Abstract/Introduction
More than 95% of newborns have cutaneous findings, which often are distressing to parents but frequently are benign and self-limited. Among them are milia, cutis marmorata, congenital dermal melanocytosis and the benign neonatal pustular eruptions. The majority of the dermatologic alterations in neonates are physiological and transient and do not require any treatment; thus the parents can be reassured about the good prognosis. An overview of the most common or important dermatoses presenting in neonatal and infant age group is illustrated in this chapter.
The clinical photographs in this chapter are photographed by Dr. Ranthilaka R. Ranawaka, consultant dermatologist, General Hospital Kalutara, Sri Lanka
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
FormalPara IntroductionMore than 95% of newborns have cutaneous findings, which often are distressing to parents but frequently are benign and self-limited. Among them are milia, cutis marmorata, congenital dermal melanocytosis and the benign neonatal pustular eruptions (Rayala and Morrell 2017; Zuniga and Nguyen 2013). The majority of the dermatologic alterations in neonates are physiological and transient and do not require any treatment; thus the parents can be reassured about the good prognosis (Patrizi et al., 2017). An overview of the most common or important dermatoses presenting in neonatal and infant age group is illustrated in this chapter.
-
1.
 A 6 months old baby was brought with this skin lesion which has been there since birth, the mother is worried that it is being progressively enlarging.
A 6 months old baby was brought with this skin lesion which has been there since birth, the mother is worried that it is being progressively enlarging.-
(a)
What is the diagnosis?
-
(b)
What is the sequelae of the disease?
-
(a)
-
2.

 A 3 months old baby was brought with mildly erythematous hypopigmented patches on the groin, back of the trunk, neck and upper chest. They were mostly asymptomatic. What is the diagnosis?
A 3 months old baby was brought with mildly erythematous hypopigmented patches on the groin, back of the trunk, neck and upper chest. They were mostly asymptomatic. What is the diagnosis? -
3.
 A 1-year-old child came with the above lesions which were asymptomatic. He was getting these lesions frequently. His 3-year-old sister also was getting few lesions on the face. What is the diagnosis?
A 1-year-old child came with the above lesions which were asymptomatic. He was getting these lesions frequently. His 3-year-old sister also was getting few lesions on the face. What is the diagnosis? -
4.
 A 4-month-old baby was brought with itchy skin lesions on the trunk, buttocks and genitalia for 3 weeks.
A 4-month-old baby was brought with itchy skin lesions on the trunk, buttocks and genitalia for 3 weeks.-
(a)
What is the diagnosis?
-
(b)
Who else do you want to examine?
-
(a)
-
5.
 The mother of this 6 months old baby is worried about these scaly lesions on the scalp which are mildly itchy.
The mother of this 6 months old baby is worried about these scaly lesions on the scalp which are mildly itchy.-
(a)
What is the diagnosis?
-
(b)
What advice would you give the mother?
-
(a)
-
6.
 A 2-year-old child has a distractible itching more pronounced during the night. On direct inquiry revealed that his whole family has generalized itching without any visible skin rash.
A 2-year-old child has a distractible itching more pronounced during the night. On direct inquiry revealed that his whole family has generalized itching without any visible skin rash.-
(a)
What is the diagnosis?
-
(b)
What is the condition shown in this picture?
-
(a)
-
7.
 A 4 days old neonate was brought with this skin eruption. What is the diagnosis?
A 4 days old neonate was brought with this skin eruption. What is the diagnosis? -
8.
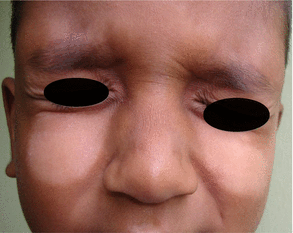 A 5-year-old boy has these asymptomatic hypopigmented patches on both cheeks for 2 months which are progressively enlarging. What is the diagnosis?
A 5-year-old boy has these asymptomatic hypopigmented patches on both cheeks for 2 months which are progressively enlarging. What is the diagnosis? -
9.
 This painless boggy mass has appeared and enlarged within 1 week despite antibiotics prescribed by the family physician. What is the diagnosis?
This painless boggy mass has appeared and enlarged within 1 week despite antibiotics prescribed by the family physician. What is the diagnosis? -
10.

 This 4-year-old child’s mother is worried about these asymptomatic lesions which appeared 4 weeks ago.
This 4-year-old child’s mother is worried about these asymptomatic lesions which appeared 4 weeks ago.-
(a)
What is the diagnosis?
-
(b)
What advice would you give the mother?
-
(a)
-
11.
 A 6-year-old child developed these patchy hair loss over 3 weeks which were treated with native remedies. What is the diagnosis?
A 6-year-old child developed these patchy hair loss over 3 weeks which were treated with native remedies. What is the diagnosis? -
12.
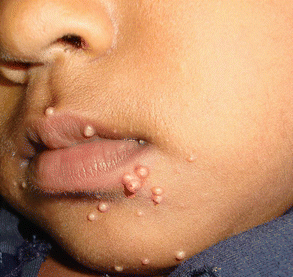 These asymptomatic lesions had appeared over 3 weeks. What is the diagnosis?
These asymptomatic lesions had appeared over 3 weeks. What is the diagnosis? -
13.
 A 4-year-old child came with these painful pustules localized to shown area.
A 4-year-old child came with these painful pustules localized to shown area.-
(a)
What are the differential diagnoses?
-
(b)
What was the diagnosis in this child?
-
(a)
-
14.
