Abstract
The field of heart regeneration has witnessed significant advancements toward developing new therapeutics in the past decade. Strategies to regenerate the adult human heart are in constant development in both the experimental and clinical arenas. Although stem cell therapies remain controversial, cell-based heart repair is a promising approach toward regenerating the adult human heart. Experience with cell therapy has resulted in several important milestones in clinical studies. There are still important roadblocks ahead before cell therapy can achieve the regeneration potential for broad numbers of patients. In this chapter, we focus on the history of cardiac cell repair and therapeutic strategies and discuss the lessons learned in cell-based heart regeneration.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
1.1 Introduction
Cardiovascular diseases remain to be one of the leading causes of mortality worldwide and represent an enormous health and economic burden (Whelan et al. 2010). Identifying strategies to regenerate the adult human heart after injury has spurred a furiously paced experimental race toward this goal.
Historically, the mammalian heart has been considered to be a postmitotic organ, without any capacity for cell turnover and regeneration post-injury (Laflamme and Murry 2011). Instead of regenerating muscle, a scar is formed to maintain the integrity of the mammalian heart following injury; hypertrophy of the remaining myocardium takes place, but the loss of myocardium can eventually lead to the development of heart failure (Jessup and Brozena 2003). Mechanical approaches for treatment of heart failure aimed to counteract the weakening of the heart muscle following injury include left ventricular assist devices (Terracciano et al. 2010). Other approaches include neurohormonal inhibition, which is widely used in clinical practice (Sharpe et al. 1991). These approaches are beneficial for patients with heart failure, but the potential to completely regenerate lost myocardium remains an important goal.
Early discoveries showed that endogenous cardiac regeneration can occur in some vertebrate organisms such as the newt and zebrafish (Oberpriller and Oberpriller 1974; Poss et al. 2002). Recently, the neonatal mouse heart was reported to regenerate in response to injury in a manner similar to lower vertebrates (Porrello et al. 2011, 2013). The regenerative response has been attributed to the ability of cardiomyocytes to proliferate with restoration of functional myocardium (Jopling et al. 2010; Kikuchi et al. 2010; Porrello et al. 2011). Cardiomyocyte cell cycle activity is maintained throughout the adult life of vertebrates, but rapidly declines with age in mammals (Li et al. 1996; Poss et al. 2002; Walsh et al. 2010). The lessons learned from lower vertebrates as well as the neonatal mouse suggest that endogenous heart regeneration can occur, and understanding this process could allow new therapeutic approaches to regenerate the human heart.
Early mouse studies showed that cardiomyocyte turnover in the adult murine heart occurs at low levels, around 1% annually (Soonpaa and Field 1997). Cardiomyocyte turnover in the adult mouse heart during aging and following injury was demonstrated at high resolution using mouse genetic lineage tracing and multi-imaging mass spectrometry showing similar levels of myocyte turnover (Senyo et al. 2013; Hsieh et al. 2007). To measure the levels of cell turnover in the adult human heart, a landmark study exploited the rise of 14C levels during the cold war testing of nuclear weapons, which created an opportunity to trace the levels of 14C from human heart samples and thus enabled the researchers to determine the rate of cardiomyocyte turnover in the adult human heart (Bergmann et al. 2009). Similar to the murine heart, the adult human heart showed cardiomyocyte turnover at extremely low levels, around 1% annually (Bergmann et al. 2009). Although the cardiomyocyte refreshment is insufficient for a substantial regenerative response following injury, this indicates that the heart is much more resilient than previously considered. Surprisingly, a recent study reported that the human neonatal heart can regenerate after a myocardial infarction (Haubner et al. 2015). The similarities between the neonatal mouse and neonatal human heart, as well as the adult mouse and adult human heart, suggest that regenerating the adult heart will be feasible.
1.2 Cell Therapy for Cardiac Repair
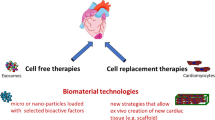
The development of many tools in regenerative medicine has inspired cardiovascular investigators to utilize these methods to regenerate the human heart to restore contractile function following injury. Stem cells have generated particular excitement for their potential for cell-based cardiac repair (Garbern and Lee 2013). The plasticity of stem cells and their ability to differentiate into multiple cell types has generated hope for the future of regenerative medicine. The past decade has witnessed numerous studies that used different cell types with varying abilities for cardiac repair, which led to many clinical trials. The results from these trials continue to generate controversy regarding the impact of cellular therapy, but it is clear that cell therapy may have an important future for human heart regeneration.
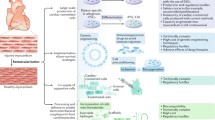
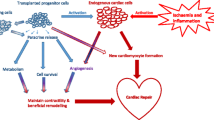
The collective knowledge of cellular plasticity in the mammalian heart as well as the explosion of the stem cell field fueled the hope to either harness the endogenous potential of the mammalian heart or utilize the potential of exogenous stem cells that can differentiate into functional myocardium. In the following paragraphs, we will discuss the utility of different types of exogenous stem cells, as well as the potential of different endogenous cardiac progenitors for cellular transplantation, in addition to cellular reprogramming, to regenerate the adult human heart.
1.2.1 Skeletal Myoblasts
Skeletal myoblasts were among the initial cell types to be introduced for clinical cardiac cell therapy. Skeletal myoblasts were reasonable candidates due to their resistance to ischemia, as well as their differentiation potential (Durrani et al. 2010). In addition, early results showed the promise of skeletal myoblasts in heart repair following injury in multiple experimental animal models (Durrani et al. 2010). However, it was shown that myoblasts fail to integrate with the host myocardium and thus fail to beat in sync with the heart (Leobon et al. 2003). Furthermore, the first multicenter, randomized, placebo-controlled human clinical trial for myoblast autologous grafting in ischemic cardiomyopathy (MAGIC) did not enhance cardiac contractile function (Menasche et al. 2008). These results led to a reduced enthusiasm toward the use of skeletal myoblasts, and regenerative approaches moved onward toward more promising cell types.
1.2.2 Bone Marrow-Derived Stem Cells
Bone marrow-derived stem cells have the capacity to differentiate into multiple cell types including vascular and cardiac cell fates both in vitro and in vivo (Hirschi and Goodell 2002). The detection of Y-chromosome-positive cardiomyocytes in female hearts that were transplanted into male patients suggested that bone marrow-derived stem cells can differentiate into cardiomyocytes (Quaini et al. 2002). Over a decade ago, bone marrow-derived stem cells that express the surface marker c-kit emerged as candidates for regenerating the heart following injury through transdifferentiation into cardiomyocytes (Orlic et al. 2001). The differentiation potential of c-kit + cells in vivo led to controversy. Although the initial report suggested transdifferentiation of these cells into cardiomyocytes, subsequent studies by other groups found no evidence of transdifferentiation into cardiomyocytes, but rather showed the formation of more mature hematopoietic cell lineages following transplantation (Murry et al. 2004; Balsam et al. 2004). Improved ventricular function was detected following bone marrow-derived stem cell injections in multiple studies; several reports suggested that this effect is due to a paracrine effect through enhancing proliferation and differentiation of endogenous cardiac progenitors, thus promoting cardiac repair indirectly (Loffredo et al. 2011; Hatzistergos et al. 2010; Urbich et al. 2005; Mathieu et al. 2009; Kinnaird et al. 2004; Gnecchi et al. 2006; Hong et al. 2014).
REPAIR-AMI was the first randomized, blinded clinical trial to use autologous bone marrow cells through intracoronary infusion for acute myocardial infarction (MI) patients (Schachinger et al. 2006). There was a significant improvement in the left ventricular function following bone marrow transplantation, an effect that persisted up to 2–5 years after transplantation but with no impact on survival, though the trial had insufficient power to study survival (Assmus et al. 2010, 2014). However, a subsequent trial (TIME) using autologous bone marrow cells in ST-segment elevation MI (STEMI) showed no effect on improving cardiac function (Traverse et al. 2012). These mixed results generated debate on the impact of bone marrow-derived cells on improving function and survival of MI patients (Marban and Malliaras 2012). Retrospective evaluation of these clinical trials revealed some of the discrepancies and potential pitfalls to be avoided for proper assessment of the value of these cells as a clinical treatment (Simari et al. 2014; Nowbar et al. 2014). A large phase 3 clinical trial to assess the value of bone marrow cells in myocardial infarction patients is currently underway (BAMI trial).
