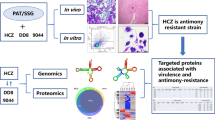
Abstract
The recent completion of the genomic sequencing of three species of Leishmania, L. (L.) major, L. (L.) infantum, and L. (V.) braziliensis has enormous relevance to the study of the leishmaniasis pathogenesis. However, since in Leishmania the control of gene expression relies on the stability or processing of the mature mRNA, as well as on the posttranslational modifications of proteins, the genomic sequences alone are insufficient to predict protein expression within the parasites. In this scenario, proteomic technologies provide feasible pathways to functional studies of this parasite. With the challenging increase of natural drug resistance by Leishmania, the combination of the available genomic resources of these parasites with powerful high-throughput proteomic analysis is urgently needed to shed light on resistance mechanisms and identify new drug targets against Leishmania. Diverse proteomic approaches have been used to describe and catalogue global protein profiles of Leishmania spp. reveal changes in protein expression during development, determine the subcellular localization of gene products, evaluate host-parasite interactions, and elucidate drug resistance mechanisms. The characterization of these proteins has advanced, although many fundamental questions remain unanswered. Here we discuss the recent proteomic discoveries that have contributed to the understanding of drug resistance mechanisms in Leishmania parasites.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
1 Introduction
Since the publication of the genome data from L. (L.) major [1], L. (L.) infantum, and L. (V.) braziliensis [2], over 14 Leishmania spp. genomes have been sequenced to date (http://tritrypdb.org/tritrypdb/). Such achievements, in addition to the accumulation of genomic data from other Leishmania species, strains, and clinical isolates (http://www.genedb.org/, http://www.uniprot.org/, [3]), offer the prospects of new drug target identification and/or the exploration of particular metabolic pathways for drug development.
For example, analysis of genomic data from L. (L.) infantum and L. (V.) braziliensis has revealed the presence of a gene encoding cyclopropane fatty acyl phospholipid synthase [2]. Because this enzyme appears to be involved in the maintenance of the parasite’s membrane and is not present in humans, it has been pointed as a putative chemotherapeutic target [2]. Such as this enzyme, many additional targets are probably encoded within the genome of Leishmania spp. The discovery of these targets is urgently needed given the increasing treatment failure observed with the mainstay chemotherapy, the pentavalent antimonials (SbV) [4], and the emergence of clinically resistant isolates [5,6,7,8,9,10,11,12].
Although all information concerning potential drug targets is contained in sequence databases, the promises of such target identifications are hampered by several factors. First, the limited functional annotation of the genomic sequence data determines that more than 50% of the predicted proteins have unknown functions [1, 2], which presents itself as an attractive challenge. Unfortunately, in 2017, 12 years after the first sequencing of a Leishmania genome, this scenario has not changed, and near 50% of the predicted proteins lacks functional annotation. Second, while the complexity of the cell cycle of these parasites would indicate that specific repertoires of genes are expressed in the promastigote and amastigote stages, global microarray genomic analyses have revealed that most Leishmania genes are constitutively transcribed [13,14,15], which is in agreement with the polycistronic organization of this parasite’s genome [1]. Third, of the approximately 8000–9000 coding genes found in Leishmania, ~6200 are common to all trypanosomatids sequenced thus far, ~1000 are Leishmania-specific, and only ~200 genes (including some pseudogenes) are species-specific [1, 2, 16,17,18]. Hence, the modest differences between the genome sequences of L. (L.) major, L. (L.) infantum, L. (V.) braziliensis, and L. (L.) mexicana do not reflect the vast differences among the clinical phenotypes of leishmaniasis that are associated with each of these species. Consequently, the Leishmania genome sequences alone are insufficient to predict whole protein expression profiles throughout the life cycle of the parasite or under specific drug pressure or other experimental conditions. Interestingly, genome heterogeneity arisen from large-scale gene copy number variation, and extensive aneuploidy is observed in natural Leishmania isolates in response to drug pressure [3, 19,20,21,22]. However, it is still unknown whether this variation in gene and chromosome copy number is followed by variation in protein abundance.
Gene regulation in Leishmania, as with other trypanosomatids, occurs principally at the posttranscriptional level [23, 24] mainly by mechanisms that involve RNA stabilization and 3′UTR signatures [25,26,27]. Seminal analyses of RNA transcripts using DNA microarrays in either broad gene expression studies [13, 14, 28,29,30,31] or studies limited to specific genes [32,33,34] have shown that less than 6 % of genes are modulated at the mRNA level during the different stages of the Leishmania life cycle. Gene expression studies specifically related to drug resistance in Leishmania have shown the same pattern [19, 20, 32, 35]. Changing this scenario, recently, RNA sequencing (RNA-seq) of L. (L.) mexicana transcriptome showed that over 3.000 genes (~40%) are differentially expressed between promastigotes and amastigotes [18].
Although mRNA quantification has resulted in the increase of knowledge of several cellular processes of Leishmania, the direct analysis of protein levels is advantageous because the relationship between transcript abundance and protein expression levels in this parasite has been shown to be poor [15, 36]. In addition, information concerning cellular localization, posttranslational modifications, or protein interactions cannot be obtained from mRNA data [37]. As aneuploidy and regulation at translational and posttranslational levels make the scenario of protein expression in this parasite more complex [36], high-resolution proteomic approaches have the potential of shedding light on protein patterns that define a clinical phenotype. This may include either a phenotype associated with a specific disease manifestation or one associated with the susceptibility or resistance to a specific drug.
Proteomic analyses, therefore, provide data that are of crucial significance for the description and comprehension of the biology of Leishmania parasites, which are not evident from the genome sequence or the mRNA transcripts. The proteome is defined as the set of proteins expressed by a cell or organism under specific conditions and at a given point in time. The field of proteomics intends to provide detailed descriptions and integration of protein data to better ascertain protein function in biological systems. By allowing the characterization of complex systems, proteomic approaches offer the opportunity to identify proteins involved with drug resistance in Leishmania, in addition to new drug targets for this parasite.
In general, most proteomic studies of Leishmania and other trypanosomatids involve protein fractionation from a protein mixture using SDS-PAGE and/or two-dimensional electrophoresis (2DE), followed by gel excision and enzymatic digestion of protein spots. Peptides are submitted to mass spectrometry (MS) methods that combine soft ionization sources [matrix-assisted laser desorption/ionization (MALDI) or electrospray ionization (ESI)] [38,39,40] with various mass analyzers. Subsequent protein identification is accomplished by linking mass spectral data to genome sequence databases using bioinformatics tools [41, 42]. Gel-free shotgun liquid chromatography tandem mass spectrometry (LC/MS/MS) analyses have the potential to map more thoughtfully the Leishmania proteome under different conditions [43,44,45]. High-resolution LC/MS/MS for quantitative analysis by isotopic labeling of proteins or even label-free approaches has in fact revealed new aspects of Leishmania stage-specific proteomes or specific parasite phenotypes [46,47,48,49,50,51,52,53].
Proteomic studies of Leishmania spp. have focused on global proteome profiling [46, 49, 54,55,56,57,58,59,60,61,62,63,64,65], detailed descriptions of stage-specific protein expression [14, 36, 43, 47, 51, 66,67,68,69,70,71,72,73,74,75,76], posttranslational modifications (PTMs) [44, 52, 59, 73, 77,78,79,80,81], identification of proteins from subcellular proteomes and secretomes [45, 71, 82,83,84,85,86,87,88,89,90,91], and determining potential drug targets or proteins involved in drug resistance [50, 53, 56, 64, 92,93,94,95,96,97,98,99,100], among others.
Proteomic studies for identifying molecules potentially involved in the drug resistance of Leishmania spp. can be classified according to the approach carried out using either (1) axenic promastigotes and/or amastigotes that have been selected to drug resistance in vitro or (2) axenic promastigotes and/or amastigotes derived from clinical isolates that are considered naturally drug resistant. The compounds evaluated in these studies include drugs currently used for the treatment of leishmaniasis, such as SbV, amphotericin-B (AMB), and miltefosine (MIL), in addition to model drugs for the study of resistance, such as methotrexate (MTX) and arsenite, and drug under development, such as bicyclic nitro drugs [24, 50, 53, 56, 79, 92,93,94,95,96,97,98,99, 101,102,103,104,105,106,107,108] (Table 10.1). This chapter will discuss the applications of proteomic approaches to the study of Leishmania drug resistance, focusing on the identified molecules and on the inferred mechanisms of resistance to current medicines used for the treatment of leishmaniasis.
2 Proteomic Approaches Used for Studying Drug Resistance in Leishmania spp.
2.1 Protein Expression Mapping by Two-Dimensional Electrophoresis
Proteomic studies of drug resistance in Leishmania spp. have traditionally used 2DE and 2D differential in-gel electrophoresis (2D-DIGE) for the comparative analysis of protein expression in drug-resistant and drug-sensitive parasites [56, 79, 92,93,94,95,96,97,98,99, 101,102,103,104,105,106,107,108]. This technique undoubtedly provided the basis for further developments in proteomics and, despite having certain limitations, is still used for protein expression mapping. The separation of complex cellular extracts by 2DE is achieved by coupling two independent electrophoretic separations, using isoelectric focusing in the first dimension and SDS-PAGE in the second [109, 110]. Soon after the first reports of 2DE appeared, this method was widely adopted by researchers around the world in several distinct applications [111,112,113].
The first works of what can be called the earliest Leishmania proteomics, even before the term “proteomics” was coined, came from the early 1980s. In these works, 2DE was used to (1) separate cell lysates of L. (L.) tropica for further detection of antigenic proteins using rabbit sera [114] and (2) for the comparative analysis of protein expression patterns from distinct Leishmania species that cause American tegumentary leishmaniasis with the aim of detecting species-specific markers [115]. However, issues concerning reproducibility, specifically involving the stability of the pH gradients, discouraged the widespread use of the method. Additionally, the absence of a protein identification system prevented the designation of interesting proteins. Identification was achieved by co-migration with purified proteins or through the use of antibodies. Using these methods, the regulation of tubulin expression during Leishmania differentiation was demonstrated [116]. Despite the drawbacks, valuable information was obtained, such as the demonstration that Leishmania resistance to MTX, an antiproliferative agent, is mediated by a mutation in the target enzyme, dihydrofolate reductase (DHFR), which alters the physicochemical properties of the protein [117].
The introduction of immobilized pH gradients in the first dimension [118] eliminated the reproducibility issues associated with pH stability. At the same time, N-terminal sequencing using traditional Edman chemistry applied to proteins separated by SDS-PAGE allowed the identification of peptides and proteins, as well as molecular mass determination [119]. However, it was the introduction of soft ionization techniques for peptides and proteins (MALDI and ESI) that allowed the acquisition of mass spectra of these molecules at the subnanomolar level and also changed the paradigm of protein identification [38,39,40]. Coupling 2DE and MS identification, Drummelsmith et al. observed up to a fourfold increase in the expression of several spots of trypanothione (TRYR) protein in transfected L. (L.) major promastigotes overexpressing the TRYR gene [56]. This assay validated the use of 2DE for drug resistance studies. Decades after 2D appeared, various studies started using fluorescent dyes, mainly the Cy dyes, which is the principle of 2D-DIGE, in order to achieve a more reliable quantification of differences among the spots detected [47, 81].