 A 7-year-old boy had developed these lesions on the face over 3 months.
A 7-year-old boy had developed these lesions on the face over 3 months.-
(a)
What are the possible diagnoses?
-
(b)
What are the other features you want to look for?
-
(c)
How do you treat this skin problem?
-
(a)
-
15.
 The mother of this 6 months old baby is worried about these linear hypopigmented patches on the trunk.
The mother of this 6 months old baby is worried about these linear hypopigmented patches on the trunk.-
(a)
What is the diagnosis?
-
(b)
What advice would you give the mother?
-
(a)
-
16.
 A newborn had this patch of alopecia.
A newborn had this patch of alopecia.-
(a)
What are the possible causes?
-
(a)
-
17.
 The mother of this 7-year-old child complains foul smell from his feet when he removes socks after school.
The mother of this 7-year-old child complains foul smell from his feet when he removes socks after school.-
(a)
What is the diagnosis?
-
(b)
What are the predisposing factors?
-
(a)
-
18.
 A 4-year-old child was brought with this nail abnormality. After few weeks these nails fall spontaneously.
A 4-year-old child was brought with this nail abnormality. After few weeks these nails fall spontaneously.-
(a)
What is the diagnosis?
-
(b)
What are the predisposing factors?
-
(c)
How do you manage this?
-
(a)
-
19.
 A 20 days old baby girl who was normal at birth had developed these blisters and erosions for the last 3 days.
A 20 days old baby girl who was normal at birth had developed these blisters and erosions for the last 3 days.-
(a)
What are the differential diagnoses?
-
(a)
-
20.
 A 5-year-old child developed this skin eruption with fever, malaise and body aches.
A 5-year-old child developed this skin eruption with fever, malaise and body aches.-
(a)
What is the diagnosis?
-
(a)
-
21.
 A 4-month-old baby was brought with this inguinal rash for 1 month.
A 4-month-old baby was brought with this inguinal rash for 1 month.
-
(a)
What are the differential diagnoses?
-
22.
 A 12-year-old child came with this linear itchy lesion on the dorsum of the hand. They noticed that the lesion is extending forward.
A 12-year-old child came with this linear itchy lesion on the dorsum of the hand. They noticed that the lesion is extending forward.
-
(a)
What is the diagnosis?
Answers
-
1.
Infantile haemangioma (Chap. 3).
It will slowly grow over the first 12 months and then regress gradually over the next 2–3 years which almost disappears leaving some slack skin.
No treatment is given unless it obstructs the function of vital organs. But there is a tendency to easy bleeding and secondary infection.
-
2.
Infantile seborrhoeic dermatitis.
-
3.
Staph impetigo.
-
4.
Tinea infection (Chap. 17).
Close relatives who look after the child, e.g. parents, grandparents, nanny, etc. Usually infants acquire this infection from adults. You should treat the adult who has tinea infection too, to avoid reinfection.
-
5.
Cradle cap.
This will spontaneously clear over months. Treat symptomatically.
-
6.
Scabies (Chap. 20).
Scabietic nodules which have predilection to genitalia, which are very itchy and can persist for weeks to months after successful treatment of scabies.
-
7.
Folliculitis.
-
8.
Polymorphic light eruption (Chap. 10).
-
9.
Kerion (Chap. 17).
-
10.
Granuloma annulare.
These are benign lesions which resolve spontaneously with time.
-
11.
Alopecia areata (Chap. 35).
-
12.
Molluscum contagiosum (Chap. 16).
-
13.
Staph impetigo and herpes infection.
Herpes infection (HSV I).
-
14.
Acneiform eruption due to topical or systemic steroids, drug-induced acne and adenoma sebaceum (angiofibromas) in tuberous sclerosis complex (TCS).
Hypomelanotic macules (ash-leaf macules) and angiofibromas are pathognomonic in TCS, also look for periungual fibromas (Koenen tumours) and shagreen patch (Chap. 4).
This is adenoma sebaceum (angiofibromas) in tuberous sclerosis complex (TCS) which can be treated with electrocautery or laser.
-
15.
Pigmentary mosaicism, streaks and whorls of hypo- or hyperpigmentation following Blaschko’s lines. Infants with pigmentary mosaicism should be thoroughly assessed for the development, the internal organs and skeletal and ophthalmological abnormalities.
-
16.
This lesion is circumscribed alopecia of congenital origin. This can be due to several causes, sebaceous naevus, aplasia cutis or sutural alopecia which will be obvious later.
-
17.
Pitted keratolysis.
Hyperhidrosis and frequent emersion of feet in water are the predisposing factors.
-
18.
Onychomadesis (Chap. 37).
This not uncommon in children after viral infection, most commonly hand, foot and mouth disease.
-
19.
Bullous impetigo and dystrophic epidermolysis bullosa (DEB).
In DEB the child is clinically well in spite of large erosions, and lesions are confined to areas of friction.
-
20.
Chickenpox (Chap. 16).
-
21.
Infantile psoriasis, napkin dermatitis and infantile seborrhoeic dermatitis.
Involvement of the napkin area (psoriatic napkin eruption) may be the first presentation of psoriasis in infancy (Burden and Kirby 2016). Edges of the lesions are well defined unless altered by medicaments.
-
22.
Cutaneous larva migrans.
1 Inflammatory Conditions
1.1 Cradle Cap
Cradle cap may be seen in the neonate; the condition is most common between the ages of 4 and 16 weeks. It can occur in isolation or in association with seborrhoeic dermatitis. Most cases of cradle cap resolve spontaneously after a few weeks (Das and Das 2014).
