Abstract
The Middle East respiratory syndrome coronavirus (MERS-CoV) is one of the newly identified viral infections affecting humans. It was recently reported in the Arabian Peninsula (AP), particularly Saudi Arabia. The virus primarily causes respiratory failure in affected patients, but can also sometimes cause renal failure. The main reservoir of this virus is dromedary camels. Although a lot is known about the diseases pattern, pathogenesis, and immunity of MERS-CoV infection in humans, very little is known about these parameters in camels. The main goals of this book chapter are to discuss the current understandings about MERS-CoV infection in animals, particularly the dromedary camels. Special attention should be paid to the clinical pattern of MERS-CoV infection in animals, including clinical signs, pathological changes during virus infection, various methods of clinical and laboratory diagnosis, and the recent advances related to the control of MERS-CoV.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
11.1 Prologue
There are 2458 laboratory-confirmed cases of MERS-CoV reported from 27 countries around the globe (till August 20, 2019). The disease was fatal in about 848 cases (34%) (WHO 2019). Unfortunately, until now, there is no effective medication or even vaccine against MERS-CoV. MERS-CoV represents a good example for the One Health concept (Hemida 2019). The virus infects humans and can cause severe illness in some patients, particularly those suffering from chronic diseases and other comorbidities such as cancer (Rahman and Sarkar 2019). The main known reservoir for the virus is the dromedary camels (Hemida et al. 2017a). MERS-CoV was isolated from dromedary camels in many countries across the Arabian Peninsula such as Saudi Arabia, UAE, Qatar, and Oman (Hemida et al. 2014a; Nowotny and Kolodziejek 2014; Yusof et al. 2015).
However, there is a scarcity of information about the actual natural infection of MERS-CoV in dromedary camels. The main objective of this article was to highlight the most up-to-date knowledge about MERS-CoV in various species of animals with special attention to dromedary camels.
11.2 Historical Background and Evolution of MERS-CoV
MERS-CoV was first identified in a patient from Saudi Arabia who presented with severe respiratory symptoms and later developed respiratory failure (Zaki et al. 2012). A retrospective study confirmed the detection of MERS-CoV in archived patient samples from Jordan (Hijawi et al. 2013). The virus was called novel coronavirus at that time (Zaki et al. 2012). Later on, based on the available epidemiological data, a study group decided to change the name of the virus to ‘Middle East respiratory syndrome’ (MERS-CoV) (de Groot et al. 2013). Initially, there was a debate about the origin of MERS-CoV. Some studies suggested bats as a potential reservoir for the MERS-CoV (Memish et al. 2013). This study sequenced a short fragment from a coronavirus genome collected from bats in Saudi Arabia and found high similarity to the circulating MERS-CoV strains at that time (Memish et al. 2013). Another recent study was conducted in Africa, in Ghana, where the camels tend to live in close contact with various species of bats. This study failed to detect a similar MERS-CoV in bats in these regions (de Groot et al. 2013). Scientists tried to speculate the potential reservoir of this new coronavirus in the Middle East, especially in the Arabian Peninsula. The first seroprevalence study for MERS-CoV in different livestock animals including dromedary camels was conducted in Oman (Reusken et al. 2013). This study revealed that only dromedary camels carried specific antibodies against MERS-CoV in their sera. Since then there have been quite a few reports of new cases coming from the Arabian Peninsula and other parts of Africa (Ali et al. 2017; Deem et al. 2015; Hemida et al. 2014b; Hemida et al. 2013). On the other hand, there are reports of detection of MERS-CoV nucleic acids in many cases in dromedary camels from both the AP and Africa (Hemida et al. 2017a; Hemida et al. 2014a; Yusof et al. 2015; El-Duah et al. 2019). MERS-CoV detected in archived serum samples, dating back to the 1990s, showed higher seroprevalence of MERS-CoV in the tested specimens (Reusken et al. 2013; Hemida et al. 2014b). This may suggest the possibility of the circulation of MERS-CoV in dromedary camels before its actual emergence in human as announced for the first time in 2012 (Zaki et al. 2012).
11.3 Aetiology, Genome Organization, and Classification of MERS-CoV
MERS-CoV belongs to the genus Betacoronavirus in the family Coronaviridae and the order Nidovirales. Betacoronaviruses are further divided into four distinct clades labelled as ‘A-D’ (de Groot et al. 2013). MERS-CoV has been recently classified as one of the members of clade C coronavirus. MERS-CoV genome is a single strand of the positive-sense RNA molecule. The viral genome is close to 30 kilobases in length. The genome is organized as follow (5′UTR, non-structural genes- structural genes- 3′UTR-Poly A tail-3′). The virus genome is characterized by the production of sets of sub-genomic messenger RNAs. The viral genome is flanked by two untranslated regions. Two-third of the 5′ genome is occupied by the non-structural genes called Gene-1. It is composed of two overlapping open reading frames with ribosomal frameshifting site. While, one-third of the genome is occupied by various structural genes, including spike (S), envelope (E), matrix (M), and the nucleocapsid (N). There are some accessory genes scattered across the viral genome (ORF3, ORF4a, ORF4b, ORF5, and ORF8b). One recent study showed that the African lineage of MERS-CoV is distinct from those circulating in the Gulf area. This study showed that African lineages lack ORF4, which is considered to be one of the virulence factors for MERS-CoV. This may explain at least in part why there are no human cases reported in the African countries which have a significant population of dromedary camels (Chu et al. 2018).
