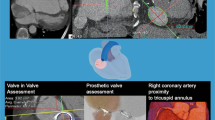
Abstract
Current cardiovascular computed tomography (CT) scanners provide a three-dimensional full volumetric dataset that covers the entire heart and its vascular connections at one or more time points. Cardiovascular CT plays an increasingly important role in the era of transcatheter aortic and mitral valve therapy. Likewise, it has a potential importance in planning of transcatheter tricuspid valve (TV) interventions. Advantages in the CT assessment of the TV include its ability to show a complete overview of the complex anatomy, its submillimetre isotropic spatial resolution and a temporal resolution as low as 66 ms. In addition, CT measurements are generally simple and accurate on good-quality images. It allows for precise anatomic measurements, which is needed for optimal valve sizing and successful valve placement. However, the use of cardiovascular CT has certain limitations. In detail visualization of the right atrioventricular junction can be challenging. It is associated with ionizing radiation, and it has other related risks, especially in dynamic imaging, and with the use of potentially nephrotoxic contrast agents. New TV therapies are evolving, although, evidence for the efficacy and safety is limited to case reports and small series. In this chapter, we will provide an overview of current and potential future applications of CT in the assessment of right heart disease with a focus on perioperative assessment of patients undergoing transcatheter TV therapy.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Tricuspid
- Stenosis
- Regurgitation
- Computed tomography
- Contrast
- Radiation
- Multiplanar reconstruction
- ECG triggering
- Annulus
- Right ventricle
- Annuloplasty
- Preprocedural planning
- Therapy
- Outcome
Imaging Technics of the Tricuspid Valve Using CT
Scan Mode
Computed Tomography has proven itself in imaging of the heart in general and the tricuspid valve (TV) in particular. Dynamic anatomical information can be obtained with CT. But in case of the TV only static anatomical information is sufficient. As the majority of the hospitals today are equipped with at least a 64 slices CT scanner, the following modes can be used:
-
1.
Conventional spiral CT (without ECG gating).
-
2.
Prospective high pitch spiral CT mode (with or without ECG triggering), this technique is only possible with Dual Source CT scanners.
-
3.
Prospective ECG triggering mode.
-
4.
Retrospective ECG gating mode (with or without ECG pulsing).
The first imaging technique is the easiest protocol and is feasible on all scanners, but suffers from motion and/or breathing artefacts. Therefore, this protocol is usually not used to image the TV. With Dual Source CT scanners double temporal resolution and high pitch values can be achieved (P = 3.4) and therefore higher table speed up to 737 mm/s. Motion free heart imaging in less than a single heart beat can be performed with an effective radiation dose less than 1 mSv. This mode has no additional radiation dose penalty compared to the first mode. Using ECG triggered high pitch CT, one can choose which phase of the heart cycle should be imaged, provided that the heart rate is regular. For TV CT imaging the diastolic phase is relevant. The inconvenient of this imaging mode is that it requires a Dual Source CT scanner.
Prospective ECG triggered mode utilizes the step-and-shoot method . The scan is performed by imaging a series of axial images at a selected cardiac phase, usually the diastolic phase. The X-ray tube is turned off during the rest of the cycle. Only wide area detector CT (16 cm) can image the heart in one heartbeat. All other scanners require multiple heart beats which can lead to stack misalignment artefacts. Single source CT scanners have a limited temporal resolution requiring either betta blockers to rule out cardiac motion artefacts or to switch to a more dose intensive retrospective protocol with multi-segment reconstruction. Dual Source scanners have sufficient temporal resolution to use prospective imaging also in high or irregular heart rates. Prospective step and shoot can provide dynamic information by using ECG-padding. With ECG padding the X-ray exposure time per heart beat will be increased or decreased depending on the desired heart phases. More dynamic information achieved by longer X-ray exposure will result in a higher radiation dose. However, in prospective step-and-shoot (SAS) mode will not obtain a full acquisition of the RR-interval. Retrospective ECG-gating exposes X-ray continuously with simultaneous ECG information acquisition. In retrospect, multiple phases of the ECG cycle can be reconstructed providing dynamic information over the full cardiac cycle. This will come at the cost of a significant higher radiation dose. ECG pulsing can be applied to select phases of the cardiac cycle where more noise can be tolerated and tube current and voltage is reduced to decrease the radiation dose. Data for a specific cardiac phase is used for image reconstruction. Retrospective ECG-gating with tube current modulation can allow 30–40% less radiation dose. This decrease in radiation dose is less effective with higher heart rates.
Contrast Injection
A similar approach to CT angiography where contrast is timed in the first pass, scans will suffer from beam hardening artefacts because the contrast agent has not sufficiently been diluted. This is worse when using low kVp. This can be partially solved by injecting a diluted contrast agent. But, although this protocol may decrease beam hardening artefacts, image quality still suffers from mixing artefacts. These are caused by the inflow of contrast free blood from the inferior vena cava (IVC) . Imaging in the venous phase will provide homogeneous contrast agent enhancement. The attenuation will be lower than in the arterial phase. To compensate for this a larger contrast agent volume must be used. A well performed venous phase is sufficient to assess the TV anatomy. As the beam hardening artefacts are solved, a low kVp can help to obtain a higher attenuation with a lower radiation dose.
