Abstract
An increasing body of evidence suggests the likelihood of a link between venous and arterial thrombosis. The two vascular complications share several risk factors, such as age, obesity, smoking, diabetes mellitus, blood hypertension, hypertriglyceridemia, and metabolic syndrome. Moreover, there are many examples of conditions accounting for both venous and arterial thrombosis, such as the antiphospholipid antibody syndrome, hyperhomocysteinemia, malignancies, infections, and the use of hormonal treatment. Finally, several recent studies have consistently shown that patients with venous thromboembolism are at a higher risk of arterial thrombotic complications than matched control individuals. We, therefore, speculate the two vascular complications are simultaneously triggered by biological stimuli responsible for activating coagulation and inflammatory pathways in both the arterial and the venous system. Future studies are needed to clarify the nature of this association, to assess its extent, and to evaluate its implications for clinical practice.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Venous thromboembolism
- Deep vein thrombosis
- Pulmonary embolism
- Myocardial infarction
- Ischemic stroke
- Atherosclerosis
1 Introduction
Venous and arterial thrombotic disorders have long been viewed as separate pathophysiological entities, partly because of the obvious anatomical differences, as well as their distinct clinical presentations. In particular, arterial thrombosis has long been held to be largely a phenomenon of platelet activation, whereas venous thrombosis is largely a matter of activation of the clotting system. However, there is evidence that this dichotomy is likely to be an oversimplification. Fibrin-rich thrombi form in the left atrial appendage of patients with atrial fibrillation and in the coronary artery system of patients with myocardial infarction. Accordingly, anticoagulant drugs are highly effective for prevention of arterial embolism related to atrial fibrillation [1], and for prevention and treatment of coronary artery disease [2]. Likewise, platelets play an inevitable role in the formation of thrombi in the venous system, and antiplatelet agents have been shown to be effective for prevention of venous thromboembolic (VTE) disorders, although to a smaller extent than anticoagulant drugs [3, 4]. As another example, subjects who sustain a retinal vein thrombosis commonly have associated cardiovascular risk factors [5], and the causes of mortality on follow-up are usually arterial vascular events [6].
2 Generation of the Hypothesis
In the second half of the 1990s, we published the results of a prospective cohort study dealing with the long-term follow-up of a wide cohort of patients after their first episode of both unprovoked and secondary acute deep vein thrombosis (DVT) of the lower extremities [7]. While the predominant interest of this observation focused on the development of recurrent VTE and late post-thrombotic sequelae, we were surprised by the unexpectedly high proportion of patients who died of acute myocardial infarction, ischemic stroke or experienced a sudden otherwise inexplicable death. Although this observation was not controlled, we had the distinct perception that this proportion would be higher than that expected in matched individual subjects free from thromboembolic disorders.
3 Association Between VTE and Atherosclerosis
In order to assess whether an association exists between VTE and atherosclerosis, in 1996, a prospective case-control study was initiated and its results were published in 2003 [8]. Ultrasonography of the carotid arteries was performed in 299 unselected patients with DVT without symptomatic atherosclerosis and in 150 control subjects. In a multivariate analysis taking into account risk factors for atherosclerosis, the odds ratio (OR) for carotid plaques in patients with unprovoked as compared to secondary DVT (i.e., DVT associated with active cancer, recent puerperium, trauma or fracture, prolonged immobilization or current estrogens use) and controls was found to be 2.4 (95 % CI, 1.4–4.0) (Fig. 1).