11.4 MERS-CoV Receptors and Tropism
MERS-CoV is one of the pneumotropic viruses, which replicates well in the cells of the respiratory tract (Park et al. 2018). It is well known that most coronaviruses utilize their S protein in the process of attachment to the host cells. MERS-CoV uses the S1 protein to attach to the sialic acid in the host cell (Widagdo et al. 2019). Several studies confirmed that dipeptidyl peptidase 4 (DPP4) play an important role in the attachment and tropism identification of MERS-CoV (van Doremalen et al. 2014). This study confirmed the possibility of using the DPP4 receptors in various animal species such as cows, sheep, and goat to establish MERS-CoV infection. This suggests the potential roles of these animals as other possible hosts for MERS-CoV (van Doremalen et al. 2014). However, this study needs further confirmation. Another study showed the involvement of another protein called glucose-regulated protein (GRP-78), in the process of MERS-CoV attachment to the target cells (Chu et al. 2018). This cellular factor may act as a key player in the MERS-CoV tropism and tissue distribution (Chu et al. 2018).
11.5 MERS-CoV Infections in Animals
Some coronaviruses are zoonotic in origin, such as the severe acute respiratory syndrome coronavirus (SARS-CoV). Animals, particularly the Palm Civet cats were the main reservoir for the SARS-CoV (Shi and Hu 2008; Wang and Eaton 2007). Culling of this reservoir and banning its distribution in the public markets contributed substantially in the control and extinction of SARS-CoV (Wang and Eaton 2007). When MERS-CoV emerged, scientists started to look for potential reservoirs in the context of the virus emergence and replication cycle. Several studies were conducted to check various domestic animals that lived in close proximity to confirmed patients, for the presence of MERS-CoV antibodies or nucleic acids (Hemida et al. 2014a; Reusken et al. 2013; Hemida et al. 2014b). Interestingly enough, dromedary camels were the only positive animal for the MERS-CoV (Reusken et al. 2013). Since that time, several research groups started to focus on this line of research and to investigate the roles of MERS-CoV in the transmission cycle of MERS-CoV (Yusof et al. 2015; Xu et al. 2019).
11.6 MERS-CoV in Dromedary Camels
Several studies reported the seroprevalence and virus detection of MERS-CoV in dromedary camels from many countries from Asia and Africa (Yusof et al. 2015; Reusken et al. 2013; Hemida et al. 2014b; Kandeil et al. 2019). Earlier studies showed the high seroprevalence of MERS-CoV in most of the tested camel sera from those two regions in the world. However, animals from Australia were seronegative for the MERS-CoV (Hemida et al. 2014b; Crameri et al. 2015). Another recent study showed the seroconversion of dromedary camels from Canary Island but the absence of virus detection in specimens collected from these group of animals (Gutierrez et al. 2015). MERS-CoV was detected in the body fluids of the infected dromedary camels, especially the nasal and rectal swabs (Hemida et al. 2014a; Yusof et al. 2015; Hemida et al. 2017b).
Meanwhile, high prevalence of MERS-CoV was detected in tissue specimens collected from the upper respiratory tract of dromedary camels (Khalafalla et al. 2015). This was in contrast to absence of the detection of any viral nucleic acids or particles in urine samples collected from camels in Qatar (Farag et al. 2019). It was found that the detection rate of MERS-CoV in naïve camels (less than 2 years old) is much higher than adult animals (Hemida et al. 2017b). This highlights the potential role of the young camels in the transmission of MERS-CoV. Another interesting phenomenon is the susceptibility of dromedary camels to the second round of MERS-CoV infection despite the presence of neutralizing antibodies in their sera (Hemida et al. 2017b). This also explains the high seroprevalence of adult camels to MERS-CoV. Another important study reported the detection of MERS-CoV in apparently normal dromedary camels (Mohran et al. 2016). This highlights the confirmed roles of dromedary camels in the sustainability of MERS-CoV in the environment. Although the role of camels in the transmission/replication cycle of MERS-CoV was confirmed a while ago, until now, there is no clear evidence of MERS-CoV infection in dromedary camels under the natural conditions.
