Abstract
Ligamentous ankle injuries remain one of the most common injuries sustained by athletes. Syndesmotic, often termed high ankle, sprains are being diagnosed more frequently due to a heightened awareness and improved diagnostic techniques. These injuries result in pain, disability, and a significant delay in return to play. Most operative syndesmotic injuries can be diagnosed on plain radiographs, including stress views; however, ultrasound, CT, and MRI have improved the detection of more subtle injuries. Arthroscopic evaluation can be used to confirm the diagnosis while assessing other intra-articular structures. There has been an abundance of recent research exploring the treatment of syndesmotic injuries in athletes, focusing on surgical intervention and rehabilitation protocols. The literature remains conflicted regarding return to play in athletes.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
It is well-established that ankle sprains and fractures are among the most common sports-related injuries [1]. Isolated syndesmotic disruptions without fracture occur more commonly in athletes than non-athletes [2]. Syndesmotic injuries comprise 1–18 % of ankle sprains but are probably underreported since the diagnosis is not always made on initial physical examination and non-weight-bearing radiographs [3–5]. Return to play after syndesmotic injury can take twice as long when compared to isolated lateral ankle ligamentous injury [6]. Return to play after syndesmotic disruption is dependent on the sport, degree of injury, and variable time to healing for each injury [7]. In addition to the short-term disability caused by these injuries, chronic ankle dysfunction can persist for months following the injury [8, 9]. Unrecognized injuries that are not properly treated can result in chronic ankle instability and post-traumatic ankle arthritis [10].
Syndesmotic disruption can occur in isolation or with concomitant adjacent bony, cartilaginous, or ligamentous injuries. Therefore, the importance of a focused and comprehensive exam of the entire foot and ankle cannot be overemphasized [9]. Considerable discrepancies exist in the literature regarding the reporting of these injuries, the use of advanced imaging and arthroscopy to aid in diagnosis, and the appropriate treatment for different degrees of injury [2]. The diagnosis and management of these injuries, especially in elite athletes, remains controversial since there is a lack of level I evidence surrounding this topic. This chapter will review relevant anatomy, etiology, pathophysiology, symptomatology, diagnosis, treatment, rehabilitation, and prevention, and summarize the highest level of existing evidence.
Etiology and Pathomechanism
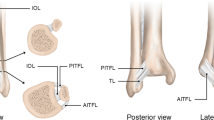
The distal tibiofibular syndesmosis is located between the convex distal fibula and the concave incisura fibularis of the tibia. A synovial-lined joint cavity, contiguous with the ankle joint, extends proximally 12–15 mm and includes articulating facets between the tibia and fibula 75 % of the time [11]. The syndesmosis is stabilized by the anterior inferior tibiofibular ligament (AITFL), interosseous ligament (IOL), and posterior ligamentous complex consisting of the posterior inferior tibiofibular ligament (PITFL) and fibrocartilaginous inferior transverse ligament (ITL) [12]. The posterior ligaments are confluent with the posterior ankle capsule. The AITFL, PITFL, and IOL limit fibular external rotation, posterior translation, and lateral translation, respectively [13]. Within the AITFL, the inferior band is most important for stability.
Normal fibular motion within the syndesmosis, albeit slight in comparison to other joints, is important in preserving ankle joint congruity [14, 15]. When the ankle is dorsiflexed, the fibula externally rotates and migrates proximally and posterolaterally to accommodate the wider anterior talar done [16]. With plantarflexion, the fibula internally rotates and translates distally and anteromedially. External rotation of the foot results in fibular external rotation and posteromedial translation [17].
The syndesmosis functions synergistically with the deltoid ligament complex to maintain stability and congruency of the ankle mortise. Congruity of the ankle joint is essential in order to maintain normal contact characteristics and thereby prevent the development of post-traumatic arthritis [18, 19]. For this reason, syndesmotic instability and malreduction is associated with poor functional outcome and secondary arthritis.
Together with the ITL, the PITFL provides 42 % of syndesmotic stability, compared to 35 % for the AITFL and 22 % for the IOL [20]. When all syndesmotic ligaments are sectioned, fibular motion relative to the tibia increases 8.8 mm in the sagittal plane and 1.5 mm in the coronal plane with stress examination [21]. In contrast, disruption of the AITFL alone results in only 0.5 mm of translation in the coronal and sagittal planes. With sectioning of the syndesmosis 4–6 cm proximal to the ankle joint with a concomitant deep deltoid ligament rupture can result in tibiotalar dislocation when the ankle is loaded in 20° of dorsiflexion [22].
Syndesmotic injuries most often result from an external rotation force applied to a hyperdorsiflexed ankle while the foot is planted [12]. This mechanism causes the fibula to externally rotate while translating posteriorly and laterally, resulting in rupture of the AITFL first, followed by the deep deltoid ligament, IOL, and lastly PITFL [23]. Most syndesmotic injuries involve rupture of only the AITFL and IOL [2]. Other described mechanisms of syndesmotic injury include inversion, inversion with external rotation, and eversion [24, 25]. More significant syndesmotic injuries are more likely to occur with external rotation compared with other mechanisms. Syndesmotic widening of at least 2 mm more than the contralateral ankle has been shown to correlate with injury to two or more syndesmotic ligaments [26].
History and Physical Examination
Athletic syndesmotic injuries occur most commonly in high-impact sports, including ice hockey and football [6, 27]. An attempt to define the mechanism of injury should be made while taking the history. Treatment varies dramatically between acute (less than 3 weeks) and chronic (greater than 3 months) injuries so it is important to establish the date of injury [28]. One should inquire about a history of previous injury or treatment. As with all foot and ankle injuries, the patient should be asked to localize the area of maximum pain. Patients may report a sense of ankle instability.
