Abstract
Liver cancer is the sixth most common cancer and the second leading cause of death worldwide. Only 30–40% of patients are candidates for curative intervention at the time of diagnosis, and up to 70% of those who undergo curative resection will recur. Cytotoxic chemotherapy in advanced disease is not effective and is often limited by concomitant hepatic dysfunction. Sorafenib, a multiple kinase inhibitor, is the only therapy to have shown an overall survival benefit that is only modest at best. Thus, there is a large unmet need to develop additional therapies. In recent years, a diverse array of phenotypic and genetic alterations have been identified in HCC patients. Following these advances, several phase III studies with therapies targeted toward these alterations have been conducted; however, none has shown a survival benefit. It remains to be seen if this new understanding in these alterations can be translated therapeutically. In this chapter, we will discuss these alterations, as well as the developing therapies targeting them.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
13.1 Introduction
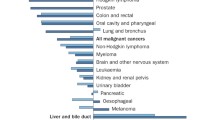
Liver cancer is the sixth most common cancer and the second leading cause of cancer death worldwide, accounting for 6% of all diagnosed cancers and approximately 745,000 deaths [1]. Hepatocellular carcinoma (HCC) accounts for up to 90% of all liver cancer cases [1]. More striking, however, is that the incidence has risen over the past several decades in numerous countries, including the United States [2, 3]. Only 30–40% of patients have early HCC at the time of diagnosis and are eligible for potentially curative therapies such as surgical resection, liver transplantation, radiofrequency ablation (RFA), or transarterial chemoembolization (TACE). Furthermore, recurrence remains the leading cause of death after curative resection, occurring in greater than 50% of patients [4]. Cytotoxic chemotherapy has had only modest benefit in advanced disease, and effectiveness is frequently limited by underlying hepatic dysfunction.
To date, sorafenib, a multiple kinase inhibitor is the only therapy to have shown an overall survival benefit in advanced disease, with an improvement from 7.9 to 10.7 months with a favorable toxicity profile. This finding has established sorafenib as the standard of care in this setting [5]. With only a modest benefit offered by sorafenib, there is a pressing need to develop additional therapies to improve outcomes in this disease.
In recent years, HCC has been shown to have a diverse array of phenotypic and genetic alterations, although a few common molecular alterations have been identified that provide an opportunity to develop targeted therapies. These targets include receptors for vascular endothelial growth factor (VEGF), epidermal growth factor (EGF), fibroblast growth factor (FGF), and platelet-derived growth factor (PDGF), as well as mammalian target of rapamycin (mTOR) and histone deacetylases (HDACs). Several phase III studies of therapies targeted toward these alterations have followed; however, none has shown a significant survival benefit. This chapter will review our current understanding of the molecular targeted pathways at play in HCC, as well as ongoing clinical trials of targeted agents, and the future direction for therapy in the treatment of HCC.
13.2 Systemic Chemotherapy for the Treatment of HCC
Despite many effective cytotoxic chemotherapy regimens in other tumor types, there remains no effective chemotherapeutic strategy for the treatment of HCC. HCC has long been considered a chemotherapy-refractory tumor through multiple mechanisms: enhanced cellular efflux mechanisms associated with an increase in drug transporter proteins such as MDR1 and P-gp [6], increased expression of TP53 mutations [7] and heat shock proteins (HSPs) [8], DNA damage repair, epithelial-mesenchymal transition (EMT), hypoxia-inducible factor 1 alpha (HIF-1α), and others [9]. Historically, response rates for any chemotherapeutic agent have been low, ranging from approximately 10 to 20% [10]. Because the majority of HCC occurs in the setting of cirrhosis, it is often difficult to determine the survival benefit of these therapies because the ability of patients to tolerate these treatments is often limited by hepatic dysfunction. Several studies have shown that systemic chemotherapy has low efficacy in patients with significant cirrhosis, particularly in those with a bilirubin >2, poor performance status, ascites, or portal vein thrombus [11]. Nonetheless, a large number of studies have been performed using both single agents and combination regimens, resulting in a wide range of responses. Additionally, many of these studies were performed in distinct patient populations (Asian, European), which likely results in important differences between study populations such as hepatitis B or C etiology, or age, thereby making the results less applicable to a more uniform population.
13.2.1 Monotherapy
The most studied single agent has been the anthracycline doxorubicin. The earliest phase II trial was done in 1975 and showed an objective response rate of 79% [12]. However, subsequent studies using the same dose of 75 mg/m2 failed to corroborate these results and suggested that the true response rate is actually 20% or less [13,127,14,83,71,10,52,122,22,136,62,96,39,38,1,126,111,120,19,53,42,112,129,23,54,82,102,6,132,139,15,106,43,84,57,133,80,50,24,92,60,78,18,51,93,37,124,25,58,61,105,85,90,5,137,65,44,91,33,34,63,56,135,64,75,11,72,16,121,70,2,12,55,32,30,114,117,26,27,36,128,125,123,109,119,48,113,86,46,20,130,4,100,103,28,115,107,3,49,76,67,45,8,9,77,79,81,118,134,17]. Despite this discrepancy, one study has demonstrated a survival benefit with doxorubicin as compared to the best supportive care alone [18]. Lower doses have even lower reported response rates [19, 20].
Many other agents have been evaluated as monotherapies in phase III trials including mitoxantrone, epirubicin, pegylated liposomal doxorubicin, gemcitabine, irinotecan, and thalidomide, all of which have similar or even lower response rates as compared to doxorubicin [21,29,104,98,89,138,108,69,110,7,74,88,97,47,13,127,14,83,71,10,52,122,22,136,62,96,39,38,1,126,111,120,19,53,42,112,129,23,54,82,102,6,132,139,15,106,43,84,57,133,80,50,24,92,60,78,18,51,93,37,124,25,58,61,105,85,90,5,137,65,44,91,33,34,63,56,135,64,75,11,72,16,121,70,2,12,55,32,30,114,117,26]. 5-FU and its oral equivalent, capecitabine, have low toxicity and can be administered more easily in the setting of hepatic dysfunction. Studies evaluating the efficacy of 5-FU monotherapy, with or without leucovorin, show response rates no higher than 28% [27, 28]. Capecitabine has been evaluated in very small trials with mixed populations of both previously treated and untreated patients, with median overall survival rates of about 10 months [29, 30]. Most patients had stable disease with a low number of partial or complete responses. However, a recent phase II trial showed superior median overall survival and progression-free survival in patients treated with sorafenib versus capecitabine, thereby making the role of capecitabine in the treatment of HCC unclear [31].
13.2.2 Combination Chemotherapy
Several different combination chemotherapy regimens using cisplatin or gemcitabine backbones have been tested in patients with advanced HCC. Gemcitabine has been used in combination with several different agents including cisplatin, pegylated liposomal doxorubicin, and oxaliplatin (GEMOX). In phase II trials, the reported overall responses rates were 20% [32], 24% [33], and 18% [34], respectively. However, median overall survival remained dismal, anywhere from 11.5 to 22.5 months, with the addition of significant toxicities including thrombocytopenia, anemia, neutropenia, and neuropathy. Additionally, numerous cisplatin, oxaliplatin, and irinotecan-based regimens have been studied, including XELOX, FOLFOX (infusional fluorouracil, leucovorin, and oxaliplatin), and FOLFOX4, all of which have not had promising results [35, 36]. The PIAF regimen (cisplatin, interferon, doxorubicin, and 5-FU) initially appeared to have some efficacy in patients with unresectable HCC after a phase II trial found a median overall survival of 8.9 months [37]. However, in a randomized phase III trial comparing PIAF to doxorubicin monotherapy, no significant survival benefit was found [17].
Overall, an abundance of cytotoxic chemotherapy regimens have been tested without convincing evidence of a survival benefit. The evaluation of these regimens has been limited by the use of small, single-arm trials with heterogenous patient populations, lack of appropriate controls, and lack of patient risk stratification. As such, there is insufficient data for the routine use of any chemotherapy regimen in HCC. Subsequently, the emergence of targeted agents such as sorafenib has since become the focus of treatment for patients with advanced HCC.
13.3 Molecular Pathogenesis of HCC
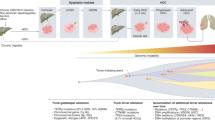
In order to develop effective targeted molecular agents, it is critical to understand the molecular pathogenesis of HCC. The most common etiologies of HCC include hepatitis B (HBV), hepatitis C (HCV), chronic alcohol consumption, and aflatoxin toxicity. Nonalcoholic fatty liver disorders (NALFD) have also been shown to contribute to the development of HCC [38]. Importantly, the underlying disease process dictates the specific molecular changes that promote carcinogenesis in HCC and is responsible for the great genomic heterogeneity associated with HCC tumors. For example, alcohol induces significant inflammation with cycles of necrosis and proliferation, whereas aflatoxin contributes to hepatocarcinogenesis specifically via p53 mutations (Fig. 13.1) [39].