If a combination with a CT angiogram of the aorta is needed, a split bolus can be used. In this case a first bolus will enhance the IVC inflow and the right heart. While the second bolus will be used to image the left ventricle and the aorta in a single scan.
Clinical Utility of Computed Tomography in Right Heart Diseases
Most cardiac CT examinations are mainly focused on the left side of the heart. Therefore, injection protocols are optimized to visualize this side of the heart. However, the right side of heart (the right atrium, atrioventricular junction and the RV) can also be depicted trough CT [1]. More importantly, it can be of added clinical value to detect and diagnose certain diseases such as arrhythmogenic right ventricular (RV) dysplasia (Fig. 9.1) [2, 3]. In this section we will discuss the clinical utility of CT and the appropriate acquisition techniques to assess the right side of the heart.
Computed Tomography Acquisition Techniques for the Right Side of the Heart
As mentioned before, due to the fact that standard injection techniques are optimized for the left side of the heart, to acquire images of the right side of the heart the injection protocol has to be modified [1]. In order to acquire images of the right side of the heart, adequate contrast quantity has to be maintained in this area. By adjusting the amount of contrast medium and the flow, prolongation of the length of administration of the entire bolus can be achieved [4], and adequate contrast quantity can be maintained on the right side of the heart. To prevent streak artefacts and to achieve clear depiction of the endocardial contour, the multiphasic infusions technique instead of monophasic injection of contrast medium can be used [1]. Furthermore, the use of different combinations of contrast material can contribute to improve the homogeneous enhancement profile. Including saline contrast mixture or saline flush [5].
Different studies have assessed the optimum protocol and modes for the delivery of contrast material [6,7,8,9]. For RV functional analysis, biphasic infusion of contrast medium followed by a contrast saline mixture was found to be optimal, mainly due to the better delineation of the ventricular wall [6]. Furthermore, for the depiction of the right side of the heart, including the valves, split bolus infusion seemed to be the optimal method [7, 9]. For additional imaging of surrounding blood vessels, these injections parameters have to be adjusted, in order to have the optimal enhancement profile.
Clinical Utility of Cardiac CT
Although, MRI is the most accurate in assessing RV volumes and function [10], CT can be used to assess a variety of cardiopulmonary conditions and detect important prognostic markers [1]. Table 9.1 lists cardiac diseases in which the assessment of RV function is highly important. In patients with an acute pulmonary embolism (Fig. 9.2) the RV/Left ventricle (LV) diameter ratio is associated with higher mortality rates [11]. In addition, RV/LV diameter ratio score greater than 1.5, estimated through CT, indicates severe RV dysfunction [3]. Furthermore, both right- and left sided valvular diseases can lead to RV dysfunction [1]. However, TV regurgitation (TR) can also occur because of RV dysfunction and subsequent annular dilatation [12]. CT can provide an anatomical delineation of the right atrioventricular junction and the RV outflow tract, in order to depict dilation or enlargements. Finally, CT can be used to rapidly asses the RV function and ejection fraction in acute settings such as RV infarction, and in chronic diseases such as heart failure [1].
Computed Tomography in a patient with acute pulmonary embolism. (a) Four-chamber view reconstruction with septal flattening (arrows). (b) Grade 4 reflux of contrast into the inferior vena cava (long arrow) and proximal hepatic veins (short arrows). (c) The maximal diameter on axial sections of (c) right and (d) left ventricular diameter. (e) The maximal diameter on four-chamber view of the right and (f) left ventricle. Right and left ventricle volumetric depicted on (g) axial section and (h) sagittal reformation. Reprinted with permission from “CT Signs of Right Ventricular Dysfunction: Prognostic Role in Acute Pulmonary Embolism” by Doo Kyoung Kang et al., JACC Cardiovasc Imaging 2011; Volume 4:8:841–849. Copyright (2017) by Elsevier Inc.
Comprehensive Assessment of Tricuspid Valve and Surrounding Structures by CT
Advanced TV disease such as severe TR is associated with increased morbidity and mortality [14, 15]. TR might not be recognized clinically until fairly late in its natural history. Early stages of TR are therefore often asymptomatic and are often observed on echocardiography. Transthoracic echocardiography (TTE) is most often used to diagnose and to assess the cause and the severity of TR. When TTE images are inadequate, transoesophageal echocardiography (TEE) can be considered, although visualization of the anteriorly located TV can be difficult [16].