Physical examination should begin with inspection for swelling, ecchymosis and deformity. In addition, it should focus reproduction of pain along the anterolateral border of the leg during ankle dorsiflexion, instability testing, and pain with weight-bearing or during push-off [29]. Tenderness localized to the AITFL is non-specific since this can occur with many other ankle injuries in the acute period [30]. Forty percent of patients with ATFL rupture resulting from a supination injury had tenderness over the AITFL without rupture of this ligament [30].
Multiple specific stress tests have been designed to assess syndesmotic stability, including the squeeze test, external rotation stress test, Cotton test, crossed-leg test and fibula-translation test [4, 26, 29, 31]. The squeeze test involves compression of the tibia and fibula proximally in the calf and is considered positive when this causes pain at the ankle joint. The external rotation stress test involves an external rotation stress applied to the foot while the ankle is dorsiflexed, with reproducible pain signifying a positive result. This test has been shown to have the lowest inter-observer error and highest sensitivity [32]. A positive Cotton test occurs with pain when the talus is translated laterally within the mortise. The fibula-translation test is performed by stabilizing the tibia and trying to displace the fibula anteriorly or posteriorly. A positive crossed-leg test occurs when pain is elicited by pushing the affected fibula downwards against the knee.
Physical examination alone has been shown to detect only 75 % of injuries [32]. With MRI-confirmed syndesmotic injuries, the external rotation stress test had a sensitivity of 20 % and specificity of 84.8 % versus 30 and 93.5 % for the squeeze test [33]. While the presence of a positive test should heighten suspicion for a syndesmotic injury, no physical exam maneuver has been shown to reliably predict the presence or degree of syndesmotic injury and therefore imaging studies are necessary [34].
Imaging
Initial imaging for evaluation of syndesmotic injuries should include anteroposterior (AP), mortise, and lateral radiographs of the affected ankle. If possible, weight-bearing radiographs are beneficial in identifying more subtle injuries but are not necessary when incongruence of the mortise is evident on non-weight-bearing views. An increase in the medial clear space between the medial malleolus and talus can occur with a combined syndesmotic and deltoid disruption (Fig. 29.1) [33]. In the case of supination-external rotation (SER) IV injuries, the integrity of the syndesmosis can only be assessed after anatomic fixation of the fibula (Fig. 29.2). While it is well-established that syndesmotic disruption is more common with pronation-type (Weber C) fibula fractures, it occurs in 20–30 % of supination-type (Weber B) fibula fractures [35, 36]. A tibiofibular clear space 1 cm proximal to the tibial plafond of greater than 6 mm on AP and mortise radiographs indicates a syndesmotic injury [37]. Since the appearance of the tibiofibular clear space does not change over an arc of 5° of external rotation to 25° of internal rotation, it has been demonstrated to be the more reliable radiographic measurement [38].
In the case of subtle injuries (Fig. 29.3a, b), contralateral comparison views can be helpful since a difference in tibiofibular clear space by at least 2 mm indicates syndesmotic injury. Fluoroscopic stress evaluation is beneficial but has a high false-negative rate in low-grade injuries and may not detect partial rupture of the AITFL and IOL [39]. In fact, it has been shown that malrotation of as much as 30° of external rotation can occur if relying on intraoperative fluoroscopy alone [40].
CT scan with fine axial cuts is most useful to evaluate the location of the distal fibula in relation to the incisura fibularis of the tibia [41]. This is especially true in cases of tibial AITFL and PITFL avulsion fractures, which can occur in as many as 50 % of syndesmotic injuries [42]. Again, with more subtle injuries, the contralateral ankle should be included in the field of view to allow comparison. While CT has its advantages, one must remember that it remains a static test, unless weight-bearing CT is used. Further study is necessary to explore the utility of weight-bearing CT.
MRI is beneficial in identifying high and low-grade syndesmotic injuries and has high inter-observer reliability [43]. It has been shown to have 100 % sensitivity and 93 % specificity for AITFL injuries and 100 % sensitivity and specificity for PITFL ruptures in cases of high-grade syndesmotic injury [44]. Since MRI, like CT, is not a dynamic test and therefore is not ideal for detecting syndesmotic instability in low-grade injuries.
Ultrasound is a quick, safe, and inexpensive imaging modality that allows dynamic testing. It can depict widening of the tibiofibular clear space and AITFL disruption when applying external rotation stress [45]. One must be cognizant that ultrasound is highly operator-dependent and diagnostic utility is likely to vary based on the skill and experience of the ultrasonographer. Compared to MRI, ultrasound is not effective in detecting osteochondral lesions and bone bruising, which are present in 28 % of cases [46].
If imaging modalities fail to provide a conclusive diagnosis, ankle arthroscopy can be used to directly visualize the syndesmosis and articular cartilage [47]. Although invasive, it can have both diagnostic and therapeutic utility. It is superior to any imaging modality in terms of its ability to definitively diagnose syndesmotic and osteochondral injuries, and allows dynamic instability to be surgically treated in the same setting [48].
Classification
Syndesmotic injuries can be classified based on physical examination as described by the West Point Ankle grading system [8]. Grade I (low-grade) injuries include mild sprains and AITFL ruptures without ankle instability. Grade II injuries involve rupture of the AITFL and IOL with slight instability. Grade III (high-grade) injuries are grossly unstable and result from disruption of all syndesmotic ligaments. It is difficult to differentiate between grade I and II injuries based on physical examination alone, so it is necessary to employ advanced imaging or arthroscopy to make this distinction.
Edwards and DeLee developed another classification of acute syndesmotic injury without fracture [49]. First, they broadly defined these injuries as sprains without diastasis, sprains with frank diastasis (evident on initial radiographs), and sprains with latent diastasis (diagnosed only on stress radiographs). Second, they categorized injuries as type I, lateral fibular translation without fracture; type II, lateral fibular translation due to plastic deformation of the fibula; type III, posterior subluxation or dislocation of the fibula; and type IV, proximal dislocation of the talus causing divergence of the distal tibia and fibula. Currently, no classification system exists that clearly defines treatment guidelines, injury severity, or prognosis.
