Abstract
Systemic lupus erythematosus (SLE) is an autoimmune disease of unknown cause that can occur at almost any age, although it affects mostly women in their 20s. The annual incidence of SLE is 50–70 people per million of the population, and prevalence is 500 per million [1]. The incidence of new cases and the survival of patients with SLE are both increasing [2]. The disease is characterized by a large variety of organ disorders involving many different immune mechanisms. The spectrum of kidney lesions predominantly involves the glomerulus and includes minimal mesangial alterations to florid proliferative lesions with necrosis and crescents but also extends to nonimmune complex lesions such as thrombotic microangiopathy (see Chap. 11) and direct podocyte injury. Correspondingly, clinical manifestations and course are equally diverse. Kidney disease develops in more than half of lupus patients and represents the first clinical manifestation of SLE in 15–20 % [3, 4]. Moreover, renal alterations are found in almost 90 % of lupus patients at autopsy. The lowest 5-year survival has been reported for patients with central nervous system and renal involvement [1].
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1 Introduction/Clinical Setting
Systemic lupus erythematosus (SLE) is an autoimmune disease of unknown cause that can occur at almost any age, although it affects mostly women in their 20s. The annual incidence of SLE is 50–70 people per million of the population, and prevalence is 500 per million [1]. The incidence of new cases and the survival of patients with SLE are both increasing [2]. The disease is characterized by a large variety of organ disorders involving many different immune mechanisms. The spectrum of kidney lesions predominantly involves the glomerulus and includes minimal mesangial alterations to florid proliferative lesions with necrosis and crescents but also extends to nonimmune complex lesions such as thrombotic microangiopathy (see Chap. 11) and direct podocyte injury. Correspondingly, clinical manifestations and course are equally diverse. Kidney disease develops in more than half of lupus patients and represents the first clinical manifestation of SLE in 15–20 % [3, 4]. Moreover, renal alterations are found in almost 90 % of lupus patients at autopsy. The lowest 5-year survival has been reported for patients with central nervous system and renal involvement [1].
The diagnosis of SLE is based on the documentation of multisystem involvement that meets at least 4 of 11 criteria established by the American College of Rheumatology [5]. Lupus nephritis is typically manifest by proteinuria, ranging from minimal to nephrotic and usually correlating with the histologic type of lesion. Severe glomerular lesions cause hematuria, a telescoped urinary sediment (i.e., red and white blood cells, as well as hyaline, granular, cellular, and broad casts), and renal insufficiency. Hypertension usually develops later in the course of the disease.
Classification of the renal pathology of lupus patients has been based on light microscopic changes, combined with immunohistochemical/immunofluorescent and ultrastructural observations. The classification was most recently revised in 2004 by a working group under the auspices of the Renal Pathology Society (RPS) and the International Society of Nephrology (ISN) (Tables 8.1, 8.2, and 8.3) [6].
2 Pathologic Findings
2.1 Light Microscopy, Immunofluorescence, and Electron Microscopy
2.1.1 Mesangial Lupus Nephritis Classes I and II
Classes I and II lupus nephritis refer to mesangial lupus nephritis. These patients present clinically with mild hematuria, or proteinuria, or both. In general, this kidney lesion has a good prognosis, and the histologic alterations remain stable in the majority of cases. However, functional deterioration and progression of glomerular lesions to more active or generalized proliferative forms occur in about 20 % of cases. In the past decades, the availability of better supportive therapy and more selective use of immunosuppressive agents have led to improved survival of patients with mild forms of lupus glomerulonephritis, while new forms of immunosuppressive therapy are being developed [7, 8].
Class I minimal mesangial lupus nephritis refers to biopsies showing normal glomeruli by light microscopy but mesangial immune deposits by immunofluorescence and/or electron microscopy. Class II contains mesangial proliferative lesions characterized by mesangial hypercellularity of any degree or mesangial matrix expansion by light microscopy with mesangial deposits. In either class I or II mesangial forms of LN, there may be a few isolated subepithelial or subendothelial deposits by immunofluorescence and/or electron microscopy but without endocapillary, sclerotic, or crescentic reactions (Fig. 8.1). If the latter changes are present, then a diagnosis of focal LN (if less than half of glomeruli manifest these reactions) or diffuse LN (more than half) is warranted.
2.1.2 Focal Lupus Nephritis Class III
Focal lupus nephritis ISN/RPS class III entails focal (involving less than half of the glomeruli available for inspection) proliferative, necrotizing, or sclerosing lesions. These lesions may be either segmental (involving <50 % of the tuft area of the affected glomeruli) or global (involving ≥50 % of the tuft area of the involved glomeruli). A subdivision is made according to the predominance of active versus sclerotic lesions as indicated in Table 8.1.
