Abstract
For molars that cannot be successfully treated with nonsurgical procedures, endodontic microsurgery may offer a promising alternative. This approach relies on technology, such as the operating microscope, ultrasonic instruments, filling materials, knowledge and manual skills on microsurgery, and guided bone regeneration techniques, all in a structured approach. This process includes a thorough diagnostic workup including a CBCT scan, a sequence of planned treatment steps, and appropriate outcome assessment. In the hands of a skilled operator, endodontic microsurgery enjoys high success rates.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Microsurgery
- Operating microscope
- Calcium silicate cement
- Apicoectomy
- Intentional replantation
- Soft tissue management
- Guided bone regeneration
Setzer FC, Shah SB, Kohli MR, Karabucak B, Kim S. Outcome of endodontic surgery: a meta-analysis of the literature-part 1: comparison of traditional root-end surgery and endodontic microsurgery. J Endod. 2010;36:1757–65.
This study investigated the outcome of root-end surgery, specifically when comparing traditional root-end surgery and endodontic microsurgery. The latter was defined to include ultrasonic preparation and filling materials as well as microsurgical instruments, high-power magnification, and illumination. A meta-analysis based on 21 studies indicated that the application of modern microsurgical methods resulted in 95 % success, while traditional methods achieved success only on 59 % of the cases. Therefore, the use of microsurgical techniques is superior for root-end surgery when compared with traditional techniques.
10.1 Introduction
As discussed previously in Chaps. 8 and 9, failing endodontic treatments are based in principle on the percolation of bacteria or their by-products from inside the root canal system to the periodontium, where interaction with the host immune system occurs. Therefore, success is related to clinical strategies and techniques that prevent this interaction [1].
Nonsurgical retreatment may provide acceptable clinical outcomes; however, this is only realistic when the clinician can overcome procedural errors that prevent thorough disinfection [2]. Surgical endodontics is then often the last opportunity to save a tooth; the decision to perform a surgery should only be made after all previous nonsurgical attempts have failed or are not feasible. The ultimate goal of endodontic microsurgery is the predictable regeneration of periapical tissues and osseous defects [3]; clinical outcomes with this strategy are clearly superior to conventional apical surgery [4].
10.2 Rationale for Endodontic Microsurgery
This treatment provides healing outcomes when spaces of the root canal system that harbor microorganisms can be readily identified, debrided, and filled with a biocompatible material.
To this end and in brief, surgical access to the involved root apices is gained and 3 mm of the respective apex is resected under magnification. The granulation tissues are then removed. A retrocavity of 3 mm depth is adequately prepared and sealed with a biocompatible material in each of the sectioned roots. The need of guided bone regeneration techniques must be evaluated before suturing the flap back in place.
10.3 Diagnostic Steps Before Endodontic Microsurgery
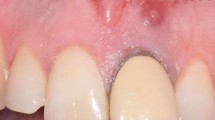
Periodontal probing has to be performed for teeth in the areas as it informs about the profile of the bony crest all around the molar, and most importantly, the width and length of any discontinuity of it (Fig. 10.1).
Classic radiographic techniques like periapical and panoramic radiographs are limited in detecting few periapical bone lesions and therefore cone beam computed tomography (CBCT) [5] is now the standard radiographic technique used to prepare a treatment plan in surgical endodontics (see Box 10.1).
Box 10.1. Diagnosis of Bony Defects
Findings | |||||
|---|---|---|---|---|---|
Type of defect | Extent | Periodeontal probing | Radiographic | CBCT | GBR/membrane recommended |
Small | Normal | Yes | Yes | No | |
“Endo” | Large | Normal | Yes | Yes | No |
Through-and-through | Normal | No | Yes | Yes | |
“Endo-Perio” | Apicomarginal | Deep | No | Yes | Yes |
Large periapical | Normal | Yes | Yes | Yes | |
Combinations | Large periapical or lateroradicular and Through-and-through | Normal | Yes | Yes | Yes |
Combinations | Apicomarginal and Through-and-through | Deep | No | Yes | Yes |
10.4 Endodontic Microsurgery Step by Step
10.4.1 Flap Design
Similar to the access cavity in nonsurgical endodontics, which provides access to canal entries and makes the treatment feasible, flap design is the “access cavity” at the soft tissue level that allows good visibility to the bone level. It is also extremely important because it must allow sufficient blood supply to the mobilized and nonmobilized soft tissues [6–10].