Conservative Treatment
Nonoperative treatment is indicated for stable grade I syndesmotic injuries. This involves rest and immobilization followed by a progressive rehabilitation program consisting of stretching, strengthening, and proprioceptive exercises [50]. After a 1-week period of protected weight-bearing in a cast or CAM boot, progression to full weight-bearing should occur over the following week. Additionally, active-assisted ankle range of motion exercises and light proprioceptive training should commence with the guidance of a physical therapist. During the following week (14–21 days post-injury), athletes may begin strength training and sports-specific exercises. Return to play is permitted when the athlete is able to single-leg hop for at least 30 s (or 15 repetitions) without pain, which usually occurs between 4 and 6 weeks post-injury [2].
The appropriate initial treatment of grade II injuries is nonoperative. There is a spectrum of injury within this grade and patients exhibit variable recovery times. In patients with persistent symptoms and protracted rehabilitation course, dynamic stress examination as well as arthroscopic evaluation can be helpful to evaluate ligamentous stability. If dynamic testing reveals diastasis of more than 2 mm, surgical intervention should be considered [26]. Although conservative management leads to good to excellent outcomes in 86–100 % of patients, the resultant prolonged rehabilitation course (average return to play of 13.4 weeks) may be problematic, particularly in elite athletes [8, 29, 34]. Not surprisingly, patient outcomes are inferior when tibiofibular diastasis persists and/or calcification develops above the syndesmotic ligaments [51].
Operative Treatment
Reduction Technique
There is some debate as to the appropriate clamp position for reduction of syndesmotic injuries. While it seems logical that an oblique clamp position should be used since the fibula is posterior in relation to the tibia, a cadaver study demonstrated that clamp orientation along the neutral anatomic axis yields an optimal reduction[52]. With regard to ankle position during clamp reduction and screw placement, it has been postulated that the ankle should be dorsiflexed to prevent overtightening of the syndesmosis since the talar dome is wider anteriorly. Yet, no difference in ankle range of motion was noted in a recent study between screws tightened in plantarflexion and dorsiflexion [53]. In fact, excessive ankle dorsiflexion can posteriorly displace the fibula out of the incisura. Therefore, we recommend clamp and screw tightening with the ankle in resting position to prevent malreduction. It is prudent to have a low threshold to dissect anteriorly to the fibula to achieve an anatomic reduction by direct visualization. Some surgeons advocate manual reduction of the syndesmosis to avoid overcompression and facilitate an anatomic reduction. The use of a smaller clamp may result in fibular translation.
Radiographic Assessment of Syndesmotic Reduction
It is advisable to obtain comparison fluoroscopic AP and lateral views of the contralateral ankle to ascertain the normal relationship of the patient’s distal tibia and fibula. Even using direct visualization and fluoroscopic guidance, anatomic reduction of the syndesmosis can be difficult. In patients with associated malleolar fractures, high rates of syndesmotic malreduction have been observed on postoperative imaging, up to 52 % using CT [54–57]. The distance between the fibula and posterior facet of the incisura was greater in 77 % of malreductions, representing iatrogenic internal rotation or anterior translation of the fibula [56]. Syndesmotic widening beyond 1.5 mm after open reduction internal fixation results in poor functional outcomes [54, 58].
In a case report, intraoperative O-arm 3-D cone-beam CT was found to be fast and effective in assessing fibular length and rotation as well as mortise congruency [59]. Another study reported the use of 3-D imaging with mobilized C-arms in 251 syndesmotic injuries [60]. This technology identified malreductions in 33 % of cases that were corrected during the same procedure. Although intraoperative 3-D imaging is appealing, it is too expensive for many institutions and it is questionable as to whether its benefit outweighs the risk of increased radiation exposure and longer surgery duration.
Diagnostic Arthroscopy
Stress radiographs and MRI have been found to be less effective than direct arthroscopic visualization in demonstrating the true degree of syndesmotic disruption (Fig. 29.3) [44, 48]. While MRI is very sensitive for detecting syndesmotic injuries with flexor hallucis longus edema being a clue to posterior tibiofibular ligament injury [61] and CT can detect minor (2–3 mm) diastasis [41], neither advanced imaging modality is predictive of syndesmotic instability. In addition, many patients with syndesmotic injury are at high risk of associated traumatic talar osteochondral lesions which can be managed arthroscopically at the time of syndesmotic evaluation [62]. Syndesmotic injuries can vary widely in the degree of severity, with some patients being appropriate candidates for non-operative management and others requiring arthroscopic debridement and/or ORIF [10].
Arthroscopy can be a particularly valuable diagnostic tool in the setting of a subtle syndesmotic injury with negative radiographs, positive MRI for edema, and a protracted recovery course with vague pain. In these situations, an exam under anesthesia is performed, the syndesmosis is probed under direct arthroscopic visualization, and distal tibiofibular instability is evaluated while performing an external rotation stress test (Fig. 29.4a, b). In a cadaveric study, the distance between the tibia and fibula at the distal tibiofibular joint averaged 1.3 mm in the anterior syndesmosis, 3.7 mm at the midsection, and 3.3 mm at the posterior aspect [63]. Therefore, physiologic opening of the syndesmosis depends on the level of testing, and an opening of more than 2 mm anteriorly is pathologic. When instability is present, arthroscopic syndesmotic debridement with percutaneous fixation provides good or excellent results [64, 65].
Treatment of Acute Injuries
Surgical intervention of acute syndesmotic injuries consists of screw fixation or dynamic stabilization with a suture-button construct or hybrid fixation. A widened mortise on weight-bearing radiographs (Fig. 29.5) necessitates surgical reduction and stabilization to reestablish normal ankle biomechanics and optimize patient outcomes by preventing post-traumatic arthritis and chronic instability [66, 67]. The only significant predictor of function after syndesmotic injury is maintenance of reduction [36]. Other indications for syndesmotic stabilization include a fibula fracture at least 4.5 cm proximal to the tibiotalar joint coupled with deltoid ligament injury and intraoperative fluoroscopic evidence of gross syndesmotic instability following malleolar fixation [68, 69].
