Abstract
This chapter provides information regarding the chronic inflammatory skin disorder atopic dermatitis (AD), highlighting the prevalence of the disease, different diagnostic criteria, diagnosis procedures and clinical features of AD. The pathogenesis of AD is multifactorial resulting from complex interplay among immune dysregulation, epidermal barrier disruption, environment, and genetic predisposition, nutritional, psychological and pharmacological factors. Immune dysregulation and epidermal barrier dysfunction are the major pathophysiological defects along with genetic variation in Filaggrin (FLG), the most recurring finding contributing towards AD development. The major risk factors of AD are positive family history, environmental and lifestyle factors, use of broad-spectrum antibiotics in pregnancy and infants especially S. aureus colonisation and superinfections. Sleep disturbance, ADHD, psychiatric disorders, asthma and allergic rhinitis are the co-morbidities associated with chronic skin disease. Though there is no cure for AD, management basically aims at improving symptoms by using therapeutic agents like emollients, calcineurin inhibitors, topical corticosteroids, systemic immunosuppressants and phototherapy depending upon the severity of the symptoms. Gut microbiome impacts AD through immunologic pathway, metabolite pathway and neuroendocrine pathway. Probiotics helps in improving the intestinal barrier by modulating the immune status and intestinal microbiome by performing immunomodulatory effect, metabolic effect and standardisation of microbial composition by protection of the mucosal surface against pathogens. This chapter also explores information regarding various studies linking gut and skin microbiome with AD and also summarises the clinical trials using probiotics as interventions in improving the disease condition.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
15.1 Introduction
Atopic dermatitis is a chronic inflammatory skin disorder characterised by its clinical hallmarks —xerosis (dry skin), intensive itching and recurring eczematous lesions. This disease is also referred as atopic eczema (Wallach and Taïeb 2014; Weidinger and Novak 2016). Plateauing at 10–20% in the developed countries, this inflammatory disorder still has a growing prevalence in the developing countries (Deckers et al. 2012; Williams et al. 2008). The disease starts affecting the individuals from infancy, manifesting from the first year of life (i.e. early onset) with the earliest clinical signs like dry skin and rough texture but the occurrence of eczematous lesions takes place in the second month or later (Garmhausen et al. 2013; Illi et al. 2004). Atopic dermatitis is equally prevalent in the adults and as the findings suggests a higher prevalent adult onset can start at any age than assumed previously (Weidinger and Novak 2016). Even after long symptom-free periods and outgrowing of disease, the patients tend to suffer from sensitive hyper-reactive skin (Garmhausen et al. 2013). The prevalence of AD in children is age related; being around 60% during the first year after birth and 90% by 5 years of age. The paediatric AD is in rising trend (approximately 30%) in the developing countries and the causes of such trend is still unknown. It may be due to genetic and environmental factors which tend to play a contributing role according to several systematic large-scale studies (Waldman et al. 2018). Various sets of diagnostic criteria like the Hanifin and Rajka criteria (Fig. 15.1) and The UK Working Party criteria (a scientific refinement of the Hanifin and Rajka criteria) are used for clinical and epidemiological studies in children (Brenninkmeijer et al. 2008).
Morphological variations lead to occurrence of clinical features. Dark skinned people tend to suffer from follicular type features mainly characterised by follicular papules that are densely aggregated (Brenninkmeijer et al. 2008; Weidinger and Novak 2016). The lesions are characterised morphologically by erythema, lichenisation, crusting, excoriation and exudation. The AD skin has poor threshold for pruritus and irritation causing an “itch-scratch” cycle leading to secondary infection, poor sleep quality, etc. Environmental irritants, coarse clothing and allergens could lead to exacerbation of pruritus (Waldman et al. 2018). The disease severity depends upon the factors like flare frequency, disease persistence, quality of life and co-morbidities. Several methods are available to delineate the severity of AD. Eczema Area Severity Index, Scoring of Atopic Dermatitis Index, Investigator Global Assessment are the preferred scoring systems to measure the signs but are generally not used in the clinical practice (Waldman et al. 2018; Weidinger and Novak 2016). The currently used disease severity scores in clinical trials include: Severity Scoring of Atopic dermatitis (SCORAD), Eczema Area and Severity Index (EASI) (based upon the template of the Psoriasis Area Severity Index (PASI) used for disease severity score for psoriasis) and Harmonising Outcome Measures for Eczema (HOME) (Laird and Lo Sicco 2017). Table 15.1 enlists the common, uncommon and rare occurring clinical disorders that must be first excluded when an individual complains about poor response to therapy, unusual infection or an atypical rash while diagnosing a patient of AD (Weidinger and Novak 2016).
Atopic dermatitis has multifactorial pathogenesis resulting from complex coactions among immune dysregulation, epidermal barrier disruption, environment and genetic predisposition, nutritional, psychological and pharmacological factors (Waldman et al. 2018 7 7). Though, the principal factors and the chief events contributing to the disease still remain the topics of debate. Immune abnormalities and epidermal barrier dysfunction are the two major and converging pathophysiological abnormalities (Elias and Steinhoff 2008). The most steadily replicating findings show involvement of genetic variations in Filaggrin (FLG) in the aetiology of AD. FLG gene copy number variation influences the FLG protein expression that in turn influences AD development. This gene influences factors like skin hydration promotion, barrier function and immune modulation of the superficial epidermis. Immune abnormalities arise majorly due to mechanical injury, microbes and allergy that activate the skin’s innate immune system inciting inflammation because of the increased expression of certain cytokines principally IL-25, IL-33 and thymic stromal lipoprotein. Further activation of T-helper (Th-2) cells and increased number of the above-mentioned cytokine release result in suppression of epidermal barrier and antimicrobial peptides (IL-4, IL-5, IL-6) and promotion of eosinophilia, IgE production and cytokine associated inflammation. IL-31 production along with the release of other mediators like neuropeptidases, histamine, tryptase is also promoted by Th-2 release leading to pruritus, one of the most prominent symptoms of AD. In chronic AD, there is also a significant increase of Th-1 and Th-22 cytokines. Structural proteins and lipids that are essential for water retention and barrier protection also show a marked decline impairing the barrier function of the skin significantly (Waldman et al. 2018).
