Abstract
DRESS is a potentially life-threatening drug reaction that typically presents with a diffuse morbilliform rash, fever, lymphadenopathy, eosinophilia, and some level of systemic organ involvement. While traditionally it was thought to be a reaction to antiepileptic drugs and sulfa-containing antibiotics, DRESS can occur after use of any medication. One of the defining characteristics of DRESS is the delayed reaction to the offending medication (2–6 weeks), differentiating it from other drug reactions which typically occur immediately after medication exposure. Systemic involvement can affect any organ system, but the hematologic, hepatic, renal, pulmonary, and cardiac abnormalities are the most commonly involved. DRESS has a 10% mortality rate mostly resulting from fulminant hepatic failure. Treatment includes admission to an ICU/burn unit for supportive care, discontinuation of the offending drug/medication, close monitoring for systemic organ involvement, and high-dose steroids with a prolonged taper (up to 3 months or more). There may be a role for antivirals but there is no current data supporting such.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Drug reaction with eosinophilia and systemic symptoms
- Drug-induced hypersensitivity syndrome
- DRESS
- DHS
- DIHS
- Dermatology
- Drug rash
- Drug reaction
- Life-threatening rash
- Anticonvulsant hypersensitivity syndrome
- Drug-induced delayed multi-organ hypersensitivity syndrome
- Drug-induced pseudolymphoma
Background
Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome, also known as drug-induced hypersensitivity syndrome (DHS), is a rare but potentially lethal adverse drug reaction that classically manifests as a morbilliform rash with associated fever, lymphadenopathy, hematologic abnormalities, and multi-organ manifestations. While anticonvulsants and sulfonamides are the most common offending agents, many other drugs can cause DRESS syndrome. Systemic involvement can manifest with hematologic, hepatic, renal, pulmonary, cardiac, neurologic, gastrointestinal, and endocrine abnormalities [1].
The list of potential offending medications is long (see Table 20.1), but the most common culprits include carbamazepine, phenytoin, phenobarbital, lamotrigine, allopurinol, dapsone, and sulfasalazine [1]. DRESS syndrome is relatively rare, with an incidence of 1/5000 to 1/10,000 prescriptions of each of the causal agents [2,3,4,5]. Most cases affect adults without gender predilection, but rare cases have been reported in children [1]. DRESS syndrome carries a 10% mortality risk, usually due to hepatic failure [1].
The pathophysiology of DRESS syndrome remains incompletely understood but involves reactivation of herpesviruses (HHV-6, HHV-7, Epstein-Barr virus [EBV], and cytomegalovirus [CMV]), against which the body mounts a strong immune response [2, 6, 7]. The offending medications may not only affect epigenetic control mechanisms, thereby promoting viral reactivation, but also induce an antiviral T-cell response by interacting with the major histocompatibility complex receptors in individuals with genetic susceptibility [2]. Two theories currently exist regarding the pathophysiology of DRESS syndrome:
-
1.
Patients with predisposing genetic mutations lack the ability to metabolize certain medications leading to the accumulation of active drug metabolites that then trigger an autoimmune response and/or induce the reactivation of herpesviral infections [1].
-
2.
The reactivation of herpesviruses (mainly HHV-6, but also CMV, EBV, and HHV-7) is triggered by an allergic immune response to a drug with the subsequent activation of T-cell populations (particularly cytotoxic CD8+ lymphocytes) that cause direct tissue damage [1].
In both hypotheses, drug-related reactivation of herpesviral infections directly influences the immune attack on the patient’s skin and affected organs leading to the clinical manifestations of DRESS syndrome. Clinical features of DRESS, such as fever, edema, lymphadenopathy, hematologic expansion, and hepatitis, are consistent with those seen in a typical herpesvirus infection and support the hypothesis of a viral infection as a trigger of the syndrome.
Classic Clinical Presentation
The common initial symptoms of DRESS syndrome are fever, malaise, lymphadenopathy, and a skin eruption. A telling feature of DRESS syndrome is the delay of the onset of symptoms in relation to exposure to the offending medication. These symptoms typically occur 2–6 weeks following the initiation of the offending agent, which is prolonged in contrast to other types of drug eruptions [1, 2]. Medications taken for more than 3 months or initiated less than 2 weeks before the onset of DRESS syndrome are unlikely to be the culprit.