As mentioned above, all proteomic studies on Leishmania drug resistance have used the combination of 2DE or 2D-DIGE and MS for protein identification. However, 2DE presents major limitations, including the inability to resolve low abundance proteins and hydrophobic proteins, which represent important sources of information in the case of drug resistance mechanisms. Also in quantitative studies, the protein co-migration is a significant issue when deciding which protein contributed the more for the change in intensity observed in one spot. Despite these limitations, 2DE is a well-characterized technique for protein separation, and it is distinguished by its visual array that allows the detection of posttranslational modified states [120, 121].
2.2 Other Proteomic Approaches for Studying Drug Resistance
Although the use of fluorescent dyes has turned 2D-DIGE into a quantitative tool with better sensitivity and reproducibility than 2D, the gel-based approaches are still very limited regarding linearity, dynamic range, and reliability for quantifying differences in protein abundance, being limited to the resolution of soluble and abundant proteins [118, 122]. These limitations have been surpassed by the development of mass spectrometry (MS)-based approaches. In MS-based proteomic approaches, proteins can be identified and quantified by means of detection and quantification of their peptides [123]. The main methods include labeling with stable isotopes or label-free approaches. Labeling methods introduce a mass tag into proteins or peptides, either metabolically, enzymatically, or by chemical means; labeling based on isobaric tags for relative and absolute quantification (iTRAQ) and stable isotope labeling by amino acids in cell culture (SILAC) has been used in several proteomic analysis of Leishmania parasites enabling quantification of stage-specific proteins, characterization of posttranslational modifications, and quantification of protein abundance in parasites selected for drug resistance [48, 50, 53, 72, 78, 107, 124]. On the other hand, label-free methods correlate the ion intensity signal of peptide mass spectra or the number of peptide spectral counts with the protein quantity [122, 125, 126]. Shotgun label-free methods for protein quantification in Leishmania have been little explored, but there is a nice example of the potential of this approach in the quantitative analysis of the proteome of L. (L.) mexicana reported by Paape et al. [43].
Using high-throughput proteomic technologies, pharmacoproteomics allows discovery and validation of novel drug targets and generates information about drug metabolism and transport as well as about drug efficacy, resistance, and toxicity [127, 128]. Successful examples of these applications can be found in cancer research [129, 130]. Pharmacoproteomics has started to be used successfully in the study of drugs under development for leishmaniasis treatment [53].
3 Proteomics of Drug Resistance in Leishmania spp.
3.1 Proteomics of Model Drugs for Understanding Resistance in Leishmania: Methotrexate and Arsenite Resistance
Model drugs such as MTX and arsenite have been widely used for the study of molecular mechanisms of drug resistance in Leishmania [131,132,133,134,135,136]. In fact, much of the current knowledge of resistance mechanisms and novel potential drug targets in this genus came from studies using resistant parasites obtained after in vitro selection with these drugs [137,138,139,140]. The resistance of Leishmania to these compounds includes events such as DNA amplification [131, 141, 142], decreased drug accumulation, and increased drug efflux [98, 143,144,145], among others. Methotrexate is an anticancer drug that inhibits DHFR which is responsible for the conversion of dihydrofolate to tetrahydrofolate. Derivatives of tetrahydrofolate are essential for the biosynthesis of purines and pyrimidines. Therefore, in the presence of MTX, DNA synthesis is prevented. Although this antifolate is toxic to Leishmania, it was found to be much more toxic to mammalian cells than for the parasites, thus preventing its use as a chemotherapeutic agent for leishmaniasis [146].
The first recorded proteomic study on drug resistance in Leishmania was conducted using L. (L.) major promastigotes that were induced in vitro to MTX resistance [56]. Comparison of MTX-resistant parasites to sensitive parasites using 2DE revealed the overexpression of the pteridine reductase PTR1, a known primary mediator of MTX resistance. It was demonstrated that the PTR1 overexpression was due to several gene amplification events in the resistant parasites [56]. As PTR1 is able to reduce dihydrofolate to tetrahydrofolate to a minimal extent, its overexpression could compensate for the inhibition of DHFR by MTX [56].
In a further study, Drummelsmith et al. [92] observed that L. (L.) major MTX-resistant promastigotes exhibited increased expression of proteins involved in stress response, such as chaperonins, heat-shock proteins, and enolase, as well as enzymes such as argininosuccinate synthetase (ARGG), which catalyzes the penultimate step in arginine biosynthesis. As in the case of PTR1, the overexpression of ARGG was also the result of gene amplification events, which was most likely a result of the structural proximity of the PTR1 and ARGG coding genes [92]. Other proteins with less easily predicted roles in drug resistance, such as methionine adenosyltransferase (MAT), were also identified in this study. This enzyme is overexpressed both in sensitive cells shocked with MTX and in mutants resistant to the drug, suggesting that it may play a significant role in the initial cellular responses to MTX in L. (L.) major. Unlike other proteins, the overexpression of MAT was not due to gene amplification events [92]. In addition, it was observed that increases in S-adenosylmethionine level, which is synthesized by MAT, correlated with the selection and emergence of MTX resistance in L. major [92].
Finally, a proteomic analysis of L. (L.) donovani induced to arsenite resistance was reported. However, as 2DE gels from wild-type and arsenite-resistant parasites were completely different, comparison of the differential protein expression between the two conditions was precluded [101].
3.2 Proteomics of Antimonial Resistance
Pentavalent antimonials in the forms of sodium stibogluconate (Pentostam) and meglumine antimoniate (Glucantime) are first-line drugs for the treatment of distinct forms of leishmaniasis [147]. Despite the fact that SbV have been used worldwide for almost 80 years, reports on the clinical resistance and descriptions of resistant parasites started to appear within the last 20 years [4,5,6,7,8,9,10,11,12]. This situation is particularly alarming in India where widespread failure to SbV treatment in previously untreated patients has been reported [see Chap. 4 in this volume; 8, 148, 149]. Recently, it was demonstrated that arsenic contamination of drinking water might have contributed to the development of antimonial resistance in Leishmania parasites circulating in the Bihar region [150]. The complexity of the resistance scenario is augmented and sometimes obscured by the variation in the clinical response to SbV due to species-specific sensitivity to these drugs [see Chap. 15 in this volume; 4, 151, 152].
The understanding of the mechanism of action of SbV drugs and resistance to them has come from laboratory parasites, in which resistance has been selected in vitro by the pressure of the drug. For antileishmanial activity, it is necessary that the SbV be reduced to the trivalent form SbIII. Although debatable, reduction of the drug can apparently occur both in the macrophage and in the amastigote [153,154,155,156]. Reduction would be accomplished by either an enzymatic mechanism involving a thiol-dependent reductase [157] and/or an arsenate/antimonate reductase [158, 159] or by some nonenzymatic mechanism [160]. Regarding the internalization of the drug, it was demonstrated that AQP1, a transporter of trivalent metalloids [161], mediates the uptake of SbIII in Leishmania [162]. The expression level of aqp1 can correlate to the sensitivity to the drug [163, 164], and a major cluster of L. (L.) donovani isolates from the Indian subcontinent (ISC), which are resistant to SbV, presents a mutation in the aqp1 gene that results in a nonfunctional protein and therefore reduced influx of SbIII [3].
The activity of antimoniate seems to center around thiol redox metabolism [165], although early reports pointed to glycolytic and fatty acid β-oxidation pathways [166] or a programmed cell death (PCD) pathway involving DNA fragmentation non-mediated by caspase [167, 168]. On the other hand, increased levels of γ-glutamylcysteine synthetase and ornithine decarboxylase [137, 169], the enzymes involved in the synthesis of glutathione and polyamines, which are precursors of trypanothione, have been observed in parasites selected for resistance to SbIII or arsenite [137, 145]. As a consequence, accumulation of trypanothione and glutathione contributes to the resistant phenotype [165, 170]. In addition, mechanisms for the increased efflux of Sb-thiol complexes [145] and/or decreased drug influx mediated by decreased/nonfunctional AQP1, besides drug sequestration involving a P-glycoprotein member of the ABC transporters (PgpA/MRPA), as well as other transporters (ABCC4, ABCC5, MRP1), might also influence the antimonial resistance [163, 171,172,173,174,175,176,177]. Despite some controversies, it seems that resistance to antimony is a multifactorial phenomenon involving various mechanisms such as decreased drug uptake, diminished metal reduction, increased glutathione and trypanothione synthesis, and augmented drug efflux/sequestration [4, 139, 140, 178].
Proteomics of antimonial resistance have provided further evidence for some of the above mechanisms and have added new pieces to the resistance puzzle. Seminal studies comparing between SbIII-sensitive and in vitro selected SbIII-resistant axenic amastigotes of L. (L.) infantum using 2DE (pH range, 5–6) and ESI-MS/MS revealed some downregulated proteins in SbIII-resistant parasites, including the LACK receptor, β-tubulin, proteasome pa26 subunit, pyruvate kinase, and the kinetoplastid membrane protein 11 (KMP-11) [94]. Although none of these proteins had previously been associated with antimony resistance, several of them have been further observed in other Leishmania species selected for antimony resistance or other drugs [79, 95, 96, 102, 124] (Table 10.2).
Regarding KMP-11, Western blot analysis confirmed that the levels of KMP-11 were lower in SbIII-resistant parasites when compared to the parental wild-type parasites. However, overexpression of the protein did not alter the SbIII susceptibility of parasites. In addition, Northern blot analysis revealed that the downregulation of KMP-11 was not due to a decrease in mRNA levels [94]. Decrease of KMP-11 abundance was also observed in the phosphoproteome analysis of L. (V.) braziliensis selected for antimonial resistance [79]. In L. (L.) donovani, it was shown that KMP11 could increase the lipid bilayer pressure [179, 180]. Thus, the marked decreased level of KMP-11, probably due to an increased turnover rate of this protein, could alter the interaction of transporters or putative efflux systems, enhancing activity for pumping SbIII out of parasites [94]. On other hand, it has been proposed that the decrease of this protein could be part of a general mechanism of response to the stress caused by the drug pressure [79].
Argininosuccinate synthetase (ARGG) was the only protein identified as overexpressed in the L. (L.) infantum drug-resistant mutant. Increased abundance of ARGG was also observed in L. braziliensis resistant to antimonial [79] and in MTX-resistant L. (L.) major [92]. Both in SbV-resistant L. (L.) donovani and in MTX-resistant L. (L.) major, it was observed that the genomic region coding for this gene is amplified [20, 92], supporting the overexpression of ARGG [94]. However, the role that ARGG plays on resistance to SbV is unknown. The role in resistance of the other identified proteins remains to be established.
