Abstract
Ovarian cancer (OC) is one of the most common and dreadful cancer types which has affected the female population worldwide with an increased number of cases. Broadly, OC has been categorized into two types based on its mutational changes. These are Type 1 OC which is found to show less aggressive tumors without any mutation of the tumor protein p53 gene and Type 2 OC which exhibits tumors resulting from significant mutation of the P53 gene. The major molecular pathways and cellular targets responsible for the progression of OC include VEGF, PDGF, FGF, (PI3K)/AKT pathway, PARP, and others. The conventional therapies for the management of OC include surgery, chemotherapy, hormonal therapy, radiotherapy, monoclonal antibodies, and others. However, conventional therapies are restricted due to a few limitations such as unintended toxicities, relapse of the conditions, high dose, less bioavailability, and prolonged therapeutic regimen. Thus, to overcome these limitations nanotherapeutic approaches can be used for the effective delivery of drugs with superior targetability and negligible or no toxicity. In this chapter, we have discussed the major molecular pathways and cellular targets causing ovarian cancer. Also, the significant role of nanotherapeutic approaches and targeting mechanisms of encapsulated bioactive/drugs against ovarian cancer cells is summarized.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Ovarian cancer
- Cellular responses
- Molecular pathways
- Nanotherapy
- Targeted delivery systems
- Bioavailability
5.1 Introduction
The need for advancements in therapeutics is often triggered by the severity of disease and the statistics that revolve around it. Ovarian cancer (OC) is one such dreadful disease that finds itself in the list of common cancers around the globe. As per the American Institute of Cancer Research, OC is the 18th most common cancer, while being the eighth most common for women (Ferlay et al. 2019). In 2021, an estimated 21,410 cases received the diagnosis and around 13,770 lives were expected to be claimed by OC in the USA. All of these data accompanied with a delayed and limited and complicated diagnosis calls for effective treatment of the disease, which shall not only lessen hospital stay, but also prevent the recurrence of the disease. Even though patients respond to treatments initially, about 50–75% of the cases see a relapse (Das and Bast Jr. 2008; Jacobs and Menon 2004; Sarojini et al. 2012). OC can be of two types; Type 1 and Type 2. Type 1 OC houses less aggressive tumors without any mutation of the Tumor Protein p53 gene; whereas Type 2 houses tumors resulting from significant mutation of the P53 gene (Kurman and IeM 2010). OC of Serous type associated with BRCA1, BRCA2, MMR, BARDI, etc. mutations is responsible for more than half the cases. Their area of metastasis is similar(Ducie et al. 2017).
As per FIGO Committee on Gynaecologic Oncology, OC can be classified under 4 stages based on the extent of metastasis. In stage 1, the tumor growth is confined to the ovaries. In stage 2, the tumor has spread to the pelvic region. When metastasis has occurred to the organs of the peritoneal cavity such as the liver and intestine, and lymph nodes, the cancer is in stage 3. If further metastasis occurs, then it can be classified as stage 4 (Prat 2014). Epithelial carcinoma constitutes 85–90% of the cases. Such type of OC includes endometrioid, mucinous, and a few other cell growths such as Brenner; but mostly constitutes epithelial cell growths. Epithelial cell growths have two subtypes; namely high-grade serous carcinoma (HGSC), which is quite common, and the uncommon low-grade serous carcinoma (LGSC) (Chen et al. 2014).
A rare type of OC includes Ovarian Malignant Germ Cell Tumors (OMGCTS), a condition arising from the malignancy of the primitive germ cells of the embryonic gonads. Their various types include the less malignant but more common, dysgerminoma, and the more malignant teratomas, yolk sac tumors, embryonal carcinomas, and polyembryomas. The tumor markers include alpha-fetoprotein, beta-human chorionic gonadotropin, and lactic dehydrogenase, all of which may or may not be present for a tumor type (Shaaban et al. 2014).
5.1.1 Conventional Therapies Used to Combat Ovarian Cancer
5.1.1.1 Surgery
In the early stages of OC, especially in stages 1 and 2, medical practitioners turn to surgeries such as Bilateral Salpingo-Oophorectomy (BSO), which has not only reduced the chance of recurrence, but also minimized the dependence on chemotherapy. BSO is a cytoreduction surgery done to remove small tumors (less than 1 cm diameter). To increase the efficacy of the treatment, the patient may be put through a cycle of cisplatin or paclitaxel administered intravenously every 21 days for 6 cycles. Carboplatin and/or cisplatin may also be used, albeit with some side effects like neuropathy (Wang and Fang 2021; McGuire et al. 1996; Elit et al. 2007).
5.1.1.2 Chemotherapy
Cytoreductive surgeries are usually followed by a few cycles of chemotherapy as mentioned above. However, the relapse of the disease in most cases remains a major challenge. Initially, the disease is seen to progress during platinum-based medication regime; possibly due to platinum resistance or sensitivity. In later stages of the regime, usually after 6–12 months, the condition is again seen to relapse due to resistance to platinum-based therapeutics. Anticancer agents, being low molecular weight compounds, are limited by their inability to attack specific targets; i.e., the site of cancer. Moreover, such agents are required in high doses during the treatment regime; thus, chemotoxicity also becomes a major hurdle. Their low bioavailability needs to be tackled as well (Bharadwaj et al. 2021; Pignata et al. 2011; Das et al. 2020d).
5.1.1.3 Intraperitoneal Chemotherapy
OC has been observed to not metastasize beyond the abdominal cavity. This is a type of treatment where the drug is administered into the abdomen region intraperitoneally (IP). A study conducted by Gynecologic Oncology Group (GOG), a randomized controlled trial with 876 patients, showed that the mean survival for intraperitoneal therapy was 61.8 months, while the same being only 51.4 months for conventional IV therapy. Thus, IP therapy was judged to be more effective when compared to IV therapy(Tewari et al. 2015; Becker et al. 2019; Barlin et al. 2012).
5.1.1.4 Hormone Therapy
Luteinizing Hormone Releasing Hormone (LHRH) receptor agonists like goserelin and leuprolide are administered to lower the gonadotropin secretion leading to lower estradiol level, which is highly increased in cases of OC. Vaginal bleeding, osteoporosis, and vaginal dryness are common side effects of the treatment (Katchman et al. 2017). Tamoxifen, a nonspecific estrogen receptor antagonist, is often used in the treatment of stromal OC. Its anticancer activity is due to the ability to competitively inhibit the binding of estrogen to its receptor leading to a reduction in freely circulating estradiol. Tamoxifen reduces tumor growth factor α. Hot flushes and vaginal dryness are some of the major limitations of this treatment (Katchman et al. 2017). Apart from this, various aromatase inhibitors such as anastrozole, exemestane, letrozole, etc. exhibit potential effects in inhibiting the binding of Oestrogen to the growth hormone receptors of tumors. It acts by competitive inhibition of aromatase enzyme, which is responsible for conversion of androgens into estrogen, primarily in women after menopause. This treatment also has its fair share of side effects like osteoporosis and hot flushes among others (Katchman et al. 2017; Kok et al. 2019).