In advance of TV interventions, a detailed knowledge of the complex surgical anatomy of the TV is fundamental. The information gained through imaging may help to plan and guide surgical decision-making and transcatheter TV interventions. Different imaging techniques have been used for the assessment of the TV and the surrounding structures. However, due to the complex anatomy of TV apparatus a 3D imaging modality is often needed. Cardiac magnetic resonance (CMR) imaging and real-time three-dimensional techniques can provide 3D information as well as accurate quantification of TR severity [10, 17,18,19]. However, CMR is not widely available and often contraindicated due to the presence of pacemaker leads. On the other hand, 3D echocardiography suffers often a low spatial and temporal resolution. CT on the other hand has acquired an increasing importance in planning transcatheter interventions because of its accurate 3D information as well as high spatial and temporal resolution. CT can be used therefore to assess TV and the surrounding structures such as the RV and adjacent blood vessels [20, 21]. In this section we discuss the assessment of the TV and the surrounding structures with CT and the clinical utility of CT in preplanning for TR interventions.
The Tricuspid Valve
The most common abnormality of TV is TR, which is often due to incomplete leaflet coaptation or incomplete closure due to dilated annulus and dilated RV. Increasing TR severity is associated with poor survival [22]. Therapeutic decisions for TR often require 3D imaging modality to unravel its mechanism [14].
The normal tricuspid apparatus (Fig. 9.3) has been described previously in Chap. 1. In brief, the TV apparatus consist of three leaflets, a partly fibrous annulus, and a supporting tension apparatus. The supporting tension apparatus consist of the chordae tendinae and papillary muscles . The leaflets include anterior, septal and posterior [23, 24]. The PMs include anterior, inferior and medial. The commissure between the septal and anterior leaflets is located over the membranous septum and divides it into the atrioventricular and inter-ventricular components [24, 25]. The chordae to the anterior and septal leaflets, provided by the medial PM of the conus or RV septal wall, represents an important surgical landmark for the location of the right bundle branch [20].
Normal appearance of tricuspid valve . (a) Four-chamber CT image shows the septal (S) and anterior (A) leaflets. (b) Two-chamber CT image shows septal (S) and posterior (P) leaflets. (c) Short-axis CT image shows all the leaflets (S, A, P). (d) MRI appearance of the tricuspid annulus, with the short-axis steady-state free precession (SSFP) image showing all the leaflets (S, A, P). Reprinted with permission from Shah et al. [26] Insights Imaging. 2016 Oct;7(5):649–67
Tricuspid Annulus
The normal tricuspid annulus is an ellipsoid, non-symmetrical, saddle-shaped structure and appears nonplanar, with the posteroseptal part the most towards the RV apex. It becomes more circular as it dilates in an anterior-posterior direction in response to RV enlargement (Fig. 9.4) [14]. Among other reasons, the TV annulus differs from the mitral annulus because of the lack of extensive fibrous elements in the peripheral (mural) part of the valve to support its leaflets [25]. Measurements of TV annulus on CT can be performed in the four-chamber views by measuring maximum and minimum diameters.
Measurements of the tricuspid valve annual diameter. Presented are the measurements of the (a) maximum and (b) minimum tricuspid valve annual diameter on electrocardiogram gated 320-slice computed tomography. Reprinted with permission from “Relationship of maximum and minimum tricuspid valve annular diameter determined by 320-slice computed tomography with right atrial and ventricular volume and estimated right ventricular systolic pressure” by Nobusada Funabashi et al., IJC 2013;168(4):4578–81. Copyright (2017) by Elsevier Inc
CT Assessment of the Tricuspid Valve and Adjacent Anatomical Structures
In detail visualization of the right atrioventricular junction can be challenging. Clear depiction of this region requires homogenous enhancement of the structures around the TV annulus. ECG gated or triggered cardiac CT angiography (CTA) techniques can provide good-quality motion-free images of the RV outlet and trabeculated portions [20]. However, the quality may not be high enough to show the details of the RV inlet [27], partially because of streaming artefacts.
Advantages
Advantages of CT use in the assessment of the TV includes, its ability to show the extent of calcification, a complete overview of the complex anatomy, good spatial and temporal resolution, it enables evaluation of the TV annuloplasty ring dislodgement, it helps to identify inappropriate positioning of the RV pacemaker lead at the TV level, and, measurements are generally simple on good-quality four-chamber cardiac CT images [20, 21]. Moreover, CT can evaluate associated extra-cardiac lesions, for example in carcinoid heart disease. Advantages and limitations are summarized in Table 9.2.
Limitations
The use of CT has certain limitations. It is associated with ionizing radiation, its related risks and with use of potentially nephrotoxic contrast agents [26]. Furthermore, dynamic evaluation or ventricular functional evaluation is possible in retrospective ECG-gated scans. However, this is associated with a higher radiation dose [26]. The use of CT is limited in patients with high or irregular heart rates and also in the characterization of tissues [26]. Finally, CT has limited value in the assessment of the valve function or for the detection of small vegetation’s (<4 mm) and small valve perforations. [26, 28].