Positive family history of AD forms the major risk factor of the disease (Apfelbacher et al. 2011). This inherited susceptibility is triggered by environmental and lifestyle factors leading to disease manifestation. Some of these environmental risk factors are small family size, western diet enriched with sugar and PUFA, urban lifestyle, low exposure to ultraviolet radiation and low humidity (Flohr and Mann 2014). Exposure to broad-spectrum antibiotics in pregnant women and infants is also one of the other risk factors of AD (Flohr and Yeo 2011). Patients with AD tend to suffer from various infectious complications due to defect in epidermal barrier and insufficient antimicrobial peptide upregulation. Staphylococcus aureus colonisation is observed in up to 90% affected skin patients of AD leading to exacerbation and chronification of disease by producing proteases, releasing enterotoxins and stimulating innate signalling pathways. In number of AD superinfections, Group A Streptococcus plays a significant role by increasing the frequency of fever, facial involvement and hospitalisation in children. The combination of factors like aberrant innate and adaptive immune responses as well as epidermal deficiency leads to Herpes simplex virus infection and Eczema herpeticum infection; it is marked by the presence of umbilicated vesicopustules. Children also tend to suffer from ailments like Molluscum contagiosum and eczema coxsackium (caused by coxsackium virus (CVA6))(Waldman et al. 2018).
Co-morbidities associated with AD include sleep disruption, ADHD (attention-deficit/hyperactivity disorder), psychiatric disorders (depression, anxiety and conduct disorders), asthma and allergic rhinitis. Some preliminary studies suggest an increased risk of rheumatoid arthritis, alopecia areata, vitiligo and inflammatory bowel disorder in AD patients (Mohan and Silverberg 2015; Schmitt et al. 2016). On the other hand, decreased risk of type 1 diabetes and cancers (glioma, meningioma and acute lymphoblastic leukaemia) is observed in patients suffering from AD. The disease has some severe effects on patients as well as the society (Deckert et al. 2014; Schmitt et al. 2016). Sleep deprivation, social embarrassment and itch tend to have a major effect on the psychosocial well-being of patients and their relatives (Beattie and Lewis-Jones 2006). Atopic dermatitis has been ranked first amidst common skin diseases with respect to disability-adjusted life years and years lived with a disease in the WHO 2010 Global Burden of Disease survey (Murray et al. 2014; Vos et al. 2012).
As there is no significant cure for AD at present, management of AD aims at improving symptoms and achieving long-term disease control following a multistep approach. The AD management has been outlined in national and international guidelines. Continuous epidermal barrier repair has always been a priority by use of emollients avoiding individual trigger factors. Calcineurin inhibitors and topical corticosteroids are selected classes of drugs for anti-inflammatory therapy. Severely affected cases are managed by systemic immunosuppressants and phototherapy (Weidinger and Novak 2016).
15.2 Relationship between Gut Microbiota and Atopic Dermatitis
Development of AD might witness a crucial role of gut microbiota by regulating the maturation of the immune system due to the crosstalk that occurs between the host and microbiome at the early life (Arpaia et al. 2013; Olszak et al. 2012). “Hygiene hypothesis” was formulated on the fact that there is an inverse relationship between the early exposure to microbial agents and AD (Derrien and Veiga 2017). Immune system alterations might take place once there is any disruption in the gut microbiome due to the production of metabolites like free phenol and paracresol in vast amounts by the gut flora (Dawson et al. 2011; Zeng et al. 2017). The metabolites tend to affect the distant sites of the organism by entering the circulation and travelling throughout the body. The disrupted epithelial barrier leads to increased intestinal permeability and increasing the levels of metabolite a condition known as “Leaky gut syndrome”(Maguire and Maguire 2017). Figure 15.2 highlights this leaky gut syndrome showcasing disruption of mucosal barrier. According to studies, paracresol and free phenol reduce the expression of keratin 10 in keratinocytes resulting in the disruption of the epidermal barrier integrity.
Disruption of mucosal barrier in AD. Patients with AD have dysbiosis and less short-chain fatty acids (SCFAs) in the gut. In response to proinflammatory cytokines, monocyte migrate and differentiate into macrophages, greater access to luminal antigens also causes T-cells to transform into Th-2 cells in the draining lymph nodes. Immunoglobulin E (Ig E) and mast cells are also more abundant in lamina propria. IgE immunoglobulin E, IL interleukin, Th2 T-helper cells, TSLP thymic stromal lymphopoietin, IgA immunoglobulin A (Kim and Kim 2019)
The mode of delivery greatly influences the microbiota of the skin and gut in the new-borns marking the exposure of microbes during the birth (Dominguez-Bello et al. 2010). A greater association has been found between the caesarean section delivery and an increased risk of immune disorders like asthma, allergy and inflammatory bowel disorders (Sevelsted et al. 2015). Infants acquire microbial species typically from the mother’s skin surface in which Staphylococcus, Corynebacterium and Propionibacterium sp. dominantly found on the mother’s skin. On the other hand, vaginally delivered infants harbour bacterial communities of general Lactobacillus and Prevotella resembling their mother’s vaginal microbiota, lactobacilli of such origin acts as a protective barrier of the immature immune system of the infants against pathogens that have a major relevance in skin disorders like Staphylococcus aureus (Dominguez-Bello et al. 2010). In early life, stress, diet and pollution are amongst the various environmental factors affecting the composition and profiling of the microbes; such diverse factors drive the contribution of the gut microbiota in the development of AD (Gensollen and Blumberg 2017). Damage of intestinal barrier is noted in individuals consuming dietary gluten; even they do not suffer from celiac disease leading to a leaky gut (Uhde et al. 2016). Severe cutaneous manifestations mimicking AD has been further associated with both celiac and non-celiac gluten sensitivity (Bhatia et al. 2014; Bonciolini et al. 2015). Severity of AD can also be correlated to the low Vitamin D levels, as the systemic Vitamin D metabolism is regulated by the gut microbiota and acts as a significant signalling mechanism between the host and microbiota (Bora et al. 2018; Ly et al. 2011). The proportion of Bifidobacteria, Bacteroides and Bacteroidetes decreases significantly in the patients of AD as compared to control; on the other hand, Clostridium difficile, Clostridia, Escherichia coli and Staphylococcus aureus tend to show a higher number in the gut microbiome. Table 15.2 shows such alterations in microbial diversity in non- affected AD skin v/s lesional AD skin (Abrahamsson et al. 2012; Adams et al. 2006; Kirjavainen et al. 2002; Lee et al. 2016; Nylund et al. 2015). Short-chain fatty acids (SCFA) such as butyrate, acetate, lactate and propionate tend to exert anti-inflammatory effect as well as maintain the epithelial barrier integrity (Smith et al. 2013). These SCFA are produced during the fibre fermentation by the gut microbiota (Maslowski et al. 2009). Species associated with Firmicutes phylum such as Roseburia intestinalis, Eubacterium hallii and Faecalibacterium prausnitzii are involved in the production of butyrate (Louis and Flint 2017). Propionate is produced by the species belonging to Bacteroidetes phylum like Bacteroides uniformis, Prevotella copri and Verrucomicrobia phylum like Akkermansia muciniphila in the patient of AD (Louis and Flint 2017; Mikó et al. 2019), indicating the gut microbiome playing role in the SCFA pathway was noted to have increased significantly. Association of AD with intestinal Clostridia and Escherichia coli is established due to eosinophilic inflammation leading to the development of AD (Lee et al. 2016). Development of host immune system is also disrupted due to the alterations of functional genes in the presence of specific gut microbiome like Akkermansia muciniphila and Ruminococcus gnavus (Song et al. 2016).