5.1.1.5 Radiation Therapy
This therapy involves the use of powerful electromagnetic waves like X-rays to treat malignancy. The radiation can be administered either externally; i.e., outside the body; or internally, also known as brachytherapy. In external beam radiation therapy, a linear accelerator machine emits x-ray or photon beams in a controlled manner to attack the malignant areas, while leaving the healthy cells unharmed. External beam radiation therapy can be of various types like Intensity-modulated radiation therapy (IMRT), Proton beam therapy, Image-guided radiation therapy (IGRT), and Stereotactic Radiation Therapy (SRT). Internal radiation therapy or brachytherapy, on the other hand, employs a radioactive material to target the tumor. This material is delivered using capsules, catheters, needles, or other special kinds of applicators. The therapy is permanent if the capsule or any other such delivery system containing the radioactive therapeutic agent is implanted in the affected tissues. The therapy is temporary if the fluidized form of the radioactive therapeutic agent is delivered using needles or catheters. Apart from this, some other specific types of radiation therapy are also used to mitigate OC.
5.1.1.5.1 Intraoperative Radiation Therapy
When vital organs are close to the tumors, surgeons make use of this therapy to deliver the radiation. This therapeutic procedure is carried out during surgical operation, where any effect due to the radiation on healthy tissues can be subsided by making way for the radiation to directly reach the affected area.
5.1.1.5.2 Systemic Radiation Therapy
For this therapy, the patient has to swallow a pill containing a radioactive therapeutic agent that is supposed to target the tumor tissues. The radioactive material gets excreted from the body through feces, urine, and sweat. (Rai et al. 2014).
5.1.1.5.3 Radioimmunotherapy
This type of therapy employs monoclonal antibodies that identify specific markers surrounding tumor tissues. IgG1 antibody, Ibritumomab, is one such therapeutic agent that has found itself useful in cases of lymphomas. It is administered in a combination with a tiuxetan, a chelator that carries a radioactive isotope like yttrium or indium. This system binds to a CD20 antigen present on malignant and normal B cells at tumor sites. The therapeutic activity occurs through two mechanisms; one, through irradiation of the tumor tissue by the beta waves emitted by the radioactive isotopes; and second, through the attachment of the antibody to the antigen to bring about antibody-dependent cell-mediated cytotoxicity. (Song and Sgouros 2011).
5.1.1.6 Monoclonal Antibodies
Following various targets present on tumor tissues and those exhibited during the physiological process of tumor progression, many monoclonal antibodies have paved the way for the effective treatment of OC. A trifunctional antibody molecule currently in Phase 2 of clinical trials, called Catumaxomab, works by targeting Epithelial Cell Adhesion Molecule (EpCAM) on cancer sites and CD3 on T cells. In doing so, it allows macrophages, dendritic cells, natural killer cells, and T cells to make their way to the cancer site that would result in tumor cell death (Das et al. 2020a). This treatment is aimed to be effective in patients who face a recurrence of cancer or in cases where their condition has become resistant to conventional platinum-based chemotherapy. This can be attributed to EpCAM-positive OC cells, which remain viable even after conventional chemotherapy (Tayama et al. 2017). CD25 is another lucrative which targets cancer for immunosuppressant monoclonal antibody in treating serous ovarian; a candidate for which is Daclizumab that suppresses T cell population; although the binding seems to be nonspecific (Santoiemma and Powell Jr. 2015).
5.2 Molecular Targets and Cellular Pathways Associated with Ovarian Cancer
Various molecular targets and pathways have been associated directly or indirectly with ovarian tumors leading to cancer. Some of the major targets have been discussed below.
5.2.1 Vascular Endothelial Growth Factor (VEGF), Platelet-Derived Growth Factor (PDGF), Fibroblast Growth Factor (FGF)
Several factors contribute to the progression of the tumor. Some of the prominent factors include VEGF, PDGF, and FGF. Anti-VEGF agents result in inhibition of angiogenesis at tumor sites by either blocking the receptor-mediated pathways of neutralization of VEGF. Bevacizumab is a monoclonal antibody formulation that inhibits angiogenesis by binding to VEGF and prevents it from binding to the receptor. Although some side effects like cardiotoxicity, hypertension, and dermatological conditions have been associated with the treatment, Bevacizumab has become a preferred addition to the conventional therapeutic regimen (Burger 2011; Amini et al. 2012). A few targeted therapeutic products that are either under clinical trial or approved are mentioned in Table 5.1.
5.2.2 (PI3K)/AKT Pathway
A signaling pathway that has a major contribution towards cancerous cell growth is the phosphatidylinositol-3-kinase (PI3K)/AKT pathway. A protein kinase in this pathway is the mTOR protein that is encoded by the mTOR gene. Immunosuppressant cytokine inhibitor drugs like Sirolimus and Everolimus target mTOR protein and inhibit cell proliferation (Das et al. 2020b).
5.2.3 Poly (ADP-Ribose) Polymerase (PARP)
Another lucrative target for beating OC is the enzyme Poly (ADP-ribose) Polymerase (PARP). This enzyme is responsible for DNA repair; in both normal and cancerous cells. PARP detects single-strand breakage on DNA and binds to it and initiates repair by synthesizing poly-ADP ribose. This acts as a trigger for other DNA repairing enzymes like DNA Ligases. Programmed cell death is also regulated by this enzyme. PARP enzyme (PARP 1, PARP 2, etc.) inhibitors like Olaparib, Rucaparib, and Niraparib have been approved for the treatment of OC (AstraZeneca 2021; Barkat et al. 2021).
5.3 Novel Drug Delivery Systems for Treatment of Ovarian Cancer
Conventional cancer therapies come with several limitations; especially unintended toxicities, relapse of the conditions, high dose, less bioavailability, and prolonged therapeutic regimen. This not only makes the treatment inaccessible to the common public, but also increases the chance of propagation of the disease to the next generation. Thus, there is a need for innovation that makes the treatment not only economic, but also effective. Various drug delivery systems based on passive and active mechanisms, aimed to improve the Spatio-temporal response of the therapeutic system, are being continuously developed.
5.3.1 Passive Drug Delivery Systems
Sound knowledge of the physiology of the cancerous tissues helps in designing a drug delivery system that can take advantage of the existing conditions to make the therapeutic agent reach the desired location of action in appropriate amounts. The regions of cancer are characterized by irregular and uncontrolled growth of fenestrated blood vessels that result in the proliferation of the cancerous tissues by a supply of nutrients; while also resulting in hypoxia at that region (Danhier et al. 2010). There are also few angiogenic regulators present at the site that cause the endothelium to become “leaky”. Matrix metalloproteinases are one such regulator whose inhibition (e.g., MMP inhibitor like Doxycycline) can form a treatment method. Moreover, the poor drainage of the lymphatic system makes the drug delivery systems like nanocarriers carrying the therapeutic moiety leak out of the fenestrated vasculatures and reach the target cancer tissue; while also staying in circulation for a longer time. This mechanism is termed enhanced permeation and retention effect and is widely employed for targeted therapy (Torchilin 2006).
The process by which passive targeting occurs is diffusion while escaping the reticuloendothelial system (RES). For diffusion to occur effectively, the nanocarriers need to have certain characteristics to remain circulating. Few of the desired characteristics include a particle size between 10 and 100 nm, a mostly hydrophilic composition, and a neutrally charged surface. Few materials that are widely used to develop nanoparticles (NPs) are poly-(vinyl alcohol) and poly-(ethylene glycol). Being immunologically inactive, PEG has been employed widely in varying molecular weights by altering PEG chain length (Tirelli et al. 2002).