Prevalence of carotid plaques in patients with unprovoked and secondary DVT and in the control subjects [8]
Subsequently, three studies have provided further evidence in support of the association between VTE and atherosclerosis. In a case-control study, Hong et al. found a higher prevalence of coronary artery calcium, as assessed by chest CT scan, in patients with unprovoked VTE than in matched control individuals [9]. In a series of almost 24,000 consecutive autopsies, Eliasson et al. found an increased prevalence of VTE in patients with arterial thrombosis, except for those with coronary artery thrombosis [10]. Finally, in a recent a case-control study conducted on subjects older than 50, we assessed the prevalence of symptomatic or subclinical atherosclerosis in 100 unselected patients with unprovoked VTE, and compared it with that of 100 patients with secondary VTE and of 100 matched control individuals free from VTE disorders [11]. In patients with unprovoked VTE, the adjusted OR for symptomatic or subclinical atherosclerosis was 5.1 (95 % CI, 2.0–13.1) in comparison to patients with secondary VTE, and 14.5 (95 % CI, 5.8–36.3) in comparison to controls. The prevalence of atherosclerosis was higher in patients with secondary VTE than in controls (OR, 3.1; 95 % CI, 1.6–6.1).
4 Risk Factors of Atherosclerosis and Venous Thromboembolism
Ageno et al. reviewed the evidence favouring the association of the most important risk factors for atherosclerosis and VTE [12]. After reviewing 21 case-control and cohort studies dealing with a total of 63,552 patients meeting the inclusion criteria, factors that were found to be significantly associated with an increased risk of VTE were obesity, blood hypertension, diabetes mellitus, and hypertriglyceridemia, According to the results of subsequent population-based study, abdominal obesity appears to be the pivotal risk factor among the individual components of the metabolic syndrome [13–15].
While the review by Ageno et al. failed to identify smoking as an additional potential risk factor for VTE, the findings from two more recent population-based studies provided strong evidence that this is the case [16, 17]. Interestingly enough, in a cross-sectional study a few markers of atherosclerosis (namely, male sex and arterial hypertension) were found to be independently associated also with an increased risk of recurrent VTE after a period of 3–6 months of vitamin K antagonist therapy for the first VTE event [18].
5 Nature of the Association
Although information coming from the above reported investigations suggests the existence of an association between VTE and atherosclerosis, it does not clarify the nature of this association. On the one hand, atherosclerosis has the potential to promote the development of thrombotic disorders in the venous system. Atherosclerosis is associated with a detectable activation of both platelets and blood coagulation as well as an increased fibrin turnover, which can lead to thrombotic complications [19–28]. The role of this prothrombotic state in favouring venous thrombotic events is plausible given the assumption that activated platelets and coagulation factors appear in the slow-flowing venous system.
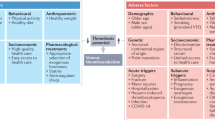
On the other hand, the two clinical conditions may share common mechanisms or risk factors. In nature, there are many examples of conditions accounting for both arterial and venous thromboembolic disorders, such as hyperhomocysteinemia, antiphospholipid antibodies, malignancies, paroxysmal nocturnal haemoglobinuria, infectious states, inflammatory bowel disease, and the use of hormonal therapy [29] (Fig. 2).
Interestingly enough, a few markers of endothelial dysfunction have been found to be significantly higher in patients with unprovoked DVT than in matched control individuals [30, 31]. In a case-control investigation enrolling patients with previous unprovoked DVT and matched control individuals, flow-mediated vasodilatation was found to be significantly lower in cases than in controls; accordingly, a few parameters of endothelial function (von Willebrand factor and soluble P-selectin) were significantly higher. Interestingly enough, a few markers of platelet activation (plasma soluble CD40 ligand and urinary 11-dehydro-TxB2 levels) did not differ between the two groups (Figs. 3 and 4). Microalbuminuria, a well know marker of endothelial dysfunction whose and of arterial cardiovascular events, was found to be independently associated with an increased risk for VTE as well [32].