The CT is technically limited in showing all TV leaflet positions at a specific time frame of the cardiac cycle in one short-axis plane, therefore, when assessing TV leaflets, a combination of different views is required. The four-chamber view is the most appropriate view to assess the septal leaflet, and in some cases, only in this projection small defects of the membranous septum can be seen [20]. Furthermore, the septal isthmus width, visualization of its relation with the coronary sinus orifice and the atrioventricular node artery can be measured with the four-chamber view [20]. The relationship of the anterior and posterior leaflets can be depicted with the two-chamber CT of the right heart, and, this is the optimum view to measure the cavotricuspid isthmus superior to the hinge of posterior TV leaflet, which might be difficult to visualize trough TTE. The long-axis views can be used for the evaluation of TV prolapse. Furthermore, when there is tethering of the leaflets and regurgitation due to incomplete coaptation of the leaflets, the distance and area of tethering (tenting) can be measured by CT. The dimensions of the TV annulus can be measured through the reconstructed short-axis view, by measuring the maximal antero-posterior and septal-lateral diameter of the annulus [21]. The perimeter and annulus area can be assessed by planimetery after the CT is performed [21].
The Right Coronary Artery
The distance of the right coronary artery (RCA) to the TV annulus and the course of the RCA through the right atrioventricular groove may vary in humans [29]. Information regarding the course of the RCA may be of added value when planning patients for transcatheter interventions that target the TV annulus, due to the risk for impingement of the RCA [30]. CT analysis can be used to determine detailed characterization of the spatial relationship between the RCA and the TV annulus (Fig. 9.5). The mid-diastolic phase volume rendered reconstructions, the two- and four-chamber long-axis and the short-axis views can be evaluated to determine the course and position of the RCA relative to the TV annulus [31]. The position of the RCA relative to the TV annulus can be classified as superior, inferior or at the same level as the TV annulus. The short-axis view can be used to measure the distance between the RCA and the TV annulus at the level of the anterior and posterior tricuspid leaflets insertions, if the RCA courses at the same level as TV annulus [31].
The Right Ventricular Apex
Certain devices, like the Forma Repair System (Edwards Lifesciences, Irvine, California) interact directly with the tricuspid leaflets. Therefore, the TV annulus dimensions and the distance from the annulus to the RV apex should be evaluated, when planning patients for these interventions [32]. To measure the maximal distance between the TV annulus and the RV apex, the long-axis four-chamber view can be used [31].
The Vena Cava
Patients selected for transcatheter caval valve implantations (CAVI) require pre-CAVI imaging with contrast-enhanced, electrocardiogram-gated CTA to assess the IVC dimensions and the distance between the junction of the right atrium and IVC to the first hepatic vein (Fig. 9.6) [33].
Computed Tomography for Caval Valve Implantation. (a) Assessment of the right atrium-inferior vena cava junction plane. (b, c) Depiction of the hepatic vein and (d) Sequential measurements of the horizontal planes for the assessment of the optimal valve size (1 cm below the right atrium-inferior vena cava junction plane and 1 cm above the identified first hepatic vein). Reprinted with permission from “Transcatheter Caval Valve Implantation Using Multimodality Imaging. Roles of TEE, CT, and 3D Printing,” by Brian O’Neill et al., JIMG 2015;8:221–225. Copyright (2015) by Elsevier Inc
The axial view with the multi-planar reformation planes oriented along the RV apex and the coronary sinus can be used to assess the dimensions of the IVC at the transition level with the right atrium down to the level of the first hepatic vein [31, 33]. To reconstruct the double oblique transverse plane parallel to the transition level of the right atrium with the IVC, single oblique and coronal views can be used while aligning the multi-planar reformation planes to the basal part of the coronary sinus [33]. Furthermore, the diameter, perimeter and area of the IVC can be assessed at this level [31]. To assess the dimensions of the IVC at the first hepatic vein, these measurements can be repeated on the double oblique transverse plane at the level of the first hepatic vein (Fig. 9.7) [31].
Vena Cava dimensions assessed through computed tomography. Computed tomography assessment of the inferior vena cava (IVC) dimensions using the Orthogonal axial view (a), single oblique sagittal view (b, f) and the Coronal view (c, g). In order to reconstruct a transverse plane of the entrance of the IVC into the right atrium (d), multi-planar reformation planes were aligned along the transition of right atrium and IVC. Panel (e) depicts the distance between the first hepatic vein and the IVC. The maximal and minimal diameter, perimeter and area of the IVC are measured in h, using a double oblique transverse plane
Surgical Interventions for the Tricuspid Valve
Functional TR is the most common abnormality of TV. When indicated, surgical repair or replacement of the TV is the only currently approved treatment option. There are two surgical options for the TV, it can be either repaired or replaced. In symptomatic patients or patients with sings of RV remodelling and primary TR, surgery is recommended. Furthermore, it is recommended in patients undergoing surgery for the left sided valves with concomitant functional TR. The preference for one of these two techniques depends on the underlying cause of the TV disease. In patients with damaged leaflets due to rheumatic or carcinoid valve disease, as in patients with extreme annulus dilatation, valve replacement is favoured [34]. However, patients require chronic anticoagulation after valve replacement, and in addition, valve replacement is associated with an increased mortality [35]. Therefore, the preferred option is valve repair (Fig. 9.8), which consists of several techniques. Incomplete band or De Vega’s suture annuloplasty and Kay bicuspidization are the most frequently used techniques in patients undergoing left sided valve surgery to treat functional TR [36]. A suture repair has the advantage that it can be performed easily and quickly. However, due to the higher incidence of recurrent TR after suture repair compared to the use of an annuloplasty band, the latter one is more favoured. Detailed surgical TV repair and replacement techniques are presented in Chap. 17.
