Abstract
The terms overweight, obese, and severe obesity refer to a clinical continuum. Obesity has attained epidemic proportions and is a major public health issue. It increases both the risk of other chronic health conditions as well as utilization of health care resources. Patients with obesity have traditionally been considered at increased cardiovascular risk. During the past few decades, along with increasing concerns about the magnitude of the problem, great progress in the understanding of the pathogenesis, manifestations, and clinical outcomes of obesity in cardiovascular medicine has been made.
In the past, the Metropolitan Life Insurance Company tables were used to characterise obesity. Since then, several anthropometric measures have been developed to assess adiposity. Nowadays, body mass index and waist circumference are two recommended clinical measures to evaluate increased health hazards associated with obesity.
With the increasing prevalence of obesity, clinicians are now facing a growing population of patients with specific features of clinical presentation, diagnostic challenges, and interventional, medical and surgical management. Features related to obesity relevant to the field of cardiology will be discussed in this chapter.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Obesity
- Atherosclerosis
- Regional adipose tissue
- Cardiometabolic risk
- Cardiac imaging
- Risk stratification
- Acute coronary syndromes
- Coronary revascularisation
Introduction
Obesity is a chronic disease that is increasing in prevalence worldwide. Based upon data collected for the National Health and Nutrition Examination Survey (NHANES) between 2011 and 2012, the prevalence of obesity in adults in the United States is 34.9 % [1] and worldwide overweight/obesity is though to be 36.9 % in men and 38 % in women [2]. Obesity is an independent risk factor for all-cause mortality as well as for cardiovascular disease (CVD) and its management (decrease in adipose tissue depots) lowers the incidence of ischemic heart disease [3–7]. Of importance, obesity shares common pathway with other metabolic-inflammatory processes leading to atherosclerosis thus increasing the incidence of all related atherosclerosis diseases [8].
Classically, obesity is classified by the body mass index (BMI) ratio. This is an easy tool that uses two anthropometric measurements commonly used: 1- weight divided by 2- height in meters squared (kg/m2). This worldwide used index classifies overweight subjects in two categories: (i) overweight (subjects with BMI between 25 and 29.9 kg/m2) and, (ii) obese (BMI ≥ 30 kg/m2). Obese subjects are then graded into three classes according to BMI; (i) 30–34.9 kg/m2, (ii) 35.0–39.9 kg/m2 and, (iii) ≥40 kg/m2. More classes have been added to the list in order to characterize very severe obesity which has been named “super-obese” (≥50 kg/m2) and “super super-obese” (≥60 kg/m2) individuals (Table 8.1a, b) [9]. However, and as detailed later, BMI may not be the best indicator of obesity prognosis and indices of regional distribution of adiposity may better predict cardiovascular risk [10
].
Several large epidemiological studies have reported the link between obesity and CVD. The definition of CVD includes angina, myocardial infarction (MI), heart failure and sudden cardiac death. The Nurses Health Study, that followed more than 100,000 women from United States, showed increased mortality with increased BMI; women with a BMI >32 kg/m2 had a relative risk of death from CVD fourfold those women with BMI <19 kg/m2 [11]. These findings were later supported by the Framingham Heart Study in which men participants were followed during 30 years; the mortality of overweighed men was fourfold those with normal weight [12]. NHANES registry followed more than one million inhabitants of the United States during 14 years and found that high BMI was predictive of cardiovascular death [13]. Obesity, in particular abdominal obesity, is one of the modifiable risk factors influencing the incidence of first MI through all ethnic groups and gender [14]. As the prevalence of obesity has been increasing in the last decades, there is an expected increase in atherosclerotic complications incidence primarily from ischemic heart disease.
