Abstract
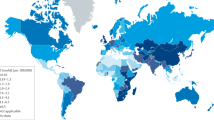
Oesophageal cancer is the third most common gastrointestinal malignancy worldwide. Over the last 40 years, the UK has seen a rise in prevalence and it is now the 13th most common cancer in adults [1]. It has an incidence of 8,300 new cases each year demonstrating a 2:1 preference for males to females. It is reported that 80 % of new cases are diagnosed in patients over 60 years of age [1]. The distribution of tumour subtype varies according to ethnicity with adenocarcinoma favouring Caucasians and squamous cell carcinomas favouring Asian, South American and African populations [2]. Despite advances in multimodality treatment, oesophageal cancer is still devastatingly aggressive with over 65 % of new cases incurable at time of presentation. The disease maintains a 5-year survival of just 15–20 % [3].
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
1.1 Epidemiology
Oesophageal cancer is the third most common gastrointestinal malignancy worldwide. Over the last 40 years, the UK has seen a rise in prevalence and it is now the 13th most common cancer in adults [1]. It has an incidence of 8,300 new cases each year demonstrating a 2:1 preference for males to females. It is reported that 80 % of new cases are diagnosed in patients over 60 years of age [1]. The distribution of tumour subtype varies according to ethnicity with adenocarcinoma favouring Caucasians and squamous cell carcinomas favouring Asian, South American and African populations [2]. Despite advances in multimodality treatment, oesophageal cancer is still devastatingly aggressive with over 65 % of new cases incurable at time of presentation. The disease maintains a 5-year survival of just 15–20 % [3].
There has been a concomitant increase in adenocarcinoma of the gastric cardia, which now accounts for 95 % of all gastric cancers, with the remaining 5 % consisting of a mixture of squamous cell cancers, lymphoma, gastrointestinal stromal tumours and neuroendocrine tumours. Because of the similar gender preference and the affected peak-age group of patients, it has been suggested that adenocarcinomas of the oesophagus and gastric cardia are similar in aetiology [4]. Despite an increase in gastric cardia tumours, the overall incidence of gastric cancer is reducing as a consequence of active health policies to eradicate Helicobacter pylori (H. pylori) infection.
One of the most established causes of oesophageal and gastro-oesophageal junctional cancers is chronic gastro-oesophageal reflux disease (GORD). Barrett’s oesophagus is a recognised premalignant condition involving replacement of normal stratified squamous epithelium within the lower oesophagus with columnar epithelium in response to chronic gastro-oesophageal reflux [4].
Obesity is another recognised risk factor as it predisposes to hiatus hernia and thus acid reflux. The risk of developing a malignancy is 3–6 times greater amongst overweight individuals [5]. Linbald et al. have reported a 67 % increase in the risk of developing oesophageal adenocarcinoma in patients with a BMI > 25 [6]. The ‘Million Women’ study confirmed that 50 % of oesophageal adenocarcinoma cases in postmenopausal women were attributed to obesity [7].
The aetiology of squamous cell carcinoma differs to that of adenocarcinoma of the oesophagus in that it is largely related to poor lifestyle habits, including smoking tobacco, drinking alcohol and a poor diet [8].
1.2 Clinical Presentation/Signs and Symptoms
The main presenting symptom for oesophageal cancer is dysphagia. Unfortunately the symptom frequently presents at a late stage, when the lumen is narrowed to 50–75 % of its normal calibre. By this stage more than 50 % of patients have locally advanced disease [9]. Other symptoms are non-specific and again may go unreported for some time. These include dyspepsia, chest pain, hoarse voice, persistent cough and weight loss.
1.3 Diagnosis
Diagnosis of oesophageal and gastric cancer is made by endoscopy and biopsy. There is a 10 % ‘failure to diagnose’ rate with patients requiring a second endoscopy [10]. The diagnostic yield to detect high-risk premalignant lesions in Barrett’s oesophagus is 100 % when a minimum of six biopsies are taken. Proton-pump inhibitors should be stopped prior to endoscopy as they may heal malignant ulcers and mask their appearances to the endoscopist [4, 11, 12].