Some passive drug delivery systems have exploited the potential of decorating the surface of nanocarriers with a copolymer block made using both hydrophilic and hydrophobic polymers. Hydrophilic polymers like PEG conjugated with hydrophobic polymers like Polyoxypropylene (PPO) form a PEG/PPO block copolymer. The PPO chains are bound to the nanocarrier by hydrophobic interaction and the PEG chains face the surrounding hydrophilic medium providing steric stability. The stability of the therapeutic system is an important consideration for sufficient circulation time in the body for an optimum therapeutic effect (Illum et al. 1987). A Phase 2 trial of combination therapy of carboplatin and pegylated liposomal doxorubicin yielded satisfactory results and the treatment was deemed feasible for gynaecologic sarcomas (Harter et al. 2016).
5.3.2 Active Drug Delivery System
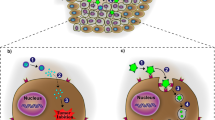
The guiding principle behind designing site-specific targeting drug delivery systems is being able to recognize the receptors on the cancerous cells’ membranes. To target these receptors, various ligands, including new generation monoclonal antibodies, can be attached to the nanocarrier. The nanocarriers after getting attached to the cells utilize uptake mechanisms like phagocytosis and endocytosis (Das et al. 2020c; Barkat et al. 2020). Nanoparticulate systems to which PEG is to be attached can be done so by attaching the PEG to polymers like poly-α-hydroxy acids (PLAs) or polylactic-co-glycolic acid (PLGA) copolymers (Milane et al. 2011). A lipidic nanocarrier like that made of distearylphosphatidylethanolamine (DSPE) can be also decorated with PEG, non-covalently; as with the case of adamantane inserted into a cyclodextrin system (Bartlett and Davis 2007; Chenjie et al. 2009). To stabilize a liposomal system, formulators often use PEG of molecular weight 2000 dalton or more. This affords a thermodynamically stable system (Garbuzenko et al. 2005).
PEG chains attached to liposomes have to be attached to a functional group like carbonyl, amide, or sulfhydryl; which can serve as active points (thus forming a bridge) where a therapeutic agent can be attached (van Vlerken et al. 2007). The attachment can take place in the presence of a linking or coupling agent like N, N’- dicyclohexylcarbodiimide or cyanuric chloride, which acts as a catalyst (Cirstoiu-Hapca et al. 2010). One of the major disadvantages of the above technique is the remains of unreacted end groups of PEG chains, those that have not been associated with any functional groups. This can lead to unsuitable interactions of the liposome with the surrounding system; while also providing hindrances to conjugation of the therapeutic moiety or other ligands to the system (Zalipsky et al. 1997). A strategy to overcome this barrier has been to form a conjugated system consisting of Lipid-PEG-Ligand and make them attach to a preformulated nontargeting liposome. This not only positions the conjugated system outside the liposomal bilayer unlike the previous strategy where the conjugate would be trapped inside the liposome, but also allows a great deal of flexibility in designing an effective drug delivery system that has highly specific actions. Commonly used linkages include peptides, transferrin, and folate moieties (Uster et al. 1996).
These actively targeting drug delivery systems mainly target various receptors, biomarkers, and some biochemicals like proteins that are expressed during tumor proliferation for delivery of the therapeutic moiety. The Follicle Stimulating Hormone or FSH is known to activate FSH Receptor (FSHR) on the ovarian epithelium. This receptor is overexpressed in OC cells which can be targeted by the drug delivery systems (Zhang et al. 2009a). Paclitaxel-loaded NPs conjugated with a peptide derived from FSH have been developed (Zhang et al. 2009b). A tumor in its course of proliferation releases various proteins or antigens that get reflected during the evaluation of the serum of the patient. One such antigen is CA-125. This gets expressed in more than 80% of the cases of OC; which makes it an ideal target for designing therapeutic agents (Bast Jr et al. 1981; Moore and Maclaughlan 2010).
HER-2 is another receptor that is overexpressed in OC that leads to tumor proliferation and various pathways attached to it. A monoclonal antibody approved by FDA and EMA that is currently being used is Trastuzumab in the treatment of HER2-positive breast cancer, but has not proven itself effective in the treatment of epithelial OC (Wilken et al. 2010). Another biomarker expressed during cancer angiogenesis is nucleolin, which is a 31-amino acid F3 peptide. This F3 peptide is synthesized from the protein High Mobility Group (HMG) 2. F3 can bind to nucleolin protein expressed at tumor sites. Thus, it was considered as a targeting moiety; the same has been demonstrated in a study conducted by designing PEG-ylated liposomes functionalized with nucleolin targeting F3 peptide and loaded with Doxorubicin and C6-Ceramide synergistic combination and results show to be effective in generating cytotoxicity towards cancerous ovarian cells (Cruz et al. 2021).
Angiogenesis is also known to be regulated by integrins. Thus, a certain combination of amino acids sequence results in a peptide such as RGD (Arginine-Glycine-Aspartic acid) that can bind to integrin molecules (Janssen et al. 2002). The Transferrin Receptor (Tfr) is overexpressed in OC and is known to be stimulated by certain antibodies and transferrin. Thus, a drug delivery system associated with transferrin and loaded with a monoclonal antibody like R17217 and OX26 (Ulbrich et al. 2009; Béduneau et al. 2007) or Docetaxel-loaded liposomal drug delivery system modified with transferrin can target the OC sites (Yuan et al. 2014).
5.3.3 Materials for Fabrication of Nanoparticulate Drug Delivery Systems
While fabricating a nano delivery system, the materials used are particularly important for compatibility with the therapeutic agent, toxicity and biodegradability, and any adverse effects. Factors governing the feasibility of scaling up the product to the industrial level are also taken into consideration. The ultimate goal shall be to design an effective drug delivery system that possesses enhanced permeation and retention effect (EPR), an optimal dissolution profile, and a good Spatio-temporal response that delivers the drug at the particular cancerous site without causing any harm to the surrounding healthy cells.
5.3.3.1 Biodegradable Polymers Used in the Fabrication of Nanoparticles
Biodegradable polymers are preferred materials for the fabrication of NPs. They are made up of naturally occurring polymers containing amide, ester, and ether functional groups which can be broken down by the biological mechanisms in the body without the generation of toxic residues (Sivasankarapillai et al. 2021). A few examples are mentioned in Table 5.2.
5.3.4 Nanocarriers for Targeted Drug Delivery in Ovarian Cancer Therapy
Various types of nanocarriers, including metallic NPs, polymeric NPs, liposomes, solid-lipid NPs, micelles, and others, have been reported for effective management of OC. These nanocarriers due to their versatile size, shape, and surface charge assist the targeted delivery of loaded drugs/bioactive to the targeted diseases to the site rather than affecting the healthy cells or tissues, thus reducing the chances of systemic toxicity.
5.3.4.1 Nanoparticles
Various metallic elements like gold, silver, and metallic oxides, especially Iron oxide NPs, have been explored to fabricate NPs (Horák et al. 2017). Iron oxide NPs have been shown to exhibit significant cytotoxic effects. The in vitro study performed on OC cell lines found an increased level of ROS, resulting in damaging the mitochondrial membrane of cancer cells. This resulted in the caspase-mediated apoptosis in the OC PA-1 cells (Ramalingam et al. 2020). The success of such systems is attributed to the superparamagnetic characteristic of iron oxide that renders enhanced Spatio-temporal control over drug delivery (Zhi et al. 2020).