However, in general, hepatocarcinogenesis is a multistep process which evolves in the setting of chronic liver disease. It often develops over a prolonged time period of up to 30 years, preceded by the chronic inflammation and pre-dysplastic processes resulting from cirrhosis and chronic hepatitis. Injury induced by these processes leads to a continuous cycle of hepatocyte necrosis and regeneration, which involves proliferation of the stem cell compartment of the liver leading to DNA mutations and genomic instability [39]. In the setting of liver damage, hepatic mesenchymal cells called stellate cells are activated and participate in extracellular matrix production and chemotaxis. Chronic liver damage leads to recurrent activation of stellate cells, resulting in alteration of the extracellular matrix and fibrosis [40]. Additionally, throughout these processes, various growth factors are secreted, which can each contribute to oncogenesis on their own through processes such as angiogenesis.
Overall, the molecular pathogenesis and specific genomic alterations that lead to the development of HCC are extremely complex and are not fully understood. However, the key mechanism appears to be formation of genomic instability in the setting cirrhosis. Specifically, telomere shortening and telomerase reactivation are key features of hepatocarcinogenesis along with loss or mutation of the p53 tumor suppressor gene [39]. Several studies have shown that there is a broad mutational profile in HCC, with approximately 30–40 mutations per tumor, among which 5–8 function as driver mutations while the rest are passenger mutations that do not contribute significantly to tumorigenesis [41,59,66,95,99,35,21,29,104,98,89,138,108,69,110,7,74,88,97,47,13,127,14,83,71,10,52,122,22,136,62,96,39,38,1,126,111,120,19,53,42,112,129,23,54,82,102,6,132,139,15,106,43,84,57,133,80,50,24,92,60,78,18,51,93,37,124,25,58,61,105,85,90,5,137,65,44,91,33,34,63,56,135,64,75,11,72,16,121,70,2,12,55,32,30,114,117,26,27,36,128,125,123,109,119,48,113,86,46,20,130,4,100,103,28,115,107,3,49,76,67,45]. Nonetheless, despite the vast heterogeneity of HCC tumors, there are several common molecular themes and pathways which are known to play prominent roles in the pathogenesis of HCC.
13.3.1 Genetic Mutations and Drivers
Comprehensive genomic analyses are essential to identify mutational signatures in heterogeneous HCC tumors which can help associate them with specific risk factors and improve personalized treatment with molecular targeted agents. Several studies have helped elucidate the most common genetic profiles and driver genes of HCC through exome sequencing analyses. Schulze et al. analyzed whole coding sequences of 243 liver tumors in three European countries [46]. Approximately, 41% were associated with alcohol, 26% with HCV, 18% with nonalcoholic steatohepatitis (NASH), and 14% with HBV. Approximately 49% of tumors were from cirrhotic livers. The authors found a median of 21 silent and 64 non-silent mutations per tumor with 8 signature patterns and 161 driver genes (Fig. 13.2). The most common gene alterations were TERT (60%), CTNNB1 (37%), TP53 (24%), and ARID1A (13%). They performed copy number analysis and were able to correlate focal copy number alterations (CNAs) and mutations to identify the 11 most commonly associated molecular pathways affecting: telomerase expression (60%), cellular inflammation and proliferation via WNT-β-catenin (54%), and PI3-AKT-mTOR (51%). The three most common clusters of alterations centered on CTNNB1, AXIN1, and TP53. Finally, the authors were able to correlate genetic profiles with specific risk factors.
Driver genes, copy number alterations, and most frequent gene alterations in HCC (reproduced from Schulze et al. [46] with the following caption). (a) The 161 putative driver genes identified by integrating mutations and focal CNAs are presented, with log-transformed mutation significance on the x axis and the net frequency of gains and deletions on the y axis. The size and color of each circle represent the alteration frequency and MutSig q value, respectively. Significantly mutated genes (q < 0.05) are labeled. (b) Frequency of CNAs along the genome. The top axis indicates the frequency of low-amplitude changes (gains and losses); the bottom axis indicates the frequency of high-amplitude changes (focal amplifications and homozygous deletions). Genes targeted by recurrent amplifications and homozygous deletions are labeled. (c) Bar plot indicating the number and type of events for the most frequently altered genes (≥4% of samples)
For example, alcohol-related HCCs were enriched in CTNNB1 and TERT alterations, whereas HCV infection was associated with more TP53 mutations. Overall 28% of patients harbored at least one molecular alteration that is targetable by an FDA-approved drug.
Other studies have reported similar findings. Gouichard et al. performed copy number analysis on 125 HCC tumors with whole exome sequencing on 24 tumors primarily associated with alcohol intake [42]. They found that the most common alterations were related to β-catenin (CTNNB1 (32.8%), AXIN1 (15.2%), APC (1.6%)), cell cycle control (TP53 (20.8%), CDKN2A (7.2%), IRF2 (4.8%)), chromatin remodeling (ARID1A (16.8%), ARID2 (5.6%)), P13K/Ras signaling (RPS6KA3 (9.6%)), and oxidative stress (NFE2L2 (6.4%)). Inactivation of the tumor suppressor IRF2 was exclusively found in HBV-related tumors and led to impaired TP53 function. Mutations in chromatin-remodeling genes were more frequently associated with alcohol-related tumors.
Overall, the most common oncogene amplifications include TERT, CCNB1, MET, MYC, FGF19, and VEGFA, whereas the most frequent homozygous deletions are CDKN2A, TP53, Rb1, and AXIN1 [5, 41, 45–49]. Additionally, HDAC2, a histone deacetylase (HDAC) enzyme that participates in chromatin remodeling, has been found to be upregulated in patients with HCC and is associated with poor survival [50, 51]. The functional classification of these genes has led to the identification of several key signaling pathways involved in the pathogenesis of HCC and serve as potential therapeutic targets. A selection of these will be discussed below.
13.3.2 Signaling Pathways
13.3.2.1 p53
The p53 tumor suppressor is an important driver in HCC, with a mutation rate of 18–50%, depending on the underlying etiology [52]. For example, aflatoxin B1-associated HCC is more common in Southeast Asia and Sub-Saharan Africa and causes a missense mutation at codon 249 (R249S) on exon 7 in 90% of cases [53, 54]. The mutated protein promotes hepatocarcinogenesis through inhibition of apoptosis and cellular proliferation. Mutations at codon 249 are suggested by some to be driver mutations, since they are also found in normal liver tissue after aflatoxin exposure [55]. However, at the same time, other studies have some that these mutations were related to tumor stage and may therefore reflect late molecular changes [56]. TP53 mutations are also prevalent in HBV and HCV HCC and may serve as a biomarker for HCC as well as chemoresistance [7, 56, 57]. A recent meta-analysis has shown that HCC patients with upregulated mutant p53 expression have a shorter overall survival than those with wild type p53 [58]. Other mutations that commonly alter p53 function include G:C to T:A transversions at codon 249 and C:G to A:T and C:G to T:A transversions at codon 250 [59].
13.3.2.2 WNT/β-Catenin
Dysregulation of the Wnt/β-catenin pathway is known to be crucial in hepatocarcinogenesis [60]. About 50% of patients with HCC have activation of this pathway through either mutations of CTNNB1, inactivation of cadherin-1, or overexpression of frizzled receptors [61]. Mutations in AXIN1, a negative regulator of Wnt/β-catenin, are also common. These mutations affect many cellular processes including homeostasis, mobility, angiogenesis, proliferation, and apoptosis. In addition, disruption of the adenomatous polyposis coli (APC) gene leads to activation of this pathway and promotes inflammation and early oncogenesis. This pathway is significantly involved in alcoholic and HBV- and HCV-related HCC [59]. Specifically, activation of this pathway leads to transcription of a variety of genes including cyclin D1, COX2, matrix metalloproteinase 7 (MMP7), COX2, and MYC, all of which are pro-tumorigenic. β-catenin signaling leads to activation of NF-κβ which also promotes inflammation and cell death [62, 63].
13.3.2.3 PI3K/AKT/mTOR
The phosphatidylinositol 3-kinase (PI3K/AKT/mTOR) pathway affects cellular processes such as cell proliferation and survival and is upregulated in 40–50% of HCC [64]. mTOR (mammalian target of rapamycin) is targeted by rapamycin (sirolimus), which was first discovered as an important immunosuppressant after kidney transplant. Important tyrosine kinase receptors such as vascular endothelial growth factor receptor (VEGFR), platelet-derived growth factor receptor (PDGFR), epidermal growth factor receptor (EGFR), and insulin-like growth factor receptor (IGFR) activate this pathway, while phosphatase and tensin homologue (PTEN) inhibits it. There are now numerous PI3K inhibitors in clinical trials [65]. Upregulation of PI3K/AKT/mTOR is associated with decreased overall survival, aggressive tumor behavior, and early recurrence [66,95,99,35,21,29,104,98,89,138,108,69,110,7,74,88,97,47,13,127,14,83,71,10,52,122,22,136,62,96,39,38,1,126,111,120,19,53,42,112,129,23,54,82,102,6,132,139,15,106,43,84,57,133,80,50,24,92,60,78,18,51,93,37,124,25,58,61,105,85,90,5,137,65,44,91,33,34,63,56,135,64,75,11,72,16,121,70,2,12,55,32,30,114,117,26,27,36,128,125,123,109,119,48,113,86,46,20,130,4,100,103,28,115,107,3,49,76,67,45,8,9,77,79,81,118,134,17,40,87,73,68].