Flow-mediated vasodilation of the brachial artery in patients with previous unprovoked DVT and in controls [30]
Endothelium and platelets activation markers in patients with previous unprovoked DVT and in controls [30]
6 Is Atherosclerosis Predictive of VTE?
In an attempt to assess whether atherosclerotic disease predisposes to VTE, the authors of two similar population-based cohort studies carried out in the U.S.A., the Atherosclerosis Risk in Communities and the Cardiovascular Health Study, evaluated the rate of VTE development in subjects younger and older than 65, respectively, who had carotid ultrasound and the assessment of other subclinical parameters of atherosclerosis, and were then followed-up prospectively for several years [33, 34].
In the former study, 13,081 adults aged 45–64 years underwent carotid ultrasonography to assess the intima-media thickness and the presence of atherosclerotic plaques [33]. After adjustment for age, sex, ethnicity, body mass index and diabetes, no association was found between ultrasound parameters of subclinical atherosclerosis and VTE development after a mean follow-up of 12.5 years (adjusted hazard ratio [HR] of VTE for presence of carotid plaques, 0.97; 95 % CI, 0.72–1.29).
In the latter study, 4108 individuals aged at least 65 years underwent non-invasive assessment of subclinical atherosclerosis using carotid ultrasound (intima-media thickness and presence of plaques), ankle-brachial blood pressure index and electrocardiogram, and then were followed-up for a median of 11.7 years [34]. Surprisingly enough, the adjusted RR of overall and unprovoked VTE for presence of any type of subclinical atherosclerosis was 0.60 (95 % CI, 0.39 to 0.91) and 0.32 (95 % CI, 0.18 to 0.59), respectively. These unexpected findings were mostly explained by an inverse association of high-risk carotid plaques and arterial events during follow-up.
While in the former of the two above reported studies, the occurrence of cardiovascular and cerebrovascular events was significantly associated with the development of VTE [33], in the latter the opposite was seen [34].
In an attempt to determine the impact of cardiovascular risk factors, including family history of myocardial infarction, on the incidence of VTE, a few investigators from Norway extracted data from more than 21,000 subjects, aged 25–96 years, who had been enrolled in a prospective, population-based study (the Tromsø Study) [35, 36]. In multivariable analysis, family history of myocardial infarction was significantly associated not only with an increased risk of infarction but also of total VTE (HR, 1.27; 95 % CI 1.01–1.60) and unprovoked VTE (HR, 1.46; 95 % CI: 1.03–2.07. The risk was found to increase with increasing number of affected individuals. The association was not explained by modifiable atherosclerotic risk factors. In another population-based study, having first degree relatives with myocardial infarction before the age of 60 years was positively associated with VTE compared to participants not having a positive family history (OR 1.3; 95 % CI 1.1–1.6) [37]. Finally, in a more recent population-based study conducted in Denmark patients with a history of arterial cardiovascular events had a clearly increased relative risk of VTE events in the first 3 months following the index event, then the risk decreased yet remained statistically significant [38].
Based on these findings, asymptomatic atherosclerosis is unlikely to constitute a risk factor of venous thromboembolic disorders. Whether patients developing symptomatic complications of atherosclerosis such as myocardial infarction or stroke are at a higher risk of VTE complications is controversial.
7 Is VTE Predictive of Arterial Cardiovascular Events?
Another scenario assumes that the same biological trigger is responsible for activating coagulation and inflammatory pathways in both arterial and venous thromboembolism, in such a way determining a simultaneous risk of arterial and venous thrombotic complications. This assumption is supported by the results of a cohort study. Indeed, in an attempt to evaluate whether elevated clotting factors, which have been linked to chronic sub-clinical inflammation and arterial thromboembolic disease, have a high prevalence in patients with VTE as well, Luxembourg et al. measured the plasma level of fibrinogen, factor VIII, and high-sensitivity C-reactive protein in a cohort of sex- and age-matched patients with unprovoked VTE, patients with secondary VTE and controls [39]. They found that these markers of inflammation were significantly higher in patients with unprovoked compared to secondary VTE and controls, in such a way providing evidence in support of the hypothesis that VTE and arterial thromboembolism may share common risk factors.
