Abstract
Early diagnosis is a top priority for women with endometriosis. However, diagnostic delays are still common. It is of utmost importance to prevent diagnostic delay as this can have an adverse impact on women’s physical and psychosocial health, including undergoing unnecessary treatments and a worsening of symptoms over time. Furthermore, women with endometriosis experience a sense of relief at diagnosis. The factors contributing to diagnostic delay are well documented and are differentiated into patient and medical factors, such as normalization of symptoms form both sides. The next step is to conduct more research into preventing diagnostic delay and translating evidence into clinical practice by educating the general public on the topic of endometriosis, by monitoring healthcare quality and by conducting research into biomarkers.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Endometriosis
- Patient centredness
- Patient centricity
- Adolescent endometriosis
- Quality of life
- Diagnosis
- Diagnostic delay
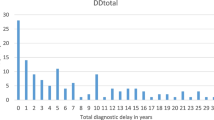
Diagnostic delay in women with endometriosis refers to the time gap between the onset of symptoms and receiving a medically confirmed diagnosis. A myriad of studies reported that diagnostic delays are common in women with endometriosis. However, reported delays seem to be much longer in patients recruited from patient associations as compared to patients recruited from secondary and tertiary care clinics (i.e. a median delay of 7 years vs. a median delay of 1.5 and 2 years, respectively) [1].
Early diagnosis is a top priority for women with endometriosis. A recent systematic review, including all studies on endometriosis patient’s perspective on healthcare , concluded that there are three related primary targets for improving the patient centredness of care, namely: respecting patients, believing patients and timely diagnosis of endometriosis [2]. These three care aspects were unequivocally reported as important and problematic by at least five studies [2]. More specifically, regarding a timely diagnosis, five qualitative studies agreed on its importance to patients [3,4,5,6,7], and nine qualitative studies agreed that patients assessed the service quality problematic in this respect [3,4,5,6,7,8,9,10,11]. An example of a patient quote: I think the biggest problem initially was getting a diagnosis which took years [6]. A recent empirical study, questioning patients from a European clinic on the importance and service quality of 38 care aspects, confirmed the relevance of this target to improve the patient centredness of endometriosis care [12].
It is our job as healthcare professionals to diagnose patients with endometriosis in time as to preserve these women from many years of unnecessary suffering.
Why Is a Delay in Diagnosis Problematic ?
Despite the reported differences in the length of diagnostic delay, the literature is unequivocal on the adverse consequences of a delayed diagnosis, both from a socio-economical perspective and a patient’s perspective. From a socio-economical perspective , a timely diagnosis is important as it might reduce endometriosis-associated costs by decreasing productivity loss and healthcare consumption [13]. A multicentre study estimated the average annual total costs of endometriosis at €9579 per patient [14]. From a patient’s perspective, the delay in diagnosis is detrimental to patients’ physical and psychosocial health.
Regarding patients’ physical health, the delay in diagnosis of endometriosis increases not only the length of suffering from symptoms but also its severity as symptoms worsen over time [15, 16]. For example, if endometriosis is already present but not diagnosed and treated during adolescence, it can progress and result in infertility during adulthood [17]. Moreover, a delayed diagnosis can also cause women to undergo many (unnecessary) medical tests and treatments [16]. Furthermore, receiving a timely diagnosis is important to start the correct treatment. Medical treatment is associated with alleviation of pain and improved pregnancy rates [18]. Surgical treatment can result in improvements of pain, quality of life and sexual functioning and is associated with good fertility rates [19, 20].
Regarding patient’s psychosocial health, quantitative studies found an association between diagnostic delays and reduced health-related quality of life [21]. Furthermore, Staal et al. [22] found that the long time lag until recognition of endometriosis symptoms as part of a disease is a traumatizing experience for patients. Patients feel angry and frustrated for not being believed or understood by their healthcare professionals who normalized their symptoms as part of menstrual pain or disregarded them as imaginary [3, 16, 23]. An example of a patient quote: When they gave me my endo-diagnosis, I was fuming that I hadn’t been believed and that I hadn’t been taken seriously [4]. Moreover, the fear of not knowing what is wrong (i.e. diagnostic uncertainty) [23] and the social stigma of not being able to perform as normal at work and at home add to the traumatizing experience [3].
Why Is Diagnosis a Relief ?
When a diagnosis is reached, women will initially feel overwhelmed and worried as there is no cure and because of the risk for infertility [16]. Later on, receiving a diagnosis is experienced as a relief for the following reasons: (1) it provides a language to talk about symptoms (i.e. possibility to communicate about the disease to family or employer); (2) it provides a sense of legitimation and, thus, justified access to psychosocial support; (3) it makes feelings of fear and self-doubt disappear; (4) it gives a feeling of liberation and empowerment; (5) it offers hope for appropriate treatment and, hence, pain reduction; and (6) it means that the symptoms are not caused by a deadly disease, such as cancer [3, 16, 23]. An example of a patient quote: I was in a way relieved because you have the answers like there was something wrong and that’s why you are experiencing what you are, plus it wasn’t sort of like an ectopic pregnancy and other things that I’d been really scared about up until being diagnosed. At the same time a bit overwhelming that it was something that was going to stay there, that it wasn’t just something that could be treated with antibiotics. Plus the risk it has to your fertility and stuff like that [16].
