Abstract
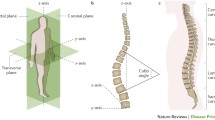
Adolescent idiopathic scoliosis (AIS) and early onset scoliosis (EOS) represent a three-dimensional rotational deformity of the spine. Adolescent idiopathic scoliosis (AIS) is recognized when the child is greater than 10 years of age and represents the most common type of idiopathic scoliosis affecting 3% of healthy adolescents [1]. The etiology of AIS is multifactorial and may include genetic factors, neurologic disorders, hormonal and metabolic dysfunctions, skeletal growth, biomechanics factors, and environmental and lifestyle factors. AIS treatment depends on various factors, such as the age of the child and initial curve magnitude. Only 10% of children require treatment, of which surgery is needed in 0.1% [2]. AIS also affects health-related quality of life (HRQoL); hence, the decision of surgical treatment versus (vs) conservative management is very important [3]. The most important prognostic factor for curve progression is the magnitude of the primary curve. The risk of progression is almost 100% for 10–12-year-old children compared with 70% for 16-year-old children [4]. Nonsurgical management is recommended for a primary curve of ≥20–25°. Nonsurgical options include bracing for a minimum of 18 h per day for flexible deformities with a success rate of approximately 72% [5]. Indications for surgery include curves ≥45°, deformity correction, preventing curve progression, back pain, and psychological disturbances.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
-
Surgery for EOS and AIS significantly improves lung capacity and pulmonary function.
-
Various implants and instrumentation systems are available for EOS with their own merits and drawbacks.
-
Although guided growth rod systems are associated with complications, they play a vital role in the treatment of EOS by delaying the need for fusion.
-
Disc degeneration has been reported as a long-term complication, but its effect on the quality of life has not been studied in detail.
-
Selection of an appropriate treatment modality, especially in EOS, can improve the outcome and prevent long-term complications.
1 Introduction
Adolescent idiopathic scoliosis (AIS) and early onset scoliosis (EOS) represent a three-dimensional rotational deformity of the spine. Adolescent idiopathic scoliosis (AIS) is recognized when the child is greater than 10 years of age and represents the most common type of idiopathic scoliosis affecting 3% of healthy adolescents [1]. The etiology of AIS is multifactorial and may include genetic factors, neurologic disorders, hormonal and metabolic dysfunctions, skeletal growth, biomechanics factors, and environmental and lifestyle factors. AIS treatment depends on various factors, such as the age of the child and initial curve magnitude. Only 10% of children require treatment, of which surgery is needed in 0.1% [2]. AIS also affects health-related quality of life (HRQoL); hence, the decision of surgical treatment versus (vs) conservative management is very important [3]. The most important prognostic factor for curve progression is the magnitude of the primary curve. The risk of progression is almost 100% for 10–12-year-old children compared with 70% for 16-year-old children [4]. Nonsurgical management is recommended for a primary curve of ≥20–25°. Nonsurgical options include bracing for a minimum of 18 h per day for flexible deformities with a success rate of approximately 72% [5]. Indications for surgery include curves ≥45°, deformity correction, preventing curve progression, back pain, and psychological disturbances.
According to the Scoliosis Research Society, early-onset scoliosis is defined as a three-dimensional spine deformity present before 10 years of age. The etiology can be idiopathic, congenital, neuromuscular, or syndromic. Children with early-onset scoliosis eventually land up in pulmonary failure due to impaired alveolar growth, resulting in an increased risk of mortality [6]. Additionally, curve progression rapidly causes severe deformities with impaired physiological growth. The congenital anomaly can be due to failure of vertebral formation, failure of vertebral segmentation, or both. The risk of progression is highest in a unilateral unsegmented bar with a contralateral hemivertebra at the same level. These patients develop structural compensatory scoliosis above or below the congenital curve. Bracing does not effectively help in congenital scoliosis but is often indicated in the early management of structural compensatory curves. Infants (0–3 years) and juveniles (4–10 years) represent approximately 19% of all idiopathic scoliosis cases. Risk factors for progression among these curves include Cobb angles greater than 30° and rib-vertebral-angle differences >20°. Corrective casting/bracing or other management is indicated for these children is surgery for idiopathic EOS is indicated for curves >60°. Neuromuscular scoliosis occurs as a result of underlying neurological or muscular disease and is associated with problems with sitting balance, hygiene, nursing care, and cardiopulmonary compromise. Treatment is the observation of small, flexible neuromuscular curves that do not cause any functional impairment, while severe deformities resulting in pulmonary impairment require surgery.
The benefits of surgery include the correction of cosmetic deformity and improved quality of life, pulmonary function, and psychosocial life.