The literature is less definitive regarding the management of low-grade injuries in athletes with more subtle radiographic abnormalities. Surgical stabilization coupled with arthroscopic treatment of concomitant intra-articular pathology has been recommended for grade II injuries [34]. Since grade III injuries are commonly associated with osteochondral defects as well as deltoid and lateral ligamentous ruptures, preoperative advanced imaging and/or intraoperative arthroscopy can be beneficial. Return to play in as early as 6 weeks has been demonstrated with early surgical intervention for grade III syndesmotic sprains paired with an aggressive rehabilitation protocol [70].
Screw Fixation
Despite an abundance of research on the topic, there remains no clear consensus regarding the ideal technique of syndesmotic stabilization. In general, most agree that implants should be placed at least 1.5 cm proximal to the tibial plafond (Fig. 29.6) to avoid the true syndesmotic joint, parallel to the joint and directed from posterolateral to anteromedial at a 25–30° angle from the coronal plane while an external clamp or other reduction aid is maintaining the reduction [71, 72]. It is well-established that screws should not be placed in lag fashion as this would overcompress the syndesmosis. Ongoing debate exists with respect to screw number and type, number of cortices penetrated, and the need for reoperation for hardware removal. Most commonly, either 3.5 or 4.5-mm fully threaded cortical screws are utilized depending on surgeon preference, patient size, and degree of instability. When using two syndesmotic screws, a cadaveric study showed that screw size (3.5 or 4.5-mm) and number of engaged cortices (tricortical or quadricortical) had no significant impact on mechanical stability [73].
Other studies have demonstrated that 4.5-mm screws have higher resistance to shear stress while 3.5-mm screws are more likely to break [74, 75]. Proponents of tricortical screws argue that more physiologic motion is preserved, while those in favor of quadricortical screws assert that more robust fixation is achieved and complete hardware removal is more easily performed after screw breakage [75]. One study showed that one quadricortical 4.5-mm screw had equivalent functional outcome, range of motion, and pain level as two 3.5-mm screws placed tricortically [76]. Bioabsorbable screws have been shown to function as effectively as conventional stainless steel screws at 1-year follow-up; [77] however, they are not commonly used because granuloma formation and foreign body reaction are potential complications [78].
Even in the absence of fibular fracture, a one-third tubular plate with fibula-only screws placed proximally and distally can be used in conjunction with syndesmotic screws. This plate functions both as a washer to distribute forces on the fibula and to optimize syndesmotic screw position within the fibula (Fig. 29.7a, b). The plate also improves stiffness and decreases the likelihood of stress fracture following syndesmotic screw removal. In a recent cadaveric study, retention of a supplementary one-third tubular plate following syndesmotic screws removal increased fibular torsional stiffness in comparison to syndesmotic screw-only specimens [79].
Dynamic Suture-Button Fixation
Dynamic stabilization of the syndesmosis using a suture-button fixation (TightRope, Arthrex, Inc., Naples, FL, USA) has become increasingly popular particularly in the treatment of athletes because it theoretically allows more physiologic motion at the syndesmosis and does not require an additional surgery for implant removal (Fig. 29.8) [80, 81]. Some authors favor the use of a one-third tubular plate with a single 4.5-mm tricortical syndesmotic screw and one suture button in elite athletes to obtain the benefits of both implants (Fig. 29.9) [25]. It is important to mention that there are several reports of skin irriation and granuloma formation from suture knots as well as osteolysis and osteomyelitis requiring surgical removal [82, 83]. Since these reports, the manufacturer has developed a knotless suture button that is currently in use but limited data exists at this time regarding long-term outcomes with this implant.
Although biomechanical studies have demonstrated marginally lower stability with suture buttons compared to screw fixation, it is this decrease in multidirectional rigidity that allows more anatomic micromotion (Fig. 29.10a, b) [84, 85]. In a cadaver model with deliberate syndesmotic malreduction, suture-button stabilization resulted in decreased post-operative displacement as opposed to conventional screw fixation [86]. Therefore, dynamic syndesmotic fixation may help to decrease the negative sequelae of iatrogenic clamp malreduction. Biomechanical studies are limited in their ability to replicate the actual forces of physiologic loading endured by the ankle during ambulation and athletic participation.
Multiple clinical studies have directly compared suture buttons and screws. In a series of 46 patients with average follow-up of 2.5 years, no malreductions were observed with the use of suture-button compared with a 21.7 % malreduction rate in the screw group [87]. Additionally, this study reported no significant differences in clinical outcome scores or time to full weight bearing. In a recent prospective randomized multicenter trial, dynamic suture-button fixation was shown to provide adequate syndesmotic stabilization without failure or loss of reduction with a significantly lower reoperation rate compared with single 3.5-mm quadricortical screw fixation [88]. In addition, better clinical outcome scores were observed in the dynamic fixation group but this difference did not reach statistical significance.
Screw Removal
We do not recommend routine removal of syndesmotic screws placed proximal to the true syndesmotic joint. Exceptions include hardware infection, symptomatic hardware, syndesmotic malreduction, and the need for revision surgery. Screws removed prematurely (median of 9 weeks after surgery) resulted in a 10 % loss of reduction [36]. Multiple studies have demonstrated that retention of syndesmotic screws, including those that are broken, does not pose a clinical problem [89, 90]. In the case of postoperative syndesmotic malreduction, the first step is to remove the syndesmotic screws. In a recent case series, 36 % of syndesmosis were malreduced after screw placement and 89 % of these reduced after screw removal [91].