What Causes the Delay in Diagnosis?
According to a recent Belgian study, a significant delay between the onset of symptoms and the patient’s initiative of seeking medical help exists (i.e. an average of 1 year for a total delay of 2 years) [13]. Indeed, Ballard et al. [3] studied the reasons for delay in diagnosis and differentiated patient factors (e.g. normalization of symptoms or feelings of embarrassment) from medical factors (e.g. normalization or hormonal suppression of symptoms or using non-discriminatory investigations). The following patient quote is exemplary for the medical factors: From the time I was 13, I went through a number of different doctors to try and find the problem, most just told me that some people have heavier periods than others and more pain and don’t cope well with the pain, and that it was normal [16]. A recent study by Moradi et al. [16] pointed out that patient factors are also related to the patient’s family, friends and colleagues. More specifically, women with endometriosis described that they normalized their symptoms amongst others because their family and friends told them that pain and bleeding were normal .
What Do We Still Need to Know?
Although the factors contributing to the diagnostic delay are well documented, many women still experience significant delays [23]. This means that the implications of previous research should be taken into account by clinical practice and that more research on preventing diagnostic delays is required. Patients will appreciate research into diagnostic delays. The participants from the study of Staal et al. [22] on diagnostic delay reported that this study helped them to emotionally deal with the disease as it made them feel understood and taken seriously.
First of all, in order to limit the medical factors causing the delay, the flaws in the current diagnostic process in case of pelvic pain should be identified. Currently, the knowledge on endometriosis and diagnostic strategies in women with endometriosis of Dutch general practitioners (GPs) are, for example, being investigated [22]. It would also be interesting to find out if diagnostic delays differ between countries with different healthcare systems.
Second, research efforts should be devoted to developing tools that aid diagnosis based on symptoms. Currently, a definitive diagnosis of endometriosis requires laparoscopy, but this invasive procedure cannot be performed on the entire population. A Scandinavian group of researchers has developed an anamnestic tool for physicians [24]. Our own group has developed a diagnostic self-screening tool [25]. Measuring menstrual pain and defining what is considered normal and what is not are still challenging. When pain begins soon after menarche, neither the patient nor the physician would know if the experienced pain is of a normal intensity or whether it was abnormal and was caused by a disease such as endometriosis [26].
Third, existing endometriosis-associated biomarkers should be validated, and new biomarkers should be identified to develop an accurate, noninvasive method to diagnose endometriosis [27]. An Iranian qualitative study found that both patients and physicians agree on the importance of reliable diagnostic indicators [28].
In order to limit the patient factors causing the delay, women with endometriosis have stressed the importance of increasing awareness and understanding in society about endometriosis, for example, at schools [16]. This is especially important since many women reported that they had not heard about endometriosis prior to their diagnosis [16].
Conclusion
Endometriosis still remains undiagnosed for years in many women, placing a significant physical and psychosocial burden on these women and an important socio-economical burden on society. To prevent diagnostic delays, both patient and medical factors related to delay need to be addressed by educating the general public, monitoring healthcare quality and conducting research into biomarkers.
References
De Graaff AA, Dirksen CD, Simoens S, De Bie B, Hummelshoj L, D’Hooghe TM, Dunselman GA. Quality of life outcomes in women with endometriosis are highly influenced by recruitment strategies. Hum Reprod. 2015;30(6):1331–41.
Dancet EA, Apers S, Kremer JA, Nelen WL, Sermeus W, D’Hooghe TM. The patient-centeredness of endometriosis care and targets for improvement: a systematic review. Gynecol Obstet Invest. 2014;78(2):69–80.
Ballard K, Lowton K, Wright J. What’s the delay? A qualitative study of women’s experiences of reaching a diagnosis of endometriosis. Fertil Steril. 2006;86(5):1296–301.
Denny E. ‘You are one of the unlucky ones’: delay in the diagnosis of endometriosis. Divers Health Social Care. 2004;1:39–44.
Denny E, Mann CH. Endometriosis and the primary care consultation. Eur J Obstet Gynecol Reprod Biol. 2008;139:111–5.
Jones G, Jenkinson C, Kennedy S. The impact of endometriosis upon quality of life: a qualitative analysis. J Psychosom Obstet Gynaecol. 2004;25:123–33.
Manderson L, Warren N, Markovic M. Circuit breaking: pathways of treatment seeking for women with endometriosis in Australia. Qual Health Res. 2008;18:522–34.
Denny E. Women’s experience of endometriosis. J Adv Nurs. 2004;46:641–8.
Greene R, Stratton P, Cleary SD, Ballweg ML, Sinaii N. Diagnostic experience among 4,334 women reporting surgically diagnosed endometriosis. Fertil Steril. 2009;91:32–9.