Clinical presentation: Thick scales adherent to scalp since birth. Mild inflammation with itching in some, but most are asymptomatic (Fig. 1.1).
Management: An emollient to lift the scale, in combination with a shampoo.
1.2 Infantile Seborrhoeic Dermatitis
Infantile seborrhoeic dermatitis (ISD) occurs between the ages of 4 and 12 weeks but most commonly before the age of 2 months.
Clinical presentation: macerated erythema on the skin folds, neck, axillae, inguinal region, elbows and skin creases. ISD may associate with cradle cap, rarely symptomatic (Sarkar and Garg 2010). Typically inflammation resolves with postinflammatory hypopigmentation which is marked in pigmented skin and is a great concern to parents (Figs. 1.1, 1.2, 1.3, 1.4 and 1.5).
Differential diagnosis: napkin dermatitis, atopic eczema, Langerhans cell histiocytosis (Leung et al. 2019).
Management: a combination of steroid–antifungal creams in cases where inflammation is marked, intermittently for short periods. Hypopigmentation resolves spontaneously within weeks to months (Victoire et al. 2019).
1.3 Atopic Eczema
In infants, AE characteristically begins on the face with subsequent spread to involve the torso and limbs. A more nummular (discoid) pattern occurs, particularly on the back and legs, especially in toddlers. AE in the majority of infants clears over time. Nearly half of children with early AE are in complete remission by age 3 years. A significant number of children were found to develop AD shortly after their ISD diagnosis. This finding demonstrates a strong association in the clinical course between the two diseases or indicates that the two diseases may be in the same clinical spectrum (Alexopoulos et al. 2014).
Clinical presentation: Mildly itchy scales mainly on the cheeks and on extensors, which change to flexural involvement when the child grows (Figs. 1.6 and 1.7).
Management: Exclusive breastfeeding for the first 6 months is advisable. This is a chronic recurrent problem in many. Topical steroid should be used sparsely with frequent emollients.
1.4 Napkin Dermatitis
Prolonged contact with urine induces an irritant erythema, which may break down to form erosions if untreated.
Clinical presentation: dermatitis is limited to the areas in contact with the irritant, while the skin folds may be spared (in contrast to seborrhoeic dermatitis or infantile psoriasis where skin folds are affected) (Figs. 1.8, 1.9 and 1.10).
Differential diagnosis: allergic contact dermatitis, intertrigo, psoriasis and atopic and seborrhoeic dermatitis (Tüzün et al. 2015).
Management: the mainstay of management is to keep the skin dry and use barrier creams or emollients to restore normal epidermis. Mild topical steroids are used if inflamed or itchy. Treat secondary bacterial or candida infection appropriately. Advise to wear disposable diapers which are much more absorbent, especially during the night.
1.5 Infantile Psoriasis
Napkin psoriasis with dissemination is the most common pattern in infants (question 21). All patterns of psoriasis have been described in children: guttate, chronic plaque, pustular and erythrodermic, but severe disease and joint involvement are relatively rare (Burden and Kirby 2016).
Differential diagnosis: napkin dermatitis, infantile seborrhoeic dermatitis and irritant contact dermatitis.
Treatments: mild topical steroids, often in combination with an anticandidal agent, and emollients usually suffice in most children.
1.6 Miliaria
Miliaria is due to blockage of eccrine sweat ducts. Immature sweat ducts are an important factor in neonates although high levels of heat and humidity are important at any age. It is subdivided into three subtypes dependent on the level of blockage: miliaria crystallina (stratum corneum), miliaria rubra (mid-epidermal) and miliaria profunda (dermal–epidermal junction) (Paige 2016; Dixit et al. 2012).
Clinical Presentation
Miliaria crystallina presents as crops of clear, thin-walled, superficial vesicles 1–2 mm in diameter, without associated erythema, resembling drops of water. These are exceedingly delicate and generally rupture within 24 h and are followed by bran-like desquamation. Lesions are asymptomatic.
Miliaria rubra (prickly heat, sweat rash) comprises erythematous papules and papulovesicles about 1–4 mm in diameter, on a background of macular erythema. Lesions can be itchy or sore.
Miliaria pustulosa: Some of the miliaria rubra lesions are pustular, but not infected.
Miliaria profunda (granulomatous giant centrifugal variant) is very uncommon in neonates as it usually occurs in adults where there have been repeated episodes of miliaria rubra.
Management: Miliaria crystalline improves spontaneously when sweat ducts are mature. Remove from conditions of high heat/humidity and any occlusive clothing or bedding (Figs. 1.11, 1.12 and 1.13).
2 Infections and Infestations
2.1 Hand, Foot and Mouth Disease
Coxsackie A viral infection, most usually A16, and infection with A6, Coxsackie B and enterovirus 71 have also been described. Highly contagious and widespread outbreaks occur every year.
Clinical presentation: Mild malaise, oral ulcers and hand and foot vesicular eruption. Crops of vesicles are grouped in elbows and knees. Very rarely, a widespread vesicular eruption occurs over the buttocks, trunk and perioral area. In some, the eruption may be papular or maculopapular without vesicles. When it resolves it may form marked scaling or postinflammatory hyperpigmentation which settles spontaneously (Sterling 2016; Higgins and Glover 2016) (Figs. 1.14, 1.15, 1.16 and 1.17).
Diagnosis: Clinical.