Rehabilitation and Back-to-Sports
Postoperatively, patients are made non-weight-bearing in a splint for 2 weeks to allow soft tissue healing and subsidence of swelling. Range of motion exercises commence 2–3 weeks after surgery if wound healing is appropriate. Partial weight bearing in a CAM boot can begin at 3–4 weeks postoperatively in a compliant, highly motivated patient. Full weight bearing as tolerated is initiated at 4 weeks after surgery along with proprioceptive and strength exercises. The return to running and high-impact sports is guided by patient symptoms and progression with a graduated rehabilitation protocol but generally is permitted at 8–10 weeks.
Again, if screws or suture-buttons are placed above the true syndesmotic joint, we do not recommend routine removal. In the case of intolerable symptomatic hardware, the surgeon should wait a minimum of 12 weeks before removing hardware to prevent recurrent diastasis. Screws placed across the true syndesmotic joint should not be removed before 12 weeks. After screw removal, a period of protected weight bearing is recommended to prevent fracture at the level of the screw holes. Leaving a one-third tubular plate in place has been shown to improve torsional strength of the fibula [79]. As previously mentioned, multiple studies have shown no difference in clinical outcome between patients with retained and removed syndesmotic screws [89, 90, 92]. Some evidence supports the contention that screw removal can facilitate improved ankle motion and patient function but generally retained screws will break to allow restoration of motion [90].
Less definitive information exists regarding suture buttons but theoretically these implants allow more physiologic syndesmotic multidirectional motion. In a recent series of 25 patients, the average reported time to full-weight-bearing was 5.5 weeks using a suture-button technique without any recurrent diastasis at 10.9 months after surgery [93]. The majority of patients in this series were treated with a single suture button, while four had two devices placed. Patients had significant improvement in SF-12 and AOFAS-Hindfoot scores.
Evidence
The vast majority of literature surrounding treatment of syndesmotic injuries is based on level IV and V data, as well as anecdotal experience. No level I studies exist on this topic to our knowledge. With regard to our references, there are 12 level II studies and one level III study. The remainder are level IV and V studies.
Summary
-
1.
In the case of subtle syndesmotic injuries, contralateral comparison weight-bearing radiographs are recommended. While CT and MRI can provide additional information, these are static tests that will not identify instability.
-
2.
Arthroscopy is a very sensitive and accurate means of diagnosing syndesmotic instability and allows the surgeon to identify and treat other intra-articular injuries. Physiologic syndesmotic opening varies among individuals, but an anterior opening of more than 2 mm is pathologic.
-
3.
Syndesmotic implants, whether screws or suture buttons, should be placed above the true syndesmotic joint (more than 15 mm above the plafond) and therefore do not require routine removal. Premature screw removal can lead to recurrent diastasis.
-
4.
Anatomic syndesmotic reduction is the most important predictor of functional outcome. To avoid iatrogenic malreduction, a large clamp should be placed in a transverse orientation with the ankle in resting position while using intraoperative fluoroscopy with comparison views.
-
5.
In cases of concomitant syndesmotic and deltoid injury, one should strongly consider visualizing and repairing the deltoid ligament. The superficial deltoid can avulse off the medial malleolus and become entrapped in the medial gutter obstructing anatomic reduction.
-
6.
The optimal treatment of syndesmotic injuries remains controversial and discrepancies exist in the literature regarding return to play for elite athletes. Future level I studies with long-term follow-up are necessary to provide these answers.
References
Brosky T, Nyland J, Nitz A, Caborn DN. The ankle ligaments: consideration of syndesmotic injury and implications for rehabilitation. J Orthop Sports Phys Ther. 1995;21(4):197–205.
McCollum GA, van den Bekerom MP, Kerkhoffs GM, Calder JD, van Dijk CN. Syndesmosis and deltoid ligament injuries in the athlete. Knee Surg Sports Traumatol Arthrosc. 2013;21(6):1328–37.
Fallat L, Grimm DJ, Saracco JA. Sprained ankle syndrome: prevalence and analysis of 639 acute injuries. J Foot Ankle Surg. 1998;37(4):280–5.
Boytim MJ, Fischer DA, Neumann L. Syndesmotic ankle sprains. Am J Sports Med. 1991;19(3):294–8.
Waterman BR, Belmont Jr PJ, Cameron KL, Svoboda SJ, Alitz CJ, Owens BD. Risk factors for syndesmotic and medial ankle sprain: role of sex, sport, and level of competition. Am J Sports Med. 2011;39(5):992–8.
Wright RW, Barile RJ, Surprenant DA, Matava MJ. Ankle syndesmosis sprains in national hockey league players. Am J Sports Med. 2004;32(8):1941–5.
Jones MH, Amendola A. Syndesmosis sprains of the ankle: a systematic review. Clin Orthop Relat Res. 2007;455:173–5.
Gerber JP, Williams GN, Scoville CR, Arciero RA, Taylor DC. Persistent disability associated with ankle sprains: a prospective examination of an athletic population. Foot Ankle Int. 1998;19(10):653–60.
Hopkinson WJ, St Pierre P, Ryan JB, Wheeler JH. Syndesmosis sprains of the ankle. Foot Ankle. 1990;10(6):325–30.
Williams GN, Jones MH, Amendola A. Syndesmotic ankle sprains in athletes. Am J Sports Med. 2007;35(7):1197–207.
Bartonicek J. Anatomy of the tibiofibular syndesmosis and its clinical relevance. Surg Radiol Anat. 2003;25(5–6):379–86.
Xenos JS, Hopkinson WJ, Mulligan ME, Olson EJ, Popovic NA. The tibiofibular syndesmosis. Evaluation of the ligamentous structures, methods of fixation, and radiographic assessment. J Bone Joint Surg Am. 1995;77(6):847–56.
Close JR. Some applications of the functional anatomy of the ankle joint. J Bone Joint Surg Am. 1956;38-A(4):761–81.