Chitosan is another biopolymer that due to its low toxicity and biocompatibility characteristics has found its way to the fabrication of NPs. Several amine and hydroxyl groups in their structure mean that they can be effective sites of associations with therapeutic moieties (Muddineti et al. 2017). NPs fabricated using chitosan and conjugated with proteins, drugs, and nucleic acids have exhibited enhanced localization at cancerous sites and taken up by cells through endocytosis among other internalization phenomena. In a bid to explore the possibility of employing biodegradable photoresponsive NPs in the treatment of OC, chitosan and PLGA-based NPs were designed and loaded with carboplatin (CP) and the near-infrared (NIR) photosensitizer indocyanine green (ICG). The study found effective cytotoxic effects against OC cell lines when the target cells were irradiated with 800 nm laser (Sánchez-Ramírez et al. 2020).
Another nanoparticulate drug delivery system fabricated from PLGA and loaded with Cannabidiol (CBD) has been shown to significantly induce apoptosis by inducing the expression PARP. The drug-loaded nanoparticle was found to have a high encapsulation efficiency of 95% and a drug release lasting about 96 h. The internalization of the NPs into the OC cell line was found to be between 2 and 4 h. Although CBD-NPs showed a tumor growth inhibition similar to CBD in solution, the IC50 value of CBD-NPs was found to be significantly lower than that of CBD solution (Fraguas-Sánchez et al. 2020).
5.3.4.2 Liposomes
Liposomes are nanoparticulate drug delivery systems in the size range of 2 to 400 nm. They are composed of lipid materials that are easily biodegradable and generally nontoxic to the patient’s body. Liposomes show high encapsulation efficiency for both hydrophilic and lipophilic pharmaceuticals while also showing Spatio-temporal control. The circulation time of liposomes is of prime importance when it comes to their efficacy. PEG-ylation is a well-explored technique to do the same. A study with PEG-ylated liposomal loaded with paclitaxel observed that the liposomal drug delivery system was able to contain the growth of OC cells both in vitro and in vivo by inducing their apoptosis by TNF-mediated ERK/AKT signaling (Alizadeh et al. 2020).
In a study involving cisplatin-resistant OC cells, Cisplatin-loaded liposomal particles functionalized to target transferrin receptors were designed. Their cell uptake in both resistant and nonresistant cells was found to be similar, but significantly better than that of free cisplatin. Cytotoxicity was related to the accumulation of platinum in both resistant and nonresistant cancer cells when treated with targeting liposomes. However, Tfr targeting was not found to have any significant advantage over nontargeting liposomes (İnce et al. 2020).
Often the idea of co-encapsulating two or more drugs in the liposome gains research attractions for their ability to synergistically act on the cancerous cells. Such a system was designed by encapsulating a topoisomerase inhibitor, Irinotecan, and a DNA transcription inhibitor through various mechanisms, Doxorubicin (in the ratio 1:1 in circulation), by the process of coordination complexation and pH gradient. The encapsulation efficiency was found to be more than 80%. This liposomal formulation was delivered in a xenograft model intraperitoneally growing a human ovarian tumor and found to have effective therapeutic potentiality (Qi et al. 2018).
5.3.4.3 Nanomicelles
Micelles are formed as self-aggregating amphiphilic structures in an aqueous medium above a certain concentration called the critical micellar concentration. Like liposomes, Nanomicelles can also be loaded with hydrophilic and hydrophobic pharmaceuticals. Nanomicelles have been shown to exhibit higher drug loading capacity than other drug delivery systems (Krieger et al. 2010; Shaikh et al. 2013). Small size and effective penetrability and endocytosis at OC sites, accompanied by their unique characteristics like in vivo stability, biocompatibility, long plasma circulation time, and site-specific action, have made them a quite sought-after candidate for OC therapeutics (Yu et al. 2018; Fathi et al. 2018).
In a study, Paclitaxel-loaded redox-sensitive nanomicelles were designed to target OC cells. Cytotoxicity studies revealed the therapeutic potential of the system (Pantshwa et al. 2020).
Similar effective cytotoxic effects were observed for a nanomicellar system loaded with Docetaxel and functionalized to target folate receptors on OC sites (Feng et al. 2014). A nanomicellar drug delivery system designed to incorporate two synergistically acting drugs has shown promising results. The study fabricated the nanomicelles from an amphiphilic copolymer, phenylboronic acid-coated methoxy poly (ethylene glycol)- block-poly-((N-2-hydroxyethyl)-aspartamide). The stability of the system was attributed to an electron donor-acceptor mechanism between the polymer particles and the encapsulated drugs doxorubicin and irinotecan. The nanomicelles were found to be biocompatible, while also affording significant cytotoxicity by the production of ROS. Apart from this, various functionalized nanocarriers have been listed in Table 5.3.
5.4 Conclusion and Future Perspectives
In western countries, OC has been reported as the second most common and the most fatal gynaecologic malice. Till now, there is a deficiency of approaches suggested for screening and early diagnosis of the disease, and if left untreated then at the final-stage OC is incurable in most of the clinical cases. In respect of treatment approaches, several conventional therapies, surgical technologies, and modern therapeutic regimes, entering the preclinical/clinical stages, have led to hope for the effective treatment of OC. In recent times, researchers have been able to develop potential nanocarriers for the establishment of targeted drug delivery systems to transport therapeutic regimens into ovarian carcinogenic cells with more precision. In this review, we have highlighted the outcomes and major findings of the recent articles and clinical trials associated with OC therapy and also have highlighted the significant impact of NPs-based drug delivery systems in OC therapeutics.
Studies have shown that as compared to other routes of administration, the intraperitoneal might be more beneficial for effectively targeting the folate-receptor in OC in vivo. Moreover, the amalgamation of intraperitoneal administration and targeting of the functionalized (peptides, antibodies, and aptamers)-NPs to the tumor-specific proteins might lead to decreased systemic toxicities and also increase the drug payload within the tumors. Apart from this, certain nanomaterial-mediated biosensors, due to superior sensitivity and selectivity, have exhibited a potential role in OC diagnosis. In the future, it is very important to explore the diverse aspects of NPs-based technologies and study their effects in improved tumor targeting, drug efficiency, and toxicity profiles.