13.3.2.4 RAS/MAPK
Over 50% of patients with early-stage HCC and nearly 100% of patients with advanced HCC have activation of the RAS/MAPK pathway, which is stimulated by several receptors including EGFR, fibroblast growth factor receptor (FGFR), and c-mesenchymal-epithelial transition factor-1 (c-MET) [69, 70]. The Ras protein belongs to a family of GTPases, which once activated, recruit Raf-1 kinase, which in turn phosphorylates MEK1 and MEK2 and ultimately ERK 1 and ERK2 [71]. It is known that both the Hbx and HCV core proteins can activate this pathway, which plays an important role in cellular proliferation and survival [72, 73]. Several studies have demonstrated increased expression of MEK and ERK proteins in both animal and human liver cancer [71]. Additionally, increased expression of Raf is associated with poor prognosis and is an independent marker of tumor recurrence in human HCC [74]. Although mutations in Raf and Ras proteins are highly prevalent in cancers such as pancreatic cancer, these genes are rarely mutated in human HCC [69]. Alternatively, downregulation of inhibitors of this pathway, such as DUSP1, RKIP, Spred, and Sprouty proteins, appears to play a prominent role in hepatocarcinogenesis [71].
13.3.2.5 JAK/STAT
The JAK/STAT pathway consists of a cell surface receptor, a Janus kinase (JAK), and a signal transducer and activator of transcription (STAT) protein. The pathway is activated by a variety of growth factors, hormones, and cytokines. Ligand binding activates JAK, ultimately resulting in phosphorylation of STAT, which then translocates to the cell nucleus and induces transcription of target genes. JAK/STAT signaling promotes cell proliferation, migration, and differentiation. Dysregulation of STAT is associated with HCC, and alterations in JAK/STAT signaling occur with a prevalence of 1.5% based on deep-sequencing analyses [44, 69]. Further, the suppressors of cytokine signaling proteins (SOCS) are negative regulators of this pathway and when altered lead to over-activation of the pathway and oncogenesis. Inactivation of SOCS-1 has also been demonstrated in HCC [52, 69].
13.3.2.6 Notch
Notch signaling via its ligands Jagged (Jag-1, Jag-2) and Delta-like (Dl-1, Dl-3, and Dl-4) is important in cell fate and differentiation. Studies have shown that Notch is involved in hepatocarcinogenesis through activation of Sox9- and K19-positive liver progenitor cells [75]. Genomic studies have shown activation of Notch in about 30% of human HCC, thereby implicating this pathway as a potential therapeutic target [76].
13.3.2.7 HDACs
Histone deacetylases are critical regulators of gene expression. Numerous studies have demonstrated aberrant expression of HDACs in human cancers, and they have been associated with an either better or worse prognosis, depending on the type of cancer [77]. HDAC inhibitors (HDACis) cause acetylation of histone and non-histone proteins leading to destabilization of various proteins and suppression of transcriptional activity [78]. They are potent inducers of apoptosis, autophagy, cell cycle arrest, and inhibition of tumor angiogenesis [79]. They have become a prominent part of cancer therapy. Upregulation of HDAC 1, 3, 4, 5, and 10 has been found in HCC tumors, although the prognosis of these markers in HCC is unclear [78, 80]. One study found that HDAC 3 was a useful biomarker for HBV-HCC recurrence after liver transplantation [81].
13.3.2.8 Other
There are multiple other molecular pathways and mechanisms known to play a strong role in HCC. These include the tumor suppressor retinoblastoma (Rb) pathway which is activated by cyclin-dependent kinases (CDKs) and induces G1/S cell cycle transition [82]. Alteration in expression or inactivation of various CDK inhibitors such as p16INK4A, p21(WAF1/CIP1), and p27Kip1 is associated with early hepatocarcinogenesis [59]. Additionally, the transforming growth factor beta (TGF-β) pathway is known to play a role in inflammation and fibrosis leading to the development of HCC. Studies have correlated late rather than early molecular alterations in TGF-β signature with poor prognosis and tumor recurrence which is likely due to TGF-β stimulation of epithelial-mesenchymal transition, which is essential for metastasis [83]. Finally, the hepatocyte growth factor (HGF)/c-mesenchymal-epithelial transition factor-1 (c-MET) pathway is associated with angiogenesis, invasion, and tumor growth. Increased expression of MET gene signature is associated with poor prognosis [84, 85]. Multiple other receptor tyrosine kinase receptors which activate the RAS/MAPK and PI3/AKT/mTOR pathways are very important in the pathogenesis of HCC as well and include the receptors for insulin-like growth factor (IGF), epidermal growth factor (EGF), platelet-derived growth factor (PDGF), vascular endothelial growth factor (VEGF), and fibroblast growth factor (FGF). The latter two growth factors play a significant role in angiogenesis as discussed below. Finally, other mediators of the cellular stress response including heat shock proteins and genes involved in oxidative stress that contribute to cellular mutations and damage in HCC are also potential targets for therapeutic intervention.
13.4 Molecular Targeted Therapies for the Treatment of HCC
Hepatocellular carcinoma is a hypervascular tumor, which frequently invades local vasculature. As a result, angiogenesis is thought to play a key role in the progression of HCC. This process is mediated by a variety of growth factors which activate many of the aforementioned molecular pathways, including VEGF. Higher circulating levels of VEGF are associated with a poor prognosis and decreased overall survival in patients with HCC and correlate with worse outcomes including tumor recurrence after surgery or local ablative procedures [86, 87]. Therefore, this receptor was one of the first targets of molecular therapy. In addition, PDGFR and FGFR are additional targets of angiogenesis which are currently being explored.
13.4.1 Anti-VEGF Agents
13.4.1.1 Sorafenib
Sorafenib is an oral multiple tyrosine kinase inhibitor that targets the Raf kinases, including VEGF receptors 1–3 and PDGF receptor (PDGFR) via the Raf-MEK-ERK pathway. In 2008, sorafenib became the first approved molecular targeted agent for the treatment of patients with advanced HCC based on positive data from the SHARP trial, a multicenter European phase III trial of sorafenib in 602 patients with advanced (unresectable) HCC and Child-Pugh Class A cirrhosis. Patients were randomly assigned to receive either sorafenib 400 mg twice daily or placebo, with the primary endpoints of overall survival and time to symptomatic progression, as measured by a 4-point decrease in the FACT hepatobiliary symptom index questionnaire. Secondary endpoints included time to radiographic progression based on the Response Evaluation Criteria in Solid Tumors (RECIST), disease control rate, and safety. Sorafenib resulted in a significant overall survival benefit (10.7 vs. 7.9 months) and an improvement in time to radiologic progression (5.5 vs. 2.8 months). However, objective response rates according to the RECIST criteria were low [5]. Seventy-one percent of patients had a partial response, with no complete responses. The survival benefit is likely due to delayed disease progression. Overall there was a low toxicity profile with primarily grade 1 and grade 2 adverse events. Grade 3 events included diarrhea, hand-foot reaction, hypertension, and abdominal pain [5].
Cheng et al. conducted a second phase II trial in the Asian-Pacific population using the same dose of sorafenib in patients with primarily HBV-related HCC and Child-Pugh Class A cirrhosis. They also found improved overall survival in the sorafenib group (6.5 vs. 4.2 months) as well as improved time to tumor progression (2.8 vs. 1.4 months) [88]. Again, sorafenib was well tolerated with similar grade 3 and 4 toxicities as in the SHARP trial. The difference in the survival benefit between the SHARP and Cheng studies may be due to the difference in the etiology of HCC, as the SHARP trial included patients with a more uniform distribution of HBV-, HCV-, and alcohol-related cirrhosis. In fact, a subgroup analysis in the SHARP trial showed that the median overall benefit was greatest in patients with hepatitis C-related cirrhosis [89]. The results of both of these studies were extremely significant and exciting at the time, as there had been no consistent survival benefits of any anti-HCC drugs in the previous decades. Therefore, sorafenib became the standard of care and benchmark to demonstrate superior or non-inferiority in future trials of molecular targeted agents for HCC.
Sorafenib has also been tested in combination with transarterial chemoembolization (TACE), as well as in combination with chemotherapy. TACE is the only transarterial treatment that has been shown to have a survival benefit as compared to placebo in randomized studies [90, 91]. Llovet et al. showed an increased overall survival of 63% vs. 27% at 2 years in patients with HCC and Child-Pugh Class A or B treated with repeated chemoembolization as compared to controls [90]. Several studies, including phase III trials, have evaluated the efficacy of sorafenib in combination with TACE. An initial phase III showed no difference in overall survival in 458 patients with unresectable HCC assigned to placebo or sorafenib (400 mg twice daily) after TACE [92]. However, the median study dose of sorafenib was only 386 mg daily due to dose reductions, much lower than the current standard of 400 mg twice daily. A subsequent phase II trial (SPACE) randomly assigned 307 to sorafenib or placebo with repeated doses of TACE with doxorubicin-eluting beads [93]. It found better trends toward TTP in the sorafenib group but no statistical differences in TTP or overall survival. Finally, there is no known benefit of using sorafenib in combination with systemic chemotherapeutic agents such as doxorubicin [94].