Also, all factors, possible incidents, and modifications of the ongoing microsurgery must be taken into consideration before the first incision is made. Therefore, when facing an apicomarginal bone defect, the flap design should be made large enough in order to have the bone donor site under the same flap, moreover, it must allow covering of the bone graft without tension on the flap [11].
Modifications to the flap after the incisions have been made can jeopardize the final result.
Rectangular and triangular flaps are the typical designs for microsurgery in the molar region. The first flap consists of one horizontal sulcular incision and two vertical ones; while the triangular one is similar, but with only one vertical incision.
“The golden rules of the flap design” [12] are critical factors the clinician must pay attention to them all the time, in order to perform an easy, fast microsurgery with less complicated post-op for the patient:
-
The incision must never cross a bone defect. Incisions should be made away from the lesion if possible.
-
Releasing incisions between bone eminences should be over concave bone surfaces and should never cross over convex bone eminences.
-
The end of a vertical incision at the gingival crest should finish at the angular line of the tooth (black line in Fig. 10.2a), perpendicular to the gingival margin (Fig. 10.2b). The other end should never enter into the mucobuccal fold, so a little inclination of the incision (blue line in Fig. 10.2a) is advantageous.
Fig. 10.2 (a) The incision (black line) must never finish on thin buccal tissue or in the center line of the papilla, as this can compromise the fine vascularization and may cause tissue necrosis with a poor esthetic result. The incision can be tilted minimally (blue line) without crossing the next alveolar bone eminence, in order to open the angle and to keep the incision in attached gingiva. It is advantageous to keep the end incision within the attached gingiva and 1–2 mm away from the mucosa. (b) Placing the incision perpendicular to the marginal gingiva toward the base of the papilla is critical to create space for a stitch that will keep the position of the gingival margin stable during the healing process
-
The base must be as wide as its free edge. Vertical releasing incisions should follow the direction of the vascularization network, which is oriented mainly perpendicular to the occlusal plane in corono-apical direction [13]. Flap blood perfusion is maintained up to the point where the ratio of length to width of the rectangular flap equals 2:1 [14, 15]. Ideally, the shorter the vertical incisions, the larger the horizontal one should be; likewise, the longer the vertical incisions, the shorter the horizontal one.
-
The periosteum must be raised all together with the flap. This makes the suturing procedure easier and speeds up the healing process, diminishing postoperative pain and inflammation.
-
The retractor must always rest on bone, never on soft tissues.
-
All sutures must start by needle insertion through the upper surface of the released tissue, before passing it through the lower surface of the unreleased tissue.
10.4.2 Incision (Low-Power Magnification)
Standard #15 or #15C blades or microsurgical scalpel blades are used and the “Pencil hold” is the most used hand position (Fig. 10.3a, b). Incisions should be made with a firm and continuous movement of the blade at 90° to the bone so that a full mucoperiostal flap is elevated.
(a) Incisions may be made perpendicularly to bone with a conventional scalpel. Alternatively, a microscalpel (b) may be used when making the incision under the microscope. (c) Prichard or Molt curettes are appropriate to initiate flap elevation. (d) Elevation may be started by inserting the elevator at the junction of the vertical and horizontal incisions; vertical force is then applied with a slow, firm, and controlled peeling motion, following closely the cortical bone contour, in order to release the flap to a level completely revealing the extent of the osseous lesion
10.4.3 Elevation of the Flap
The purpose of this step is to raise the already cut flap to allow visibility of the bone. The flap should be elevated in such a way that, when back in place, it will rest passively in the desired position. A sharp, small, straight, or curved elevator, for example Molt 9, P145S, P9HM, or similar (Fig. 10.3c), is placed at the junction of the horizontal and vertical incisions, with its concave surface against the bone (Fig. 10.3d).
10.4.4 Retraction
Retraction is done to maintain the flap allowing maximum access and visibility without causing damage to the flap or neighboring tissues. A correct retraction technique improves ergonomics, reduces the surgery time, and the postoperative pain and inflammation. During surgery, soft tissue management is commonly overlooked because, once the flap is retracted, attention is usually concentrated on the defect (Fig. 10.4a, b).
