Abstract
Numerous fecal biomarkers have been shown to correlate with disease activity in Crohn disease (CD) and ulcerative colitis (UC). Fecal calprotectin (FC) and lactoferrin are the two most frequently studied. FC in particular has been extensively studied and shown to have sufficient sensitivity and specificity for detecting mucosal inflammation to aid in initial diagnosis prior to ileocolonoscopy. Emerging research in CD and UC shows acceptable correlation of FC with endoscopic activity, prediction of inflammatory bowel disease (IBD) relapse, and therapy responsiveness. Given their relative ease of collection and lower cost, fecal biomarkers appear promising as a noninvasive test to improve disease monitoring in standard of care.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Inflammatory bowel disease
- Ulcerative colitis
- Crohn disease
- Fecal biomarkers
- Calprotectin
- Lactoferrin
- Mucosal healing
- Monitoring
Introduction
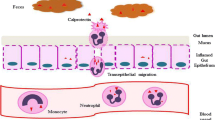
Inflammatory bowel diseases (IBDs), including ulcerative colitis (UC) and Crohn disease (CD), are chronic relapsing and remitting diseases due to intestinal inflammation. Endoscopic evaluation and histologic confirmation are required for diagnosis and are often used to monitor disease progression and response to therapy. After diagnosis of IBD, clinical disease remission is the goal of therapy; however, evidence suggests that mucosal healing is the outcome measure of choice [1–3]. While endoscopic confirmation is the gold standard in detecting mucosal healing [4], repeated endoscopy is costly and invasive. Because serial endoscopies to monitor disease activity is unrealistic, especially in children who require general anesthesia for endoscopic procedures, many gastroenterologists rely on surrogate markers of inflammation. These include serologic biomarkers (e.g. C-reactive protein (CRP), erythrocyte sedimentation rate (ESR)), clinical disease activity indices (e.g. CDAI, Pediatric Crohn’s disease Activity Index (PCDAI)), and patient-reported symptoms. While these indices can be helpful in the diagnosis and monitoring of IBD, they have low specificity for accurate endoscopic correlation. Because inflamed mucosa contains a high number of neutrophils, fecal neutrophil-derived biomarkers such as fecal calprotectin (FC, structure shown in Fig. 19.1) and lactoferrin have emerged as promising tools to accurately assess mucosal-level inflammation to aid in the diagnosis and monitoring of IBD [6].
Fecal calprotectin (Taken from Vogl et al. [5]) Tertiary and quaternary structures of S100A8 and S100A9 proteins presented by ribbon diagrams: (a) S100A8 homodimer; individual subunits are shown in purple and dark blue; (b) S100A9 homodimer; subunits are shown in sea-blue and yellow; (c) S100A8/A9 heterodimers shown in two projections rotated by 180°; (d) S100A8/A9 heterotetramer calprotectin and (e) S100A8/A9 dodecamer assembled from three calprotectins; (f) Schematic outline of the arrangements of S100SA8 and S100A9 in calprotectin. Subunits are presented in individual colors as in (a, b). Bound Ca2+ ions are shown by green spheres or squares, respectively
The goal of this chapter is to summarize current literature on the clinically available fecal biomarkers used in IBD practice. Of these biomarkers, FC and lactoferrin are the two most frequently studied. FC in particular has been extensively studied and shown to have sufficient sensitivity and specificity for detecting mucosal inflammation. This chapter will focus on FC because of the clinical utility and increasing use in clinical practice. This includes the diagnosis of IBD, monitoring of disease activity, response to pharmacologic therapy, detecting mucosal inflammation, and predicting relapse [7, 8–13]. We will also discuss the use of FC in distinguishing between symptoms caused by IBD and those due to other causes, such as irritable bowel syndrome (IBS) [11, 14–16]. Table 19.1 summarizes other available fecal biomarkers.
Fecal biomarkers play an important role in helping guide clinical decision making in patients with suspected or confirmed IBD. These surrogate markers of inflammation, with their ease of collection and relatively low cost, can be widely used in the diagnosis and long-term monitoring of IBD, with the potential to reduce the number of invasive and costly endoscopic procedures and improve patient outcomes.
Fecal Calprotectin Use in Distinguishing Irritable Bowel Syndrome from Inflammatory Bowel Disease
Irritable bowel syndrome (IBS) is a highly prevalent disorder, affecting an estimated 10–15% of the population [38], and accounts for up to 25% of a gastroenterologist’s time in the outpatient setting [39]. IBS patients are also reported to utilize health care resources disproportionately to the seriousness of their symptoms [40]. In a study to estimate total costs for patients with IBS, functional diarrhea, functional constipation, and functional abdominal pain, Nyrop et al. found that the mean annual direct health care costs were $5049, $6140, $7522, and $7646, respectively [41]. There are many symptoms that overlap in patients with IBS and IBD (e.g., abdominal pain, bloating, diarrhea). Additionally, studies have found the prevalence of IBS in patients with IBD to be as high as 39% [42]. This overlap makes the treatment of IBD symptoms due to true intestinal inflammation difficult. Because IBD management relies on patient reported outcomes, this can lead to both overtreatment of IBS and undertreatment of IBD.