If this is true, subjects with VTE may be at a higher risk of subsequent arterial cardiovascular events than matched control individuals. This hypothesis was tested in 11 studies [40–50] (Table 1) and summarized in a meta-analysis [51]. All together, the results of these studies are in keeping with the observation of a higher prevalence of carotid atherosclerosis in patients with unprovoked DVT than in matched control individuals [8, 11], and strongly suggest that patients with VTE have also an increased risk of subsequent symptomatic arterial cardiovascular events. Of particular relevance is a population-based cohort study carried out in Denmark. Using nationwide Danish medical databases, Sorensen et al. assessed the risk of hospitalization due to myocardial infarction, stroke and transient ischemic attack among 25,199 patients with DVT, 16,925 patients with PE and 163,566 population controls discharged from the Danish hospitals in a 25-year period [45]. Patients with both DVT and PE were found to have a substantially increased risk of myocardial infarction and stroke during the first year after the thrombotic event. For patients with DVT, the RRs varied from 1.60 for myocardial infarction (95 % CI 1.35–1.91) to 2.19 (95 % CI 1.85–2.60) for stroke. For patients with PE, the RRs were 2.60 (95 % CI 2.14–3.14) for myocardial infarction and 2.93 (95 % CI 2.34–3.66) for stroke. The RRs were also elevated, though less markedly, during the subsequent 20 years of follow-up, with 20–40 % increases in risk for arterial cardiovascular events. RRs were similar for those with provoked and unprovoked DVT and PE (Figs. 5 and 6).
Risk of acute myocardial infarction and stroke in patients with unprovoked VTE in relation to the length of the follow-up period [45]
Risk of acute myocardial infarction and stroke in patients with secondary VTE in relation to the length of the follow-up period [45]
Whether the risk of subsequent arterial thrombotic disorders applies to all VTE patients or to the only patients with unprovoked disease is uncertain. According to the results of a meta-analysis of six studies, the risk appears higher in patients with unprovoked VTE compared to those with provoked VTE (IRR 1.86, 95 % CI 1.19–2.89) [51]. Of interest, based on recent findings the persistence of residual thrombosis, as assessed with ultrasonography 3 months after an episode of proximal DVT, predicts the development of arterial thrombotic disorders both in patients with unprovoked and in those with secondary DVT [52].
8 Implications of the Association
We speculate that venous and arterial thrombosis are two aspects of the same disease (i.e., thrombosis), and that this disease may electively affect genetically predisposed individuals resulting in clinically manifestations that are, in turn, depending on a variety of elements including the age of patients, their lifestyle, and the occurrence of co-morbidities and circumstantial factors: the venous thrombotic events being more frequent, for example, after triggering risk factors such as surgery or trauma, and the arterial thrombotic events being more frequent in subjects who have developed atherosclerosis.
These findings have several implications for both research and medical practice. Patients with VTE of unknown origin could be examined for asymptomatic atherosclerosis, in order to modify aggressively the risk profile in those with abnormal test results. Measures could include appropriate counselling about lifestyle changes and control of risk factors for atherosclerosis. Interestingly enough, lifestyle factors are likely to have a major impact on the risk of VTE. A diet including more plant food and fish and less red and processed meat [53] and more in general the Mediterranean diet [54], the supplementation of vitamin E [55], and alcohol consumption [56, 57] have recently been found to be associated with a lower incidence of venous thrombosis. Whether regular sport activity decreases this risk as well is controversial, as there data in favour [58] and against [59] this association. Consistent with these findings are the results of a prospective cohort study conducted in Sweden on 40 000 Swedish women who were followed-up for a mean of 11 years: women non-smokers who were physically active and who consumed alcohol in moderation were found to have a lower risk of VTE [60]. Conversely, sedentary life was recently found to increase the risk of unprovoked PE in women [61].