References
Alizadeh L, Alizadeh E, Zarebkohan A, Ahmadi E, Rahmati-Yamchi M, Salehi R (2020) AS1411 aptamer-functionalized chitosan-silica nanoparticles for targeted delivery of epigallocatechin gallate to the Skov-3 ovarian cancer cell lines. J Nanopart Res 22(1):9123. https://doi.org/10.1007/s11051-019-4735-7
Amini A, Masoumi Moghaddam S, Morris DL, Pourgholami MH (2012) Utility of vascular endothelial growth factor inhibitors in the treatment of ovarian cancer: from concept to application. J Oncol 2012:540791. https://doi.org/10.1155/2012/540791
Astete CE, Sabliov CM (2006) Synthesis and characterization of PLGA nanoparticles. J Biomater Sci Polym Ed 17(3):247–289. https://doi.org/10.1163/156856206775997322
AstraZeneca (2016, December-2021, January) Olaparib tablets as a treatment for ovarian cancer subjects with different hrd tumor status. Identifier NCT02983799. https://clinicaltrials.gov/ct2/show/NCT02983799?term=olaparib &recrs=e&cond=Ovarian+Cancer&draw=2&rank=5. Accessed on 14 Jan, 2022
Babu A, Wang Q, Muralidharan R, Shanker M, Munshi A, Ramesh R (2014) Chitosan coated polylactic acid nanoparticle-mediated combinatorial delivery of cisplatin and siRNA/plasmid DNA chemosensitizes cisplatin-resistant human ovarian cancer cells. Mol Pharm [Internet] 11(8):2720–2733. https://doi.org/10.1021/mp500259e. Accessed on 28, Nov, 2021
Barkat HA, Barkat MA, Taleuzzaman M, Das SS, Rizwanullah M, Hadi HA (2021) Receptor-based combinatorial nanomedicines: a new Hope for cancer management. In: Kumar S, Rizvi MA, Verma S (eds) Handbook of research on advancements in cancer therapeutics. IGI Global, pp 339–355. https://doi.org/10.4018/978-1-7998-6530-8.ch011
Barkat HA, Das SS, Barkat MA, Beg S, Hadi HA (2020) Selective targeting of cancer signaling pathways with nanomedicines: challenges and progress. Future Oncol 16(35):2959–2979. https://doi.org/10.2217/fon-2020-0198
Barlin JN, Dao F, Bou Zgheib N, Ferguson SE, Sabbatini PJ, Hensley ML, Bell-McGuinn KM, Konner J, Tew WP, Aghajanian C, Chi DS (2012) Progression-free and overall survival of a modified outpatient regimen of primary intravenous/intraperitoneal paclitaxel and intraperitoneal cisplatin in ovarian, fallopian tube, and primary peritoneal cancer. Gynecol Oncol 125(3):621–624. https://doi.org/10.1016/j.ygyno.2012.03.027
Bartlett DW, Davis ME (2007) Physicochemical and biological characterization of targeted, nucleic acid-containing nanoparticles. Bioconjug Chem 18(2):456–468. https://doi.org/10.1021/bc0603539
Bast RC Jr, Feeney M, Lazarus H, Nadler LM, Colvin RB, Knapp RC (1981) Reactivity of a monoclonal antibody with human ovarian carcinoma. J Clin Invest 68(5):1331–1337. https://doi.org/10.1172/jci110380
Becker DA, Leath CA 3rd, Walters-Haygood CL, Smith BQ, Bevis KS (2019) Utilization of an alternative docetaxel-based intraperitoneal chemotherapy regimen in patients with ovarian, fallopian tube or primary peritoneal carcinoma: a continued need for ovarian cancer patients. Am J Clin Oncol 42(1):12–16. https://doi.org/10.1097/COC.0000000000000468
Béduneau A, Saulnier P, Hindré F, Clavreul A, Leroux JC, Benoit JP (2007) Design of targeted lipid nanocapsules by conjugation of whole antibodies and antibody Fab’ fragments. Biomaterials 28(33):4978–4990. https://doi.org/10.1016/j.biomaterials.2007.05.014
Bharadwaj P, Das SS, Beg S, Rahman M (2021) Formulation and biological stability of nanomedicines in cancer treatment. In: Beg S, Choudhry H, Ahmad FJ, Rahman M, Souto EB (eds) Nanoformulation strategies for cancer treatment-micro and Nano Technologies. Elsevier, pp 277–289. https://doi.org/10.1016/C2019-0-01815-8
Burger RA (2011) Overview of anti-angiogenic agents in development for ovarian cancer. Gynecol Oncol 121(1):230–238. https://doi.org/10.1016/j.ygyno.2010.11.035
Cai L, Xu G, Shi C, Guo D, Wang X, Luo J (2015) Telodendrimer nanocarrier for co-delivery of paclitaxel and cisplatin: a synergistic combination nanotherapy for ovarian cancer treatment. Biomaterials 37:456–468. https://doi.org/10.1016/j.biomaterials.2014.10.044
Chan JK, Brady W, Monk BJ, Brown J, Shahin MS, Rose PG, Kim JH, Secord AA, Walker JL, Gershenson DM (2018) A phase II evaluation of sunitinib in the treatment of persistent or recurrent clear cell ovarian carcinoma: an NRG oncology/Gynecologic oncology group study (GOG-254). Gynecol Oncol 150(2):247–252. https://doi.org/10.1016/j.ygyno.2018.05.029
Chen M, Jin Y, Bi Y, Yin J, Wang Y, Pan L (2014) A survival analysis comparing women with ovarian low-grade serous carcinoma to those with high-grade histology. Onco Targets Ther 7:1891–1899. https://doi.org/10.2147/OTT.S67812
Chenjie X, Yuan Z, Kohler N, Kim J, Chung MA, Sun S (2009) J Am Chem Soc 131(42):15346–15351. https://doi.org/10.1021/ja905938a
Cirstoiu-Hapca A, Buchegger F, Lange N, Bossy L, Gurny R, Delie F (2010) Benefit of anti-HER2-coated paclitaxel-loaded immuno-nanoparticles in the treatment of disseminated ovarian cancer: therapeutic efficacy and biodistribution in mice. J Control Release 144(3):324–331. https://doi.org/10.1016/j.jconrel.2010.02.026
Cruz AF, Caleiras MB, Fonseca NA, Gonçalves N, Mendes VM, Sampaio SF, Moura V, Melo JB, Almeida RD, Manadas B, Simões S, Moreira JN (2021) The enhanced efficacy of intracellular delivery of doxorubicin/C6-ceramide combination mediated by the F3 peptide/Nucleolin system is supported by the downregulation of the PI3K/Akt pathway. Cancers 13(12):3052. https://doi.org/10.3390/cancers13123052
Cruz A, Mota P, Ramos C, Pires RF, Mendes C, Silva JP, Nunes SC, Bonifácio VDB, Serpa J (2020) Polyurea dendrimer folate-targeted Nanodelivery of l-Buthionine sulfoximine as a tool to tackle ovarian cancer Chemoresistance. Antioxidants (Basel) 9(2):133. https://doi.org/10.3390/antiox9020133
Danhier F, Feron O, Préat V (2010) To exploit the tumor microenvironment: passive and active tumor targeting of nanocarriers for anti-cancer drug delivery. J Control Release 148(2):135–146. https://doi.org/10.1016/j.jconrel.2010.08.027
Das SS, Alkahtani S, Bharadwaj P, Ansari MT, ALKahtani MDF, Pang Z, Hasnain MS, Nayak AK, Aminabhavi TM (2020b) Molecular insights and novel approaches for targeting tumor metastasis. Int J Pharm 30(585):119556. https://doi.org/10.1016/j.ijpharm.2020.119556
