Abstract
Cerebral iron overload causes brain injury after intracerebral hemorrhage (ICH) in rats and pigs. The current study examined whether an iron chelator, deferoxamine, can reduce ICH-induced DNA damage in pigs. Pigs received an injection of autologous blood into the right frontal lobe. Deferoxamine (50 mg/kg, i.m.) or vehicle was given 2 h after ICH and then every 12 h up to 7 days. Animals were killed at day 3 or day 7 after ICH to examine iron accumulation and DNA damage. We found that ICH resulted in the development of a reddish perihematomal zone, with iron accumulation and DNA damage within that zone. Deferoxamine treatment reduced the perihematomal reddish zone, and the number of Perls’ (p < 0.01) and TUNEL (p < 0.01) positive cells. In conclusion, iron accumulates in the perihematomal zone and causes DNA damage. Systemic deferoxamine treatment reduces ICH-induced iron overload and DNA damage in pigs.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Iron accumulation occurs in the brain after intracerebral hemorrhage (ICH) and results in brain injury [1–3]. Iron-induced brain injury including DNA damage may result from oxidative stress [4, 5]. Terminal deoxynucleotidyl transferase-mediated dUTP nick end-labeling (TUNEL) is a DNA injury marker that is often used to detect double-strand DNA damage [4].
Deferoxamine (DFX), an iron chelator, is a FDA-approved drug for the treatment of acute iron intoxication and chronic iron overload due to transfusion-dependent anemia. DFX reduces brain edema, neuronal death and neurological deficits following ICH in rats [6–8]. DFX also reduces hemorrhagic transformation in a rat model of cerebral ischemia [9].
The current study examined whether systemic DFX treatment reduces brain iron accumulation and DNA damage in a pig model of ICH.
Materials and Methods
Animal Preparation, Intracerebral Infusion and DFX Treatment
Animal use protocols were approved by the University of Michigan Committee on the Use and Care of Animals. Male pigs (8–10 kg, Michigan State University) were sedated with ketamine (25 mg/kg, i.m.) and anesthetized with isoflurane. After a surgical plane of anesthesia was reached, animals were orotracheally intubated. The right femoral artery was catheterized for monitoring of blood pressure, blood gases and glucose concentrations. Body temperature was maintained at 37.5 ± 0.5°C.
A cranial burr hole (1.5 mm) was drilled 11 mm to the right of the sagittal and 11 mm anterior to the coronal suture. A 20-gauge sterile plastic catheter was then placed stereotaxically into the center of the right frontal cerebral white matter and cemented in place. Silicone elastomer tubing connected to the arterial catheter was filled with 5 mL of autologous arterial blood. An infusion pump was connected, and 1.0 mL of whole blood was injected over 15 min. After a 5 min break, another 1.5 mL of whole blood was injected over 15 min [10].
Brain Histology
Pigs were treated with DFX (50 mg/kg; i.m., given at 2 h after ICH and then every 12 h for up to 7 days) or vehicle. Pigs were reanesthetized on day 3 or day 7, and the brains perfused with 10% formalin. Paraffin-embedded brain was cut coronally into 10-μm-thick sections.
Enhanced Perls’ Staining
Enhanced Perls’ staining was performed to detect iron accumulation [11]. Paraffin sections were deparaffinized in xylol and alcohols of descending concentration, rinsed in distilled water, and incubated in Perls’ Prussian blue staining solution (1:1, 5% potassium ferrocyanide/5% hydrochloric acid) for 45 min, followed by washing with distilled water. The sections were then incubated in 0.5% diamine benzidine tetrahydrochloride with nickel for 45 min.
Immunohistochemistry
Ferritin was examined by immunohistochemistry. The primary antibody was polyclonal rabbit anti-human ferritin IgG (DACO, 1:400 dilution). Normal rabbit IgG was used as a negative control.