Differential diagnosis: Oral lesions may suggest herpes simplex or Stevens–Johnson syndrome
and, if widespread, chickenpox or Kaposi varicelliform eruption.
Management: Symptomatic treatment only is required in many children. In very extensive eruption, oral acyclovir is given three times daily for 3 days.
2.2 Varicella/Chickenpox
The incubation period is 14–21 days. Small erythematous papules and vesicles appear on the trunk, scalp or genital regions. The onset of the rash may be preceded by 1–2 days of malaise and fever. Lesions in different stages of evolution are evident. Centripetal pattern. The child should be isolated until the lesions have crusted over (Fig. 1.18).
2.3 Impetigo
Caused by Staphylococcus aureus but less frequently Streptococcus pyogenes. Honey-coloured crusts appear on a background of erythema. Bullous and non-bullous forms exist (Hay and Morris-Jones 2016; Ghosh 2015) (Figs. 1.19, 1.20, 1.21 and 1.22).
2.4 Staphylococcal Scalded Skin Syndrome
Causative organisms: Staphylococcus aureus strains producing exfoliative toxins.
It is an exfoliative dermatosis in which most of the body surface becomes tender and erythematous and the superficial epidermis strips off. Children (under the age of 6 years) and neonates are most commonly affected by the generalized form of SSSS; rarely adults may be affected (Leung et al. 2018).
Differential diagnosis: Toxic epidermal necrolysis (TEN).
Treatments: Depend on the antibiotic sensitivity • flucloxacillin • clindamycin • temocillin • tigecycline • daptomycin, if MRSA is suspected, • vancomycin • tobramycin (Figs. 1.23 and 1.24).
2.5 Pitted Keratolysis
Causative organisms: Corynebacterium spp.
Clinical presentation: Numerous superficial punched out erosions on soles, undersurfaces of the toes and rarely palms. But pressure-bearing or friction areas are most common. Hyperhidrosis is often associated, sometimes with maceration, stickiness and a foul odour. Soaking the feet in water for 15 min causes swelling of the horny layer and accentuates the lesions. Irritation is minimal, and in most cases, patients are unaware of the condition (Makhecha et al. 2017; Pranteda et al. 2014) (Fig. 1.25).
Differential diagnosis: Tinea pedis.
Management: Treat hyperhidrosis with potassium permanganate soaks, aluminium chloride and iontophoresis, if resistant botulinum toxin. Topical fucidin ointment, imidazoles such as clotrimazole are also effective.
2.6 Cutaneous Fungal Infections
Candida infection: Secondary colonization of eroded or macerated skin in intertriginous areas, especially the napkin region, may occur but is much less common since the decline in diaper dermatitis. Satellite pustules are characteristic. If children get recurrent candida infection, underlying predisposing factors should be sought; inherited immune deficiency, or acquired habit disorder (Figs. 1.26, 1.27 and 1.28).
Tinea corporis: nearly always acquired from an older child or from an infected adult (mother, grandmother, caretaker, etc.) (Figs. 1.29 and 1.30).
Tinea capitis: mildly scaly and mildly itchy well-demarcated patch on the scalp (Figs. 1.31 and 1.32).
2.7 Scabies
Infestation with the mite Sarcoptes scabiei. In infants, burrows may be seen on the palms and soles more characteristically than in the finger webs, and the wrists are also commonly involved. Burrows can appear quite inflammatory with surrounding secondary eczematous changes. Nodular lesions develop in the axillae and genital region if the infection is untreated. Post-scabietic pruritus may be prolonged and symptomatic treatment is usually required (Figs. 1.33, 1.34 and 1.35).
2.8 Cutaneous Larva Migrans
Creeping or migrating lesion due to the presence of moving parasites in the skin. These are all hookworms of mainly dogs and cats. The lesion is exceedingly itchy, slightly raised, skin coloured or pink and forms bizarre, serpentine patterns.
Causative organisms: Ancylostoma braziliense: Dog and cat hookworm is the commonest cause of creeping eruption in humans. • Ancylostoma caninum: Dog hookworm.
Treatment: Ivermectin 200 μg/kg orally once daily for 1–2 days or albendazole 400 mg orally for 3 days (Fig. 1.36).
2.9 Molluscum Contagiosum
Characterized by discrete, pearly, umbilicated papules 2–5 mm in diameter. The eruption is usually self-limiting but is often a source of great parental concern.
Management: cryotherapy (if tolerated) or topical treatment with either hydrogen peroxide creams or commercially available potassium hydroxide solutions can speed resolution (Fig. 1.37).
Staphylococcal scalded skin syndrome in an infant. A 2-month-old baby came with fever and generalized erythema. On examination scaling of skin was noted which was marked around the orifices and flexures. Initial widespread erythematous eruption may not be obvious in dark-skinned infants as seen in this baby. That may lead to late diagnosis unless vigilant
3 Reactive Conditions
3.1 Acute Haemorrhagic Oedema in Infancy
Benign, cutaneous, leukocytoclastic vasculitis, arising after respiratory infection, medication administration or immunization. It is thought likely to be an immune complex-mediated vasculitis. The condition affects children between the ages of 4 months and 2 years, with males being affected twice as frequently as females. Fever is mild and systemic disturbance is minor. Resolution occurs within 3 weeks, and recurrences are not a feature (Fig. 1.38).
3.2 Papular Urticaria
Papular urticaria arises as a result of a hypersensitivity reaction to insect bites.
Clinical presentation: crops of more or less symmetrically distributed, itchy papules and papulovesicles most frequently on exposed areas of the extremities. They are often heavily excoriated, and secondary bacterial infection is common.