Given its ease of collection and analysis, low cost, and high sensitivity in detecting intestinal inflammation, FC is currently being used as a screening tool to differentiate between IBD and IBS, possibly decreasing the number of unnecessary diagnostic endoscopies. Because of the many overlapping symptoms between IBD and IBS, many patients with IBS undergo endoscopic evaluation, which is an invasive and costly evaluation [43]. Tibble et al. performed a prospective study to assess the value of FC in discriminating between patients with Crohn disease and IBS [10]. Results of this study showed that all patients with CD had increased FC (median 135 mg/L), which differed significantly from normal controls and patients with IBS. At a cutoff level of 30 mg/L, FC had a 100% sensitivity and 97% specificity in discriminating between active CD and IBS. FC was therefore found to be a useful biomarker to differentiate between symptoms due to IBD versus other noninflammatory states.
In a meta-analysis by van Rheenen et al. that included both adult and pediatric patients, quantitative FC was found to be a useful screening tool for identifying patients who warrant endoscopy for suspected IBD [11]. This meta-analysis showed that screening by measuring FC resulted in a 67% reduction in the number of adults requiring endoscopy, and a reduction of 35% in children. This study also highlighted a downside of using FC as a screening method in that it led to a delayed diagnosis in 6% of adults and 8% of children with IBD due to false negative results. This study also found that FC had a lower specificity in children when compared to adults [11]. However, in a more recent meta-analysis by Henderson et al. that included two newer pediatric studies, with the strict selection of only children undergoing their primary investigation for IBD, sensitivity was found to be increased, whereas specificity was slightly decreased [14]. In this meta-analysis, which included a total of 715 pediatric patients, FC was found to have a very high sensitivity of 98% and a moderate specificity of 68% in the diagnosis of suspected pediatric IBD [14].
In a meta-analysis by von Roon et al. assessing the diagnostic precision of FC in IBD, FC was found to potentially discriminate between patients with IBD and those without IBD for both adult and pediatric populations [44]. A cutoff of 100 mcg/g was found to be more precise than a cutoff of 50 mcg/g. FC was found to have a good diagnostic precision in predicting relapse in IBD, and the precision of FC for the diagnosis of IBD was found to be superior to serological markers such as CRP, ESR, anti-saccharomyces cerevisiae antibodies (ASCA), anti-neutrophil cytoplasmic antibodies (ANCA), and outer membrane protein c (OmpC).
Park et al. compared the cost effectiveness of measuring FC before endoscopy in adult and pediatric patients with suspected IBD versus direct endoscopy alone, which is the current standard of care [45]. Results showed that screening adults and children to measure FC is effective and cost-effective in identifying patients with IBD when the pretest probability is <75% for adults and >65% in children. This analysis, using data from van Rheenen et al. [11], showed that in adults, FC screening saved $417 per patient but delayed diagnosis for 2 of the 32 patients who had IBD among 100 screened patients. In children, FC screening saved $300/patient but delayed diagnosis for 5 of the 61 patients who had IBD among 100 screened patients. If direct endoscopic evaluation remains standard of care for diagnosis of IBD, it would cost an additional $18,955 in adults and $6250 in children to avoid one false-negative result from FC screening [45]. These studies highlight that FC can be used to distinguish disorders of intestinal inflammation versus other noninflammatory disorders that may mimic IBD.
Fecal Calprotectin for Inflammatory Bowel Disease
Calprotectin Levels Correspond Directly with Endoscopic Activity
There is growing evidence to support mucosal healing as the outcome measure of choice in IBD [2, 46, 47–49, 50]. It has been shown that mucosal healing indicates better disease outcomes [1–3], reduced risk of relapse and reduced development of cancer and need for surgery in UC [49]. Evaluation of mucosal healing, however, requires endoscopy for direct visualization and histopathologic confirmation, which is costly and invasive. Targeting mucosal healing in children is particularly difficult given the invasive nature of frequent endoscopies that require general anesthesia. Given the impracticality of serial endoscopies, clinicians rely on other surrogate markers of clinical disease activity, including Clinical Disease Activity Index (CDAI), Pediatric Crohn’s Disease Activity Index (PCDAI), Simple Clinical Colitis Activity Index, Mayo Clinic score, as well as serum and fecal biomarkers of inflammation such as CRP, ESR, FC, and lactoferrin. Because scoring mechanisms give substantive weight to subjective patient-reported symptoms, the use of these activity indices to guide therapy has recently been questioned since subjective patient reports do not always correlate with mucosal-level disease activity.