In contrast, surgery may result in complications such as the neurological deficit, crankshaft phenomenon, progression of the curve, implant failure, pseudarthrosis, decompensation, worsening of deformity, etc.
For advancements in modern surgical practice, we must collect and process patient outcome data.
2 Pulmonary Function
New alveolar growth occurs until the age of 5–8 years of life. However, it can continue until approximately 18–23 in males and 17–21 in females. Surgical correction of AIS can improve the structural deformity of the chest wall, but its effect on pulmonary function is unclear. There is inconclusive evidence, with some showing evidence [7] and some showing no change [8] or even some deterioration [9] after surgery. The surgical approach utilized is one of the factors causing this discrepancy. Some studies with a follow-up of 2–5 years in which they have performed anterior fusion via thoracotomy or rib resection thoracoplasty [10] have shown worse pulmonary function results compared to those surgeries that spare the chest wall. Surgical techniques involving Harrington instrumentation or segmental spinal instrumentation utilizing multiple hook-rod constructs have shown differing results, with some showing improvement and others showing no or even deterioration. A study with more than 20 years of follow-up utilizing Harrington rod instrumentation of 110 patients found an increase in FEV1, FVC, and percent predicted FCV and FEV1 [7]. Newton and colleagues [11] published their results of factors that independently predicted postoperative pulmonary function in 254 AIS patients. Their results found that aside from preoperative PFTs, the largest predictors of postoperative PFTs were an open anterior approach and a thoracoplasty. Both were negatively associated with postoperative pulmonary function. A study performed by Gitelman et al. [12] with a follow-up of 10 years suggests that procedures that violate the chest wall will leave patients with worse pulmonary reserves than procedures that spare the chest wall.
3 Implant-Related Outcome
Implant-related complications associated with hooks, screws, or rods account for approximately 0.64–1.37% of all complications in surgery for AIS [13]. Pedicle screw instrumentation is a safe and effective technique in these patients [14, 15]. However, they are associated with complications such as pedicle breach, pedicle cut out, screw loosening, dural tear, CSF leak, pleural injury resulting in pneumothorax, pleural effusion, screw prominence in thin children resulting in pressure sores, and wound dehiscence [14, 16].
4 Complications of Various Surgical Techniques for EOS
One of the most important disadvantages of traditional growth rods, which utilize the principle of distraction to correct the deformity, is the need for repetitive surgery (every 6 months) to distract the rods through the connectors. This poses the child at risk of anesthetic complications, infection, and financial burden. According to Bess et al. [17], the complication rates reached 55% in their study of 140 patients, with an average of 2.2 complications per patient. Implant failure, anchor failure, and surgical site infections were the common complications. The other reported complication of the growth rod technique is the spontaneous fusion of the uninstrumented segments. Although subperiosteal dissection was not performed in these patients and the rods were introduced intramuscularly, spontaneous fusion occurred in 80% of them after an average of 5 lengthening procedures [18]. Additionally, the “law of diminishing returns” described by Sankar et al. can happen, which is a reduced ability to lengthen or distract the rods further and correct the deformity due to stiffening of the instrumented portion of the spine. The other documented complications of growth rod procedures include proximal junctional kyphosis and failure due to kyphosis produced by distraction and lengthening of the posterior column and exacerbation of chest torsion, as this technique cannot control vertebral rotation.
The principle of magnetic growth rods is similar to that of traditional growth rods, but repetitive surgeries are not needed because the telescopic connector can be manipulated by external remote control. However, the complication rates and spontaneous fusion are similar to those of the traditional growth rod technique. The most common complications with magnetic rods include revision surgery, implant failure, and foundation failure [19].
The anterior vertebral body tethering technique is used for mild to moderate flexible thoracic idiopathic curves in skeletally immature patients. Although the short-term results are promising with this technique, long-term outcomes are awaited. Newton et al. compared the anterior vertebral body tethering technique with definitive fusion and found that the maintenance of correction was better with definitive fusion with fewer complications and revision procedures.
The guided growth systems for EOS include a modified Luque trolley and Shilla technique. However, the complication rates, which include spontaneous spine fusion, rod breakage, and revision surgeries, are significantly higher than those of the traditional growth rod technique.
4.1 Degenerative Disc Disease
One of the delayed complications of AIS both before and after surgery is degenerative disc disease. Pain due to degenerative disc disease has been reported [20]. According to Green et al., a higher rate and grade of disc degeneration was seen in patients with a lower level of fusion after posterior spinal fusion surgery [21]. In contrast, Harding et al. found no correlation between the number of fused vertebrae and disc degeneration [22]. Danielsson et al. [23] analyzed 32 AIS patients who were followed for 25 years postspinal fusion with Harrington rod instrumentation. They noted more degenerative disc changes, reduction in disc height, and end-plate changes in the lowest nonfused disc on MRI scans compared with the control group.