Management: topical steroids and systemic antihistamines. Avoid insect bites (Fig. 1.39).
4 Developmental Problems
4.1 Pigmentary Mosaicism
Streaks and whorls of hypo- or hyperpigmentation following Blaschko’s lines. Infants with pigmentary mosaicism should be thoroughly assessed with particular attention to development, the internal organs and skeletal and ophthalmological abnormalities (Figs. 1.40, 1.41 and 1.42).
5 Genetic Disorders
5.1 Epidermolysis Bullosa
Epidermolysis bullosa comprises a group of genetically determined skin fragility disorders characterized by blistering of the skin and mucosae following mild mechanical trauma (McGrath 2016). Epidermolysis bullosa is categorized according to inheritance, clinical presentation and level of cleavage (Figs. 1.43, 1.44, 1.45, 1.46 and 1.47).
5.2 Inherited Generalized Cutis Laxa
Cutis laxa is characterized clinically by lax pendulous skin that only slowly recoils when pulled.
Histology: there is loss and fragmentation of elastic tissue in the dermis (Fig. 1.48).
5.3 Hypohidrotic Ectodermal Dysplasia
X-linked hypohidrotic ectodermal dysplasia (Freire-Maia 1-2-3-4) is the most common of the ectodermal dysplasias. The disorder is characterized by hypotrichosis with fine, slow-growing scalp and body hair, sparse eyebrows, hypohidrosis, nail anomalies and hypodontia.
Clinical presentation: The hair is sparse, dry and lusterless with a light colour. Eyebrows are scanty or absent occasionally; just the outer two-thirds are missing. Eyelashes may be normal, sparse or completely absent. Hair on the torso and extremities is usually absent. Secondary sexual hair in the beard, pubic and axillary regions is variably present and may be normal.
Peg-shaped primary and secondary teeth are typical.
Decreased sweating leads to heat intolerance and enhances dryness of the skin. Sweating is often severely diminished or absent due to a paucity or absence of eccrine glands. An absence of sweating leads to an inability to thermoregulate by evaporative cooling, and hyperthermia can occur with physical exertion or in a warm environment (Itin 2016).
Disease course and prognosis: Early diagnosis is important to avoid life-threatening complications induced by hyperthermia and infections. Avoiding heat and physical overexertion is the most important preventative measure to recommend. Cooling the body with wet clothing and cool drinks is the only efficient way of treating hyperthermia. Orthodontic intervention is necessary (Fig. 1.49).
5.4 Acrodermatitis Enteropathica
Autosomal recessive disorder affecting the intestinal absorption of zinc. The resulting zinc deficiency leads to dermatitis, alopecia and diarrhoea. This is very rare (approximately 1: 500,000). Zinc is a cofactor for many enzymes. The skin, intestine and immune system are most severely affected because of their rapid cell turnover.
Clinical features: Patients present with apathy or irritability and a rash around the mouth and anus and on the hands and feet. Symptoms start after weaning in breastfed babies and at 4–10 weeks of age if they are formula-fed. Erythema progresses to vesicles, bullae, pustules, desquamation and crusting. There is alopecia and frequently blepharitis, conjunctivitis and photophobia. Infections are common, including secondary infections of the skin, for example, with Candida albicans. Wound healing is poor, and many patients have diarrhoea and growth faltering. Without treatment, the condition can be fatal, but some patients survive into adulthood (Morris 2016).
Investigations: The serum zinc concentration is usually low but can be normal. Decreased zinc absorption can be demonstrated using radioisotopes. But it is easier to undertake a trial of zinc therapy: patients respond within a week.
Management: Patients respond to oral zinc sulphate within a few days. The normal dose is 150–400 mg/day in childhood; a lower dose may suffice after puberty. A 400–500 mg/day is needed during pregnancy. Monitoring for copper deficiency should be undertaken (Figs. 1.50, 1.51, 1.52 and 1.53).
6 Miscellaneous Conditions
6.1 Hair Loss in Infancy
Occipital hair loss: Shedding of hair occurs during the 7th to 8th month in utero in all areas except the occiput, where shedding is delayed until 2–3 months postpartum, leading to the normal occipital alopecia in this age group. Trauma due to repeated friction also may contribute (Brar et al. 2019) (Fig. 1.54).
Alopecia areata: Is relatively rare in the 1st year of life, and early onset tends to indicate a poor prognosis (Fig. 1.55).
6.2 Circumscribed Alopecia of Congenital Origin
Differential diagnosis. Alopecia areata and the acquired cicatricial alopecias.
Sebaceous naevus (organoid naevus). Sebaceous naevus usually presents in childhood as a hairless patch on the scalp, often in a linear configuration. The affected skin may have a yellowish hue (Figs. 1.56 and 1.57).
Aplasia cutis. Aplasia cutis is a heterogenous group of conditions characterized by the localized absence of a portion of skin at birth. It most commonly presents as a single patch on the scalp vertex. At birth the affected skin may be superficially or deeply ulcerated or may have healed leaving an atrophic scar.
Sutural alopecia. Multiple patches of hair loss overlying the cranial sutures (Fig. 1.58).
Triangular alopecia. This usually presents during childhood although often referred to as congenital it is often not noticed at birth.
6.3 Congenital Localized Hypertrichosis
Congenital localized hypertrichosis refers to both areas of excess hair present at birth and hamartomas that may have a delayed clinical presentation. They may occur in isolation as an area of increased hair density or in association with congenital melanocytic naevi, Becker naevi, spinal dysraphism or neurofibromas (Messenger et al. 2016) (Fig. 1.59).