Some studies reported the results of the experimental infection of dromedary camels with MERS-CoV (Adney et al. 2014). These studies reported the course of the MERS-CoV infection in a limited number of animals and the curve of the virus shedding over the time of the experiments (Adney et al. 2014). According to these studies there were no characteristic clinical signs observed after the experimental challenges with MERS-CoV, except for very mild elevation of the body temperature and some mild nasal discharges (Adney et al. 2014). The nasal discharge ranged from very mild serous exudate to purulent and sometimes haemorrhagic (Adney et al. 2014). According to same study, virus shedding from the nasal secretions started in less than one-week post-inoculation (PI) and lasted for up to 35 days PI (Adney et al. 2014). However, no viral shedding was reported in faecal swabs or urine during infection (Adney et al. 2014). Interestingly, very low virus concentration was detected in the exhaled breath from the infected animals (Adney et al. 2014). Post-mortem inspection of these animals revealed that the viral antigens were detected in the upper respiratory tracts, especially nasal passages, trachea, and nasal turbinate bones by the immunohistochemistry technique (IHC) (Adney et al. 2014). However, no signal was detected on the alveolar epithelium (Adney et al. 2014). These studies were quite useful in the determination of the viral tropism and tissue distribution, which explains the pathogenesis of the viral infection in dromedary camels. Meanwhile, seroconversion of the inoculated animals was observed within 14 days PI (Adney et al. 2014).
11.7 MERS-CoV in Other Members of the Family Camelidae
The family Camelidae includes dromedary camels, alpaca, and llama. One recent study showed seroprevalence of alpaca kept in close proximity to dromedary camels in Qatar (Reusken et al. 2016). Another study was conducted to check the status of MERS-CoV in dromedary camels, alpaca, and llama. This study found all swabs were negative while some llama were seropositive indicating an active infection among this species of animals in Israel (David et al. 2018). Based on the susceptibility of alpaca to MERS-CoV infection, one study tested the efficacy of a new MERS-CoV-spike based subunit vaccine in both dromedary camels and alpaca. This study showed the induction of a high level of neutralizing antibodies in sera of the challenged animals, which reduced the titre of virus after challenging (Adney et al. 2019a). Recent studies showed that alpaca is susceptible to experimental infection with MERS-CoV (Crameri et al. 2016). The challenged animals shed the virus in their secretions particularly the nasal tract and showed protection when challenged with the wild virus at the end of the experiment (Crameri et al. 2016).
11.8 MERS-CoV in Other Species of Animals
Earlier studies reported the absence of MERS-CoV antibodies in sera of Bactrian camels from Mongolia (Chan et al. 2015; Miguel et al. 2016). However, one recent study reported high virus shedding in secretions of the MERS-CoV experimentally infected Bactrians (Adney et al. 2019b). This explains the potential role of genetic factors in the susceptibility/resistance of the members of the family Camelidae to the MERS-CoV infection. This line of research requires further studies in future. Previous studies showed the absence of any detectable antibodies of MERS-CoV in sera of other livestock animals such as sheep, goat, cattle, horses, and many other animals (El-Duah et al. 2019; Zohaib et al. 2018). This is in contrast to a recent study conducted in Egypt, Tunisia, and Senegal, which showed the detection of specific antibodies in sera collected from of sheep, goat, and donkeys that lived in close contact with camels from these countries (Kandeil et al. 2019). Furthermore, viral nucleic acids were detected in specimens from sheep, goat, and cattle (Kandeil et al. 2019). This line of research requires large-scale studies to understand the dynamics of MERS-CoV among livestock animals in countries where camels live in close contact with these species of animals.
11.9 Animal Models for MERS-CoV
Since the emergence of MERS-CoV in 2012, there was a great demand in finding some potential animal models. Confirmation of the roles of dromedary camels in the transmission cycle of MERS-CoV increased this demand. This is because of the difficulty in access to dromedary camels in North America and Europe. There is also a scarcity of the animal biosafety, level-3 laboratories that are equipped to adopt large animals, especially camels. Initial trials considered the Syrian hamster as a good animal model for the SARS-CoV research (Schaecher et al. 2008); however, it is not a suitable animal model for MERS-CoV (de Wit et al. 2013). The MERS-CoV experimental infection in the golden Syrian hamster was not successful since the virus neither replicates in various body organs nor produces any detectable immune response or antibodies after infection (de Wit et al. 2013). The wild type mouse is non-susceptible to MERS-CoV infection, but recently a MERS-CoV transgenic mouse was developed by the expression of the human DPP4 receptors (hDPP4) (Agrawal et al. 2015). These transgenic mice developed severe clinical signs after the challenge with MERS-CoV. The infected transgenic mice suffered from ruffled fur, severe respiratory manifestations, and finally death, a few days after infection (Agrawal et al. 2015). Both rhesus macaques and marmosets are susceptible to MERS-CoV infection. Both animals were shown to develop signs similar to humans infected with MERS-CoV, including several lesions on the respiratory tract with pulmonary oedema, haemorrhage, and pneumonia (Yu et al. 2017). Pigs were found to be refractory to MERS-CoV infection. Very low virus titre was detected in challenged animals after infection, suggesting that pigs are not a suitable animal model for MERS-CoV, in contrast to dromedary camels and alpaca.