(a) If a retractor rests on the flap, pressure will compromise the perfusion and causes ischemia within the flap, and causes more postoperative pain and inflammation. (b) Another important detail to pay attention to is the tension on the flap produced by the retractor. This tension also prevents flap perfusion; in order to decrease this tension, changes need to be made intraoperatively, for example a notch can be prepared in bone to secure retractor placement (arrows)
Retractors are one of the most important instruments for surgical endodontics. They must be:
-
Wide enough to hold flap completely (15 mm)
-
Thin enough (~0.5 mm) to improve access
-
Have a serrated working end to prevent sliding
-
Have a matte surface, so light is not reflected
The working end of a retractor should adapt, as far as possible, to the cortical bone plate of the specific surgical area.
10.4.5 Osteotomy Window (Low-Power Magnification)
An osteotomy window approximately 5 mm diameter has to be made in order to allow easy access for instruments and devices to the apex. A round tungsten bur or a 5 mm trephine may be used to create the “access cavity” at the hard tissue level, to the involved molar apices.
The endodontic surgeon can now encounter three different clinical situations:
-
Intact cortical bone table
-
Perforation of the cortical bone plate without periosteum
-
Perforation of the cortical bone plate with periosteum
10.4.6 Curretage (Medium-Power Magnification)
To remove pathological tissues, foreign bodies, and bone particles from the periradicular or lateroradicular areas, curettage provides visibility and accessibility to the apex or lateral canal. Curettage should be performed as clean and fast as possible because the surgical hemostasis is directly related to a complete curettage. Lingual/palatal bone crypt walls are the most difficult areas to clean. A Lucas bone curette, 33 L spoon excavator, and Molt curettes can be used for medium and large lesions. Alternatively, Columbia #13/14, Molt, or Jaquette 34/35 curettes may be used for small lesions and lingual-palatal bone crypt walls (see Fig. 10.5).
(a) Frequently, just removing granulation tissues with a Lucas curette ( sharp edge with concave and convex surfaces) is sufficient to achieve good access to the apex without removing any bone. (b, c) Jaquette 34/35 curette is specially designed to peel away the granulation tissues situated between the root and the palatal-lingual walls of the bone crypt
10.4.7 Hemostasis (Medium-Power Magnification)
Clearly, hemostasis is an indispensable factor for microsurgery because a dry surgical field provides better visualization of the microanatomy, dramatically improves the surgical efficiency, and minimizes root-end filling contamination. Anesthesia (see Chap. 3 in this book) is essential in providing effective presurgical hemostasis; specifically, solutions with 1:50,000 epinephrine should be used if there are no medical contraindications. Both block and buccal/lingual-palatal injections are required to get effective hemostasis. The use of anesthetics during surgery to get surgical hemostasis is typically ineffective.
Topical hemostatic may be achieved with cotton pellets with or without epinephrine (Fig. 10.6) in the osseous crypt; ferric sulfate pellets can be used to achieve hemostasis outside the crypt when applied to bleeding sites on the buccal bone.
Hemostasis in the surgical crypt may be achieved with the epinephrine pellet technique. (a) The first cotton pellet is applied against the bony crypt bottom walls. (b) Several more pellets are placed after until the bone cavity is totally filled. Pressure is applied for 4 min. (c) Then all pellets are removed subsequently, except the very first one that remains in place until final irrigation. This first pellet has two critical functions: it prevents the nicked vessels from reopening during surgery and also it prevents operative debris from lodging into the palatal/lingual bone wall of the crypt that is otherwise difficult to remove
10.4.8 Apicoectomy (Low-Power Magnification for Apicoectomy and Medium- to High-Power Magnification for Inspection)
The apical 3 mm of the root(s) involved are resected (Fig. 10.7), where more complex anatomy exists; this has for example been shown histologically in extracted molars, in electron microscopic studies, and micro-computed tomography data (see also Chap. 1 in this book). Preferably there should be a 0° bevel and a fluted carbide or Lindemann bur should be used with an Impact Air handpiece, under copious irrigation. Current microinstruments like micromirrors, small ultrasonic tips, and micropluggers permit to work with such a small bevel. After resecting the apical root segment, methylene blue dye is used to ensure the resection is complete and for canals and isthmus inspection (Fig. 10.8).