Congenital melanocytic naevi and neurofibromas. Congenital melanocytic naevi are often associated with prominent terminal hairs. The hair may be present from infancy or may develop after puberty.
Lumbosacral hypertrichosis. Lumbosacral hypertrichosis or the faun tail sign is a tuft of hair in the lumbosacral region that is often associated with spina bifida or diastematomyelia.
Naevoid hypertrichosis. Naevoid hypertrichosis refers to a localized area of hypertrichosis. This is usually well circumscribed (Fig. 1.60).
6.4 Juvenile Xanthogranuloma
Juvenile xanthogranuloma is a well-circumscribed yellowish nodule with an erythematous margin. Localized cutaneous JXG heals spontaneously, sometimes leaving atrophic scars.
Diagnosis: clinical, can confirm by histopathology (Figs. 1.61, 1.62 and 1.63).
6.5 Anetoderma
Anetoderma is a circumscribed area of slack skin associated with a loss of dermal substance on palpation and a loss of elastic tissue on histological examination.
Primary anetoderma remains unchanged throughout life, and new lesions often continue to develop for many years.
Secondary anetoderma is seen in association with systemic or chronic cutaneous lupus erythematosus and lupus profundus.
Investigations: In patients with primary anetoderma, it is important to test for antiphospholipid syndrome and treat appropriately, e.g. with aspirin or warfarin.
Management: No specific treatment exists (Figs. 1.64 and 1.65).
6.6 Mastocytosis
Mastocytosis in infancy is usually limited to the skin, with three distinct clinical presentations: maculopapular (formerly urticaria pigmentosa), diffuse cutaneous mastocytosis and solitary mastocytoma.
Clinical presentation: Present with patchy hyperpigmentation which urticate on rubbing.
Investigations: A skin biopsy is usually required to confirm a clinical diagnosis of cutaneous mastocytosis. Solitary mastocytoma can be diagnosed clinically.
Histopathology: The epidermis is normal apart from an increase in melanin. Mast cell numbers are increased in the dermis of all types of mastocytosis. They are well demonstrated by toluidine blue, Giemsa, tryptase or chloroacetate esterase stains in formalin-fixed biopsies.
Disease course and prognosis: Most mastocytomas resolve in childhood. Around 50% of children with urticaria pigmentosa clear by adolescence.
Management: Parents of infants with extensive skin involvement should be given advice on the avoidance of factors known to stimulate mast cell degranulation, including aspirin, nonsteroidal anti-inflammatory drugs, codeine, opiates, polymyxin B and intravenous radiograph contrast fluids and MRI contrast media. (Figs. 1.66, 1.67, 1.68, 1.69, 1.70 and 1.71).
6.7 Milia
Small, firm, white papules, predominantly occurring on the face of newborn babies and infants, are common and harmless. These are follicular epidermal cysts. If milia are exceptionally extensive or persistent, or whose distribution is atypical, may associate with syndromes.
Management: this disappears spontaneously.
6.8 Neonatal Lupus Erythematosus (see Chap. 31)
Well-defined areas of macular or slightly elevated erythema, frequently annular, occurring predominantly on the face, particularly the forehead, temples and upper cheeks and on the scalp and neck (A ‘spectacle-like’ distribution of lesions around the eyes is especially characteristic. It is now accepted that this disease is provoked in the fetus or newborn infant by maternal IgG autoantibodies that have crossed the placenta.
Management: The skin lesions of neonatal LE require no treatment, but sun protection is essential.
6.9 Collodion Baby (see Chap. 7)
Highly characteristic clinical entity present at birth where a child is born with an ‘extra’ skin resembling a shiny membrane or collodion. Almost 90% of collodion babies will go on to develop a severe form of autosomal recessive ichthyosis in the first few weeks of life: lamellar ichthyosis and non-bullous ichthyosiform erythroderma (syn. congenital ichthyosiform erythroderma) are the most common (Oji et al. 2016).
6.10 Harlequin Ichthyosis (see Chap. 7)
Harlequin ichthyosis has much thicker skin, which typically encases the baby like a suit of armour with deep fissures. Harlequin ichthyosis shows almost fusion of the fingers and toes with thick palmoplantar skin. Finally, the ears are usually bound down to the scalp in harlequin ichthyosis, whereas they are normally ‘free’ in collodion babies.
6.11 Neonatal Purpura Fulminans
Potentially lethal disorder characterized by progressive haemorrhagic necrosis of the skin associated with cutaneous vascular thrombosis.
6.12 Median Raphe Cysts
Cystic or nodular and linear swellings of the ventral penis occur near the glans. In adolescence or adulthood, they may become traumatized or infected with staphylococci, gonococci or Trichomonas and present as tender, erythematous and purulent nodules.
Histology: they are either dermoid or mucoid, depending on their embryology or epithelial lining. Very rarely, the basal epithelial lining of the cysts may contain melanocytes, imparting a brown-black pigment to the lesion.
Congenital cystic median raphe anomalies may remain unobtrusive until adulthood (Fig. 1.72).
6.13 Granuloma Annulare
This is most common in children and young adults but can occur at any age.
Clinical features: Four clinical variants identified, localized GA (commonest type in children), generalized or disseminated GA (mostly in adults), perforating GA (in all ages, infancy and in HIV) and subcutaneous GA (uncommon but mostly in children).