11.10 Isolation of MERS-CoV
The success of isolating MERS-CoV from clinical specimens collected from human or animal mainly depends on the quality of the collected specimen and its preservation, as well as maintenance, until it is processed in the laboratory. In case of transportation of these specimens from the field to the laboratory, it should be transported on ice and kept cool till it reaches the destination laboratory. Transport medium like foetal bovine sera and antibiotic cocktail should be added to the transport medium containing minimal essential media. Some common cell lines are used in the isolation of MERS-CoV collected from patients or animals, especially Vero cell line (Chan et al. 2014; Park et al. 2016). Successful virus isolation is associated with the induction of cytopathic effects (CPE) on the inoculated cell culture. The observed CPE in case of MERS-CoV isolation is the rounding and detachment of cells from the confluent monolayer sheet within three days from the infection of the cell culture (Chan et al. 2014; Park et al. 2016).
11.11 Laboratory Techniques for the Diagnosis of MERS-CoV
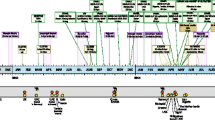
Since the clinical diagnosis of MERS-CoV in dromedary camels is not accurate or even suggestive due to the absence of any pathognomonic clinical signs or post-mortem lesions, laboratory diagnosis is the only way to confirm the presence or absence of MERS-CoV infection in a certain animal. There are two strategies for the diagnosis of MERS-CoV infection in dromedary camels (Fig. 11.1). The first one is the detection of specific viral antibodies in sera of dromedary camels. Several in house and commercial diagnostic antibody detention and titration kits, particularly the enzyme-linked immunosorbent assay (ELISA) are commercially available for MERS-CoV antibodies (Hashem et al. 2019a; Lee et al. 2018; Okba et al. 2019). These tests showed good aptitude in the detection of MERS-CoV in sera of dromedary camels. However, their specificity and sensitivity still need further evaluation. This may be due to the possibility of cross-reactivity that reported between MERS-CoV and other closely related coronaviruses affecting dromedary camels particularly the Bovine coronavirus (Hemida et al. 2014b).
A standard protocol for the laboratory diagnosis of MERS-CoV in animals detection and titration of MERS-CoV antibodies in sera of dromedary camels by commercial or in house ELISA. Confirmation of the ELIA results by the pseudoparticle naturalization assay. Detection and titration of MERS-CoV nucleic acids in swabs (nasal and rectal) collected from animals. Extraction of the viral nucleic acids by standard commercial kits. Detection of the viral nucleic acids by real-time PCR using two targets (up-E and ORF1a). Confirmation of the real-time PCR results by amplification of some viral target genes or the full-length genome by the next-generation sequencing. Revealing the identity of the amplicons can be done by blasting obtained sequences against the available MERS-CoV in the GenBank
Meanwhile, there are some other reliable laboratory accurate techniques used for the detection and quantification of the MERS-CoV specific antibodies in dromedary camel sera. These techniques include, for example, the pseudoparticle neutralization assay (Hemida et al. 2014b). The other strategy is the detection of MERS-CoV infectious virus particles or the viral nucleic acids in the body secretions of the tested animals. The ideal samples for the detecting of the virus or its nucleic acids are the nasal and rectal swabs (Hemida et al. 2014a). There are some quick latex agglutination based tests recently introduced for the quick identification of positive MERS-CoV camels (Kasem et al. 2018). However, these methods are not accurate and prone to false positive/negative results. It is mainly depended on the concentration of the viral antigens in the tested samples. The most accurate technique, considered the gold standard, is the detection of the viral nucleic acids in body secretions by the reverse transcriptase-polymerase chain reactions (RT-PCR) (Hemida et al. 2013). There are many modifications for the RT-PCR technique in the diagnosis of MERS-CoV infection in both humans and animals. One of the robust and user-friendly techniques is the isothermal PCR technique (Shirato et al. 2014). As per the WHO’s instruction, confirmation of active MERS-CoV case depends on the testing of suspected samples by RT-PCR using two different gene targets particularly (up-E and ORF1a) (Corman et al. 2012). The definite diagnosis is the sequencing of the obtained PCR products then blasting the results against the available sequences in the Genebank. Currently, the application of the next-generation sequencing of the partial or the full-length genome is of great value in the diagnosis, classification, and mentoring of changes on the MERS-CoV genomes on the genomic levels (Yusof et al. 2015; Hemida et al. 2013). The application of the IHC techniques to study the antigen localization of the MERS-CoV in various tissues is a good diagnostic approach (Adney et al. 2014).
