Abstract
Diagnosis of frozen shoulder is based upon the recognition of the characteristic features of the pain and limitation of both active and passive elevation, external rotation, and internal rotation. The macroscopic and histological features of the capsular contracture are well defined; however, the underlying pathological processes remain poorly understood. Furthermore, clearly defined diagnostic criteria are lacking. Contracture may cause protracted disability. Most patients are still managed by medication of nonsteroidal antiinflammatory drugs and physiotherapy in primary care, and only the more refractory cases are referred for specialist intervention. Targeted therapy is not possible, and treatment remains predominantly symptomatic. However, during the past 10 years, more active interventions that may shorten the clinical course, such as manipulation under anesthesia and arthroscopic capsular release, have become more popular.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Frozen shoulder
- Manipulation under anaesthesia
- Arthroscopic capsular release
- Continuous passive motion machine
13.1 Introduction
Frozen shoulder is a common disorder in orthopedic practice, characterized by pain in the shoulder and physical restriction of movements of the glenohumeral joint. Frozen shoulder is a term coined by Codman in 1934 [1], who described the common features of a slow onset of pain felt near the insertion of the deltoid muscle, inability to sleep on the affected side with restriction in both active and passive elevation and external rotation, yet with normal radiographic appearance. Synonyms include pe’riarthrite scapulohume’rale [2] and adhesive capsulitis [3]. Although identification of the syndrome rests on the recognition of characteristic clinical features, clearly defined diagnostic criteria are lacking. Frozen shoulder may arise spontaneously without an obvious preceding cause, or may be associated with local or systemic disorders. The need for detection in diagnosis has recently been emphasized, and a system of terminology and classification based on consensus would be advantageous. A survey of the members of the British Elbow and Shoulder Society overwhelmingly agreed with the definition of frozen shoulder as seen in Table 13.1 [4]. In the United States, Zuckerman proposed to classify frozen shoulder into primary and secondary, and subdivided secondary frozen shoulder into intrinsic, extrinsic, and systemic ones [5] (Table 13.2). Diabetes mellitus is the condition most commonly associated with frozen shoulder, secondary systemic frozen shoulder. Diabetics have a 10–20 % lifetime risk of developing a frozen shoulder [6], with a risk two to four times greater than the general population [7].
13.2 Natural History
Many studies suggest that frozen shoulder is a benign condition, passing through phases of pain, pain and stiffness, stiffness and resolution, and typically leading to a functional recovery after 2–3 years [8, 9]. However, it is now accepted that up to 50 % of patients continued to have mild pain or stiffness 7 years after the initial symptoms as well as a deficit in shoulder range of motion compared with the contralateral shoulder [10]. It is estimated that approximately 7–15 % have some degree of permanent loss of movement, although few have persistent functional disability [11].
13.3 Pathology
The most common cause of painful restriction of movement is an idiopathic frozen shoulder, which is characterized by an inflammatory contracture of the capsule and ligaments, which reduces the available intraarticular volume, limiting glenohumeral movement. Macroscopically, the capsule has a glassy appearance with acute vasculitis, inflammation, and thickening, progressing to a more indolent fibrotic appearance with time.
Ide and Takagi reported intraarticular findings at arthroscopic capsular release [12]. All 42 patients (44 shoulders) manifested reduced intraarticular volume and highly vascular papillary infolding of the synovium (Fig. 13.1). Pathological findings, categorized as traumatic and nontraumatic frozen shoulder, are shown in Table 13.3. Regardless of etiology, all shoulders had similar intraarticular findings. After capsular release, capsule thickening was observed. The pathology of this condition is a soft tissue fibrosing and inflammation. There are no ‘adhesions’ within the joint. Future studies should be directed to give light on the initiator of inflammation, as well as of fibrosis, with the final aim to better treat or prevent frozen shoulder.
Histological examinations of synovial and capsular biopsies in patients with frozen shoulder demonstrate synovial hyperplasia with a normal underlying capsule (Fig. 13.2).
13.4 Imaging
Radiographic appearance is normal in patients with frozen shoulder. Anteroposterior radiograph in active elevation indicates that there is no glenohumeral joint movement (Fig. 13.3). The decrease of joint volume at arthrography indicates shortening of the joint capsule (Fig. 13.4). Magnetic resonance imaging (MRI) can detect thickening of the joint capsule. particularly in the axillary region [13, 14]. MRI also demonstrates thickening of the coracohumeral ligament [15]. MR arthrography may show obliteration of the subcoracoid fat triangle, resulting from shortening or fibrosis of the rotator interval capsule [15, 16]. Using dynamic MRI enhanced with intravenous gadolinium administration, Tamai et al. [17] demonstrated a greater increase of signal intensity in the glenohumeral joint synovium in frozen shoulder. This finding indicates an increased perfusion of gadolinium from the vessels to the synovium, which most probably is the result of synovial inflammation. The bone mineral density usually returns to near normal with the improvement of clinical symptoms [18]. A bone scan generally shows positive, which indicates increased local blood flow in frozen shoulder [19].