Currently, sorafenib remains first-line therapy for patients with unresectable HCC. However, further studies are needed to further characterize predictive biomarkers of response to sorafenib. The SHARP trial has served as a template for the design of trials investigating other targeted therapies, and several important design features have been replicated in subsequent studies. First, the majority of patients being enrolled have Child-Pugh Class A cirrhosis, thereby eliminating the risk of patients dying as a result of liver decompensation. Also, patients with advanced HCC who do not qualify for curative therapies such as resection or transplant, or those who progress after conventional therapies such as TACE, are good candidates for clinical trials. Lastly, overall survival and time to progression are more frequently serving as primary endpoints, as progression-free survival may be confounded by outcomes related to the severity of liver dysfunction.
13.4.1.2 Sunitinib
Sunitinib is another oral tyrosine kinase inhibitor that targets VEGFR as well as PDGFR, c-Kit, rearranged during transfection (RET), and fms-like tyrosine receptor kinases (FLT3). In several phase II trials, sunitinib resulted in high levels of grade 3 and 4 toxicities, such as thrombocytopenia, neutropenia, and hand-foot skin reaction. More importantly, sunitinib has repeatedly resulted in minimal objective responses [95, 96]. A phase III trial of over 1000 patients with previously untreated advanced HCC comparing sunitinib to sorafenib was closed prematurely due to the inferiority of sunitinib. At the time of trial cessation, the median survival of patients was 7.9 months in the sunitinib group versus 10.2 months in the sorafenib group. Treatment-related deaths accounted for 3.3% of patients versus 0.3% of patients, respectively. Additionally, the median OS was shorter in HCV-infected patients [97].
13.4.1.3 Regorafenib
Similar to sorafenib, regorafenib also targets VEGF receptors 1 and 3, in addition to other kinases that promote tumor growth and angiogenesis. The recent RESORCE trial has preliminarily suggested a benefit with regorafenib as compared to placebo in 573 patients with Child-Pugh Class A cirrhosis who had radiologic progression on sorafenib. Regorafenib was associated with improved median overall survival (10.6 versus 7.8 months) and objective response rate (11% vs. 4%) [98]. This study is still ongoing. This has suggested that regorafenib may be a reasonable second-line therapy in patients who progress on or are intolerant of sorafenib.
13.4.1.4 Bevacizumab
Bevacizumab (Avastin) is an anti-VEGF monoclonal antibody which was first approved in 2004 for the treatment of metastatic colon cancer in combination with chemotherapy. Several phase I/II trials have shown that it is safe and potentially effective against HCC at doses of 5–10 mg/kg in several trials [99, 100]. However, these trials had small sample sizes of only 30–45 patients. Therefore, the efficacy of bevacizumab either alone or in combination needs to be further evaluated in phase III randomized trials. Additionally, studies have shown this agent to have a moderate effect on objective response rate, progression-free survival, and median overall survival when combined with gemcitabine and oxaliplatin (GEMOX) [101] or in combination with capecitabine with or without oxaliplatin [102, 103]. Outcomes of bevacizumab when combined with erlotinib, which targets EGFR, are discussed below. Lastly, bevacizumab may diminish neo-vessel formation after TACE due to its anti-angiogenesis effects [104].
13.4.1.5 Brivanib
Brivanib is an oral inhibitor of both VEGF and FGF signaling pathways, which was first tested as a second-line agent in patients who progressed or were intolerant of sorafenib. However, results of a phase III randomized trial did not show that brivanib improved overall survival [105]. Subsequently, the BRISK-FL phase III trial randomized 1150 patients with advanced HCC and no prior systemic treatment to receive either sorafenib 400 mg twice daily or brivanib 800 mg daily. The primary endpoint was median overall survival which was 9.9 months in the sorafenib group and 9.5 months in the brivanib group. However, although the study did not meet its primary endpoint of non-inferiority, the objective response rates and TTP were similar. Patients on brivanib had a higher rate of discontinuation due to adverse events (43 vs. 33%) [106]. Despite the trend toward increased OS in the brivanib, the drug could not meet approval for first-line therapy, owing to the strict requirements of non-inferiority trials, which required a hazard ratio for survival with 95% confidence interval between 1 and 1.08.
13.4.1.6 Others
Several other anti-VEGF agents have been evaluated in both phase II and phase III trials, some of which are still ongoing (Tables 13.1 and 13.2). These include axitinib, ramucirumab, and lenvatinib. Overall, despite the promise of some of these agents such as brivanib, none has shown a clinically significant improvement in overall survival as compared to either placebo or sorafenib.
13.4.2 Anti-PDGF Agents
13.4.2.1 Linifanib
Linifanib is a more potent targeted inhibitor of both VEGFR and PDGFR than sorafenib. In a phase II trial of 44 patients with advanced or metastatic HCC, treatment with linifanib yielded a median overall survival of 9.7 months, suggesting possible clinical efficacy. Patients were primarily Asian (89%), Child-Pugh Class A (86%), and HBV infected (61%) [107]. However, the phase III head-to-head trial of linifanib versus sorafenib in over 1000 patients failed to meet non-inferiority boundaries, and the overall survival rates were 9.1 versus 9.8 months, respectively. Linifanib also appeared to be more toxic with adverse events in 54% of patients versus 38% with sorafenib [108].
13.4.3 Anti-FGF Agents
FGFR signaling has a role in both proliferation and angiogenesis which contributes to hepatocarcinogenesis [109]. Studies in pancreatic tumors have suggested that resistance to VEGF-targeted therapy may be mediated by upregulation of FGFR signaling [110]. Thus, it was hypothesized that brivanib, mentioned above, might have increased efficacy in treatment of HCC by targeting both VEGFR and FGFR. Since the phase III non-inferiority trial of sorafenib versus brivanib did not demonstrate a clear clinical effect, there has been focus on the development of more specific FGFR agents and biomarkers which may demonstrate response to treatment. FGF19 is one such potential biomarker, amplified in 5–10% of HCC, which may predict response to targeted FGF therapy [47, 48]. In addition, blocking FGFR4 may help prevent hepatic tumor formation by interfering with the FGR19 signaling axis [111]. As a result, several generations of targeted FGFR agents have been developed and are underway in clinical studies. The first generation of these drugs were either pan-FGFR inhibitors or those with weak activity against FGFR4, including LY-2874455, ponatinib, BGJ398, and AZD4547 [112]. Currently, there are only a few phase I/II studies underway evaluating specific FGFR inhibitors (Table 13.1). Recent development of another selective FGFR4 inhibitor, BLU9931, may have promise as a future therapy for HCC [113].
13.4.4 Anti-EGRF Agents
13.4.4.1 Erlotinib
Erlotinib inhibits the tyrosine kinase domain of EGFR and has demonstrated antitumor activity and a median overall survival of 11–13 (11–13 months) in phase II clinical trials of patients with unresectable HCC [114, 115]. Expanding upon this earlier study, the phase III SEARCH trial included 720 patients with advanced HCC who were randomized to receive either sorafenib and erlotinib or sorafenib and placebo [116]. The trial did not show a significant benefit of combination therapy with erlotinib and sorafenib as compared to sorafenib alone (OS 9.5 vs. 8.5 months), and the addition of erlotinib resulted in increased toxicity resulting in shorter durations of treatment. Additionally, a phase II trial of erlotinib plus bevacizumab failed to validate the use of this combination strategy [117]. Other phase II trials of erlotinib and bevacizumab are underway.
13.4.5 Newer Drugs Under Development
13.4.5.1 MET
As previously mentioned, MET is part of the HGF signaling pathway, and expression of MET signature phenotype is correlated with tumor progression and metastasis [84]. Therefore, MET is a target of new drug development for treatment of HCC. Cabozantinib, which inhibits both MET and VEGFR2, has been shown to suppress tumor growth and metastasis both in vitro and in vivo [118]. This same study also showed high levels of activated MET that are associated with poor response to sorafenib, making this an attractive target for intervention. A phase III randomized trial (the CELESTIAL trial) of cabozantinib versus placebo in advanced HCC is still ongoing (Table 13.2). Tivantinib (ARQ197) which selectively targets c-MET may also be a valuable drug for second-line therapy. A randomized phase II trial of tivantinib versus placebo showed that patients with MET-high tumors who received tivantinib had median OS of 7.2 months, compared to 3.8 months for MET-high patients who received the placebo (HR, 0.38) [119]. A Japanese phase III trial (JET-HCC) with this drug is underway (Table 13.2).
13.4.5.2 TGF-β
TGF-β signaling is associated with cirrhosis, fibrosis, and inflammation as mentioned previously resulting in epithelial-to-mesenchymal transition and hepatocarcinogenesis [120]. Furthermore, late TGF-β signature correlates to tumor invasiveness and recurrence [83]. Therefore, it is hypothesized that inhibition of TGF-β in HCC will block both inflammation related to liver cirrhosis and HCC tumor metastasis. However, in many cancers, TGF-β has been shown to have both tumor suppressor and tumor promotor functions [121], making it difficult to develop novel inhibitors for therapy. LY2157299 (galunisertib) is a TGF-β inhibitor that has been shown to block HCC tumor invasion and angiogenesis in preclinical studies [122]. Preliminary results of a phase II trial demonstrated tolerable toxicity and increased TTP in patients with declines in serum alpha-fetoprotein and TGF-β levels [123]. Phase II clinical trials of galunisertib alone or in combination with sorafenib are ongoing (Table 13.1). Identification of biomarkers which are predictive of response will be useful for development of anti-TGF-β agents.