(a) “Rule of threes”: The goal is to remove the apical 3 mm of each involved root by the apicoectomy and another 3 mm of the canal is instrumented and sealed by the retrofill. The final 6 mm of the canal is treated to eliminate or block most frequent communications at the apical third area between main canal and the periodontium. (b) Micro-computed tomography rendering of the mesiobuccal apex of a maxillary molar with multiple apical ramifications, indicating the complex anatomy that may be present in the apical portion of any molar root (Image B courtesy of Dr. O. Peters)
Staining the resected apex with methylene blue dye discloses the presence of connective tissue and can serve to demonstrate that the cut of the root has been complete (360° continuously stained outline) or incomplete (broken outline). This staining step is also important to detect otherwise undiscovered canals, isthmuses, apical fractures, and craze lines
10.4.9 Isthmus
One small detail left uncorrected can render the whole procedure ineffective. In this context, the “micro tissue” within the isthmus is as important as the “macro tissue” of the main canals.
Although an isthmus is an important structure in endodontic microsurgery, it was ignored in dental textbooks or scientific literature until 1983 [16]. It represents the communications that normally exist, at different levels, between two canals inside a root (Fig. 10.9a), but surgically exposed at the resected apex root area. It contains pulp tissue and should be treated in the same way as the pulp tissue of the canals. Figure 10.9b illustrates schematically how the isthmus should be prepared.
(a) Clinical view of high-power magnification of a prepared isthmus (arrow) in a mesial root of a mandibular molar. Only the complete but dentin-preserving preparation of an isthmus permits adequate disinfection. (b) After the main canals are retrogradely prepared, the isthmus (arrowhead) must be prepared and cleaned with either a round or potentially a blade-shaped ultrasonic tip. Care has to be taken to retain sufficient dentin wall thickness (arrows), specifically along the isthmus in roots with figure-eight cross-sections such as the mesiobuccal roots in maxillary molars and the mesial roots in mandibular molars
10.4.10 Root-End Preparation
In order to create a clean and well-defined Class 1 cavity into the already sectioned root it must have walls that are parallel to the major axis and well centered within the root, so as not to weaken the root walls, and deep enough to retain the biocompatible material of obturation (Fig. 10.10). The retrocavity should have at least 3 mm depth according to the “Rule of Threes” (see Fig. 10.7). Retrocavity preparation has been dramatically improved since ultrasonic (US) microtips and micromirrors were introduced [17]. Low-power magnification (4×) should be used for microtip alignment with the long axis of the root (Fig. 10.11); poor alignments can produce root perforations. Medium-power magnification (10–16×) should be used for retrocavity preparation, while high-power magnification (20–25×) is used for the final inspection of the retrocavity.
(a) The ultrasonic tip must follow the canal trajectory to prevent thinning of radicular structure or perforation. Proper alignment of a zirconium oxide microtip in relation to the long root axis seen at low-power microscope magnification. (b, c) Incorrect angulations may lead to perforation toward the buccal or lingual direction
Properly designed ultrasonic microtips, ideally with abrasive coating, should be used at the correct power setting and with adequate irrigation, in order to prevent microfractures at the tooth apex.
In order not to overly thin out the radicular wall, there should be a relationship between the size of the microtip and the wall thickness, so that thinner microtips are selected for buccal roots of upper molars and mesial roots of lower molars; conversely larger tips may be selected for palatal roots of upper molars and distal ones of lower molars (Fig. 10.12).
Adequate retrograde tips must be selected to prepare different root cross-sections in molars (a, b) to avoid excessive thinning of the radicular structure and possible sequelae such as vertical root fracture. Round cross-sections such as in maxillary anteriors are amenable to larger retrograde tips due to the bulkier root cross-section (c, d) (Courtesy Dr. C. Peters)
10.4.11 Drying of the Preparation (Medium-Power Magnification)
The retrocavity has to be cleaned and dried before filling it. Air can be used with the Stropko’s syringe, except in a through-and-through bone defect, perforating the maxillary sinus membrane where the use of paper points is mandatory (Fig. 10.13, see also bone defect classification in Box 10.1 and further below).
After preparation, the cavity has to be dried. The use of paper points is not a reliable method for this, because residual blood, debris and moisture may prevent the filling material from forming an adequate retrocavity seal, which could cause the case to fail. But in a case like this one, with a perforation of the buccal bone plate and the sinus membrane too, air should not be blown into the retrocavity because it could introduce necrotic material from the retrocavity into the sinus cavity (Reprinted from Merino 2009, with permission)
10.4.12 Retrograde Fill (Medium-Power Magnification)
A biocompatible material is used to produce a stable hermetic seal that can prevent the percolation of bacteria or their products between root canal system and periradicular tissues. Mineral-trioxide aggregate or MTA currently is the standard cement for retrograde fills because of its biocompatibility, sealing ability, and dimension stability (Fig. 10.14). Other bioceramic materials such as root repair putty (RRM) may provide similar healing rates [18, 19].