1.4 Staging Investigations
The principal imaging modalities for staging are endoscopic ultrasound (EUS), multidetector CT (MDCT) and PET/CT.
1.4.1 Endoscopic Ultrasound
Endoscopic ultrasound (EUS) offers the most accurate method for local staging and is used in patients with localised oesophageal and GOJ tumours who are being considered for radical therapy. It is able to depict the layers of the oesophageal and gastric wall and thus determine the depth of tumour spread through the submucosal layers, allowing identification of patients suitable for local therapy as opposed to surgical resection [13]. The technique also enables fine needle aspiration cytology (FNAC) samples to be taken from local lymph nodes, improving the accuracy of nodal staging [14, 15]
1.4.2 Multidetector CT
MDCT of the chest, abdomen and pelvis is routinely performed as the initial staging investigation. The use of multiplanar reformats in conjunction with axial images has been shown to be particularly useful in accurately distinguishing between T3 and T4 diseases due to the ability to evaluate tumour invasion into surrounding structures [16, 17]. Its primary use however is for detection of metastases. It has a reported 88 % sensitivity and 99 % specificity for detecting liver metastases [18].
1.4.3 PET/CT
PET/CT is now routinely used to refine staging in patients who are considered potentially curable on conventional (MDCT) imaging. It has been shown to detect occult metastases in around 16 % of patients [19]. Recently it has also been reported to be of use in assessing response to neoadjuvant therapy [20].
1.4.4 Other
Laparoscopy is used to assess for peritoneal disease. Direct visualisation of the peritoneal surface can identify 2–3 mm nodules of disease, undetectable on all cross-sectional imaging modalities. It may also detect occult surface deposits on the liver. Its use is advocated in all potentially operable gastric cancer patients and oesophageal patients who have disease extending below the diaphragm.
Currently MRI is reserved for problem-solving, for example, in the characterisation of indeterminate liver lesions [4].
1.5 Staging Classification
The gold standard method for staging utilises a tumour-node metastasis (TNM) classification as defined by the American Joint Committee on Cancer (AJCC) [21]. Cancers of the GOJ and those within the proximal 5 cm of the stomach are staged as oesophageal cancers. Cancers that occur more distally within the stomach are staged as true gastric carcinomas. Specific TNM groups are then classified according to particular cancer stages. These stages provide prognostic information for individual patients. Tables 1.1 and 1.2 give details of the oesophageal staging, and Tables 1.3 and 1.4 below provide detail of the classification for gastric carcinomas.
Key Points
-
Oesophageal cancer is the third most common gastrointestinal malignancy worldwide.
-
Distribution of oesophageal tumour subtype varies according to ethnicity.
-
Oesophageal cancer maintains a 5-year survival of just 15–20 %.
-
Over 65 % of new cases of oesophageal cancer are incurable at time of presentation.
-
Adenocarcinoma of the gastric cardia accounts for 95 % of all gastric cancers.
-
Adenocarcinomas of the oesophagus and gastric cardia are similar in aetiology.
-
One of the most established causes of oesophageal and gastro-oesophageal junctional cancers is chronic gastro-oesophageal reflux disease (GORD).
-
The main presenting symptom for oesophageal cancer is dysphagia.
-
Diagnosis of oesophageal and gastric cancer is made by endoscopy and biopsy.
-
The principal imaging modalities for staging are endoscopic ultrasound (EUS), multidetector CT (MDCT) and PET/CT.
References
Oesophageal Cancer Incidence. URL: http://www.cancerresearchuk.org/cancer-info/cancerstats/types/oesophagus/incidence/uk-oesophageal-cancer-incidence-statistics. 11 June 2014.
Farin K, Wong-Ho C, Christian A, Sanford D. Environmental causes of esophageal cancer. Gastroenterol Clin North Am. 2009;38(1):27–vii.
Pennathur A, Gibson MK, Jobe BA, Luketich JD. Oesophageal carcinoma. Lancet. 2013;381:400–12.
Allum WH, et al. Guidelines for the management of oesophageal and gastric cancer. Gut. 2011;60(11):1449–72.