13.4.5.3 RAS/MAPK
Selective inhibitors of the RAS/MAPK pathway, which affects cellular proliferation, include those targeting MEK and RAF. A phase II trial of the MEK inhibitor, refametinib (BAY 86-9766), was conducted in 95 Asian, primary HBV-infected patients assigned to receive refametinib 50 mg twice daily and sorafenib 200 mg (morning)/400 mg (evening), with dose escalation to sorafenib 400 mg twice daily if tolerated. Disease control rate was 44.8% with median TTP of 122 days. Interestingly, the best clinical responders had RAS mutations, suggesting efficacy of this treatment in selected RAS-mutated patients. Unfortunately, dose modifications due to adverse events such as diarrhea, nausea, and vomiting occurred in most patients, which may limit the benefit of this therapeutic combination [124]. Additionally, a low proportion of HCC patients are known to have Ras mutation, thus limiting the feasibility of MEK inhibitors. Additionally, BRAF inhibitors, such as dabrafenib, are under early investigation for treatment in HCC. Many of these drugs are already FDA approved for treatment of advanced melanoma, which commonly harbors BRAF mutations (Table 13.1).
13.4.5.4 Antiproliferative/Cell Cycle
Cyclin-dependent kinases (CDK) are critical regulators of cell cycle control and apoptosis which are known to be deregulated in cancer [125]. CDKS are known to be altered in HCC, through gene deletions such as CDKN2A, which control CDK inhibitory proteins such as p16Ink4, p21, p27, and p57 [126]. Thus CDK inhibitors that can halt cell cycle progression are another potential therapeutic intervention in the treatment of HCC. Examples of this are currently in preclinical phases of development and include xylocydine, an inhibitor of CDK 1, 2, 7, and 9 which has shown the ability to suppress growth of HCC xenografts in nude mice [127]. Additionally, CDK4/6 inhibition can block proliferation in hepatoma cell lines [128]. A third study showed that treatment of xenografted HCC with the novel compounds BA-12 and BP-14 that antagonize CDK1/2/5/7 and CDK9 decreased tumor formation. It also diminished diethylnitrosamine (DEN)-induced hepatoma development in mice, suggesting a role for efficacy in the treatment of HCC [129].
13.4.5.5 PI3K/mTOR Inhibitors
Everolimus is an mTOR inhibitor which has been shown to improve survival and prevent tumor progression in preclinical models [130]. After success of early clinical studies [131], everolimus was tested in a phase III randomized controlled trial (EVOLVE-1) of 546 patients with sorafenib-refractory or intolerant advanced HCC. There was no difference in median OS in patients who received everolimus as compared to placebo (7.6 vs. 7.3 months). Interestingly, patients with HBV infection fared better than those with HCV (HR 0.63 vs. 0.93). Furthermore, the authors show that HBV-infected patients were more likely to have tuberous sclerosis 2 (TSC2)-null phenotype. This is significant since previous studies have shown that this phenotype is a predictive biomarker for response to everolimus [132]. Therefore, further studies are needed to validate the use of mTOR inhibitors in selected HCC patients.
13.4.5.6 HDACis
Histone deacetylases (HDAC) are important in chromatin remodeling, and epigenetic dysregulation plays a key role in HCC as previously described. HDAC inhibitors have become important in cancer therapy. They mediate cell death through a variety of mechanisms including cell growth arrest, induction of apoptosis, induction of autophagy, and anti-angiogenesis [80]. In an early phase I/II trial, 42 patients with unresectable HCC received intravenous dosing of belinostat, an HDAC inhibitor which is FDA approved for the treatment of peripheral T-cell lymphoma. The study found that belinostat was well tolerated and resulted in disease stabilization. Also, expression of HR23B, which is known to increase sensitivity to HDAC inhibitors [133], was associated with improved disease stabilization [134]. Currently, several phase I and II trials are underway evaluating the use of different HDAC inhibitors alone or in combination with sorafenib (Table 13.1).
13.4.5.7 Immunomodulators
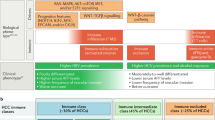
Immune checkpoint inhibitors have shown tremendous therapeutic activity in the treatment of advanced melanoma [135]. These include antibodies against cytotoxic T-lymphocyte protein (CTLA-4) and programmed cell death protein 1 (PD-1) and its ligand (PD-L1). CTLA-4 is expressed on regulatory T cells (Tregs) and serves as an inhibitory signal to activated T cells. Cancer cells protect themselves against activated T cells in part by expressing PD-L1 which interacts with PD-1 to attenuate T-cell responses. Therefore, inhibition of these immune checkpoints will improve tumor-associated immune responses. Thus far, results in clinical trials are promising. A phase I/II trial of nivolumab (anti-PD-1 antibody) showed that it was safe at doses up to 10 mL/kg. A total of 47 patients with noninfected HBV- and HCV-related HCC were examined, of whom 70% had extrahepatic metastasis. Most patients had failed sorafenib therapy. The overall objective response rate was 19%, with two patients (5%) demonstrating a complete response. Moreover, the dose escalation part of the study assessed the efficacy of nivolumab at doses between 0.1 and 10 mL/kg. Most importantly, patients demonstrated stable or improved response over time without the development of drug resistance [136]. This trial is still ongoing, and results were recently presented at the ASCO meeting in 2016. Currently, a phase III trial of nivolumab in HCC is underway (Table 13.2), as are other phase I and II trials of CTLA-4 and PD-1 antibodies (Table 13.1).
13.5 Future Directions
Overall there have been substantial developments in understanding the molecular pathogenesis of HCC. Unfortunately, this has not yet translated into more robust therapeutic advances other than sorafenib. For patients with HCC not amenable to potentially curative therapies such as resection, transplant, or ablation, there remain limited options. For early-stage patients who are able to undergo potentially curative resection, the majority (70%) recur with no proven adjuvant therapy [137]. Even sorafenib has failed to have success in the adjuvant setting. In the STORM randomized controlled phase III trial, over 1000 patients with early HCC who had a complete radiologic response to surgical resection or local ablation were treated with sorafenib 400 mg twice daily or placebo for up to 4 years. There was no difference in overall median recurrence-free survival between the two groups (33.7 vs. 33.3 months) [138]. These findings suggest that sorafenib may not prevent progression of early undetected tumor clones or de novo hepatocarcinogenesis. This highlights the fact that further research is indicated to better understand the molecular pathways and signatures which are associated with tumor recurrence.
Many promising drugs have failed to meet primary endpoints in phase II or phase III clinical trials based on the failure to show objective response rates based on the RECIST criteria. However, these criteria can be misleading and may underestimate response to immunotherapy or molecular targeted agents. As a result, the modified RECIST criteria have been developed which characterizes active tumor tissue based on arterial phase enhancement on imaging. These new criteria should be applied to future trials and can be enhanced through identification of other markers of tumor activity as opposed to just tumor size.
Other reasons for the lack of success in molecular targeted therapy thus far include the highly heterogeneic nature of HCC which encompasses numerous alterations in genetic pathways and epigenetic changes. Basket trials designed to enroll patients based on a specific molecular alteration in their tumor may be a more promising strategy to evaluate targeted agents in clinical trials such has been done with vemurafenib in V600E BRAF mutant cancers [139].
Further improvements in targeted therapy for HCC will focus on gaining a better understanding of molecular drivers and, most importantly, designing specific therapy for each patient based on molecular classification and/or etiology of his or her individual tumor(s). In addition, identification of biomarkers which will help identify responder from nonresponder to a specific therapy is also critical. Other promising avenues for research in the therapeutics of HCC include epigenetic modifiers and miRNA-based therapies and agents that target HCC tumor-initiating cells (the so-called cancer stem cells). Ultimately, the development of molecular targeted agents for HCC hinges on more effective translational research that will be able to show which agents are effective for which types of HCC.
References
Ferlay J, Soerjomataram I, Dikshit R, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359–86.
Nordenstedt H, White DL, El-Serag HB. The changing pattern of epidemiology in hepatocellular carcinoma. Dig Liver Dis. 2010;42(Suppl 3):S206–14.
Torre LA, Bray F, Siegel RL, et al. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108.
Shah SA, Cleary SP, Wei AC, et al. Recurrence after liver resection for hepatocellular carcinoma: risk factors, treatment, and outcomes. Surgery. 2007;141:330–9.
Llovet JM, Ricci S, Mazzaferro V, et al. Sorafenib in advanced hepatocellular carcinoma. N Engl J Med. 2008;359:378–90.
Huang C, Xu D, Xia Q, et al. Reversal of P-glycoprotein-mediated multidrug resistance of human hepatic cancer cells by Astragaloside II. J Pharm Pharmacol. 2012;64:1741–50.
Chan KT, Lung ML. Mutant p53 expression enhances drug resistance in a hepatocellular carcinoma cell line. Cancer Chemother Pharmacol. 2004;53:519–26.
Wang C, Zhang Y, Guo K, et al. Heat shock proteins in hepatocellular carcinoma: molecular mechanism and therapeutic potential. Int J Cancer. 2016;138:1824–34.
Wen L, Liang C, Chen E, et al. Regulation of multi-drug resistance in hepatocellular carcinoma cells is TRPC6/calcium dependent. Sci Rep. 2016;6:23269.