Histopathology: The most characteristic histological lesion in GA is the necrobiotic granuloma. Management: No treatment and reassurance of eventual resolution in localized GA. For generalized GA PUVA, laser, systemic therapies have tried with variable success (Bourke 2016) (Figs. 1.73, 1.74, 1.75 and 1.76).
Juvenile xanthogranuloma is characterized by a dense infiltrate of small histiocytes in the dermis, which stain positively for factor XIIIa, CD68, CD163, CD14 and fascin. H & E Stain X 100 (picture courtesy Dr. Priyanka H. Abeygunasekara, Consultant Pathologist, National Cancer Institute Maharagama, Sri Lanka)
Juvenile xanthogranuloma, Touton giant cells, seen in 85% of JXG cases, can be distinguished by the characteristic wreath of nuclei around a homogenous eosinophilic centre and prominent xanthomatization in the periphery H & E stain X 400 (picture courtesy Dr. Priyanka H. Abeygunasekara, Consultant Pathologist, National Cancer Institute Maharagama, Sri Lanka)
Mastocytosis (H & E stain X 400). The epidermis is normal apart from an increase in melanin. The mast cells are usually oval or spindle-shaped. Mast cell infiltrates are predominantly found around blood vessels and skin appendages in the papillary dermis (picture courtesy Dr. Priyanka H. Abeygunasekara, Consultant Pathologist, National Cancer Institute Maharagama, Sri Lanka)
References
Alexopoulos A, Kakourou T, Orfanou I et al (2014) Retrospective analysis of the relationship between infantile seborrheic dermatitis and atopic dermatitis. Pediatr Dermatol 31(2):125–130. https://doi.org/10.1111/pde.12216
Bourke J (2016) Granulomatous disorders of the skin. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 97.1
Brar BK, Brar SK, Kaur R, Sethi N (2019) Hair and scalp disorders in children below 2 years: an unremarked sphere. Int J Trichology 11(5):207–212. https://doi.org/10.4103/ijt.ijt_77_16
Burden AD, Kirby B (2016) Psoriasis and related disorders. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 35.11
Das A, Das NK (2014) Cradle cap. Indian Pediatr 51(6):509–510
Dixit S, Jain A, Datar S, Khurana VK (2012) Congenital miliaria crystallina – a diagnostic dilemma. Med J Armed Forces India 68(4):386–388. https://doi.org/10.1016/j.mjafi.2012.01.004
Ghosh S (2015) Neonatal pustular dermatosis: an overview. Indian J Dermatol 60(2):211. https://doi.org/10.4103/0019-5154.152558
Hay RJ, Morris-Jones R (2016) Bacterial infections. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, pp 26.13–26.42
Higgins EM, Glover MT (2016) Dermatoses and haemangiomas of infancy. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, pp 117.1–117.24
Itin P (2016) Ectodermal dysplasias. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s text book of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 67.11
Leung AKC, Barankin B, Leong KF (2018) Staphylococcal-scalded skin syndrome: evaluation, diagnosis, and management. World J Pediatr 14(2):116–120. https://doi.org/10.1007/s12519-018-0150-x
Leung AKC, Lam JM, Leong KF (2019) Childhood Langerhans cell histiocytosis: a disease with many faces. World J Pediatr 15(6):536–545. https://doi.org/10.1007/s12519-019-00304-9
Lovell CR (2016) Acquired disorders of dermal connective tissue. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 96.20
Makhecha M, Dass S, Singh T et al (2017) Pitted keratolysis - a study of various clinical manifestations. Int J Dermatol 56(11):1154–1160. https://doi.org/10.1111/ijd.13744
McGrath JA (2016) Genetic blistering diseases. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 71.2
Messenger AG, Sinclair RD, Farrant P, de Berker DAR (2016) Acquired disorders of hair. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 89.49
Morris A (2016) Inherited metabolic diseases. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 81.17
Oji V, Metze D, Traupe H (2016) Inherited disorders of cornification. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 65.9
Paige DG (2016) Dermatoses of the neonate. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, pp 116.1–116.27
Patrizi A, Neri I, Ricci G, Cipriani F, Ravaioli GM (2017) Advances in pharmacotherapeutic management of common skin diseases in neonates and infants. Expert Opin Pharmacother 18(7):717–725. https://doi.org/10.1080/14656566.2017.1316371
Pranteda G, Carlesimo M, Pranteda G et al (2014) Pitted keratolysis, erythromycin, and hyperhidrosis. Dermatol Ther 27(2):101–104. https://doi.org/10.1111/dth.12064
Rayala BZ, Morrell DS (2017) Common skin conditions in children: neonatal skin lesions. FP Essent 453:11–17
Sarkar R, Garg VK (2010) Erythroderma in children. Indian J Dermatol Venereol Leprol 76(4):341–347. https://doi.org/10.4103/0378-6323.66576
Sterling JC (2016) Viral infections. In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer D (eds) Rook’s textbook of dermatology, 9th edn. Wiley-Blackwell Science, Oxford, p 25.16
Tüzün Y, Wolf R, Bağlam S, Engin B (2015) Diaper (napkin) dermatitis: a fold (intertriginous) dermatosis. Clin Dermatol 33(4):477–482. https://doi.org/10.1016/j.clindermatol.2015.04.012
Victoire A, Magin P, Coughlan J, van Driel ML (2019) Interventions for infantile seborrhoeic dermatitis (including cradle cap). Cochrane Database Syst Rev 3:CD011380. https://doi.org/10.1002/14651858.CD011380.pub2
Zuniga R, Nguyen T (2013) Skin conditions: common skin rashes in infants. FP Essent 407:31–41
Acknowledgement
I thank Dr. Sandya Doluweera (consultant paediatrician) and Dr. Maduranga Mendis (medical officer) at the neonatology unit, General Hospital Kalutara, Sri Lanka, for assisting me on collecting clinical photos to this chapter.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Ranawaka, R.R. (2021). Dermatoses of the Neonate and Infancy. In: Ranawaka, R.R., Kannangara, A.P., Karawita, A. (eds) Atlas of Dermatoses in Pigmented Skin. Springer, Singapore. https://doi.org/10.1007/978-981-15-5483-4_1
Download citation
DOI: https://doi.org/10.1007/978-981-15-5483-4_1
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-15-5482-7
Online ISBN: 978-981-15-5483-4
eBook Packages: MedicineMedicine (R0)





 A 6 months old baby was brought with this skin lesion which has been there since birth, the mother is worried that it is being progressively enlarging.