Cheng KK, Sharp L, McKinney PA, et al. A case control study of oesophageal adenocarcinoma in women: a preventable disease. Br J Cancer. 2000;83:127e32.
Lindblad M, Rodriguez LA, Lagergren J. Body mass, tobacco and alcohol and risk of oesophageal, gastric cardia and gastric non-cardia adenocarcinoma among men and women in a nested case control study. Cancer Causes Control. 2005;16:285e94.
Reeves GK, Pirie K, Beral V, et al. Cancer incidence and mortality in relation to body mass index in the Million Women Study: a cohort study. BMJ. 2007;335:1134.
Zhang HZ, Jin GF, Shen HB. Epidemiologic differences in esophageal cancer between Asian and Western populations. Chin J Cancer. 2012;31(6):281–6. doi:10.5732/cjc.011.10390.PMC3777490.
Koshy M, Esiashvilli N, et al. Multiple management modalities in esophageal cancer: epidemiology, presentation and progression, work-up and surgical approaches. Oncologist. 2004;9(2):137–46.
Yalamarthi S, Witherspoon P, McCole D, et al. Missed diagnoses in patients with upper gastrointestinal cancers. Endoscopy. 2004;36:874e9.
Fitzgerald RC, Saeed IT, Khoo D, et al. Rigorous surveillance protocol increases detection of curable cancers associated with Barrett’s esophagus. Dig Dis Sci. 2001;46:1892e8.
Bramble MG, Suvakovic Z, Hungin AP. Detection of upper gastrointestinal cancer in patients taking antisecretory therapy prior to gastroscopy. Gut. 2000;46:464e7.
Meister T, Heinzow HS, et al. Miniprobe endoscopic ultrasound accurately stages esophageal cancer and guides therapeutic decisions in the era of neoadjuvant therapy: results of a multicenter cohort analysis. Surg Endosc. 2013;27(8):2813–9.
Catalano MF, Sivak Jr MV, Rice T, et al. Endosonographic features predictive of lymph node metastasis. Gastrointest Endosc. 1994;40:442e6.
Vazquez-Sequeiros E, Norton ID, Clain JE, et al. Impact of EUS-guided fine-needle aspiration on lymph node staging in patients with esophageal carcinoma. Gastrointest Endosc. 2001;53:751e7.13. Catalano MF, Sivak MV Jr, Rice T, et al. Endosonographic features predictive of lymph node metastasis. Gastrointest Endosc. 1994;40:442e6.
Bhandari S, Shim CS, Kim JH, et al. Usefulness of three-dimensional, multidetector row CT (virtual gastroscopy and multiplanar reconstruction) in the evaluation of gastric cancer: a comparison with conventional endoscopy, EUS, and histopathology. Gastrointest Endosc. 2004;59:619e26.
Fukuya T, Honda H, Kaneko K, et al. Efficacy of helical CT in T-staging of gastric cancer. J Comput Assist Tomogr. 1997;21:73e81.
Yajima K, et al. Clinical and diagnostic significance of preoperative computed tomography findings of ascites in patients with advanced gastric cancer. Am J Surg. 2006;192(2):185–90.
Purandare NC, et al. Incremental value of 18F-FDG PET/CT in therapeutic decision-making of potentially curable esophageal adenocarcinoma. Nucl Med Commun. 2014;35(8):864–9.
Bruzzi JF, et al. PET/CT of esophageal cancer: its role in clinical management. Radiographics. 2007;27(6):1635–52.
Edge S, et al. AJCC Cancer Staging Manual. 7th ed. New York, NY: Springer, 2010, pp 129–35.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Islam, S., Riddell, A.M. (2016). Introduction and Epidemiology. In: Szyszko, T. (eds) PET/CT in Oesophageal and Gastric Cancer. Clinicians’ Guides to Radionuclide Hybrid Imaging(). Springer, Cham. https://doi.org/10.1007/978-3-319-29240-3_1
Download citation
DOI: https://doi.org/10.1007/978-3-319-29240-3_1
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-29238-0
Online ISBN: 978-3-319-29240-3
eBook Packages: MedicineMedicine (R0)