Regarding proteomic studies of field isolates, a proteomic analysis recently compared L. (L.) donovani parasites obtained from both a SbV-unresponsive and SbV-responsive patient to identify proteins involved in antimonial resistance [93]. First, the SbV-resistant and SbV-sensitive phenotypes of these isolates were corroborated by in vitro growth inhibition assays. Second, RT-PCR analysis showed that the expression levels of aqp1, gsh1, and PgpA (mrpa), which are genes associated with in vitro-induced resistance, were not differentially expressed between the sensitive and resistant clinical isolates. Third, it was shown that the parasites from the SbV-unresponsive patient were more resistant to SbIII- and SbV-induced PCD. The PCD features analyzed were the mitochondrial membrane potential (Δψm), DNA fragmentation, and externalization of phosphatidylserine residues followed by membrane permeabilization [93]. Thus, based on previous evidence suggesting that SbV kill Leishmania by a process involving several features of PCD [167, 168, 181], the soluble proteomes of these isolates naturally resistant and sensitive to SbV were analyzed by 2DE (pH range, 4–5) and MS/MS. Enolase, 14-3-3, ATP-dependent RNA helicase, dipeptidyl-peptidase III, 20 S proteasome α5 subunit, small kinetoplastid calpain-related protein SKCRP14.1, and many heat-shock proteins (HSP) were among the identified proteins. From this group, the 14-3-3 protein; the HSP83, whose abundances are increased in resistant parasites; and the SKCRP14.1, which is decreased in resistant parasites, were highlighted as having different roles in PCD. In fact, Leishmania HSP83 is an orthologue of the mammalian HSP90, which is involved in mitochondrial apoptotic pathways [182] (Table 10.2).
The genes coding for 14-3-3, HSP83, and SKCRP14.1 were cloned and the 14-3-3 and HSP83 constructs were transfected individually into the sensitive parasites, whereas the SKCRP14.1 construct was transfected into the resistant parasites [93]. While sensitive parasites transfected with the 14-3-3 construct did not show any increase in resistance to SbIII or SbV when compared with sensitive control parasites, the sensitive parasites overexpressing HSP83 were more than twofold resistant to SbIII compared with sensitive control parasites. In SbIII-treated parasites, a more intense drug-mediated DNA fragmentation was observed in the control parasites when compared to HSP83-overexpressing parasites. It was also found that after treatment with SbIII, the Δψm was higher in HSP83-overexpressing parasites than in control cells [93]. Overexpression of SKCRP14.1 increased the sensitivity of resistant parasites to SbIII and SbV, in addition to the sensitivity of transfectant parasites to SbIII-induced DNA fragmentation. After treatment with SbIII, no variations in the Δψm were observed between SKCRP14.1 transfectants and control cells [93]. As will be described below, several of these effects were also observed in MIL-treated parasites [93], which highlights the phenomenon of cross-resistance but also reveals contrasting mechanisms involved in Leishmania drug resistance. Hence, although the network of molecules through which HSP83 and SKCRP14.1 interfere with drug-induced PCD pathways in L. (L.) donovani remains to be elucidated, this study demonstrated that these proteins modulate drug susceptibility in this parasite. It remains to be established if these phenomena are observed in other L. (L.) donovani clinical isolates and in other Leishmania species for which resistance has been reported. Interestingly, it recently was demonstrated that antimony-resistant L. (L.) infantum exhibited decreased abundance of SKCRP14.1, reinforcing the observation that antimonial resistance is associated with a decrease in cell death-related proteins [106]. In addition, increased abundance of HSP83, as well other HSPs and chaperones, has been further observed in different Leishmania species selected for antimonial resistance [79, 95, 103,104,105,106, 124], including L. (L.) infantum, L. (V.) panamensis, and L. (V.) braziliensis (Table 10.2). Remarkably, parasites selected for MIL, amphotericin-B, or alpha-difluoromethylornithine resistance also present a significant increase in various heat-shock proteins [50, 96, 107, 108], suggesting that these proteins are part of a general response to the stress caused by the drug pressure. The increased protection against drug-related stress and drug-related programmed cell death may contribute to the resistance phenotype as a whole [79, 104], resulting in parasites able/adapted to cope with the oxidative stress caused by drug, probably by maintaining functional proteostasis mediated by HSPs.
Cell membrane proteins are very interesting for understanding drug transport in resistant parasites. In this context, Kumar et al. reported a set of overexpressed proteins in membrane- and cytosolic-enriched fractions of an L. (L.) donovani clinical isolate resistant to SbV, when compared to a sensitive isolate [102]. The six proteins identified in the membrane-enriched fraction were two ABC transporters, a fragment of HSP83, a cysteine-leucine-rich protein (CLrP), a GPI transamidase, and a 60S ribosomal protein (L23a). Remarkably, these authors further demonstrated that CLrP is a glycosylated protein with dual localization, in the membrane and nucleolus, whereas the 60s ribosomal L23a protein (60sRL23a) is localized in the cytosol [183, 184]. It was also shown that antimonial-resistant clinical isolates of L. (L.) donovani present higher mRNA and protein levels of CLrP and 60sRL23a as compared to antimonial-sensitive parasites [183, 184]. Overexpression of CLrP or 60sRL23a in a sensitive isolate of L. (L.) donovani significantly decreased its responsiveness to SbV and SbIII, in the case of CLrP, and also to MIL and paromomycin, in the case of 60sRL23a. Such reduction on drug sensitivity was followed by increased parasite infectivity to murine macrophages or increased proliferation rate, for CLrP- or 60sRL23a-overexpressing mutants, respectively [183, 184]. Such studies reveal that resistant parasites exhibit a higher fitness than sensitive parasites, showing increased infectivity capability to host cells and increased proliferation rate.
Metabolic isotopic labeling of L. (L.) infantum resistant to SbIII followed by comparative proteomic analysis of membrane and cytosolic fractions allowed the observation of increased levels of the ABC transporter MRPA (ABCC3) for the first time in a proteomic study [106]. The increased abundance of MRPA, a well-known protein involved in antimonial sequestration, was accompanied by alterations in the abundance of other transporters such as folate/biopterin transporters that presented diminished abundance in resistant parasites. Interestingly, folate/biopterin transporters have been previously pointed out as potential chemotherapeutic targets in Leishmania [185, 186].
It is pertinent to mention that in the proteomic studies that aimed to analyze Leishmania membrane proteins associated with drug resistance, the identification of a higher number of membrane proteins, more representative of this fraction, has been hampered possibly by the inherent limitation of 2DE for resolving hydrophobic proteins. Furthermore, the methods hitherto used for sample preparation do not favor the representativeness of such proteins. Such limitations can be overcome using better solubilizing agents and gel-free shotgun proteomic approaches, as demonstrated for other cells and tissues [187,188,189].
Seminal proteomic studies of antimonial resistance in L. (L.) donovani isolates identified β-tubulin, enolase, fructose-1,6-bisphosphate aldolase, the proteasome subunit α5, a carboxypeptidase, a fragment of HSP70, and the proliferative cell nuclear antigen (PCNA) [102]. Interestingly, further expression analyses, by Western blot and qPCR, confirmed that promastigote and amastigotes of resistant parasites exhibit ≥threefold and ~fivefold increased levels of PCNA, respectively, compared to the antimonial-sensitive parasites [190]. Overexpression of PCNA in antimonial-sensitive isolate resulted in significant increase of SbV IC50, and parasites overexpressing PCNA exhibited less DNA fragmentation compared to wild-type sensitive parasites upon treatment. In addition, parasites overexpressing PCNA modulated negatively nitric oxide (NO) production in infected macrophages [190].
Because many of the soluble proteins detected in drug resistance studies are among the abundant proteins commonly identified in proteomic studies of Leishmania and other trypanosomatids [59, 68, 71, 191], it is difficult to elucidate a clear role in resistance for them. However, as mentioned above, further proteomic analyses of Leishmania resistance mechanisms either to SbV or to other drugs have corroborated that HSPs, glycolytic enzymes, TCA-related enzymes, transcription-/translation-related proteins, peptidases, as well as DNA repair-related proteins, among other noncanonical resistance proteins, exhibit altered abundance in resistant parasites (Table 10.2) [50, 79, 95, 96, 103,104,105,106,107,108, 124]. Such findings reinforce the idea that resistant parasites exhibit a better general fitness than sensitive parasites, mediated by the (1) remodeling of their glycolytic metabolism, (2) increasing of virulence factor abundance, (3) and more efficient protein homeostasis and DNA repair, which together result in an increased proliferation and infectivity capability to host cells. Some of these phenotypic traits have been corroborated in a mutant Leishmania line that is deficient in glucose transport [100]. A detailed description of the association between fitness and drug resistance in Leishmania can be found in Chap. 15, this same volume. Proteomic studies of antimonial resistance have also shown that enzymes that are precursors of trypanothione, such as S-adenosylmethionine synthetase (SAMS) and S-adenosylhomocysteine hydrolase (SAHH), present increased abundance in L. (V.) panamensis, L. (L.) infantum, and L. (L.) donovani resistant parasites [95, 104, 124]. In addition, proteins involved in redox homeostasis, such as tryparedoxin, peroxiredoxin, and pteridine reductase, are also more abundant in resistant parasites [79, 95, 106]. Together, these findings corroborate the hypothesis that antimonial resistance is closely associated with nitrosative and oxidative stress resistance and remodels the parasite thiol redox metabolism.
3.3 Proteomics of Miltefosine Resistance
MIL [hexadecylphosphocholine (HePC]), an alkyl phospholipid compound, is the only oral drug currently available for the treatment of leishmaniasis. Originally intended for breast cancer treatment, MIL proved to be effective against Leishmania both in vitro and in animal models [192, 193]. This drug was registered and approved for visceral leishmaniasis (VL) treatment in India in 2002, followed by Germany in 2004. In Colombia in 2005, MIL was approved for the treatment of cutaneous leishmaniasis (CL), where it reached cure rates of over 91% [194, 195]. In 2005, the governments of India, Nepal, and Bangladesh adopted MIL as the first-line treatment for VL elimination [196, 197]. The oral administration of MIL avoids the need of patient hospitalization in VL cases and reduces the inconvenience of injectable drugs, augmenting treatment adherence [195, 198]. Despite the recent approval of MIL for disease treatment, clinical failures during treatment of VL and CL caused by different Leishmania species have already been reported [199,200,201]. MIL is registered for the oral treatment of canine leishmaniasis in several European countries since 2007 (Milteforan®) and was authorized recently (2016) for the treatment of dogs with VL in Brazil, despite studies showing that the improvement in the clinical symptoms was not followed by parasitological clearance [202]. In fact, that study did not recommend the use of MIL for dog treatment, especially in endemic areas of Brazil where dogs have a crucial role in the maintenance and transmission of the parasite [202]. In addition, failure treatment has been reported in naturally infected dogs treated with MIL [203].
Although MIL exhibits in vitro activity against various Leishmania species [204], the mechanism of action of this compound is not well understood. However, based on evidence obtained in tumor cell lines, it is known that MIL acts by triggering apoptotic pathways [205]. Evidences of PCD induced by MIL have also been reported for L. (L.) donovani promastigotes [206]. This drug appears to affect the integrity of cellular membranes by interfering with lipid metabolism, resulting in the decrease of phosphatidylcholine synthesis [207, 208]. In addition, intracellular drug accumulation seems to be required for the drug’s activity. Accumulation involves, among other steps, the translocation of the drug across the cellular membrane, which is accomplished with a recently identified complex of proteins including a P-type ATPase termed L. (L.) donovani MIL transporter (LdMT) and its β-subunit, LdRos3 [209]. Interestingly, the expression levels of these proteins are diminished in L. (V.) braziliensis, which would help to explain the low sensitivity of this species to the drug [210]. In addition, a common feature of MIL-resistant parasites consists of a decrease in drug accumulation mainly due to either the decreased uptake or increased efflux of the drug [211].