Serum surrogate markers such as CRP and ESR have been used to monitor disease activity in IBD; however, the relationship between these markers and disease activity is not fully understood [47, 51–57, 58]. Although widely used and readily available, a significant limitation of most biomarkers of inflammation is that they are nonspecific and can be elevated in many other non-intestinal diseases. CRP is a widely used marker and previous studies have examined the relationship between CRP and other clinical measures of disease activity in IBD [9, 47, 53, 54, 59, 60]. CRP has been found to be associated with clinical and endoscopic activity in IBD [7, 47, 61] but has been shown to have poor sensitivity for endoscopic activity in patients with IBD [62]. CRP also has been shown to be persistently normal in patients with CD despite active disease, making this a poor test to differentiate quiescent from active CD [52]. In a retrospective study examining the relationship between CRP and clinical, endoscopic, histologic, and radiographic activity in IBD, Solem et al. [62] found that CRP elevation was significantly associated with active clinical disease, other biomarkers of inflammation, and active disease at ileocolonoscopy in patients with CD. However, this study showed that 63% of CD patients with active clinical disease and a normal CRP had active disease by ileocolonoscopy. Furthermore, there was no association between CRP and radiographic activity. This study found that in patients with UC, while CRP elevation was significantly associated with clinical disease activity, biomarkers of inflammation and active disease at ileocolonoscopy, CRP concentrations were not associated with histologic activity in UC patients. In a review by Lewis et al. studying the role of several biomarkers in assessing endoscopic activity in IBD, FC showed the best correlation with endoscopic activity in both CD and UC [63]. Schoepfer et al. showed that FC correlated closest with the widely used Simple Endoscopic Score for Crohn’s disease (SES-CD), followed by CRP, blood leukocytes, and the CDAI [9]. This study also showed that FC was the only biomarker that reliably discriminated inactive from mild, moderate, and highly active disease, highlighting the usefulness of FC in monitoring disease activity.
FC has also emerged as a potential surrogate marker that can be used to predict mucosal healing, which has become the outcome measurement of choice in monitoring IBD [1–3]. Lobaton et al. showed a significant correlation between FC levels and endoscopic activity in patients with UC [64]. In this study, a cutoff value of 250 mcg/g for Fecal Calprotectin ELISA (FC-ELISA) or a 280 mcg/g cutoff level for Fecal Calprotectin quantitative point of care test (FC-QPOCT) was found to be a more accurate marker of endoscopic activity than both clinical activity and measurement of other frequently used biomarkers. FC was shown to be an accurate biomarker of both “endoscopic remission” and “no endoscopic activity” (Mayo endoscopic subscore grade ≤1 and ≤ 0, respectively) [64]. In another study assessing the value of FC as a surrogate marker of mucosal inflammation, D’Haens et al. concluded that FC was the best available surrogate marker for the presence of mucosal inflammation and therefore should be considered a useful alternative to repeated endoscopic evaluations [46]. In this study, endoscopic scores correlated significantly with the level of fecal calprotectin in both CD and UC. Of note, this study reported median FC level of 465 mcg/g in UC patients, 175 mcg/g in CD patients, and 45 mcg/g in patients with IBS. In a recent study examining FC correlation with histologic remission and mucosal healing in IBD, Zittan et al. found that FC below 100 mcg/g was highly correlated with histologic remission and absence of basal plasmacytosis in both UC and CD, and a level <100 mcg/g had the highest sensitivity in terms of clinical and endoscopic remission for both CD and UC [65]. In a recent study by Langhorst et al., results showed that fecal biomarkers FC, lactoferrin, and Polymorphonuclear neutrophil (PMN)-elastase were able to distinguish between UC patients with mucosal healing from clinical remission and mild disease, showed significant correlations with endoscopy, and were predictive of flare [66]. These studies highlight the potential role of fecal biomarkers, FC in particular, in predicting endoscopic activity, which can potentially reduce the number of endoscopies performed for monitoring of mucosal healing.
Calprotectin Predicts IBD Relapse
Inflammatory bowel diseases are chronic diseases of inflammation that have a typical relapsing and remitting courses [67]. The primary goal of management is to prevent relapses and increase periods of remission. Because subclinical inflammation can lead to relapse [68], noninvasive biomarkers and clinical activity indices have been used in an attempt to predict relapses. Unfortunately, many widely used inflammatory markers have poor specificity and do not predict relapse [63, 47, 52, 62], and clinical disease indices (e.g., CDAI) have been shown to not correlate with disease activity [12]. FC has been proposed as the gold standard in non-invasive testing to evaluate intestinal inflammation in patients with IBD [10, 69–71] and has been shown to accurately predict relapse [12, 72–74].