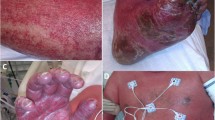
A diffuse morbilliform rash with associated pruritus is the most common cutaneous finding [1]. Occasionally the rash can generalize and progress to erythroderma (>90% involvement). The rash typically begins on the face with characteristic associated facial edema that appears similar to angioedema (Fig. 20.1). The rash then progresses to the upper trunk and arms (Fig. 20.2) and can also involve the lower extremities (Fig. 20.3). The rash often involves more than 50% of body surface area (BSA) [1]. Other possible cutaneous manifestations include vesicles, bullae, targetoid plaques, purpura, pustules, scaling, and mucosal inflammation with erosions [1] (Fig. 20.4).
Atypical Presentation
There are rare cases of DRESS syndrome that exist without “D” (causative drug relation), “R” (rash), “E” (eosinophilia), or “SS” systemic symptoms [9]. In one review of 216 cases over a 15-year period in France, they found a morbilliform eruption in only 70% of cases and eosinophilia in only 50% of cases [10].
Associated Systemic Symptoms
Hematologic and lymphatic involvement are common. Hematologic abnormalities occur in 30–90% of cases and diffuse lymphadenopathy occurs in 30–60% of cases [6, 8, 9]. Hematologic abnormalities include lymphocytosis, eosinophilia, and atypical lymphocytes (mononucleosis-like). Thrombocytopenia and anemia may also be present as part of a hemophagocytic syndrome. Lymphadenopathy is commonly present at cervical lymph nodes but can be found elsewhere and is typically found at multiple sites.
Associated systemic symptoms other than fever, malaise, and rash are directly related to the organ system involved (Table 20.2). Systemic involvement of at least one visceral organ occurs in approximately 90% of patients. The liver is the most common organ affected with 60–80% of cases showing liver impairment. Renal involvement occurs in 10–30% of cases and lung involvement occurs in 5–25% of cases [11,12,13]. Hepatic necrosis with fulminant liver failure is the most common cause of mortality in DRESS syndrome. Other organ systems that may be involved include the heart, gastrointestinal tract, pancreas, thyroid, neurologic system (brain and peripheral nerves), muscles, and eyes [9]. Clinical symptoms, laboratory abnormalities, and imaging studies will reflect specific organ involvement (Table 20.2). While multiple drugs can cause DRESS syndrome, some specific drugs have a predilection for specific organ dysfunction (Table 20.2) [16].
Key Physical Exam Findings and Diagnostic Features
A thorough history and physical examination should be performed. DRESS syndrome should be suspected in patients who have received a high-risk medication initiated within the past 2–6 weeks who present with a constellation of the following signs and symptoms [2]:
-
Morbilliform skin eruption that may progress to confluent and infiltrated erythema or exfoliative dermatitis.
-
Facial edema.
-
Fever (38–40°C).
-
Enlarged cervical lymph nodes and/or generalized lymphadenopathy
-
Systemic manifestations with organ involvement (hepatitis, nephritis, pneumonitis, carditis).
-
Histopathology of the skin biopsy can help exclude other entities but is most commonly non-specific .
Since DRESS syndrome cannot be diagnosed solely on the clinical signs and symptoms, a thorough initial evaluation for DRESS syndrome to exclude other causes would include CBC, BMP, LFTs, urinalysis, 24-h urine protein and urinary eosinophil count, CPK, LDH, ferritin, triglycerides, calcium, PTH, TSH, PT/PTT, lipase, serum protein electrophoresis, CRP, quantitative PCR (HHV-6, HHV-7, EBV, and CMV), blood culture, viral hepatitis serologies, and ANA.
