Abstract
Embolization of atheromatous debris is a known cause of major morbidity and mortality during complex endovascular repair. Potential complications include solid organ infarction, loss of renal function, bowel ischemia, and multisystem organ failure. Few studies have analyzed predictive factors of risk of atheroembolization during complex endovascular repair. We have recently analyzed atherosclerotic aortic wall thrombus (AWT) and clinical outcomes in 212 patients treated by fenestrated-branched endovascular aortic repair (F-BEVAR). Computed tomography angiography (CTA) was reviewed in all patients to determine the location, extent, and severity of atherosclerotic AWT. The aorta was divided into three segments and volumetric measurements of AWT were performed using Terarecon software. A classification system is proposed using objective assessment of number of affected segments, thrombus type, thickness, area, and circumference. AWT was classified as mild in 98 patients (46 %) and was considered moderate or severe in 114 (54 %). Solid organ infarction was present in 50 patients (24 %), acute renal injury occurred in 45 patients (21 %) by RIFLE criteria or 48 patients (23 %) by AKIN criteria. Patients with these complications had significantly higher (P < 0.05) AWT index scores. This chapter describes volumetric AWT assessment by image software and presents a novel score-based classification.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Embolization of atheromatous debris is a known cause of major morbidity and mortality during complex endovascular procedures. Microembolizations of cholesterol fragments or macroscopic particles of thrombus and plaque can result in end-organ damage and loss of renal function, bowel infarction, spinal cord injury, or stroke [1–7]. Patel et al. reported the association of increased thrombus burden in the aorta as a predictor of mesenteric and renal ischemia in patients treated by fenestrated endografts [8]. In the thoracic and abdominal aorta, severe and irregular thrombus or debris has been identified as a predictor of renal deterioration, and embolic events were associated with floating thrombus [9–11]. Although assessment of aortic thrombus is done routinely as part of preoperative planning, few studies have correlated the severity of aortic wall thrombus (AWT) with specific events using a standardized classification system. This chapter summarizes current results of fenestrated and branched endovascular aortic repair (F-BEVAR) and parallel stent-grafts and presents a novel classification system to evaluate aortic wall thrombus.
Clinical Implications
Few studies have reported specific embolic events following endovascular treatment of complex aortic aneurysms. Although most published series have included high-risk patients with multiple comorbidities, specific embolic complications are poorly reported. Acute kidney injury is the most common complication occurring in up to 40 % of the patients, depending on which criteria are used to define renal dysfunction. Postoperative dialysis has been reported in 1–10 % of the patients. Spinal cord injury, with transient or persistent symptoms, has been reported in up to 30 % of patients with thoracoabdominal aortic aneurysms. Strokes or transient ischemic attacks are less frequent. Regarding gastrointestinal complications, the most common complication is prolonged ileus. Bowel ischemia occurs in up to 9 % of the patients, whereas pancreatitis is infrequent (Table 46.1) [12–57].
Risk Stratification
None of the prior reports has described a standardized method to quantify aortic wall thrombus. We have recently analyzed 212 patients entered in a prospective database from 2007 to 2015. The study included patients treated for pararenal (PRA) or type IV thoracoabdominal aortic aneurysms (TAAAs) with F-BEVAR who had normal or relatively normal aortic segments in the arch, thoracic aorta, and above the renal arteries.
Aortic Wall Thrombus Assessment
Volumetric measurement of aortic wall thrombus (AWT) was performed using computed tomography angiography (CTA) and Terarecon Software (Fig. 46.1) in non-aneurysmal aortic segments (≤4 cm) of the ascending aorta and arch (Segment A), descending thoracic aorta (Segment B), and renal-mesenteric aorta (Segment C). An index was calculated using the Terarecon software volumetric tool to measure AWT burden in the three segments and in the entire length of aorta starting at the aortic annulus and extending 1-cm below the renal arteries. The infra-renal aorta , which was typically affected by large aneurysm and extensive laminated thrombus, was not measured. Because it is not possible to measure the volume of the thin walled intima, media, and adventitia, an AWT index was calculated by subtracting the volume of the aortic lumen from the total aortic volume, which includes the aortic lumen, any AWT, and the intima, media, and adventitia. Therefore, the AWT index was representative of the solid portion of the aortic wall. The AWT index was presented as a percent value (AWT Index = [Total Aortic Volume−Aortic Lumen Volume/Total Aortic Volume] × 100, Fig. 46.2).