In the pathology report, the proportion of glomeruli with active and with sclerotic lesions and the proportion of glomeruli with fibrinoid necrosis or cellular crescents should be indicated. The proliferative lesions include variable mesangial proliferation and endocapillary proliferation with variable inflammatory cells. Double contours of the GBM on silver stain may be present. Necrotizing lesions with fibrinoid necrosis and crescent reaction are often present in active lesions (Figs. 8.2 and 8.3). In these areas, there is nuclear debris as well as influx of inflammatory cells. The inflammatory process may also lead to disruption of the glomerular basement membrane and fibrinoid necrosis. Fibrinoid necrosis appears as amorphous eosinophilic material staining bright red in trichrome staining, often associated with GBM breaks and karyorrhexis. Interstitial inflammation may be marked adjacent to glomeruli disrupted by crescents and/or necrosis, particularly if Bowman’s capsule is ruptured by the destructive lesion. Segmental sclerotic scars with broad-based adhesions to Bowman’s capsule can develop from focal crescents with necrotic lesions. Tubular atrophy and interstitial fibrosis are proportional to glomerular scarring.
Focal lupus nephritis ISN/RPS class III (A + C) with active endocapillary proliferation and an early necrotizing lesion with rupture of the glomerular basement membrane and early crescent formation in the middle glomerulus and a small adhesion and fibrocellular crescent in the lower right glomerulus. However, less than half of the glomeruli showed such lesions (Jones silver stain)
Immunofluorescent staining shows the presence of immunoglobulin G (IgG), IgM, IgA, and complement factors C3 and C1q (“full-house” immunofluorescence) in chunky granular and globular depositions along the glomerular capillary walls and in the mesangium (Fig. 8.4). These capillary wall deposits are largely subendothelial, seen by their smooth outer contour as they are molded under the GBM, and confirmed by electron microscopy. Although the light microscopic proliferative changes are focal, the immunofluorescence is usually positive in all glomeruli. Electron microscopy typically demonstrates deposits in the mesangium and also in the subendothelial area. There may be scattered subepithelial deposits, but if these are extensive (i.e., >50 % of loops in most glomeruli), membranous LN should be diagnosed in addition to the proliferative process (Fig. 8.5) [6].
Patients with focal lupus nephritis class III present almost invariably with proteinuria and in the majority of cases with mixed findings of nephrotic and nephritic syndromes. The lesions can transform to diffuse proliferative (class IV) or membranous lupus nephritis class V.
2.1.3 Diffuse Lupus Nephritis Class IV
Patients with diffuse lupus nephritis class IV typically have increased renal dysfunction and significant proteinuria and active urine sediment. This class is the most common and severe form of lupus nephritis detected in renal biopsies. The biopsy shows diffuse segmental (IV-S) or global (IV-G) lesions, characterized by proliferative, sclerosing, and/or necrotizing lesions in more than 50 % of the glomeruli. The lesions may thus be either active or inactive and have a segmental or global distribution. There is variable mesangial and endocapillary proliferation. Cellular crescents and necrosis are frequently present in active cases, whereas broad-based adhesions with segmental sclerosis and fibrocellular to fibrous crescents characterize the chronic lesions. Some investigators revealed a poor outcome of diffuse “segmental” necrotizing glomerulonephritis involving over 50 % of glomeruli, as compared to other forms of class IV lupus nephritis [9]. Attempts to capture the possible significance of these severe segmental lesions were therefore made by dividing class IV diffuse lupus nephritis into diffuse segmental (IV-S) when ≥50 % of the involved glomeruli have segmental lesions and diffuse global (IV-G) when ≥50 % of the involved glomeruli have global lesions (Fig. 8.6) [6]. Furthermore, a subdivision is made according to the presence of active versus chronic lesions as was indicated for class III lesions (Table 8.1). However, the definition of “segmental” as <50 % of the tuft is not congruent with that used by the original investigators, who considered lesions “segmental” if even a single loop of the glomerular tuft was not involved. Thus, the ISN/RPS S versus G lesions may not adequately capture this subgroup of patients.