In addition, a potential role for prophylaxis of both recurrent VTE and arterial cardiovascular events with antiplatelet therapy or statins may be explored. Interest in statins has increased, given recent data that consistently suggest an unexpected role in lowering the risk of venous thromboembolism [62–67]. As far as the role of aspirin is concerned, according to the results of recent studies, aspirin in low doses when administered for the long-term management of patients with unprovoked VTE reduces by approximately 35 % the risk of recurrent VTE while offering a considerable protection against the development of arterial cardiovascular events [68–70].
In conclusion, the separate nature of arterial and venous thrombotic disorders has been challenged. Future studies are needed to clarify the nature of this association, to assess its extent, and to evaluate its implications for clinical practice.
References
You JJ, Singer DE, Howard PA et al (2012) Antithrombotic therapy for atrial fibrillation: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2 Suppl):e531S–e575S
Vandvik PO, Lincoff AM, Gore JM et al (2012) Primary and secondary prevention of cardiovascular disease: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2 Suppl):e637S–e668S
Antithrombotic Trialist’s Collaboration (2002) Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high-risk patients. Br Med J 324:71–86
Warkentin TE (2012) Aspirin for dual prevention of venous and arterial thrombosis. N Engl J Med 367:2039–2041
Janssen MC, den Heijer M, Cruysberg JR, Wollersheim H, Bredie SJ (2005) Retinal vein occlusion: a form of venous thrombosis or a complication of atherosclerosis? A meta-analysis of thrombophilic factors. Thromb Haemost 93:1021–1026
Tsaloumas MD, Kirwan J, Vinall H et al (2000) Nine year follow-up study of morbidity and mortality in retinal vein occlusion. Eye 14:821–827
Prandoni P, Lensing AWA, Cogo A et al (1996) The long-term clinical course of acute deep venous thrombosis. Ann Intern Med 125:1–7
Prandoni P, Bilora F, Marchiori A et al (2003) An association between atherosclerosis and venous thrombosis. N Engl J Med 348:1435–1441
Hong C, Zhu F, Du D, Pilgram TK, Sicard GA, Bae KT (2005) Coronary artery calcification and risk factors for atherosclerosis in patients with venous thromboembolism. Atherosclerosis 183:169–174
Eliasson A, Bergqvist D, Bjorck M, Acosta S, Sternby NH, Ogren M (2006) Prevalence and risk of venous thromboembolism in patients with verified arterial thrombosis: a population study based on 23 796 consecutive autopsies. J Thromb Haemost 4:1897–1902
Milan M, Vedovetto V, Bilora F, Pesavento R, Prandoni P (2015) Further evidence in support of the association between venous thrombosis and atherosclerosis: a case-control study. Thromb Res 134:1028–1031
Ageno W, Becattini C, Brighton T, Selby R, Kamphuisen PW (2008) Cardiovascular risk factors and venous thromboembolism: a meta-analysis. Circulation 117:93–102
Borch KH, Brækkan SK, Mathiesen EB et al (2009) Abdominal obesity is essential for the risk of venous thromboembolism in the metabolic syndrome – the Tromsø study. J Thromb Haemost 7:739–745
Steffen LM, Cushman M, Peacock JM et al (2009) Metabolic syndrome and risk of venous thromboembolism: Longitudinal Investigation of Thromboembolism Etiology (LITE). J Thromb Haemost 7:746–751
Ageno W, Di Minno MN, Ay C et al (2014) Association between the metabolic syndrome, its individual components, and unprovoked venous thromboembolism. Results of a patient-level meta-analysis. Arterioscler Thromb Vasc Biol 34:2478–2485