Aortic wall thrombus volume measurement sequence . Total segmental volume measurement (step 1). Luminal volume subtraction (step 2). Remaining residual volume corresponding to the aortic wall and thrombus volume (step 3). By permission of Mayo Foundation for Medical Education and Research. All rights reserved
In order to facilitate assessment of AWT in clinical practice, a novel classification was proposed using a 0–10 score system to quantify thrombus type, thickness, area of involvement, circumference, and number of affected segments. The patients were classified as mild (score 0–3), moderate (score 4–8), and severe AWT (score 9 and 10, Fig. 46.3). For purposes of this classification, we analyzed the most severely affected segment of the aorta using axial cuts. The area was selected after examination of the entire length of the aorta. The final score was correlated with the AWT volume index measured in the three aortic segments and in the entire aorta to validate the proposed classification.
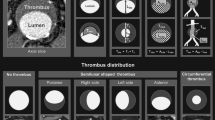
Qualitative score-based classification . The most severely affected aortic area in CTA cross-section is classified for thrombus type (none, smooth lining or finger-like projections), thickness (none, 1–4 mm or ≥5 mm), area (0–24 %, 25–50 % or ≥50 %), and circumference (0–90°, 91–179° or ≥180°). Number of affected segments is also contemplated. Individual items are graded from 0 to 2. Mild AWT range from 0 to 4, moderate AWT from 4 to 8, and severe AWT scores 9 and 10. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
From the 212 patients, 98 (46 %) had minimal AWT, 75 (35 %) had moderate AWT, and 39 (18 %) had severe AWT (Table 46.2). The proposed classification correlated with objective assessment of AWT volume using the index in all three segments. Aortic wall thrombus index averaged 15 ± 4 % for segment A, 22 ± 5 % for segment B, 26 ± 7 % for segment C, and 20 ± 4 % for the three segments. Thirteen patients (6 %) had AWT index <15 %.
Study Patients
From the 212 patients included in the study, there were 169 male (80 %) and 43 female (20 %), with mean age of 76 ± 7 years old. Aneurysm extent was PRA in 157 patients (74 %) and type IV TAAA in 55 patients (26 %). The maximum aneurysm diameter average was 63 ± 15 mm (Table 46.3). All procedures were performed in a hybrid endovascular room with fixed imaging unit using general endotracheal anesthesia in 210 patients (99 %). Cerebrospinal fluid drainage was used in 67 patients (32 %) and neuro-monitoring in 55 patients (26 %). Ninety-six patients (46 %) had percutaneous trans-femoral approach and 29 required iliac conduits (14 %). There were 700 renal-mesenteric arteries incorporated by 609 fenestrations, 66 scallops, and 25 branches, with a mean of 3.1 ± 1 stented vessels per patient. Total volume of contrast and fluoroscopy time averaged 158 ± 63 ml and 88 ± 42 min, respectively. Technical success, defined by placement of the aortic stent and all intended side branches, was achieved in 207 patients (98 %). Estimated blood loss was 757 ± 859 ml. Seventy-two patients (34 %) received transfusion of packed red blood cells during the procedure (see Table 46.3). All risk factors, stent design, and procedure variables were similar in the mild, moderate, and severe AWT patients.
Clinical Events
Clinical outcomes included 30-day mortality, neurological complications (stroke and spinal cord injury), gastrointestinal (bowel ischemia, pancreatitis and time to resume regular diet) and renal injury by RIFLE and AKIN classification and decline in the estimated glomerular filtration rate (eGFR ) . Evidence of solid organ infarction was also reviewed in the postoperative CTA. Renal infarctions due to inadvertent occlusion of a main or accessory renal artery were excluded from analysis.
The was one 30-day mortality (0.5 %) for the entire cohort, which included a patient treated for suprarenal aortic aneurysm who died from complications of a type B dissection 8 days following the initial procedure (Table 46.4). The patient had AWT index of 17 % and was classified as moderate AWT. Four patients (1.9 %) had strokes, which occurred in the absence of significant AWT on Segment A, although three patients had moderate to severe AWT in the thoracic or renal-mesenteric segments and one had thrombus within the innominate artery origin (Table 46.5).