Das PM, Bast RC Jr (2008) Early detection of ovarian cancer. Biomark Med 2(3):291–303. https://doi.org/10.2217/17520363.2.3.291
Das SS, Bharadwaj P, Bilal M, Barani M, Rahdar A, Taboada P, Bungau S, Kyzas GZ (2020c) Stimuli-responsive polymeric Nanocarriers for drug delivery, imaging, and Theragnosis. Polymers (Basel) 12(6):1397. https://doi.org/10.3390/polym12061397
Das SS, Hussain A, Verma PRP, Imam SS, Altamimi MA, Alshehri S, Singh SK (2020d) Recent advances in liposomal drug delivery system of quercetin for cancer targeting: a mechanistic approach. Curr Drug Deliv 17(10):845–860. https://doi.org/10.2174/1567201817666200415112657
Das SS, Verma PRP, Kar S, Singh SK (2020a) Quercetin-loaded nanomedicine as oncotherapy. In: Rahman M, Beg S, Kumar V, Ahmad FJ (eds) Nanomedicine for bioactives: healthcare applications, 1st edn. Springer, Singapore, pp 155–183. https://doi.org/10.1007/978-981-15-1664-1_5
Desale SS, Soni KS, Romanova S, Cohen SM, Bronich TK (2015) Targeted delivery of platinum-taxane combination therapy in ovarian cancer. J Control Release 220(Pt B):651–659. https://doi.org/10.1016/j.jconrel.2015.09.007
Drugs@FDA: FDA-Approved Drugs (n.d.-a) US-FDA https://www.accessdata.fda.gov/scripts/cder/daf/index.cfm?event=overviewprocess&ApplNo=125418. Accessed on 14 Jan, 2022
Drugs@FDA: FDA-Approved Drugs (n.d.-b) US-FDA https://www.accessdata.fda.gov/drugsatfda_docs/label/2005/021923lbl.pdf. Accessed on 14 Jan, 2022
Drugs@FDA: FDA-Approved Drugs (n.d.-c) US-FDA https://www.accessdata.fda.gov/scripts/cder/daf/index.cfm?event=BasicSearch. process. Accessed on 14 Jan, 2022
Ducie J, Dao F, Considine M, Olvera N, Shaw PA, Kurman RJ, Shih IM, Soslow RA, Cope L, Levine DA (2017) Molecular analysis of high-grade serous ovarian carcinoma with and without associated serous tubal intra-epithelial carcinoma. Nat Commun 8(1):990. https://doi.org/10.1038/s41467-017-01217-9
Elit L, Oliver TK, Covens A, Kwon J, Fung MF, Hirte HW, Oza AM (2007) Intraperitoneal chemotherapy in the first-line treatment of women with stage III epithelial ovarian cancer: a systematic review with metaanalyses. Cancer 109(4):692–702. https://doi.org/10.1002/cncr.22466
Fathi M, Majidi S, Zangabad PS, Barar J, Erfan-Niya H, Omidi Y (2018) Chitosan-based multifunctional nanomedicines and theranostics for targeted therapy of cancer. Med Res Rev 38(6):2110–2136. https://doi.org/10.1002/med.21506
FDA approves ramucirumab plus erlotinib for first-line metastatic NSCLC (n.d.) US-FDA https://www.fda.gov/drugs/resources-information-approved-drugs/fda-approves-ramucirumab-plus-erlotinib-first-line-metastatic-nsclc. Accessed on 14 Jan, 2022
Feng ST, Li J, Luo Y, Yin T, Cai H, Wang Y, Dong Z, Shuai X, Li ZP (2014) pH-sensitive nanomicelles for controlled and efficient drug delivery to human colorectal carcinoma LoVo cells. PLoS One 9(6):e100732. https://doi.org/10.1371/journal.pone.0100732
Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Piñeros M, Znaor A, Bray F (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144(8):1941–1953. https://doi.org/10.1002/ijc.31937
Fraguas-Sánchez AI, Torres-Suárez AI, Cohen M, Delie F, Bastida-Ruiz D, Yart L, Martin-Sabroso C, Fernández-Carballido A (2020) PLGA nanoparticles for the intraperitoneal administration of CBD in the treatment of ovarian cancer: in vitro and in Ovo assessment. Pharmaceutics [Internet] MDPI AG 12(5):439. https://doi.org/10.3390/pharmaceutics12050439
Garbuzenko O, Barenholz Y, Priev A (2005) Effect of grafted PEG on liposome size and on compressibility and packing of lipid bilayer. Chem Phys Lipids 135(2):117–129. https://doi.org/10.1016/j.chemphyslip.2005.02.003
Han S, Dwivedi P, Mangrio FA, Dwivedi M, Khatik R, Cohn DE, Si T, Xu RX (2019) Sustained release paclitaxel-loaded core-shell-structured solid lipid microparticles for intraperitoneal chemotherapy of ovarian cancer. Artif Cells Nanomed Biotechnol 47(1):957–967. https://doi.org/10.1080/21691401.2019.1576705
Harter P, Sehouli J, Reuss A, Baumann K, Hanker L, Kimmig R, Schröder W, Burges A, Gropp-Meier M, Kurzeder C, Mahner S, Canzler U, Lück HJ, Meier W, Fehm T, du Bois A (2016) Phase II study evaluating PegLiposomal doxorubicin and carboplatin combination chemotherapy in Gynecologic sarcomas and mixed epithelial-mesenchymal Tumors a phase II protocol of the Arbeitsgemeinschaft Gynaekologische Onkologie study group (AGO-GYN 7). Int J Gynecol Cancer 26(9):1636–1641. https://doi.org/10.1097/IGC.0000000000000831
Horák D, Pustovyy VI, Babinskyi AV, Palyvoda OM, Chekhun VF, Todor IN, Kuzmenko OI (2017) Enhanced antitumor activity of surface-modified iron oxide nanoparticles and an α-tocopherol derivative in a rat model of mammary gland carcinosarcoma. Int J Nanomedicine 12:4257–4268. https://doi.org/10.2147/IJN.S137574
Illum L, Davis SS, Müller RH, Mak E, West P (1987) The organ distribution and circulation time of intravenously injected colloidal carriers sterically stabilized with a block copolymer–poloxamine 908. Life Sci 40(4):367–374. https://doi.org/10.1016/0024-3205(87)90138-x
İnce İ, Yıldırım Y, Güler G, Medine Eİ, Ballıca G, Kuşdemir BC et al (2020) Synthesis and characterization of folic acid-chitosan nanoparticles loaded with thymoquinone to target ovarian cancer cells. J Radioanal Nucl Chem 324(1):71–85. https://doi.org/10.1007/s10967-020-07058-z
Jacobs IJ, Menon U (2004) Progress and challenges in screening for early detection of ovarian cancer. Mol Cell Proteomics 3(4):355–366. https://doi.org/10.1074/mcp.R400006-MCP200
Janssen M, Oyen WJ, Massuger LF, Frielink C, Dijkgraaf I, Edwards DS, Radjopadhye M, Corstens FH, Boerman OC (2002) Comparison of a monomeric and dimeric radiolabeled RGD-peptide for tumor targeting. Cancer Biother Radiopharm 17(6):641–646. https://doi.org/10.1089/108497802320970244
Kasper B, Hohenberger P (2011) Pazopanib: a promising new agent in the treatment of soft tissue sarcomas. Future Oncol 7(12):1373–1383. https://doi.org/10.2217/fon.11.116
Katchman BA, Chowell D, Wallstrom G, Vitonis AF, LaBaer J, Cramer DW, Anderson KS (2017) Autoantibody biomarkers for the detection of serous ovarian cancer. Gynecol Oncol 146(1):129–136. https://doi.org/10.1016/j.ygyno.2017.04.005
Kirkpatrick GJ, Plumb JA, Sutcliffe OB, Flint DJ, Wheate NJ (2011) Evaluation of anionic half generation 3.5-6.5 poly(amidoamine) dendrimers as delivery vehicles for the active component of the anticancer drug cisplatin. J Inorg Biochem 105(9):1115–1122. https://doi.org/10.1016/j.jinorgbio.2011.05.017