Secondary bile acids like the litocholic acid and deoxycholic acid produced by Firmicutes and Bacteroidetes phyla also reported to have impacts on the physiology of the skin (Mikó et al. 2018; Ridlon et al. 2006). Adaptive immune response is greatly affected due to faulty activation of Th-1 cells reportedly caused by litocholic acid (Pols et al. 2017). Reports show that Clostridium difficile infection that affects the skin in the secondary bile acid dependent manner could confer resistance in the presence of Clostridium scindens belonging to Firmicutes phyla (Buffie et al. 2015). The combined effects of gut microbiome dynamics and varied environmental factors should be studied further for more accurate evaluation of the impact of gut microbiome in AD development.
15.3 Mechanism Involved
Gut microbiome impacts AD through three major pathways, namely immunologic, metabolite and neuroendocrine pathways (Fig. 15.3) (Kim and Kim 2019).
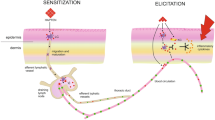
Disruption of epidermal barrier in the AD skin. Trans-epithelial water loss (TEWL), pH, serum IgE, serum thymus and activated cytokine (TARC/CCL17), and eosinophils are significantly elevated in AD patients. Filaggrin and stratum corneum (SC) lipid composition, and serine protease (Kallikreins) are also altered in AD, allowing S. aureus colonisation. With decrease in coagulase-negative Staphylococci (CoNS) and its antimicrobial peptides (AMP), S. aureus proliferates and also forms biofilms. AD atopic dermatitis, CER ceramide, FFA free fatty acid, IL interleukin, S. aureus staphylococcus aureus, TNF tumour necrosis factor, TSLP thymic stromal lymphopoietin (Kim and Kim 2019)
15.3.1 Immunologic Pathway
Barrier dysfunction and immune response are two major biological pathways involved in the clinical manifestation of AD. Secretion of T-helper (Th) 2 cytokines like IL-4, IL-5 and IL-13 due to TH1/TH2 imbalance leads to increased production of immunoglobulin E (IgE) and increased binding of S. aureus to AD infected skin. Being the most common pathogen affecting AD akin, S. aureus carries a combination of superantigens and adhesion genes that affects AD development in infancy negatively by stimulating and promoting the immune system of infants. Although S. aureus leads to increase in the severity of established AD, commensal mucosal colonisation by S. aureus before the “atopic march” could provide a possibility of a broad immune stimulation by this bacterium generating a protective effect (Huang et al. 2017).
15.3.2 Metabolite Pathway
The relationship between dietary supplements, microbiome and immune system of skin can be established by the SCFAs released by the gut microbiome, majorly by Akkermansia muciniphila playing a significant role in various inflammatory diseases like AD (Reichardt et al. 2014; Song et al. 2016; Thorburn et al. 2014). Various studies supported that the anti-allergic and anti-inflammatory effects due to the oral administration of the metabolites can modulate various skin diseases (Miyamoto et al. 2015). Alleviation of AD and gut microbiome modulation in a mouse model was observed after the administration of linoleic acid and 10-hydroxy-cis-12-octadecenoic acid. While in another study, reduced scratching behaviour in AD mice due to administration of probiotic Bifidobacterium animalis subsp. lactis (LKM512) was observed, which was attributed to increased levels of the metabolite kynurenic acid (Lee et al. 2018b; Matsumoto et al. 2014). These diverse studies support that there is an existence of gut-skin axis communications mediated by metabolites.
15.3.3 Neuroendocrine Pathway
Neuroendocrine molecules produced by the gut microbiome show effects on the gut-skin axis. The degree of AD symptoms depends on the release of diverse neuromodulators and neurotransmitters, now being associated to differences in composition and proportion of gut microbiome. These neuromodulators and neurotransmitters affect the immune system dysregulation and skin barrier dysfunction, which are the two key pathophysiologies in AD development (Lee et al. 2018b). Direct and indirect pathways are undertaken by the gut microbiome in order to modulate the gut-skin axis (Yokoyama et al. 2015). Tryptophan released by the gut microbiome directly affects the gut-skin axis by producing an itching sensation in the skin (Jin et al. 2014). Skin pigmentation can occur by serotonin produced by Escherichia and Enterococcus species (Cryan and Dinan 2012; Lee et al. 2011). Indirect pathways involve the release of cortisol under stress conditions that could alter the gut microbiome composition leading to changes like alteration in barrier function and gut epithelium permeability (Cryan and Dinan 2012). Cytokine levels in the bloodstream can also be modulated indirectly by gut microbiome affecting anxiety and stress, further affecting the levels of cortisol (Yokoyama et al. 2015).
S. aureus colonisation takes place due to alterations in filaggrin and stratum corneum lipid composition as well as serine protease, i.e. kallikreins. Proliferation of S. aureus and formation of biofilms occur due to decrease in Coagulates-negative Staphylococci (CoNS) and its associated antimicrobial peptides (AMP). AD patients show an elevation in pH, eosinophils, serum IgE, activated cytokine (TARC/CCL17), serum thymus and trans-epithelial water loss (TEWL) (Kim and Kim 2019). Probiotics help in improving the intestinal barrier by modulating the immune status and intestinal microbiome that further helps in reducing the allergic phenomenon as well as AD severity (Alvarez-Olmos and Oberhelman 2001). There are increasing number of studies being conducted in recent years to evaluate the effect of probiotics administration in patients at different stages of their life, i.e. during pregnancy and lactation, infancy, childhood and adulthood (Rusu et al. 2019). Studies suggest that probiotics contributed significantly in combating the severe symptoms of atopic dermatitis and providing efficient and beneficial treatment to the patients suffering from AD.
Probiotics follows different mechanism of actions in order to provide relief to the inflammatory skin disorder (Kim and Kim 2019) (Fig. 15.4).