1.2.3 Endothelial Progenitors
Endothelial progenitor cells (EPCs) are a small population of adult hematopoietic CD34+ progenitors that were identified in 1997 and which have the capacity to differentiate into endothelial cells (Asahara et al. 1997). Preclinical studies of EPCs showed promising results in enhancing recovery following ischemia in different tissues, mainly by enhancing neovascularization (Kawamoto and Losordo 2008). Following myocardial infarction, EPC transplantation may enhance functional recovery and myocardial integrity in vivo (Iwasaki et al. 2006; Kawamoto et al. 2001). This requires the homing of the EPCs to the site of ischemia followed by proliferation and differentiation into functional endothelial cells (Hristov et al. 2007). In addition to neovascularization, endothelial cells enhance cardiomyocyte survival and organization and contraction of surrounding cardiomyocytes through paracrine signaling (Narmoneva et al. 2004). These data suggest that endothelial cells can promote cardiac repair through different mechanisms.
Early phase clinical trials using cell transplantation of EPCs showed promising results for functional recovery following a cardiac insult (Vrtovec et al. 2013; Stamm et al. 2007). Similarly, pharmacological mobilization of EPCs using granulocyte colony-stimulating factor (G-CSF) showed enhanced cardiac function post-injury (Achilli et al. 2010). A major impediment to the understanding the full potential of EPCs is the different isolation methods for EPCs between different groups; thus the identity and purity of the EPC populations have not been consistent. Owing to the limited size of previous trials, large studies would be required to establish the efficacy of EPCs for heart repair.
1.2.4 Mesenchymal Stem Cells
Another subset of progenitors within the bone marrow is mesenchymal stem cells (MSCs). MSCs are multipotent and can differentiate into adipocytes, chondrocytes, and osteoblasts (Pittenger et al. 1999). MSCs are found in multiple tissues, and they can be expanded to the large numbers necessary for transplantation. Furthermore, MSCs appear less immunogenic due to the absence of MHC-II complex and may have lower probability of rejection (Kuraitis et al. 2011). Allogeneic MSCs showed therapeutic benefits following transplantation in the injured rodent and swine heart (Williams and Hare 2011). Initially there was evidence that allogeneic MSCs can differentiate into cardiomyocytes in vivo following engraftment in the adult murine and swine heart (Toma et al. 2002; Quevedo et al. 2009). Subsequent studies showed that MSCs probably accomplish beneficial effects via paracrine mechanisms (Mirotsou et al. 2007; Gnecchi et al. 2005, 2008). MSC transplantation in large animals showed activation and differentiation of cardiac stem cells (Hatzistergos et al. 2010). The POSEIDON trial showed improved patient outcome and ventricular remodeling, but no significant improvement in ventricular function (Hare et al. 2012). A randomized phase 3 clinical trial using MSCs for ischemic heart failure is currently ongoing (CHART-1), and the results from this trial will shed light on the future of MSCs in the clinic.
1.2.5 Endogenous Cardiac Stem Cells
1.2.5.1 C-kit + Cardiac Progenitors
Following the developments in the hematopoietic stem cell (HSC) field, c-kit, the receptor for stem cell factor, was described as a surface marker of HSC stemness. It was reported that the heart has an endogenous cardiac progenitor cell (CPC) population that is c-kit + without any hematopoietic lineage marker expression (Lin-) (Beltrami et al. 2003). These cells were described as clonogenic and multipotent due to their ability to differentiate into cardiomyocytes, endothelial cells, and smooth muscle cells in vitro and in vivo. Expansion of the c-kit + CPCs ex vivo and injection of the cells in vivo following MI showed a dramatic regenerative effect on the heart (Beltrami et al. 2003). Furthermore, a similar population of c-kit + CPCs was reported in the adult human heart and could repopulate the infarcted murine myocardium (Bearzi et al. 2007). The ability of c-kit + CPCs to enhance myocardial regeneration was demonstrated by different groups in small and large animal studies (Linke et al. 2005; Fischer et al. 2009; Angert et al. 2011). In contrast, other groups showed that c-kit + CPCs from adult hearts do not differentiate into cardiomyocytes ex vivo (Zaruba et al. 2010; Jesty et al. 2012). One study reported that c-kit + CPCs are not only necessary but also sufficient for myocardial regeneration following cardiac injury (Ellison et al. 2013). These conflicting results regarding the differentiation potential and functional impact of c-kit + CPCs on myocardial regeneration were addressed by a very well-designed lineage tracing study aimed to label the putative c-kit + CPCs in the heart to trace their lineage during aging and following injury (Van Berlo et al. 2014). Although this study showed that c-kit + CPCs could differentiate into cardiomyocytes, this occurred at negligibly low rates, which suggested that c-kit + CPCs would have no impact on myocyte replenishment following injury (Van Berlo et al. 2014). In contrast, c-kit + CPCs produced a high percentage of cardiac endothelial cells, suggesting that the endogenous c-kit + CPCs are more likely to be endothelial progenitor cells rather than true cardiomyocyte progenitors.
Although it is still unclear how c-kit + CPCs can enhance myocardial repair, their impact over the past decade has led to a number of clinical trials to assess their therapeutic potential. An early clinical trial to test the safety of c-kit + CPCs was a phase 1, randomized clinical trial for CPC intracoronary infusion in patients with ischemic cardiomyopathy (SCIPIO) (Bolli et al. 2011). This trial showed that CPC injection is safe with no adverse effects up to 1 year, with an improvement in LV function. The phase 1 trial was very small, however.
1.2.5.2 Cardiosphere and Cardiosphere-Derived Cells
Cardiosphere-derived cells represent another subset of cardiac progenitor cells in both murine and human hearts that are multipotent and can differentiate into different cardiac cell types (Messina et al. 2004). Cardiosphere-derived cells (CDCs) can be isolated from cells cultured from endomyocardial biopsies, and injection of CDCs in a large animal model of infarct has led to enhancement of cardiac function (Smith et al. 2007). Cardiosphere-derived cells were isolated from human hearts as well, and intracoronary injection of human CDCs in a pig infarct model improved cardiac function and reduced scar formation (Johnston et al. 2009). A phase 1 clinical trial using cardiosphere-derived autologous stem cells to reverse ventricular dysfunction (CADUCEUS) for intracoronary injection in myocardial infarction patients suggested the safety of these cells for clinical use, with potential benefits on cardiac function (Makkar et al. 2012). Further mechanistic studies of cardiosphere-derived cells showed that intracoronary injection of CDCs post MI stimulate endogenous cardiomyocyte proliferation, as well as recruitment of endogenous progenitors (Malliaras et al. 2013). These dual mechanisms may explain the beneficial outcomes following CDC cell therapy. Larger studies will be necessary to reveal the impact of cardiospheres and CDCs on this cell type as a candidate for myocardial regeneration in humans.
1.2.5.3 Side Population Cells
Side population (SP) cells are a population of cells characterized by their ability to exclude the Hoechst dye, since they express the ATP-binding cassette transporter proteins. These cells were first characterized as a hematopoietic stem cell population in the bone marrow (Goodell et al. 1996). To determine whether SP cells from the bone marrow can enhance cardiac repair, SP cells were transplanted in mice following an ischemia reperfusion injury and shown to have some therapeutic benefit and enhance myocardial repair (Jackson et al. 2001). Cardiac SP cells were further isolated from the developing and adult mouse heart, with the capacity to differentiate into cardiomyocytes, endothelial cells, and smooth muscle cells (Martin et al. 2004). Intravenous infusion of cardiac SP cells into rats that underwent myocardial infarction demonstrated that cardiac SP cells were able to migrate and home to the injured myocardium, differentiate into different cardiac cell types, and enhance heart regeneration (Oyama et al. 2007). These preclinical studies suggest a potential benefit for SP cells for cell therapy, although human clinical trials have not been performed with SP cells injected into the heart.