Hirsh KW, Ladipo OA, Bhal PS, Shaw RW. The management of endometriosis: a survey of patients’ aspirations. J Obstet Gynaecol. 2001;21:500–3.
Huntington A, Gilmour JA. A life shaped by pain: women and endometriosis. J Clin Nurs. 2005;14:1124–32.
Dancet EA, Apers S, Kluivers KB, Kremer JA, Sermeus W, Devriendt C, Nelen WL, D’Hooghe TM. The ENDOCARE questionnaire guides European endometriosis clinics to improve the patient-centeredness of their care. Hum Reprod. 2012;27(11):3168–78.
Klein S, D’Hooghe T, Meuleman C, Dirksen C, Dunselman G, Simoens S. What is the societal burden of endometriosis-associated symptoms? A prospective Belgian study. Reprod Biomed Online. 2014;28(1):116–24.
Simoens S, Dunselman G, Dirksen C, Hummelshoj L, Bokor A, Brandes I, Brodszky V, Canis M, Colombo GL, DeLeire T, Falcone T, Graham B, Halis G, Horne A, Kanj O, Kjer JJ, Kristensen J, Lebovic D, Mueller M, Vigano P, Wullschleger M, D’Hooghe T. The burden of endometriosis: costs and quality of life of women with endometriosis and treated in referral centres. Hum Reprod. 2012;27(5):1292–9.
Kennedy S. What is important to the patient with endometriosis? Br J Clin Pract Suppl. 1991;72:8–10, discussion 11–3.
Moradi M, Parker M, Sneddon A, Lopez V, Ellwood D. Impact of endometriosis on women’s lives: a qualitative study. BMC Womens Health. 2014;14:123.
Brosens I, Gordts S, Benagiano G. Endometriosis in adolescents is a hidden, progressive and severe disease that deserves attention, not just compassion. Hum Reprod. 2013;28(8):2026–31.
Brown J, Farquhar C. Endometriosis: an overview of Cochrane Reviews. Cochrane Database Syst Rev. 2014;(3):CD009590.
Meuleman C, D’Hoore A, Van Cleynenbreugel B, Beks N, D’Hooghe T. Outcome after multidisciplinary CO2 laser laparoscopic excision of deep infiltrating colorectal endometriosis. Reprod Biomed Online. 2009;18(2):282–9.
Meuleman C, Tomassetti C, D’Hoore A, Van Cleynenbreugel B, Penninckx F, Vergote I, D’Hooghe T. Surgical treatment of deeply infiltrating endometriosis with colorectal involvement. Hum Reprod Update. 2011;17(3):311–26.
Nnoaham KE, Hummelshoj L, Webster P, D’Hooghe T, de Cicco Nardone F, de Cicco Nardone C, Jenkinson C, Kennedy SH, Zondervan KT, World Endometriosis Research Foundation Global Study of Women’s Health Consortium. Impact of endometriosis on quality of life and work productivity: a multicenter study across ten countries. Fertil Steril. 2011;96(2):366–373.e8.
Staal AH, van der Zanden M, Nap AW. Diagnostic delay of endometriosis in the Netherlands. Gynecol Obstet Invest. 2016;81(4):321–4.
Culley L, Law C, Hudson N, Denny E, Mitchell H, Baumgarten M, Raine-Fenning N. The social and psychological impact of endometriosis on women’s lives: a critical narrative review. Hum Reprod Update. 2013;19(6):625–39.
Steenberg CK, Tanbo TG, Qvigstad E. Endometriosis in adolescence: predictive markers and management. Acta Obstet Gynecol Scand. 2013;92(5):491.
Geysenbergh B, Dancet EAF, D’Hooghe T. Detecting endometriosis in adolescents: Why not start from self-Report screening questionnaires for adult women? Gynecol Obstet Invest. 2017;82(4):322–28. doi:10.1159/000452098. Epub 2016 Nov 5.
Stratton P. The tangled web of reasons for the delay in diagnosis of endometriosis in women with chronic pelvic pain: will the suffering end? Fertil Steril. 2006;86(5):1302–4; discussion 1317.
Rogers PA, D’Hooghe TM, Fazleabas A, Giudice LC, Montgomery GW, Petraglia F, Taylor RN. Defining future directions for endometriosis research: workshop report from the 2011 world congress of endometriosis in Montpellier, France. Reprod Sci. 2013;20(5):483–99.
Riazi H, Tehranian N, Ziaei S, Mohammadi E, Hajizadeh E, Montazeri A. Patients’ and physicians’ descriptions of occurrence and diagnosis of endometriosis: a qualitative study from Iran. BMC Womens Health. 2014;14:103.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Apers, S., Dancet, E.A.F., D’Hooghe, T. (2017). Endometriosis and Diagnostic Delay: The Patient’s Perspective. In: D'Hooghe, T. (eds) Biomarkers for Endometriosis. Springer, Cham. https://doi.org/10.1007/978-3-319-59856-7_4
Download citation
DOI: https://doi.org/10.1007/978-3-319-59856-7_4
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-59854-3
Online ISBN: 978-3-319-59856-7
eBook Packages: MedicineMedicine (R0)