As in focal LN class III, the proportion of glomeruli with active and with sclerotic lesions and the proportion of glomeruli with fibrinoid necrosis or cellular crescents should be indicated in the pathology report. “Wire-loop” lesions, that is, local periodic acid-Schiff (PAS)-positive thickenings of the glomerular capillary walls, are characteristic of this form of lupus nephritis (Fig. 8.7). This thickening of the capillary walls is related to the presence of large, subendothelial electron dense deposits. Glomerular lesions run the gamut from diffuse hypercellularity to severe necrotizing “crescentic” glomerulonephritis or, in chronic cases, diffuse global glomerulosclerosis with loss of renal function. Tubular atrophy and interstitial fibrosis are often more extensive in diffuse LN, class IV than in focal LN, class III. The predictive value of these lesions with respect to renal function, however, is disputed [10, 11]. The tubular epithelium shows cytoplasmic hyaline droplets, hydropic degeneration, cytoplasmic vacuolization, hyaline protein cylinders, and, in more advanced stages, disease glomerulosclerosis, tubular atrophy, and interstitial fibrosis. Arteries and arterioles may show varying lesions (see below).
Immunofluorescence in diffuse lupus nephritis class IV shows irregular “full-house” deposits of immunoglobulins and complements along the glomerular capillary walls and in the mesangium (Fig. 8.8). Ultrastructurally, electron dense deposits are seen in the mesangium and subendothelially along the capillary walls, in larger quantities than in the other classes. There is frequent interposition of mononuclear cells with new GBM matrix laid down, resulting in double contours. By electron microscopy, frequent mesangial and subendothelial deposits are confirmed. Foot processes of podocytes are variably effaced.
Tubuloreticular inclusions (TRIs) (also called reticular aggregates) can be found in the cytoplasm of endothelial cells. These TRIs are not specific for SLE but are often seen in endothelial cells throughout the body in patients with AIDS and other viral infections or in patients receiving exogenous interferon therapy, reflecting high levels of interferon. Large and often confluent subendothelial deposits represent the ultrastructural analogue of the “wire-loop” lesions seen light microscopically. Variable subepithelial deposits are present but, if extensive, warrant concurrent diagnosis of additional membranous class V lupus nephritis (see below). As in the other classes of lupus nephritis, the electron dense deposits can show a typical fingerprint-like crystalline pattern, possibly representing the presence of cryoglobulins.
Patients with diffuse lupus nephritis class IV typically have marked proteinuria, an active urine sediment and decreased renal dysfunction.
2.1.4 Membranous Lupus Nephritis Class V
Membranous class V lupus nephritis is characterized by diffuse subepithelial deposits, involving ≥50 % of the loops in ≥50 % of the glomeruli. Among patients with lupus nephritis, the incidence of membranous nephritis varies between 8 and 27 %. The prognosis of patients with membranous lupus nephritis is relatively favorable, with a reported 10-year kidney survival of 91 % [12]. Still, one-third of patients with membranous lupus nephritis progress to proliferative lupus nephritis [13]. Patients most often present with marked proteinuria.
By light microscopy, there is variable mesangial expansion with diffuse thickening of the glomerular capillary walls in hematoxylin and eosin and PAS stains. With silver-methenamine staining, argyrophilic spikelike formations often can be seen along the glomerular basement membrane, corresponding to basement membrane reaction between and around the subepithelially localized immune deposits. By immunofluorescence, granular deposits of immunoglobulins and complement are present peripherally along the glomerular capillary walls and in the mesangium, corresponding to the presence of subepithelial and mesangial electron dense deposits. Membranous lupus nephritis is distinguished from idiopathic membranous nephropathy by full-house staining of deposits by immunofluorescence, reticular aggregates by electron microscopy, and most often mesangial deposits [14, 15]. Absence of staining for the phospholipase A2 receptor in the deposits, the antigen present in most cases of idiopathic membranous nephropathy, may also be useful [16]. Foot processes are diffusely effaced by electron microscopy.
Class V membranous lupus nephritis may occur in combination with classes III or IV (focal or diffuse lupus nephritis), in which case both are diagnosed. Patients with pure membranous lupus nephritis experience a relatively benign course, whereas those with mixed membranous and diffuse proliferative lesions have survival rates similar to those of patients with diffuse lupus nephritis alone. Likewise, in a study of membranous lupus nephritis, patients with additional proliferative lesions had higher serum creatinine levels at entry and were more likely to experience a decline in renal function than those without proliferation [17].