1.2.5.4 Sca1+ Cardiac Progenitors
Stem cell antigen1 (Sca1) is a cell surface marker expressed on the surface of multiple tissue-specific resident stem cells (Holmes and Stanford 2007). A Sca1+ cardiac stem cell population has been identified in the adult mouse heart and can differentiate into cardiomyocytes in vitro following treatment with 5-azacytidine as well as oxytocin (Oh et al. 2003; Matsuura et al. 2004). Intravenously injected Sca1+ cells were able to home to injured myocardium, differentiate into cardiomyocytes or fuse with host cells, and enhance repair following ischemia reperfusion injury (Oh et al. 2003). Similarly, intramyocardial transplantation of Sca1+ cardiac stem cells improved LV function post MI, although this effect was probably mediated through a paracrine effect by increased neovascularization and enhanced cardiomyocyte function (Wang et al. 2006). Lineage tracing of Sca1+ cells in the heart suggested that Sca1+ cells contribute to cardiomyocyte renewal in the adult heart, as well as in response to injury (Uchida et al. 2013). A major impediment to the clinical potential of Sca1+ cardiac stem cells is the lack of the Sca1 antigen in humans, which limits the use of these cells for human therapy.
1.2.5.5 Islet1+ Cardiac Progenitors
Islet1 (Isl1) is a transcription factor that marks a cardiac progenitor population from the second heart field that can differentiate into multiple cardiac lineages during heart embryonic development (Moretti et al. 2006; Cai et al. 2003). Interestingly, an Isl1+ cardiac progenitor population was identified in the early postnatal heart that can differentiate into mature cardiac lineages (Laugwitz et al. 2005). However, the Isl1+ progenitor population only persists in the sinoatrial node in the adult murine heart and is nearly absent from the left ventricle either at baseline or following MI (Weinberger et al. 2012). Isl1+ cardiac progenitors have not been studied for human cell therapy.
1.2.5.6 Epicardial Progenitors
Epicardial progenitor cells that express the transcription factor Wt1 have an important role during murine heart development, as they contribute to the formation of functional cardiomyocytes (Zhou et al. 2008). This role of epicardial progenitors led to the search for a similar progenitor population in the adult mammalian heart. Lineage tracing of Wt1 in the adult heart showed that Wt1 epicardial progenitors are present in the adult mouse heart and can give rise to bona fide cardiomyocytes following MI (Smart et al. 2011). Priming the Wt1 epicardial progenitors with thymosin β4 before MI may be an important step for these progenitors to give rise to cardiomyocytes, as priming them with thymosin β4 after MI does not seem to contribute to the differentiation of epicardial progenitors into cardiomyocytes (Zhou et al. 2012). However, embryonic and adult epicardial progenitors seem to be different subpopulations, as adult epicardial progenitors are more heterogeneous and have a different expression profile at the molecular level than embryonic progenitors (Bollini et al. 2014). Interestingly, a recent protocol described the derivation of primary human epicardial-derived cells from right atrial appendage biopsies, which can serve as a platform to further identify the therapeutic potential of epicardial progenitors for adult cardiac cell repair (Clunie-O’Connor et al. 2015).
1.2.6 ES-Derived Cardiomyocytes
Generation of differentiated, mature, and functional cardiomyocytes from pluripotent ES cells is a promising approach to replenish lost myocardium following injury (Xu et al. 2002). The development of directed differentiation protocols of pluripotent embryonic stem cells (ES) into cardiomyocytes has witnessed significant advances (Mummery et al. 2012). Purified human ES cell-derived cardiomyocytes (hESC-CM) can be derived when cultured with activin A and bone morphogenetic protein 4, which can improve cardiac function of the infarcted rat heart (Laflamme et al. 2007). Transplantation of cardiovascular progenitors derived from hESC led to engraftment in the infarcted hearts of nonhuman primates (Blin et al. 2010).
To establish the electrophysiological properties of hESC-CM, purified hESC-CM were transplanted in guinea pigs following injury (Shiba et al. 2012). These grafts led to reduced arrhythmias and were able to electrically couple with the host myocardium and thus efficiently enhance myocardial function following cryoinjury (Shiba et al. 2012). Recently, a large animal study in macaques showed that hESC-CM was able to remuscularize and regenerate the infarcted monkey heart (Chong et al. 2014). These recent promising results show the significant potential of hESC-CM. However, the ability of the transplanted hESC-CM to integrate efficiently in syncytium and prevent arrhythmias is still a concern (Chong et al. 2014). These issues will need to be addressed before hESC-CMs can be used for clinical trials. While ethical concerns might hamper ES use in the clinic, induced pluripotent stem cells (iPSCs) could replace hESC as the source of cardiomyocytes for cell therapy.
1.2.7 Induced Pluripotent Stem Cells and Reprogramming
1.2.7.1 iPSCs
Reprogramming adult mouse and human fibroblasts into a pluripotent state by transduction of four transcription factors, OCT4, SOX2, KLF4, and c-MYC (OSKM), was a revolutionary moment in biomedicine (Takahashi and Yamanaka 2006; Takahashi et al. 2007). iPSCs resemble ES cells morphologically and molecularly, and thus they provide an alternative to ES cell use, in addition to the advantage of generating patient-specific cell lines for autologous regenerative therapies. Although there was an initial concern toward using iPSCs clinically due to the use of oncogenes and viral vectors which can lead to teratoma formation, new methods and protocols are emerging that utilize small molecules, episomes, or proteins for reprogramming, which will increase the safety of the generated iPSCs (Zhou et al. 2009; Lin et al. 2009; Okita et al. 2008). Human iPSCs (hiPSCs) have been successfully used to generate numerous cell types including cardiomyocytes (Karakikes et al. 2015; Zhang et al. 2009). More importantly, hiPSCs provide a novel platform to dissect the underlying mechanisms of disease in patients (Bellin et al. 2012; Wang et al. 2014; Davis et al. 2012). Furthermore, intramyocardial transplantation of hiPSC-derived cardiomyocytes (hiPSC-CM) in a large animal model following MI led to a significant improvement of ventricular function and reduction of scar size while abrogating ventricular arrhythmias (Ye et al. 2014). Although further studies are required to truly understand the optimal way to use hiPSC-CMs, the recent developments indicate that this approach holds significant promise for future cell therapy (Okano et al. 2013).
1.2.7.2 Direct Reprogramming into Cardiomyocytes
Reprogramming fibroblasts into pluripotent cells led to a race toward reprogramming one cell type to another differentiated cell type. Transdifferentiation of fibroblasts to cardiomyocytes is an appealing approach as it could use the fibroblasts in the scar region to generate new myocardium. Using multiple combinations of cardiac transcription factors, a combination of three transcription factors, GATA4, MEF2C, and TBX5 (known as GMT), was able to reprogram mouse fibroblasts into induced cardiac-like myocytes in vitro (Ieda et al. 2010). To further examine whether direct reprogramming can occur in vivo, GMT and GHMT (H for HAND2) retroviral injections successfully reprogrammed cardiac fibroblasts into cardiomyocytes in vivo that resulted in an improved cardiac function and reduced scar following MI (Qian et al. 2012; Song et al. 2012). Furthermore, reprogramming fibroblasts into cardiomyocytes was achieved using microRNAs both in vitro and in vivo with improved cardiac regeneration (Jayawardena et al. 2012, 2015). Similar to iPSCs, reprogramming fibroblasts into cardiomyocytes occurs at low efficiency and may lead to the formation of immature cardiomyocyte-like cells rather than bona fide mature cardiomyocytes. Interestingly, recent studies showed that reprogramming efficiency could be enhanced significantly via upregulation of Akt1, as well as through inhibition of pro-fibrotic signaling (Zhou et al. 2015; Zhao et al. 2015). Further studies are necessary in order to generate mature and functional cardiomyocytes, as well as to fully understand the molecular mechanisms of reprogramming before moving forward to the clinic.
