive) phenytoin to very precisely measure the phenytoin clearance, one study found that advancing age was not as much of a factor as had been previously reported [32]. A range of 5–15 mg/L total may be more appropriate as a therapeutic range for the elderly due to abnormal protein binding [33].
Phenytoin has many drug–drug interactions and should be used cautiously in elderly patients receiving other medications. There is also some indication that selective serotonin reuptake inhibitor (SSRI) antidepressants may inhibit the cytochrome 2C family of P450 enzymes responsible for metabolizing phenytoin. Fluoxetine and norfluoxetine are more potent inhibitors of this enzyme, followed by sertraline and paroxetine. The latter two SSRI antidepressants may prove to be a safer choice in the elderly. Coumadin also has a very complicated interaction with phenytoin, and often doses of both need to be manipulated.
Phenytoin is also known to be a mild blocker of cardiac conduction, and should be used cautiously in persons with conduction defects, especially heart blocks. Phenytoin is the least expensive major AED, but because of its issues that may lead to complications, its global cost may be greater than the cost of newer AEDs .
Carbamazepine
Carbamazepine is effective for localization-related epilepsies, and thus has an efficacy profile appropriate for the elderly. Evidence from two large VA cooperative studies showed it to be as effective as phenytoin, phenobarbital, primidone, and valproate, but better tolerated than the latter three [31, 34]. Two studies of new-onset epilepsy in the community-dwelling elderly found it to be as effective as lamotrigine, but noted that it had a higher incidence of side effects [29, 30].
The apparent clearance of carbamazepine has been reported to be 20–40 % lower in the elderly as compared to adults [26, 35, 36]. Carbamazepine has some significant drug–drug interactions with medications that inhibit the cytochrome P450 enzyme, CYP3A4. Among the inhibitors are erythromycin, fluoxetine, ketoconazole, propoxyphene (Darvon), and cimetidine (Tagamet). At least one food (grapefruit juice) has been identified to interact with carbamazepine, causing increase in its serum concentrations. Elderly healthy patients will need to be cautioned about these interactions, and should be instructed to inform the physician whenever they are beginning a new medication, including any over-the-counter medications. A major concern with carbamazepine is its effect on sodium levels. The hyponatremia associated with carbamazepine is more pronounced as a person becomes older [37]. This may become more problematic if a person is on a salt restriction diet or a diuretic. Carbamazepine is also known to affect cardiac rhythms, and should be used cautiously, if at all, in persons with rhythm disturbances.
Phenobarbital
Although phenobarbital is the least expensive of all AEDs, its side-effect profile, which includes worsening of cognition and depression, makes it an undesirable drug for the elderly, especially in the nursing home setting where declines in cognition are already present.
Valproic Acid
Only a few studies have compared the pharmacokinetics of valproic acid in young and old patients [38, 39]. Total valproic acid clearances are similar in young and elderly individuals; however, unbound clearance is higher in the elderly [40].
Much like phenytoin, valproic acid is associated with reduced protein binding and unbound clearance in the elderly. Because of its effects on mood stabilization, it may be especially appropriate for elderly patients with a need for this effect.
Gabapentin
Gabapentin is effective for localization-related epilepsies, and has an efficacy profile appropriate for the elderly. Gabapentin is not metabolized by the liver, but rather renally excreted; therefore, there are no drug–drug interactions [41].There is, however, a reduction of renal function that correlates with advancing age, so doses may need to be adjusted. Because gabapentin is effective in treating neuralgic pain, it may be additionally beneficial for someone suffering from both epilepsy and pain. The VA Cooperative Study #428 compared carbamazepine with gabapentin and lamotrigine. Efficacies were similar but withdrawal related to side effects was highest for carbamazepine [30].
Lamotrigine
Lamotrigine is effective for localization-related epilepsies, and has an efficacy profile appropriate for the elderly. However, very few studies regarding lamotrigine and its effects on the elderly have been published. Lamotrigine is primarily metabolized by the liver using the glucuronidation pathway, which, unlike the P450 system, is thought to be less affected by age [42]. Data from a population pharmacokinetic study of 163 epilepsy patients, which only included 30 subjects greater than 65 years of age, 10 subjects between 70 and 76 years of age and no subjects from the old-old age group, showed that age did not affect lamotrigine apparent clearance [43]. Based on a study of 150 elderly subjects, the dropout rate due to adverse events was lower with lamotrigine (18 %) than with carbamazepine (42 %). The difference was attributable to the finding that lamotrigine subjects had fewer rashes (lamotrigine 3 %, carbamazepine 19 %) and fewer complaints of somnolence (lamotrigine 12 %, carbamazepine 29 %) [29]. Elderly community-dwelling epilepsy patients aged 59–92 years from the VA Cooperative Study #428 showed that lamotrigine apparent clearance can be effected by blood urea nitrogen and serum creatinine ratio, weight, and phenytoin use [44].