11.12 Zoonotic Potential of MERS-CoV
MERS-CoV is one of the most important newly emerged viral zoonosis (Azhar et al. 2017). The first observation about the potential zoonotic roles of MERS-CoV was reported in 2014 (Azhar et al. 2014). This study sequenced MERS-CoV from both patients who died from severe pneumonia and from some of the patients’ camels that suffered from mild respiratory signs (Azhar et al. 2014). Sequences from both the patient and camels were identical, suggesting the zoonotic transmission of MERS-CoV from camels to human (Azhar et al. 2014). Since that time, there is an ongoing evaluation of the zoonotic potential of MERS-CoV, particularly in the at-risk group of people who come in close contact with dromedary camels on a daily basis. Although some research failed to detect any specific antibodies for MERS-CoV in sera of people in close contact with positive camel herds (Hemida et al. 2015), some other studies reported the seroprevalence of MERS-CoV in people who came in close contact with dromedary camels in Qatar (Reusken et al. 2015). One large-scale serosurveillance study was conducted across Saudi Arabia to investigate the nationwide prevalence of MERS-CoV in people with a history of close contact experience with dromedary camels. This study showed that 0.15% of tested individuals had antibodies against MERS-CoV (Muller et al. 2015). Another recent study conducted in UAE to assess the risk seroprevalence of MERS-CoV among workers in two slaughterhouses and local camel markets found that around 1.7% of the tested individuals have specific antibodies against MERS-CoV (Adney et al. 2019b). Taking into consideration all these facts, dromedary camels pose some risk to human in the context of MERS-CoV transmission cycle. Further studies are needed to unveil the exact mechanisms of MERS-CoV transmission from camels to humans.
11.13 Control Measures for MERS-CoV
Unfortunately, until now, there is no effective medication or vaccine to treat or prevent MERS-CoV infection in human or animals. The control measures for most viral infections are mainly based on the variability of effective vaccines and the adoption of high standard hygienic measures in both the health care settings and in the farm animals. Implementation of novel strategies based on the One Health concept will help in the reduction of virus shedding from dromedary camels. This will have great benefits on the spillover of MERS-CoV from dromedary camels to human (Hemida and Alnaeem 2019). One of these approaches is the development of novel vaccines against MERS-CoV in dromedary camels. There is some progress in the development and testing of potential vaccines for MERS-CoV in dromedary camels. Some trials have used various approaches to prepare and test these vaccine candidates in laboratory animals as well as in camels. These approaches include some common vaccine strategies such as DNA vaccines, vector-based vaccines, the subunit vaccines, and the viral-like particles based vaccines (Yong et al. 2019). One recent subunit vaccine showed a high degree of protection and reduction in the time of viral shedding in MERS-CoV challenges alpaca and dromedary camels, respectively (Adney et al. 2019a). Several vaccine candidates used the full-length spike protein or its receptor binding domains (RBD) as a base for the preparation of recombinant vaccines against EMRS-CoV (Song et al. 2013; Volz et al. 2015). Several studies used the adenovirus-based recombinant MERS-CoV-S glycoprotein and proved to induce a high level of potent neutralizing antibodies against MERS-CoV (Hashem et al. 2019b; Jia et al. 2019; Kim et al. 2019). Currently, there are two potential MERS-CoV vaccines which have entered the clinical trials phase—the GLS-5300 and the MERS001 (Xu et al. 2019). The other arm of the control measures against MERS-CoV is the implementation of high degree of biosafety precautions among the at-risk people. Those include people who are in daily close contact with dromedary camels, particularly the camel owners, herders, veterinarians, and slaughterhouse personnel (Hemida et al. 2017a).
References
Adney DR, van Doremalen N, Brown VR, Bushmaker T, Scott D, de Wit E et al (2014) Replication and shedding of MERS-CoV in upper respiratory tract of inoculated dromedary camels. Emerg Infect Dis 20(12):1999–2005
Adney DR, Wang L, van Doremalen N, Shi W, Zhang Y, Kong WP et al (2019a) Efficacy of an adjuvanted middle east respiratory syndrome coronavirus spike protein vaccine in dromedary camels and alpacas. Viruses 11(3):E212