(a) In a mesiobuccal root of a maxillary molar, placement of gray MTA (Dentsply) retrofill material using a microplugger. (b) Clinical view at medium-power magnification. (c) Apical view of a distal root of a maxillary molar after MTA retrofill at high-power magnification (a, b Courtesy of Dr. C. Peters)
Cited disadvantages of MTA are that, although moisture is required for setting, during packing, isolation is critical because excess moisture can remove the filling from the retrocavity. Also, there are no final wash and polish phases and its setting time is very long while radiopacity is not high. Newer materials provide shorter setting times [19–22].
10.5 Bone Defect Classification
Classic studies of endodontic surgery [23, 24] noticed that some failures originated not from the surgical technique itself, but from the size of the lesion and the configuration of cortical bone being perforated at the time of the surgery. Although every step of endodontic microsurgery has dramatically improved over the last few years, comparatively little attention has been paid to the bone defect topography underlying the soft tissue.
The shapes, sizes, and locations of the bone defects encountered during endodontic microsurgery differ substantially. However, bone defect topography dictates the long-term prognosis of microsurgery, independent of the perfectly performed steps of the microsurgery itself [3].
The areas of interest in apical surgery can be divided into two major classes, the apical endodontic area (green) and the cervical or periodontal area (red) (Fig. 10.15). Then clinically osseous defects may be classified in endo lesions, endo-perio lesions, and a combination of them (see Box 10.1). Specific clinical conditions associated with these bone defects are listed below:
-
Small bone defects
A localized defect around the periapical area, related to the main apical foramina or major accessory canals localized in the periapical area (Fig 10.16.).
Fig. 10.16 (a) This small periapical and lateroradicular bone defect is far away from the bone crest. (b) This large periapical bone defect affects two roots and the furcation area. (c) Early periapical bone lesion on the mesiobuccal root of this first upper left molar with the cortical plate intact (white arrow). However, the sinus membrane is already inflamed (red arrow). (d) Right first maxillary molar with a large osseous defect requiring apical surgery. There is a large through-and-through bone defect with total destruction of the buccal and sinus bone cortical plates (white arrows) related to the tooth in question (Reprinted from Merino 2009, with permission)
-
Large bone defects
These defects can cause collapse of the periosteum over the root surface; or if they are close to the bone crest, to invagination of the dentogingival junction into the furcation area (Fig. 10.16b).
-
Through-and-through bone defect
There is a close relationship between the apexes of the upper molars and the maxillary sinus. This is the reason for the fact that an inflamed sinus membrane is an early radiological sign for a periapical infection starting in the apical area [25] (Fig. 10.16c). Also, after the root canal treatment, the return to its normal width is an early sign of a successful treatment. The spatial position of the buccal roots (and their foramina with relation to the root apices) of the upper molars and the maxillary sinus inside the bone compartment, and the amount of bacterial toxins leached out to the periodontium, produces a simple bone lesion contained inside the bone compartment, or perforates one of the cortical bone or two cortical walls ending up in a complex osseous defect (Fig. 10.16d). Typically, through-and-through defects require a specific surgical strategy:
If the root canal treatment or retreatment cannot stop the infection, then the surgical intervention will consist of both on a standard endodontic microsurgery (to prevent the bacterial percolation) and the application of guided bone regeneration procedure, to regenerate the bony compartment.
If the root canal treatment or retreatment can stop the infection, then the final surgical intervention may consist of only guided bone regeneration, in order to reconstruct the lost periodontium.
-
Apicomarginal bone defect
This condition can be seen as a mix of two bone defects: a periapical bone defect plus a total root dehiscence. Due to the structural differences between bone maxilla and mandible, root dehiscences in the maxilla tend to be larger overall and wider than the ones encountered in the mandible.
Although the diagnosis of an apicomarginal defect can be easily made after reflection of the mucoperiosteal flap, clinical and radiographic data obtained beforehand [20] can advance us to this point and allow the patient to be informed about the special surgery, increased budget, and longer surgery time.