Immune mechanisms of Pre- and probiotics. Probiotics and commensal bacteria when fed along with prebiotics, probiotics seem to modulate the microenvironment, competing with pathogens, balancing the cell mediated immune response (decreases response of Th2, increases Treg cells) and humoral response (increases IgA and decreases IgE). SCFA short-chain fatty acid, AMP antimicrobial peptide, DC dendritic cells, IL interleukin, TGF tumour growth factor, IgE immunoglobulin E, IgA Immunoglobulin A, Th1 T-helper 1 cells, Th2 T-helper 2 cells (Kim and Kim 2019)
15.3.4 Immunomodulatory Effect
Probiotics act by stabilising the Th1/Th2 ratio reducing the severity of AD. They also inhibit the Th-2 mediated response, further leading to decreased or no release of the cytokines (IL-4, IL-5, IL-6 and IL-13) (Enomoto et al. 2014; Feleszko et al. 2007; Jang et al. 2012; Nwanodi 2018). There is a significant reduction in the proinflammatory cytokines, tumour necrosis factor-a (TNF-a), IL-4, IL-6, INF gamma and high sensitivity C reactive protein (hsCRP) (Zheng et al. 2018) and a remarkable increment in the expression of Treg-related cytokines and IL-10 at the mesenteric lymph nodes leading to reduced inflammation contributed by the probiotics (Rusu et al. 2019). The efficacy of probiotics was suggested in a new mechanism where its ability to inhibit the mature dendritic cell differentiation and transforming of naive T cells into Th-2 is demonstrated (Kim et al. 2013). Probiotics promote phagocytosis; stimulate the release of IL-10 and transforming growth factor-b (TGF-b) as well as increases level of serum IgA (Tatu et al. 2016). Probiotics also modulate the intestine-skin axis and brain function reducing the susceptibility to inflammatory and allergic factors and stress to the intestine-skin axis, respectively (Messaoudi et al. 2011; Rusu et al. 2019).
15.3.5 Protection of the Mucosal Surface against Pathogens by Standardisation of the Microbial Composition
The prevalence of allergic diseases is influenced by the abundance of varied Bifidobacterium species in the faeces of the newborn. A notable higher level of Bifidobacterium longum was observed in healthy children when a study was conducted to detect the levels of varied Bifidobacterium species in the faeces of allergic children as compared to healthy ones proposing the role of this strain in avoiding the occurrence of allergic dermatitis and bronchial asthma (Akay et al. 2014). Lactobacillus is also amongst the popular probiotic agent providing benefits like an acceleration of the skin barrier recovery as well as inhibiting inflammation of skin related to substance P (Gueniche et al. 2010). Human origin Lactobacillus along with Enterococcus also indicated that probiotics could lead to the strengthening of mucosal barrier as it increases the production of SCFA (Nagpal et al. 2018; Salem et al. 2018). In fact, modulation in the microbial composition can also occur by using probiotics as a therapeutic tool.
15.3.6 Metabolic Effect
Proinflammatory cytokines (IL-6, TNF-a, CRP), chronic systemic inflammation, inflated oxidative stress and changing expressions of inflammatory genes establish a relationship between AD and metabolic disorders like obesity, dyslipidaemia, etc. (Rusu et al. 2019). There is an association between probiotic consumption and reduced blood glucose, insulin resistance and insulinaemia (Ruan et al. 2015). Various meta-analysis studies were also conducted to collect more evidences relating the probiotics and metabolic effect. One study was conducted in patients suffering from non-alcoholic fatty liver disease where the decrease in alanine aminotransferase and insulin resistance showed favourable effects (Ma et al. 2013). Other suggested the association of decreased total cholesterol, triglycerides, low density lipoprotein cholesterol and increased high density lipoprotein cholesterol with administration of probiotics (He et al. 2017). Overweight and obese patients had a higher risk of AD development, highlighted by the systematic review conducted by Zhang and Silverberg (Zhang and Silverberg 2015).
15.4 Clinical and In-Vivo Status
There have been various studies that show the involvement of both gut microbiome and skin microbiome in AD. Table 15.3 summarises previous studies that report the involvement of gut microbiome in AD. Table 15.4 summarises the previous studies of involvement of skin microbiome in AD.
COCHRANE review assessed the effects of probiotics on the patients with eczema and examines the advantageous effects of probiotics on the AD patients (Hulshof et al. 2017). According to the review, no evidence was found suggesting that probiotics showed any major difference in the quality of life of eczema patients. Even little or no difference was made by probiotics in the participant or patient related symptoms that were associated with eczema. The review also indicates reduced investigator rated eczema severity scores but clinically the results were not sufficient. Above findings concluded that currently usage of probiotics for the treatment of eczema is not evidence based. The variance in response is observed as species and strains employed in the treatment have significant variations, thus Meta-analysis does not support the use of probiotics for treatment of AD (Hulshof et al. 2017).
Randomised control trials also took place as the results of past clinical interventions showed inconclusive results of probiotics in AD treatment (Hulshof et al. 2017). Four randomised clinical trials conducted by Han et al. (2012), Woo et al. (2010), Miniello et al. (2010) and Torii et al. (2011) provided results of study using only one probiotic as dietary intervention (Table 15.5) (Han et al. 2012; Miniello et al. 2010; Torii et al. 2011; Woo et al. 2010). AD severity was improved in three out of four trials using one probiotic strain (Hulshof et al. 2017). Additional effect was observed in the (Han et al. 2012) clinical trial, the cytokine level of IL-4 and IFN-y significantly lowered or did not fluctuate as was changing before the intervention. On the other hand, two randomised clinical trials conducted by Wang and Wang (2015) and Gore et al. (2012) used more than one probiotic strain in the study (Table 15.6) (Gore et al. 2012; Wang and Wang 2015). Gore et al. trial revealed a reduction in SCORAD score in both the groups, whereas (Wang and Wang 2015) reported that selected AD children having at least one elevated specific IgE level or at least one positive skin prick test showed improvement in AD with probiotic administration. Both these studies showed IgE level changes but there was no significance between treatment and control (Hulshof et al. 2017).