Adney DR, Letko M, Ragan IK, Scott D, van Doremalen N, Bowen RA et al (2019b) Bactrian camels shed large quantities of Middle East respiratory syndrome coronavirus (MERS-CoV) after experimental infection. Emerg Microbes Infect 8(1):717–723
Agrawal AS, Garron T, Tao X, Peng BH, Wakamiya M, Chan TS et al (2015) Generation of a transgenic mouse model of Middle East respiratory syndrome coronavirus infection and disease. J Virol 89(7):3659–3670
Ali M, El-Shesheny R, Kandeil A, Shehata M, Elsokary B, Gomaa M et al (2017) Cross-sectional surveillance of Middle East respiratory syndrome coronavirus (MERS-CoV) in dromedary camels and other mammals in Egypt, August 2015 to January 2016. Euro Surveill 22(11):30487
Azhar EI, El-Kafrawy SA, Farraj SA, Hassan AM, Al-Saeed MS, Hashem AM et al (2014) Evidence for camel-to-human transmission of MERS coronavirus. N Engl J Med 370(26):2499–2505
Azhar EI, Lanini S, Ippolito G, Zumla A (2017) The Middle East respiratory syndrome coronavirus—a continuing risk to global health security. Adv Exp Med Biol 972:49–60
Chan RW, Hemida MG, Kayali G, Chu DK, Poon LL, Alnaeem A et al (2014) Tropism and replication of Middle East respiratory syndrome coronavirus from dromedary camels in the human respiratory tract: an in-vitro and ex-vivo study. Lancet Respir Med 2(10):813–822
Chan SM, Damdinjav B, Perera RA, Chu DK, Khishgee B, Enkhbold B et al (2015) Absence of MERS-Coronavirus in Bactrian Camels, Southern Mongolia, November 2014. Emerg Infect Dis 21(7):1269–1271
Chu H, Chan CM, Zhang X, Wang Y, Yuan S, Zhou J et al (2018) Middle East respiratory syndrome coronavirus and bat coronavirus HKU9 both can utilize GRP78 for attachment onto host cells. J Biol Chem 293(30):11709–11726
Corman VM, Muller MA, Costabel U, Timm J, Binger T, Meyer B et al (2012) Assays for laboratory confirmation of novel human coronavirus (hCoV-EMC) infections. Euro Surveill 17(49):20334
Crameri G, Durr PA, Barr J, Yu M, Graham K, Williams OJ et al (2015) Absence of MERS-CoV antibodies in feral camels in Australia: implications for the pathogen’s origin and spread. One Health 1:76–82
Crameri G, Durr PA, Klein R, Foord A, Yu M, Riddell S et al (2016) Experimental infection and response to rechallenge of alpacas with Middle East respiratory syndrome coronavirus. Emerg Infect Dis 22(6):1071–1074
David D, Rotenberg D, Khinich E, Erster O, Bardenstein S, van Straten M et al (2018) Middle East respiratory syndrome coronavirus specific antibodies in naturally exposed Israeli llamas, alpacas and camels. One Health 5:65–68
de Groot RJ, Baker SC, Baric RS, Brown CS, Drosten C, Enjuanes L et al (2013) Middle East respiratory syndrome coronavirus (MERS-CoV): announcement of the Coronavirus Study Group. J Virol 87(14):7790–7792
de Wit E, Prescott J, Baseler L, Bushmaker T, Thomas T, Lackemeyer MG et al (2013) The Middle East respiratory syndrome coronavirus (MERS-CoV) does not replicate in Syrian hamsters. PLoS One 8(7):e69127
Deem SL, Fevre EM, Kinnaird M, Browne AS, Muloi D, Godeke GJ et al (2015) Serological evidence of MERS-CoV antibodies in dromedary camels (Camelus dromedaries) in Laikipia County, Kenya. PLoS One 10(10):e0140125
El-Duah P, Sylverken A, Owusu M, Yeboah R, Lamptey J, Frimpong YO et al (2019) Potential intermediate hosts for Coronavirus transmission: no evidence of Clade 2c Coronaviruses in domestic livestock from Ghana. Trop Med Infect Dis 4(1):E34
Farag E, Haagmans BL, Al Romaihi HE, Mohran KA, Haroun M, El-Sayed AM, Koopmans M, AlHajri M, Reusken CBEM (2019) Failure to detect MERS-CoV RNA in urine of naturally infected dromedary camels. Zoonoses Public Health 66(5):437–438
Gutierrez C, Tejedor-Junco MT, Gonzalez M, Lattwein E, Renneker S (2015) Presence of antibodies but no evidence for circulation of MERS-CoV in dromedaries on the Canary Islands, 2015. Euro Surveill 20(37)
Hashem AM, Al-Amri SS, Al-Subhi TL, Siddiq LA, Hassan AM, Alawi MM et al (2019a) Development and validation of different indirect ELISAs for MERS-CoV serological testing. J Immunol Methods 466:41–46
Hashem AM, Algaissi A, Agrawal A, Al-Amri SS, Alhabbab RY, Sohrab SS et al (2019b) A highly immunogenic, protective and safe adenovirus-based vaccine expressing MERS-CoV S1-CD40L fusion protein in transgenic human DPP4 mouse model. J Infect Dis 220(10):1558–1567
Hemida MG (2019) Middle east respiratory syndrome coronavirus and the one health concept. Peer J 7:e7556
Hemida MG, Alnaeem AA (2019) Some One Health based control strategies for the Middle East respiratory syndrome coronavirus. One Health 8:100102