The use of FC to predict relapse in patients with IBD could be particularly useful in initiating treatment in an earlier stage of relapse, even before onset of symptoms, to lessen severity of relapse and prolong periods between relapses. Many serum biomarkers, such as CRP, ESR, platelet count, white cell count, interleukin (IL)-1β, and tumor necrosis factor alpha (TNFα) have been used to help predict relapse in IBD. However, these markers are nonspecific and do not directly measure intestinal inflammation [72]. In a prospective study examining clinical, biologic, and histologic parameters as predictors of relapse in UC, Bitton et al. found that ESR, CRP, IL-β, IL-6, and IL-15 did not predict relapse in patients with quiescent UC [47]. Tibble et al. found that FC predicts clinical relapse of disease activity in patients with both CD and UC [72]. Results of this study showed that a single FC level of >50 mg/L predicted clinical relapse with a 90% sensitivity and 83% specificity. In another prospective, randomized, controlled trial evaluating utility of serially measured FC, CRP, and CDAI in predicting endoscopic recurrence in CD patients after intestinal resection, Wright et al. showed that patients with endoscopic recurrence had higher FC values [12]. The study showed that 6- and 18-month FC levels correlated significantly with presence and severity of endoscopic recurrence, whereas CRP level and the CDAI did not. A FC cutoff of >100 mcg/g identified patients with endoscopic recurrence with an 89% sensitivity and 58% specificity [12].
Some studies have suggested that FC is less predictive of relapse in patients with CD compared to UC, or with ileal CD compared with colonic and ileocolonic CD [73–75]. Therefore, patients may need stratification based on phenotype to improve predictive value of FC in CD [74, 75]. In a study by Kallel et al. investigators showed when patients with CD confined to small bowel were excluded, FC levels above 340 μg/g had an almost 19-fold greater risk of relapse than those with lower concentrations [76]. Costa et al. found FC to be a stronger predictor of clinical relapse in UC than in CD [61]. In this study, investigators found that among IBD patients in clinical remission with a high FC >150 mcg/g, 50% of CD patients maintained remission compared with 19% of those with UC. This is in contrast to a study by Tibble et al. that showed FC was an equally reliable predictor of relapse in UC and CD [72]. Of note, in the study by Costa et al., it was also found that ESR and CRP did not prove to be useful predictors of clinical relapse in IBD as a whole [61].
Calprotectin Predicts Drug Responsiveness
FC has also been shown to predict response to medical therapy in patients with IBD [77]. De Vos et al. performed a study to evaluate the evolution of FC levels under infliximab induction therapy and its correlation with mucosal healing as compared to Mayo score in patients with UC [77]. Results showed that median FC levels decreased from 1260 mg/kg at baseline to 72.5 mg/kg at 10 weeks. After 10 weeks, infliximab therapy induced endoscopic remission and a decrease in FC to <50 mg/kg or at least 80% decrease from baseline level in 58% of patients. Furthermore, all patients with a FC level <50 mg/kg were found to be in endoscopic remission. This study highlighted the fast and sharp decrease in FC levels after Infliximab infusion, as well as showing the absence of this decrease identifies patients who may be nonresponders.
In a recent post hoc analysis by Sanborn et al., FC was found to correlate with clinical and endoscopic outcomes of patients with moderate to severe UC receiving tofacitinib (a JAK inhibitor) [8]. While this study found a strong correlation between FC and other clinical measurement outcomes at a population level, this was less strong at an individual level, likely due to high inter- and intrapatient variability in FC concentrations. These studies highlight the potential use of FC as a predictor of drug responsiveness, which could help guide therapeutic treatment options for patients with IBD.
On the Horizon: Monitoring
Although disease monitoring is common in clinical practice across specialties, the principles of monitoring are not well conceptualized, which can lead to suboptimal care [78]. In patients with IBD, disease monitoring strategies should focus on the judicious use of tests and procedures to accurately monitor disease progression, monitor response to medical therapy, reduce risk, prevent relapse, reduce costs, and improve patient care. The current outcome measure of choice in patients with IBD is mucosal healing [1, 2, 49], and direct endoscopic visualization and histologic evidence is gold standard in detecting mucosal healing.