The above-mentioned clinical trials have several confounding factors that should be considered while interpreting the results of the study. For example, SCORAD score is used and validated for clinical outcome comparisons in order to assess the AD severity but such scoring is difficult when noted in infants due to inter-observer variability and the constant relapsing–remitting nature of AD in young patients complicates the process of assessing AD severity and nutritional intervention effects at a particular time (Hulshof et al. 2017). AD severity recommendations for future clinical trials were made based on evaluation using core symptom instruments such as SIS (skin intensity score), POEM (patient–oriented eczema measure), SA-EASI (self-administered eczema area and severity index score), SCORAD (severity scoring of atopic dermatitis index) and adapted SA-EASI. Mucosal immune system programming and prevention of AD development via microbial modulation is basically preferred in the first year of life. Though dietary intervention studies during pregnancy, lactation or in the early life of infants revealed decreased risk of AD development but tend to have no effect on the development of other allergies unlike some of the meta-analysis studies justifying the clinical evidence of dietary intervention in AD. Due to inconsistent results obtained from various studies substantial evidence is still low. In order to maintain the consistency in the various studies, a defined criterion should be set up for easy comparability of the clinical trial outcomes. Such consistency in studies subsequently motivates to provide reliable advice for implementation of dietary interventions in AD management (Gerbens et al. 2018).
15.5 Conclusion
This chapter provides elaborate information on the chronic inflammatory skin disorder, atopic dermatitis (AD), highlighting the prevalence of the disease, different diagnostic criteria and differential diagnosis tools of AD. The pathogenesis of AD is multifactorial resulting from complex interplay among immune dysregulation, epidermal barrier disruption, environment, genetic predisposition, nutritional, psychological and pharmacological factors. Immune abnormalities and epidermal barrier dysfunction are the major pathophysiological abnormalities along with genetic variation in FLG play significant role in AD development. The major risk factors of AD are also enlisted with various co-morbidities associated with the disease. AD management basically aims at combating symptoms by using therapeutic agents like emollients, calcineurin inhibitors, topical corticosteroids, systemic immunosuppressants and phototherapy depending upon the severity of the symptoms, as there is no significant cure of AD.
There is an established relationship between the gut microbiome and atopic dermatitis. Gut microbiome impacts AD through immunologic pathway, metabolite pathway and neuroendocrine pathway. Stress, diet and pollution are amongst the various environmental factors that affect the composition and proliferation of the microbes leading to development of AD. Low vitamin D, short-chain fatty acids (SCFA) and secondary bile acids like the litocholic acid and deoxycholic acid play different roles in gut dysbiosis and impacting epithelial barrier integrity and physiology of the skin, respectively. Probiotics improves the intestinal barrier by modulating the immune status and intestinal microbiome by performing immunomodulatory, metabolic effect and protection of the mucosal surface against pathogens by standardisation of the microbial composition. The chapter in the end summarises various studies linking gut and skin microbiome with atopic dermatitis. It also summarises different clinical trials reporting the role of probiotics as dietary intervention in improvement of disease condition.
References
Abrahamsson TR, Jakobsson HE, Andersson AF, Björkstén B, Engstrand L, Jenmalm MC (2012) Low diversity of the gut microbiota in infants with atopic eczema. J Allerg Clin Immunol 129(2):434–440.e432
Adams H, Penders J, van den Brandt P, Ree CV, Vink C, Thijs C, Stobberingh E (2006) Molecular fingerprinting of the intestinal microbiota of infants in whom atopic eczema was or was not developing
Akay HK, Tokman HB, Hatipoglu N, Hatipoglu H, Siraneci R, Demirci M, Borsa BA, Yuksel P, Karakullukcu A, Kangaba AA (2014) The relationship between bifidobacteria and allergic asthma and/or allergic dermatitis: a prospective study of 0–3 years-old children in Turkey. Anaerobe 28:98–103
Alvarez-Olmos MI, Oberhelman RA (2001) Probiotic agents and infectious diseases: a modern perspective on a traditional therapy. Clin Infect Dis 32(11):1567–1576
Apfelbacher C, Diepgen T, Schmitt J (2011) Determinants of eczema: population-based cross-sectional study in Germany. Allergy 66(2):206–213
Arpaia N, Campbell C, Fan X, Dikiy S, van der Veeken J, Deroos P, Liu H, Cross JR, Pfeffer K, Coffer PJ (2013) Metabolites produced by commensal bacteria promote peripheral regulatory T-cell generation. Nature 504(7480):451–455
Beattie P, Lewis-Jones M (2006) A comparative study of impairment of quality of life in children with skin disease and children with other chronic childhood diseases. Br J Dermatol 155(1):145–151
Bhatia BK, Millsop JW, Debbaneh M, Koo J, Linos E, Liao W (2014) Diet and psoriasis, part II: celiac disease and role of a gluten-free diet. J Am Acad Dermatol 71(2):350–358
Bonciolini V, Bianchi B, Del Bianco E, Verdelli A, Caproni M (2015) Cutaneous manifestations of non-celiac gluten sensitivity: clinical histological and immunopathological features. Nutrients 7(9):7798–7805
Bora SA, Kennett MJ, Smith PB, Patterson AD, Cantorna MT (2018) The gut microbiota regulates endocrine vitamin D metabolism through fibroblast growth factor 23. Front Immunol 9:408
Brenninkmeijer E, Schram M, Leeflang M, Bos J, Spuls PI (2008) Diagnostic criteria for atopic dermatitis: a systematic review. Br J Dermatol 158(4):754–765