Pathophysiology
Atherosclerosis has been shown to begin early in childhood and progresses with increasing age. Accelerated or prompt atherosclerosis is probably the key to understand the fact that obese subjects are more prone to die at younger ages from CVD. This datum is supported by postmortem examinations of young individuals dying from accidental injuries and sudden death. In a series of 243 subjects younger than 40 years who died suddenly, coronary artery disease was responsible for 37 % of deaths in subjects 20–30 years of age and 80 % of subjects dying suddenly at 30–40 years of age [15]. The Pathobiological Determinants of Atherosclerosis in Youth (PDAY) study analyzed coronary arteries from autopsy materials of more than 2800 subjects aged 15–34 who died of external injuries. Subjects with higher BMI were more prone to have higher degree of left anterior descending artery stenosis and intimal and thin cap lesions [16]. A series of 40 autopsy studies of boys aged 13–19 years showed that intima thickness and density of macrophage foam cells in atherosclerotic lesions were correlated with increased visceral fat [17]. These two studies emphasized the importance of the regional distribution of excess adiposity and the link between excess abdominal fat and more complex coronary lesions in the youth. The FATE study and the Dallas Heart Study documented the relationship between surrogates of subclinical atherosclerosis (carotid intimal-media thickness and coronary artery calcium) with abdominal obesity as assessed by the waist-to-hip ratio [18, 19]. Moreover, decreased endothelial dependent vasodilation, a marker of early atherosclerosis, has been shown in obese subjects and was correlated with visceral fat diameter measured by ultrasound [20]. Abdominal fat, and in particular visceral fat measured by magnetic resonance imaging, was correlated with a worse metabolic profile in young and apparently healthy adults [21]. The InterHeart study showed that waist-to-hip ratio was the strongest anthropometric measure associated to MI even when adjusting for gender, age and ethnicity [22]. In addition to its importance as an independent risk factor for coronary atherosclerosis, obesity, defined by BMI, but more specifically abdominal fat depots, usually assessed in clinic by waist circumference, waist-to-hip and/or waist-to-height ratio, promote metabolic abnormalities of numerous cardiovascular risk factors that may accelerate atherosclerotic processes.
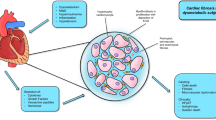
Non-ectopic fat (or subcutaneous fat) appear to be less metabolically deleterious since its primary role is one of energy storage [23]. In contrast, excess abdominal visceral adipose tissue has been associated with known pro-atherosclerotic factors like insulin resistance, increased triglycerides and apolipoprotein B levels, low high-density lipoprotein cholesterol and increased small dense low-density and small dense high density lipoprotein levels, high blood pressure and a prothrombotic state [24]. Therefore, common pathophysiological pathways involving systemic inflammation and lipid metabolism relate obesity to accelerated atherosclerosis. In a state of positive energy balance, free fatty acids and triglycerides are initially stored in adipose tissue. Adipocytes expand and become mature as the pressure of storage increases. Once the normal site of adipose tissue depots becomes saturated and no more storage can be permitted, the adipocytes contain return to the circulation as free fatty acids. This “spill-over” results in an ectopic deposition of fat with preference in lean viscera (liver, kidney), muscle (skeletal muscle, myocardial/epicardial) and also perivascular (Fig. 8.1).
Adipose tissue has not only the role of energy reserve of the human body but also acts as an endocrine organ that controls the deposition of new ectopic fat and its homeostasis through the production of molecules/hormones/adipokines. The deposition of ectopic fat may induce a combined state of inflammation, insulin resistance and adipokines production influencing cardiometabolic risk [25]. Adipokines secreted by adipose tissue are also involved in the modulation of some of the steps promoting atherosclerosis such as endothelial dysfunction, hypercoagulability and dyslipidemia [26]. These cytokines may be classified in two main groups such as beneficial adipokines (adiponectin and omentin) and deleterious adipokines (TNF-α, IL-6, plasminogen activator inhibirot-1, adipocyte fatty acid-binding protein, lipocalin-2, chemerin, leptin, visfatin, vaspin and resistin). The levels of “bad” adipokines are upregulated in obesity, particularly in the presence of abdominal obesity, contributing to the inflammatory profile [27, 28]. These adipokines promote specific actions such as: (i) induce cellular changes in macrophages, that become active while secreting pro-inflammatory factors and, (ii) induce a miss-match in the oxygen supply to ectopic adipose tissue leading to hypoxia that perpetuates the inflammatory state and metabolic disease [29–31] (Fig. 8.1).
Among visceral fat depots, the epicardial adipose tissue surrounds the heart and is in close contact to the coronary vessels. This tissue is involved into myocardial energy supply, thermoregulation and interacts with the cardiac autonomic nervous system influencing the regulation of coronary vessel motion and lumen diameter [32]. Epicardial adipose tissue shows greater inflammatory cell infiltrate (macrophages) than subcutaneous adipose tissue and produces highly atherogenic and inflammatory adipokines in patients with coronary artery disease [33]. As well as the intra-abdominal fat, epicardial adipose tissue is probably involved into subclinical atherosclerosis processes through increased arterial stiffness and increased intima-media thickness [34]. Furthermore, epicardial adipose tissue thickness and volume is correlated with the incidence and severity of coronary artery disease and coronary calcification [35]. Also, epicardial adipose tissue does correlate with the percentage of necrotic plaque tissue, low-density lipoprotein levels and micro-vascular dysfunction even in the absence of symptomatic coronary artery disease [36, 37].