13.5 Conservative Treatment
The goal of treatment is to relieve pain, restore movement, and regain function of the shoulder. There are many alternative forms of treatment for this condition, but evidence of their efficacy is not well established from clinical trials [20], and it is unclear if several interventions used in combination are better.
13.5.1 Physiotherapy
A recent Cochrane review concluded that the existing literature was insufficient to prove that physiotherapy alone was beneficial, with two small clinical trials concluding that physiotherapy alone did not offer any benefit when compared with no-treatment controls [21].
13.5.2 Steroid Injection
Although some studies have shown improvement with intraarticular steroid injection, others have found that this treatment produces little benefit [22]. A recent meta-analysis showed little evidence of benefit from steroid injection [23]. Steroid injections appear to provide earlier relief from pain, when compared with placebo, but whether this is sustained in the long term is unknown.
13.5.3 Distension Arthrography
This local anesthetic has the advantage of producing rapid improvement in movement, without recourse to a more interventional surgical procedure. Under fluoroscopic control, an arthrogram is initially performed to exclude a rotator cuff tear. The diagnosis of frozen shoulder is supported by the characteristic arthrographic appearance of a contracted capsule. Sterile water is then injected under pressure sufficient to cause capsular rupture. Data from a small placebo-controlled trial suggested that arthrographic distension provides significant short-term benefit, which is maintained in the medium term [24]. Further comparative studies are required to evaluate the efficacy of this technique.
13.5.4 Manipulation Under Anaesthesia
Manipulation under anesthesia (MUA) has been used extensively if physiotherapy fails. It has been successfully used alone or combined with a steroid injection or with an arthroscopic capsular release, and usually results in a rapid return of movement of the shoulder [25].
13.6 Surgical Treatment
My indications for arthroscopic treatment of shoulder stiffness are as follows [12]: limitation of active and passive range of motion, pain and dysfunction, at least 6 weeks of conservative treatment without progress, and symptoms for at least 3 months. Patients were subjected to arthroscopic capsular release if a closed manipulation did not restore at least 80 % of the range of motion of the normal, contralateral shoulder in all planes. It is my opinion that the major role of an arthroscopic treatment for shoulder stiffness is fast recovery and long-term efficacy.
I released the capsule using electrocautery from the anterior portal after diagnostic arthroscopy from the posterior portal in the lateral position. I did not release the whole portion of the capsule, especially the inferior portion, if adequate range of motion was restored. A release of the superior and middle glenohumeral ligaments, the rotator interval, the coracohumeral ligament extraarticularly, or the intraarticular portion of the subscapularis was performed for loss of external rotation; a release of the anterior-inferior capsule including the anterior band of the inferior glenohumeral ligament was performed for loss of elevation; and a posterosuperior capsular release was performed for loss of internal rotation [12] (Fig. 13.5).
Arthroscopic capsular release. Cadaveric specimen demonstrating capsular release (red line). Using electrocautery, we released the capsule including the superior glenohumeral ligament (SGHL) rotator interval, the middle glenohumeral ligament (MGHL), the anterior band of the inferior glenohumeral ligament (IGHL), the coracohumeral ligament extraarticularly, and/or the intraarticular portion of the subscapularis (SubS). To avoid axillary nerve injury, we did not release the inferior portion of the IGHL
Preoperative pain and function of the shoulder joints in my patients were significantly improved at 4 weeks after the operation, and 91 % continued to be in good condition for a mean of 7.5 years [12]. There were no complications related to the arthroscopic procedure. I recommend selective arthroscopic capsular release for shoulder stiffness for which physiotherapy and manipulation under anesthesia have failed.
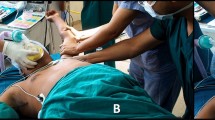
Intensive rehabilitation should begin immediately postoperatively with daily stretching exercises. Continuous passive motion (CPM) machines may also be useful to maintain movement, although controversy persists concerning the use of CPM machine exercise in patients with restricted shoulder motion. CPM exercise may be useful in retaining the range of motion of the shoulder joint after restoring it by arthroscopic capsular release [12]. The CPM machine design in this study provides for external and internal rotating motion of the shoulder joint in abduction in the supine position, which supports scapular stability (Fig. 13.6).
The extent of capsular release depends on clinical judgement: some authors have advocated routinely performing a ‘360-degree’ release [26], whereas others have adopted a more cautious approach [12, 27, 28]. Le Lievre and Murrell reported that shoulder range of motion at 7 years after 360° arthroscopic capsular release in patients with idiopathic adhesive capsulitis was equivalent to that in the contralateral shoulder, in contrast to results reported for nonoperative treatment [29]. Further investigation is needed to determine the optimal extent of the release.