Kelly et al. [24] evaluated the long-term outcome for AIS patients who underwent anterior spinal fusion and found that all six patients had narrowing of disc space and loss of signal intensity in the unfused disc below the fusion mass in T2-weighted MRI images. According to Akazawa et al. [25], with 35 years of follow-up after spinal fusion surgery in AIS, patients with the last instrumented vertebra L4 or lower had severe disc degeneration, reduced lumbar lordosis and global sagittal imbalance than those with the last instrumented vertebrae at L3 or higher. In a study performed by Chiu et al. [26], there was no difference in the degeneration of unfused lumbar discs below the level of fusion, and it was not related to the selection of LIV. However, they found that patients with fusion to L4 or lower had significant back pain compared to those in whom the fusion ended at L3 or higher.
The postsurgical rigid spine can cause strain on the unfused vertebra. A higher degree of correction is associated with increased rates of degenerative osteoarthritis. This can result in excessive stress on the rigid spine, leading to serious injuries even with trivial trauma and low-velocity injuries.
4.2 Postsurgical Pain
Postsurgical pain is one of the primary indications for reoperation [27]. Cook S et al. [28], in their study of 190 patients, documented a reoperation rate within 2–8 years postsurgery of 19%, and postsurgical pain was the main indication in these patients. In a study performed by Islam NC et al., among 34 patients with significant postsurgical pain, 56% had relief of pain after revision surgery, whereas the remaining 44% had persistent pain. Additionally, two patients without preoperative pain reported fresh onset pain during follow-up [29]. Pain and donor-site morbidity after bone grafting are well-documented complications. According to Skaggs et al. [30], in a study of 87 patients, 24% had donor site pain, and 15% of the patients reported severe pain that interfered with their daily activities.
4.3 Curve Progression and Crankshaft Phenomenon
Some curves continue to progress even after spinal fusion. This could be due to rod breakage or other forms of implant failure. Pseudarthrosis can occur years after surgery and can be difficult to diagnose [31]. The crankshaft phenomenon is a well-known complication and usually occurs in young skeletally immature children after rigid fusion. It is a condition that occurs after isolated posterior instrumentation where there is continued spinal growth in the unfused anterior part causing rotation around the fusion mass [32, 33], resulting in the progression of the deformity and decompensation.
4.4 Decompensation and Flat Back Syndrome
Another delayed complication after surgery for AIS is sagittal imbalance and decompensation [34]. Distraction-based maneuvers for spinal deformity correction can reduce thoracic kyphosis. This can lead to altered global sagittal spinal imbalance by flattening the thoracic and lumbar spine. Postoperative flatback syndrome can lead to persistent and severe back pain, impaired quality of life, and significant disability [35].
4.5 Increased Deformity of the Thorax
The rib hump can worsen even after straightening and derotating the spine [36]. Costoplasty is a technique of excision of the ribs on the convex side with a significant rib hump. It significantly improves the cosmetic appearance of patients [37]. However, costoplasty can lead to a flail chest because of the destabilizing effects of rib removal [38]. It can also lead to torsional deformities of the thorax and the progression of scoliosis. Furthermore, excision of the ribs can result in a reduced volume of the thoracic cavity, resulting in impaired pulmonary function [39].
5 Conclusion
Surgery is an effective and recommended treatment for EOS and AIS. However, the treating surgeon should be aware of the long-term outcomes and complications of the procedure as well as of the implants and instrumentation techniques to prevent delayed and disabling complications in these patients.
References
Weinstein SL, Dolan LA, Cheng JC, Danielsson A, Morcuende JA. Adolescent idiopathic scoliosis. Lancet. 2008;371:1527–37.
Lonstein JE. Scoliosis: surgical versus nonsurgical treatment. Clin Orthop Relat Res. 2006;443:248–59.
Yang M, Zhao Y, Yin X, Chen Z, Yang C, Li L, Li M. Prevalence, risk factors, and characteristics of the “adding-on” phenomenon in idiopathic scoliosis after correction surgery: a systematic review and meta-analysis. Spine (Phila Pa 1976). 2018;43:780–90.
Bunnell WP. The natural history of idiopathic scoliosis. Clin Orthop Relat Res. 1988;(229):20–25.
Weinstein SL, Dolan LA, Wright JG, Dobbs MB. Effects of bracing in adolescents with idiopathic scoliosis. N Engl J Med. 2013;369:1512–21.