As described above, in L. (L.) donovani field isolates, HSP83 and SKCRP14.1 were implicated in the modulation of parasite sensitivity to SbV through a mechanism involving features of PCD [93]. In the same study, it was observed that SbV-resistant parasites were also cross-resistant to both MIL and AMB when compared with the SbV-sensitive parasites. It was also shown that the parasites from the SbV-unresponsive patient were more resistant to MIL-induced PCD. Besides being resistant to antimonial, the HSP83-overexpressing parasites were also resistant to MIL and were less sensitive to drug-mediated DNA fragmentation when compared to control parasites. In addition, 10 μM MIL first induced a more rapid hyperpolarization of the mitochondria in HSP83 transfectants when compared to the control cells, followed by a depolarization that took place more slowly in HSP83-overexpressing parasites than in control ones [93]. However, the effect of MIL treatment on SKCRP14.1-overexpressing parasites was the opposite of that observed with antimonial treatment. Resistant parasites transfected with SKCRP14.1 became more resistant to MIL compared with the transfectant control. In addition, SKCRP14.1 overexpression was significantly protected against MIL-induced mitochondrial depolarization and led to resistance against MIL-mediated DNA fragmentation when compared with the control [93]. These results reveal the contrasting roles of the proteins in the resistance mechanisms of Leishmania and highlight the importance of setting the individual action scenarios for each drug.
Recently, a study was conducted using a MIL-resistant L. (L.) donovani isolate, which was selected in vitro by sequential exposure to the drug [97]. In this study, the total cell extracts of sensitive and resistant promastigotes were analyzed by 2DE (pH range, 4–7), and two differentially expressed spots were identified by LC/MS/MS. The identified spots corresponded to the probable eukaryotic initiation factor 4A (eIF4A), a protein belonging to the DEAD-box subfamily of ATP-dependent helicases. This protein participates in the regulation of translation initiation, and it has been reported that its overexpression confers lithium resistance in Saccharomyces cerevisiae, probably by restoring protein synthesis [212].
In a recent study, Carnielli et al. used 2D-DIGE/MS to study the differences in protein abundances between MIL-sensitive and MIL-resistant L. (L.) infantum isolates from VL patients with different MIL treatment outcomes [96]. Among 46 spots exhibiting different intensity, 22 proteins were identified. Proteins with increased abundance in MIL-resistant isolates were associated with (1) redox homeostasis, such as peroxiredoxin and S-adenosylmethionine synthetase (SAMS); (2) stress response, including several HSPs; (3) DNA repair, such as PCNA and mitochondrial ATPase β-subunit; and (4) glycolytic and TCA-related enzymes, among others. A very similar group of proteins was observed in proteomic studies of L. (L.) infantum in vitro selected for amphotericin-B resistance [107] and in L. (L.) donovani selected for resistance against DL-α-difluoromethylornithine (DFMO), an inhibitor of ornithine decarboxylase, the first enzyme of the polyamine biosynthetic pathway [50] (Table 10.2). These results corroborate the multifactorial character of drug resistance phenomenon in Leishmania and also show that irrespective of the chemotherapy used to select the resistant lines, resistant parasites respond in similar ways to the drug pressure (either in vivo or in vitro) exhibiting increased resistance to oxidative and nitrosative stress, remodeling their glycolytic metabolism and increasing their virulence.
4 Proteomic Challenges in the Study of Drug Resistance
Proteomic studies of drug resistance in Leishmania have increased over the last decade. The reports reviewed here illustrate the value of proteomic approaches for the identification of proteins and mechanisms involved in resistance phenomenon. Those studies show that proteomic screens are useful in defining new roles for already well-characterized proteins in addition to assigning roles for proteins of unknown function. A summary of the proteins identified from proteomic studies using either resistant parasites selected in vitro or parasites from clinical isolates that are considered naturally drug resistant (proteins highlighted by the authors) is presented in Table 10.2. As can be seen in this table, many proteins identified in these studies have been implicated in Leishmania drug resistance using other approaches, but many other proteins are new or even unexpected in the scenario of drug resistance.
Several proteins classically described as being involved in various resistance mechanisms are membrane proteins, and this fraction has not been widely explored in drug resistance studies in Leishmania. This fact points to the first challenge: the deep analysis of distinct subcellular fractions of the parasite. Besides the contribution of protein annotation, subcellular proteomic analysis offers the possibility of inferring protein function and elucidating biochemical pathways in drug resistance, which can be exploited for purposes of drug development. In addition, it should be taken into account that the approach used for the proteomic studies revisited here has been 2DE, with the already mentioned limitations, applied to whole cell extracts and analyzing only some pH ranges. As a result, a large part of the Leishmania “resistance” proteome remains to be analyzed, which points to the second challenge: the need for a comprehensive proteomic study using better solubilizing detergents for sample preparation and gel-free methods [213] that ensures greater coverage of the proteome. Such an approach will require more powerful and specific bioinformatics tools to cope with the analysis of the enormous quantity of data that would be produced. In fact, data analysis represents a considerable bottleneck in the proteomic studies of parasites, mainly because ~50% of the coding genes do not have a functional annotation, which is why it represents the third challenge.
In very nice example of the exploitation of pharmacoproteomics for the study of drug targets and mechanisms of action, Wyllie et al. [53] studied by proteomic and genomic approaches the effects of bicyclic nitro-compounds on L. (L.) donovani. Nitro drugs are being used as part of a combination therapy for human African trypanosomiasis (HAT) [214], and bicyclic nitro-compounds are potential candidates for the treatment of VL (www.dndi.org). Comparing susceptible and drug-resistant parasites, authors identified the hypothetical NADH/FMN-dependent oxidoreductase as the activating nitroreductase (NTR2) and demonstrated that its overexpression rendered parasite hypersensitive to bicyclic nitro-compounds. In addition, it was demonstrated that knockout of NTR2 rendered parasites completely resistant to the compounds [53]. This study shows the potential of pharmacoproteomics to study drug mechanisms and resistance in trypanosomatids.
A common trait of proteomic studies in Leishmania, as well as in other organisms, is the recurrent identification of a group of proteins that correspond to the most abundant ones [215]. This precludes the identification of the less abundant proteins and obscures the studied phenomenon. Thus, a dedicated analysis of Leishmania most abundant proteins with the subsequent construction of an interactive database containing raw mass data and mass spectra data of these proteins would allow a better exploitation of the proteomic studies, saving time and optimizing resources [216]. In addition, the wide use of transfection models and the potential exploitation of a putative RNA interference (RNAi) pathway, at least in L. (Viannia) parasites [2, 217], would reinforce and complement the proteomic analysis of changes associated with drug resistance. Finally, as far as we know, proteomic studies of the resistance to other drugs used for leishmaniasis treatment, such as pentamidine, paromomycin, and azoles, have not been reported.
5 Concluding Remarks
As the cellular proteome is a dynamic scenario, it should be considered that inter- and intraspecific Leishmania genetic variation, in addition to host immune responses and host genetic background, might influence the resistant or sensitive phenotype of the parasites [218]. Thus, despite being rich and detailed, proteomic profiles represent specific patterns that need to be contextualized into a “biological system” level where the complexity must be governed by well-defined mechanisms. The continued advances in proteomic technology development, together with genome data and bioinformatics analysis, could reveal effective therapeutic strategies for species-specific treatments in the future, individualizing the epidemiological settings and valorizing the patients [219]. A large endeavor joining expertise, technologies, facilities, and knowledge would be desirable for obtaining and (re-) interpreting proteomic data of drug resistance in Leishmania.
References
Ivens AC, Peacock CS, Worthey EA, Murphy L, et al. The genome of the kinetoplastid parasite, Leishmania major. Science. 2005;309:436–42.
Peacock CS, Seeger K, Harris D, Murphy L, et al. Comparative genomic analysis of three Leishmania species that cause diverse human disease. Nat Genet. 2007;39:839–47.
Imamura H, Downing T, Van den Broeck F, Sanders MJ, et al. Evolutionary genomics of epidemic visceral leishmaniasis in the Indian subcontinent. Elife. 2016;5:e12613.
Croft SL, Sundar S, Fairlamb AH. Drug resistance in leishmaniasis. Clin Microbiol Rev. 2006;19:111–26.
Faraut-Gambarelli F, Piarroux R, Deniau M, Giusiano B, et al. In vitro and in vivo resistance of Leishmania infantum to meglumine antimoniate: a study of 37 strains collected from patients with visceral leishmaniasis. Antimicrob Agents Chemother. 1997;41:827–30.
Lira R, Sundar S, Makharia A, Kenney R, et al. Evidence that the high incidence of treatment failures in Indian kalaazar is due to the emergence of antimony-resistant strains of Leishmania donovani. J Infect Dis. 1999;180:564–7.
Palacios R, Osorio LE, Grajalew LF, Ochoa MT. Treatment failure in children in a randomized clinical trial with 10 and 20 days of meglumine antimonate for cutaneous leishmaniasis due to Leishmania Viannia species. Am J Trop Med Hyg. 2001;64:187–93.
Sundar S. Drug resistance in Indian visceral leishmaniasis. Trop Med Int Health. 2001;6:849–54.
Abdo MG, Elamin WM, Khalil EA, Mukhtar MM. Antimony-resistant Leishmania donovani in eastern Sudan: incidence and in vitro correlation. East Mediterr Health J. 2003;9:837–43.
Das VN, Ranjan A, Bimal S, Siddique NA, et al. Magnitude of unresponsiveness to sodium stibogluconate in the treatment of visceral leishmaniasis in Bihar. Natl Med J India. 2005;18:131–3.
Hadighi R, Mohebali M, Boucher P, Hajjaran H, et al. Unresponsiveness to Glucantime treatment in Iranian cutaneous leishmaniasis due to drug-resistant Leishmania tropica parasites. PLoS Med. 2006;3:e162.
Rojas R, Valderrama L, Valderrama M, Varona MX, et al. Resistance to antimony and treatment failure in human Leishmania (Viannia) infection. J Infect Dis. 2006;193:1375–83.
Holzer TR, McMaster WR, Forney JD. Expression profiling by whole-genome interspecies microarray hybridization reveals differential gene expression in procyclic promastigotes, lesion-derived amastigotes, and axenic amastigotes in Leishmania mexicana. Mol Biochem Parasitol. 2006;146:198–218.
Leifso K, Cohen-Freue G, Dogra N, Murray A, et al. Genomic and proteomic expression analysis of Leishmania promastigote and amastigote life stages: the Leishmania genome is constitutively expressed. Mol Biochem Parasitol. 2007;152:35–46.
Cohen-Freue G, Holzer TR, Forney JD, McMaster WR. Global gene expression in Leishmania. Int J Parasitol. 2007;37:1077–86.