2.1.5 Advanced Sclerosing Lupus Nephritis Class VI
This class refers to a late stage, resembling morphologically any late or end stage in chronic glomerulonephritis with global or extensive segmental sclerosis of >90 % of glomeruli without residual activity. Specific features of lupus nephritis are usually lacking. However, in patients with lupus nephritis such chronic end-stage glomerulosclerotic lesions are seldom seen. Patients with lupus nephritis who have been treated for longer periods may show chronic glomerular lesions at autopsy. These may be morphologically similar to other late stages of glomerulonephritis and of focal global sclerotic lesions that occur invariably at an older age [18–20].
2.1.6 Lupus Podocytopathy
Some patients with SLE may have only mesangial lesions but widespread foot process effacement and the nephrotic syndrome with extensive foot process effacement by EM [21–23]. Some of these patients have responded rapidly to steroid therapy, suggesting that the podocyte lesions are more like minimal change disease rather than related to consequences of immune complexes. It is not established whether such podocyte injury could reflect a second superimposed minimal change disease-type process or secondary injury related to cytokines activated by an immune complex process.
2.1.7 Vascular Lesions in SLE
Several types of vascular lesions may be seen in SLE patients [24]. Patients with SLE are not protected from banal vascular lesions related to hypertension and thus may show nonspecific sclerosis of arteries and arterials with associated hyaline. Uncomplicated vascular immune deposits also occur commonly in lupus nephritis and are highly specific for this condition (Fig. 8.9). Immune deposits may be detected by immunofluorescence and electron microscopy in arteries or arterioles within the media or along the intimal basement membrane, with staining for immunoglobulins as well as complement components, typically both C3 and C1q. These uncomplicated vascular immune deposits are not associated with any particular clinical manifestations.
Bland vascular deposits are evident in the arteriole at the top, documented to contain IgG and C3 by immunofluorescence. The glomerulus shows segmental endocapillary proliferation and a fibrocellular crescent with segmental adhesion and sclerosis and double contours of GBM in addition to mesangial proliferation (Jones’ silver stain)
In contrast, necrosis of arterioles and occasionally larger arteries without inflammation may occur in patients with severe lupus nephritis, a lesion called lupus vasculopathy. This fibrinoid material is present within the intima and stains eosinophilic with a smudgy appearance. The fibrinoid material may expand to the lumen. Vascular smooth muscle cells and endothelial cells often show necrosis, but there is no true vasculitis in that there are no inflammatory cells associated with this lesion. Immunoglobulins are detected by immunofluorescence. Electron microscopy has documented both hyaline-type material with insudated plasma proteins and immune deposits in addition to fibrin. This lesion has a poor prognosis [25, 26].
Patients with SLE may also have thrombotic microangiopathy with or without a detectable circulating lupus anticoagulant or antiphospholipid antibody. These lesions do not contain immune deposits but rather show fibrin within glomeruli and small arteries, often with glomerular involvement manifest as mesangiolysis with fibrin thrombi in capillary loops. The glomerular capillary wall shows double contours in the more chronic state. Acutely, there is intimal proliferation of arteries and arterials and mucoid change with red blood cell fragments within the injured vascular walls.
Vasculitis is very rare in patients with SLE. This lesion is defined as fibrinoid necrosis with associated inflammatory infiltrate through the vascular wall, with or without immune complex deposits.
2.1.8 Tubulointerstitial Lesions in SLE
Deposits may be present along tubular basement membranes and can be diagnosed based on the presence of granular immunoglobulin and complement deposition (Fig. 8.10). Corresponding electron dense deposits are then visualized by electron microscopy. Such deposits are often, but not invariably, associated with interstitial inflammation comprised predominately of lymphocytes, with scattered monocytes and plasma cells [27–29]. Of note, interstitial inflammation does not correlate directly with tubulointerstitial immune deposits. There may be active injury with tubulitis related to these deposits. More frequently, significant tubulointerstitial inflammation is associated with areas of glomeruli destroyed or injured by crescents. Tubular basement membrane deposits are detected in about half of biopsied patients with lupus nephritis and may be associated with any type of glomerular lesion but most frequently with class IV diffuse lupus nephritis. Deposits may also be present in peritubular capillaries [30].
Tubular atrophy and interstitial fibrosis develop most often in association with severe glomerular disease with marked chronicity. These tubulointerstitial chronic changes correlate well with degree of loss of GFR.