Tricuspid annuloplasty repair techniques (a) Tricuspid valve before surgical intervention, (b) Kay bicuspidization repair, (c) De Vega suture repair and (d) ring annuloplasty with use of an incomplete semirigid prosthetic ring. Reprinted with permission from “Diagnosis and treatment of tricuspid valve disease: current and future perspectives,” by Josep Rodés-Cabau et al., The Lancet 388(10058), Pages 2431–2442 (November 2016) Copyright (2016) by Elsevier Inc
Clinical Utility of CT in Planning Transcatheter Interventions for Functional TR
Transcatheter TV therapy is a less invasive alternative to surgery for patients with functional TR and deemed to be high-risk surgical candidates [37]. Currently, transcatheter devices are designed to target TR via one or more of TV apparatus components such as TV annulus, TV leaflets or caval veins. Annuloplasty devices such as TriAlign and the TriCinch System aim at reduction or modulation of TV annulus. Coaptation devices such as the Spacer aims at improving TV leaflets coaptation. Heterotopic caval vein implantation aims at secure a functioning valve(s) between right atrium and venous communication. Details of these devices and technical considerations are provided in other chapters of this book.
To minimize the risk for complications and to optimize the results, specific anatomical aspects should be taken into consideration before performing one of the currently available transcatheter procedures for the TV. In contrast to echocardiography, CT can provide better information on the anatomical spatial relationship of the TV apparatus and surrounding structures [31] Table 9.3. Lists key anatomic measurements, which are required for pre-procedural planning of transcatheter TV repair or replacement.
Percutaneous Tricuspid Annuloplasty
The Mitralign device (Mitralign, Inc. Tewksbury, USA), has been used to treat functional TR performing a transcatheter bicuspidization of the TV [38]. The TriCinch device (4Tech Cardio, Galway, Ireland) is a catheter-based device designed to perform tricuspid annular cinching [39], in order to reduce anteroseptal annular dimension and reduce TR improving leaflet coaptation. In the latter procedure, the tricuspid annulus dimensions are reduced by positioning of a corkscrew anchor at the anterior tricuspid leaflet that is connected through a Dacron band to a self-expandable stent implanted in the inferior vena cava. [40]. A schematic view of the percutaneous interventions for the treatment of tricuspid regurgitation is presented in Fig. 9.9. Continuous monitoring with TEE and demarcation of the right coronary artery (RCA) course with wires and angiography are needed to safely perform the intervention with the Mitralgn device. In addition, before performing the annulus reduction with the TrinCinch device , the distance from the insertion of the anterior tricuspid leaflet into the annulus to the RCA should be studied (Fig. 9.10) [31]. One of the most feared complications in these procedures is impingement of the RCA. Even in normal human hearts the distance between the TV annulus and the RCA is variable. [29] According to an anatomical study by Ueda et al., [33] the median nearest distance from the RCA to the base of the anterior tricuspid leaflet was 6.8 mm [range 5.9–11.0 mm] and to the posterior tricuspid leaflet 2.1 mm [range 2.0–4.0 mm] in normal human hearts. However, the distance between the RCA and the TV measured with CT was larger at the insertion level of the anterior tricuspid leaflet whereas the RCA coursed more closely to the annulus at the level of the insertion of the posterior leaflet , in a study including patients with and without significant TR. [31] Furthermore, a less favourable course of the RCA (≤2.0 mm distance to the annulus) was depicted through CT analysis in 12.5% of the patients with TR ≥ 3+ at the anterior tricuspid leaflet and in 27.5% of the patients with TR ≥ 3+ at the posterior tricuspid leaflet [39] Therefore, evaluation of the RCA course through CT analysis can be of value in patients with severe TR, awaiting percutaneous tricuspid annuloplasty.
Transcatheter therapies for tricuspid regurgitation. Transcatheter options, heterotopic caval valve implantation, coaptation devices, annuloplasty devices. Reprinted with permission from “Transcatheter Therapies for Treating Tricuspid Regurgitation” by Josep Rodés-Cabau et al., J Am Coll Cardiol 2015 volume 67:15:1829–1845. Copyright (2017) by Elsevier Inc
Distance between RCA and TV annulus. Computed tomography assessment of the distance between the right coronary artery and the tricupid valve annulus. Panel (a), long-axis two-chamber view and (b), long-axis four-chamber view. The (c) short-axis view was reconstructed using the long-axis views of (a) and (b). A 3D reconstruction spatial relationship between the RCA and the TV annulus is depicted in panel D
Tricuspid Orifice
CT assessment of the orientation of the TV annulus plane relative to the RV apex may be of value in pre-procedural planning of patients for devices that interfere or are placed within the TV orifice , like the Forma Repair System [31, 32]. This is an inflatable spacer device that is positioned within the regurgitant orifice area of the TV and provides a surface for native leaflet coaptation [32]. Trough a rail, the inflatable spacer is attached to the RV apex. In order to reduce the TR grade effectively, the spacer needs to be positioned in the center of the regurgitant orifice area perpidencular to the valve plane [32], which is currently assisted by three-dimensional TEE. The implanting cardiologist could benefit from geometrical information of the TV annulus plane orientation and distance relative to the RV apex, assessed through CT (Fig. 9.11), to the benefit of catheter manoeuvring during the procedure [31].