El-Sayed NM, Myler PJ, Blandin G, Berriman M, et al. Comparative genomics of trypanosomatid parasitic protozoa. Science. 2005;309:404–9.
Rogers MB, Hilley JD, Dickens NJ, Wilkes J, et al. Chromosome and gene copy number variation allow major structural change between species and strains of Leishmania. Genome Res. 2011;21:2129–42.
Fiebig M, Kelly S, Gluenz E. Comparative life cycle transcriptomics revises Leishmania mexicana genome annotation and links a chromosome duplication with parasitism of vertebrates. PLoS Pathog. 2015;11:e1005186.
Ubeda JM, Légaré D, Raymond F, Ouameur AA, et al. Modulation of gene expression in drug resistant Leishmania is associated with gene amplification, gene deletion and chromosome aneuploidy. Genome Biol. 2008;9:R115.
Leprohon P, Légaré D, Raymond F, Hardiman G, et al. Gene expression modulation is associated with gene amplification, supernumerary chromosomes and chromosome loss in antimony-resistant Leishmania infantum. Nucleic Acids Res. 2009;37:1387–99.
Downing T, Imamura H, Decuypere S, Clark TG, et al. Whole genome sequencing of multiple Leishmania donovani clinical isolates provides insights into population structure and mechanisms of drug resistance. Genome Res. 2011;21:2143–56.
Mannaert A, Downing T, Imamura H, Dujardin JC. Adaptive mechanisms in pathogens: universal aneuploidy in Leishmania. Trends Parasitol. 2012;28:370–6.
Clayton C, Shapira M. Post-transcriptional regulation of gene expression in trypanosomes and leishmanias. Mol Biochem Parasitol. 2007;156:93–101.
Haile S, Papadopoulou B. Developmental regulation of gene expression in trypanosomatid parasitic protozoa. Curr Opin Microbiol. 2007;10:569–77.
Lee MG, Atkinson BL, Giannini SH, Van der Ploeg LH. Structure and expression of the hsp 70 gene family of Leishmania major. Nucleic Acids Res. 1988;16:9567–85.
Quijada L, Soto M, Alonso C, Requena JM. Analysis of post-transcriptional regulation operating on transcription products of the tandemly linked Leishmania infantum hsp70 genes. J Biol Chem. 1997;272:4493–9.
Holzer TR, Mishra KK, LeBowitz JH, Forney JD. Coordinate regulation of a family of promastigote-enriched mRNAs by the 3′UTR PRE element in Leishmania mexicana. Mol Biochem Parasitol. 2008;157:54–64.
Saxena A, Lahav T, Holland N, Aggarwal G, et al. Analysis of the Leishmania donovani transcriptome reveals an ordered progression of transient and permanent changes in gene expression during differentiation. Mol Biochem Parasitol. 2007;152:53–65.
Almeida R, Gilmartin BJ, McCann SH, Norrish A, et al. Expression profiling of the Leishmania life cycle: cDNA arrays identify developmentally regulated genes present but not annotated in the genome. Mol Biochem Parasitol. 2004;136:87–100.
Akopyants NS, Matlib RS, Bukanova EN, Smeds MR, et al. Expression profiling using random genomic DNA microarrays identifies differentially expressed genes associated with three major developmental stages of the protozoan parasite Leishmania major. Mol Biochem Parasitol. 2004;136:71–86.
Rochette A, Raymond F, Ubeda JM, Smith M, et al. Genome-wide gene expression profiling analysis of Leishmania major and Leishmania infantum developmental stages reveals substantial differences between the two species. BMC Genomics. 2008;9:255.
Guimond C, Trudel N, Brochu C, Marquis N, et al. Modulation of gene expression in Leishmania drug resistant mutants as determined by targeted DNA microarrays. Nucleic Acids Res. 2003;31:5886–96.
Quijada L, Soto M, Requena JM. Genomic DNA macroarrays as a tool for analysis of gene expression in Leishmania. Exp Parasitol. 2005;111:64–70.
Depledge DP, Evans KJ, Ivens AC, Aziz N, et al. Comparative expression profiling of Leishmania: modulation in gene expression between species and in different host genetic backgrounds. PLoS Negl Trop Dis. 2009;3:e476.
Leprohon P, Légaré D, Girard I, Papadopoulou B, et al. Modulation of Leishmania ABC protein gene expression through life stages and among drug-resistant parasites. Eukaryot Cell. 2006;5:1713–25.
McNicoll F, Drummelsmith J, Müller M, Madore E, et al. A combined proteomic and transcriptomic approach to the study of stage differentiation in Leishmania infantum. Proteomics. 2006;6:3567–81.
Walther TC, Mann M. Mass spectrometry-based proteomics in cell biology. J Cell Biol. 2010;190:491–500.
Karas M, Hillemkamp F. Laser desorption ionization of proteins with molecular masses exceeding 10000 kDa. Anal Chem. 1988;60:2299–301.
Tanaka K, Waki H, Ido Y, Akita S, et al. Protein and polymer analyses up to m/z 100000 by laser ionization time-of-flight mass spectrometry. Rapid Commun Mass Spectrom. 1988;2:151–3.
Fenn J, Mann M, Meng CK, Wong SF, et al. Electrospray ionization for mass spectrometry of large biomolecules. Science. 1989;246:64–71.
Cuervo P, Domont GB, De Jesus JB. Proteomics of trypanosomatids of human medical importance. J Proteomics. 2010;73:845–67.
Paape D, Aebischer T. Contribution of proteomics of Leishmania spp. to the understanding of differentiation, drug resistance mechanisms, vaccine and drug development. J Proteomics. 2011;74:1614–24.
Paape D, Barrios-Llerena ME, Le BT, Mackay L, et al. Gel free analysis of the proteome of intracellular Leishmania mexicana. Mol Biochem Parasitol. 2010;169:108–14.
Tsigankov P, Gherardini PF, Helmer-Citterich M, Späth GF, et al. Phosphoproteomic analysis of differentiating Leishmania parasites reveals a unique stage-specific phosphorylation motif. J Proteome Res. 2013;12:3405–12.
Braga MS, Neves LX, Campos JM, Roatt BM, et al. Shotgun proteomics to unravel the complexity of the Leishmania infantum exoproteome and the relative abundance of its constituents. Mol Biochem Parasitol. 2014;195:43–53.
Pawar H, Sahasrabuddhe NA, Renuse S, Keerthikumar S, et al. A proteogenomic approach to map the proteome of an unsequenced pathogen - Leishmania donovani. Proteomics. 2012;12:832–44.
Pescher P, Blisnick T, Bastin P, Spath GF. Quantitative proteome profiling informs on phenotypic traits that adapt Leishmania donovani for axenic and intracellular proliferation. Cell Microbiol. 2011;13:978–91.
Biyani N, Madhubala R. Quantitative proteomic profiling of the promastigotes and the intracellular amastigotes of Leishmania donovani isolates identifies novel proteins having a role in Leishmania differentiation and intracellular survival. Biochim Biophys Acta. 2012;1824:1342–50.
Sardar AH, Kumar S, Kumar A, Purkait B, et al. Proteome changes associated with Leishmania donovani promastigote adaptation to oxidative and nitrosative stresses. J Proteomics. 2013;81:185–99.
Singh AK, Roberts S, Ullman B, Madhubala R. A quantitative proteomic screen to identify potential drug resistance mechanism in alpha-difluoromethylornithine (DFMO) resistant Leishmania donovani. J Proteomics. 2014;102:44–59.
Tsigankov P, Gherardini PF, Helmer-Citterich M, Späth GF, et al. Regulation dynamics of Leishmania differentiation: deconvoluting signals and identifying phosphorylation trends. Mol Cell Proteomics. 2014;13:1787–99.
Zilberstein D. Proteomic analysis of posttranslational modifications using iTRAQ in Leishmania. Methods Mol Biol. 2015;1201:261–8.
Wyllie S, Roberts AJ, Norval S, Patterson S, et al. Activation of bicyclic nitro-drugs by a novel nitroreductase (NTR2) in Leishmania. PLoS Pathog. 2016;12:e1005971.
Acestor N, Masina S, Walker J, Saravia NG, et al. Establishing two-dimensional gels for the analysis of Leishmania proteomes. Proteomics. 2002;2:877–9.
Góngora R, Acestor N, Quadroni M, Fasel N, et al. Mapping the proteome of Leishmania Viannia parasites using two-dimensional polyacrylamide gel electrophoresis and associated technologies. Biomédica. 2003;23:153–60.
Drummelsmith J, Brochu V, Girard I, Messier N, et al. Proteome mapping of the protozoan parasite Leishmania and application to the study of drug targets and resistance mechanisms. Mol Cell Proteomics. 2003;2:146–55.
Brobey RK, Mei FC, Cheng X, Soong L. Comparative two-dimensional gel electrophoresis maps for promastigotes of Leishmania amazonensis and Leishmania major. Braz J Infect Dis. 2006;10:1–6.
Brobey RK, Soong L. Establishing a liquid-phase IEF in combination with 2-DE for the analysis of Leishmania proteins. Proteomics. 2007;7:116–20.
Cuervo P, de Jesus JB, Junqueira M, Mendonça-Lima L, et al. Proteome analysis of Leishmania (Viannia) braziliensis by two-dimensional gel electrophoresis and mass spectrometry. Mol Biochem Parasitol. 2007;154:6–21.
Costa MM, Andrade HM, Bartholomeu DC, Freitas LM, et al. Analysis of Leishmania chagasi by 2-D difference gel electrophoresis (2-D DIGE) and immunoproteomic: identification of novel candidate antigens for diagnostic tests and vaccine. J Proteome Res. 2011;10:2172–84.
Aebischer T. Leishmania spp. proteome data sets: a comprehensive resource for vaccine development to target visceral leishmaniasis. Front Immunol. 2014;5:260.
da Fonseca Pires S, Fialho LC Jr, Silva SO, Melo MN, et al. Identification of virulence factors in Leishmania infantum strains by a proteomic approach. J Proteome Res. 2014;13:1860–72.
McCall LI, Zhang WW, Dejgaard K, Atayde VD, et al. Adaptation of Leishmania donovani to cutaneous and visceral environments: in vivo selection and proteomic analysis. J Proteome Res. 2015;14:1033–59.
Alcolea PJ, Tuñón GI, Alonso A, García-Tabares F, et al. Differential protein abundance in promastigotes of nitric oxide-sensitive and resistant Leishmania chagasi strains. Proteomics Clin Appl. 2016;10:1132–46.
Yau WL, Lambertz U, Colineau L, Pescher P, et al. Phenotypic characterization of a Leishmania donovani cyclophilin 40 null mutant. J Eukaryot Microbiol. 2016;63:823–33.
Thiel M, Bruchhaus I. Comparative proteome analysis of Leishmania donovani at different stages of transformation from promastigotes to amastigotes. Med Microbiol Immunol. 2001;190:33–6.
El Fakhry Y, Ouellette M, Papadopoulou B. A proteomic approach to identify developmentally regulated proteins in Leishmania infantum. Proteomics. 2002;2:1007–17.