Buffie CG, Bucci V, Stein RR, McKenney PT, Ling L, Gobourne A, No D, Liu H, Kinnebrew M, Viale A (2015) Precision microbiome reconstitution restores bile acid mediated resistance to Clostridium difficile. Nature 517(7533):205–208
Cryan JF, Dinan TG (2012) Mind-altering microorganisms: the impact of the gut microbiota on brain and behaviour. Nat Rev Neurosci 13(10):701–712
Dawson LF, Donahue EH, Cartman ST, Barton RH, Bundy J, McNerney R, Minton NP, Wren BW (2011) The analysis of Para-cresol production and tolerance in Clostridium difficile 027 and 012 strains. BMC Microbiol 11(1):86
Deckers IAG, McLean S, Linssen S, Mommers M, van Schayck CP, Sheikh A (2012) Investigating international time trends in the incidence and prevalence of atopic eczema 1990-2010: a systematic review of epidemiological studies. PLoS One 7(7)
Deckert S, Kopkow C, Schmitt J (2014) Nonallergic comorbidities of atopic eczema: an overview of systematic reviews. Allergy 69(1):37–45
Derrien M, Veiga P (2017) Rethinking diet to aid human–microbe symbiosis. Trends Microbiol 25(2):100–112
Dominguez-Bello MG, Costello EK, Contreras M, Magris M, Hidalgo G, Fierer N, Knight R (2010) Delivery mode shapes the acquisition and structure of the initial microbiota across multiple body habitats in newborns. Proc Natl Acad Sci 107(26):11971–11975
Drago L, De Grandi R, Altomare G, Pigatto P, Rossi O, Toscano M (2016) Skin microbiota of first cousins affected by psoriasis and atopic dermatitis. Clin Mol Allerg 14(1):2
Elias PM, Steinhoff M (2008) “Outside-to-inside”(and now back to “outside”) pathogenic mechanisms in atopic dermatitis. J Investig Dermatol 128(5):1067–1070
Enomoto T, Sowa M, Nishimori K, Shimazu S, Yoshida A, Yamada K, Furukawa F, Nakagawa T, Yanagisawa N, Iwabuchi N (2014) Effects of bifidobacterial supplementation to pregnant women and infants in the prevention of allergy development in infants and on fecal microbiota. Allergol Int 63(4):575–585
Feleszko W, Jaworska J, Rha RD, Steinhausen S, Avagyan A, Jaudszus A, Ahrens B, Groneberg D, Wahn U, Hamelmann E (2007) Probiotic-induced suppression of allergic sensitization and airway inflammation is associated with an increase of T regulatory-dependent mechanisms in a murine model of asthma. Clin Exp Allergy 37(4):498–505
Flohr C, Mann J (2014) New insights into the epidemiology of childhood atopic dermatitis. Allergy 69(1):3–16
Flohr C, Yeo L (2011) Atopic dermatitis and the hygiene hypothesis revisited. In: Pathogenesis and management of atopic dermatitis, vol 41. Karger Publishers, pp 1–34
Garmhausen D, Hagemann T, Bieber T, Dimitriou I, Fimmers R, Diepgen T, Novak N (2013) Characterization of different courses of atopic dermatitis in adolescent and adult patients. Allergy 68(4):498–506
Gensollen T, Blumberg RS (2017) Correlation between early-life regulation of the immune system by microbiota and allergy development. J Allergy Clin Immunol 139(4):1084–1091
Gerbens L, Prinsen C, Chalmers J, Drucker A, von Kobyletzki L, Limpens J, Nankervis H, Svensson Å, Terwee C, Zhang J (2018) Evaluation of the measurement properties of symptom measurement instruments for atopic eczema. A bird’s-eye view on eczema. p 43
Gore C, Custovic A, Tannock G, Munro K, Kerry G, Johnson K, Peterson C, Morris J, Chaloner C, Murray C (2012) Treatment and secondary prevention effects of the probiotics L actobacillus paracasei or B ifidobacterium lactis on early infant eczema: randomized controlled trial with follow-up until age 3 years. Clin Exp Allergy 42(1):112–122
Gueniche A, Benyacoub J, Philippe D, Bastien P, Kusy N, Breton L, Blum S, Castiel-Higounenc I (2010) Lactobacillus paracasei CNCM I-2116 (ST11) inhibits substance P-induced skin inflammation and accelerates skin barrier function recovery in vitro. Eur J Dermatol 20(6):731–737
Han Y, Kim B, Ban J, Lee J, Kim BJ, Choi BS, Hwang S, Ahn K, Kim J (2012) A randomized trial of L actobacillus plantarum CJLP 133 for the treatment of atopic dermatitis. Pediatr Allergy Immunol 23(7):667–673
He J, Zhang F, Han Y (2017) Effect of probiotics on lipid profiles and blood pressure in patients with type 2 diabetes: a meta-analysis of RCTs. Medicine 96(51)
Huang YJ, Marsland BJ, Bunyavanich S, O'Mahony L, Leung DY, Muraro A, Fleisher TA (2017) The microbiome in allergic disease: current understanding and future opportunities—2017 PRACTALL document of the American Academy of Allergy, Asthma & Immunology and the European academy of allergy and clinical immunology. J Allergy Clin Immunol 139(4):1099–1110
Hulshof L, Van’t Land B, Sprikkelman AB, Garssen J (2017) Role of microbial modulation in management of atopic dermatitis in children. Nutrients 9(8):854
Illi S, von Mutius E, Lau S, Nickel R, Grüber C, Niggemann B, Wahn U, Group MAS (2004) The natural course of atopic dermatitis from birth to age 7 years and the association with asthma. J Allergy Clin Immunol 113(5):925–931
Jang S-O, Kim H-J, Kim Y-J, Kang M-J, Kwon J-W, Seo J-H, Kim HY, Kim B-J, Yu J, Hong S-J (2012) Asthma prevention by lactobacillus rhamnosus in a mouse model is associated with CD4+ CD25+ Foxp3+ T cells. Allergy Asthma Immunol Res 4(3):150–156
Jin U-H, Lee S-O, Sridharan G, Lee K, Davidson LA, Jayaraman A, Chapkin RS, Alaniz R, Safe S (2014) Microbiome-derived tryptophan metabolites and their aryl hydrocarbon receptor-dependent agonist and antagonist activities. Mol Pharmacol 85(5):777–788
Kennedy EA, Connolly J, Hourihane JOB, Fallon PG, McLean WI, Murray D, Jo J-H, Segre JA, Kong HH, Irvine AD (2017) Skin microbiome before development of atopic dermatitis: early colonization with commensal staphylococci at 2 months is associated with a lower risk of atopic dermatitis at 1 year. J Allergy Clin Immunol 139(1):166–172
Kim JE, Kim HS (2019) Microbiome of the skin and gut in atopic dermatitis (AD): understanding the pathophysiology and finding novel management strategies. J Clin Med 8(4):444
Kim H-J, Kim HY, Lee S-Y, Seo J-H, Lee E, Hong S-J (2013) Clinical efficacy and mechanism of probiotics in allergic diseases. Korean J Pediatr 56(9):369