Because repeated endoscopy is invasive and costly, IBD practitioners rely on non-invasive tools for disease monitoring, including physician-dependent global disease assessments, patient reported symptoms, clinical disease activity indices, and trends in serum biomarkers such as CRP and ESR to estimate mucosal-level inflammation. Fecal biomarkers have emerged as potentially superior surrogate markers to guide clinical decision making in patients with suspected or confirmed IBD. They are simple, non-invasive, low-cost, and many studies have shown superior accuracy and sensitivity when compared to other disease monitoring strategies. The most extensively studied and frequently used fecal biomarker in current clinical practice is FC. Although large-scale studies are required to definitively evaluate the role of FC in early and accurate detection of mucosal-level inflammation [79], FC has emerged as a superior marker that can be used for long-term monitoring in patients with IBD to accurately detect mucosal level healing and to guide clinical decision making without repeated invasive endoscopy.
References
Colombel JF, Rutgeerts P, Reinisch W, Esser D, Wang Y, et al. Early mucosal healing with infliximab is associated with improved long-term clinical outcomes in ulcerative colitis. Gastroenterology. 2011;141:1194–201.
KF F, Jahnsen J, BA M, MH V, Group I. Mucosal healing in inflammatory bowel disease: results from a Norwegian population-based cohort. Gastroenterol. 2007;133:412–22.
Meucci G, Fasoli R, Saibeni S, Valpiani D, Gullotta R, et al. Prognostic significance of endoscopic remission in patients with active ulcerative colitis treated with oral and topical mesalazine: a prospective, multicenter study. Inflamm Bowel Dis. 2012;18:1006–10.
Stange EF, Travis SP, Vermeire S, Beglinger C, Kupcinkas L, et al. European evidence based consensus on the diagnosis and management of Crohn’s disease: definitions and diagnosis. Gut. 2006;55(Suppl 1):i1–15.
Vogl T, Gharibyan AL, Morozova-Roche LA. Pro-inflammatory S100A8 and S100A9 proteins: self-assembly into multifunctional native and amyloid complexes. Int J Mol Sci. 2012;13:2893–917.
Abraham BP, Kane S. Fecal markers: calprotectin and lactoferrin. Gastroenterol Clin N Am. 2012;41:483–95.
Schoepfer AM, Lewis JD. Serial fecal calprotectin measurements to detect endoscopic recurrence in postoperative Crohn’s disease: is colonoscopic surveillance no longer needed? Gastroenterology. 2015;148:889–92.
Sandborn WJ, Panes J, Zhang H, Yu D, Niezychowski W, Su C. Correlation between concentrations of fecal calprotectin and outcomes of patients with ulcerative colitis in a phase 2 trial. Gastroenterology. 2016;150:96–102.
Schoepfer AM, Beglinger C, Straumann A, Trummler M, Vavricka SR, et al. Fecal calprotectin correlates more closely with the simple endoscopic score for Crohn’s disease (SES-CD) than CRP, blood leukocytes, and the CDAI. Am J Gastroenterol. 2010;105:162–9.
Tibble J, Teahon K, Thjodleifsson B, Roseth A, Sigthorsson G, et al. A simple method for assessing intestinal inflammation in Crohn’s disease. Gut. 2000;47:506–13.
van Rheenen PF, Van de Vijver E, Fidler V. Faecal calprotectin for screening of patients with suspected inflammatory bowel disease: diagnostic meta-analysis. BMJ. 2010;341:c3369.
Wright EK, Kamm MA, De Cruz P, Hamilton AL, Ritchie KJ, et al. Measurement of fecal calprotectin improves monitoring and detection of recurrence of Crohn’s disease after surgery. Gastroenterology. 2015;148:938–47.e1.
Yang Z, Clark N, Park KT. Effectiveness and cost-effectiveness of measuring fecal calprotectin in diagnosis of inflammatory bowel disease in adults and children. Clin Gastroenterol Hepatol. 2014;12:253–62.e2.
Henderson P, Anderson NH, Wilson DC. The diagnostic accuracy of fecal calprotectin during the investigation of suspected pediatric inflammatory bowel disease: a systematic review and meta-analysis. Am J Gastroenterol. 2014;109:637–45.
Tibble JA, Sigthorsson G, Foster R, Forgacs I, Bjarnason I. Use of surrogate markers of inflammation and Rome criteria to distinguish organic from nonorganic intestinal disease. Gastroenterology. 2002;123:450–60.
Van de Vijver E, Schreuder AB, Cnossen WR, Muller Kobold AC, van Rheenen PF, North Netherlands Pediatric IBDC. Safely ruling out inflammatory bowel disease in children and teenagers without referral for endoscopy. Arch Dis Child. 2012;97:1014–8.
Wright EK, Kamm MA, De Cruz P, Hamilton AL, Ritchie KJ, et al. Comparison of fecal inflammatory markers in Crohn’s disease. Inflamm Bowel Dis. 2016;22(5):1086–94.
Kopylov U, Rosenfeld G, Bressler B, Seidman E. Clinical utility of fecal biomarkers for the diagnosis and management of inflammatory bowel disease. Inflamm Bowel Dis. 2014;20:742–56.