Bente M, Harder S, Wiesgigl M, Heukeshoven J, et al. Developmentally induced changes of the proteome in the protozoan parasite Leishmania donovani. Proteomics. 2003;3:1811–29.
Nugent PG, Karsani SA, Wait R, Tempero J, et al. Proteomic analysis of Leishmania mexicana differentiation. Mol Biochem Parasitol. 2004;136:51–62.
Walker J, Vasquez JJ, Gomez MA, Drummelsmith J, et al. Identification of developmentally-regulated proteins in Leishmania panamensis by proteome profiling of promastigotes and axenic amastigotes. Mol Biochem Parasitol. 2006;147:64–73.
Foucher AL, Papadopoulou B, Ouellette M. Prefractionation by digitonin extraction increases representation of the cytosolic and intracellular proteome of Leishmania infantum. J Proteome Res. 2006;5:1741–50.
Rosenzweig D, Smith D, Opperdoes F, Stern S, et al. Retooling Leishmania metabolism: from sand fly gut to human macrophage. FASEB J. 2008a;22:590–602.
Morales MA, Watanabe R, Laurent C, Lenormand P, et al. Phosphoproteomic analysis of Leishmania donovani pro- and amastigote stages. Proteomics. 2008;8:350–63.
Mojtahedi Z, Clos J, Kamali-Sarvestani E. Leishmania major: identification of developmentally regulated proteins in procyclic and metacyclic promastigotes. Exp Parasitol. 2008;119:422–9.
Paape D, Lippuner C, Schmid M, Ackermann R, et al. Transgenic, fluorescent Leishmania mexicana allow direct analysis of the proteome of intracellular amastigotes. Mol Cell Proteomics. 2008;7:1688–701.
Nirujogi RS, Pawar H, Renuse S, Kumar P, et al. Moving from unsequenced to sequenced genome: reanalysis of the proteome of Leishmania donovani. J Proteomics. 2014;97:48–61.
Rosenzweig D, Smith D, Myler PJ, Olafson RW, et al. Post-translational modification of cellular proteins during Leishmania donovani differentiation. Proteomics. 2008b;8:1843–50.
Hem S, Gherardini PF, Osorio y Fortéa J, Hourdel V, et al. Identification of Leishmania-specific protein phosphorylation sites by LC-ESI-MS/MS and comparative genomics analyses. Proteomics. 2010;10:3868–83.
Moreira D de S, Pescher P, Laurent C, Lenormand P, et al. Phosphoproteomic analysis of wild-type and antimony-resistant Leishmania braziliensis lines by 2D-DIGE technology. Proteomics. 2015;15:2999–3019.
Bachmaier S, Witztum R, Tsigankov P, Koren R, et al. Protein kinase A signaling during bidirectional axenic differentiation in Leishmania. Int J Parasitol. 2016;46:75–82.
Morales MA, Watanabe R, Dacher M, Chafey P, et al. Phosphoproteome dynamics reveal heat-shock protein complexes specific to the Leishmania donovani infectious stage. Proc Natl Acad Sci USA. 2010;107:8381–6.
de Oliveira AH, Ruiz JC, Cruz AK, Greene LJ, et al. Subproteomic analysis of soluble proteins of the microsomal fraction from two Leishmania species. Comp Biochem Physiol Part D Genomic Proteomics. 2006;1:300–8.
Hide M, Ritleng AS, Brizard JP, Monte-Allegre A, et al. Leishmania infantum: tuning digitonin fractionation for comparative proteomic of the mitochondrial protein content. Parasitol Res. 2008;103:989–92.
Silverman JM, Chan SK, Robinson DP, Dwyer DM, et al. Proteomic analysis of the secretome of Leishmania donovani. Genome Biol. 2008;9:R35.
Cuervo P, De Jesus JB, Saboia-Vahia L, Mendonça-Lima L, et al. Proteomic characterization of the released/secreted proteins of Leishmania (Viannia) braziliensis promastigotes. J Proteomics. 2009;73:79–92.
Brotherton MC, Racine G, Ouameur AA, Leprohon P, et al. Analysis of membrane-enriched and high molecular weight proteins in Leishmania infantum promastigotes and axenic amastigotes. J Proteome Res. 2012;11:3974–85.
Lynn MA, Marr AK, McMaster WR. Differential quantitative proteomic profiling of Leishmania infantum and Leishmania mexicana density gradient separated membranous fractions. J Proteomics. 2013;82:179–92.
Santarém N, Racine G, Silvestre R, Cordeiro-da-Silva A, et al. Exoproteome dynamics in Leishmania infantum. J Proteomics. 2013;84:106–18.
Atayde VD, Aslan H, Townsend S, Hassani K, et al. Exosome secretion by the parasitic protozoan Leishmania within the sand fly midgut. Cell Rep. 2015;13:957–67.
Kumar A, Misra P, Sisodia B, Shasany AK, et al. Proteomic analyses of membrane enriched proteins of Leishmania donovani Indian clinical isolate by mass spectrometry. Parasitol Int. 2015;64:36–42.
Lima BS, Fialho LC Jr, Pires SF, Tafuri WL, et al. Immunoproteomic and bioinformatic approaches to identify secreted Leishmania amazonensis, L. braziliensis, and L. infantum proteins with specific reactivity using canine serum. Vet Parasitol. 2016;223:115–9.
Drummelsmith J, Girard I, Trudel N, Ouellette M. Differential protein expression analysis of Leishmania major reveals novel roles for methionine adenosyltransferase and S-adenosylmethionine in methotrexate resistance. J Biol Chem. 2004;279:33273–80.
Vergnes B, Gourbal B, Girard I, Sundar S, et al. A proteomics screen implicates HSP83 and a small kinetoplastid calpain-related protein in drug resistance in Leishmania donovani clinical field isolates by modulating drug-induced programmed cell death. Mol Cell Proteomics. 2007;6:88–101.
El Fadili K, Drummelsmith J, Roy G, Jardim A, et al. Down regulation of KMP-11 in Leishmania infantum axenic antimony resistant amastigotes as revealed by a proteomic screen. Exp Parasitol. 2009;123:51–7.
Matrangolo FS, Liarte DB, Andrade LC, de Melo MF, et al. Comparative proteomic analysis of antimony-resistant and -susceptible Leishmania braziliensis and Leishmania infantum chagasi lines. Mol Biochem Parasitol. 2013;190:63–75.
Carnielli JB, de Andrade HM, Pires SF, Chapeaurouge AD, et al. Proteomic analysis of the soluble proteomes of miltefosine-sensitive and -resistant Leishmania infantum chagasi isolates obtained from Brazilian patients with different treatment outcomes. J Proteomics. 2014;108:198–208.
Singh G, Chavan HD, Dey CS. Proteomic analysis of miltefosine-resistant Leishmania reveals the possible involvement of eukaryotic initiation factor 4A (eIF4A). Int J Antimicrob Agents. 2008a;31:584–6.
Singh G, Jayanarayan KG, Dey CS. Arsenite resistance in Leishmania and possible drug targets. Adv Exp Med Biol. 2008b;625:1–8.
Vincent IM, Racine G, Légaré D, Ouellette M. Mitochondrial proteomics of antimony and miltefosine resistant Leishmania infantum. Proteomes. 2015;3:328–46.
Akpunarlieva S, Weidt S, Lamasudin D, Naula C, et al. Integration of proteomics and metabolomics to elucidate metabolic adaptation in Leishmania. J Proteomics. 2017;155:85–98.
Sharma S, Singh G, Chavan HD, Dey CS. Proteomic analysis of wild type and arsenite-resistant Leishmania donovani. Exp Parasitol. 2009;123:369–76.
Kumar A, Sisodia B, Misra P, Sundar S, et al. Proteome mapping of overexpressed membrane-enriched and cytosolic proteins in sodium antimony gluconate (SAG) resistant clinical isolate of Leishmania donovani. Br J Clin Pharmacol. 2010;70:609–17.
Peláez RG, Muskus CE, Cuervo P, Marín-Villa M. Differential expression of proteins in Leishmania (Viannia) panamensis associated with mechanisms of resistance to meglumine antimoniate. Biomedica. 2012;32:418–29.
Walker J, Gongora R, Vasquez JJ, Drummelsmith J, et al. Discovery of factors linked to antimony resistance in Leishmania panamensis through differential proteome analysis. Mol Biochem Parasitol. 2012;183:166–76.
Messaritakis I, Christodoulou V, Mazeris A, Koutala E, et al. Drug resistance in natural isolates of Leishmania donovani s.l. promastigotes is dependent of Pgp170 expression. PLoS One. 2013;8:e65467.
Brotherton MC, Bourassa S, Leprohon P, Légaré D, et al. Proteomic and genomic analyses of antimony resistant Leishmania infantum mutant. PLoS One. 2013;8:e81899.
Brotherton MC, Bourassa S, Légaré D, Poirier GG, et al. Quantitative proteomic analysis of amphotericin B resistance in Leishmania infantum. Int J Parasitol Drugs Drug Resist. 2014;4:126–32.
Vacchina P, Norris-Mullins B, Carlson ES, Morales MA. A mitochondrial HSP70 (HSPA9B) is linked to miltefosine resistance and stress response in Leishmania donovani. Parasit Vectors. 2016;9:621.
MacGillivray AJ, Rickwood D. The heterogeneity of mouse-chromatin nonhistone proteins as evidenced by two-dimensional polyacrylamide-gel electrophoresis and ion-exchange chromatography. Eur J Biochem. 1974;41:181–90.
O’Farrell PH. High resolution two-dimensional electrophoresis of proteins. J Biol Chem. 1975;250:4007–21.
Anderson L, Anderson NG. High resolution two-dimensional electrophoresis of human plasma proteins. Proc Natl Acad Sci USA. 1977;74:5421–5.
Bravo R, Celis JE. A search for differential polypeptide synthesis throughout the cell cycle of HeLa cells. J Cell Biol. 1980;84:795–802.
Taylor J, Anderson NL, Scandora AE Jr, Willard KE, et al. Design and implementation of a prototype human protein index. Clin Chem. 1982;28:861–6.
Handman E, Mitchell GF, Goding JW. Identification and characterization of protein antigens of Leishmania tropica isolates. J Immunol. 1981;126:508–12.
Saravia NG, Gemmell MA, Nance SL, Anderson NL. Two-dimensional electrophoresis used to differentiate the causal agents of American tegumentary leishmaniasis. Clin Chem. 1984;30:2048–52.
Fong D, Chang KP. Tubulin biosynthesis in the developmental cycle of a parasitic protozoan, Leishmania mexicana: changes during differentiation of motile and nonmotile stages. Proc Natl Acad Sci USA. 1981;78:7624–8.
Arrebola R, Olmo A, Reche P, Garvey EP, et al. Isolation and characterization of a mutant dihydrofolate reductase-thymidylate synthase from methotrexate-resistant Leishmania cells. J Biol Chem. 1994;269:10590–6.
Görg A, Postel W, Günther S. The current state of two-dimensional electrophoresis with immobilized pH gradients. Electrophoresis. 1988;9:531–46.
Matsudaira PT. Sequence from picomole quantities of proteins electroblotted onto polyvinylidene difluoride membranes. J Biol Chem. 1987;262:10035–8.