Hemida MG, Perera RA, Wang P, Alhammadi MA, Siu LY, Li M et al (2013) Middle East respiratory syndrome (MERS) coronavirus seroprevalence in domestic livestock in Saudi Arabia, 2010 to 2013. Euro Surveill 18(50):20659
Hemida MG, Chu DK, Poon LL, Perera RA, Alhammadi MA, Ng HY et al (2014a) MERS coronavirus in dromedary camel herd, Saudi Arabia. Emerg Infect Dis 20(7):1231–1234
Hemida MG, Perera RA, Al Jassim RA, Kayali G, Siu LY, Wang P et al (2014b) Seroepidemiology of Middle East respiratory syndrome (MERS) coronavirus in Saudi Arabia (1993) and Australia (2014) and characterisation of assay specificity. Euro Surveill 19(23):20828
Hemida MG, Al-Naeem A, Perera RA, Chin AW, Poon LL, Peiris M (2015) Lack of middle East respiratory syndrome coronavirus transmission from infected camels. Emerg Infect Dis 21(4):699–701
Hemida MG, Elmoslemany A, Al-Hizab F, Alnaeem A, Almathen F, Faye B et al (2017a) Dromedary camels and the transmission of middle east respiratory syndrome coronavirus (MERS-CoV). Transbound Emerg Dis 64(2):344–353
Hemida MG, Alnaeem A, Chu DK, Perera RA, Chan SM, Almathen F et al (2017b) Longitudinal study of Middle East Respiratory Syndrome coronavirus infection in dromedary camel herds in Saudi Arabia, 2014–2015. Emerg Microbes Infect 6(6):e56
Hijawi B, Abdallat M, Sayaydeh A, Alqasrawi S, Haddadin A, Jaarour N et al (2013) Novel coronavirus infections in Jordan, April 2012: epidemiological findings from a retrospective investigation. East Mediterr Health J 19(Suppl 1):S12–S18
Jia W, Channappanavar R, Zhang C, Li M, Zhou H, Zhang S et al (2019) Single intranasal immunization with chimpanzee adenovirus-based vaccine induces sustained and protective immunity against MERS-CoV infection. Emerg Microbes Infect 8(1):760–772
Kandeil A, Gomaa M, Nageh A, Shehata MM, Kayed AE, Sabir JSM et al (2019) Middle East respiratory syndrome coronavirus (MERS-CoV) in dromedary camels in Africa and Middle East. Viruses 11(8):717
Kasem S, Qasim I, Al-Doweriej A, Hashim O, Alkarar A, Abu-Obeida A et al (2018) The prevalence of Middle East respiratory syndrome coronavirus (MERS-CoV) infection in livestock and temporal relation to locations and seasons. J Infect Public Health 11(6):884–888
Khalafalla AI, Lu X, Al-Mubarak AI, Dalab AH, Al-Busadah KA, Erdman DD (2015) MERS-CoV in upper respiratory tract and lungs of dromedary camels, Saudi Arabia, 2013–2014. Emerg Infect Dis 21(7):1153–1158
Kim MH, Kim HJ, Chang J (2019) Superior immune responses induced by intranasal immunization with recombinant adenovirus-based vaccine expressing full-length Spike protein of Middle East respiratory syndrome coronavirus. PLoS One 14(7):e0220196
Lee K, Ko HL, Lee EY, Park HJ, Kim YS, Kim YS et al (2018) Development of a diagnostic system for detection of specific antibodies and antigens against Middle East respiratory syndrome coronavirus. Microbiol Immunol 62(9):574–584
Memish ZA, Mishra N, Olival KJ, Fagbo SF, Kapoor V, Epstein JH et al (2013) Middle East respiratory syndrome coronavirus in bats, Saudi Arabia. Emerg Infect Dis 19(11):1819–1823
Miguel E, Perera RA, Baubekova A, Chevalier V, Faye B, Akhmetsadykov N et al (2016) Absence of Middle East respiratory syndrome coronavirus in Camelids, Kazakhstan, 2015. Emerg Infect Dis 22(3):555–557
Mohran KA, Farag EA, Reusken CB, Raj VS, Lamers MM, Pas SD et al (2016) The sample of choice for detecting Middle East respiratory syndrome coronavirus in asymptomatic dromedary camels using real-time reversetranscription polymerase chain reaction. Rev Sci Tech 35(3):905–911
Muller MA, Meyer B, Corman VM, Al-Masri M, Turkestani A, Ritz D et al (2015) Presence of Middle East respiratory syndrome coronavirus antibodies in Saudi Arabia: a nationwide, cross-sectional, serological study. Lancet Infect Dis 15(5):559–564
Nowotny N, Kolodziejek J (2014) Middle East respiratory syndrome coronavirus (MERS-CoV) in dromedary camels, Oman. Euro Surveill 19(16):20781
Okba NMA, Raj VS, Widjaja I, Geurts van Kessel CH, de Bruin E, Chandler FD et al (2019) Sensitive and specific detection of low-level antibody responses in mild Middle East respiratory syndrome coronavirus infections. Emerg Infect Dis 25(10):1868–1877
Park WB, Kwon NJ, Choe PG, Choi SJ, Oh HS, Lee SM et al (2016) Isolation of Middle East respiratory syndrome coronavirus from a patient of the 2015 Korean outbreak. J Korean Med Sci 31(2):315–320