Three patients (1.4 %) developed SCI , including two with PRA and one with type IV TAAA. Of these, one had permanent paraplegia and two had improvements, being able to recover the ambulatory status. Patients with any SCI had higher AWT index in segment B (28 ± 3 % versus 22 ± 5 %) and C (30 ± 11 % versus 26 ± 7 %). Although there was no association of AWT index for any neurological events, six of the seven patients (86 %) who developed either stroke or SCI had moderate to severe AWT scores (see Tables 46.4 and 46.5).
The mean time to resume a regular diet was 2.9 ± 1.7 days and was significantly longer in patients with higher AWT volume index in segment B (P = 0.018), segment C (P = 0.0001) and in the three segments using linear regression analysis (P = 0.0004, Fig. 46.4). There was also longer time to resume regular diet for patients with severe and moderate thrombus burden (3.4 ± 2 and 3.1 ± 2 days versus 2.9 ± 1.7 days, P = 0.0115). Gastrointestinal complications included ischemic colitis in four patients (1.8 %) and pancreatitis in two patients (1 %). There was no association between these two complications and AWT index.
Linear regression analysis curve showing the association between AWT index and postoperative diet resumption. All segments were analyzed as a whole. As higher is the AWT index depicted in the y axis as longer is the time to resume the regular diet depicted in the x axis. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
Forty-five patients (21 %) had acute kidney injury (AKI) using the definitions proposed by RIFLE criteria (see Table 46.4). Thirty-two patients (15 %) reached the “Risk” stage, eight (4 %) the “Injury” stage, four (2 %) the “Failure” stage, and one (0.5 %) the “Loss” stage, requiring temporary hemodialysis. None of the patients require permanent hemodialysis. Among patients who developed acute kidney injury, AWT index was higher in segment B (25 ± 6 % versus 22 ± 4 %, p = 0.002), with the highest AWT index observed for those patients who had “failure” (27 ± 7 %). Results were similar using the definitions proposed by the AKIN classification , including 48 patients (23 %) who had any AKI. Thirty-nine patients (18 %) reached stage one, seven (3 %) stage two, and two (0.9 %) stage three. Segment B had the highest AWT index for patients who developed AKI (24 ± 6 % versus 22 ± 4 %, p = 0.04, see Table 46.4).
There was also direct association between decline in postoperative eGFR and AWT index in segments A and B and for entire evaluated aorta (Fig. 46.5, P = 0.023) using the linear regression analysis. Using multivariate analysis, AWT index in segment B was associated with AKI using both the RIFLE (P = 0.02) and AKIN criteria (P = 0.0128 and P = 0.0007, respectively). Other independent risk factors for AKI were pre-existing CKD stage III–V and volume of contrast. AKI for was significantly more frequent in patients with moderate to severe AWT scores using either RIFLE or AKIN criteria (P = 0.034 and P = 0.024, respectively).
Linear regression analysis curve showing the association between AWT index and early postoperative decline in eGFR . All segments were analyzed as a whole. To evaluate the changes in the renal function, postoperative eGFR was divided by its preoperative value. By deduction, as lower is this ratio as greater is the eGFR decline. The graph depicts an inverse correlation i.e., as higher is the AWT index, as lower is the ratio and, therefore, more severe is the eGFR decline. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
Solid organ infarctions (Fig. 46.6) were observed in 50 patients (24 %). Three patients had hepatic infarction with significantly higher AWT index scores in segment C (37 ± 15 % versus 26 ± 7 %, P = 0.043) compared to patients with no hepatic infarction (see Tables 46.4 and 46.5). Twenty-five patients (12 %) had splenic infarctions with higher scores in segments B (25 ± 5 % versus 22 ± 5 %, P = 0.011) and C (29 ± 7 % versus 26 ± 7, P = 0.033) compared to patients with no splenic infarcts. Thirty-five patients (17 %) had renal infarctions with higher scores in segment A (16 ± 3 versus 14 ± 4, P = 0.039), B (versus 24 ± 6 % versus 22 ± 5, P = 0.025), and C (29 ± 8 % versus 26 ± 7, P = 0.031) compared to patients with no renal infarcts. The composite of any solid organ infarction was associated with higher AWT index scores for segments A (16 ± 4 % versus 14 ± 4 %, P = 0.016), B (24 ± 5 % versus 22 ± 5 %, p = 0.005) and C (28 ± 8 % versus 25 ± 7 %, P = 0.029). Using multivariate analysis, AWT index in segment B was associated with solid organ embolization in all three organs (P = 0.0028). Kidney infarctions and any solid organ infarction were more frequent in the severe group (P = 0.009 and P = 0.01, respectively).