Carrette O, Burkhard PR, Sanchez JC, Hochstrasser DF. State-of-the-art two-dimensional gel electrophoresis: a key tool of proteomics research. Nat Protoc. 2006;1:812–23.
Rabilloud T, Chevallet M, Luche S, Lelong C. Two-dimensional gel electrophoresis in proteomics: past, present and future. J Proteomics. 2010;73:2064–77.
Bantscheff M, Lemeer S, Savitski MM, Kuster B. Quantitative mass spectrometry in proteomics: critical review update from 2007 to the present. Anal Bioanal Chem. 2012;404:939–65.
Duncan MW, Aebersold R, Caprioli RM. The pros and cons of peptide-centric proteomics. Nat Biotechnol. 2010;28:659–64.
Biyani N, Singh AK, Mandal S, Chawla B. Differential expression of proteins in antimony-susceptible and -resistant isolates of Leishmania donovani. Mol Biochem Parasitol. 2011;179:91–9.
Altelaar AF, Munoz J, Heck AJ. Next-generation proteomics: towards an integrative view of proteome dynamics. Nat Rev Genet. 2013;14:35–48.
Wiśniewski JR, Hein M, Cox J, Mann M. A “Proteomic Ruler” for protein copy number and concentration estimation without spike-in standards. Mol Cell Proteomics. 2014;13:3497–506.
Reddy PJ, Jain R, Paik YK, Downey R, et al. Personalized medicine in the age of pharmacoproteomics: a close up on India and need for social science engagement for responsible innovation in post-proteomic biology. Curr Pharmacogenomics Person Med. 2011;9:67–75.
Matthews H, Hanison J, Nirmalan N. “Omics”-informed drug and biomarker discovery: opportunities, challenges and future perspectives. Proteomes. 2016;4:E28.
Goldstein RL, Yang SN, Taldone T, Chang B, et al. Pharmacoproteomics identifies combinatorial therapy targets for diffuse large B cell lymphoma. J Clin Invest. 2015;125:4559–71.
Shu S, Lin CY, He HH, Witwicki RM, et al. Response and resistance to BET bromodomain inhibitors in triple-negative breast cancer. Nature. 2016;529:413–7.
Detke S, Katakura K, Chang KP. DNA amplification in arsenite resistant Leishmania. Exp Cell Res. 1989;180:161–70.
Ouellette M, Hettema E, Wust D, Fase-Fowler F, et al. Direct and inverted DNA repeats associated with P-glycoprotein gene amplification in drug resistant Leishmania. EMBO J. 1991;10:1009–16.
Callahan HL, Beverley SM. Heavy metal resistance: A new role for P-glycoproteins in Leishmania. J Biol Chem. 1991;266:18427–30.
Bello AR, Nare B, Freedman D, Hardy L, et al. PTR1: a reductase mediating salvage of oxidized pteridines and methotrexate resistance in the protozoan parasite Leishmania major. Proc Natl Acad Sci USA. 1994;91:11442–6.
Prasad V, Kaur J, Dey CS. Arsenite-resistant Leishmania donovani promastigotes express an enhanced membrane P-type adenosine triphosphatase activity that is sensitive to verapamil treatment. Parasitol Res. 2000;86:661–4.
Richard D, Kündig C, Ouellette M. A new type of high affinity folic acid transporter in the protozoan parasite Leishmania and deletion of its gene in methotrexate-resistant cells. J Biol Chem. 2002;277:29460–7.
HaimeurA GC, Pilote S, Mukhopadhyay R, Rosen BP, et al. Elevated levels of polyamines and trypanothione resulting from overexpression of the ornithine decarboxylase gene in arsenite-resistant Leishmania. Mol Microbiol. 1999;34:726–35.
Brochu C, Wang J, Roy G, Messier N, et al. Antimony uptake systems in the protozoan parasite Leishmania and accumulation differences in antimony-resistant parasites. Antimicrob Agents Chemother. 2003;47:3073–9.
Ouellette M, Drummelsmith J, Papadopoulou B. Leishmaniasis: drugs in the clinic, resistance and new developments. Drug Resist Updat. 2004;7:257–66.
Ashutosh SS, Goyal N. Molecular mechanisms of antimony resistance in Leishmania. J Med Microbiol. 2007;56:143–53.
Ouellette M, Borst P. Drug resistance and P-glycoprotein gene amplification in the protozoan parasite Leishmania. Res Microbiol. 1991;142:737–46.
Beverley SM. Gene amplification in Leishmania. Annu Rev Microbiol. 1991;45:417–44.
Dey S, Papadopoulou B, Haimeur A, Roy G, et al. High level arsenite resistance in Leishmania tarentolae is mediated by an active extrusion system. Mol Biochem Parasitol. 1994;67:49–57.
Dey S, Ouellette M, Lightbody J, Papadopoulou B, Rosen BP. An ATP-dependent As(III)-glutathione transport system in membrane vesicles of Leishmania tarentolae. Proc Natl Acad Sci USA. 1996;93:2192–7.
Mukhopadhyay R, Dey S, Xu N, Gage D, et al. Trypanothione overproduction and resistance to antimonials and arsenicals in Leishmania. Proc Natl Acad Sci USA. 1996;93:10383–7.
Coderre JA, Beverley SM, Schimke RT, Santi DV. Overproduction of a bifunctional thymidylate synthetase-dihydrofolate reductase and DNA amplification in methotrexate-resistant Leishmania tropica. Proc Natl Acad Sci USA. 1983;80:2132–6.
Croft SL, Coombs GH. Leishmaniasis—current chemotherapy and recent advances in the search for novel drugs. Trends Parasitol. 2003;19:502–8.
Thakur CP, Sinha GP, Pandey AK, Kumar N, et al. Do the diminishing efficacy and increasing toxicity of sodium stibogluconate in the treatment of visceral leishmaniasis in Bihar, India, justify its continued use as a first-line drug? An observational study of 80 cases. Ann Trop Med Parasitol. 1998;92:561–9.
Sundar S, More DK, Singh MK, Singh VP, et al. Failure of pentavalent antimony in visceral leishmaniasis in India: report from the center of the Indian epidemic. Clin Infect Dis. 2000;31:1104–1107s.
Perry MR, Wyllie S, Prajapati VK, Feldmann J, et al. Visceral leishmaniasis and arsenic: an ancient poison contributing to antimonial treatment failure in the Indian subcontinent? PLoS Negl Trop Dis. 2011;5:e1227.
Berman JD, Chulay JD, Hendricks LD, Oster CN. Susceptibility of clinically sensitive and resistant Leishmania to pentavalent antimony in vitro. Am J Trop Med Hyg. 1982;31:459–65.
Navin TR, Arana BA, Arana FE, Berman JD, et al. Placebo-controlled clinical trial of sodium stibogluconate (Pentostam) versus ketoconazole for treating cutaneous leishmaniasis in Guatemala. J Infect Dis. 1992;165:528–34.
Burguera J, Burguera M, Petit de Pena Y, Lugo A, et al. Selective determination of antimony(III) and antimony(V) in serum and urine and of total antimony in skin biopsies of patients with cutaneous leishmaniasis treated with meglumine antimoniate. Trace Elem Med. 1993;10:66–70.
Callahan HL, Portal AC, Devereaux R, Grogl M. An axenic amastigote system for drug screening. Antimicrob Agents Chemother. 1997;41:818–22.
Ephros M, Bitnun A, Shaked P, Waldman E, Zilberstein D. Stage-specific activity of pentavalent antimony against Leishmania donovani axenic amastigotes. Antimicrob Agents Chemother. 1999;43:278–82.
Shaked-Mishan P, Ulrich N, Ephros M, Zilberstein D. Novel intracellular SbV reducing activity correlates with antimony susceptibility in Leishmania donovani. J Biol Chem. 2001;276:3971–6.
Denton H, McGregor JC, Coombs GH. Reduction of anti-leishmanial pentavalent antimonial drugs by a parasite-specific thiol-dependent reductase, TDR1. Biochem J. 2004;381:405–12.
Zhou Y, Messier N, Ouellette M, Rosen BP, et al. Leishmania major LmACR2 is a pentavalent antimony reductase that confers sensitivity to the drug pentostam. J Biol Chem. 2004;279:37445–51.
Mukhopadhyay R, Bisacchi D, Zhou Y, Armirotti A, et al. Structural characterization of the As/Sb reductase LmACR2 from Leishmania major. J Mol Biol. 2009;386:1229–39.
Frézard F, Demicheli C, Ferreira CS, Costa MA. Glutathione-induced conversion of pentavalent antimony to trivalent antimony in meglumine antimoniate. Antimicrob Agents Chemother. 2001;45:913–6.
Tsukaguchi H, Shayakul C, Berger UV, Mackenzie B, et al. Molecular characterization of a broad selectivity neutral solute channel. J Biol Chem. 1998;273:24737–43.
Gourbal B, Sonuc N, Bhattacharjee H, Legare D, et al. Drug uptake and modulation of drug resistance in Leishmania by an aquaglyceroporin. J Biol Chem. 2004;279:31010–7.
Decuypere S, Rijal S, Yardley V, De Doncker S, et al. Gene expression analysis of the mechanism of natural Sb(V) resistance in Leishmania donovani isolates from Nepal. Antimicrob Agents Chemother. 2005;49:4616–21.
Marquis N, Gourbal B, Rosen BP, Mukhopadhyay R. Modulation in aquaglyceroporin AQP1 gene transcript levels in drug-resistant Leishmania. Mol Microbiol. 2005;57:1690–9.
Wyllie S, Cunningham ML, Fairlamb AH. Dual action of antimonial drugs on thiol redox metabolism in the human pathogen Leishmania donovani. J Biol Chem. 2004;279:39925–32.
Berman JD, Waddell D, Hanson BD. Biochemical mechanisms of the antileishmanial activity of sodium stibogluconate. Antimicrob Agents Chemother. 1985;27:916–20.
Sereno D, Holzmuller P, Mangot I, Cuny G. Antimonial-mediated DNA fragmentation in Leishmania infantum amastigotes. Antimicrob Agents Chemother. 2001;45:2064–9.
Sudhandiran G, Shaha C. Antimonial-induced increase in intracellular Ca2+ through non-selective cation channels in the host and the parasite is responsible for apoptosis of intracellular Leishmania donovani amastigotes. J Biol Chem. 2003;278:25120–32.
Grondin K, Haimeur A, Mukhopadhyay R, Rosen BP, et al. Co-amplification of the gamma-glutamylcysteine synthetase gene gsh1 and of the ABC transporter gene pgpA in arsenite-resistant Leishmania tarentolae. EMBO J. 1997;16:3057–65.
Haimeur A, Brochu C, Genest P, Papadopoulou B, et al. Amplification of the ABC transporter gene PGPA and increased trypanothione levels in potassium antimonyl tartrate (SbIII) resistant Leishmania tarentolae. Mol Biochem Parasitol. 2000;108:131–5.
Callahan HL, Roberts WL, Rainey PM, Beverley SM. The PGPA gene of Leishmania major mediates antimony (SbIII) resistance by decreasing influx and not by increasing efflux. Mol Biochem Parasitol. 1994;68:145–9.