Michelson JD, Helgemo Jr SL. Kinematics of the axially loaded ankle. Foot Ankle Int. 1995;16(9):577–82.
Lundberg A. Kinematics of the ankle and foot. In vivo roentgen stereophotogrammetry. Acta Orthop Scand Suppl. 1989;233:1–24.
Beumer A, van Hemert WL, Niesing R, Entius CA, Ginai AZ, Mulder PG, et al. Radiographic measurement of the distal tibiofibular syndesmosis has limited use. Clin Orthop Relat Res. 2004;423:227–34.
Beumer A, Valstar ER, Garling EH, Niesing R, Ranstam J, Lofvenberg R, et al. Kinematics of the distal tibiofibular syndesmosis: radiostereometry in 11 normal ankles. Acta Orthop Scand. 2003;74(3):337–43.
Ramsey PL, Hamilton W. Changes in tibiotalar area of contact caused by lateral talar shift. J Bone Joint Surg Am. 1976;58(3):356–7.
Calhoun JH, Li F, Ledbetter BR, Viegas SF. A comprehensive study of pressure distribution in the ankle joint with inversion and eversion. Foot Ankle Int. 1994;15(3):125–33.
Ogilvie-Harris DJ, Reed SC, Hedman TP. Disruption of the ankle syndesmosis: biomechanical study of the ligamentous restraints. Arthroscopy. 1994;10(5):558–60.
Candal-Couto JJ, Burrow D, Bromage S, Briggs PJ. Instability of the tibio-fibular syndesmosis: have we been pulling in the wrong direction? Injury. 2004;35(8):814–8.
Michelson JD, Waldman B. An axially loaded model of the ankle after pronation external rotation injury. Clin Orthop Relat Res. 1996;328:285–93.
Beumer A, Valstar ER, Garling EH, Niesing R, Ginai AZ, Ranstam J, et al. Effects of ligament sectioning on the kinematics of the distal tibiofibular syndesmosis: a radiostereometric study of 10 cadaveric specimens based on presumed trauma mechanisms with suggestions for treatment. Acta Orthop. 2006;77(3):531–40.
Lauge-Hansen N. Fractures of the ankle. II. Combined experimental-surgical and experimental-roentgenologic investigations. Arch Surg. 1950;60(5):957–85.
Anderson RB, Hunt KJ, McCormick JJ. Management of common sports-related injuries about the foot and ankle. J Am Acad Orthop Surg. 2010;18(9):546–56.
Beumer A, van Hemert WL, Swierstra BA, Jasper LE, Belkoff SM. A biomechanical evaluation of clinical stress tests for syndesmotic ankle instability. Foot Ankle Int. 2003;24(4):358–63.
Hunt KJ, George E, Harris AH, Dragoo JL. Epidemiology of syndesmosis injuries in intercollegiate football: incidence and risk factors from National Collegiate Athletic Association injury surveillance system data from 2004–2005 to 2008–2009. Clin J Sport Med. 2013;23(4):278–82.
Mak MF, Gartner L, Pearce CJ. Management of syndesmosis injuries in the elite athlete. Foot Ankle Clin. 2013;18(2):195–214.
Nussbaum ED, Hosea TM, Sieler SD, Incremona BR, Kessler DE. Prospective evaluation of syndesmotic ankle sprains without diastasis. Am J Sports Med. 2001;29(1):31–5.
van Dijk CN, Mol BW, Lim LS, Marti RK, Bossuyt PM. Diagnosis of ligament rupture of the ankle joint. Physical examination, arthrography, stress radiography and sonography compared in 160 patients after inversion trauma. Acta Orthop Scand. 1996;67(6):566–70.
Kiter E, Bozkurt M. The crossed-leg test for examination of ankle syndesmosis injuries. Foot Ankle Int. 2005;26(2):187–8.
Beumer A, Swierstra BA, Mulder PG. Clinical diagnosis of syndesmotic ankle instability: evaluation of stress tests behind the curtains. Acta Orthop Scand. 2002;73(6):667–9.
de Cesar PC, Avila EM, de Abreu MR. Comparison of magnetic resonance imaging to physical examination for syndesmotic injury after lateral ankle sprain. Foot Ankle Int. 2011;32(12):1110–4.
Amendola A, Williams G, Foster D. Evidence-based approach to treatment of acute traumatic syndesmosis (high ankle) sprains. Sports Med Arthrosc. 2006;14(4):232–6.
Ebraheim NA, Elgafy H, Padanilam T. Syndesmotic disruption in low fibular fractures associated with deltoid ligament injury. Clin Orthop Relat Res. 2003;409:260–7.
Weening B, Bhandari M. Predictors of functional outcome following transsyndesmotic screw fixation of ankle fractures. J Orthop Trauma. 2005;19(2):102–8.
Harper MC, Keller TS. A radiographic evaluation of the tibiofibular syndesmosis. Foot Ankle. 1989;10(3):156–60.
Ostrum RF, De Meo P, Subramanian R. A critical analysis of the anterior-posterior radiographic anatomy of the ankle syndesmosis. Foot Ankle Int. 1995;16(3):128–31.
Beumer A, Valstar ER, Garling EH, van Leeuwen WJ, Sikma W, Niesing R, et al. External rotation stress imaging in syndesmotic injuries of the ankle: comparison of lateral radiography and radiostereometry in a cadaveric model. Acta Orthop Scand. 2003;74(2):201–5.
Marmor M, Hansen E, Han HK, Buckley J, Matityahu A. Limitations of standard fluoroscopy in detecting rotational malreduction of the syndesmosis in an ankle fracture model. Foot Ankle Int. 2011;32(6):616–22.
Ebraheim NA, Lu J, Yang H, Mekhail AO, Yeasting RA. Radiographic and CT evaluation of tibiofibular syndesmotic diastasis: a cadaver study. Foot Ankle Int. 1997;18(11):693–8.