A 6 months old baby was brought with this skin lesion which has been there since birth, the mother is worried that it is being progressively enlarging.
 A 3 months old baby was brought with mildly erythematous hypopigmented patches on the groin, back of the trunk, neck and upper chest. They were mostly asymptomatic. What is the diagnosis?
A 3 months old baby was brought with mildly erythematous hypopigmented patches on the groin, back of the trunk, neck and upper chest. They were mostly asymptomatic. What is the diagnosis? A 1-year-old child came with the above lesions which were asymptomatic. He was getting these lesions frequently. His 3-year-old sister also was getting few lesions on the face. What is the diagnosis?
A 1-year-old child came with the above lesions which were asymptomatic. He was getting these lesions frequently. His 3-year-old sister also was getting few lesions on the face. What is the diagnosis? A 4-month-old baby was brought with itchy skin lesions on the trunk, buttocks and genitalia for 3 weeks.
A 4-month-old baby was brought with itchy skin lesions on the trunk, buttocks and genitalia for 3 weeks. The mother of this 6 months old baby is worried about these scaly lesions on the scalp which are mildly itchy.
The mother of this 6 months old baby is worried about these scaly lesions on the scalp which are mildly itchy. A 2-year-old child has a distractible itching more pronounced during the night. On direct inquiry revealed that his whole family has generalized itching without any visible skin rash.
A 2-year-old child has a distractible itching more pronounced during the night. On direct inquiry revealed that his whole family has generalized itching without any visible skin rash. A 4 days old neonate was brought with this skin eruption. What is the diagnosis?
A 4 days old neonate was brought with this skin eruption. What is the diagnosis? A 5-year-old boy has these asymptomatic hypopigmented patches on both cheeks for 2 months which are progressively enlarging. What is the diagnosis?
A 5-year-old boy has these asymptomatic hypopigmented patches on both cheeks for 2 months which are progressively enlarging. What is the diagnosis? This painless boggy mass has appeared and enlarged within 1 week despite antibiotics prescribed by the family physician. What is the diagnosis?
This painless boggy mass has appeared and enlarged within 1 week despite antibiotics prescribed by the family physician. What is the diagnosis?
 This 4-year-old child’s mother is worried about these asymptomatic lesions which appeared 4 weeks ago.
This 4-year-old child’s mother is worried about these asymptomatic lesions which appeared 4 weeks ago. A 6-year-old child developed these patchy hair loss over 3 weeks which were treated with native remedies. What is the diagnosis?
A 6-year-old child developed these patchy hair loss over 3 weeks which were treated with native remedies. What is the diagnosis? These asymptomatic lesions had appeared over 3 weeks. What is the diagnosis?
These asymptomatic lesions had appeared over 3 weeks. What is the diagnosis? A 4-year-old child came with these painful pustules localized to shown area.
A 4-year-old child came with these painful pustules localized to shown area. A 7-year-old boy had developed these lesions on the face over 3 months.
A 7-year-old boy had developed these lesions on the face over 3 months. The mother of this 6 months old baby is worried about these linear hypopigmented patches on the trunk.
The mother of this 6 months old baby is worried about these linear hypopigmented patches on the trunk. A newborn had this patch of alopecia.
A newborn had this patch of alopecia. The mother of this 7-year-old child complains foul smell from his feet when he removes socks after school.
The mother of this 7-year-old child complains foul smell from his feet when he removes socks after school. A 4-year-old child was brought with this nail abnormality. After few weeks these nails fall spontaneously.
A 4-year-old child was brought with this nail abnormality. After few weeks these nails fall spontaneously. A 20 days old baby girl who was normal at birth had developed these blisters and erosions for the last 3 days.
A 20 days old baby girl who was normal at birth had developed these blisters and erosions for the last 3 days. A 5-year-old child developed this skin eruption with fever, malaise and body aches.
A 5-year-old child developed this skin eruption with fever, malaise and body aches. A 4-month-old baby was brought with this inguinal rash for 1 month.
A 4-month-old baby was brought with this inguinal rash for 1 month. A 12-year-old child came with this linear itchy lesion on the dorsum of the hand. They noticed that the lesion is extending forward.
A 12-year-old child came with this linear itchy lesion on the dorsum of the hand. They noticed that the lesion is extending forward.










































