Evaluation and Treatment
Stratification Strategies
Standard treadmill stress test with continuous electrocardiography and non-invasive blood pressure determination may be of limited value in obese patients due to several factors. Firstly, the electrocardiogram may depicts specific alterations in obese patients due to the increased distance between the heart and the electrodes but also due to structural changes secondary to a more horizontal position (false positive Q-waves in the inferior leads that disappear with the standing position), left ventricle (LV) overload and LV enlargement [38, 39]. Secondary, obese patients have impaired aerobic capacity and most fail to achieve the age-predicted heart rate in order to have a valid diagnostic stress test [40, 41]. As well as for elderly patients, modified protocols have been designed to increase exercise time. However, these modified protocols achieve lower metabolic equivalents, lower heart rates and lower pressure-rate products [42]. Stress echocardiography is a useful technique if a good echocardiographic window can be achieved. As in non-obese patients, the presence of detected myocardial ischemia, is an excellent predictor of adverse events [43]. The use of contrast agents may help to improve the acoustic window and increase diagnostic accuracy [44]. Single-photon emission tomography (SPECT) in obese patients has a good sensitivity for the detection of myocardial ischemia. However, photon attenuation through adipose tissue and decreased signal-to-noise ratio despite higher doses may impair its accuracy. In fact, there is conflicting data regarding the prognostic value of a negative SPECT test in obese patients [45]. The positron emission tomography (PET) scan has a high accuracy to detect ischemia in obese patients. A normal rubidium PET imaging ruling out myocardial ischemia is highly predictive of low cardiac events [46]. However, issues concerning the availability of the radiotracer and the ionizing radiation pose important limitations to its widespread use. Coronary computed tomography angiography (CTA) has been suggested for the assessment of patients with intermediate risk of coronary artery disease, those with electrocardiographic abnormalities or those unable to exercise due to its high negative predictive value [47]. However, image quality in obese patients is still suboptimal despite higher radiation doses administered (2–5 mSv with a 120 kV energy) compared to less obese patients [48]. Also, the need to test for ischemia and not only anatomy would make CTA a second line of option for stratification. Nevertheless, new scanners with better resolution and shorter acquisition times may improve the quality of diagnostic images and dual-source energy may add functional information to the anatomical one. A recent international registry has shown that BMI was positively associated with the prevalence of coronary artery disease and increased number of segments with atherosclerotic plaque [49].
Cardiovascular magnetic resonance imaging can assess ventricular function, rest and stress perfusion and viability in a single examination. Relative to alternative techniques, stress cardiovascular magnetic resonance imaging has high spatial and temporal resolution and is not limited by acoustic windows or image acquisition. Scanner with wider-bores (70 cm) and higher capacity weight scanners are progressively available to study severely obese patients. Recent data show that stress cardiovascular magnetic resonance imaging is feasible and the main cause of failure (mainly claustrophobia) is manageable. Cardiovascular magnetic resonance stress ischemia is a powerful predictor of myocardial infarction and cardiovascular death [50].
Treatment Strategies
Invasive early strategies in acute coronary syndromes have shown to improve cardiovascular prognosis [51, 52]. Stratification tools commonly used in clinical cardiology have partially integrated blood markers or anthropometric measurements involved in inflammation and metabolic disorders [53].
Coronary Angiography and Percutaneous Treatment
Obese patients are increasingly being studied in cardiac catheterization laboratories. Maximum weight supported by the new equipment is up to 250 kg and vendors facilitate equipment to comfortably fit the patient within the table range. Radial access is definitely preferred in obese patients for coronary angiography and intervention because of lower bleeding rates, lower vascular complications, faster re-empowerment and mobilization and eventually shorter hospital admissions [54–56]. Echography guided artery puncture may be useful in obese patients who require femoral access. Higher BMI are associated with higher radiation dose during the procedure despite similar procedural times and contrast doses than non-obese patients [57]. Quality image acquisition may be improved with newer X-ray tubes and upgraded image acquisition protocols avoiding non-diagnostic views with high radiation dose. Other studies report higher incidence of contrast induced nephropathy and hemodialysis requirements after coronary angiography in obese patients showing the importance of adequate hydration prior the procedure, use of non-ionic contrasts and saving-contrast protocols [58]. Despite all measures, obesity is still independently associated with a greater in-hospital mortality rate [59].