Laboratory studies in DRESS syndrome:
-
CBC: eosinophilia, lymphocytosis, atypical lymphocytes
-
Liver function tests: ALT > 2× upper limit, Alk Phos >1.5× upper limit)
-
Creatinine and urinalysis (moderately increased creatinine, proteinuria, urinary sedimentation rate, eosinophilia)
Imaging/diagnostic studies in DRESS syndrome:
-
CXR/CT chest: interstitial pneumonitis and/or pleural effusion
-
Echocardiogram and electrocardiogram: pericarditis and/or myocarditis
-
Brain MRI: brain lesions
-
Skin biopsy: non-specific but can help to exclude other causes
Diagnosis
There is no reliable standard for the diagnosis of DRESS syndrome. Diagnostic criteria are based on clinical and laboratory findings. There are three known scoring systems that may be helpful in making the diagnosis of DRESS syndrome. The most commonly used in the United States and Europe is known as RegiSCAR [11]. The following table (Table 20.3) presents a scoring system for classifying DRESS cases as definite, probable, or no case based on the 201 cases reviewed in the RegiSCAR’s multinational registry [11, 18].
Common Mimics and Differential Diagnosis
Management
The cornerstone of treatment of DRESS syndrome is prompt diagnosis, discontinuation of the offending medication, aggressive supportive therapy, and high-dose steroids [8, 16]. Topical corticosteroids can be used for symptomatic relief, but high-dose systemic steroid therapy is generally required, especially when there is systemic organ involvement [16]. Current clinical recommendations are to start systemic steroids at a dose equivalent to at least 1 mg/kg/day of prednisone with increased dosing based on lack of clinical response or when there is significant organ involvement [8]. Steroids should be continued at that dose until adequate clinical response is obtained. Steroids then need to be tapered slowly, over 3–9 months, in order to prevent relapse [ 2, 16]. In particularly severe cases or in those unresponsive to oral steroids, high-dose IV methylprednisolone may be required for several days with transition to oral prednisone [16].
No prospective randomized trials are available upon which to base the management of DRESS syndrome. Antiviral agents, such as ganciclovir, foscarnet, or cidofovir, may be indicated if active viral replication is detected. However, there is no current data to support such and the potential toxicities of these agents limit their use [2, 17]. Patients with DRESS syndrome should be managed in an ICU or burn unit for appropriate care and infection control. In addition, appropriate specialists should be consulted based on the affected organ systems.
Disease Progression
Most cases of DRESS syndrome will resolve over the course of 2–9 weeks depending on the severity of the initial disease and institution of appropriate treatment [9]. Without proper treatment, symptoms may be persistent and approximately 20% of cases relapse [14]. Relapse usually occurs due to early termination of steroid therapy, reintroduction to the original offending medication, or reactivation of the involved herpesvirus [14, 15]. Those that develop severe organ involvement can progress to fulminant liver failure requiring liver transplantation, renal insufficiency requiring hemodialysis, or other long-term sequelae based on the affected organ system. Death occurs in 10% of cases, usually secondary to hepatic failure.
Prognosis
The severity of DRESS syndrome and associated complications are related to the organ involvement (Table 20.2) [2]. Most patients with DRESS recover completely in the weeks to months after drug withdrawal and appropriate therapy. Occasionally patients will have a prolonged course with flares despite discontinuation of the offending medication [ 2, 16]. Patients developing liver failure or multi-organ involvement are at risk for chronic complications or death [2]. Careful continued clinical monitoring is crucial as organ involvement may be delayed, and flares may occur, particularly when the glucocorticoid dose is tapered too fast or other drugs are introduced [2].
Complications
End-organ dysfunction can occur almost at any site, and multi-organ failure can lead to shock and disseminated intravascular coagulation. Liver failure is the most common cause of death, but renal and cardiac involvement can become severe and are often more difficult to control with steroids than the hepatic involvement. Endocrinopathies, such as thyroiditis, more often occur late and require continued clinical observation for several months. Other complications include dehydration and electrolyte imbalances, secondary bacterial or fungal infections, and sepsis related to the breakdown of the skin barrier.
Bottom Line: DRESS Clinical Pearls
-
Consider the diagnosis of DRESS syndrome in a patient with rash, facial edema, lymphadenopathy, eosinophilia, and systemic symptoms/organ involvement.
-
Delayed onset of rash after drug exposure. Occurs at 2–6 weeks after drug initiation (longer than most other drug eruptions).
-
Promptly discontinue the offending drug.