1.3 Future of Cell Therapy
Cardiac cell therapy has witnessed enormous achievements over the past decade. Cardiac cell therapy appears to be safe, with minimal adverse effects, while showing potential therapeutic benefits. However, cardiac cell therapy is not yet a clear success, as some analyses revealed no therapeutic benefit in acute myocardial infarction patients (Gyongyosi et al. 2015; Fisher et al. 2015). There is no consensus on which cell type will prove to be most effective. A recent study aimed at comparing hESC-CMs, cardiovascular progenitors (CVPs), and bone marrow mononuclear cells in a nude rat model of myocardial infarction (Fernandes et al. 2015). Interestingly, hESC-CMs and CVPs showed comparable improvement of cardiac repair, while bone marrow cells were less efficient (Fernandes et al. 2015). Comparing different cells is an important step in order to understand the optimal cell therapy for humans.
The results from large outcome trials are highly anticipated in order to determine the impact and the usefulness of cells in cardiac therapy. Although the mechanism of action of different cell types may vary, whether through direct differentiation into new myocardium, neovascularization, or paracrine effects, we need to expand our understanding at the molecular level. Clinical trials are the gold standard for assessing any treatment, but owing to the controversies within the cell therapy field, it is important to take a step back and progress at both the bench and the bedside. The lessons learned from heart regeneration in lower vertebrates and neonatal mice should improve our understanding of the promising approaches to regenerating the adult heart. Cardiac cellular therapy does lead to the complete regenerative response seen in animal models of endogenous heart regeneration, and thus there are many lessons to be learned from nature.
References
Achilli F, Malafronte C, Lenatti L, Gentile F, Dadone V, Gibelli G, Maggiolini S, Squadroni L, Di Leo C, Burba I, Pesce M, Mircoli L, Capogrossi MC, Di Lelio A, Camisasca P, Morabito A, Colombo G, Pompilio G, Investigators S-A (2010) Granulocyte colony-stimulating factor attenuates left ventricular remodelling after acute anterior STEMI: results of the single-blind, randomized, placebo-controlled multicentre stem cell Mobilization in acute myocardial infarction (STEM-AMI) trial. Eur J Heart Fail 12:1111–1121
Angert D, Berretta RM, Kubo H, Zhang H, Chen X, Wang W, Ogorek B, Barbe M, Houser SR (2011) Repair of the injured adult heart involves new myocytes potentially derived from resident cardiac stem cells. Circ Res 108:1226–1237
Asahara T, Murohara T, Sullivan A, Silver M, van der Zee R, Li T, Witzenbichler B, Schatteman G, Isner JM (1997) Isolation of putative progenitor endothelial cells for angiogenesis. Science 275:964–967
Assmus B, Leistner DM, Schachinger V, Erbs S, Elsasser A, Haberbosch W, Hambrecht R, Sedding D, Yu J, Corti R, Mathey DG, Barth C, Mayer-Wehrstein C, Burck I, Sueselbeck T, Dill T, Hamm CW, Tonn T, Dimmeler S, Zeiher AM, Group R-AS (2014) Long-term clinical outcome after intracoronary application of bone marrow-derived mononuclear cells for acute myocardial infarction: migratory capacity of administered cells determines event-free survival. Eur Heart J 35:1275–1283
Assmus B, Rolf A, Erbs S, Elsasser A, Haberbosch W, Hambrecht R, Tillmanns H, Yu J, Corti R, Mathey DG, Hamm CW, Suselbeck T, Tonn T, Dimmeler S, Dill T, Zeiher AM, Schachinger V, Investigators R-A (2010) Clinical outcome 2 years after intracoronary administration of bone marrow-derived progenitor cells in acute myocardial infarction. Circ Heart Fail 3:89–96
Balsam LB, Wagers AJ, Christensen JL, Kofidis T, Weissman IL, Robbins RC (2004) Haematopoietic stem cells adopt mature haematopoietic fates in ischaemic myocardium. Nature 428:668–673
Bearzi C, Rota M, Hosoda T, Tillmanns J, Nascimbene A, De Angelis A, Yasuzawa-Amano S, Trofimova I, Siggins RW, Lecapitaine N, Cascapera S, Beltrami AP, D’Alessandro DA, Zias E, Quaini F, Urbanek K, Michler RE, Bolli R, Kajstura J, Leri A, Anversa P (2007) Human cardiac stem cells. Proc Natl Acad Sci U S A 104:14068–14073
Bellin M, Marchetto MC, Gage FH, Mummery CL (2012) Induced pluripotent stem cells: the new patient? Nat Rev Mol Cell Biol 13:713–726
Beltrami AP, Barlucchi L, Torella D, Baker M, Limana F, Chimenti S, Kasahara H, Rota M, Musso E, Urbanek K, Leri A, Kajstura J, Nadal-Ginard B, Anversa P (2003) Adult cardiac stem cells are multipotent and support myocardial regeneration. Cell 114:763–776
Bergmann O, Bhardwaj RD, Bernard S, Zdunek S, Barnabe-Heider F, Walsh S, Zupicich J, Alkass K, Buchholz BA, Druid H, Jovinge S, Frisen J (2009) Evidence for cardiomyocyte renewal in humans. Science 324:98–102
Blin G, Nury D, Stefanovic S, Neri T, Guillevic O, Brinon B, Bellamy V, Rucker-Martin C, Barbry P, Bel A, Bruneval P, Cowan C, Pouly J, Mitalipov S, Gouadon E, Binder P, Hagege A, Desnos M, Renaud JF, Menasche P, Puceat M (2010) A purified population of multipotent cardiovascular progenitors derived from primate pluripotent stem cells engrafts in postmyocardial infarcted nonhuman primates. J Clin Invest 120:1125–1139
Bolli R, Chugh AR, D'Amario D, Loughran JH, Stoddard MF, Ikram S, Beache GM, Wagner SG, Leri A, Hosoda T, Sanada F, Elmore JB, Goichberg P, Cappetta D, Solankhi NK, Fahsah I, Rokosh DG, Slaughter MS, Kajstura J, Anversa P (2011) Cardiac stem cells in patients with ischaemic cardiomyopathy (SCIPIO): initial results of a randomised phase 1 trial. Lancet 378:1847–1857
Bollini S, Vieira JM, Howard S, Dube KN, Balmer GM, Smart N, Riley PR (2014) Re-activated adult epicardial progenitor cells are a heterogeneous population molecularly distinct from their embryonic counterparts. Stem Cells Dev 23:1719–1730
Cai CL, Liang X, Shi Y, Chu PH, Pfaff SL, Chen J, Evans S (2003) Isl1 identifies a cardiac progenitor population that proliferates prior to differentiation and contributes a majority of cells to the heart. Dev Cell 5:877–889
Chong JJ, Yang X, Don CW, Minami E, Liu YW, Weyers JJ, Mahoney WM, van Biber B, Cook SM, Palpant NJ, Gantz JA, Fugate JA, Muskheli V, Gough GM, Vogel KW, Astley CA, Hotchkiss CE, Baldessari A, Pabon L, Reinecke H, Gill EA, Nelson V, Kiem HP, Laflamme MA, Murry CE (2014) Human embryonic-stem-cell-derived cardiomyocytes regenerate non-human primate hearts. Nature 510:273–277