Kok PS, Beale P, O'Connell RL, Grant P, Bonaventura T, Scurry J, Antill Y, Goh J, Sjoquist K, De Fazio A, Mapagu C, Amant F, Friedlander M (2019) PARAGON investigators. PARAGON (ANZGOG-0903): a phase 2 study of anastrozole in asymptomatic patients with estrogen and progesterone receptor-positive recurrent ovarian cancer and CA125 progression. J Gynecol Oncol 30(5):e86. https://doi.org/10.3802/jgo.2019.30.e86
Krieger ML, Eckstein N, Schneider V, Koch M, Royer HD, Jaehde U, Bendas G (2010) Overcoming cisplatin resistance of ovarian cancer cells by targeted liposomes in vitro. Int J Pharm 389(1–2):10–17. https://doi.org/10.1016/j.ijpharm.2009.12.061
Kurman RJ, IeM S (2010) The origin and pathogenesis of epithelial ovarian cancer: a proposed unifying theory. Am J Surg Pathol 34(3):433–443. https://doi.org/10.1097/PAS.0b013e3181cf3d79
Lee MK, Lim SJ, Kim CK (2007) Preparation, characterization and in vitro cytotoxicity of paclitaxel-loaded sterically stabilized solid lipid nanoparticles. Biomaterials 28(12):2137–2146. https://doi.org/10.1016/j.biomaterials.2007.01.014
McGuire WP, Hoskins WJ, Brady MF, Kucera PR, Partridge EE, Look KY, Clarke-Pearson DL, Davidson M (1996) Cyclophosphamide and cisplatin compared with paclitaxel and cisplatin in patients with stage III and stage IV ovarian cancer. N Engl J Med 334(1):1–6. https://doi.org/10.1056/NEJM199601043340101
Michy T, Massias T, Bernard C, Vanwonterghem L, Henry M, Guidetti M, Royal G, Coll JL, Texier I, Josserand V, Hurbin AA (2019) Verteporfin-loaded lipid nanoparticles improve ovarian cancer photodynamic therapy in vitro and in vivo. Cancers (Basel) 11(11):1760. https://doi.org/10.3390/cancers11111760
Milane L, Duan Z, Amiji M (2011) Development of EGFR-targeted polymer blend nanocarriers for combination paclitaxel/lonidamine delivery to treat multi-drug resistance in human breast and ovarian tumor cells. Mol Pharm 8(1):185–203. https://doi.org/10.1021/mp1002653
Moore RG, Maclaughlan S (2010) Current clinical use of biomarkers for epithelial ovarian cancer. Curr Opin Oncol 22(5):492–497. https://doi.org/10.1097/CCO.0b013e32833c3351
Muddineti OS, Kumari P, Ray E, Ghosh B, Biswas S (2017 Jun) Curcumin-loaded chitosan-cholesterol micelles: evaluation in monolayers and 3D cancer spheroid model. Nanomedicine (Lond) 12(12):1435–1453. https://doi.org/10.2217/nnm-2017-0036
Mutlu-Agardan NB, Sarisozen C, Torchilin VP (2020) Cytotoxicity of novel redox sensitive PEG2000-S-S-PTX micelles against drug-resistant ovarian and breast cancer cells. Pharm Res 37(3):65. https://doi.org/10.1007/s11095-020-2759-4
Noorani L, Stenzel M, Liang R, Pourgholami MH, Morris DL (2015) Albumin nanoparticles increase the anticancer efficacy of albendazole in ovarian cancer xenograft model. J Nanobiotechnology. 13:25. https://doi.org/10.1186/s12951-015-0082-8
Novartis Pharmaceuticals (2009, March–2013, December) Efficacy and safety of pazopanib monotherapy after first line chemotherapy in ovarian, fallopian tube, or primary peritoneal cancer. Identifier NCT00866697. https://clinicaltrials.gov/ct2/show/NCT00866697?term=pazopanib&cond=Ovarian+Cancer&draw=2&rank=9. Accessed on 14 Jan, 2022
Pan Q, Tian J, Zhu H, Hong L, Mao Z, Oliveira JM, Reis RL, Li X (2020) Tumor-targeting Polycaprolactone nanoparticles with Codelivery of paclitaxel and IR780 for combinational therapy of drug-resistant ovarian cancer. ACS Biomater Sci Eng 6(4):2175–2185. https://doi.org/10.1021/acsbiomaterials.0c00163
Pantshwa JM, Kondiah PPD, Choonara YE, Marimuthu T, Pillay V (2020) Nanodrug delivery Systems for the Treatment of ovarian cancer. Cancers (Basel). 12(1):213. https://doi.org/10.3390/cancers12010213
Pignata S, Cannella L, Leopardo D, Pisano C, Bruni GS, Facchini G (2011) Chemotherapy in epithelial ovarian cancer. Cancer Lett 303(2):73–83. https://doi.org/10.1016/j.canlet.2011.01.026
Prat J (2014) FIGO committee on Gynecologic oncology. Staging classification for cancer of the ovary, fallopian tube, and peritoneum. Int J Gynaecol Obstet 124(1):1–5. https://doi.org/10.1016/j.ijgo.2013.10.001
Qi Z, Yin L, Xu Y, Wang F (2018) Pegylated liposomal-paclitaxel induces ovarian cancer cell apoptosis via TNF-induced ERK/AKT signaling pathway. Mol Med Rep 17(6):7497–7504. https://doi.org/10.3892/mmr.2018.8811
Rai B, Bansal A, Patel FD, Sharma SC (2014) Radiotherapy for ovarian cancers–redefining the role. Asian Pac J Cancer Prev 15(12):4759–4763. https://doi.org/10.7314/apjcp.2014.15.12.4759
Ramalingam V, Mohan Harshavardhan S, Kumar D, Malathi S, devi. (2020) Wet chemical mediated hematite α-Fe2O3 nanoparticles synthesis: preparation, characterization and anticancer activity against human metastatic ovarian cancer. Journal of Alloys and Compounds 834:155118. https://doi.org/10.1016/j.jallcom.2020.155118
Sánchez-Ramírez DR, Domínguez-Ríos R, Juárez J, Valdés M, Hassan N, Quintero-Ramos A, Del Toro-Arreola A, Barbosa S, Taboada P, Topete A, Daneri-Navarro A (2020) Biodegradable photoresponsive nanoparticles for chemo-, photothermal- and photodynamic therapy of ovarian cancer. Mater Sci Eng C Mater Biol Appl 116:111196. https://doi.org/10.1016/j.msec.2020.111196
Santoiemma PP, Powell DJ Jr (2015) Tumor infiltrating lymphocytes in ovarian cancer. Cancer Biol Ther 16(6):807–820. https://doi.org/10.1080/15384047.2015.1040960
Sarojini S, Tamir A, Lim H, Li S, Zhang S, Goy A, Pecora A, Suh KS (2012) Early detection biomarkers for ovarian cancer. J Oncol 2012:709049. https://doi.org/10.1155/2012/709049
Shaaban AM, Rezvani M, Elsayes KM, Baskin H Jr, Mourad A, Foster BR, Jarboe EA, Menias CO (2014) Ovarian malignant germ cell tumors: cellular classification and clinical and imaging features. Radiographics 34(3):777–801. https://doi.org/10.1148/rg.343130067
Shaikh IM, Tan KB, Chaudhury A, Liu Y, Tan BJ, Tan BM, Chiu GN (2013) Liposome co-encapsulation of synergistic combination of irinotecan and doxorubicin for the treatment of intraperitoneally grown ovarian tumor xenograft. J Control Release 172(3):852–861
Sivasankarapillai V, Das SS, Sabir F, Sundaramahalingam M, Colmenares J, Prasannakumar S, Rajan M, Rahdar A, Kyzas G (2021) Progress in natural polymer engineered biomaterials for transdermal drug delivery systems. Materials Today Chemistry 19:100382. https://doi.org/10.1016/j.mtchem.2020.100382