The prognosis of endodontic microsurgery in the presence of an apicomarginal defect depends on the following:
-
Crown/root ratio
-
Width of the dehiscence at the bone crest
-
Thickness of the proximal bone margins
Regardless, a successful treatment outcome depends more on the control of the epithelial downgrowth, that is, epithelial proliferation, at the crestal level than on the management of the periapical defect (see Fig. 10.15).
-
-
Combination of Apicomarginal and Through-and-through defects
This condition can be seen frequently in maxillary molars (Fig. 10.17). A schematic approach to the diagnosis of bone defects can be seen in Box 10.1. Most of the lesions encountered need guided tissue regeneration techniques in order to be successfully managed.
Fig. 10.17 (a) Apical surgery for the mesiobuccal root of a maxillary first molar. A total dehiscence of the mesiobuccal root was evident after raising the flap and the apical part of the bone defect has destroyed the cortical bone of the maxillary sinus floor, with bone visible in lower power magnification. (b) In order to prevent operational debris from getting into the sinus during retrograde preparation and fill, a collagen piece was inserted between the root apex and the sinus membrane. (c) Retrocavity was filled with SuperEBA (Bosworth) cement and the collagen piece was removed. (d) Before placement of a membrane, a new piece of collagen is inserted into the crypt. (e) A Gore-Tex nonresorbable membrane No. GT4, selected to function as an external barrier, was trimmed to adapt to the root dehiscence at the bone crest and fixed using a titanium tag. Bone chips were used to cover the root dehiscence and the membrane were fixed in its final position. (f) No dehiscence was detected in the area when titanium tags and membrane were removed. (g) Clinical condition and probing at a 5-year follow-up (Reprinted from Merino 2009, with permission)
Materials and techniques to treat the different bone defects are listed in Box 10.2. Autologous bone is the only material that promotes regeneration, while a xenograft material should be used as a space maintaining material while membranes prevent soft tissue interference in the bone regeneration process. All three materials must be used when the root is protruding out of the osseous envelope.
Box 10.2. Treatment Techniques for Bony Defects
Materials | |||
|---|---|---|---|
Extent of defect | Augmentation | Membrane | GBR/membrane recommended |
Apical 1/3 | No | Yes | No |
Apical and middle 1/3 | Bone xenograft | Yes | Resorbable, one side |
Through-and-through | Variable | Yes | Resorbable, two sides |
Apicomarginal | |||
- intraosseous; space-making - extraosseous; non-space-making | Autologous graft Autologous (first layer), xenograft (second layer) | Yes Yes | Resorbable Nonresorbable fixed |
10.6 Intentional Replanation
Intentional replantation is defined as the “insertion of a tooth into its alveolus after the tooth has been extracted for the purpose of performing treatment, such as root-end filling (s) or perforation repair” [26]. This is not a mysterious or exotic procedure but a safe and standard clinical technique to retain an otherwise untreatable tooth, with a high success rate [27–31].
10.6.1 Potential Indications
-
Difficult access, for example to apices of second or third mandibular molars is extremely difficult and apicoectomy is typically contraindicated (Fig. 10.18).
Fig. 10.18 (Left and right) The external oblique ridge complicates the surgical access to the apex of second and third molars. In many cases, the distance is too large for a buccal approach. Also structures such as the inferior alveolar never are close to the lingual cortical bone as shown in this specimen (Image courtesy of Dr. J. Gutmann)
-
Anatomical limitations, for example close proximity of the apices of premolars or molars to the inferior alveolar nerve (Fig. 10.18) or occasionally the maxillary sinus. Here, less experienced clinicians may choose intentional replantation instead of surgical standard approach.
-
Difficult access to perforation or resorption areas.
-
An intraradicular post cannot be removed neither nonsurgically nor surgically.
-
Previously attempted and failing retreatment.
-
Previous attempted and failing apicoectomy.
-
Severe periodontal problem and/or removal of bone to gain surgical access, which would leave the patient with an untreatable periodontal problem.
-
Patient limitations: Medical or geriatric patients who cannot cooperate during the surgery time.
10.6.2 Contraindications
-
Medical history with anticoagulation medication or compromised healing.
-
Nonrestorable tooth.
-
Large periodontal lesions that compromise the tooth stability.
-
Difficult extraction with high risk of bone cortical plate fracture.
-
Root fracture during extraction leaving a poor crown-root ratio.
10.6.3 Clinical Case Selection
Apart from the technique procedure itself, case selection is the most important factor in replantation prognosis. A clinical case is shown in Fig. 10.19; here the inability to debride and prepare via an orthograde approach necessitated the surgery and the access was too close to the mandibular canal.