RØseth AG, Fagerhol MK, Aadland E, Schjønsby H. Assessment of the neutrophil dominating protein calprotectin in feces: a Methodologic Study. Scand J Gastroenterol. 1992;27:793–8.
Klimczak K, Lykowska-Szuber L, Eder P, Krela-Kazmierczak I, Stawczyk-Eder K, et al. The diagnostic usefulness of fecal lactoferrin in the assessment of Crohn’s disease activity. Eur J Intern Med. 2015;26:623–7.
Roszak D, Galecka M, Cichy W, Szachta P. Determination of faecal inflammatory marker concentration as a noninvasive method of evaluation of pathological activity in children with inflammatory bowel diseases. Adv Med Sci. 2015;60:246–52.
Chung-Faye G, Hayee B, Maestranzi S, Donaldson N, Forgacs I, Sherwood R. Fecal M2-pyruvate kinase (M2-PK): a novel marker of intestinal inflammation. Inflamm Bowel Dis. 2007;13:1374–8.
Ghisoni K, Martins Rde P, Barbeito L, Latini A. Neopterin as a potential cytoprotective brain molecule. J Psychiatr Res. 2015;71:134–9.
Parker DC, Mielke MM, Yu Q, Rosenberg PB, Jain A, et al. Plasma neopterin level as a marker of peripheral immune activation in amnestic mild cognitive impairment and Alzheimer’s disease. Int J Geriatr Psychiatry. 2013;28:149–54.
Widner B, Leblhuber F, Fuchs D. Increased neopterin production and tryptophan degradation in advanced Parkinson’s disease. J Neural Transm (Vienna). 2002;109:181–9.
Wirleitner B, Reider D, Ebner S, Bock G, Widner B, et al. Monocyte-derived dendritic cells release neopterin. J Leukoc Biol. 2002;72:1148–53.
O’Sullivan S, Gilmer JF, Medina C. Matrix metalloproteinases in inflammatory bowel disease: an update. Mediat Inflamm. 2015;2015:964131.
Rodriguez D, Morrison CJ, Overall CM. Matrix metalloproteinases: what do they not do? New substrates and biological roles identified by murine models and proteomics. Biochim Biophys Acta. 2010;1803:39–54.
Sternlicht MD, Werb Z. How matrix metalloproteinases regulate cell behavior. Annu Rev Cell Dev Biol. 2001;17:463–516.
Annahazi A, Molnar T, Farkas K, Rosztoczy A, Izbeki F, et al. Fecal MMP-9: a new noninvasive differential diagnostic and activity marker in ulcerative colitis. Inflamm Bowel Dis. 2013;19:316–20.
Matusiewicz M, Neubauer K, Mierzchala-Pasierb M, Gamian A, Krzystek-Korpacka M. Matrix metalloproteinase-9: its interplay with angiogenic factors in inflammatory bowel diseases. Dis Markers. 2014;2014:643645.
Klebanoff SJ. Myeloperoxidase: friend and foe. J Leukoc Biol. 2005;77:598–625.
Chua F, Laurent GJ. Neutrophil elastase: mediator of extracellular matrix destruction and accumulation. Proc Am Thorac Soc. 2006;3:424–7.
Doring G. The role of neutrophil elastase in chronic inflammation. Am J Respir Crit Care Med. 1994;150:S114–7.
Hara T, Ogawa F, Yanaba K, Iwata Y, Muroi E, et al. Elevated serum concentrations of polymorphonuclear neutrophilic leukocyte elastase in systemic sclerosis: association with pulmonary fibrosis. J Rheumatol. 2009;36:99–105.
Janoff A. Elastase in tissue injury. Annu Rev Med. 1985;36:207–16.
Inokuchi T, Kato J, Hiraoka S, Takashima S, Nakarai A, et al. Fecal immunochemical test versus fecal calprotectin for prediction of mucosal healing in Crohn’s disease. Inflamm Bowel Dis. 2016;22(5):1078–85.
Saito YA, Schoenfeld P, Locke 3rd GR. The epidemiology of irritable bowel syndrome in North America: a systematic review. Am J Gastroenterol. 2002;97:1910–5.
Harvey RF, Salih SY, Read AE. Organic and functional disorders in 2000 gastroenterology outpatients. Lancet. 1983;1:632–4.
Russo MW, Wei JT, Thiny MT, Gangarosa LM, Brown A, et al. Digestive and liver diseases statistics, 2004. Gastroenterology. 2004;126:1448–53.
Nyrop KA, Palsson OS, Levy RL, Von Korff M, Feld AD, et al. Costs of health care for irritable bowel syndrome, chronic constipation, functional diarrhoea and functional abdominal pain. Aliment Pharmacol Ther. 2007;26:237–48.