Sclafani SJ. Ligamentous injury of the lower tibiofibular syndesmosis: radiographic evidence. Radiology. 1985;156(1):21–7.
Muhle C, Frank LR, Rand T, Ahn JM, Yeh LR, Trudell D, et al. Tibiofibular syndesmosis: high-resolution MRI using a local gradient coil. J Comput Assist Tomogr. 1998;22(6):938–44.
Takao M, Ochi M, Oae K, Naito K, Uchio Y. Diagnosis of a tear of the tibiofibular syndesmosis. The role of arthroscopy of the ankle. J Bone Joint Surg Br. 2003;85(3):324–9.
Mei-Dan O, Kots E, Barchilon V, Massarwe S, Nyska M, Mann G. A dynamic ultrasound examination for the diagnosis of ankle syndesmotic injury in professional athletes: a preliminary study. Am J Sports Med. 2009;37(5):1009–16.
Brown KW, Morrison WB, Schweitzer ME, Parellada JA, Nothnagel H. MRI findings associated with distal tibiofibular syndesmosis injury. AJR Am J Roentgenol. 2004;182(1):131–6.
Hepple S, Guha A. The role of ankle arthroscopy in acute ankle injuries of the athlete. Foot Ankle Clin. 2013;18(2):185–94.
Ogilvie-Harris DJ, Gilbart MK, Chorney K. Chronic pain following ankle sprains in athletes: the role of arthroscopic surgery. Arthroscopy. 1997;13(5):564–74.
Edwards Jr GS, DeLee JC. Ankle diastasis without fracture. Foot Ankle. 1984;4(6):305–12.
Williams GN, Allen EJ. Rehabilitation of syndesmotic (high) ankle sprains. Sports Health. 2010;2(6):460–70.
Amendola A. Controversies in diagnosis and management of syndesmosis injuries of the ankle. Foot Ankle. 1992;13(1):44–50.
Phisitkul P, Ebinger T, Goetz J, Vaseenon T, Marsh JL. Forceps reduction of the syndesmosis in rotational ankle fractures: a cadaveric study. J Bone Joint Surg Am. 2012;94(24):2256–61.
Tornetta 3rd P, Spoo JE, Reynolds FA, Lee C. Overtightening of the ankle syndesmosis: is it really possible? J Bone Joint Surg Am. 2001;83-A(4):489–92.
Sagi HC, Shah AR, Sanders RW. The functional consequence of syndesmotic joint malreduction at a minimum 2-year follow-up. J Orthop Trauma. 2012;26(7):439–43.
Miller AN, Barei DP, Iaquinto JM, Ledoux WR, Beingessner DM. Iatrogenic syndesmosis malreduction via clamp and screw placement. J Orthop Trauma. 2013;27(2):100–6.
Gardner MJ, Demetrakopoulos D, Briggs SM, Helfet DL, Lorich DG. Malreduction of the tibiofibular syndesmosis in ankle fractures. Foot Ankle Int. 2006;27(10):788–92.
Miller AN, Carroll EA, Parker RJ, Boraiah S, Helfet DL, Lorich DG. Direct visualization for syndesmotic stabilization of ankle fractures. Foot Ankle Int. 2009;30(5):419–26.
Chissell HR, Jones J. The influence of a diastasis screw on the outcome of Weber type-C ankle fractures. J Bone Joint Surg Br. 1995;77(3):435–8.
Hsu AR, Gross CE, Lee S. Intraoperative O-arm computed tomography evaluation of syndesmotic reduction: case report. Foot Ankle Int. 2013;34(5):753–9.
Franke J, von Recum J, Suda AJ, Grutzner PA, Wendl K. Intraoperative three-dimensional imaging in the treatment of acute unstable syndesmotic injuries. J Bone Joint Surg Am. 2012;94(15):1386–90.
Oae K, Takao M, Naito K, Uchio Y, Kono T, Ishida J, et al. Injury of the tibiofibular syndesmosis: value of MR imaging for diagnosis. Radiology. 2003;227(1):155–61.
Loren GJ, Ferkel RD. Arthroscopic assessment of occult intra-articular injury in acute ankle fractures. Arthroscopy. 2002;18(4):412–21.
Dijk CN, SpringerLink (Online service). Ankle arthroscopy techniques developed by the Amsterdam Foot and Ankle School. Available from: http://dx.doi.org/10.1007/978-3-642-35989-7.
Ogilvie-Harris DJ, Reed SC. Disruption of the ankle syndesmosis: diagnosis and treatment by arthroscopic surgery. Arthroscopy. 1994;10(5):561–8.
Wolf BR, Amendola A. Syndesmosis injuries in the athlete: when and how to operate. Curr Opin Orthop. 2002;13(2):151–4.
Miller SD. Controversies in ankle fracture treatment. Indications for fixation of stable Weber type B fractures and indications for syndesmosis stabilization. Foot Ankle Clin. 2000;5(4):841–51. vi.
Stufkens SA, van den Bekerom MP, Doornberg JN, van Dijk CN, Kloen P. Evidence-based treatment of maisonneuve fractures. J Foot Ankle Surg. 2011;50(1):62–7.
Yamaguchi K, Martin CH, Boden SD, Labropoulos PA. Operative treatment of syndesmotic disruptions without use of a syndesmotic screw: a prospective clinical study. Foot Ankle Int. 1994;15(8):407–14.
Boden SD, Labropoulos PA, McCowin P, Lestini WF, Hurwitz SR. Mechanical considerations for the syndesmosis screw. A cadaver study. J Bone Joint Surg Am. 1989;71(10):1548–55.
Taylor DC, Tenuta JJ, Uhorchak JM, Arciero RA. Aggressive surgical treatment and early return to sports in athletes with grade III syndesmosis sprains. Am J Sports Med. 2007;35(11):1833–8.