Caval Valve Implantation Concept
Knowledge regarding the use of CT in the assessment of the right atriocaval junction, the vena cava and the distance to the first hepatic vein for prosthesis sizing and the avoidance of hepatic vein obstruction during CAVI remains limited. A small number of studies have reported about the success of this procedure [33]. The mean cross-sectional area of the right atriocaval junction and the distance from this point to the first hepatic vein can be assessed with the CT in patients with severe TR (Fig. 9.7) [31]. This study also discusses that the design of customized caval valve prosthesis fitted to the vena cava geometry of the patient assessed by CT may provide the most favourable results. The intraoperative TEE and post-CAVI CT are depicted in Fig. 9.12.
Periprocedural multimodality imaging: role of intraoperative TEE and post-CAVI CT. Intraprocedural TEE (a) at the level of the coronary sinus, (b) visualization of the mouth of the inferior vena cava. (c, d) 5 days post-procedure CT illustrating opening and closure of the SAPIEN XT valve (Edwards Lifesciences, Irvine, California) and (e) three-dimensional volumetric CT reconstruction of the SAPIEN XT valve within the Cook stent (Cook Medical, Bloomington, Indiana). TEE transesophageal echocardiography, CAVI caval valve implantation, CT Computed Tomography. Reprinted with permission from “Transcatheter Caval Valve Implantation Using Multimodality Imaging. Roles of TEE, CT, and 3D Printing,” by Brian O’Neill et al., JIMG 2015;8:221–225. Copyright (2015) by Elsevier Inc
Conclusion
CT scan plays an important role in the assessment of right heart disease. Moreover, CT role has been increasingly used in preinterventional percutaneous valve therapy. Assessment of patients with CT before percutaneous transcatheter tricuspid valve intervention could be of great value for implanting cardiologists, especially in locating the right coronary artery. New tricuspid valve therapies are evolving, although, evidence for the efficacy and safety is limited to case reports and small series. CT enables acquisition of high quality images of the tricuspid valve and the complex anatomical structures around it. Furthermore, CT provides important insights into the geometrical dimensions of the tricuspid valve and adjacent veins. These insights may help to guide the interventional cardiologists in the decision-making process and to prepare for the tricuspid valve intervention.
Appendix
Summary of MSCT planning of transcatheter tricuspid valve repair or replacement.
Due to increased attention and recognition of the need for TV repair or replacement, MSCT preplanning has gained more attention of analysis software developers. MSCT assists in patient selection, provides insight in anatomy and can serve as a roadmap to guide transcatheter valvular interventions. From single or multiphase CT scans e.g. the annulus shape and dimensions, relationship between annulus and right coronary artery position and location of right ventricular papillary muscles. Additionally, percutaneous access routes can be evaluated such as the vena cava inferior and jugular access. All information can be visualized as a virtual angiogram providing an essential link between the MSCT scan and the actual implantation procedure under X-ray. Currently dedicated MSCT planning software is being developed such as 3mensio Structural Heart.
The following figures (9.13–9.18) summerize a MSCT scan analysis using 3mensio Structural Heart.
Virtual angiogram showing tricuspid annulus, right coronary artery centerline (purple) and vena cava superior (green) and inferior centerlines (blue) (3mensio Structural Heart). The virtual angiogram shows what the operator can expect during the angiography guided procedure and shows optimal implantation views (bottom S-curve) on tricuspid annulus (e.g. co-axial, en-face), right ventricle and vena cava
References
Gopalan D. Right heart on multidetector CT. Br J Radiol. 2011;84(3):S306–23.
Schoepf UJ, Kucher N, Kipfmueller F, Quiroz R, Costello P, Goldhaber SZ. Right ventricular enlargement on chest computed tomography: a predictor of early death in acute pulmonary embolism. Circulation. 2004;110(20):3276–80.
Quiroz R, Kucher N, Schoepf UJ, Kipfmueller F, Solomon SD, Costello P, et al. Right ventricular enlargement on chest computed tomography: prognostic role in acute pulmonary embolism. Circulation. 2004;109(20):2401–4.
Johnson TR, Nikolaou K, Wintersperger BJ, Knez A, Boekstegers P, Reiser MF, et al. ECG-gated 64-MDCT angiography in the differential diagnosis of acute chest pain. AJR Am J Roentgenol. 2007;188(1):76–82.
Setty BN, Sahani DV, Ouellette-Piazzo K, Hahn PF, Shepard JA. Comparison of enhancement, image quality, cost, and adverse reactions using 2 different contrast medium concentrations for routine chest CT on 16-slice MDCT. J Comput Assist Tomogr. 2006;30(5):818–22.