Levetiracetam
Levetiracetam has been approved as an adjunctive therapy for partial-onset seizures in adults. Levetiracetam is extremely water soluble, which allows for rapid and complete absorption after oral administration. Levetiracetam is not metabolized by the liver, and thus is free of nonlinear elimination kinetics, auto-induction kinetics, and drug–drug interactions. Lack of protein binding (< 10 %) also avoids the problems of displacing highly protein-bound drugs and the monitoring of unbound concentrations. Also, lack of drug interactions would make it useful for treating elderly epilepsy patients, particularly those patients who have other illnesses and are taking other medications [45]. Notably, the manufacturer reports a decrease of 38 % in total body clearance and an increased half-life up to 2.5 h longer in elderly subjects (age 61–88 years) who exhibited creatinine clearances ranging from 30 to 74 mL/min. However, doses do need to be adjusted depending on the renal function of the patient as measured by serum creatinine and levetiracetam concentrations [46].
One prospective phase 4 study indicates a favorable efficacy profile in the elderly [47]. Levetiracetam also appears to have a favorable safety profile. It was initially studied as a potential agent for treating cognitive disorders in the elderly, and thus a considerable amount of data regarding its tolerability in this age group is available. Analysis of 3252 elderly persons involved in studies of levetiracetam for epilepsy and other conditions demonstrated that levetiracetam was well tolerated by the elderly [48] .
Oxcarbazepine
Oxcarbazepine appears to have a more powerful effect on sodium balance than carbamazepine, and this effect has been shown to increase with age resulting in more pronounced hyponatremia in this age group [37]. This effect may make it a particularly problematic AED in the elderly who may likely be on antihypertensive agents and other drugs that can alter sodium balance.
Pregabalin
Pregabalin is related to gabapentin but is more potent, with doses of only one fifth those of gabapentin needed for therapeutic effect. Its absorption also appears to be more predictable because of the lower amounts transported across the intestinal system. Although it may prove to be a favorable AED for the elderly, its cost and lack of experimental and clinical data may limit its use.
Topiramate
Topiramate is effective for localization-related epilepsies, and thus has an efficacy profile appropriate for the elderly. Topiramate is approximately 20 % bound to serum proteins and is both metabolized by the liver and excreted unchanged in the urine. The enzymes involved in topiramate’s metabolism have not been identified; however, the cytochrome P450 system may be involved. Topiramate clearance may decrease with age, causing higher than expected serum concentrations with doses that are used in younger adults. Topiramate does have effects on cognitive functioning, especially at higher levels. However, it is not known if the elderly will be more sensitive to this problem.
Zonisamide
Zonisamide is effective for localization-related epilepsies [49]. Protein binding is approximately 40 % and its major elimination pathway is hepatic as a substrate of CYP3A4. It may thus have interactions with other drugs using this pathway. In addition to the usual side effects of AEDs of somnolence and dizziness, zonisamide may be associated with weight loss. It has an association with the development of renal calculi in approximately 1–2 % of persons during chronic use [50].
Drug Interactions with Non-AEDs
Co-medications are frequently used by elderly patients. Many concomitant medications taken by elderly patients can alter the absorption, distribution, and metabolism of AEDs, thereby increasing the risk of toxicity or therapeutic failure.
Calcium-containing antacids and sucralfate reduce the absorption of phenytoin [51, 52].The absorption of phenytoin, carbamazepine, and valproate may be reduced significantly by oral antineoplastic drugs that damage gastrointestinal cells [53, 54]. In addition, phenytoin concentrations may be lowered by intravenously administered antineoplastic agents [53, 54]. The use of folic acid for treatment of megaloblastic anemia may decrease serum concentrations of phenytoin and enteral feedings can also lower serum concentrations in patients receiving orally administered phenytoin [55].