Kukreti S, Faraj A, Miles JN. Does position of syndesmotic screw affect functional and radiological outcome in ankle fractures? Injury. 2005;36(9):1121–4.
McBryde A, Chiasson B, Wilhelm A, Donovan F, Ray T, Bacilla P. Syndesmotic screw placement: a biomechanical analysis. Foot Ankle Int. 1997;18(5):262–6.
Markolf KL, Jackson SR, McAllister DR. Syndesmosis fixation using dual 3.5 mm and 4.5 mm screws with tricortical and quadricortical purchase: a biomechanical study. Foot Ankle Int. 2013;34(5):734–9.
Hansen M, Le L, Wertheimer S, Meyer E, Haut R. Syndesmosis fixation: analysis of shear stress via axial load on 3.5-mm and 4.5-mm quadricortical syndesmotic screws. J Foot Ankle Surg. 2006;45(2):65–9.
Thompson MC, Gesink DS. Biomechanical comparison of syndesmosis fixation with 3.5- and 4.5-millimeter stainless steel screws. Foot Ankle Int. 2000;21(9):736–41.
Hoiness P, Stromsoe K. Tricortical versus quadricortical syndesmosis fixation in ankle fractures: a prospective, randomized study comparing two methods of syndesmosis fixation. J Orthop Trauma. 2004;18(6):331–7.
Thordarson DB, Samuelson M, Shepherd LE, Merkle PF, Lee J. Bioabsorbable versus stainless steel screw fixation of the syndesmosis in pronation-lateral rotation ankle fractures: a prospective randomized trial. Foot Ankle Int. 2001;22(4):335–8.
Bostman OM, Pihlajamaki HK. Late foreign-body reaction to an intraosseous bioabsorbable polylactic acid screw. A case report. J Bone Joint Surg Am. 1998;80(12):1791–4.
Clanton TO, Matheny LM, Jarvis HC, Lewis EV, Ambrose CG. Quantitative analysis of torsional stiffness in supplemental one-third tubular plate fixation in the management of isolated syndesmosis injuries: a biomechanical study. Foot Ankle Int. 2013;34(2):267–72.
Seitz Jr WH, Bachner EJ, Abram LJ, Postak P, Polando G, Brooks DB, et al. Repair of the tibiofibular syndesmosis with a flexible implant. J Orthop Trauma. 1991;5(1):78–82.
Thornes B, Walsh A, Hislop M, Murray P, O'Brien M. Suture-endobutton fixation of ankle tibio-fibular diastasis: a cadaver study. Foot Ankle Int. 2003;24(2):142–6.
Willmott HJ, Singh B, David LA. Outcome and complications of treatment of ankle diastasis with tightrope fixation. Injury. 2009;40(11):1204–6.
Storey P, Gadd RJ, Blundell C, Davies MB. Complications of suture button ankle syndesmosis stabilization with modifications of surgical technique. Foot Ankle Int. 2012;33(9):717–21.
Soin SP, Knight TA, Dinah AF, Mears SC, Swierstra BA, Belkoff SM. Suture-button versus screw fixation in a syndesmosis rupture model: a biomechanical comparison. Foot Ankle Int. 2009;30(4):346–52.
Teramoto A, Suzuki D, Kamiya T, Chikenji T, Watanabe K, Yamashita T. Comparison of different fixation methods of the suture-button implant for tibiofibular syndesmosis injuries. Am J Sports Med. 2011;39(10):2226–32.
Westermann RW, Rungprai C, Goetz JE, Femino J, Amendola A, Phisitkul P. The effect of suture-button fixation on simulated syndesmotic malreduction: a cadaveric study. J Bone Joint Surg Am. 2014;96(20):1732–8.
Naqvi GA, Cunningham P, Lynch B, Galvin R, Awan N. Fixation of ankle syndesmotic injuries: comparison of tightrope fixation and syndesmotic screw fixation for accuracy of syndesmotic reduction. Am J Sports Med. 2012;40(12):2828–35.
Laflamme M, Belzile EL, Bedard L, van den Bekerom MP, Glazebrook M, Pelet S. A prospective randomized multicenter trial comparing clinical outcomes of patients treated surgically with a static or dynamic implant for acute ankle syndesmosis rupture. J Orthop Trauma. 2014;29(5):216–23.
Moore Jr JA, Shank JR, Morgan SJ, Smith WR. Syndesmosis fixation: a comparison of three and four cortices of screw fixation without hardware removal. Foot Ankle Int. 2006;27(8):567–72.
Hamid N, Loeffler BJ, Braddy W, Kellam JF, Cohen BE, Bosse MJ. Outcome after fixation of ankle fractures with an injury to the syndesmosis: the effect of the syndesmosis screw. J Bone Joint Surg Br. 2009;91(8):1069–73.
Song DJ, Lanzi JT, Groth AT, Drake M, Orchowski JR, Shaha SH, et al. The effect of syndesmosis screw removal on the reduction of the distal tibiofibular joint: a Prospective Radiographic Study. Foot Ankle Int. 2014;35(6):543–8.
Schepers T. To retain or remove the syndesmotic screw: a review of literature. Arch Orthop Trauma Surg. 2011;131(7):879–83.
Cottom JM, Hyer CF, Philbin TM, Berlet GC. Treatment of syndesmotic disruptions with the Arthrex Tightrope: a report of 25 cases. Foot Ankle Int. 2008;29(8):773–80.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Lareau, C.R., Hsu, A.R., Cohen, B.E. (2016). Acute Syndesmotic Injuries. In: Valderrabano, V., Easley, M. (eds) Foot and Ankle Sports Orthopaedics. Springer, Cham. https://doi.org/10.1007/978-3-319-15735-1_29
Download citation
DOI: https://doi.org/10.1007/978-3-319-15735-1_29
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-15734-4
Online ISBN: 978-3-319-15735-1
eBook Packages: MedicineMedicine (R0)