References
Codman EA (1934) The shoulder. G. Miller, New York, pp 216–224
Duplay ES (1872) De la pe’riarthrite scapulohume’rale et des raideurs de l’epaule qui en son la consequence. Arch Gen Med 20:513–542
Neviaser JS (1945) Adhesive capsulitis of the shoulder. J Bone Joint Surg 27:211–222
Bunker TD, Schranz PJ (1998) Clinical challenges in orthopaedics: the shoulder. ISIS Medical Media, Oxford
Zuckerman JD, Rokito A (2011) Frozen shoulder: a consensus definition. J Shoulder Elbow Surg 20:322–325
Bridgman JF (1972) Periarthritis of the shoulder and diabetes mellitus. Ann Rheum Dis 31:69–71
Tighe CB, Oakley WS Jr (2008) The prevalence of a diabetic condition and adhesive capsulitis of the shoulder. South Med J 101:591–595
Grey RG (1978) The natural history of “idiopathic” frozen shoulder. J Bone Joint Surg Am 60:564
Reeves B (1975) The natural history of the frozen shoulder syndrome. Scand J Rheumatol 4:193–196
Shaffer B, Tibone JE, Kerlan RK (1992) Frozen shoulder. A long-term follow-up. J Bone Joint Surg Am 74:738–746
Binder AI, Bulgen DY, Hazleman BL, Roberts S (1984) Frozen shoulder: a long-term prospective study. Ann Rheum Dis 43:361–364
Ide J, Takagi K (2004) Early and long-term results of arthroscopic treatment for shoulder stiffness. J Shoulder Elbow Surg 13:174–179
Emig EW, Schweitzer ME, Karasick D, Lubowitz J (1995) Adhesive capsulitis of the shoulder. MR diagnosis. Am J Roentgenol 164:1457–1459
Gokalp G, Algin O, Yildirim N, Yazici Z (2011) Adhesive capsulitis: contrast-enhanced shoulder MRI findings. J Med Imaging Radiat Oncol 55:119–125
Gokalp MB, Pfirrmann CW, Gerber C, Hodler J, Zanetti M (2004) Frozen shoulder: MR arthrographic findings. Radiology 233:486–492
Zhao W, Zheng X, Liu Y, Yang W, Amirbekian V, Diaz LE, Huang X (2012) An MRI study of symptomatic adhesive capsulitis. PLoS One 7:e47277
Tamai K, Yamato M (1997) Abnormal synovium in the frozen shoulder. A preliminary report with dynamic magnetic resonance imaging. J Should Elbow Surg 6:534–543
Müller LP, Müller LA, Happ J, Kerschbaumer F (2000) Frozen shoulder: a sympathetic dystrophy? Arch Orthop Trauma Surg 120:84–87
Senocak O, Degirmenci B, Ozdogan O, Akalin E, Arslan G, Kaner B, Tasci C, Peker O (2002) Technetium-99m human immunoglobulin scintigraphy in patients with adhesive capsulitis: a correlative study with bone scintigraphy. Ann Nucl Med 16:243–248
Rookmoneea M, Dennis L, Brealey S et al (2010) The effectiveness of interventions in the management of patients with primary frozen shoulder. J Bone Joint Surg Br 92:1267–1272
Green S, Buchbinder R, Hetrick S (2003) Physiotherapy interventions for shoulder pain. Cochrane Database Syst Rev 2:CD004258
Robinson CM, Seah KT, Chee YH, Hindle P, Murray IR (2012) Frozen shoulder. J Bone Joint Surg Br 94:1–9
Buchbinder R, Green S, Youd JM (2003) Corticosteroid injections for shoulder pain. Cochrane Database Syst Rev 1:CD004016
Buchbinder R, Hoving JL, Green S, Hall S, Forbes A, Nash P (2004) Short course prednisolone for adhesive capsulitis (frozen shoulder or stiff painful shoulder): a randomised, double blind, placebo controlled trial. Ann Rheum Dis 63:1460–1469
Thomas WJ, Jenkins EF, Owen JM, Sangster MJ, Kirubanandan R, Beynon C, Woods DA (2011) Treatment of frozen shoulder by manipulation under anaesthetic and injection: does the timing of treatment affect the outcome? J Bone Joint Surg Br 93:1377–1381
Jerosch J (2001) 360 degrees arthroscopic capsular release in patients with adhesive capsulitis of the glenohumeral joint: indication, surgical technique, results. Knee Surg Sports Traumatol Arthrosc 9:178–186
Harryman DT 2nd (1993) Shoulders: frozen and stiff. Instr Course Lect 42:247–257
Warner JJ, Allen A, Marks PH, Wong P (1996) Arthroscopic release for chronic, refractory adhesive capsulitis of the shoulder. J Bone Joint Surg Am 78:1808–1816
Le Lievre HM, Murrell GA (2012) Long-term outcomes after arthroscopic capsular release for idiopathic adhesive capsulitis. J Bone Joint Surg Am 94:1208–1212
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer Japan
About this chapter
Cite this chapter
Ide, J. (2016). Frozen Shoulder. In: Tamai, K., Itoi, E., Takagishi, K. (eds) Advances in Shoulder Surgery. Springer, Tokyo. https://doi.org/10.1007/978-4-431-55988-7_13
Download citation
DOI: https://doi.org/10.1007/978-4-431-55988-7_13
Published:
Publisher Name: Springer, Tokyo
Print ISBN: 978-4-431-55986-3
Online ISBN: 978-4-431-55988-7
eBook Packages: MedicineMedicine (R0)