Holst AG, Jensen G, Prescott E (2010) Risk factors for venous thromboembolism. Results from the Copenhagen City Heart Study. Circulation 121:1896–1903
Severinsen MT, Kristensen SR, Johnsen SP et al (2009) Smoking and venous thromboembolism: a Danish follow-up study. J Thromb Haemost 7:1297–1303
Linnemann B, Zgouras D, Schindewolf M et al (2008) Impact of sex and traditional cardiovascular risk factors on the risk of recurrent venous thromboembolism: results from the German MAISTHRO Registry. Blood Coagul Fibrinolysis 19:159–165
Wilhelmsen L, Svardsudd K, Korsan-Bengtsen K, Larsson B, Welin L, Tibblin G (1984) Fibrinogen as a risk factor for stroke and myocardial infarction. N Engl J Med 311:501–505
Meade TW, Mellows S, Brozovic M et al (1986) Haemostatic function and ischemic heart disease: principal results from the Northwick Park Heart Study. Lancet 2:533–537
Thompson SG, Kienast J, Pyke SD, Haverkate F, van de Loo JC (1995) Hemostatic factors and the risk of myocardial infarction or sudden death in patients with angina pectoris. N Engl J Med 332:635–641
Miller GJ, Bauer KA, Barzegar S, Cooper JA, Rosenberg RD (1996) Increased activation of the haemostatic system in men at high risk of fatal coronary heart disease. Thromb Haemost 75:767–771
Folsom AR, Wu KK, Rosamond WR, Sharrett AR, Chambless LE (1997) Prospective study of hemostatic factors and incidence of coronary heart disease. Circulation 96:1102–1108
Folsom AR, Aleksic N, Park E, Salomaa V, Juneja H, Wu KK (2001) Prospective study of fibrinolytic factors and incident coronary heart disease. Arterioscler Thromb Vasc Biol 21:611–617
Koenig W, Rothenbacher D, Hoffmeister A, Griesshammer M, Brenner H (2001) Plasma fibrin D-dimer levels and risk of stable coronary artery disease: results of a large case-control study. Arterioscler Thromb Vasc Biol 21:1701–1705
Strano A, Hoppensteadt D, Walenga JM et al (1996) Plasma levels of the molecular markers of coagulation and fibrinolysis in patients with peripheral arterial disease. Semin Thromb Hemost 22(Suppl 1):35–40
De Buyzere M, Philippe J, Duprez D, Baele G, Clement DL (1993) Coagulation system activation and increased D-dimer levels in peripheral arterial occlusive disease. Am J Hematol 43:91–94
Lowe GD, Fowkes FG, Dawes J, Donnan PT, Lennie SE, Housley E (1993) Blood viscosity, fibrinogen, and activation of coagulation and leukocytes in peripheral arterial disease and the normal population in the Edinburgh Artery Study. Circulation 87:1915–1920
Prandoni P, Piovella C, Pesavento R (2012) Venous thromboembolism and arterial complications. Semin Respir Crit Care Med 33:205–210
Migliacci R, Becattini C, Pesavento R et al (2007) Endothelial dysfunction in patients with spontaneous venous thromboembolism. Haematologica 92:812–818
Gresele P, Momi S, Migliacci R (2010) Endothelium, venous thromboembolism and ischaemic cardiovascular events. Thromb Haemost 103:56–61
Mahmoodi BK, Gansevoort RT, Veeger NJGM et al (2009) Microalbuminuria and risk of venous thromboembolism. JAMA 301:1790–1797
Reich LM, Folsom AR, Key NS et al (2006) Prospective study of subclinical atherosclerosis as a risk factor for venous thromboembolism. J Thromb Haemost 4:1909–1913
van der Hagen PB, Folsom AR, Jenny NS et al (2006) Subclinical atherosclerosis and the risk of future venous thrombosis in the Cardiovascular Health Study. J Thromb Haemost 4:1903–1908