Terminal Deoxynucleotidyl Transferase-Mediated dUTP Nick End-Labeling (TUNEL)
TUNEL staining was performed using a ApopTag Peroxidase Kit (Intergen). First, 3% hydrogen peroxide in 0.1MPBS was applied to sections for 5 min to quench endogenous peroxidases. After washing with PBS and equilibrating with the solution supplied, the specimens were incubated with TdT enzyme at 37°C for 1 h. The reaction was stopped by washing with buffer for 10 min. Anti-digoxingenin peroxidase conjugate was then applied to the slide for 30 min at room temperature. 3,3′ diaminobenzidine (DAB) was used for visualization. Omission of the terminal deoxynucleotidyl transferase was used as the negative control.
Photography for Cell Counting
Light microphotographs (×40, 4 fields from each distance) were taken at 200, 500 and 1,000 μm from the edge of the hematoma.
Statistical Analysis
Data from different animal groups and brain sites were expressed as mean ± SD and analyzed by Student’s t-test. Differences were considered significant at p < 0.05.
Results
ICH resulted in the development of a reddish zone around the clot in pigs at day 3 and 7. Systemic DFX treatment reduced this reddish zone (Fig. 1). There were many Perls’-positive cells in the reddish zone, and DFX also reduced the number of these cells (p < 0.01).
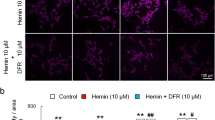
Ferritin was upregulated in the perihematomal area. Ferritin-positive cells around the hematoma were glia-like (Fig. 2). Most ferritin-positive cells were detected immediately next to the clot. There were fewer ferritin-positive cells in DFX-treated compared to vehicle-treated pigs (Fig. 2).
Ferritin-positive cells in the perihematoma zone at different distances away from the edge of hematoma at day 7 after ICH. (a, b) 200 μm, (c, d) 500 μm and (e, f) 1,000 μm from the hematoma edge. The rats were treated by vehicle (a, c, e) or deferoxamine (b, d, f). Scale bar = 50 μm. (g) Quantification of ferritin-positive cells. Values are means ± SD, #p < 0.01 vs. ICH + Vehicle
TUNEL staining was used to detect DNA damage in the brain. TUNEL-positive cells were found in the vicinity of the clot (Fig. 3). DFX treatment reduced the number of TUNEL-positive cells around the hematoma (p < 0.01, Fig. 3).
TUNEL staining in the perihematoma zone at different distances away from the edge of the hematoma 3 days after ICH. (a, b) 200 μm, (c, d) 500 μm and (e, f) 1,000 μm from the edge. Rats were treated with vehicle (a, c, e) or deferoxamine (b, d, f). Scale bar = 50 μm. (g) Quantification of TUNEL-positive cells. Values are means ± SD, *p < 0.05, #p < 0.01 vs. ICH + Vehicle
Discussion
This study found that systemic DFX treatment reduces perihematomal iron accumulation and DNA damage in pigs. Our previous studies found that DFX is neuroprotective and can reduce brain edema and atrophy after ICH in young and aged rats [6–8]. DFX has protective effects in ICH models in two species (rats and pigs), as well as in young and aged animals, suggesting that DFX may also work in humans.
DNA damage was found in the perihematomal zone in pigs. Two pathways that can result in DNA damage are endonuclease-mediated DNA fragmentation and oxidative injury [12]. It is well known that reactive oxygen species can attack DNA directly, forming oxidative base damage and strand breaks [13], and that DNA damage by reactive oxygen species can be greatly amplified in the presence of free iron [14]. Our previous study showed that oxidative stress is a major cause of DNA damage in a rat model of ICH [4]. The current results suggest that iron released from the clot can cause DNA damage in pigs.
Iron overload following ICH is toxic to the brain. The duration over which clot lysis and iron release occurs is likely to be dependent on hematoma size. Our former data in rats [6–8] and present results in pigs show that DFX is effective in reducing brain injury in different ICH models with different sizes of clots.
In conclusion, iron accumulation occurs in the pig brain, and systemic DFX treatment reduces ICH-induced DNA damage.