(a) After crown preparation and root canal treatment with significant overextension of root canal filling, this patient complained about persistent pain. (b) During intentional replantation, the tooth was gently lifted out of the socket and retrograde prepared. Care was taken to keep the periodontal ligament moist and the retrograde cavities were filled with Root Repair Material (Brasseler). (c, d) Clinical and radiographic condition immediately after replantation. The postoperative course for this patient was uneventful
10.6.4 Technique
Replantation is biologically based on the viability of the cells and fibers of the periodontal ligament after it’s stay outside of the socket. It was previously believed that a tooth that was outside of the alveolar socket will suffer from resorption or ankylosis upon replantation but current data overwhelmingly show that this depends on the viability of the cells of the periodontal ligament: the longer the root is outside of the socket, the more readily resorption and ankylosis will occur [31–34]. This is the reason that, before the extraction, the clinical team must rehearse all the surgical steps, so that once the tooth has been removed, the procedure can be carried out efficiently and in minimum time [30].
10.6.5 Recommendations
-
Intentional replantation is the last resort to maintain a tooth; therefore, case selection is critical.
-
Crown or root fracture is always a possibility of replantation procedure termination and the patient must be informed orally and in writing in the informed consent form.
-
A fast procedure is significantly related to success. Therefore, “ergonomics is everything.”
-
Gentle extraction without touching the root surface compressing neither of the alveolus walls promoted periodontal healing.
-
The extraction forceps handles should be grabbed aided with a rubber band.
-
Root inspection should be done at maximum-power magnification, and preparation and obturation of cavities at medium-power magnification.
-
The tooth should be rinsed constantly with saline, serum, or tissue culture solution.
-
Do not curette the socket, rather aspirate socket clot without touching the walls.
-
The shorter the time the tooth is out of the socket, the better. Maximum extraoral time is about 5–10 min.
-
A gentle reinsertion should be done. If there is too much pressure in any area, the periodontal fibers will lack vascularization and resorption will start.
-
Rigid stabilization is typically not needed; if necessary, maximum duration will be 1 week’s time.
As shown, the scope of contemporary apical microsurgery includes more than apicoectomies; however, procedures such as hemisections and root amputations have largely fallen into disfavor, since long-term outcomes do appear to compare favorably with implant therapy [35]. Regardless, the overall success rate of endodontic microsurgery is according to the literature and with modern techniques in the range of nonsurgical root canal treatment [4, 36].
References
Siqueira Jr JF. Aetiology of root canal treatment failure: why well-treated teeth can fail. Int Endod J. 2001;34:1–10.
Gorni FG, Gagliani MM. The outcome of endodontic retreatment: a 2-yr follow-up. J Endod. 2004;30:1–4.
Merino E. Endodontic microsurgery. Quintessence Pub; 2009; Chapter 6: Treatment of bone defects in apical microsurgery, Berlin. p. 176.
Setzer FC, Shah SB, Kohli MR, Karabucak B, Kim S. Outcome of endodontic surgery: a meta-analysis of the literature-part 1: comparison of traditional root-end surgery and endodontic microsurgery. J Endod. 2010;36:1757–65.
Patel S, Durack C, Abella F, Shemesh H, Roig M, Lemberg K. Cone beam computed tomography in endodontics-a review. Int Endod J. 2015;48:3–15.
Gutmann JL, Harrison JW. Flap design and incisions. In: Surgical endodontics. Boston: Blackwell; 1991. p. 162–75.
Carr G, Bentkover S. Surgical endodontics. In: Cohen S, Burns R, editors. Pathways of the pulp. St Louis: Mosby; 1998. p. 608–56.
Mörmann W, Meier C, Firestone A. Gingival blood circulation after experimental wounds in man. J Clin Periodontol. 1979;6:417–24.
Kim S. Principles of endodontic microsurgery. Dent Clin North Am. 1997;41:481–97.
Velvart P, Peters CI, Peters OA. Soft tissue management: suturing and wound closure. Endod Top. 2005;11:179–95.
Merino E. Endodontic microsurgery. Quintessence Pub; 2009; Chapter 3: Microsurgery step by step, Berlin. p. 51.
Arens DE, Adams WR, De Castro RA. Endodontic surgery. New York: Harper & Row; 1984. p. 102–32.