Deng GL, Zeng S, Shen H. Chemotherapy and target therapy for hepatocellular carcinoma: new advances and challenges. World J Hepatol. 2015;7:787–98.
Nagahama H, Okada S, Okusaka T, et al. Predictive factors for tumor response to systemic chemotherapy in patients with hepatocellular carcinoma. Jpn J Clin Oncol. 1997;27:321–4.
Olweny CL, Toya T, Katongole-Mbidde E, et al. Treatment of hepatocellular carcinoma with adriamycin. Preliminary communication. Cancer. 1975;36:1250–7.
Chlebowski RT, Brzechwa-Adjukiewicz A, Cowden A, et al. Doxorubicin (75 mg/m2) for hepatocellular carcinoma: clinical and pharmacokinetic results. Cancer Treat Rep. 1984;68:487–91.
Choi TK, Lee NW, Wong J. Chemotherapy for advanced hepatocellular carcinoma. Adriamycin versus quadruple chemotherapy. Cancer. 1984;53:401–5.
Ihde DC, Kane RC, Cohen MH, et al. Adriamycin therapy in American patients with hepatocellular carcinoma. Cancer Treat Rep. 1977;61:1385–7.
Nerenstone SR, Ihde DC, Friedman MA. Clinical trials in primary hepatocellular carcinoma: current status and future directions. Cancer Treat Rev. 1988;15:1–31.
Yeo W, Mok TS, Zee B, et al. A randomized phase III study of doxorubicin versus cisplatin/interferon alpha-2b/doxorubicin/fluorouracil (PIAF) combination chemotherapy for unresectable hepatocellular carcinoma. J Natl Cancer Inst. 2005;97:1532–8.
Lai CL, PC W, Chan GC, et al. Doxorubicin versus no antitumor therapy in inoperable hepatocellular carcinoma. A prospective randomized trial. Cancer. 1988;62:479–83.
Gish RG, Porta C, Lazar L, et al. Phase III randomized controlled trial comparing the survival of patients with unresectable hepatocellular carcinoma treated with nolatrexed or doxorubicin. J Clin Oncol. 2007;25:3069–75.
Sciarrino E, Simonetti RG, Le Moli S, et al. Adriamycin treatment for hepatocellular carcinoma. Experience with 109 patients. Cancer. 1985;56:2751–5.
Boige V, Taieb J, Hebbar M, et al. Irinotecan as first-line chemotherapy in patients with advanced hepatocellular carcinoma: a multicenter phase II study with dose adjustment according to baseline serum bilirubin level. Eur J Cancer. 2006;42:456–9.
Dunk AA, Scott SC, Johnson PJ, et al. Mitozantrone as single agent therapy in hepatocellular carcinoma. A phase II study. J Hepatol. 1985;1:395–404.
Halm U, Etzrodt G, Schiefke I, et al. A phase II study of pegylated liposomal doxorubicin for treatment of advanced hepatocellular carcinoma. Ann Oncol. 2000;11:113–4.
Kubicka S, Rudolph KL, Tietze MK, et al. Phase II study of systemic gemcitabine chemotherapy for advanced unresectable hepatobiliary carcinomas. Hepato-Gastroenterology. 2001;48:783–9.
Lin AY, Brophy N, Fisher GA, et al. Phase II study of thalidomide in patients with unresectable hepatocellular carcinoma. Cancer. 2005;103:119–25.
Pohl J, Zuna I, Stremmel W, et al. Systemic chemotherapy with epirubicin for treatment of advanced or multifocal hepatocellular carcinoma. Chemotherapy. 2001;47:359–65.
Porta C, Moroni M, Nastasi G, et al. 5-Fluorouracil and d,l-leucovorin calcium are active to treat unresectable hepatocellular carcinoma patients: preliminary results of a phase II study. Oncology. 1995;52:487–91.
Tetef M, Doroshow J, Akman S, et al. 5-fluorouracil and high-dose calcium leucovorin for hepatocellular carcinoma: a phase II trial. Cancer Investig. 1995;13:460–3.
Brandi G, De Rosa F, Agostini V, et al. Metronomic capecitabine in advanced hepatocellular carcinoma patients: a phase II study. Oncologist. 2013;18:1256–7.
Patt YZ, Hassan MM, Aguayo A, et al. Oral capecitabine for the treatment of hepatocellular carcinoma, cholangiocarcinoma, and gallbladder carcinoma. Cancer. 2004;101:578–86.
Abdel-Rahman O, Abdel-Wahab M, Shaker M, et al. Sorafenib versus capecitabine in the management of advanced hepatocellular carcinoma. Med Oncol. 2013;30:655.
Parikh PM, Fuloria J, Babu G, et al. A phase II study of gemcitabine and cisplatin in patients with advanced hepatocellular carcinoma. Trop Gastroenterol. 2005;26:115–8.
Lombardi G, Zustovich F, Farinati F, et al. Pegylated liposomal doxorubicin and gemcitabine in patients with advanced hepatocellular carcinoma: results of a phase 2 study. Cancer. 2011;117:125–33.
Louafi S, Boige V, Ducreux M, et al. Gemcitabine plus oxaliplatin (GEMOX) in patients with advanced hepatocellular carcinoma (HCC): results of a phase II study. Cancer. 2007;109:1384–90.
Boige V, Raoul JL, Pignon JP, et al. Multicentre phase II trial of capecitabine plus oxaliplatin (XELOX) in patients with advanced hepatocellular carcinoma: FFCD 03-03 trial. Br J Cancer. 2007;97:862–7.
Qin S, Bai Y, Lim HY, et al. Randomized, multicenter, open-label study of oxaliplatin plus fluorouracil/leucovorin versus doxorubicin as palliative chemotherapy in patients with advanced hepatocellular carcinoma from Asia. J Clin Oncol. 2013;31:3501–8.
Leung TW, Patt YZ, Lau WY, et al. Complete pathological remission is possible with systemic combination chemotherapy for inoperable hepatocellular carcinoma. Clin Cancer Res. 1999;5:1676–81.
Farrell GC, Larter CZ. Nonalcoholic fatty liver disease: from steatosis to cirrhosis. Hepatology. 2006;43:S99–S112.
Farazi PA, Depinho RA. Hepatocellular carcinoma pathogenesis: from genes to environment. Nat Rev Cancer. 2006;6:674–87.
Yin C, Evason KJ, Asahina K, et al. Hepatic stellate cells in liver development, regeneration, and cancer. J Clin Invest. 2013;123:1902–10.
Ahn SM, Jang SJ, Shim JH, et al. Genomic portrait of resectable hepatocellular carcinomas: implications of RB1 and FGF19 aberrations for patient stratification. Hepatology. 2014;60:1972–82.
Guichard C, Amaddeo G, Imbeaud S, et al. Integrated analysis of somatic mutations and focal copy-number changes identifies key genes and pathways in hepatocellular carcinoma. Nat Genet. 2012;44:694–8.
Kan Z, Zheng H, Liu X, et al. Whole-genome sequencing identifies recurrent mutations in hepatocellular carcinoma. Genome Res. 2013;23:1422–33.
Llovet JM, Villanueva A, Lachenmayer A, et al. Advances in targeted therapies for hepatocellular carcinoma in the genomic era. Nat Rev Clin Oncol. 2015;12:436.
Villanueva A, Llovet JM. Liver cancer in 2013: mutational landscape of HCC—the end of the beginning. Nat Rev Clin Oncol. 2014;11:73–4.
Schulze K, Imbeaud S, Letouze E, et al. Exome sequencing of hepatocellular carcinomas identifies new mutational signatures and potential therapeutic targets. Nat Genet. 2015;47:505–11.
Chiang DY, Villanueva A, Hoshida Y, et al. Focal gains of VEGFA and molecular classification of hepatocellular carcinoma. Cancer Res. 2008;68:6779–88.
Sawey ET, Chanrion M, Cai C, et al. Identification of a therapeutic strategy targeting amplified FGF19 in liver cancer by oncogenomic screening. Cancer Cell. 2011;19:347–58.
Totoki Y, Tatsuno K, Covington KR, et al. Trans-ancestry mutational landscape of hepatocellular carcinoma genomes. Nat Genet. 2014;46:1267–73.
Kramer OH. HDAC2: a critical factor in health and disease. Trends Pharmacol Sci. 2009;30:647–55.
Lee JS, Chu IS, Heo J, et al. Classification and prediction of survival in hepatocellular carcinoma by gene expression profiling. Hepatology. 2004;40:667–76.
Dhanasekaran R, Bandoh S, Roberts LR. Molecular pathogenesis of hepatocellular carcinoma and impact of therapeutic advances. F1000Res. 2016;5:879.
Gouas DA, Shi H, Hautefeuille AH, et al. Effects of the TP53 p.R249S mutant on proliferation and clonogenic properties in human hepatocellular carcinoma cell lines: interaction with hepatitis B virus X protein. Carcinogenesis. 2010;31:1475–82.
Hamid AS, Tesfamariam IG, Zhang Y, et al. Aflatoxin B1-induced hepatocellular carcinoma in developing countries: geographical distribution, mechanism of action and prevention. Oncol Lett. 2013;5:1087–92.
Ozturk M. p53 mutation in hepatocellular carcinoma after aflatoxin exposure. Lancet. 1991;338:1356–9.