Obesity was thought to be a protective factor after coronary angioplasty. This was coined the “obesity paradox”. However, recent larger registries show that obese patients have still increased mortality and that longer follow up are required to understand the whole impact of obesity on cardiovascular health [31, 60]. Obese patients treated with bare metal stents had increased rates of binary restenosis, repeated revascularization and major cardiac events at 9-months follow up compared with those treated with first generation drug-eluting stents [61]. Repeated target vessel revascularization and acute stent thrombosis are still increased in obese patients treated with a third generation drug eluting stent [62]. However, in the absence of contraindication of prolonged dual antiplatelet therapy, a drug eluting stent is preferred over a bare metal stent [63]. Intravascular ultrasound and optical coherence tomography may help to size the vessel and assess the immediate result of a percutaneous revascularization procedure if angiography is not optimal. Bioabsorbable scaffolds may confer additional benefits in different subsets including obese patients. Despite the fact that the prevalence of obesity is “epidemic”, there is paucity of data about percutaneous revascularization on this specific group of patients. As an example, obesity does not account for the Syntax or Syntax II Scores to evaluate the risk and major cardiovascular events comparing percutaneous versus surgical treatment [64, 65].
Surgical Revascularization
As obesity is steadily increasing, the need for surgical revascularization in obese patients also increases [66]. Obesity remains a challenge for surgical myocardial revascularization due to the complex management of the pre-procedural conditions, intra-procedural use of drugs and pump and post-procedural complications. There is conflicting evidence about the mortality of obese patients undergoing surgical myocardial revascularization. Initial reports showed increased mortality especially in severely obese patients [67]. However, more recent studies show similar mortality of obese patients compared to non-obese patients [56, 68]. Different registries have still show the association of obesity and several peri-procedural complications such as renal failure, respiratory failure, arrhythmias as atrial fibrillation, deep sternal wound infections and, greater intraoperative transfusion rates [69–72]. Newer surgical approaches, pharmacology and technology have been implemented to minimize the risk of obese patients. Concentration of cases in specialized-high volume centers may increase specialization and decrease complications. Off-pump coronary by-pass surgery shows increased benefit in obese patients compared to on pump procedures [56, 73, 74].
Pharmacotherapy
Anticoagulation and dual antiplatelet therapy has been considered as a cornerstone therapy in patients with acute coronary syndromes and thienopiridines have demonstrated clinical benefit in large randomized controlled trials [75, 76]. Obese patients show increased markers of inflammation including increased baseline platelet activation and variable response to different antiplatelet agents, including increased platelet reactivity while under treatment with aspirin [77, 78]. This pro-aggregation state is even more accentuated in obesity and patients with diabetes [79]. The impact of obesity on thienopyridines remains controversial. As well as with aspirin treatment, greater platelet reactivity under clopidogrel treatment has been shown in patients with increased BMI [56]. Insulin resistance, increased intracellular calcium and oxidative stress may influence the response of obese patients to clopidogrel [80, 81]. The meaning of increased platelet reactivity and its final clinical net effect or clinical relevance has yet to be determined. Patients receiving ticagrelor in the PLATelet inhibition and patient Outcomes (PLATO) trial had no significant difference in the primary endpoint of death from vascular causes, MI or stroke in obese patients compared to normal weight or overweight patients [76]. Recent studies observed the association of greater platelet reactivity under prasugrel treatment and BMI whereas there is no such association with ticagrelor [82, 83]. In addition, prasugrel has poorer action, reflected in higher platelet reactivity, in obese patients with metabolic syndrome [84]. Data on anticoagulation in obese patients and acute coronary syndromes are scarce. A large registry that examined in-hospital complications of severely obese patients who underwent percutaneous intervention showed that obesity was associated with a greater mortality rate than non-obese but also that obesity seemed to protect against major bleeding [59]. There is no standard dosing of unfractioned heparin in patients with weights above 100 kg who undergo both percutaneous and surgical interventions for myocardial ischemia [85]. Heparin dosage is based on body weight assuming that all tissues, both perfused and less-well perfused (as fat), assume the same metabolic rate. This may be the cause of increased bleeding rates during surgical interventions in obese patients [72]. The dosage of heparin is therefore suggested to be calculated through lean body mass in obese patients [86]. During percutaneous intervention, bivalirudin shows benefits only in obese patients who undergo femoral access in terms of transfusion of blood units [56, 87].
Conclusions
Obesity is a highly prevalent chronic disease that is an independent risk factor for cardiovascular mortality and also interacts with other risk factors to accelerate atherosclerosis. Visceral adipose tissue is an active pro-inflammatory organ that combined with other CVD risk factors, increases the prevalence of subclinical coronary artery disease and the incidence of acute coronary syndromes at younger ages. Regional adipose tissue indices allow more accurate stratification of cardiovascular prognosis. Newer technologies allow better study and stratification of obese patients with coronary artery disease. Both percutaneous and surgical revascularization strategies have finally improved to enhance immediate and mid-term results to this increasingly growing and aging population.
References
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011–2012. JAMA. 2014;311:806–14.