3 Additional Challenges
Although some incomplete definitions and distinctions of subclasses in previous WHO classifications have been clarified in the newer ISN/RPS classification [31], challenges and issues remain. The attempt to analyze segmental versus global class IV lesions does not quite recapitulate the important findings of the group of Lewis et al., in that the ISN/RPS classification divides segmental versus global lesions depending upon whether less than half or more than half of the tuft is involved [6, 9]. In contrast, the original observations were based on definition of “segmental” as a lesion where any part of the glomerulus was left uninvolved. When the original cases were reexamined based on the current ISN/RPS classification, designating classes as class IV segmental versus global indeed did not show significant differences in outcome. In contrast, when cases were divided according to the Lewis definition of segmental, meaning that only at least some part of the glomerulus remained uninvolved by injury, distinct differences in renal survival were noted [32]. Of interest, these segmental lesions have generally been found to have fewer immune deposits, more necrosis, and more crescents and have been postulated to be more vasculitic-like rather than immune complex driven, analogous to lesions of ANCA-associated glomerulonephritis and polyangiitis, with important potential implications for therapy.
In addition, activity and chronicity indices have not yet been shown to be reproducible and thus have not been incorporated into the ISN/RPS classification [11, 20]. Specific development of better indices of disease activity and chronicity is warranted. A further conundrum arises when nonspecific segmental or global scars are present in cases that otherwise show only mesangial or membranous-type lesions. Clearly, sclerosis may develop nonspecifically with aging, and even idiopathic membranous nephropathy may have segmental scars and global sclerosis. Whether such sclerosed glomeruli warrant additional diagnosis of class III or IV chronic lupus nephritis has not been established. Further, the assessment of whether more than half or less than half of glomeruli are involved with significant lesions to differentiate class III versus class IV may be problematic with the presence of many remotely globally sclerosed glomeruli. Particularly with small sample sizes, this conundrum is amplified. Finally, the current classification does not account for extraglomerular lesions (see above), which may be present and important in patients with SLE.
4 Etiology/Pathogenesis
SLE has an autoimmune basis, and the disease can affect numerous organs, including the skin, joints, serous membranes, lungs, central nervous system, and kidney. SLE can affect the kidney in various ways. Lupus nephritis is used to describe the lesions related to immune complex-mediated injury in patients secondary to SLE. The commonly used classifications, including past World Health Organization (WHO) and the current International Society of Nephrology/Renal Pathology Society (ISN/RPS) classifications, only focus on the glomerular lesions. However, immune complexes maybe present along tubular basement membranes and blood vessels as well. Some renal lesions associated with SLE do not have an immune complex deposition etiology. The sites and nature of immune deposits also may vary, and disease manifestations may remit or flare, and the dominant pattern of immune complex localization and the subsequent pattern of injury may change either spontaneously or in response to treatment.
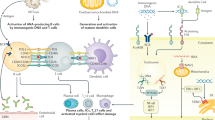
The precise etiology of SLE remains unknown. Autoimmunity is proposed to be related to dysregulated apoptosis with ineffectual clearance of apoptotic cell fragments [33]. There is important genetic susceptibility with increased risk if a family member is affected and HLA associations to DR2, DR3, and B8. SLE-like conditions and lupus nephritis-like immune complex deposits may also develop in patients with HIV infection, illustrating the importance of dysregulated immunity in the evolution of SLE and kidney disease. Immune complexes may be circulating and deposit in specific locations based on size, charge, affinity, and avidity or may form in situ in response to planted exogenous antigens with circulating immunoglobulins reaching the planted antigens or local endogenous antigens of specific cells. Circulating antibodies may also cross-react with antigens present within kidney parenchyma. Numerous antigens, including histones, or DNA bound to histones may be antigenic in SLE. When complexes are small and stable with high-affinity antibodies, these tend to localize in the mesangium and elicit a limited mesangial reaction with mesangial hypercellularity. Larger size or number of complexes with high-avidity antibodies may spill over to the subendothelial area, where inflammatory mechanisms are easily activated, including complement and leukocyte Fc receptors, resulting in infiltration of inflammatory cells and proliferation of endogenous cells, filling up the capillary lumens, so-called endocapillary proliferation. Over time, new matrix may be formed internal to the subendothelial deposits along with infiltrating interposed cells, resulting in the double contour visualized by silver stain. The presence of subepithelial immune deposits in lupus nephritis may result from dissociation of low-avidity and/or low-affinity complexes that reassemble after passing through the GBM. These deposits activate complement and perturb the adjacent podocyte, resulting in foot process effacement, a leaky capillary wall and proteinuria, and a GBM reaction visualized as spikes by silver stain.