Kim M-H, Rho M, Choi J-P, Choi H-I, Park H-K, Song W-J, Min T-K, Cho S-H, Cho Y-J, Kim Y-K (2017) A metagenomic analysis provides a culture-independent pathogen detection for atopic dermatitis. Allergy Asthma Immunol Res 9(5):453–461
Kirjavainen P, Arvola T, Salminen S, Isolauri E (2002) Aberrant composition of gut microbiota of allergic infants: a target of bifidobacterial therapy at weaning? Gut 51(1):51–55
Kong HH, Oh J, Deming C, Conlan S, Grice EA, Beatson MA, Nomicos E, Polley EC, Komarow HD, Murray PR (2012) Temporal shifts in the skin microbiome associated with disease flares and treatment in children with atopic dermatitis. Genome Res 22(5):850–859
Laborel-Préneron E, Bianchi P, Boralevi F, Lehours P, Fraysse F, Morice-Picard F, Sugai M, Sato'o Y, Badiou C, Lina G (2015) Effects of the Staphylococcus aureus and Staphylococcus epidermidis secretomes isolated from the skin microbiota of atopic children on CD4+ T cell activation. PLoS One 10(10)
Laird M, Lo Sicco K (2017) Defining and measuring the scope of atopic dermatitis. Adv Exp Med Biol 1027:93–104. https://doi.org/10.1007/978-3-319-64804-0_9
Lee H, Park M, Kim S, Park Choo H, Lee A, Lee C (2011) Serotonin induces melanogenesis via serotonin receptor 2A. Br J Dermatol 165(6):1344–1348
Lee E, Lee S-Y, Kang M-J, Kim K, Won S, Kim B-J, Choi KY, Kim B-S, Cho H-J, Kim Y (2016) Clostridia in the gut and onset of atopic dermatitis via eosinophilic inflammation. Annal Allergy Asthma Immunol 117(1):91–92.e91
Lee M-J, Kang M-J, Lee S-Y, Lee E, Kim K, Won S, Suh DI, Kim KW, Sheen YH, Ahn K (2018a) Perturbations of gut microbiome genes in infants with atopic dermatitis according to feeding type. J Allergy Clin Immunol 141(4):1310–1319
Lee S-Y, Lee E, Park YM, Hong S-J (2018b) Microbiome in the gut-skin axis in atopic dermatitis. Allergy Asthma Immunol Res 10(4):354–362
Louis P, Flint HJ (2017) Formation of propionate and butyrate by the human colonic microbiota. Environ Microbiol 19(1):29–41
Ly NP, Litonjua A, Gold DR, Celedón JC (2011) Gut microbiota, probiotics, and vitamin D: interrelated exposures influencing allergy, asthma, and obesity? J Allergy Clin Immunol 127(5):1087–1094
Ma Y-Y, Li L, Yu C-H, Shen Z, Chen L-H, Li Y-M (2013) Effects of probiotics on nonalcoholic fatty liver disease: a meta-analysis. World J Gastroenterol WJG 19(40):6911
Maguire M, Maguire G (2017) The role of microbiota, and probiotics and prebiotics in skin health. Arch Dermatol Res 309(6):411–421
Maslowski KM, Vieira AT, Ng A, Kranich J, Sierro F, Yu D, Schilter HC, Rolph MS, Mackay F, Artis D (2009) Regulation of inflammatory responses by gut microbiota and chemoattractant receptor GPR43. Nature 461(7268):1282–1286
Matsumoto M, Ebata T, Hirooka J, Hosoya R, Inoue N, Itami S, Tsuji K, Yaginuma T, Muramatsu K, Nakamura A (2014) Antipruritic effects of the probiotic strain LKM512 in adults with atopic dermatitis. Annal Allergy Asthma Immunol 113(2):209–216.e207
Messaoudi M, Lalonde R, Violle N, Javelot H, Desor D, Nejdi A, Bisson J-F, Rougeot C, Pichelin M, Cazaubiel M (2011) Assessment of psychotropic-like properties of a probiotic formulation (lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in rats and human subjects. Br J Nutr 105(5):755–764
Mikó E, Vida A, Kovács T, Ujlaki G, Trencsényi G, Márton J, Sári Z, Kovács P, Boratkó A, Hujber Z (2018) Lithocholic acid, a bacterial metabolite reduces breast cancer cell proliferation and aggressiveness. Biochim Biophys Acta (BBA) Bioenergey 1859(9):958–974
Mikó E, Kovács T, Sebő É, Tóth J, Csonka T, Ujlaki G, Sipos A, Szabó J, Méhes G, Bai P (2019) Microbiome—microbial metabolome—cancer cell interactions in breast cancer—familiar, but unexplored. Cell 8(4):293
Miniello VL, Brunetti L, Tesse R, Natile M, Armenio L, Francavilla R (2010) Lactobacillus reuteri modulates cytokines production in exhaled breath condensate of children with atopic dermatitis. J Pediatr Gastroenterol Nutr 50(5):573–576
Miyamoto J, Mizukure T, Park S-B, Kishino S, Kimura I, Hirano K, Bergamo P, Rossi M, Suzuki T, Arita M (2015) A gut microbial metabolite of linoleic acid, 10-hydroxy-cis-12-octadecenoic acid, ameliorates intestinal epithelial barrier impairment partially via GPR40-MEK-ERK pathway. J Biol Chem 290(5):2902–2918
Mohan GC, Silverberg JI (2015) Association of vitiligo and alopecia areata with atopic dermatitis: a systematic review and meta-analysis. JAMA Dermatol 151(5):522–528
Murray C, Vos T, Lozano R, AlMazroa MA, Memish ZA (2014) Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the global burden of disease study 2010, vol 380. pp 2197, 2012
Nagpal R, Wang S, Ahmadi S, Hayes J, Gagliano J, Subashchandrabose S, Kitzman DW, Becton T, Read R, Yadav H (2018) Human-origin probiotic cocktail increases short-chain fatty acid production via modulation of mice and human gut microbiome. Sci Rep 8(1):1–15
Nakatsuji T, Chen TH, Narala S, Chun KA, Two AM, Yun T, Shafiq F, Kotol PF, Bouslimani A, Melnik AV (2017) Antimicrobials from human skin commensal bacteria protect against Staphylococcus aureus and are deficient in atopic dermatitis. Sci Trans Med 9(378):eaah4680
Nwanodi O (2018) Skin protective nutraceuticals: the current evidence in brief. In: Healthcare, vol 2. Multidisciplinary Digital Publishing Institute, p 40
Nylund L, Nermes M, Isolauri E, Salminen S, De Vos W, Satokari R (2015) Severity of atopic disease inversely correlates with intestinal microbiota diversity and butyrate-producing bacteria. Allergy 70(2):241–244
Oh J, Freeman AF, Park M, Sokolic R, Candotti F, Holland SM, Segre JA, Kong HH, Program NCS (2013) The altered landscape of the human skin microbiome in patients with primary immunodeficiencies. Genome Res 23(12):2103–2114
Olszak T, An D, Zeissig S, Vera MP, Richter J, Franke A, Glickman JN, Siebert R, Baron RM, Kasper DL (2012) Microbial exposure during early life has persistent effects on natural killer T cell function. Science 336(6080):489–493