Utsunomiya D, Awai K, Sakamoto T, Nishiharu T, Urata J, Taniguchi A, et al. Cardiac 16-MDCT for anatomic and functional analysis: assessment of a biphasic contrast injection protocol. AJR Am J Roentgenol. 2006;187(3):638–44.
Kerl JM, Ravenel JG, Nguyen SA, Suranyi P, Thilo C, Costello P, et al. Right heart: split-bolus injection of diluted contrast medium for visualization at coronary CT angiography. Radiology. 2008;247(2):356–64.
Cao L, Du X, Li P, Liu Y, Li K. Multiphase contrast-saline mixture injection with dual-flow in 64-row MDCT coronary CTA. Eur J Radiol. 2009;69(3):496–9.
Lu JG, Lv B, Chen XB, Tang X, Jiang SL, Dai RP. What is the best contrast injection protocol for 64-row multi-detector cardiac computed tomography? Eur J Radiol. 2010;75(2):159–65.
Sugeng L, Mor-Avi V, Weinert L, Niel J, Ebner C, Steringer-Mascherbauer R, et al. Multimodality comparison of quantitative volumetric analysis of the right ventricle. JACC Cardiovasc Imaging. 2010;3(1):10–8.
Ghaye B, Ghuysen A, Bruyere PJ, D’Orio V, Dondelinger RF. Can CT pulmonary angiography allow assessment of severity and prognosis in patients presenting with pulmonary embolism? What the radiologist needs to know. Radiographics. 2006;26(1):23–39. discussion-40
Dreyfus GD, Corbi PJ, Chan KM, Bahrami T. Secondary tricuspid regurgitation or dilatation: which should be the criteria for surgical repair? Ann Thorac Surg. 2005;79(1):127–32.
Kimura F, Sakai F, Sakomura Y, Fujimura M, Ueno E, Matsuda N, et al. Helical CT features of arrhythmogenic right ventricular cardiomyopathy. Radiographics. 2002;22(5):1111–24.
Fukuda S, Saracino G, Matsumura Y, Daimon M, Tran H, Greenberg NL, et al. Three-dimensional geometry of the tricuspid annulus in healthy subjects and in patients with functional tricuspid regurgitation: a real-time, 3-dimensional echocardiographic study. Circulation. 2006;114(1 Suppl):I492–8.
Shah PM, Raney AA. Tricuspid valve disease. Curr Probl Cardiol. 2008;33(2):47–84.
Rodes-Cabau J, Taramasso M, O'Gara PT. Diagnosis and treatment of tricuspid valve disease: current and future perspectives. Lancet. 2016;388(10058):2431–42.
Nesser HJ, Tkalec W, Patel AR, Masani ND, Niel J, Markt B, et al. Quantitation of right ventricular volumes and ejection fraction by three-dimensional echocardiography in patients: comparison with magnetic resonance imaging and radionuclide ventriculography. Echocardiography. 2006;23(8):666–80.
Anwar AM, Soliman OI, Nemes A, van Geuns RJ, Geleijnse ML, Ten Cate FJ. Value of assessment of tricuspid annulus: real-time three-dimensional echocardiography and magnetic resonance imaging. Int J Cardiovasc Imaging. 2007;23(6):701–5.
van der Zwaan HB, Geleijnse ML, McGhie JS, Boersma E, Helbing WA, Meijboom FJ, et al. Right ventricular quantification in clinical practice: two-dimensional vs. three-dimensional echocardiography compared with cardiac magnetic resonance imaging. Eur J Echocardiogr. 2011;12(9):656–64.
Saremi F, Hassani C, Millan-Nunez V, Sanchez-Quintana D. Imaging evaluation of tricuspid valve: analysis of morphology and function with CT and MRI. AJR Am J Roentgenol. 2015;204(5):W531–42.
van Rosendael PJ, Joyce E, Katsanos S, Debonnaire P, Kamperidis V, van der Kley F, et al. Tricuspid valve remodelling in functional tricuspid regurgitation: multidetector row computed tomography insights. Eur Heart J Cardiovasc Imaging. 2016;17(1):96–105.
Nath J, Foster E, Heidenreich PA. Impact of tricuspid regurgitation on long-term survival. J Am Coll Cardiol. 2004;43(3):405–9.
Virmani R. The tricuspid valve. Mayo Clin Proc. 1988;63(9):943–6.
Anderson RH, Ho SY, Becker AE. Anatomy of the human atrioventricular junctions revisited. Anat Rec. 2000;260(1):81–91.
Restivo A, Smith A, Wilkinson JL, Anderson RH. Normal variations in the relationship of the tricuspid valve to the membranous septum in the human heart. Anat Rec. 1990;226(2):258–63.
Shah S, Jenkins T, Markowitz A, Gilkeson R, Rajiah P. Multimodal imaging of the tricuspid valve: normal appearance and pathological entities. Insights Imaging. 2016;7(5):649–67.
Saremi F, Ho SY, Cabrera JA, Sanchez-Quintana D. Right ventricular outflow tract imaging with CT and MRI: part 1, morphology. Am J Roentgenol. 2013;200(1):W39–50.