Many drugs displace AEDs from plasma proteins, an effect that is especially serious when the interacting drug also inhibits the metabolism of the displaced drug; this occurs when valproate interacts with phenytoin. Several drugs used on a short-term basis (including propoxyphene and erythromycin) or as a maintenance therapy (such as cimetidine, diltiazem, fluoxetine, and verapamil) significantly inhibit the metabolism of one or more AEDs that are metabolized by the P450 system. Certain agents can induce the P450 system or other enzymes, causing an increase in drug metabolism. The most commonly prescribed inducers of drug metabolism are phenytoin, phenobarbital, carbamazepine, and primidone. Ethanol, when used chronically, also induces drug metabolism [56] .
The interaction between antipsychotic drugs and AEDs is complex. Hepatic metabolism of certain antipsychotics such as haloperidol can be increased by carbamazepine, resulting in diminished psychotropic response. Antipsychotic medications, especially chlorpromazine, promazine, trifluoperazine, and perphenazine, can reduce the threshold for seizures, and the risk of seizure is directly proportional to the total number of psychotropic medications being taken, their doses, any abrupt increases in doses, and the presence of organized brain pathology [57]. The epileptic patient taking antipsychotic drugs may need a higher dose of antiepileptic medication to control seizures. In contrast, central nervous system depressants are likely to lower the maximum dose of AEDs that can be administered before toxic symptoms occur [58–60].
Compliance
Adherence to a prescribed regimen (compliance) is a challenge in the elderly due to multiple medications, memory problems, and visual issues. In general, twice-daily dosing is preferable. In long-term care facilities, drug adherence may be less of an issue than with community-dwelling elderly patients; however, reductions in staff and time spent on the multiple administration of medicines may help to reduce errors and cost [61–69].
Summary
Seizures after a stroke are not uncommon, and early recognition and appropriate management can lead to reduction in morbidity and mortality as well as contribute to reducing functional restrictions. This is particularly important in the elderly, who may have other comorbidities which result in delayed diagnosis, especially if nonconvulsive status epilepticus is present. Although there is no role of primary prevention of seizures after stroke, AED is often introduced after a seizure. The duration and choice of agent have to be carefully determined according to patient profile. As the care of both stroke and seizures continues to improve, better guidelines may emerge in the future to evaluate, manage, and prevent further morbidity and mortality in those patients with poststroke seizures. At the present time, management of seizures in the elderly is more an art than a science, and more studies are needed.
References
Leppik IE, Walczak TS, Birnbaum AK. Challenges of epilepsy in the elderly. Lancet. 2012;380:1128–30.
Ferro JM, Pinto F. Poststroke epilepsy: epidemiology, pathophysiology and management. Drugs Aging. 2004;21(10):639–53.
Forsgren L, Bucht G, Eriksson S, Bergmark L. Incidence and clinical characterization of unprovoked seizures in adults: a prospective population-based study. Epilepsia. 1996;37(3):224–9.
Bladin CF, Alexandrov AV, Bellavance A, Bornstein N, Chambers B, Cote R, Lebrun L, Pirisi A, Norris JW. Seizures after stroke: a prospective multicenter study. Arch Neurol. 2000;57(11):1617–22.
Labovitz DL, Hauser WA, Sacco RL. Prevalence and predictors of early seizure and status epilepticus after first stroke. Neurology. 2001;57(2):200–6.
Lamy C, Domigo V, Semah F, Arquizan C, Trystram D, Coste J, Mas JL, Patent Foramen Ovale and Atrial Septal Aneurysm Study Group. Early and late seizures after cryptogenic ischemic stroke in young adults. Neurology. 2003;60(3):400–4.
Gupta SR, Naheedy MH, Elias D, Rubino FA. Postinfarction seizures. A clinical study. Stroke. 1988;19(12):1477–81.
Kilpatrick CJ, Davis SM, Hopper JL, Rossiter SC. Early seizures after acute stroke. Risk of late seizures. Arch Neurol. 1992;49(5): 509–11.
Giroud M, Gras P, Fayolle H, Andre N, Soichot P, Dumas R. Early seizures after acute stroke: a study of 1,640 cases. Epilepsia. 1994;35(5):959–64.
Ryvlin P, Montavont A, Nighoghossian N. Optimizing therapy of seizures in stroke patients. Neurology. 2006; 67(12 Suppl 4):S3–9.