Clunie-O’Connor C, Smits AM, Antoniades C, Russell AJ, Yellon DM, Goumans MJ, Riley PR (2015) The derivation of primary human epicardium-derived cells. Curr Protoc Stem Cell Biol 35:2C.5.1–2C.5.12
Davis RP, Casini S, van den Berg CW, Hoekstra M, Remme CA, Dambrot C, Salvatori D, Oostwaard DW, Wilde AA, Bezzina CR, Verkerk AO, Freund C, Mummery CL (2012) Cardiomyocytes derived from pluripotent stem cells recapitulate electrophysiological characteristics of an overlap syndrome of cardiac sodium channel disease. Circulation 125:3079–3091
Durrani S, Konoplyannikov M, Ashraf M, Haider KH (2010) Skeletal myoblasts for cardiac repair. Regen Med 5:919–932
Ellison GM, Vicinanza C, Smith AJ, Aquila I, Leone A, Waring CD, Henning BJ, Stirparo GG, Papait R, Scarfo M, Agosti V, Viglietto G, Condorelli G, Indolfi C, Ottolenghi S, Torella D, Nadal-Ginard B (2013) Adult c-kit(pos) cardiac stem cells are necessary and sufficient for functional cardiac regeneration and repair. Cell 154:827–842
Fernandes S, Chong JJ, Paige SL, Iwata M, Torok-Storb B, Keller G, Reinecke H, Murry CE (2015) Comparison of human embryonic stem cell-derived cardiomyocytes, cardiovascular progenitors, and bone marrow mononuclear cells for cardiac repair. Stem Cell Reports 5(5):P753–P762
Fischer KM, Cottage CT, Wu W, Din S, Gude NA, Avitabile D, Quijada P, Collins BL, Fransioli J, Sussman MA (2009) Enhancement of myocardial regeneration through genetic engineering of cardiac progenitor cells expressing Pim-1 kinase. Circulation 120:2077–2087
Fisher SA, Doree C, Mathur A, Martin-Rendon E (2015) Meta-analysis of cell therapy trials for patients with heart failure. Circ Res 116:1361–1377
Garbern JC, Lee RT (2013) Cardiac stem cell therapy and the promise of heart regeneration. Cell Stem Cell 12:689–698
Gnecchi M, He H, Liang OD, Melo LG, Morello F, Mu H, Noiseux N, Zhang L, Pratt RE, Ingwall JS, Dzau VJ (2005) Paracrine action accounts for marked protection of ischemic heart by Akt-modified mesenchymal stem cells. Nat Med 11:367–368
Gnecchi M, He H, Noiseux N, Liang OD, Zhang L, Morello F, Mu H, Melo LG, Pratt RE, Ingwall JS, Dzau VJ (2006) Evidence supporting paracrine hypothesis for Akt-modified mesenchymal stem cell-mediated cardiac protection and functional improvement. FASEB J 20:661–669
Gnecchi M, Zhang Z, Ni A, Dzau VJ (2008) Paracrine mechanisms in adult stem cell signaling and therapy. Circ Res 103:1204–1219
Goodell MA, Brose K, Paradis G, Conner AS, Mulligan RC (1996) Isolation and functional properties of murine hematopoietic stem cells that are replicating in vivo. J Exp Med 183:1797–1806
Gyongyosi M, Wojakowski W, Lemarchand P, Lunde K, Tendera M, Bartunek J, Marban E, Assmus B, Henry TD, Traverse JH, Moye LA, Surder D, Corti R, Huikuri H, Miettinen J, Wohrle J, Obradovic S, Roncalli J, Malliaras K, Pokushalov E, Romanov A, Kastrup J, Bergmann MW, Atsma DE, Diederichsen A, Edes I, Benedek I, Benedek T, Pejkov H, Nyolczas N, Pavo N, Bergler-Klein J, Pavo IJ, Sylven C, Berti S, Navarese EP, Maurer G, Investigators A (2015) Meta-Analysis of Cell-based CaRdiac stUdiEs (ACCRUE) in patients with acute myocardial infarction based on individual patient data. Circ Res 116:1346–1360
Hare JM, Fishman JE, Gerstenblith G, Difede Velazquez DL, Zambrano JP, Suncion VY, Tracy M, Ghersin E, Johnston PV, Brinker JA, Breton E, Davis-Sproul J, Schulman IH, Byrnes J, Mendizabal AM, Lowery MH, Rouy D, Altman P, Wong Po Foo C, Ruiz P, Amador A, da Silva J, Mcniece IK, Heldman AW, George R, Lardo A (2012) Comparison of allogeneic vs autologous bone marrow-derived mesenchymal stem cells delivered by transendocardial injection in patients with ischemic cardiomyopathy: the POSEIDON randomized trial. JAMA 308:2369–2379
Hatzistergos KE, Quevedo H, Oskouei BN, Hu Q, Feigenbaum GS, Margitich IS, Mazhari R, Boyle AJ, Zambrano JP, Rodriguez JE, Dulce R, Pattany PM, Valdes D, Revilla C, Heldman AW, Mcniece I, Hare JM (2010) Bone marrow mesenchymal stem cells stimulate cardiac stem cell proliferation and differentiation. Circ Res 107:913–922
Haubner BJ, Schneider J, Schweigmann UU, Schuetz T, Dichtl W, Velik-Salchner C, Stein JI, Penninger JM (2015) Functional recovery of a human neonatal heart after severe myocardial infarction. Circ Res 118(2):216–221
Hirschi KK, Goodell MA (2002) Hematopoietic, vascular and cardiac fates of bone marrow-derived stem cells. Gene Ther 9:648–652
Holmes C, Stanford WL (2007) Concise review: stem cell antigen-1: expression, function, and enigma. Stem Cells 25:1339–1347
Hong KU, Guo Y, Li QH, Cao P, Al-Maqtari T, Vajravelu BN, Du J, Book MJ, Zhu X, Nong Y, Bhatnagar A, Bolli R (2014) c-kit+ Cardiac stem cells alleviate post-myocardial infarction left ventricular dysfunction despite poor engraftment and negligible retention in the recipient heart. PLoS One 9:e96725
Hristov M, Zernecke A, Liehn EA, Weber C (2007) Regulation of endothelial progenitor cell homing after arterial injury. Thromb Haemost 98:274–277
Hsieh PC, Segers VF, Davis ME, Macgillivray C, Gannon J, Molkentin JD, Robbins J, Lee RT (2007) Evidence from a genetic fate-mapping study that stem cells refresh adult mammalian cardiomyocytes after injury. Nat Med 13:970–974
Ieda M, Fu JD, Delgado-Olguin P, Vedantham V, Hayashi Y, Bruneau BG, Srivastava D (2010) Direct reprogramming of fibroblasts into functional cardiomyocytes by defined factors. Cell 142:375–386
Iwasaki H, Kawamoto A, Ishikawa M, Oyamada A, Nakamori S, Nishimura H, Sadamoto K, Horii M, Matsumoto T, Murasawa S, Shibata T, Suehiro S, Asahara T (2006) Dose-dependent contribution of CD34-positive cell transplantation to concurrent vasculogenesis and cardiomyogenesis for functional regenerative recovery after myocardial infarction. Circulation 113:1311–1325
Jackson KA, Majka SM, Wang H, Pocius J, Hartley CJ, Majesky MW, Entman ML, Michael LH, Hirschi KK, Goodell MA (2001) Regeneration of ischemic cardiac muscle and vascular endothelium by adult stem cells. J Clin Invest 107:1395–1402
Jayawardena TM, Egemnazarov B, Finch EA, Zhang L, Payne JA, Pandya K, Zhang Z, Rosenberg P, Mirotsou M, Dzau VJ (2012) MicroRNA-mediated in vitro and in vivo direct reprogramming of cardiac fibroblasts to cardiomyocytes. Circ Res 110:1465–1473
Jayawardena TM, Finch EA, Zhang L, Zhang H, Hodgkinson CP, Pratt RE, Rosenberg PB, Mirotsou M, Dzau VJ (2015) MicroRNA induced cardiac reprogramming in vivo: evidence for mature cardiac myocytes and improved cardiac function. Circ Res 116:418–424