5 Clinicopathologic Correlations
Classification of lupus nephritis is considered useful to describe the patient’s clinical status and for grouping patients with similar clinical profiles. For instance, membranous and diffuse proliferative forms usually present with proteinuria, and severe activity in a renal biopsy is usually associated with the clinical syndrome of a rapidly progressive glomerulonephritis. Moreover, the classification is related to prognosis with respect to renal function and patient survival [4]. The use of the lupus nephritis classification facilitates the ease and reliability with which nephrologists and nephropathologists communicate information and has improved standardization and reproducibility of biopsy interpretation [31]. In contrast, the prognostic value of the so-called activity and chronicity indices used by some in lupus nephritis is subject to discussion, and the utility of these indices is limited by concerns about their irreproducibility [6, 10, 11]. Nevertheless, distinguishing “active” and “sclerosing” lesions (Table 8.3) may help determine prognosis and sensitivity to treatment in both lupus and other glomerulonephritides [34–36]. In general, lesions that are potentially sensitive to treatment and reversible show activity, characterized by hypercellularity, leukocyte exudation, necrosis/karyorrhexis, cellular crescents, hyaline deposits, and interstitial inflammatory infiltrate. More chronic lesions less sensitive to treatment are glomerulosclerosis, fibrous crescents, tubular atrophy, and interstitial fibrosis [37]. Persistent macrophages in second biopsies after therapy portend worse prognosis [38]. Interstitial lesions are most severe in class IV. Interstitial inflammation, tubular atrophy, and interstitial fibrosis each have been independently associated with poor outcomes, and in turn, severe glomerular active lesions correlated with more interstitial inflammation. Sclerosis of glomeruli also correlated with tubular atrophy and interstitial fibrosis [29].
The persistence of subendothelial deposits has been associated with the progression of lupus nephritis, whereas a decrease in the amount of subendothelial and mesangial deposits was linked to a lower risk for renal impairment in SLE. Thus, patients with more proliferative lesions and more activity and chronicity had worse long-term outcomes [39].
Lupus lesions may not remain static over time in many patients. The type of glomerular lesion remains unchanged in about half of the cases. In the other half transformation occurs to either more ominous or more benign histologic patterns, the latter particularly under the influence of therapy. In patients with the most severe forms of lupus nephritis, a remission of clinical renal abnormalities, usually in response to aggressive treatment, is associated with dramatic improvement in long-term patient and renal survival [20, 40]. With current management strategies, in general the long-term outlook for patients with lupus nephritis has improved, but only a minority of patients are able to stop treatment altogether, and the incidence of serious complications is high [37, 41, 42], infection being the leading cause of death. Trials are ongoing of novel immunomodulatory drugs such as rituximab, which depletes B lymphocytes [43, 44]. Overall, only 10–15 % of patients with lupus nephritis now go into end-stage renal failure, with 10–30 % of those with class III, IV, or V reaching end-stage kidney disease within 15 years [4, 45].
References
Picken MM (1998) The role of kidney biopsy in the management of patients with systemic lupus erythematosus. Pathol Case Rev 3:204–209
Ruiz-Irastorza G, Khamashta MA, Castellino G, Hughes GRV (2001) Systemic lupus erythematosus. Lancet 357:1027–1032
Appel GB, Radhakrishnan J, D'Agati V (2007) The kidney, 8th edn. Saunders, Philadelphia
Cameron JS (1999) Lupus nephritis. J Am Soc Nephrol 10:413–424
Petri M (2005) Review of classification criteria for systemic lupus erythematosus. Rheum Dis Clin North Am 31:245–254