-
Obtain labs to evaluate for systemic organ involvement and appropriate imaging studies as indicated.
-
Admit to the intensive care or unit burn unit (if severe erosions) with prompt dermatology consultation.
-
Treatment includes high-dose steroid therapy of ≥ prednisone 1 mg/kg/day, perhaps IV methylprednisolone 1 g/day for several days in severe cases.
-
Prolonged steroid taper is required to prevent relapse (3–9 months).
-
Closely monitor patients’ clinical symptoms and labs after resolution for relapse or late complications (i.e., endocrinopathies).
References
Husain Z, Reddy BY, Schwartz RA. Dress syndrome: Part I. Clinical perspectives. J Am Acad Dermatol. 2013;68:693.
Descamps V, Ranger-Rogez S. Dress syndrome. Joint Bone Spine. 2014;81:15–21.
Fiszenson-Albala F, Auzerie V, Mahe E, et al. A 6-month prospective survey of cutaneous drug reactions in a hospital setting. Br J Dermatol. 2003;149:1018–22.
Tennis P, Sterns RS. Risk of serious cutaneous disorders after initiation of use of phenytoin, carbamazepine, or sodium valproate: a record linkage study. Neurology. 1997;49:542.
Guberman AH, Besag FM, Brodie MJ, et al. Lamotrigine-associated rash: risk/benefit consideration in adults and children. Epilepsia. 1999;40:985.
Shiohara T, et al. Drug-induced hypersensitivity syndrome (DIHS). A reaction induced by a complex interplay among herpesviruses and antiviral and antidrug immune responses. Allergol Int. 2006;55:1–8.
Picard D, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): a multiorgan antiviral T cell response. Sci Transl Med. 2010;2(46):46ra62.
Tas S, et al. Management of drug rash with eosinophilia and systemic symptoms (DRESS syndrome): an update. Dermatology. 2003;206:353–6.
Cacoub P, Mussett P, Descamps V, et al. The DRESS syndrome: a literature review. Am J Med. 2011;124:588.
Peyriere H, et al. Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: dose a DRESS syndrome really exist? Br J Dermatol. 2006;155:422–8.
Kardaun SH, Sekula P, Valeyrie-Allanore L, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): an original multisystem adverse drug reaction. Results from the prospective RegiSCAR study. Br J Dermatol. 2013;169:1071.
Lee T, Lee YS, Yoon SY, et al. Characteristics of liver injury in drug-induced systemic hypersensitivity reactions. J Am Acad Dermatol. 2013;69:407.
Lin IC, Yang HC, Strong C, et al. Liver injury in patients with DRESS: a clinical study of 72 cases. J Am Acad Dermatol. 2015;72:984.
Tetart F, Picard D, Janela B, et al. Prolonged evolution of drug reaction with eosinophilia and systemic symptoms: clinical, virologic, and biologic features. JAMA Dermatol. 2014;150:206.
Tohyama M, Hashimoto K, Yasukawa M, et al. Association of human herpesvirus 6 reactivation with the flaring and severity of drug-induced hypersensitivity syndrome. Br J Dermatol. 2007;157:934.
Husain Z, Reddy BY, Schwartz RA. Dress Syndrome: Part II. Management and therapeutics. J Am Acad Dermatol. 2013;68:702.
Moling O, et al. Treatment of DIHS/DRESS syndrome with combined N-acetylcysteine, prednisone and valganciclovir--a hypothesis. Med Sci Monit. 2012;18:cs57–63.
Kardaun SH, Sidoroff A, Valeryrie-Allanore L, et al. Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist? Br J Dermatol. 2007;156:609.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
DeClerck, M.P., DeClerck, B.K. (2018). DRESS Syndrome: Drug Reaction with Eosinophilia and Systemic Symptoms/Drug-Induced Hypersensitivity Syndrome (DHS). In: Rose, E. (eds) Life-Threatening Rashes. Springer, Cham. https://doi.org/10.1007/978-3-319-75623-3_20
Download citation
DOI: https://doi.org/10.1007/978-3-319-75623-3_20
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-75622-6
Online ISBN: 978-3-319-75623-3
eBook Packages: MedicineMedicine (R0)