Redding G, Song K, Inscore S, et al. Lung function asymmetry in children with congenital and infantile scoliosis. Spine J. 2008;J8:639–44.
Pehrsson K, Danielsson A, Nachemson A. Pulmonary function in adolescent idiopathic scoliosis: a 25 year follow up after surgery or start of brace treatment. Thorax. 2001;56:388–93.
Nash CL, Nevins K. A lateral look at pulmonary function in scoliosis [abstract]. In: Proceedings of the Scoliosis Research Society. J Bone Joint Surg Am. 1974;56:440.
Upadhyay SS, Ho EK, Gunawardene WM, et al. Changes in residual volume relative to vital capacity and total lung capacity after arthrodesis of the spine in patients who have adolescent idiopathic scoliosis. J Bone Joint Surg Am. 1993;75:46–52.
Kim YJ, Lenke LG, Bridwell KH, et al. Pulmonary function in adolescent idiopathic scoliosis relative to the surgical procedure. J Bone Joint Surg Am. 2005;87:1534–41.
Newton PO, Perry A, Bastrom TP, et al. Predictors of change in postoperative pulmonary function in adolescent idiopathic scoliosis: a prospective study of 254 patients. Spine (Phila Pa 1976). 2007;32:1875–82.
Gitelman Y, Lenke LG, Bridwell KH, Auerbach JD, Sides BA. Pulmonary function in adolescent idiopathic scoliosis relative to the surgical procedure. Spine (Phila Pa 1976). 2011;36(20):1665–72.
Reames DL, Smith JS, Fu KM, et al. Complications in the surgical treatment of 19,360 cases of pediatric scoliosis: a review of the Scoliosis Research Society morbidity and mortality database. Spine (Phila Pa 1976). 2011;36:1484–91. https://doi.org/10.1097/BRS.0b013e3181f3a326.
Hicks JM, Singla A, Shen FH, Arlet V. Complications of pedicle screw fixation in scoliosis surgery: a systematic review. Spine (Phila Pa 1976). 2010;35:E465–70. https://doi.org/10.1097/BRS.0b013e3181d1021a.
Ledonio CG, Polly DW Jr, Vitale MG, Wang Q, Richards BS. Pediatric pedicle screws: comparative effectiveness and safety: a systematic literature review from the Scoliosis Research Society and the Pediatric Orthopedic Society of North America task force. J Bone Joint Surg Am. 2011;93:1227–34. https://doi.org/10.2106/JBJS.J.00678.
Botolin S, Merritt C, Erickson M. Aseptic loosening of pedicle screw as a result of metal wear debris in a pediatric patient. Spine (Phila Pa 1976). 2013;38:E38–42. https://doi.org/10.1097/BRS.0b013e3182793e51.
Bess S, Akbarnia BA, Thompson GH, et al. Complications of growing-rod treatment for early-onset scoliosis: analysis of one hundred and forty patients. J Bone Joint Surg Am. 2010;92:2533–43.
Sankar WN, Skaggs DL, Yazici M, et al. Lengthening of dual growing rods and the law of diminishing returns. Spine (Phila Pa 1976). 2011;36:806–9.
Thakar C, Kieser DC, Mardare M, Haleem S, Fairbank J, Nnadi C. Systematic review of the complications associated with magnetically controlled growing rods for the treatment of early onset scoliosis. Eur Spine J. 2018;27:2062–71.
Buttermann GR, Mullin WJ. Pain and disability correlated with disc degeneration via magnetic resonance imaging in scoliosis patients. Eur Spine J. 2008;17:240–9.
Green DW, Lawhorne TW III, Widmann RF, Kepler CK, Ahern C, Mintz DN, Rawlins BA, Burke SW, Boachie-Adjei O. Long-term magnetic resonance imaging follow-up demonstrates minimal transitional level lumbar disc degeneration after posterior spine fusion for adolescent idiopathic scoliosis. Spine (Phila Pa 1976). 2011;36:1948–54.
Harding IJ, Charosky S, Vialle R, Chopin DH. Lumbar disc degeneration below a long arthrodesis (performed for scoliosis in adults) to L4 or L5. Eur Spine J. 2008;17:250–4.
Danielsson AJ, Cederlund CG, Ekholm S, Nachemson AL. The prevalence of disc aging and back pain after fusion extending into the lower lumbar spine. A matched MR study twenty-five years after surgery for adolescent idiopathic scoliosis. Acta Radiol. 2001;42:187–97.
Kelly DM, McCarthy RE, McCullough FL, Kelly HR. Long-term outcomes of anterior spinal fusion with instrumentation for thoracolumbar and lumbar curves in adolescent idiopathic scoliosis. Spine (Phila Pa 1976). 2010;35:194–8.