Burneo JG, Fang J, Saposnik G, and Investigators of the Registry of the Canadian Stroke Network. Impact of seizures on morbidity and mortality after stroke: a Canadian multi-centre cohort study. Eur J Neurol. 2010;17(1):52–8.
Kwan J, Wood E. Antiepileptic drugs for the primary and secondary prevention of seizures after stroke. Cochrane Database Syst Rev. 2010;2010(1):CD005398.
Marigold R, Gunther A, Tiwari D, Kwan J. Antiepileptic drugs for the primary and secondary prevention of seizures after subarachnoid haemorrhage. Cochrane Database Syst Rev. 2013;6:CD008710.
Consoli D, Bosco D, Postorino P, Galati F, Plastino M, Perticoni GF, Ottonello GA, Passarella B, Ricci S, Neri G, Toni D, and EPIC Study. Levetiracetam versus carbamazepine in patients with late poststroke seizures: a multicenter prospective randomized open-label study (EpIC Project). Cerebrovasc Dis. 2012;34(4):282–9.
Kutlu G, Gomceli YB, Unal Y, Inan LE. Levetiracetam monotherapy for late poststroke seizures in the elderly. Epilepsy Behav. 2008;13(3):542–4.
Gilad R. Management of seizures following a stroke: what are the options? Drugs Aging. 2012;29(7):533–8.
Glauser T, Ben-Menachem E, Bourgeois B, Cnaan A, Chadwick D, Guerreiro C, Kalviainen R, Mattson R, Perucca E, Tomson T. ILAE treatment guidelines: evidence-based analysis of antiepileptic drug efficacy and effectiveness as initial monotherapy for epileptic seizures and syndromes. Epilepsia. 2006;47(7):1094–120.
Cervoni L, Artico M, Salvati M, Bristot R, Franco C, Delfini R. Epileptic seizures in intracerebral hemorrhage: a clinical and prognostic study of 55 cases. Neurosurg Rev. 1994;17(3):185–8.
Qureshi AI, Tuhrim S, Broderick JP, Batjer HH, Hondo H, Hanley DF. Spontaneous intracerebral hemorrhage. N Engl J Med. 2001;344(19):1450–60.
Myint PK, Staufenberg EF, Sabanathan K. Post-stroke seizure and post-stroke epilepsy. Postgrad Med J. 2006;82(971):568–72.
Cusack BJ. Drug metabolism in the elderly. J Clin Pharmacol. 1988;28(6):571–6.
Ahn JE, Cloyd JC, Brundage RC, Marino SE, Conway JM, Ramsay RE, White JR, Musib LC, Rarick JO, Birnbaum AK, Leppik IE. Phenytoin half-life and clearance during maintenance therapy in adults and elderly patients with epilepsy. Neurology. 2008;71(1):38–43.
Rowe JW, Andres R, Tobin JD, Norris AH, Shock NW. The effect of age on creatinine clearance in men: a cross-sectional and longitudinal study. J Gerontol. 1976;31(2):155–63.
Fehrman-Ekholm I, Skeppholm L. Renal function in the elderly (> 70 years old) measured by means of iohexol clearance, serum creatinine, serum urea and estimated clearance. Scand J Urol Nephrol. 2004;38(1):73–7.
Leppik IE, Cloyd JD, Sawchuk RJ, Pepin SM. Compliance and variability of plasmaphenytoin levels in epileptic patients. Ther Drug Mon. 1979;1:475–83.
Graves NM, Holmes GB, Leppik IE. Compliant populations: variability in serum concentrations. Epilepsy Res Suppl. 1988;1:91–9.
Privitera MD, Strawsburg RH. 1994. Electroencephalographic monitoring in the emergency department. Emerg Med Clin North Am. 12(4):1089–100.
Ramsay R, Rowan A, Slater J, Collins J, Nemire R, Oritz W. Effect of age on epilepsy and its treatment results from the VA cooperative study. Epilepsia. 1994;35 Suppl 8:91.
Brodie MJ, Overstall PW, Giorgi L. Multicentre, double-blind, randomised comparison between lamotrigine and carbamazepine in elderly patients with newly diagnosed epilepsy. The UK Lamotrigine 1Elderly Study Group. Epilepsy Res. 1999;37(1):81–7.
Rowan AJ, Ramsay RE, Collins JF, Pryor F, Boardman KD, Uthman BM, Spitz M, Frederick T, Towne A, Carter GS, Marks W, Felicetta J, Tomyanovich ML. New onset geriatric epilepsy: a randomized study of gabapentin, lamotrigine, and carbamazepine. Neurology. 2005;64(11):1868–73.