Weening JJ, d’Agati VD, Schwartz MM, Seshan SV, Alpers CE, Appel GB, Balow JE, Bruijn JA, Cook T, Ferrario F, Fogo AB, Ginzler EM, Hebert L, Hill G, Hill P, Jennette JC, Kong NC, Lesavre P, Lockshin M, Looi LM, Makino H, Moura LA, Nagata M, International Society of Nephrology Working Group on the Classification of Lupus Nephritis; Renal Pathology Society Working Group on the Classification of Lupus Nephritis (2004) The classification of glomerulonephritis in systemic lupus erythematosus revisited. J Am Soc Nephrol 15:241–250
Donadio JV Jr, Glassock RJ (1993) Immunosuppressive drug therapy in lupus nephritis. Am J Kidney Dis 21:239–250
Entani C, Izumino K, Iida H, Fujita M, Asaka M, Takata M, Sasayama S (1993) Effect of a novel immunosuppressant, FK506, on spontaneous lupus nephritis in MRL/MpJ-lpr/lpr mice. Nephron 64:471–475
Najafi CC, Korbet SM, Lewis EJ, Schwartz MM, Reichlin M, Evans J (2001) Significance of histologic patterns of glomerular injury upon long-term prognosis in severe lupus glomerulonephritis. Kidney Int 59:2156–2163
Schwartz MM, Lan S-P, Bernstein J, Hill GS, Holley K, Lewis EJ, Lupus Nephritis Collaboration Study Group (1992) Role of pathology indices in the management of severe lupus glomerulonephritis. Kidney Int 42:743–748
Schwartz MM, Lan S-P, Bernstein J, Hill GS, Holley K, Lewis EJ, Lupus Nephritis Collaboration Study Group (1993) Irreproducibility of the activity and chronicity indices limits their utility in the management of lupus nephritis. Am J Kidney Dis 21:374–377
Pasquali S, Banfi G, Zucchelli A, Moroni G, Ponticelli C, Zucchelli P (1993) Lupus membranous nephropathy: long-term outcome. Clin Nephrol 39:175–182
Mercadal L, Tezenas du Montcel S, Nochy D, Queffeulou G, Piette JC, Isnard-Bagnis C, Martinez F (2002) Factors affecting outcome and prognosis in membranous lupus nephropathy. Nephrol Dial Transplant 17:1771–1778
Jennette JC, Iskandar SS, Dalldorf FG (1983) Pathologic differentiation between lupus and nonlupus membranous glomerulopathy. Kidney Int 24:377–385
Haas M, Zikos D (1998) Membranous nephropathy. Distinction of latent membranous lupus nephritis from idiopathic membranous nephropathy on renal biopsy. Pathol Case Rev 3:175–179
Gunnarsson I, Schlumberger W, Rönnelid J (2012) Antibodies to M-type phospholipase A2 receptor (PLA2R) and membranous lupus nephritis. Am J Kidney Dis 59:585–586
Schwartz MM, Kawala K, Roberts JL, Humes C, Lewis EJ (1984) Clinical and pathological features of membranous glomerulonephritis of systemic lupus erythematosus. Am J Nephrol 4:301–311
D’Agati V, Fogo AB, Bruijn JA, Jennette JC (2004) Pathologic classification of focal segmental glomerulosclerosis: a working proposal. Am J Kidney Dis 2:368–382
Bruijn JA, Cotran RS (1992) The aging kidney: pathologic alterations. In: Martinez-Maldonado M (ed) Hypertension and renal disease in the elderly. Blackwell Scientific, Boston, pp 1–10
Giannico G, Fogo AB (2013) Lupus nephritis: is the kidney biopsy currently necessary in the management of lupus nephritis? Clin J Am Soc Nephrol 8:138–145
Dube GK, Markowitz GS, Radhakrishnan J, Appel GB, D’Agati VD (2002) Minimal change disease in systemic lupus erythematosus. Clin Nephrol 57:120–126
Kraft SW, Schwartz MM, Korbet SM, Lewis EJ (2005) Glomerular podocytopathy in patients with systemic lupus erythematosus. J Am Soc Nephrol 16:175–179
Han TS, Schwartz MM, Lewis EJ (2006) Association of glomerular podocytopathy and nephrotic proteinuria in mesangial lupus nephritis. Lupus 15:71–75
Barber C, Herzenberg A, Aghdassi E, Su J, Lou W, Qian G, Yip J, Nasr SH, Thomas D, Scholey JW, Wither J, Urowitz M, Gladman D, Reich H, Fortin PR (2012) Evaluation of clinical outcomes and renal vascular pathology among patients with lupus. Clin J Am Soc Nephrol 7:757–774
Appel GB, Pirani CL, D’Agati V (1994) Renal vascular complications of systemic lupus erythematosus. J Am Soc Nephrol 4:1499–1515
Banfi G, Bertani T, Boeri V, Faraggiana T, Mazzucco G, Monga G, Sacchi G (1991) Renal vascular lesions as a marker of poor prognosis in patients with lupus nephritis. Gruppo Italiano per lo Studio della Nefrite Lupica (GISNEL). Am J Kidney Dis 18:240–248