Peters LB, Wesselink PR. Soft tissue management in endodontic surgery. Dent Clin North Am. 1997;41(3):513–28.
Ohmori S, Kurata K. Experimental studies on the blood supply to various types of skin grafts in rabbits using isotope 32p. Plast Reconstr Surg. 1960;25:547–55.
Patterson TJ. The survival of skin flaps in the pig. Br J Plast Surg. 1968;21:113–7.
Cambruzzi JV, Marshall FJ. Molar endodontic surgery. J Can Dent Assoc. 1983;1:61–6.
Wuchenich M, Torabinejad M. A comparison between two root end preparations techniques in human cadavers. J Endod. 1994;20(6):279–82.
Torabinejad M, Pitt Ford TR. Root end fillings materials: a review. Endod Dent Traumatol. 1996;12:161–78.
Chen I, Karabucak B, Wang C, Wang HG, Koyama E, Kohli MR, Nah HD, Kim S. Healing after root-end microsurgery by using mineral trioxide aggregate and a new calcium silicate-based bioceramic material as root-end filling materials in dogs. J Endod. 2015;41:389–99.
Rud J, Andreasen JO, Jensen JE. Radiographic criteria for the assessment of healing after endodontic surgery. Int J Oral Surg. 1972;1:195–214.
Rud J, Andreasen JO. A study of failures after endodontic surgery by radiographic, histologic and stereomicroscopic methods. Int J Oral Surg. 1972;1:311–28.
Molven O, Halse A, Grung B. Surgical management of endodontic failures: indications and treatment results. Int Dent J. 1991;41:33–42.
Skoglund A, Persson G. A follow-up study of apicoectomized teeth with total loss of the buccal bone plate. Oral Surg Oral Med Oral Pathol. 1985;59:78–81.
Hirsch JM, Ahlstrom U, Henrikson PA, Heyden G, Peterson LE. Periapical surgery. Int J Oral Surg. 1979;8:173–85.
Nunes CA, Guedes OA, Alencar AH, Peters OA, Estrela CR, Estrela C. Evaluation of periapical lesions and their association with maxillary sinus abnormalities on cone-beam computed tomographic images. J Endod. 2016;42:42–6.
Amercian Association of Endodontists. Glossary of endodontic terms. 2015. Available from http://www.nxtbook.com/nxtbooks/aae/endodonticglossary2015/. Accessed 27 Feb 2016.
Koenig KH, Nguyen NT, Barkhordar RA. Tooth replantation of mandibular molars and premolars. Gen Dent. 1988;36:327–31.
Kinsbury BC, Weisenbaught JM. Tooth replantation of mandibular molars and premolars. J Am Dent Assoc. 1971;83:1053–7.
Lindeberg RW, Girardi AF, Troxell JB. Tooth replantation: management in contraindicated cases. Compend Contin Educ. 1986;7:248–58.
Caffesse RG, Nasjleti CE, Castelli WA. Long-term results after intentional tooth reimplantation in monkeys. Oral Surg. 1977;44:666–78.
Roos WJ. Tooth replantation: an alternative. Compend Contin Educ. 1985;6:735–9.
Andreasen JO. Relationship between cell damage in the periodontal ligament after replantation and subsequent development of root resorption: a time-related study in monkeys. Acta Odontol Scand. 1981;39:15–25.
Andreasen JO. Effect of extra-alveolar period and storage media upon periodontal and pulpal healing after replantation of mature permanent incisors in monkeys. Int J Oral Surg. 1981;10:43–53.
Andreasen JO. The effect of pulp extirpation or root canal treatment on periodontal healing after replantation permanent incisors in monkeys. J Endod. 1981;7:245–52.
Cho GC. Evidence-based approach for treatment planning options for the extensively damaged dentition. J Calif Dent Assoc. 2004;32:983–90.
Danin J, Strömberg T, Forsgren H, Linder LE, Ramsköld LO. Clinical management of nonhealing periradicular pathosis. Surgery versus endodontic retreatment. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996;82:213–7.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Merino, E.M. (2017). Endodontic Microsurgery for Molars. In: Peters, O. (eds) The Guidebook to Molar Endodontics. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-52901-0_10
Download citation
DOI: https://doi.org/10.1007/978-3-662-52901-0_10
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-662-52899-0
Online ISBN: 978-3-662-52901-0
eBook Packages: MedicineMedicine (R0)