Mattson RH, Cramer JA, Collins JF, Smith DB, Delgado-Escueta AV, Browne TR, Williamson PD, Treiman DM, McNamara JO, McCutchen CB, et al. Comparison of carbamazepine, phenobarbital, phenytoin, and primidone in partial and secondarily generalized tonic-clonic seizures. N Engl J Med. 1985;313(3):145–51.
Ahn J, Cloyd J, Brundage R, Marino S, Conway J, Ramsay R, White J, Musib L, Rarick J, Birnbaum A, Leppik I. Phenytoin half-life and clearance during maintenance therapy in adults and elderly patients with epilepsy. Neurology. 2008;71:38–43.
Leppik IE. Contemporary diagnosis and management of the patient with epilepsy. 6th ed. Newtown: Handbooks in Healthcare; 2006.
Mattson RH, Cramer JA, Collins JF. A comparison of valproate with carbamazepine for the treatment of complex partial seizures and secondarily generalized tonic-clonic seizures in adults. The Department of Veterans Affairs Epilepsy Cooperative Study No. 264 Group. N Engl J Med. 1992;327(11):765–71.
Cloyd JC, Lackner TE, Leppik IE. Antiepileptics in the elderly. Pharmacoepidemiology and pharmacokinetics. Arch Fam Med. 1994;3(7):589–98.
Graves NM, Brundage RC, Wen Y, Cascino G, So E, Ahman P, Rarick J, Krause S, Leppik IE. Population pharmacokinetics of carbamazepine in adults with epilepsy. Pharmacotherapy. 1998;18(2):273–81.
Dong X, Leppik IE, White J, Rarick J. Hyponatremia from oxcarbazepine and carbamazepine. Neurology. 2005;65(12):1976–8.
Bryson SM, Verma N, Scott PJ, Rubin PC. Pharmacokinetics of valproic acid in young and elderly subjects. Br J Clin Pharmacol. 1983;16(1):104–5.
Perucca E, Grimaldi R, Gatti G, Pirracchio S, Crema F, Frigo GM. Pharmacokinetics of valproic acid in the elderly. Br J Clin Pharmacol. 1984;17(6):665–9.
Birnbaum AK, Hardie NA, Conway JM, Bowers SE, Lackner TE, Graves NM, Leppik IE. Valproic acid doses, concentrations, and clearances in elderly nursing home residents. Epilepsy Res. 2004;62(2–3):157–62.
Richens A. Clinical pharmacokinetics of gabapentin. London: Royal Society of Medicine Services; 1993.
Peck AW. Clinical pharmacology of lamotrigine. Epilepsia. 1991;32 Suppl 2:S9–12.
Hussein Z, Posner J. Population pharmacokinetics of lamotrigine monotherapy in patients with epilepsy: retrospective analysis of routine monitoring data. Br J Clin Pharmacol. 1997;43(5):457–65.
Rowan A, Ramsay R, Collins J, et al. New onset geriatric epilepsy: a randomized study of gabapentin, lamotrigine, and carbamazepine. Neurology. 2005;64:1868–73.
Patsalos PN, Sander JW. Newer antiepileptic drugs. Towards an improved risk-benefit ratio. Drug Saf. 1994;11(1):37–67.
French J. Use of levetiracetam in special populations. Epilepsia. 2001;42 Suppl 4:40–3.
Morrell MJ, Leppik I, French J, Ferrendelli J, Han J, Magnus L. The KEEPER trial: levetiracetam adjunctive treatment of partial-onset seizures in an open-label community-based study. Epilepsy Res. 2003;54(2–3):153–61.
Cramer JA, Leppik IE, Rue KD, Edrich P, Kramer G. Tolerability of levetiracetam in elderly patients with CNS disorders. Epilepsy Res. 2003;56(2–3):135–45.
Leppik IE, Willmore LJ, Homan RW, From G, Oommen KJ, Penry JK, Sackellares JC, Smith DB, Lesser RP, Wallace JD, Trudeau JL, Lamoreaux LK, Spencer M. Efficacy and safety of zonisamide: results of a multicenter study. Epilepsy Res. 1993;14:165–73.
Wroe O. Zonisamide and renal calculi in patients with epilepsy: how big an issue? Curr Med Res Opin. 2007;23(8):1765–73.