Jessup M, Brozena S (2003) Heart failure. N Engl J Med 348:2007–2018
Jesty SA, Steffey MA, Lee FK, Breitbach M, Hesse M, Reining S, Lee JC, Doran RM, Nikitin AY, Fleischmann BK, Kotlikoff MI (2012) c-kit+ precursors support postinfarction myogenesis in the neonatal, but not adult, heart. Proc Natl Acad Sci U S A 109:13380–13385
Johnston PV, Sasano T, Mills K, Evers R, Lee ST, Smith RR, Lardo AC, Lai S, Steenbergen C, Gerstenblith G, Lange R, Marban E (2009) Engraftment, differentiation, and functional benefits of autologous cardiosphere-derived cells in porcine ischemic cardiomyopathy. Circulation 120:1075–1083
Jopling C, Sleep E, Raya M, Marti M, Raya A, Izpisua Belmonte JC (2010) Zebrafish heart regeneration occurs by cardiomyocyte dedifferentiation and proliferation. Nature 464:606–609
Karakikes I, Ameen M, Termglinchan V, Wu JC (2015) Human induced pluripotent stem cell-derived cardiomyocytes: insights into molecular, cellular, and functional phenotypes. Circ Res 117:80–88
Kawamoto A, Gwon HC, Iwaguro H, Yamaguchi JI, Uchida S, Masuda H, Silver M, Ma H, Kearney M, Isner JM, Asahara T (2001) Therapeutic potential of ex vivo expanded endothelial progenitor cells for myocardial ischemia. Circulation 103:634–637
Kawamoto A, Losordo DW (2008) Endothelial progenitor cells for cardiovascular regeneration. Trends Cardiovasc Med 18:33–37
Kikuchi K, Holdway JE, Werdich AA, Anderson RM, Fang Y, Egnaczyk GF, Evans T, Macrae CA, Stainier DY, Poss KD (2010) Primary contribution to zebrafish heart regeneration by gata4(+) cardiomyocytes. Nature 464:601–605
Kinnaird T, Stabile E, Burnett MS, Lee CW, Barr S, Fuchs S, Epstein SE (2004) Marrow-derived stromal cells express genes encoding a broad spectrum of arteriogenic cytokines and promote in vitro and in vivo arteriogenesis through paracrine mechanisms. Circ Res 94:678–685
Kuraitis D, Ruel M, Suuronen EJ (2011) Mesenchymal stem cells for cardiovascular regeneration. Cardiovasc Drugs Ther 25:349–362
Laflamme MA, Chen KY, Naumova AV, Muskheli V, Fugate JA, Dupras SK, Reinecke H, Xu C, Hassanipour M, Police S, O’Sullivan C, Collins L, Chen Y, Minami E, Gill EA, Ueno S, Yuan C, Gold J, Murry CE (2007) Cardiomyocytes derived from human embryonic stem cells in pro-survival factors enhance function of infarcted rat hearts. Nat Biotechnol 25:1015–1024
Laflamme MA, Murry CE (2011) Heart regeneration. Nature 473:326–335
Laugwitz KL, Moretti A, Lam J, Gruber P, Chen Y, Woodard S, Lin LZ, Cai CL, Lu MM, Reth M, Platoshyn O, Yuan JX, Evans S, Chien KR (2005) Postnatal isl1+ cardioblasts enter fully differentiated cardiomyocyte lineages. Nature 433:647–653
Leobon B, Garcin I, Menasche P, Vilquin JT, Audinat E, Charpak S (2003) Myoblasts transplanted into rat infarcted myocardium are functionally isolated from their host. Proc Natl Acad Sci U S A 100:7808–7811
Li F, Wang X, Capasso JM, Gerdes AM (1996) Rapid transition of cardiac myocytes from hyperplasia to hypertrophy during postnatal development. J Mol Cell Cardiol 28:1737–1746
Lin T, Ambasudhan R, Yuan X, Li W, Hilcove S, Abujarour R, Lin X, Hahm HS, Hao E, Hayek A, Ding S (2009) A chemical platform for improved induction of human iPSCs. Nat Methods 6:805–808
Linke A, Muller P, Nurzynska D, Casarsa C, Torella D, Nascimbene A, Castaldo C, Cascapera S, Bohm M, Quaini F, Urbanek K, Leri A, Hintze TH, Kajstura J, Anversa P (2005) Stem cells in the dog heart are self-renewing, clonogenic, and multipotent and regenerate infarcted myocardium, improving cardiac function. Proc Natl Acad Sci U S A 102:8966–8971
Loffredo FS, Steinhauser ML, Gannon J, Lee RT (2011) Bone marrow-derived cell therapy stimulates endogenous cardiomyocyte progenitors and promotes cardiac repair. Cell Stem Cell 8:389–398
Makkar RR, Smith RR, Cheng K, Malliaras K, Thomson LE, Berman D, Czer LS, Marban L, Mendizabal A, Johnston PV, Russell SD, Schuleri KH, Lardo AC, Gerstenblith G, Marban E (2012) Intracoronary cardiosphere-derived cells for heart regeneration after myocardial infarction (Caduceus): a prospective, randomised phase 1 trial. Lancet 379:895–904
Malliaras K, Zhang Y, Seinfeld J, Galang G, Tseliou E, Cheng K, Sun B, Aminzadeh M, Marban E (2013) Cardiomyocyte proliferation and progenitor cell recruitment underlie therapeutic regeneration after myocardial infarction in the adult mouse heart. EMBO Mol Med 5:191–209
Marban E, Malliaras K (2012) Mixed results for bone marrow-derived cell therapy for ischemic heart disease. JAMA 308:2405–2406
Martin CM, Meeson AP, Robertson SM, Hawke TJ, Richardson JA, Bates S, Goetsch SC, Gallardo TD, Garry DJ (2004) Persistent expression of the Atp-binding cassette transporter, Abcg2, identifies cardiac Sp cells in the developing and adult heart. Dev Biol 265:262–275
Mathieu M, Bartunek J, El Oumeiri B, Touihri K, Hadad I, Thoma P, Metens T, Da Costa AM, Mahmoudabady M, Egrise D, Blocklet D, Mazouz N, Naeije R, Heyndrickx G, Mcentee K (2009) Cell therapy with autologous bone marrow mononuclear stem cells is associated with superior cardiac recovery compared with use of nonmodified mesenchymal stem cells in a canine model of chronic myocardial infarction. J Thorac Cardiovasc Surg 138:646–653
Matsuura K, Nagai T, Nishigaki N, Oyama T, Nishi J, Wada H, Sano M, Toko H, Akazawa H, Sato T, Nakaya H, Kasanuki H, Komuro I (2004) Adult cardiac Sca-1-positive cells differentiate into beating cardiomyocytes. J Biol Chem 279:11384–11391
Menasche P, Alfieri O, Janssens S, Mckenna W, Reichenspurner H, Trinquart L, Vilquin JT, Marolleau JP, Seymour B, Larghero J, Lake S, Chatellier G, Solomon S, Desnos M, Hagege AA (2008) The myoblast autologous grafting in ischemic cardiomyopathy (magic) trial: first randomized placebo-controlled study of myoblast transplantation. Circulation 117:1189–1200
Messina E, De Angelis L, Frati G, Morrone S, Chimenti S, Fiordaliso F, Salio M, Battaglia M, Latronico MV, Coletta M, Vivarelli E, Frati L, Cossu G, Giacomello A (2004) Isolation and expansion of adult cardiac stem cells from human and murine heart. Circ Res 95:911–921
Mirotsou M, Zhang Z, Deb A, Zhang L, Gnecchi M, Noiseux N, Mu H, Pachori A, Dzau V (2007) Secreted frizzled related protein 2 (Sfrp2) is the key Akt-mesenchymal stem cell-released paracrine factor mediating myocardial survival and repair. Proc Natl Acad Sci U S A 104:1643–1648