References
Wagner KR, Sharp FR, Ardizzone TD, Lu A, Clark JF (2003) Heme and iron metabolism: role in cerebral hemorrhage. J Cereb Blood Flow Metab 23:629–652
Wu G, Xi G, Hua Y, Sagher O (2010) T2* Magnetic resonance imaging sequences reflect brain tissue iron deposition following intracerebral hemorrhage. Transl Stroke Res 1:31–34
Xi G, Keep RF, Hoff JT (2006) Mechanisms of brain injury after intracerebral hemorrhage. Lancet Neurol 5:53–63
Nakamura T, Keep RF, Hua Y, Hoff JT, Xi G (2005) Oxidative DNA injury after experimental intracerebral hemorrhage. Brain Res 1039:30–36
Nakamura T, Kuroda Y, Yamashita S, Zhang X, Miyamoto O, Tamiya T, Nagao S, Xi G, Keep RF, Itano T (2008) Edaravone attenuates brain edema and neurologic deficits in a rat model of acute intracerebral hemorrhage. Stroke 39:463–469
Hua Y, Nakamura T, Keep RF, Wu J, Schallert T, Hoff JT, Xi G (2006) Long-term effects of experimental intracerebral hemorrhage: the role of iron. J Neurosurg 104:305–312
Nakamura T, Keep R, Hua Y, Schallert T, Hoff J, Xi G (2004) Deferoxamine-induced attenuation of brain edema and neurological deficits in a rat model of intracerebral hemorrhage. J Neurosurg 100:672–678
Okauchi M, Hua Y, Keep RF, Morgenstern LB, Schallert T, Xi G (2010) Deferoxamine treatment for intracerebral hemorrhage in aged rats: therapeutic time window and optimal duration. Stroke 41:375–382
Xing Y, Hua Y, Keep RF, Xi G (2009) Effects of deferoxamine on brain injury after transient focal cerebral ischemia in rats with hyperglycemia. Brain Res 1291:113–121
Xi G, Wagner KR, Keep RF, Hua Y, de Courten-Myers GM, Broderick JP, Brott TG, Hoff JT (1998) The role of blood clot formation on early edema development following experimental intracerebral hemorrhage. Stroke 29:2580–2586
Wu J, Hua Y, Keep RF, Nakamura T, Hoff JT, Xi G (2003) Iron and iron-handling proteins in the brain after intracerebral hemorrhage. Stroke 34:2964–2969
Graham SH, Chen J (2001) Programmed cell death in cerebral ischemia. J Cereb Blood Flow Metab 21:99–109
Nagayama T, Lan J, Henshall DC, Chen D, O’Horo C, Simon RP, Chen J (2000) Induction of oxidative DNA damage in the peri-infarct region after permanent focal cerebral ischemia. J Neurochem 75:1716–1728
Aruoma OI, Halliwell B, Dizdaroglu M (1989) Iron ion-dependent modification of bases in DNA by the superoxide radical-generating system hypoxanthine/xanthine oxidase. J Biol Chem 264:13024–13028
Acknowledgment
This study was supported by grants NS-017760, NS-039866, NS-052510 and NS-057539 from the National Institutes of Health (NIH) and 0840016N from the American Heart Association (AHA). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH and AHA. Dr. Gu was supported by a grant 30700864 from the China National Natural Science Foundation.
Conflict of interest statement We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2011 Springer-Verlag/Wien
About this chapter
Cite this chapter
Gu, Y. et al. (2011). Iron Accumulation and DNA Damage in a Pig Model of Intracerebral Hemorrhage. In: Zhang, J., Colohan, A. (eds) Intracerebral Hemorrhage Research. Acta Neurochirurgica Supplementum, vol 111. Springer, Vienna. https://doi.org/10.1007/978-3-7091-0693-8_20
Download citation
DOI: https://doi.org/10.1007/978-3-7091-0693-8_20
Published:
Publisher Name: Springer, Vienna
Print ISBN: 978-3-7091-0692-1
Online ISBN: 978-3-7091-0693-8
eBook Packages: MedicineMedicine (R0)