Nation RL, Evans AM, Milne RW. Pharmacokinetic drug interactions with phenytoin (Part I). Clin Pharmacokinet. 1990a;18(1):37–60.
Nation RL, Evans AM, Milne RW. Pharmacokinetic drug interactions with phenytoin (Part II). Clin Pharmacokinet. 1990b;18(2):131–50.
Bollini P, Riva R, Albani F, Ida N, Cacciari L, Bollini C, Baruzzi A. Decreased phenytoin level during antineoplastic therapy: a case report. Epilepsia. 1983;24(1):75–8.
Neef C, de Voogd-van der Straaten I. An interaction between cytostatic and anticonvulsant drugs. Clin Pharmacol Ther. 1988;43(4):372–5.
Haley CJ, Nelson J. Phenytoin-enteral feeding interaction. Dicp—Ann Pharmacother. 1989;23(10):796–8.
Sandor P, Sellers EM, Dumbrell M, Khouw V. Effect of short- and long-term alcohol use on phenytoin kinetics in chronic alcoholics. Clin Pharmacol Ther. 1981;30(3):390–7.
Cold JA, Wells BG, Froemming JH. Seizure activity associated with antipsychotic therapy. Dicp—Ann Pharmacother. 1990;24(6):601–6.
Alvarez-Sabin J, Montaner J, Padro L, Molina CA, Rovira R, Codina A, Quintana M. Gabapentin in late-onset poststroke seizures. Neurology. 2002;59(12):1991–3.
Belcastro V, Vidale S, Pierguidi L, Sironi L, Tancredi L, Striano P, Taborelli A, Arnaboldi M. Intravenous lacosamide as treatment option in post-stroke non convulsive status epilepticus in the elderly: a proof-of-concept, observational study. Seizure. 2013;22(10):905–7.
Carrera E, Michel P, Despland PA, Maeder-Ingvar M, Ruffieux C, Debatisse D, Ghika J, Devuyst G, Bogousslavsky J. Continuous assessment of electrical epileptic activity in acute stroke. Neurology. 2006;67(1):99–104.
Dawling S, Crome P. Clinical pharmacokinetic considerations in the elderly. An update. Clin Pharmacokinet. 1989;17(4):236–63.
Greenblatt DJ. Reduced serum albumin concentration in the elderly: a report from the Boston collaborative drug surveillance program. J Am Geriatr Soc. 1979;27(1):20–2.
Jordan KG. Continuous EEG and evoked potential monitoring in the neuroscience intensive care unit. J Clin Neurophysiol. 1993;10(4):445–75.
Nelson MH, Birnbaum AK, Remmel RP. Inhibition of phenytoin hydroxylation in human liver microsomes by several selective serotonin re-uptake inhibitors. Epilepsy Res. 2001;44(1):71–82.
Tiula E, Neuvonen PJ. Antiepileptic drugs and alpha 1-acid glycoprotein. N Engl J Med. 1982;307(18):1148.
Towne AR, Waterhouse EJ, Boggs JG, Garnett LK, Brown AJ, Smith JR, Jr., DeLorenzo RJ. Prevalence of nonconvulsive status epilepticus in comatose patients. Neurology. 2000;54(2):340–5.
Verbeeck RK, Cardinal JA, Wallace SM. Effect of age and sex on the plasma binding of acidic and basic drugs. Eur J Clin Pharmacol. 1984;27(1):91–7.
Wallace S, Verbeeck R. Effect of age and sex on the plasma binding of acidic and basic drugs. Clin Pharmacokinet. 1987;12:91–7.
Wynne HA, Cope LH, Mutch E, Rawlins MD, Woodhouse KW, James OF. The effect of age upon liver volume and apparent liver blood flow in healthy man. Hepatology. 1989;9(2):297–301.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer Science+Business Media New York
About this chapter
Cite this chapter
Menon, U., Leppik, I. (2015). Medical Management of Seizures in Cerebrovascular Disorders. In: Koubeissi, M., Alshekhlee, A., Mehndiratta, P. (eds) Seizures in Cerebrovascular Disorders. Springer, New York, NY. https://doi.org/10.1007/978-1-4939-2559-9_10
Download citation
DOI: https://doi.org/10.1007/978-1-4939-2559-9_10
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4939-2558-2
Online ISBN: 978-1-4939-2559-9
eBook Packages: MedicineMedicine (R0)