Swinburn BA, Sacks G, Hall KD, et al. The global obesity pandemic: shaped by global drivers and local environments. Lancet. 2011;378:804–14.
Flegal KM, Kit BK, Orpana H, Graubard BI. Association of all-cause mortality with overweight and obesity using standard body mass index categories: a systematic review and meta-analysis. JAMA. 2013;309:71–82.
Eckel RH, Krauss RM. American Heart Association call to action: obesity as a major risk factor for coronary heart disease. AHA Nutrition Committee. Circulation. 1998;97:2099–100.
Krauss RM, Winston M, Fletcher BJ, Grundy SM. Obesity : impact on cardiovascular disease. Circulation. 1998;98:1472–6.
Poirier P, Giles TD, Bray GA, et al. Obesity and cardiovascular disease: pathophysiology, evaluation, and effect of weight loss. Arterioscler Thromb Vasc Biol. 2006;26:968–76.
27th Bethesda Conference. Matching the intensity of risk factor management with the hazard for coronary disease events. September 14–15, 1995. J Am Coll Cardiol. 1996;27:957–1047.
Poirier P, Eckel RH. Obesity and cardiovascular disease. Curr Atheroscler Rep. 2002;4:448–53.
Poirier P, Alpert MA, Fleisher LA, et al. Cardiovascular evaluation and management of severely obese patients undergoing surgery: a science advisory from the American Heart Association. Circulation. 2009;120:86–95.
Cornier MA, Despres JP, Davis N, et al. Assessing adiposity: a scientific statement from the American Heart Association. Circulation. 2011;124:1996–2019.
Mark DH. Deaths attributable to obesity. JAMA. 2005;293:1918–9.
Tsai AG, Wadden TA. In the clinic: obesity. Ann Intern Med. 2013;159:ITC3-1–ITC3-15; quiz ITC3-16.
Wildman RP, Muntner P, Reynolds K, et al. The obese without cardiometabolic risk factor clustering and the normal weight with cardiometabolic risk factor clustering: prevalence and correlates of 2 phenotypes among the US population (NHANES 1999–2004). Arch Intern Med. 2008;168:1617–24.
Yusuf S, Hawken S, Ounpuu S, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet. 2004;364:937–52.
Arzamendi D, Benito B, Tizon-Marcos H, et al. Increase in sudden death from coronary artery disease in young adults. Am Heart J. 2011;161:574–80.
McGill Jr HC, McMahan CA, Herderick EE, et al. Obesity accelerates the progression of coronary atherosclerosis in young men. Circulation. 2002;105:2712–8.
Kortelainen ML, Sarkioja T. Visceral fat and coronary pathology in male adolescents. Int J Obes Relat Metab Disord. 2001;25:228–32.
Yan RT, Yan AT, Anderson TJ, et al. The differential association between various anthropometric indices of obesity and subclinical atherosclerosis. Atherosclerosis. 2009;207:232–8.
See R, Abdullah SM, McGuire DK, et al. The association of differing measures of overweight and obesity with prevalent atherosclerosis: the Dallas Heart Study. J Am Coll Cardiol. 2007;50:752–9.
Sturm W, Sandhofer A, Engl J, et al. Influence of visceral obesity and liver fat on vascular structure and function in obese subjects. Obesity. 2009;17:1783–8.
De Larochelliere E, Cote J, Gilbert G, et al. Visceral/epicardial adiposity in nonobese and apparently healthy young adults: association with the cardiometabolic profile. Atherosclerosis. 2014;234:23–9.
Yusuf S, Hawken S, Ounpuu S, et al. Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet. 2005;366:1640–9.
Despres JP. Body fat distribution and risk of cardiovascular disease: an update. Circulation. 2012;126:1301–13.
Emerging Risk Factors C, Wormser D, Kaptoge S, et al. Separate and combined associations of body-mass index and abdominal adiposity with cardiovascular disease: collaborative analysis of 58 prospective studies. Lancet. 2011;377:1085–95.
Mathieu P, Poirier P, Pibarot P, Lemieux I, Despres JP. Visceral obesity: the link among inflammation, hypertension, and cardiovascular disease. Hypertension. 2009;53:577–84.
Van Gaal LF, Mertens IL, De Block CE. Mechanisms linking obesity with cardiovascular disease. Nature. 2006;444:875–80.
Rocha VZ, Libby P. Obesity, inflammation, and atherosclerosis. Nat Rev Cardiol. 2009;6:399–409.
Visser M, Bouter LM, McQuillan GM, Wener MH, Harris TB. Elevated C-reactive protein levels in overweight and obese adults. JAMA. 1999;282:2131–5.