Moretti A, Caron L, Nakano A, Lam JT, Bernshausen A, Chen Y, Qyang Y, Bu L, Sasaki M, Martin-Puig S, Sun Y, Evans SM, Laugwitz KL, Chien KR (2006) Multipotent embryonic isl1+ progenitor cells lead to cardiac, smooth muscle, and endothelial cell diversification. Cell 127:1151–1165
Mummery CL, Zhang J, Ng ES, Elliott DA, Elefanty AG, Kamp TJ (2012) Differentiation of human embryonic stem cells and induced pluripotent stem cells to cardiomyocytes: a methods overview. Circ Res 111:344–358
Murry CE, Soonpaa MH, Reinecke H, Nakajima H, Nakajima HO, Rubart M, Pasumarthi KB, Virag JI, Bartelmez SH, Poppa V, Bradford G, Dowell JD, Williams DA, Field LJ (2004) Haematopoietic stem cells do not transdifferentiate into cardiac myocytes in myocardial infarcts. Nature 428:664–668
Narmoneva DA, Vukmirovic R, Davis ME, Kamm RD, Lee RT (2004) Endothelial cells promote cardiac myocyte survival and spatial reorganization: implications for cardiac regeneration. Circulation 110:962–968
Nowbar AN, Mielewczik M, Karavassilis M, Dehbi HM, Shun-Shin MJ, Jones S, Howard JP, Cole GD, Francis DP, Group DW (2014) Discrepancies in autologous bone marrow stem cell trials and enhancement of ejection fraction (Damascene): weighted regression and meta-analysis. BMJ 348:g2688
Oberpriller JO, Oberpriller JC (1974) Response of the adult newt ventricle to injury. J Exp Zool 187:249–253
Oh H, Bradfute SB, Gallardo TD, Nakamura T, Gaussin V, Mishina Y, Pocius J, Michael LH, Behringer RR, Garry DJ, Entman ML, Schneider MD (2003) Cardiac progenitor cells from adult myocardium: homing, differentiation, and fusion after infarction. Proc Natl Acad Sci U S A 100:12313–12318
Okano H, Nakamura M, Yoshida K, Okada Y, Tsuji O, Nori S, Ikeda E, Yamanaka S, Miura K (2013) Steps toward safe cell therapy using induced pluripotent stem cells. Circ Res 112:523–533
Okita K, Nakagawa M, Hyenjong H, Ichisaka T, Yamanaka S (2008) Generation of mouse induced pluripotent stem cells without viral vectors. Science 322:949–953
Orlic D, Kajstura J, Chimenti S, Jakoniuk I, Anderson SM, Li B, Pickel J, Mckay R, Nadal-Ginard B, Bodine DM, Leri A, Anversa P (2001) Bone marrow cells regenerate infarcted myocardium. Nature 410:701–705
Oyama T, Nagai T, Wada H, Naito AT, Matsuura K, Iwanaga K, Takahashi T, Goto M, Mikami Y, Yasuda N, Akazawa H, Uezumi A, Takeda S, Komuro I (2007) Cardiac side population cells have a potential to migrate and differentiate into cardiomyocytes in vitro and in vivo. J Cell Biol 176:329–341
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, Moorman MA, Simonetti DW, Craig S, Marshak DR (1999) Multilineage potential of adult human mesenchymal stem cells. Science 284:143–147
Porrello ER, Mahmoud AI, Simpson E, Hill JA, Richardson JA, Olson EN, Sadek HA (2011) Transient regenerative potential of the neonatal mouse heart. Science 331:1078–1080
Porrello ER, Mahmoud AI, Simpson E, Johnson BA, Grinsfelder D, Canseco D, Mammen PP, Rothermel BA, Olson EN, Sadek HA (2013) Regulation of neonatal and adult mammalian heart regeneration by the miR-15 family. Proc Natl Acad Sci U S A 110:187–192
Poss KD, Wilson LG, Keating MT (2002) Heart regeneration in zebrafish. Science 298:2188–2190
Qian L, Huang Y, Spencer CI, Foley A, Vedantham V, Liu L, Conway SJ, Fu JD, Srivastava D (2012) In vivo reprogramming of murine cardiac fibroblasts into induced cardiomyocytes. Nature 485:593–598
Quaini F, Urbanek K, Beltrami AP, Finato N, Beltrami CA, Nadal-Ginard B, Kajstura J, Leri A, Anversa P (2002) Chimerism of the transplanted heart. N Engl J Med 346:5–15
Quevedo HC, Hatzistergos KE, Oskouei BN, Feigenbaum GS, Rodriguez JE, Valdes D, Pattany PM, Zambrano JP, Hu Q, Mcniece I, Heldman AW, Hare JM (2009) Allogeneic mesenchymal stem cells restore cardiac function in chronic ischemic cardiomyopathy via trilineage differentiating capacity. Proc Natl Acad Sci U S A 106:14022–14027
Schachinger V, Erbs S, Elsasser A, Haberbosch W, Hambrecht R, Holschermann H, Yu J, Corti R, Mathey DG, Hamm CW, Suselbeck T, Assmus B, Tonn T, Dimmeler S, Zeiher AM, Investigators R-A (2006) Intracoronary bone marrow-derived progenitor cells in acute myocardial infarction. N Engl J Med 355:1210–1221
Senyo SE, Steinhauser ML, Pizzimenti CL, Yang VK, Cai L, Wang M, Wu TD, Guerquin-Kern JL, Lechene CP, Lee RT (2013) Mammalian heart renewal by pre-existing cardiomyocytes. Nature 493:433–436
Sharpe N, Smith H, Murphy J, Greaves S, Hart H, Gamble G (1991) Early prevention of left ventricular dysfunction after myocardial infarction with angiotensin-converting-enzyme inhibition. Lancet 337:872–876
Shiba Y, Fernandes S, Zhu WZ, Filice D, Muskheli V, Kim J, Palpant NJ, Gantz J, Moyes KW, Reinecke H, Van Biber B, Dardas T, Mignone JL, Izawa A, Hanna R, Viswanathan M, Gold JD, Kotlikoff MI, Sarvazyan N, Kay MW, Murry CE, Laflamme MA (2012) Human ES-cell-derived cardiomyocytes electrically couple and suppress arrhythmias in injured hearts. Nature 489:322–325
Simari RD, Pepine CJ, Traverse JH, Henry TD, Bolli R, Spoon DB, Yeh E, Hare JM, Schulman IH, Anderson RD, Lambert C, Sayre SL, Taylor DA, Ebert RF, Moye LA (2014) Bone marrow mononuclear cell therapy for acute myocardial infarction: a perspective from the cardiovascular cell therapy research network. Circ Res 114:1564–1568
Smart N, Bollini S, Dube KN, Vieira JM, Zhou B, Davidson S, Yellon D, Riegler J, Price AN, Lythgoe MF, Pu WT, Riley PR (2011) De novo cardiomyocytes from within the activated adult heart after injury. Nature 474:640–644
Smith RR, Barile L, Cho HC, Leppo MK, Hare JM, Messina E, Giacomello A, Abraham MR, Marban E (2007) Regenerative potential of cardiosphere-derived cells expanded from percutaneous endomyocardial biopsy specimens. Circulation 115:896–908
Song K, Nam YJ, Luo X, Qi X, Tan W, Huang GN, Acharya A, Smith CL, Tallquist MD, Neilson EG, Hill JA, Bassel-Duby R, Olson EN (2012) Heart repair by reprogramming non-myocytes with cardiac transcription factors. Nature 485:599–604
Soonpaa MH, Field LJ (1997) Assessment of cardiomyocyte DNA synthesis in normal and injured adult mouse hearts. Am J Phys 272:H220–H226
Stamm C, Kleine HD, Choi YH, Dunkelmann S, Lauffs JA, Lorenzen B, David A, Liebold A, Nienaber C, Zurakowski D, Freund M, Steinhoff G (2007) Intramyocardial delivery of CD133+ bone marrow cells and coronary artery bypass grafting for chronic ischemic heart disease: safety and efficacy studies. J Thorac Cardiovasc Surg 133:717–725
Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T, Tomoda K, Yamanaka S (2007) Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131:861–872
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126:663–676
Terracciano CM, Miller LW, Yacoub MH (2010) Contemporary use of ventricular assist devices. Annu Rev Med 61:255–270
Toma C, Pittenger MF, Cahill KS, Byrne BJ, Kessler PD (2002) Human mesenchymal stem cells differentiate to a cardiomyocyte phenotype in the adult murine heart. Circulation 105:93–98
Traverse JH, Henry TD, Pepine CJ, Willerson JT, Zhao DX, Ellis SG, Forder JR, Anderson RD, Hatzopoulos AK, Penn MS, Perin EC, Chambers J, Baran KW, Raveendran G, Lambert C, Lerman A, Simon DI, Vaughan DE, Lai D, Gee AP, Taylor DA, Cogle CR, Thomas JD, Olson RE, Bowman S, Francescon J, Geither C, Handberg E, Kappenman C, Westbrook L, Piller LB, Simpson LM, Baraniuk S, Loghin C, Aguilar D, Richman S, Zierold C, Spoon DB, Bettencourt J, Sayre SL, Vojvodic RW, Skarlatos SI, Gordon DJ, Ebert RF, Kwak M, Moye LA, Simari RD, Cardiovascular Cell Therapy Research, N (2012) Effect of the use and timing of bone marrow mononuclear cell delivery on left ventricular function after acute myocardial infarction: the TIME randomized trial. JAMA 308:2380–2389
Uchida S, De Gaspari P, Kostin S, Jenniches K, Kilic A, Izumiya Y, Shiojima I, Grosse Kreymborg K, Renz H, Walsh K, Braun T (2013) Sca1-derived cells are a source of myocardial renewal in the murine adult heart. Stem Cell Reports 1:397–410
Urbich C, Aicher A, Heeschen C, Dernbach E, Hofmann WK, Zeiher AM, Dimmeler S (2005) Soluble factors released by endothelial progenitor cells promote migration of endothelial cells and cardiac resident progenitor cells. J Mol Cell Cardiol 39:733–742
Van Berlo JH, Kanisicak O, Maillet M, Vagnozzi RJ, Karch J, Lin SC, Middleton RC, Marban E, Molkentin JD (2014) c-kit+ cells minimally contribute cardiomyocytes to the heart. Nature 509:337–341
Vrtovec B, Poglajen G, Lezaic L, Sever M, Domanovic D, Cernelc P, Socan A, Schrepfer S, Torre-Amione G, Haddad F, Wu JC (2013) Effects of intracoronary CD34+ stem cell transplantation in nonischemic dilated cardiomyopathy patients: 5-year follow-up. Circ Res 112:165–173
Walsh S, Ponten A, Fleischmann BK, Jovinge S (2010) Cardiomyocyte cell cycle control and growth estimation in vivo--an analysis based on cardiomyocyte nuclei. Cardiovasc Res 86:365–373
Wang G, Mccain ML, Yang L, He A, Pasqualini FS, Agarwal A, Yuan H, Jiang D, Zhang D, Zangi L, Geva J, Roberts AE, Ma Q, Ding J, Chen J, Wang DZ, Li K, Wang J, Wanders RJ, Kulik W, Vaz FM, Laflamme MA, Murry CE, Chien KR, Kelley RI, Church GM, Parker KK, Pu WT (2014) Modeling the mitochondrial cardiomyopathy of Barth syndrome with induced pluripotent stem cell and heart-on-chip technologies. Nat Med 20:616–623
Wang X, Hu Q, Nakamura Y, Lee J, Zhang G, From AH, Zhang J (2006) The role of the sca-1+/CD31- cardiac progenitor cell population in postinfarction left ventricular remodeling. Stem Cells 24:1779–1788
Weinberger F, Mehrkens D, Friedrich FW, Stubbendorff M, Hua X, Muller JC, Schrepfer S, Evans SM, Carrier L, Eschenhagen T (2012) Localization of Islet-1-positive cells in the healthy and infarcted adult murine heart. Circ Res 110:1303–1310
Whelan RS, Kaplinskiy V, Kitsis RN (2010) Cell death in the pathogenesis of heart disease: mechanisms and significance. Annu Rev Physiol 72:19–44
Williams AR, Hare JM (2011) Mesenchymal stem cells: biology, pathophysiology, translational findings, and therapeutic implications for cardiac disease. Circ Res 109:923–940
Xu C, Police S, Rao N, Carpenter MK (2002) Characterization and enrichment of cardiomyocytes derived from human embryonic stem cells. Circ Res 91:501–508
Ye L, Chang YH, Xiong Q, Zhang P, Zhang L, Somasundaram P, Lepley M, Swingen C, Su L, Wendel JS, Guo J, Jang A, Rosenbush D, Greder L, Dutton JR, Zhang J, Kamp TJ, Kaufman DS, Ge Y, Zhang J (2014) Cardiac repair in a porcine model of acute myocardial infarction with human induced pluripotent stem cell-derived cardiovascular cells. Cell Stem Cell 15:750–761
Zaruba MM, Soonpaa M, Reuter S, Field LJ (2010) Cardiomyogenic potential of C-kit(+)-expressing cells derived from neonatal and adult mouse hearts. Circulation 121:1992–2000
Zhang J, Wilson GF, Soerens AG, Koonce CH, Yu J, Palecek SP, Thomson JA, Kamp TJ (2009) Functional cardiomyocytes derived from human induced pluripotent stem cells. Circ Res 104:e30–e41
Zhao Y, Londono P, Cao Y, Sharpe EJ, Proenza C, O'Rourke R, Jones KL, Jeong MY, Walker LA, Buttrick PM, Mckinsey TA, Song K (2015) High-efficiency reprogramming of fibroblasts into cardiomyocytes requires suppression of pro-fibrotic signalling. Nat Commun 6:8243
Zhou B, Honor LB, Ma Q, Oh JH, Lin RZ, Melero-Martin JM, Von Gise A, Zhou P, Hu T, He L, Wu KH, Zhang H, Zhang Y, Pu WT (2012) Thymosin beta 4 treatment after myocardial infarction does not reprogram epicardial cells into cardiomyocytes. J Mol Cell Cardiol 52:43–47
Zhou B, Ma Q, Rajagopal S, Wu SM, Domian I, Rivera-Feliciano J, Jiang D, Von Gise A, Ikeda S, Chien KR, Pu WT (2008) Epicardial progenitors contribute to the cardiomyocyte lineage in the developing heart. Nature 454:109–113
Zhou H, Dickson ME, Kim MS, Bassel-Duby R, Olson EN (2015) Akt1/protein kinase B enhances transcriptional reprogramming of fibroblasts to functional cardiomyocytes. Proc Natl Acad Sci U S A 112:11864–11869
Zhou H, Wu S, Joo JY, Zhu S, Han DW, Lin T, Trauger S, Bien G, Yao S, Zhu Y, Siuzdak G, Scholer HR, Duan L, Ding S (2009) Generation of induced pluripotent stem cells using recombinant proteins. Cell Stem Cell 4:381–384
Acknowledgments
This work was supported by an American Heart Association Postdoctoral Fellowship (15POST21870000) to AIM. This work was supported by NIH grants (AG040019) and (HL117986) to RTL and by the Leducq Foundation.
Compliance with Ethical Standards
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Mahmoud, A.I., Lee, R.T. (2017). Past and Future of Cell-Based Heart Repair. In: Ieda, M., Zimmermann, WH. (eds) Cardiac Regeneration. Cardiac and Vascular Biology, vol 4. Springer, Cham. https://doi.org/10.1007/978-3-319-56106-6_1
Download citation
DOI: https://doi.org/10.1007/978-3-319-56106-6_1
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-56104-2
Online ISBN: 978-3-319-56106-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)