Song H, Sgouros G (2011) Radioimmunotherapy of solid tumors: searching for the right target. Curr Drug Deliv 8(1):26–44. https://doi.org/10.2174/156720111793663651
Tayama S, Motohara T, Narantuya D, Li C, Fujimoto K, Sakaguchi I, Tashiro H, Saya H, Nagano O, Katabuchi H (2017) The impact of EpCAM expression on response to chemotherapy and clinical outcomes in patients with epithelial ovarian cancer. Oncotarget 8(27):44312–44325. https://doi.org/10.18632/oncotarget.17871
Tewari D, Java JJ, Salani R, Armstrong DK, Markman M, Herzog T, Monk BJ, Chan JK (2015) Long-term survival advantage and prognostic factors associated with intraperitoneal chemotherapy treatment in advanced ovarian cancer: a gynecologic oncology group study. J Clin Oncol 33(13):1460–1466. https://doi.org/10.1200/JCO.2014.55.9898
Tirelli N, Lutolf MP, Napoli A, Hubbell JA (2002) Poly(ethylene glycol) block copolymers. J Biotechnol 90(1):3–15. https://doi.org/10.1016/s1389-0352(01)00057-5
Torchilin VP (2006) Multifunctional nanocarriers. Adv Drug Deliv Rev 58(14):1532–1555. https://doi.org/10.1016/j.addr.2006.09.009
Ulbrich K, Hekmatara T, Herbert E, Kreuter J (2009) Transferrin- and transferrin-receptor-antibody-modified nanoparticles enable drug delivery across the blood-brain barrier (BBB). Eur J Pharm Biopharm 71(2):251–256. https://doi.org/10.1016/j.ejpb.2008.08.021
Uster PS, Allen TM, Daniel BE, Mendez CJ, Newman MS, Zhu GZ (1996) Insertion of poly(ethylene glycol) derivatized phospholipid into pre-formed liposomes results in prolonged in vivo circulation time. FEBS Lett 386(2–3):243–246. https://doi.org/10.1016/0014-5793(96)00452-8
van Vlerken LE, Vyas TK, Amiji MM (2007) Poly(ethylene glycol)-modified nanocarriers for tumor-targeted and intracellular delivery. Pharm Res 24(8):1405–1414. https://doi.org/10.1007/s11095-007-9284-6
Varki A, Cummings RD, Esko JD, Stanley P, Hart GW, Aebi M, et al. Essentials of Glycobiology (3rd). Cold Spring Harbor (NY): Cold Spring Harbor Laboratory Press; 2015–2017. https://www.ncbi.nlm.nih.gov/books/NBK310274/
Vergara D, Bellomo C, Zhang X, Vergaro V, Tinelli A, Lorusso V, Rinaldi R, Lvov YM, Leporatti S, Maffia M (2012) Lapatinib/paclitaxel polyelectrolyte nanocapsules for overcoming multidrug resistance in ovarian cancer. Nanomedicine 8(6):891–899. https://doi.org/10.1016/j.nano.2011.10.014
Vergote I, du Bois A, Floquet A, Rau J, Kim JW, Del Campo JM, Friedlander M, Pignata S, Fujiwara K, Colombo N, Mirza MR, Monk BJ, Tsibulak I, Calvert PM, Herzog TJ, Hanker LC, Meunier J, Lee JY, Bologna A, Carrasco-Alfonso MJ, Harter P (2019) Overall survival results of AGO-OVAR16: a phase 3 study of maintenance pazopanib versus placebo in women who have not progressed after first-line chemotherapy for advanced ovarian cancer. Gynecol Oncol 155(2):186–191. https://doi.org/10.1016/j.ygyno.2019.08.024
Vilos C, Morales FA, Solar PA, Herrera NS, Gonzalez-Nilo FD, Aguayo DA, Mendoza HL, Comer J, Bravo ML, Gonzalez PA, Kato S, Cuello MA, Alonso C, Bravo EJ, Bustamante EI, Owen GI, Velasquez LA (2013) Paclitaxel-PHBV nanoparticles and their toxicity to endometrial and primary ovarian cancer cells. Biomaterials 34(16):4098–4108. https://doi.org/10.1016/j.biomaterials.2013.02.034
Wang P, Fang L (2021) Salpingo-oophorectomy versus cystectomy in patients with borderline ovarian tumors: a systemic review and meta-analysis on postoperative recurrence and fertility. World J Surg Oncol 19(1):132. https://doi.org/10.1186/s12957-021-02241-2
Wilken JA, Webster KT, Maihle NJ (2010) Trastuzumab sensitizes ovarian cancer cells to EGFR-targeted therapeutics. J Ovarian Res 3:7. https://doi.org/10.1186/1757-2215-3-7
Yu F, Jiang F, Tang X, Wang B (2018) N-octyl-N-arginine-chitosan micelles for gambogic acid intravenous delivery: characterization, cell uptake, pharmacokinetics, and biodistribution. Drug Dev Ind Pharm 44(4):615–623. https://doi.org/10.1080/03639045.2017.1405973
Yuan MQ, Zhu F, Lou JY, Yuan WM, Fu L, Liu S, Zhang ZZ, Liu CY, He Q (2014) The anti-tumoral efficacy of a docetaxel-loaded liposomal drug delivery system modified with transferrin for ovarian cancer. Drug Res (Stuttg) 64(4):195–202. https://doi.org/10.1055/s-0033-1355335
Zalipsky S, Mullah N, Harding JA, Gittelman J, Guo L, DeFrees SA (1997) Poly(ethylene glycol)-grafted liposomes with oligopeptide or oligosaccharide ligands appended to the termini of the polymer chains. Bioconjug Chem 8(2):111–118. https://doi.org/10.1021/bc9600832
Zhang Y (2008) Progress and challenges in protein structure prediction. Curr Opin Struct Biol 18(3):342–348. https://doi.org/10.1016/j.sbi.2008.02.004
Zhang XY, Chen J, Zheng YF, Gao XL, Kang Y, Liu JC, Cheng MJ, Sun H, Xu CJ (2009b) Follicle-stimulating hormone peptide can facilitate paclitaxel nanoparticles to target ovarian carcinoma in vivo. Cancer Res 69(16):6506–6514. https://doi.org/10.1158/0008-5472.CAN-08-4721
Zhang Z, Jia L, Feng Y, Zheng W (2009a) Overexpression of follicle-stimulating hormone receptor facilitates the development of ovarian epithelial cancer. Cancer Lett 278(1):56–64. https://doi.org/10.1016/j.canlet.2008.12.024
Zhi D, Yang T, Yang J, Fu S, Zhang S (2020) Targeting strategies for superparamagnetic iron oxide nanoparticles in cancer therapy. Acta Biomater 102:13–34. https://doi.org/10.1016/j.actbio.2019.11.027
Zhou M, Luo Y, Zeng W, Yang X, Chen T, Zhang L, He X, Yi X, Li Y, Yi X (2021) A co-delivery system based on a dimeric prodrug and star-shaped polymeric prodrug micelles for drug delivery. Front Chem 9:765021. https://doi.org/10.3389/fchem.2021.765021
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Das, S.S., Moitra, I., Das, S., Singh, N., Verma, P.R.P., Singh, S.K. (2022). Conventional to Nanoscale-Based Carrier Systems in the Management of Ovarian Cancer. In: Rahman, M., H Almalki, W., Alrobaian, M., Beg, S., Alharbi, K.S. (eds) Hormone Related Cancer Mechanistic and Nanomedicines. Springer, Singapore. https://doi.org/10.1007/978-981-19-5558-7_5
Download citation
DOI: https://doi.org/10.1007/978-981-19-5558-7_5
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-19-5557-0
Online ISBN: 978-981-19-5558-7
eBook Packages: MedicineMedicine (R0)