Halpin SJ, Ford AC. Prevalence of symptoms meeting criteria for irritable bowel syndrome in inflammatory bowel disease: systematic review and meta-analysis. Am J Gastroenterol. 2012;107:1474–82.
Lasson A, Kilander A, Stotzer PO. Diagnostic yield of colonoscopy based on symptoms. Scand J Gastroenterol. 2008;43:356–62.
von Roon AC, Karamountzos L, Purkayastha S, Reese GE, Darzi AW, et al. Diagnostic precision of fecal calprotectin for inflammatory bowel disease and colorectal malignancy. Am J Gastroenterol. 2007;102:803–13.
Park KT, Colletti RB, Rubin DT, Sharma BK, Thompson A, Krueger A. Health insurance paid costs and drivers of costs for patients with Crohn’s disease in the United States. Am J Gastroenterol. 2016;111:15–23.
D’Haens G, Ferrante M, Vermeire S, Baert F, Noman M, et al. Fecal calprotectin is a surrogate marker for endoscopic lesions in inflammatory bowel disease. Inflamm Bowel Dis. 2012;18:2218–24.
Bitton A, Peppercorn MA, Antonioli DA, Niles JL, Shah S, et al. Clinical, biological, and histologic parameters as predictors of relapse in ulcerative colitis. Gastroenterology. 2001;120:13–20.
Schnitzler F, Fidder H, Ferrante M, Noman M, Arijs I, et al. Mucosal healing predicts long-term outcome of maintenance therapy with infliximab in Crohn’s disease. Inflamm Bowel Dis. 2009;15:1295–301.
Peyrin-Biroulet L, Bressenot A, Kampman W. Histologic remission: the ultimate therapeutic goal in ulcerative colitis? Clin Gastroenterol Hepatol. 2014;12:929–34.e2.
Gheorghe C, Cotruta B, Iacob R, Becheanu G, Dumbrava M, Gheorghe L. Endomicroscopy for assessing mucosal healing in patients with ulcerative colitis. J Gastrointestin Liver Dis. 2011;20:423–6.
Boirivant M, Leoni M, Tariciotti D, Fais S, Squarcia O, Pallone F. The clinical significance of serum C reactive protein levels in Crohn’s disease. Results of a prospective longitudinal study. J Clin Gastroenterol. 1988;10:401–5.
Fagan EA, Dyck RF, Maton PN, Hodgson HJ, Chadwick VS, et al. Serum levels of C-reactive protein in Crohn’s disease and ulcerative colitis. Eur J Clin Investig. 1982;12:351–9.
Linskens RK, van Bodegraven AA, Schoorl M, Tuynman HA, Bartels P. Predictive value of inflammatory and coagulation parameters in the course of severe ulcerative colitis. Dig Dis Sci. 2001;46:644–8.
Moran A, Jones A, Asquith P. Laboratory markers of colonoscopic activity in ulcerative colitis and Crohn’s colitis. Scand J Gastroenterol. 1995;30:356–60.
Niederau C, Backmerhoff F, Schumacher B, Niederau C. Inflammatory mediators and acute phase proteins in patients with Crohn’s disease and ulcerative colitis. Hepato-Gastroenterology. 1997;44:90–107.
Nielsen OH, Vainer B, Madsen SM, Seidelin JB, Heegaard NH. Established and emerging biological activity markers of inflammatory bowel disease. Am J Gastroenterol. 2000;95:359–67.
Vermeire S, Van Assche G, Rutgeerts P. C-reactive protein as a marker for inflammatory bowel disease. Inflamm Bowel Dis. 2004;10:661–5.
Schoepfer AM, Trummler M, Seeholzer P, Seibold-Schmid B, Seibold F. Discriminating IBD from IBS: comparison of the test performance of fecal markers, blood leukocytes, CRP, and IBD antibodies. Inflamm Bowel Dis. 2008;14:32–9.
Gomes P, du Boulay C, Smith CL, Holdstock G. Relationship between disease activity indices and colonoscopic findings in patients with colonic inflammatory bowel disease. Gut. 1986;27:92–5.
Schunk K, Kern A, Oberholzer K, Kalden P, Mayer I, et al. Hydro-MRI in Crohn’s disease: appraisal of disease activity. Investig Radiol. 2000;35:431–7.
Costa F, Mumolo MG, Ceccarelli L, Bellini M, Romano MR, et al. Calprotectin is a stronger predictive marker of relapse in ulcerative colitis than in Crohn’s disease. Gut. 2005;54:364–8.