Akazawa T, Kotani T, Sakuma T, Minami S, Orita S, Fujimoto K, Shiga Y, Takaso M, Inoue G, Miyagi M, Aoki Y, Niki H, Torii Y, Morioka S, Ohtori S, Takahashi K. Spinal fusion on adolescent idiopathic scoliosis patients with the level of L4 or lower can increase lumbar disc degeneration with sagittal imbalance 35 years after surgery. Spine Surg Relat Res. 2017;1:72–7.
Chiu CK, Tan CS, Chung WH, et al. Mid-long-term outcome and degeneration of the remaining unfused lumbar intervertebral disc in adolescent idiopathic scoliosis patients who had posterior spinal fusion surgery. Eur Spine J. 2021;30:1978–87.
Burton DC, Asher MA, Lai SM. Patient-based outcomes analysis of patients with single torsion thoracolumbar-lumbar scoliosis treated with anterior or posterior instrumentation. An average 5- to 9-year followup. Spine (Phila Pa 1976). 2002;27:2363–7.
Cook S, Asher MA, Lai SM, Shobe J. Reoperation after primary posterior instrumentation and fusion for idiopathic scoliosis, toward defining late operative site pain of unknown cause. Spine (Phila Pa 1976). 2000;25:463–8.
Islam NC, Wood KB, Transfeldt EE, Winter RB, Dnis F, Lonstein JE, Ogilvie JW. Extension of fusions to the pelvis in IS. Spine (Phila Pa 1976). 2001;26:166–73.
Skaggs DL, Samuelson MA, Hale JM, Kay RM, Tolo VT. Complications of posterior iliac crest bone grafting in spine surgery in children. Spine (Phila Pa 1976). 2000;25:2400–2.
Woolf SK, Gross RH. Perceptions of allograft safety and efficacy among spinal deformity surgeons. J Pediatr Orthop. 2001;21:767–71.
Lee CS, Nachemson AL. The crankshaft phenomenon after posterior Harrington fusion in skeletally immature patients with thoracic or thoracolumbar IS followed to maturity. Spine (Phila Pa 1976). 1997;22:58–67. https://doi.org/10.1097/00007632-199701010-00010.
Roberto RE, Lonstein JE, Winter RB, Danis F. Curve progression in Risser stage 0 or 1 patients after posterior spinal fusion for IS. J Pediatr Orthop. 1997;17:718–25. https://doi.org/10.1097/00004694-199711000-00005.
Arlet V, Marchesi D, Papin P, Aebi M. Decompensation following scoliosis surgery: treatment by decreasing the correction of the main thoracic curve or ‘letting the spine go’. Eur Spine J. 2000;9:156–60. https://doi.org/10.1007/s005860050227.
Van Ooij A, van Belle A, Timmer R, van Rhijn L. The destroyed lung syndrome report of a case after Harrington rod instrumentation and fusion for IS. Spine (Phila Pa 1976). 2002;27:E337–41. https://doi.org/10.1097/00007632-200207150-00021.
Pratt RK, Webb JK, Burwell RG, Cole AA. Changes in surface and radiographic deformity after universal spine system for right thoracic adolescent IS. Is rib hump reassertion a mechanical problem of the thoracic rib cage rather than an effect of relative anterior spinal overgrowth? Spine (Phila Pa 1976). 2001;26:1778–87. https://doi.org/10.1097/00007632-200108150-00009.
Barrett DS, MacLean JGB, Bettan J, Ransford AO, Edgar MA. Costoplasty in AIS: objective results in 55 patients. J Bone Joint Surg Br. 1993;75-B:881–5.
Winter RB. Flail chest secondary to excessive rib resection in IS: case report. Spine (Phila Pa 1976). 2002;27:668. https://doi.org/10.1097/00007632-200203150-00021.
Hawes M. Impact of spine surgery on signs and symptoms of spinal deformity. Pediatr Rehabil. 2006;9:318–39. https://doi.org/10.1080/13638490500402264.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Sudhir, G., Sharief, N., Kailash, K.K. (2023). Long-term Outcomes in the Surgical Management of Adolescent Idiopathic Scoliosis and Early-Onset Scoliosis. In: Zacharia, B., Raja, S.D.C., KV, N. (eds) Paediatric Scoliosis . Springer, Singapore. https://doi.org/10.1007/978-981-99-3017-3_31
Download citation
DOI: https://doi.org/10.1007/978-981-99-3017-3_31
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-99-3016-6
Online ISBN: 978-981-99-3017-3
eBook Packages: MedicineMedicine (R0)