Lunn RM, Zhang YJ, Wang LY, et al. p53 mutations, chronic hepatitis B virus infection, and aflatoxin exposure in hepatocellular carcinoma in Taiwan. Cancer Res. 1997;57:3471–7.
Kasprzak A, Adamek A, Przybyszewska W, et al. p53 immunocytochemistry and TP53 gene mutations in patients with chronic hepatitis C virus (HCV) infection. Folia Histochem Cytobiol. 2009;47:35–42.
Liu J, Ma Q, Zhang M, et al. Alterations of TP53 are associated with a poor outcome for patients with hepatocellular carcinoma: evidence from a systematic review and meta-analysis. Eur J Cancer. 2012;48:2328–38.
Aravalli RN, Steer CJ, Cressman EN. Molecular mechanisms of hepatocellular carcinoma. Hepatology. 2008;48:2047–63.
Lachenmayer A, Alsinet C, Savic R, et al. Wnt-pathway activation in two molecular classes of hepatocellular carcinoma and experimental modulation by sorafenib. Clin Cancer Res. 2012;18:4997–5007.
Llovet JM, Chen Y, Wurmbach E, et al. A molecular signature to discriminate dysplastic nodules from early hepatocellular carcinoma in HCV cirrhosis. Gastroenterology. 2006;131:1758–67.
Elsharkawy AM, Mann DA. Nuclear factor-kappaB and the hepatic inflammation-fibrosis-cancer axis. Hepatology. 2007;46:590–7.
Luedde T, Schwabe RF. NF-kappaB in the liver—linking injury, fibrosis and hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol. 2011;8:108–18.
Matter MS, Decaens T, Andersen JB, et al. Targeting the mTOR pathway in hepatocellular carcinoma: current state and future trends. J Hepatol. 2014;60:855–65.
Llovet JM, Villanueva A, Lachenmayer A, et al. Advances in targeted therapies for hepatocellular carcinoma in the genomic era. Nat Rev Clin Oncol. 2015;12:408–24.
Baba HA, Wohlschlaeger J, Cicinnati VR, et al. Phosphorylation of p70S6 kinase predicts overall survival in patients with clear margin-resected hepatocellular carcinoma. Liver Int. 2009;29:399–405.
Villanueva A, Chiang DY, Newell P, et al. Pivotal role of mTOR signaling in hepatocellular carcinoma. Gastroenterology. 2008;135:1972–1983, 1983 e1–11.
Zhou L, Huang Y, Li J, et al. The mTOR pathway is associated with the poor prognosis of human hepatocellular carcinoma. Med Oncol. 2010;27:255–61.
Calvisi DF, Ladu S, Gorden A, et al. Ubiquitous activation of Ras and Jak/Stat pathways in human HCC. Gastroenterology. 2006;130:1117–28.
Newell P, Toffanin S, Villanueva A, et al. Ras pathway activation in hepatocellular carcinoma and anti-tumoral effect of combined sorafenib and rapamycin in vivo. J Hepatol. 2009;51:725–33.
Delire B, Starkel P. The Ras/MAPK pathway and hepatocarcinoma: pathogenesis and therapeutic implications. Eur J Clin Investig. 2015;45:609–23.
Nakamura H, Aoki H, Hino O, et al. HCV core protein promotes heparin binding EGF-like growth factor expression and activates Akt. Hepatol Res. 2011;41:455–62.
Zhang X, Zhang H, Ye L. Effects of hepatitis B virus X protein on the development of liver cancer. J Lab Clin Med. 2006;147:58–66.
Chen L, Shi Y, Jiang CY, et al. Expression and prognostic role of pan-Ras, Raf-1, pMEK1 and pERK1/2 in patients with hepatocellular carcinoma. Eur J Surg Oncol. 2011;37:513–20.
Morell CM, Strazzabosco M. Notch signaling and new therapeutic options in liver disease. J Hepatol. 2014;60:885–90.
Villanueva A, Alsinet C, Yanger K, et al. Notch signaling is activated in human hepatocellular carcinoma and induces tumor formation in mice. Gastroenterology. 2012;143:1660.
West AC, Johnstone RW. New and emerging HDAC inhibitors for cancer treatment. J Clin Invest. 2014;124:30–9.
Lachenmayer A, Toffanin S, Cabellos L, et al. Combination therapy for hepatocellular carcinoma: additive preclinical efficacy of the HDAC inhibitor panobinostat with sorafenib. J Hepatol. 2012;56:1343–50.
Witt O, Lindemann R. HDAC inhibitors: magic bullets, dirty drugs or just another targeted therapy. Cancer Lett. 2009;280:123–4.
Khan O, La Thangue NB. HDAC inhibitors in cancer biology: emerging mechanisms and clinical applications. Immunol Cell Biol. 2012;90:85–94.
LM W, Yang Z, Zhou L, et al. Identification of histone deacetylase 3 as a biomarker for tumor recurrence following liver transplantation in HBV-associated hepatocellular carcinoma. PLoS One. 2010;5:e14460.
Harbour JW, Dean DC. The Rb/E2F pathway: expanding roles and emerging paradigms. Genes Dev. 2000;14:2393–409.
Coulouarn C, Factor VM, Thorgeirsson SS. Transforming growth factor-beta gene expression signature in mouse hepatocytes predicts clinical outcome in human cancer. Hepatology. 2008;47:2059–67.
Kaposi-Novak P, Lee JS, Gomez-Quiroz L, et al. Met-regulated expression signature defines a subset of human hepatocellular carcinomas with poor prognosis and aggressive phenotype. J Clin Invest. 2006;116:1582–95.
Llovet JM, Pena CE, Lathia CD, et al. Plasma biomarkers as predictors of outcome in patients with advanced hepatocellular carcinoma. Clin Cancer Res. 2012;18:2290–300.
Schoenleber SJ, Kurtz DM, Talwalkar JA, et al. Prognostic role of vascular endothelial growth factor in hepatocellular carcinoma: systematic review and meta-analysis. Br J Cancer. 2009;100:1385–92.
Zhang W, Kim R, Quintini C, et al. Prognostic role of plasma vascular endothelial growth factor in patients with hepatocellular carcinoma undergoing liver transplantation. Liver Transplant. 2015;21:101–11.
Cheng AL, Kang YK, Chen Z, et al. Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: a phase III randomised, double-blind, placebo-controlled trial. Lancet Oncol. 2009;10:25–34.
Bruix J, Raoul JL, Sherman M, et al. Efficacy and safety of sorafenib in patients with advanced hepatocellular carcinoma: subanalyses of a phase III trial. J Hepatol. 2012;57:821–9.
Llovet JM, Real MI, Montana X, et al. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: a randomised controlled trial. Lancet. 2002;359:1734–9.
Lo CM, Ngan H, Tso WK, et al. Randomized controlled trial of transarterial lipiodol chemoembolization for unresectable hepatocellular carcinoma. Hepatology. 2002;35:1164–71.
Kudo M, Imanaka K, Chida N, et al. Phase III study of sorafenib after transarterial chemoembolisation in Japanese and Korean patients with unresectable hepatocellular carcinoma. Eur J Cancer. 2011;47:2117–27.
Lencioni R, Llovet JM, Han G, et al. Sorafenib or placebo plus TACE with doxorubicin-eluting beads for intermediate stage HCC: the SPACE trial. J Hepatol. 2016;64:1090–8.
Abou-Alfa GK, Johnson P, Knox JJ, et al. Doxorubicin plus sorafenib vs doxorubicin alone in patients with advanced hepatocellular carcinoma: a randomized trial. JAMA. 2010;304:2154–60.
Barone C, Basso M, Biolato M, et al. A phase II study of sunitinib in advanced hepatocellular carcinoma. Dig Liver dis. 2013;45:692–8.
Faivre S, Raymond E, Boucher E, et al. Safety and efficacy of sunitinib in patients with advanced hepatocellular carcinoma: an open-label, multicentre, phase II study. Lancet Oncol. 2009;10:794–800.
Cheng AL, Kang YK, Lin DY, et al. Sunitinib versus sorafenib in advanced hepatocellular cancer: results of a randomized phase III trial. J Clin Oncol. 2013;31:4067–75.
Bruix J, Merle P, Granito A, et al. Efficacy and safety of regorafenib versus placebo in patients with hepatocellular carcinoma progressing on sorafenib: results of the international, randomized phase 3 Resorce trial. Esmo World Congress on Gastrointestinal Cancer. Abstract Lba-03. Presented June 30, 2016.
Boige V, Malka D, Bourredjem A, et al. Efficacy, safety, and biomarkers of single-agent bevacizumab therapy in patients with advanced hepatocellular carcinoma. Oncologist. 2012;17:1063–72.
Siegel AB, Cohen EI, Ocean A, et al. Phase II trial evaluating the clinical and biologic effects of bevacizumab in unresectable hepatocellular carcinoma. J Clin Oncol. 2008;26:2992–8.
Zhu AX, Blaszkowsky LS, Ryan DP, et al. Phase II study of gemcitabine and oxaliplatin in combination with bevacizumab in patients with advanced hepatocellular carcinoma. J Clin Oncol. 2006;24:1898–903.