Park WB, Poon LLM, Choi SJ, Choe PG, Song KH, Bang JH et al (2018) Replicative virus shedding in the respiratory tract of patients with Middle East respiratory syndrome coronavirus infection. Int J Infect Dis 72:8–10
Rahman A, Sarkar A (2019) Risk factors for fatal middle east respiratory syndrome coronavirus infections in Saudi Arabia: analysis of the WHO line list, 2013–2018. Am J Public Health 109(9):1288–1293
Reusken CB, Haagmans BL, Muller MA, Gutierrez C, Godeke GJ, Meyer B et al (2013) Middle East respiratory syndrome coronavirus neutralising serum antibodies in dromedary camels: a comparative serological study. Lancet Infect Dis 13(10):859–866
Reusken CB, Farag EA, Haagmans BL, Mohran KA, Gert-Jan Godeke V, Raj S et al (2015) Occupational exposure to dromedaries and risk for MERS-CoV infection, Qatar, 2013–2014. Emerg Infect Dis 21(8):1422–1425
Reusken CB, Schilp C, Raj VS, De Bruin E, Kohl RH, Farag EA et al (2016) MERS-CoV infection of Alpaca in a region where MERS-CoV is endemic. Emerg Infect Dis 22(6):1129–1131
Schaecher SR, Stabenow J, Oberle C, Schriewer J, Buller RM, Sagartz JE et al (2008) An immunosuppressed Syrian golden hamster model for SARS-CoV infection. Virology 380(2):312–321
Shi Z, Hu Z (2008) A review of studies on animal reservoirs of the SARS coronavirus. Virus Res 133(1):74–87
Shirato K, Yano T, Senba S, Akachi S, Kobayashi T, Nishinaka T et al (2014) Detection of Middle East respiratory syndrome coronavirus using reverse transcription loop-mediated isothermal amplification (RT-LAMP). Virol J 11:139
Song F, Fux R, Provacia LB, Volz A, Eickmann M, Becker S et al (2013) Middle East respiratory syndrome coronavirus spike protein delivered by modified vaccinia virus Ankara efficiently induces virus-neutralizing antibodies. J Virol 87(21):11950–11954
van Doremalen N, Miazgowicz KL, Milne-Price S, Bushmaker T, Robertson S, Scott D et al (2014) Host species restriction of Middle East respiratory syndrome coronavirus through its receptor, dipeptidyl peptidase 4. J Virol 88(16):9220–9232
Volz A, Kupke A, Song F, Jany S, Fux R, Shams-Eldin H et al (2015) Protective efficacy of recombinant modified Vaccinia virus Ankara delivering Middle East respiratory syndrome coronavirus spike glycoprotein. J Virol 89(16):8651–8656
Wang LF, Eaton BT (2007) Bats, civets and the emergence of SARS. Curr Top Microbiol Immunol 315:325–344
WHO (2019) MERS global summary an assessment of risk. Available on line at: https://www.who.int/emergencies/mers-cov/en/
Widagdo W, Okba NMA, Li W, de Jong A, de Swart RL, Begeman L et al (2019) Species-specific colocalization of middle east respiratory syndrome coronavirus attachment and entry receptors. J Virol 93(16):e00107-19
Xu J, Jia W, Wang P, Zhang S, Shi X, Wang X et al (2019) Antibodies and vaccines against Middle East respiratory syndrome coronavirus. Emerg Microbes Infect 8(1):841–856
Yong CY, Ong HK, Yeap SK, Ho KL, Tan WS (2019) Recent advances in the vaccine development against Middle East respiratory syndrome-coronavirus. Front Microbiol 10:1781
Yu P, Xu Y, Deng W, Bao L, Huang L, Xu Y et al (2017) Comparative pathology of rhesus macaque and common marmoset animal models with Middle East respiratory syndrome coronavirus. PLoS One 12(2):e0172093
Yusof MF, Eltahir YM, Serhan WS, Hashem FM, Elsayed EA, Marzoug BA et al (2015) Prevalence of Middle East respiratory syndrome coronavirus (MERS-CoV) in dromedary camels in Abu Dhabi Emirate, United Arab Emirates. Virus Genes 50(3):509–513
Zaki AM, van Boheemen S, Bestebroer TM, Osterhaus AD, Fouchier RA (2012) Isolation of a novel coronavirus from a man with pneumonia in Saudi Arabia. N Engl J Med 367(19):1814–1820
Zohaib A, Saqib M, Athar MA, Chen J, Sial AU, Khan S et al (2018) Countrywide survey for MERS-coronavirus antibodies in dromedaries and humans in Pakistan. Virol Sin 33(5):410–417
Acknowledgements
The author thanks the King Abdul-Aziz City for Science and Technology (KACST) for their generous funding through the MERS-CoV research grant program (number 20-0004), which is a part of the Targeted Research Program (TRP).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Hemida, M.G. (2020). The Middle East Respiratory Syndrome Coronavirus (MERS-CoV). In: Malik, Y.S., Singh, R.K., Dhama, K. (eds) Animal-Origin Viral Zoonoses. Livestock Diseases and Management. Springer, Singapore. https://doi.org/10.1007/978-981-15-2651-0_11
Download citation
DOI: https://doi.org/10.1007/978-981-15-2651-0_11
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-15-2650-3
Online ISBN: 978-981-15-2651-0
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)