Légaré D, Richard D, Mukhopadhyay R, Stierhof YD, et al. The Leishmania ATP-binding cassette protein PGPA is an intracellular metal-thiol transporter ATPase. J Biol Chem. 2001;276:26301–7.
Mittal MK, Rai S, Ravinder GS, Sundar S, et al. Characterization of natural antimony resistance in Leishmania donovani isolates. Am J Trop Med Hyg. 2007;76:681–8.
Goyeneche-Patino DA, Valderrama L, Walker J, Saravia NG. Antimony resistance and trypanothione in experimentally selected and clinical strains of Leishmania panamensis. Antimicrob Agents Chemother. 2008;52:4503–6.
Mukherjee A, Padmanabhan PK, Singh S, Roy G, et al. Role of ABC transporter MRPA, gamma-glutamylcysteine synthetase and ornithine decarboxylase in natural antimony-resistant isolates of Leishmania donovani. J Antimicrob Chemother. 2007;59:204–11.
Mandal G, Sarkar A, Saha P, Singh N, et al. Functionality of drug efflux pumps in antimonial resistant Leishmania donovani field isolates. Indian J Biochem Biophys. 2009;46:86–92.
Monte-Neto R, Laffitte MC, Leprohon P, Reis P, et al. Intrachromosomal amplification, locus deletion and point mutation in the aquaglyceroporin AQP1 gene in antimony resistant Leishmania (Viannia) guyanensis. PLoS Negl Trop Dis. 2015;9:e0003476.
Hefnawy A, Berg M, Dujardin JC, De Muylder G. Exploiting knowledge on Leishmania drug resistance to support the quest for new drugs. Trends Parasitol. 2017;33:162–74.
Jardim A, Hanson S, Ullman B, McCubbin WD, et al. Cloning and structure-function analysis of the Leishmania donovani kinetoplastid membrane protein-11. Biochem J. 1995;305:315–20.
Fuertes MA, Berberich C, Lozano RM, Gimenez-Gallego G, et al. Folding stability of the kinetoplastid membrane protein-11 (KMP-11) from Leishmania infantum. Eur J Biochem. 1999;260:559–67.
Lee N, Bertholet S, Debrabant A, Muller J, et al. Programmed cell death in the unicellular protozoan parasite Leishmania. Cell Death Differ. 2002;9:53–64.
Cohen-Saidon C, Carmi I, Keren A, Razin E. Antiapoptotic function of Bcl-2 in mast cells is dependent on its association with heat shock protein 90. Blood. 2006;107:1413–20.
Das S, Shah P, Tandon R, Yadav NK, et al. Over-expression of cysteine leucine rich protein is related to SAG resistance in clinical isolates of Leishmania donovani. PLoS Negl Trop Dis. 2015;9:e0003992.
Das S, Shah P, Baharia RK, Tandon R, et al. Over-expression of 60s ribosomal L23a is associated with cellular proliferation in SAG resistant clinical isolates of Leishmania donovani. PLoS Negl Trop Dis. 2013;7:e2527.
Dridi L, Ahmed Ouameur A, Ouellette M. High affinity S-Adenosylmethionine plasma membrane transporter of Leishmania is a member of the folate biopterin transporter (FBT) family. J Biol Chem. 2010;285:19767–75.
Vickers TJ, Beverley SM. Folate metabolic pathways in Leishmania. Essays Biochem. 2011;51:63–80.
Wiśniewski JR, Zougman A, Mann M. Combination of FASP and StageTip-based fractionation allows in-depth analysis of the hippocampal membrane proteome. J Proteome Res. 2009a;8:5674–8.
Wiśniewski JR, Duś-Szachniewicz K, Ostasiewicz P, Ziółkowski P, et al. Absolute proteome analysis of colorectal mucosa, adenoma, and cancer reveals drastic changes in fatty acid metabolism and plasma membrane transporters. J Proteome Res. 2015;14:4005–18.
Vildhede A, Wiśniewski JR, Norén A, Karlgren M, et al. Comparative proteomic analysis of human liver tissue and isolated hepatocytes with a focus on proteins determining drug exposure. J Proteome Res. 2015;14:3305–14.
Tandon R, Chandra S, Baharia RK, Das S, et al. Characterization of the proliferating cell nuclear antigen of Leishmania donovani clinical isolates and its association with antimony resistance. Antimicrob Agents Chemother. 2014;58:2997–3007.
Parodi-Talice A, Durán R, Arrambide N, Prieto V, et al. Proteome analysis of the causative agent of Chagas disease: Trypanosoma cruzi. Int J Parasitol. 2004;34:881–6.
Croft SL, Neal RA, Pendergast W, Chan JH. The activity of alkyl phosphorylcholines and related derivatives against Leishmania donovani. Biochem Pharmacol. 1987;36:2633–6.
Kuhlencord A, Maniera T, Eibl H, Unger C. Hexadecylphosphocholine: oral treatment of visceral leishmaniasis in mice. Antimicrob Agents Chemother. 1992;36:1630–4.
Sundar S, Jha TK, Thakur CP, Engel J, et al. Oral miltefosine for Indian visceral leishmaniasis. N Engl J Med. 2002;347:1739–46.
Soto J, Soto P. Miltefosine: oral treatment of leishmaniasis. Expert Rev Anti Infect Ther. 2006;4:177–85.
Sundar S, Mondal D, Rijal S, Bhattacharya S, et al. Implementation research to support the initiative on the elimination of kala azar from Bangladesh, India and Nepal–the challenges for diagnosis and treatment. Trop Med Int Health. 2008;13:2–5.
World Health Organization. Regional strategic framework for elimination of Kala-azar from the South-East Asia region (2005–2015). New Delhi: WHO Regional Office for South-East Asia; 2005.
Murray HW, Berman JD, Davies CR, Saravia NG. Advances in leishmaniasis. Lancet. 2005;366:1561–77.
Calvopina M, Gomez EA, Sindermann H, Cooper PJ, et al. Relapse of new world diffuse cutaneous leishmaniasis caused by Leishmania (Leishmania) mexicana after miltefosine treatment. Am J Trop Med Hyg. 2006;75:1074–7.
Zerpa O, Ulrich M, Blanco B, Polegre M, et al. Diffuse cutaneous leishmaniasis responds to miltefosine but then relapses. Br J Dermatol. 2007;156:1328–35.
Pandey BD, Pandey K, Kaneko O, Yanagi T, et al. Relapse of visceral leishmaniasis after miltefosine treatment in a Nepalese patient. Am J Trop Med Hyg. 2009;80:580–2.
Andrade HM, Toledo VP, Pinheiro MB, Guimarães TM, et al. Evaluation of miltefosine for the treatment of dogs naturally infected with L. infantum (= L. chagasi) in Brazil. Vet Parasitol. 2011;181:83–90.
Proverbio D, Spada E, Bagnagatti De Giorgi G, Perego R. Failure of miltefosine treatment in two dogs with natural Leishmania infantum infection. Case Rep Vet Med. 2014;640151. https://doi.org/10.1155/2014/640151
Escobar P, Matu S, Marques C, Croft SL. Sensitivities of Leishmania species to hexadecylphosphocholine (miltefosine), ET-18-OCH(3) (edelfosine) and amphotericin B. Acta Trop. 2002;81:151–7.
van Blitterswijk WJ, Verheij M. Anticancer alkylphospholipids: mechanisms of action, cellular sensitivity and resistance, and clinical prospects. Curr Pharm Des. 2008;14:2061–74.
Paris C, Loiseau PM, Bories C, Bréard J. Miltefosine induces apoptosis-like death in Leishmania donovani promastigotes. Antimicrob Agents Chemother. 2004;48:852–9.
Croft SL, Seifert K, Duchêne M. Antiprotozoal activities of phospholipid analogues. Mol Biochem Parasitol. 2003;126:165–72.
Rakotomanga M, Blanc S, Gaudin K, Chaminade P, et al. Miltefosine affects lipid metabolism in Leishmania donovani promastigotes. Antimicrob Agents Chemother. 2007;51:1425–30.
Pérez-Victoria FJ, Sánchez-Cañete MP, Castanys S, Gamarro F. Phospholipid translocation and miltefosine potency require both L. donovani miltefosine transporter and the new protein LdRos3 in Leishmania parasites. J Biol Chem. 2006a;281:23766–75.
Sánchez-Cañete MP, Carvalho L, Pérez-Victoria FJ, Gamarro F, et al. Low plasma membrane expression of the miltefosine transport complex renders Leishmania braziliensis refractory to the drug. Antimicrob Agents Chemother. 2009;53:1305–13.
Pérez-Victoria FJ, Sánchez-Cañete MP, Seifert K, Croft SL, et al. Mechanisms of experimental resistance of Leishmania to miltefosine: Implications for clinical use. Drug Resist Updat. 2006b;9:26–39.
Montero-Lomelí M, Morais BL, Figueiredo DL, Neto DC, et al. The initiation factor eIF4A is involved in the response to lithium stress in Saccharomyces cerevisiae. J Biol Chem. 2002;277:21542–8.
Wiśniewski JR, Zougman A, Nagaraj N, Mann M. Universal sample preparation method for proteome analysis. Nat Methods. 2009b;6:359–62.
Priotto G, Kasparian S, Mutombo W, Ngouama D, et al. Nifurtimox-eflornithine combination therapy for second-stage African Trypanosoma brucei gambiense trypanosomiasis: a multicentre, randomised, phase III, non-inferiority trial. Lancet. 2009;374:56–64.
Gygi SP, Corthals GL, Zhang Y, Rochon Y, et al. Evaluation of two-dimensional gel electrophoresis-based proteome analysis technology. Proc Natl Acad Sci USA. 2000;97:9390–5.
Junqueira M, Spirin V, Santana Balbuena T, Waridel P, et al. Separating the wheat from the chaff: unbiased filtering of background tandem mass spectra improves protein identification. J Proteome Res. 2008;7:3382–95.
Lye LF, Owens K, Shi H, Murta SM, et al. Retention and loss of RNA interference pathways in trypanosomatid protozoans. PLoS Pathog. 2010;6:e1001161.
Carter KC, Hutchison S, Henriquez FL, Légaré D, et al. Resistance of Leishmania donovani to sodium stibogluconate is related to the expression of host and parasite gamma-glutamylcysteine synthetase. Antimicrob Agents Chemother. 2006;50:88–95.
Araujo RP, Liotta LA, Petricoin EF. Proteins, drug targets and the mechanisms they control: the simple truth about complex networks. Nat Rev Drug Discov. 2007;6:871–80.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Saboia-Vahia, L., de Jesus, J.B., Cuervo, P. (2018). The Role of Proteomics in the Study of Drug Resistance. In: Ponte-Sucre, A., Padrón-Nieves, M. (eds) Drug Resistance in Leishmania Parasites. Springer, Cham. https://doi.org/10.1007/978-3-319-74186-4_10
Download citation
DOI: https://doi.org/10.1007/978-3-319-74186-4_10
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-74185-7
Online ISBN: 978-3-319-74186-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)