Rutkowski JM, Davis KE, Scherer PE. Mechanisms of obesity and related pathologies: the macro- and microcirculation of adipose tissue. FEBS J. 2009;276:5738–46.
Van de Voorde J, Pauwels B, Boydens C, Decaluwe K. Adipocytokines in relation to cardiovascular disease. Metabolism. 2013;62:1513–21.
Bastien M, Poirier P, Lemieux I, Despres JP. Overview of epidemiology and contribution of obesity to cardiovascular disease. Prog Cardiovasc Dis. 2014;56:369–81.
Wronska A, Kmiec Z. Structural and biochemical characteristics of various white adipose tissue depots. Acta Physiol (Oxf). 2012;205:194–208.
Baker AR, Silva NF, Quinn DW, et al. Human epicardial adipose tissue expresses a pathogenic profile of adipocytokines in patients with cardiovascular disease. Cardiovasc Diabetol. 2006;5:1.
Natale F, Tedesco MA, Mocerino R, et al. Visceral adiposity and arterial stiffness: echocardiographic epicardial fat thickness reflects, better than waist circumference, carotid arterial stiffness in a large population of hypertensives. Eur J Echocardiogr. 2009;10:549–55.
Huang G, Wang D, Zeb I, et al. Intra-thoracic fat, cardiometabolic risk factors, and subclinical cardiovascular disease in healthy, recently menopausal women screened for the Kronos Early Estrogen Prevention Study (KEEPS). Atherosclerosis. 2012;221:198–205.
Yamashita K, Yamamoto MH, Ebara S, et al. Association between increased epicardial adipose tissue volume and coronary plaque composition. Heart Vessels. 2014;29:569–77.
Alam MS, Green R, de Kemp R, Beanlands RS, Chow BJ. Epicardial adipose tissue thickness as a predictor of impaired microvascular function in patients with non-obstructive coronary artery disease. J Nucl Cardiol. 2013;20:804–12.
Poirier P, Giles TD, Bray GA, et al. Obesity and cardiovascular disease: pathophysiology, evaluation, and effect of weight loss: an update of the 1997 American Heart Association Scientific Statement on Obesity and Heart Disease from the Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Circulation. 2006;113:898–918.
Alpert MA, Terry BE, Cohen MV, Fan TM, Painter JA, Massey CV. The electrocardiogram in morbid obesity. Am J Cardiol. 2000;85:908–10, A10.
Gondoni LA, Titon AM, Nibbio F, Augello G, Caetani G, Liuzzi A. Heart rate behavior during an exercise stress test in obese patients. Nutr Metab Cardiovasc Dis. 2009;19:170–6.
Lear SA, Brozic A, Myers JN, Ignaszewski A. Exercise stress testing. An overview of current guidelines. Sports Med. 1999;27:285–312.
Bires AM, Lawson D, Wasser TE, Raber-Baer D. Comparison of Bruce treadmill exercise test protocols: is ramped Bruce equal or superior to standard bruce in producing clinically valid studies for patients presenting for evaluation of cardiac ischemia or arrhythmia with body mass index equal to or greater than 30? J Nucl Med Technol. 2013;41:274–8.
Supariwala A, Makani H, Kahan J, et al. Feasibility and prognostic value of stress echocardiography in obese, morbidly obese, and super obese patients referred for bariatric surgery. Echocardiography. 2014;31:879–85.
Colonna P, Cadeddu C, Chen L, Iliceto S. Clinical applications of contrast echocardiography. Am Heart J. 2001;141:S36–44.
Korbee RS, Boiten HJ, Ottenhof M, Valkema R, van Domburg RT, Schinkel AF. What is the value of stress (99 m)Tc-tetrofosmin myocardial perfusion imaging for the assessment of very long-term outcome in obese patients? J Nucl Cardiol. 2013;20:227–33.
Chow BJ, Dorbala S, Di Carli MF, et al. Prognostic value of PET myocardial perfusion imaging in obese patients. JACC Cardiovasc Imaging. 2014;7:278–87.
Hendel RC, Patel MR, Kramer CM, et al. ACCF/ACR/SCCT/SCMR/ASNC/NASCI/SCAI/SIR 2006 appropriateness criteria for cardiac computed tomography and cardiac magnetic resonance imaging: a report of the American College of Cardiology Foundation Quality Strategic Directions Committee Appropriateness Criteria Working Group, American College of Radiology, Society of Cardiovascular Computed Tomography, Society for Cardiovascular Magnetic Resonance, American Society of Nuclear Cardiology, North American Society for Cardiac Imaging, Society for Cardiovascular Angiography and Interventions, and Society of Interventional Radiology. J Am Coll Cardiol. 2006;48:1475–97.