Brækkan SK, Mathiesen EB, Njølstad I et al (2008) Family history of myocardial infarction is an independent risk factor for venous thromboembolism – the Tromsø study. J Thromb Haemost 6:1851–1857
Lind C, Enga KF, Mathiesen EB, Njølstad I, Brækkan SK, Hansen JB (2014) Family history of myocardial infarction and cause-specific risk of myocardial infarction and venous thromboembolism – the Tromsø Study. Circ Cardiovasc Genet 7:684–691
Quist-Paulsen P, Næss IA, Cannegieter SC et al (2009) Arterial cardiovascular risk factors and venous thrombosis: results from a population based prospective study (the HUNT 2). Haematologica 95:119–125
Sørensen HT, Horvath-Puho E, Kobberøe Søgaard K et al (2009) Arterial cardiovascular events, statins, low dose aspirin and subsequent risk of venous thromboembolism: a population based case control study. J Thromb Haemost 7:521–528
Luxembourg B, Schmitt J, Humpich M et al (2009) Cardiovascular risk factors in idiopathic compared to risk-associated venous thromboembolism: a focus on fibrinogen, factor VIII, and high-sensitivity C-reactive protein (hs-CRP). Thromb Haemost 102:668–675
Becattini C, Agnelli G, Prandoni P et al (2005) A prospective study on cardiovascular events after acute pulmonary embolism. Eur Heart J 26:77–83
Prandoni P, Ghirarduzzi A, Prins MH et al (2006) Venous thromboembolism and the risk of subsequent symptomatic atherosclerosis. J Thromb Haemost 4:1891–1896
Schulman S, Lindmarker P, Holmstrom M et al (2006) Post-thrombotic syndrome, recurrence, and death 10 years after the first episode of venous thromboembolism treated with warfarin for 6 weeks or 6 months. J Thromb Haemost 4:734–742
Bova C, Marchiori A, Noto A et al (2006) Incidence of arterial cardiovascular events in patients with idiopathic venous thromboembolism. A retrospective cohort study. Thromb Haemost 96:132–136
Young L, Ockelford P, Milne D, Rolfe-Vyson V, McKelvie S, Harper P (2006) Post treatment residual thrombus increases the risk of recurrent deep vein thrombosis and mortality. J Thromb Haemost 4:1919–1924
Sørensen HT, Horvath-Puho E, Pedersen L, Baron JA, Prandoni P (2007) Venous thromboembolism and subsequent hospitalization due to acute arterial cardiovascular events – a 20 year cohort study. Lancet 370:1773–1779
Spencer FA, Ginsberg JS, Chong A, Alter DA (2008) The relationship between unprovoked venous thromboembolism, age, and acute myocardial infarction. J Thromb Haemost 6:1507–1513
Klok FA, Mos IC, Broek L et al (2009) Risk of arterial cardiovascular events in patients after pulmonary embolism. Blood 114:1484–1488
Barsoum MK, Cohoon KP, Roger VL et al (2014) Are myocardial infarction and venous thromboembolism associated? Population-based case-control and cohort studies. Thromb Res 134:593–598
Madridano O, Del Toro Y, Lorenzo A et al (2015) Subsequent arterial ischemic events in patients receiving anticoagulant therapy for venous thromboembolism. J Vasc Surg [epub ahead of print] 3:135–141
Pasha SM, Tan M, van Rees Vellinga TF, Klok FA, Huisman MV (2014) Risk of atherothrombotic events in patients after proximal deep-vein thrombosis. Blood Coagul Fibrinolysis. 27(1):13–18
Becattini C, Cristina Vedovati M, Ageno W, Dentali F, Agnelli G (2010) Incidence of arterial cardiovascular events after venous thromboembolism. A systematic review and a meta-analysis. J Thromb Haemost 8:891–897
Prandoni P, Lensing AWA, Prins MH et al (2015) The impact of residual thrombosis on the long-term outcome of patients with deep venous thrombosis treated with conventional anticoagulation. Sem Thromb Haemost 41:133–140