Feuchtner GM, Stolzmann P, Dichtl W, Schertler T, Bonatti J, Scheffel H, et al. Multislice computed tomography in infective endocarditis: comparison with transesophageal echocardiography and intraoperative findings. J Am Coll Cardiol. 2009;53(5):436–44.
Ueda A, McCarthy KP, Sanchez-Quintana D, Ho SY. Right atrial appendage and vestibule: further anatomical insights with implications for invasive electrophysiology. Europace. 2013;15(5):728–34.
Diez-Villanueva P, Gutierrez-Ibanes E, Cuerpo-Caballero GP, Sanz-Ruiz R, Abeytua M, Soriano J, et al. Direct injury to right coronary artery in patients undergoing tricuspid annuloplasty. Ann Thorac Surg. 2014;97(4):1300–5.
van Rosendael PJ, Kamperidis V, Kong WK, van Rosendael AR, van der Kley F, Ajmone Marsan N, et al. Computed tomography for planning transcatheter tricuspid valve therapy. Eur Heart J. 2017;38(9):665–74.
Campelo-Parada F, Perlman G, Philippon F, Ye J, Thompson C, Bedard E, et al. First-in-man experience of a novel transcatheter repair system for treating severe tricuspid regurgitation. J Am Coll Cardiol. 2015;66(22):2475–83.
O’Neill B, Wang DD, Pantelic M, Song T, Guerrero M, Greenbaum A, et al. Transcatheter caval valve implantation using multimodality imaging: roles of TEE, CT, and 3D printing. JACC Cardiovasc Imaging. 2015;8(2):221–5.
Shinn SH, Schaff HV. Evidence-based surgical management of acquired tricuspid valve disease. Nat Rev Cardiol. 2013;10(4):190–203.
Vassileva CM, Shabosky J, Boley T, Markwell S, Hazelrigg S. Tricuspid valve surgery: the past 10 years from the Nationwide Inpatient Sample (NIS) database. J Thorac Cardiovasc Surg. 2012;143(5):1043–9.
Fender EA, Nishimura RA, Holmes DR. Percutaneous therapies for tricuspid regurgitation. Expert Rev Med Devices. 2017;14(1):37–48.
Agarwal S, Tuzcu EM, Rodriguez ER, Tan CD, Rodriguez LL, Kapadia SR. Interventional cardiology perspective of functional tricuspid regurgitation. Circ Cardiovasc Interv. 2009;2(6):565–73.
Schofer J, Bijuklic K, Tiburtius C, Hansen L, Groothuis A, Hahn RT. First-in-human transcatheter tricuspid valve repair in a patient with severely regurgitant tricuspid valve. J Am Coll Cardiol. 2015;65(12):1190–5.
Latib A, Agricola E, Pozzoli A, Denti P, Taramasso M, Spagnolo P, et al. First-in-man implantation of a tricuspid annular remodeling device for functional tricuspid regurgitation. JACC Cardiovasc Interv. 2015;8(13):e211–4.
Taramasso M, Pozzoli A, Guidotti A, Nietlispach F, Inderbitzin DT, Benussi S, et al. Percutaneous tricuspid valve therapies: the new frontier. Eur Heart J. 2017;38(9):639–47.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Review Questions
Review Questions
Select the Single Best Sentence
-
51.
Which of the following is the best imaging modality for the assessment of tricuspid valve leaflets?
-
(a)
Cardiac MRI
-
(b)
Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
52.
Which of the following is the best imaging modality for the assessment of tricuspid valve annulus?
-
(a)
Cardiac MRI
-
(b)
2D Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
53.
Which of the following is the best imaging modality for the assessment of tricuspid valve vegetation and masses?
-
(a)
Cardiac MRI
-
(b)
Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
54.
Which of the following is the best imaging modality for the assessment of right heart size?
-
(a)
Cardiac MRI
-
(b)
Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
55.
Which of the following is the best imaging modality for the assessment of tricuspid valve regurgitation?
-
(a)
Cardiac MRI
-
(b)
Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
56.
Which of the following is the best imaging modality for intraprocedural guidance of tricuspid valve interventions?
-
(a)
Cardiac MRI
-
(b)
Transoesophageal Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
-
57.
Which of the following is the best imaging modality for the serial assessment of outcome of tricuspid valve interventions?
-
(a)
Cardiac MRI
-
(b)
Echocardiography
-
(c)
Cardiovascular Computed Tomography
-
(d)
Angiography
-
(a)
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Muslem, R., Ouhlous, M., Akin, S., Fares, A.A., Soliman, O.I. (2018). Tricuspid Valve Disease: A Computed Tomographic Assessment. In: Soliman, O.I., ten Cate, F.J. (eds) Practical Manual of Tricuspid Valve Diseases. Springer, Cham. https://doi.org/10.1007/978-3-319-58229-0_9
Download citation
DOI: https://doi.org/10.1007/978-3-319-58229-0_9
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-58228-3
Online ISBN: 978-3-319-58229-0
eBook Packages: MedicineMedicine (R0)