Park MH, D’Agati V, Appel GB, Pirani CL (1986) Tubulointerstitial disease in lupus nephritis: relationship to immune deposits, interstitial inflammation, glomerular changes, renal function, and prognosis. Nephron 44:309–319
Nath KA (1992) Tubulointerstitial changes as a major determinant in the progression of renal damage. Am J Kidney Dis 20:1–17
Yu F, Wu LH, Tan Y, Li LH, Wang CL, Wang WK, Qu Z, Chen MH, Gao JJ, Li ZY, Zheng X, Ao J, Zhu SN, Wang SX, Zhao MH, Zou WZ, Liu G (2010) Tubulointerstitial lesions of patients with LN classified by the 2003 International Society of Nephrology and Renal Pathology Society system. Kidney Int 77:820–829
Hayakawa S, Nakabayashi K, Karube M, Arimura Y, Soejima A, Yamada A, Fujioka Y (2006) Tubulointerstitial immune complex nephritis in a patient with systemic lupus erythematosus: role of peritubular capillaritis with immune complex deposits in the pathogenesis of the tubulointerstitial nephritis. Clin Exp Nephrol 10:146–151
Furness PN, Taub N (2006) Interobserver reproducibility and application of the ISN/RPS classification of lupus nephritis-a UK-wide study. Am J Surg Pathol 30:1030–1035
Schwartz MM, Korbet SM, Lewis EJ, Collaborative Study Group (2008) The prognosis and pathogenesis of severe lupus glomerulonephritis. Nephrol Dial Transplant 23:1298–1306
van der Vlag J, Berden JH (2011) Lupus nephritis: role of antinucleosome autoantibodies. Semin Nephrol 31:376–389
Bajema IM, Hagen EC, Hermans J, Noël LH, Waldherr R, Ferrario F, Van Der Woude FJ, Bruijn JA (1999) Kidney biopsy as a predictor for renal outcome in ANCA-associated necrotizing glomerulonephritis. Kidney Int 56:1751–1758
Hauer HA, Bajema IM, Hagen EC, Noël LH, Ferrario F, Waldherr R, van Houwelingen HC, Lesavre P, Sinico RA, van der Woude F, Gaskin G, Verburgh CA, de Heer E, Bruijn JA (2002) Long-term renal injury in ANCA- associated vasculitis: an analysis of 31 patients with follow-up biopsies. Nephrol Dial Transplant 17:587–596
Yoo CW, Kim M-K, Lee HS (2000) Predictors of renal outcome in diffuse proliferative lupus nephropathy: data from repeat renal biopsy. Nephrol Dial Transplant 15:1604–1608
Martins L, Rocha G, Rodrigues A, Santos J, Vasconcelos C, Correia J, Farinha F, Almeida I, Barbosa P, Guimarães S (2002) Lupus nephritis: a retrospective review of 78 cases from a single center. Clin Nephrol 57:114–119
Hill GS, Delahousse M, Nochy D, Rémy P, Mignon F, Méry JP, Bariéty J (2001) Predictive power of the second biopsy in lupus nephritis: significance of macrophages. Kidney Int 59:304–316
Contreras G, Pardo V, Cely C, Borja E, Hurtado A, De La Cuesta C, Iqbal K, Lenz O, Asif A, Nahar N, Leclerq B, Leon C, Schulman I, Ramirez-Seijas F, Paredes A, Cepero A, Khan T, Pachon F, Tozman E, Barreto G, Hoffman D, Almeida Suarez M, Busse JC, Esquenazi M, Esquenazi A, Garcia Mayol L, Garcia Estrada H (2005) Factors associated with poor outcomes in patients with lupus nephritis. Lupus 14:890–895
Korbet SM, Lewis EJ, Schwartz MM, Reichlin M, Evans J, Rohde RD (2000) Factors predictive of outcome in severe lupus nephritis. Am J Kidney Dis 35:904–914
Bono L, Cameron JS, Hicks JA (1999) The very long-term prognosis and complications of lupus nephritis and its treatment. Q J Med 92:211–218
Ward MM (2000) Changes in the incidence of end-stage renal disease due to lupus nephritis, 1982–1995. Arch Intern Med 160:3136–3140
Lightstone L (2013) Minimising steroids in lupus nephritis – will B cell depletion pave the way? Lupus 22:390–399
Hogan J, Appel GB (2013) Update on the treatment of lupus nephritis. Curr Opin Nephrol Hypertens 22:224–230
Maroz N, Segal MS (2013) Lupus nephritis and end-stage kidney disease. Am J Med Sci (in press)
Author information
Authors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
Fogo, A.B., Cohen, A.H., Colvin, R.B., Jennette, J.C., Alpers, C.E. (2014). Lupus Nephritis. In: Fundamentals of Renal Pathology. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-39080-7_8
Download citation
DOI: https://doi.org/10.1007/978-3-642-39080-7_8
Published:
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-39079-1
Online ISBN: 978-3-642-39080-7
eBook Packages: MedicineMedicine (R0)