Steffen LM, Folsom AR, Cushman M, Jacobs DR Jr, Rosamond WD (2006) Greater fish, fruit, and vegetable intakes are related to lower incidence of venous thromboembolism. Circulation 115:188–195
Hoevenaar-Blom MP, Nooyens AC, Kromhout D et al (2012) Mediterranean style diet and 12-year incidence of cardiovascular diseases: the EPIC-NL cohort study. PLoS One 7:e45458
Glynn RJ, Ridker PM, Goldhaber SZ, Zee RY, Buring JE (2007) Effects of random allocation to vitamin e supplementation on the occurrence of venous thromboembolism. Report from the Women’s Health Study. Circulation 116:1497–1503
Pomp ER, Rosendaal FR, Doggen CJ (2008) Alcohol consumption is associated with a decreased risk of venous thrombosis. Thromb Haemost 99:59–63
Lutsey PL, Steffen LM, Virnig BA, Folsom AR (2009) Diet and incident venous thromboembolism: the Iowa women’s health study. Am Heart J 157:1081–1087
van Stralen KJ, Le Cessie S, Rosendaal FR, Doggen CJ (2007) Regular sports activities decrease the risk of venous thrombosis. J Thromb Haemost 5:2186–2192
Borch KH, Hansen-Krone I, Braekkan S et al (2010) Physical activity and risk of venous thromboembolism. The Tromso study. Haematologica 95:2088–2094
Lindqvist PG, Epstein E, Olsson H (2008) The relationship between lifestyle factors and venous thromboembolism among women: a report from the MISS study. Br J Haematol 144:234–240
Kabrhel C, Varraso R, Goldhaber SZ, Rimm E, Camargo CA Jr (2011) Physical inactivity and idiopathic pulmonary embolism in women: prospective study. BMJ 343:d3867
Agarwal V, Phung OJ, Tongbram V, Bhardwaj A, Coleman CI (2010) Statin use and the prevention of venous thromboembolism: a meta-analysis. Int J Clin Pract 64:1375–1383
Glynn RJ, Danielson E, Fonseca FA et al (2009) A randomized trial of rosuvastatin in the prevention of venous thromboembolism. N Engl J Med 360:1851–1861
Khemasuwan D, Divietro ML, Tangdhanakanond K, Pomerantz SC, Eiger G (2010) Statins decrease the occurrence of venous thromboembolism in patients with cancer. Am J Med 123:60–65
Biere-Rafi S, Hutten BA, Squizzato A et al (2013) Statin treatment and the risk of recurrent pulmonary embolism. Eur Heart J 34:1800–1806
Nguyen CD, Andersson C, Jensen TB et al (2013) Statin treatment and risk of recurrent venous thromboembolism: a nationwide cohort study. BMJ Open 3:e003135
Schmidt M, Cannegieter SC, Johannesdottir SA, Dekkers OM, Horváth-Puhó E, Sørensen HT (2014) Statin use and venous thromboembolism recurrence: a combined nationwide cohort and nested case-control study. J Thromb Haemost 12:1207–1215
Becattini C, Agnelli G, Schenone A et al (2012) Aspirin for preventing the recurrence of venous thromboembolism. N Engl J Med 366:1959–1967
Brighton TA, Eikelboom JW, Mann K et al (2012) Low-dose aspirin for preventing recurrent venous thromboembolism. N Engl J Med 367:1979–1987
Simes J, Becattini C, Agnelli G et al (2014) Aspirin for the prevention of recurrent venous thromboembolism: the INSPIRE collaboration. Circulation 130:1062–1071
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Prandoni, P. (2016). Venous and Arterial Thrombosis: Is There a Link?. In: Islam, M. (eds) Thrombosis and Embolism: from Research to Clinical Practice. Advances in Experimental Medicine and Biology(), vol 906. Springer, Cham. https://doi.org/10.1007/5584_2016_121
Download citation
DOI: https://doi.org/10.1007/5584_2016_121
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-22107-6
Online ISBN: 978-3-319-22108-3
eBook Packages: MedicineMedicine (R0)