Penders J, Thijs C, van den Brandt PA, Kummeling I, Snijders B, Stelma F, Adams H, van Ree R, Stobberingh EE (2007) Gut microbiota composition and development of atopic manifestations in infancy: the KOALA birth cohort study. Gut 56(5):661–667
Penders J, Gerhold K, Stobberingh EE, Thijs C, Zimmermann K, Lau S, Hamelmann E (2013) Establishment of the intestinal microbiota and its role for atopic dermatitis in early childhood. J Allergy Clin Immunol 132(3):601–607.e608
Pols TW, Puchner T, Korkmaz HI, Vos M, Soeters MR, de Vries CJ (2017) Lithocholic acid controls adaptive immune responses by inhibition of Th1 activation through the vitamin D receptor. PLoS One 12(5)
Reichardt N, Duncan SH, Young P, Belenguer A, Leitch CM, Scott KP, Flint HJ, Louis P (2014) Phylogenetic distribution of three pathways for propionate production within the human gut microbiota. ISME J 8(6):1323–1335
Ridlon JM, Kang D-J, Hylemon PB (2006) Bile salt biotransformations by human intestinal bacteria. J Lipid Res 47(2):241–259
Ruan Y, Sun J, He J, Chen F, Chen R, Chen H (2015) Effect of probiotics on glycemic control: a systematic review and meta-analysis of randomized, controlled trials. PLoS One 10(7)
Rusu E, Enache G, Cursaru R, Alexescu A, Radu R, Onila O, Cavallioti T, Rusu F, Posea M, Jinga M (2019) Prebiotics and probiotics in atopic dermatitis. Exp Ther Med 18(2):926–931
Salem I, Ramser A, Isham N, Ghannoum MA (2018) The gut microbiome as a major regulator of the gut-skin axis. Front Microbiol 9:1459
Schmitt J, Schwarz K, Baurecht H, Hotze M, Fölster-Holst R, Rodríguez E, Lee YA, Franke A, Degenhardt F, Lieb W (2016) Atopic dermatitis is associated with an increased risk for rheumatoid arthritis and inflammatory bowel disease, and a decreased risk for type 1 diabetes. J Allergy Clin Immunol 137(1):130–136
Sevelsted A, Stokholm J, Bønnelykke K, Bisgaard H (2015) Cesarean section and chronic immune disorders. Pediatrics 135(1):e92–e98
Shi B, Bangayan NJ, Curd E, Taylor PA, Gallo RL, Leung DY, Li H (2016) The skin microbiome is different in pediatric versus adult atopic dermatitis. J Allergy Clin Immunol 138(4):1233–1236
Smith PM, Howitt MR, Panikov N, Michaud M, Gallini CA, Bohlooly-Y M, Glickman JN, Garrett WS (2013) The microbial metabolites, short-chain fatty acids, regulate colonic Treg cell homeostasis. Science 341(6145):569–573
Song H, Yoo Y, Hwang J, Na Y-C, Kim HS (2016) Faecalibacterium prausnitzii subspecies–level dysbiosis in the human gut microbiome underlying atopic dermatitis. J Allergy Clin Immunol 137(3):852–860
Tatu AL, Ionescu MA, Clatici VG, Cristea VC (2016) Bacillus cereus strain isolated from Demodex folliculorum in patients with topical steroid-induced rosaceiform facial dermatitis. An Bras Dermatol 91(5):676–678
Thorburn AN, Macia L, Mackay CR (2014) Diet, metabolites, and “western-lifestyle” inflammatory diseases. Immunity 40(6):833–842
Torii S, Torii A, Itoh K, Urisu A, Terada A, Fujisawa T, Yamada K, Suzuki H, Ishida Y, Nakamura F (2011) Effects of oral administration of lactobacillus acidophilus L-92 on the symptoms and serum markers of atopic dermatitis in children. Int Arch Allergy Immunol 154(3):236–245
Uhde M, Ajamian M, Caio G, De Giorgio R, Indart A, Green PH, Verna EC, Volta U, Alaedini A (2016) Intestinal cell damage and systemic immune activation in individuals reporting sensitivity to wheat in the absence of coeliac disease. Gut 65(12):1930–1937
van Nimwegen FA, Penders J, Stobberingh EE, Postma DS, Koppelman GH, Kerkhof M, Reijmerink NE, Dompeling E, van den Brandt PA, Ferreira I (2011) Mode and place of delivery, gastrointestinal microbiota, and their influence on asthma and atopy. J Allergy Clin Immunol 128(5):948–955.e943
Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V (2012) Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the global burden of disease study 2010. Lancet 380(9859):2163–2196
Waldman AR, Ahluwalia J, Udkoff J, Borok JF, Eichenfield LF (2018) Atopic dermatitis. Pediatr Rev 39(4):180–193. https://doi.org/10.1542/pir.2016-0169
Wallach D, Taïeb A (2014) Atopic dermatitis/atopic eczema. In: Karger Publishers (ed) History of allergy, vol 100, pp 81–96
Wang IJ, Wang JY (2015) Children with atopic dermatitis show clinical improvement after lactobacillus exposure. Clin Exp Allergy 45(4):779–787
Weidinger S, Novak N (2016) Atopic dermatitis. Lancet 387(10023):1109–1122
Williams H, Stewart A, von Mutius E, Cookson W, Anderson HR, of Asthma IS (2008) Is eczema really on the increase worldwide? J Allergy Clin Immunol 121(4):947–954.e915
Woo S-I, Kim J-Y, Lee Y-J, Kim N-S, Hahn Y-S (2010) Effect of lactobacillus sakei supplementation in children with atopic eczema–dermatitis syndrome. Ann Allergy Asthma Immunol 104(4):343–348
Yokoyama S, Hiramoto K, Koyama M, Ooi K (2015) Impairment of skin barrier function via cholinergic signal transduction in a dextran sulphate sodium-induced colitis mouse model. Exp Dermatol 24(10):779–784
Zeng M, Inohara N, Nuñez G (2017) Mechanisms of inflammation-driven bacterial dysbiosis in the gut. Mucosal Immunol 10(1):18–26
Zhang A, Silverberg JI (2015) Association of atopic dermatitis with being overweight and obese: a systematic review and metaanalysis. J Am Acad Dermatol 72(4):606–616.e604
Zheng J, Feng Q, Zheng S, Xiao X (2018) The effects of probiotics supplementation on metabolic health in pregnant women: An evidence based meta-analysis. PLoS One 13(5)
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive licence to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Khanna, N., Devi, P., Kumar, A., Pawar, S.V. (2021). Probiotics for Atopic Dermatitis. In: Pawar, S.V., Rishi, P. (eds) Probiotic Research in Therapeutics. Springer, Singapore. https://doi.org/10.1007/978-981-33-6236-9_15
Download citation
DOI: https://doi.org/10.1007/978-981-33-6236-9_15
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-33-6235-2
Online ISBN: 978-981-33-6236-9
eBook Packages: Chemistry and Materials ScienceChemistry and Material Science (R0)