Solem CA, Loftus Jr EV, Tremaine WJ, Harmsen WS, Zinsmeister AR, Sandborn WJ. Correlation of C-reactive protein with clinical, endoscopic, histologic, and radiographic activity in inflammatory bowel disease. Inflamm Bowel Dis. 2005;11:707–12.
Lewis JD. The utility of biomarkers in the diagnosis and therapy of inflammatory bowel disease. Gastroenterology. 2011;140:1817–26.e2.
Lobaton T, Rodriguez-Moranta F, Lopez A, Sanchez E, Rodriguez-Alonso L, Guardiola J. A new rapid quantitative test for fecal calprotectin predicts endoscopic activity in ulcerative colitis. Inflamm Bowel Dis. 2013;19:1034–42.
Zittan E, Kelly OB, Kirsch R, Milgrom R, Burns J, et al. Low fecal calprotectin correlates with histological remission and mucosal healing in ulcerative colitis and colonic Crohn’s disease. Inflamm Bowel Dis. 2016;22(3):623–30.
Langhorst J, Boone J, Lauche R, Rueffer A, Dobos G. Fecal lactoferrin, calprotectin, PMN-elastase, CRP and white blood cell count as an indicator for mucosal healing and clinical course of disease in patients with mild to moderate ulcerative colitis: post HOC analysis of a prospective clinical trial. J Crohns Colitis. 2016;10(7):786–94.
Langholz E, Munkholm P, Davidsen M, Binder V. Course of ulcerative colitis: analysis of changes in disease activity over years. Gastroenterology. 1994;107:3–11.
Riley SA, Mani V, Goodman MJ, Dutt S, Herd ME. Microscopic activity in ulcerative colitis: what does it mean? Gut. 1991;32:174–8.
Limburg PJ, Ahlquist DA, Sandborn WJ, Mahoney DW, Devens ME, et al. Fecal calprotectin levels predict colorectal inflammation among patients with chronic diarrhea referred for colonoscopy. Am J Gastroenterol. 2000;95:2831–7.
Roseth AG, Aadland E, Jahnsen J, Raknerud N. Assessment of disease activity in ulcerative colitis by faecal calprotectin, a novel granulocyte marker protein. Digestion. 1997;58:176–80.
Roseth AG, Schmidt PN, Fagerhol MK. Correlation between faecal excretion of indium-111-labelled granulocytes and calprotectin, a granulocyte marker protein, in patients with inflammatory bowel disease. Scand J Gastroenterol. 1999;34:50–4.
Tibble JA, Sigthorsson G, Bridger S, Fagerhol MK, Bjarnason I. Surrogate markers of intestinal inflammation are predictive of relapse in patients with inflammatory bowel disease. Gastroenterology. 2000;119:15–22.
D’Inca R, Dal Pont E, Di Leo V, Benazzato L, Martinato M, et al. Can calprotectin predict relapse risk in inflammatory bowel disease? Am J Gastroenterol. 2008;103:2007–14.
Gisbert JP, Bermejo F, Perez-Calle JL, Taxonera C, Vera I, et al. Fecal calprotectin and lactoferrin for the prediction of inflammatory bowel disease relapse. Inflamm Bowel Dis. 2009;15:1190–8.
Garcia-Sanchez V, Iglesias-Flores E, Gonzalez R, Gisbert JP, Gallardo-Valverde JM, et al. Does fecal calprotectin predict relapse in patients with Crohn’s disease and ulcerative colitis? J Crohns Colitis. 2010;4:144–52.
Kallel L, Ayadi I, Matri S, Fekih M, Mahmoud NB, et al. Fecal calprotectin is a predictive marker of relapse in Crohn’s disease involving the colon: a prospective study. Eur J Gastroenterol Hepatol. 2010;22:340–5.
De Vos M, Dewit O, D’Haens G, Baert F, Fontaine F, et al. Fast and sharp decrease in calprotectin predicts remission by infliximab in anti-TNF naive patients with ulcerative colitis. J Crohns Colitis. 2012;6:557–62.
Glasziou P, Irwig L, Mant D. Monitoring in chronic disease: a rational approach. BMJ. 2005;330:644–8.
Yamamoto T, Shimoyama T. Can fecal biomarkers detect ileal inflammation in inflammatory bowel disease? Am J Gastroenterol. 2015;110:1370.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Damman, J., Park, K.T. (2017). Fecal Biomarkers in Inflammatory Bowel Disease. In: Mamula, P., Grossman, A., Baldassano, R., Kelsen, J., Markowitz, J. (eds) Pediatric Inflammatory Bowel Disease. Springer, Cham. https://doi.org/10.1007/978-3-319-49215-5_19
Download citation
DOI: https://doi.org/10.1007/978-3-319-49215-5_19
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-49213-1
Online ISBN: 978-3-319-49215-5
eBook Packages: MedicineMedicine (R0)