Lee AM, Engel LC, Hui GC, et al. Coronary computed tomography angiography at 140 kV versus 120 kV: assessment of image quality and radiation exposure in overweight and moderately obese patients. Acta Radiol. 2014;55:554–62.
Labounty TM, Gomez MJ, Achenbach S, et al. Body mass index and the prevalence, severity, and risk of coronary artery disease: an international multicentre study of 13,874 patients. Eur Heart J Cardiovasc Imaging. 2013;14:456–63.
Shah RV, Heydari B, Coelho-Filho O, et al. Vasodilator stress perfusion CMR imaging is feasible and prognostic in obese patients. JACC Cardiovasc Imaging. 2014;7:462–72.
Cannon CP, Weintraub WS, Demopoulos LA, et al. Comparison of early invasive and conservative strategies in patients with unstable coronary syndromes treated with the glycoprotein IIb/IIIa inhibitor tirofiban. N Engl J Med. 2001;344:1879–87.
Morrow DA, Cannon CP, Rifai N, et al. Ability of minor elevations of troponins I and T to predict benefit from an early invasive strategy in patients with unstable angina and non-ST elevation myocardial infarction: results from a randomized trial. JAMA. 2001;286:2405–12.
Fox KA, Goodman SG, Klein W, et al. Management of acute coronary syndromes. Variations in practice and outcome; findings from the Global Registry of Acute Coronary Events (GRACE). Eur Heart J. 2002;23:1177–89.
Benamer H, Louvard Y, Sanmartin M, et al. A multicentre comparison of transradial and transfemoral approaches for coronary angiography and PTCA in obese patients: the TROP registry. EuroIntervention. 2007;3:327–32.
Hibbert B, Simard T, Wilson KR, et al. Transradial versus transfemoral artery approach for coronary angiography and percutaneous coronary intervention in the extremely obese. JACC Cardiovasc Interv. 2012;5:819–26.
Garcia-Labbe D, Ruka E, Bertrand OF, Voisine P, Costerousse O, Poirier P. Obesity and coronary artery disease: evaluation and treatment. Can J Cardiol. 2015;31:184–94.
Shah A, Das P, Subkovas E, Buch AN, Rees M, Bellamy C. Radiation dose during coronary angiogram: relation to body mass index. Heart Lung Circ. 2015;24:21–5.
Buschur ME, Smith D, Share D, et al. The burgeoning epidemic of morbid obesity in patients undergoing percutaneous coronary intervention: insight from the Blue Cross Blue Shield of Michigan Cardiovascular Consortium. J Am Coll Cardiol. 2013;62:685–91.
Payvar S, Kim S, Rao SV, et al. In-hospital outcomes of percutaneous coronary interventions in extremely obese and normal-weight patients: findings from the NCDR (National Cardiovascular Data Registry). J Am Coll Cardiol. 2013;62:692–6.
Lin GM, Li YH, Lin CL, Wang JH, Han CL. Relation of body mass index to bleeding events among patients with percutaneous coronary intervention: a meta-analysis. Int J Cardiol. 2013;168:4831–5.
Nikolsky E, Kosinski E, Mishkel GJ, et al. Impact of obesity on revascularization and restenosis rates after bare-metal and drug-eluting stent implantation (from the TAXUS-IV trial). Am J Cardiol. 2005;95:709–15.
Sarno G, Garg S, Onuma Y, et al. The impact of body mass index on the one year outcomes of patients treated by percutaneous coronary intervention with Biolimus- and Sirolimus-eluting stents (from the LEADERS trial). Am J Cardiol. 2010;105:475–9.
Kolh P, Windecker S. ESC/EACTS myocardial revascularization guidelines 2014. Eur Heart J. 2014;35:3235–6.
Sianos G, Morel MA, Kappetein AP, et al. The SYNTAX Score: an angiographic tool grading the complexity of coronary artery disease. EuroIntervention. 2005;1:219–27.
Farooq V, van Klaveren D, Steyerberg EW, et al. Anatomical and clinical characteristics to guide decision making between coronary artery bypass surgery and percutaneous coronary intervention for individual patients: development and validation of SYNTAX score II. Lancet. 2013;381:639–50.
Twells LK, Gregory DM, Reddigan J, Midodzi WK. Current and predicted prevalence of obesity in Canada: a trend analysis. CMAJ Open. 2014;2:E18–26.
Prabhakar G, Haan CK, Peterson ED, Coombs LP, Cruzzavala JL, Murray GF. The risks of moderate and extreme obesity for coronary artery bypass grafting outcomes: a study from the Society of Thoracic Surgeons’ database. Ann Thorac Surg. 2002;74:1125–30; discussion 1130–1.