Hsu CH, Yang TS, Hsu C, et al. Efficacy and tolerability of bevacizumab plus capecitabine as first-line therapy in patients with advanced hepatocellular carcinoma. Br J Cancer. 2010;102:981–6.
Sun W, Sohal D, Haller DG, et al. Phase 2 trial of bevacizumab, capecitabine, and oxaliplatin in treatment of advanced hepatocellular carcinoma. Cancer. 2011;117:3187–92.
Britten CD, Gomes AS, Wainberg ZA, et al. Transarterial chemoembolization plus or minus intravenous bevacizumab in the treatment of hepatocellular cancer: a pilot study. BMC Cancer. 2012;12:16.
Llovet JM, Decaens T, Raoul JL, et al. Brivanib in patients with advanced hepatocellular carcinoma who were intolerant to sorafenib or for whom sorafenib failed: results from the randomized phase III BRISK-PS study. J Clin Oncol. 2013;31:3509–16.
Johnson PJ, Qin S, Park JW, et al. Brivanib versus sorafenib as first-line therapy in patients with unresectable, advanced hepatocellular carcinoma: results from the randomized phase III BRISK-FL study. J Clin Oncol. 2013;31:3517–24.
Toh HC, Chen PJ, Carr BI, et al. Phase 2 trial of linifanib (ABT-869) in patients with unresectable or metastatic hepatocellular carcinoma. Cancer. 2013;119:380–7.
Cainap C, Qin S, Huang WT, et al. Linifanib versus Sorafenib in patients with advanced hepatocellular carcinoma: results of a randomized phase III trial. J Clin Oncol. 2015;33:172–9.
Sandhu DS, Baichoo E, Roberts LR. Fibroblast growth factor signaling in liver carcinogenesis. Hepatology. 2014;59:1166–73.
Casanovas O, Hicklin DJ, Bergers G, et al. Drug resistance by evasion of antiangiogenic targeting of VEGF signaling in late-stage pancreatic islet tumors. Cancer Cell. 2005;8:299–309.
French DM, Lin BC, Wang M, et al. Targeting FGFR4 inhibits hepatocellular carcinoma in preclinical mouse models. PLoS One. 2012;7:e36713.
Hagel M, Miduturu C, Sheets M, et al. First selective small molecule inhibitor of FGFR4 for the treatment of hepatocellular carcinomas with an activated FGFR4 signaling pathway. Cancer Discov. 2015;5:424–37.
Schmidt B, Wei L, Deperalta DK, et al. Molecular subclasses of hepatocellular carcinoma predict sensitivity to fibroblast growth factor receptor inhibition. Int J Cancer. 2016;138:1494–505.
Philip PA, Mahoney MR, Allmer C, et al. Phase II study of Erlotinib (OSI-774) in patients with advanced hepatocellular cancer. J Clin Oncol. 2005;23:6657–63.
Thomas MB, Chadha R, Glover K, et al. Phase 2 study of erlotinib in patients with unresectable hepatocellular carcinoma. Cancer. 2007;110:1059–67.
Zhu AX, Rosmorduc O, Evans TR, et al. SEARCH: a phase III, randomized, double-blind, placebo-controlled trial of sorafenib plus erlotinib in patients with advanced hepatocellular carcinoma. J Clin Oncol. 2015;33:559–66.
Philip PA, Mahoney MR, Holen KD, et al. Phase 2 study of bevacizumab plus erlotinib in patients with advanced hepatocellular cancer. Cancer. 2012;118:2424–30.
Xiang Q, Chen W, Ren M, et al. Cabozantinib suppresses tumor growth and metastasis in hepatocellular carcinoma by a dual blockade of VEGFR2 and MET. Clin Cancer Res. 2014;20:2959–70.
Santoro A, Rimassa L, Borbath I, et al. Tivantinib for second-line treatment of advanced hepatocellular carcinoma: a randomised, placebo-controlled phase 2 study. Lancet Oncol. 2013;14:55–63.
Giannelli G, Villa E, Lahn M. Transforming growth factor-beta as a therapeutic target in hepatocellular carcinoma. Cancer Res. 2014;74:1890–4.
Neuzillet C, Tijeras-Raballand A, Cohen R, et al. Targeting the TGFbeta pathway for cancer therapy. Pharmacol Ther. 2015;147:22–31.
Dituri F, Mazzocca A, Fernando J, et al. Differential inhibition of the TGF-beta signaling pathway in HCC cells using the small molecule inhibitor LY2157299 and the D10 monoclonal antibody against TGF-beta receptor type II. PLoS One. 2013;8:e67109.
Faivre SJ, Santoro A, Kelley RK, Merle P, Gane E, Douillard J-Y, Waldschmidt D, Mulcahy MF, Costentin C, Minguez B, Papappicco P, Gueorguieva I, Cleverly A, Desaiah D, Lahn MMF, Murray N, Benhadji KA, Raymond E, Giannelli G. Randomized dose comparison phase II study of the oral transforming growth factor-Beta (Tgf-S) receptor I kinase inhibitor Ly2157299 monohydrate (Ly) in patients with advanced hepatocellular carcinoma (Hcc). Asco gastrointestinal cancers symposium; 2014.
Lim HY, Heo J, Choi HJ, et al. A phase II study of the efficacy and safety of the combination therapy of the MEK inhibitor refametinib (BAY 86-9766) plus sorafenib for Asian patients with unresectable hepatocellular carcinoma. Clin Cancer Res. 2014;20:5976–85.
Rossi AG, Sawatzky DA, Walker A, et al. Cyclin-dependent kinase inhibitors enhance the resolution of inflammation by promoting inflammatory cell apoptosis. Nat Med. 2006;12:1056–64.
Fornari F, Gramantieri L, Ferracin M, et al. MiR-221 controls CDKN1C/p57 and CDKN1B/p27 expression in human hepatocellular carcinoma. Oncogene. 2008;27:5651–61.
Cho SJ, Lee SS, Kim YJ, et al. Xylocydine, a novel Cdk inhibitor, is an effective inducer of apoptosis in hepatocellular carcinoma cells in vitro and in vivo. Cancer Lett. 2010;287:196–206.
Rivadeneira DB, Mayhew CN, Thangavel C, et al. Proliferative suppression by CDK4/6 inhibition: complex function of the retinoblastoma pathway in liver tissue and hepatoma cells. Gastroenterology. 2010;138:1920–30.
Haider C, Grubinger M, Reznickova E, et al. Novel inhibitors of cyclin-dependent kinases combat hepatocellular carcinoma without inducing chemoresistance. Mol Cancer Ther. 2013;12:1947–57.
Semela D, Piguet AC, Kolev M, et al. Vascular remodeling and antitumoral effects of mTOR inhibition in a rat model of hepatocellular carcinoma. J Hepatol. 2007;46:840–8.
Zhu AX, Abrams TA, Miksad R, et al. Phase 1/2 study of everolimus in advanced hepatocellular carcinoma. Cancer. 2011;117:5094–102.
Huynh H, Hao HX, Chan SL, et al. Loss of tuberous sclerosis complex 2 (TSC2) is frequent in hepatocellular carcinoma and predicts response to mTORC1 inhibitor Everolimus. Mol Cancer Ther. 2015;14:1224–35.
Khan O, Fotheringham S, Wood V, et al. HR23B is a biomarker for tumor sensitivity to HDAC inhibitor-based therapy. Proc Natl Acad Sci U S A. 2010;107:6532–7.
Yeo W, Chung HC, Chan SL, et al. Epigenetic therapy using belinostat for patients with unresectable hepatocellular carcinoma: a multicenter phase I/II study with biomarker and pharmacokinetic analysis of tumors from patients in the Mayo phase II consortium and the cancer therapeutics research group. J Clin Oncol. 2012;30:3361–7.
Marquez-Rodas I, Cerezuela P, Soria A, et al. Immune checkpoint inhibitors: therapeutic advances in melanoma. Ann Transl Med. 2015;3:267.
El-Khoueiry AB, Ignacio M, Crocenzi TS, et al. Phase I/II safety and antitumor activity of nivolumab in patients with advanced hepatocellular carcinoma (Hcc): CA209-040. J Clin Oncol. 2015;33(Suppl; Abstr Lba101).
Llovet JM, Schwartz M, Mazzaferro V. Resection and liver transplantation for hepatocellular carcinoma. Semin Liver Dis. 2005;25:181–200.
Bruix J, Takayama T, Mazzaferro V, et al. Adjuvant sorafenib for hepatocellular carcinoma after resection or ablation (STORM): a phase 3, randomised, double-blind, placebo-controlled trial. Lancet Oncol. 2015;16:1344–54.
Hyman DM, Puzanov I, Subbiah V, et al. Vemurafenib in multiple nonmelanoma cancers with BRAF V600 mutations. N Engl J Med. 2015;373:726–36.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Greco, S.H., Spencer, K., Carpizo, D.R. (2018). The Future Prospect of Targeted Therapy in Hepatocellular Carcinoma. In: Liu, C. (eds) Precision Molecular Pathology of Liver Cancer. Molecular Pathology Library. Springer, Cham. https://doi.org/10.1007/978-3-319-68082-8_13
Download citation
DOI: https://doi.org/10.1007/978-3-319-68082-8_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-68080-4
Online ISBN: 978-3-319-68082-8
eBook Packages: MedicineMedicine (R0)