Benedetto U, Danese C, Codispoti M. Obesity paradox in coronary artery bypass grafting: myth or reality? J Thorac Cardiovasc Surg. 2014;147:1517–23.
Hernandez AV, Kaw R, Pasupuleti V, et al. Association between obesity and postoperative atrial fibrillation in patients undergoing cardiac operations: a systematic review and meta-analysis. Ann Thorac Surg. 2013;96:1104–16.
Kelly R, Buth KJ, Legare JF. Bilateral internal thoracic artery grafting is superior to other forms of multiple arterial grafting in providing survival benefit after coronary bypass surgery. J Thorac Cardiovasc Surg. 2012;144:1408–15.
Virani SS, Nambi V, Lee VV, et al. Obesity: an independent predictor of in-hospital postoperative renal insufficiency among patients undergoing cardiac surgery? Texas Heart Institute journal/from the Texas Heart Institute of St Luke’s Episcopal Hospital. Tex Child Hosp. 2009;36:540–5.
Nolan HR, Davenport DL, Ramaiah C. BMI is an independent preoperative predictor of intraoperative transfusion and postoperative chest-tube output. Int J Angiol. 2013;22:31–6.
Lamy A, Devereaux PJ, Yusuf S. Off-pump or on-pump coronary-artery bypass grafting. N Engl J Med. 2013;369:196.
Pullan M, Kirmani BH, Conley T, et al. Should obese patients undergo on- or off-pump coronary artery bypass grafting? Eur J Cardiothorac Surg. 2015;47:309–15.
Wiviott SD, Braunwald E, McCabe CH, et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2007;357:2001–15.
Wallentin L, Becker RC, Budaj A, et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2009;361:1045–57.
Badimon L, Hernandez Vera R, Padro T, Vilahur G. Antithrombotic therapy in obesity. Thromb Haemost. 2013;110:681–8.
Salama MM, Morad AR, Saleh MA, Sabri NA, Zaki MM, ElSafady LA. Resistance to low-dose aspirin therapy among patients with acute coronary syndrome in relation to associated risk factors. J Clin Pharm Ther. 2012;37:630–6.
Cohen HW, Crandall JP, Hailpern SM, Billett HH. Aspirin resistance associated with HbA1c and obesity in diabetic patients. J Diabetes Complications. 2008;22:224–8.
Angiolillo DJ, Fernandez-Ortiz A, Bernardo E, et al. Platelet aggregation according to body mass index in patients undergoing coronary stenting: should clopidogrel loading-dose be weight adjusted? J Invasive Cardiol. 2004;16:169–74.
Anfossi G, Russo I, Trovati M. Platelet dysfunction in central obesity. Nutr Metab Cardiovasc Dis. 2009;19:440–9.
Darlington A, Tello-Montoliu A, Rollini F, et al. Pharmacodynamic effects of standard dose prasugrel versus high dose clopidogrel in non-diabetic obese patients with coronary artery disease. Thromb Haemost. 2014;111:258–65.
Mayer K, Orban M, Bernlochner I, et al. Predictors of antiplatelet response to prasugrel during maintenance treatment. Platelets. 2015;26:53–8.
Deharo P, Pankert M, Bonnet G, et al. Body mass index has no impact on platelet inhibition induced by ticagrelor after acute coronary syndrome, conversely to prasugrel. Int J Cardiol. 2014;176:1200–2.
Joncas SX, Poirier P, Ardilouze JL, Carrier N, Fayad T, Farand P. Delayed efficient anticoagulation with heparin in patients with a weight of 110 kg and more treated for acute coronary syndrome. Obesity. 2013;21:1753–8.
Baker MS, Skoyles JR, Shajar FM, Skinner H, Richens D, Mitchell IM. Can lean body mass be used to reduce the dose of heparin and protamine for obese patients undergoing cardiopulmonary bypass? J Extra Corpor Technol. 2005;37:153–6.
Delhaye C, Wakabayashi K, Maluenda G, et al. Safety and efficacy of bivalirudin for percutaneous coronary intervention with rotational atherectomy. J Interv Cardiol. 2010;23:223–9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Tizón-Marcos, H., Poirier, P. (2016). Obesity and Coronary Heart Disease. In: Ahmad, S., Imam, S. (eds) Obesity. Springer, Cham. https://doi.org/10.1007/978-3-319-19821-7_8
Download citation
DOI: https://doi.org/10.1007/978-3-319-19821-7_8
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-19820-0
Online ISBN: 978-3-319-19821-7
eBook Packages: MedicineMedicine (R0)