Cases Examples
Case 1
An 81-year-old male patient presented with asymptomatic type IV thoracoabdominal aneurysm with maximum diameter of 60 mm. His medical comorbidities were hypertension, congestive heart failure, hypercholesterolemia, active smoking, previous myocardial infarction and CABG, peripheral arterial disease and chronic kidney disease stage III with a baseline estimated glomerular filtration rate of 46 ml/min/1.73 m2 (serum creatinine: 1.4 mg/dl). Using the preoperative risk scales, he was scored as ASA II and 17 by the SVS total score. Preoperative cardiac stress test was positive for myocardial ischemia with an ejection fraction of 43 %. He had no prior aortic surgeries or other relevant surgical history.
There was significant aortic wall thrombus in the descending thoracic and renal-mesenteric aorta with a total AWT index of 29 % including 31 % for segment B and 47 % for segment C (both in the highest quartile). Using the score-based classification he had a score of 9 (severe AWT) achieving two points for number of segments, thrombus type, thickness, circumference and 1 point for area (Fig. 46.7). He underwent a fenestrated endovascular repair with four-vessel incorporation by fenestrations with a customized non-standard device. There were no intercurrences during the procedure with a total time of 186 min and 180 ml of contrast used.
In the postoperative time, the patient presented abdominal pain and acute renal injury (AKI) with a decline in the eGFR to 20 ml/min/1.73 m2, classified as “Injury” by RIFLE criteria . Postoperative CTA showed kidney, spleen, and liver infarctions (see Fig. 46.6). In the postoperative day 3, patient had troponin elevations due to a non-Q-wave myocardial infarction. He also had transitory lower limb weakness with complete recovery before discharge. ICU length of stay was 6-day long with progressive improvement of the abdominal pain and clinical condition. He had his regular diet resumed in the postoperative day 5 which was significantly longer than the average time of 2.9 days. Total length of stay was 9 days being discharge in good conditions and with partial recovery of the renal function presenting at the dismissal a serum creatinine of 1.9 mg/dl and an eGFR of 32 ml/min/1.73 m2.
Case 2
A 58-year-old male presented with an asymptomatic type IV thoracoabdominal aneurysm with maximum diameter of 57 mm. He was an active smoker and his preoperative cardiac stress test was negative with ejection fraction of 65 % and normal baseline renal function. He had a history of resected prostate and testicular cancer without other prior surgeries. He was classified as ASA II and SVS score three. There was regular aortic wall thrombus mainly in renal-mesenteric aorta with a total AWT index of 23 % including 25 % for segment B and 41 % for segment C, within the fourth quartile. Using the score-based classification he had a score of 7 (moderate AWT) achieving two points for number of segments and thickness and one point for thrombus type, circumference, and area (Fig. 46.8).
Preoperative CTA showing significant aortic thrombus in the posterior aortic wall in the renal-mesenteric segment. Note its regular characteristic even though was classified as moderate due its expressive volume. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
He underwent a fenestrated endovascular repair with four-vessel fenestrated component using a customized non-standard device. The length of surgery was 176 min with a total contrast volume of 170 ml without any major technical issue. Postoperative CTA showed mild spleen and left kidney infarctions (Fig. 46.9). However, there was no change in the renal function, being discharged 3 days after the procedure.
Case 3
An 84-year-old male presented with an asymptomatic parvisceral abdominal aneurysm with 59 mm in the maximum diameter. He had hypercholesterolemia and moderate pulmonary dysfunction due to asbestosis. He did not have renal dysfunction with a baseline creatinine of 0.8 mg/dl and an eGFR of 92 ml/min/1.73 m2. His SVS score was 12 mostly due to his pulmonary disease and age. No previous aortic surgeries.
There was mild to moderate aortic wall thrombus mostly in segment C with a total AWT index of 20 % and an index of 26 % for segment C which matches the third quartile. Using the score-based classification he had a score of 8 (moderate AWT) achieving two points for thrombus type, thickness, circumference and one point for area and number of segments (Fig. 46.10).
He underwent an endovascular repair of his aneurysm with a five-vessel fenestrated endograft with one double-scallop for celiac axis and fenestrations for superior mesenteric artery, right renal artery, and two left-sided renal arteries. Length of surgery was 300 min long (endovascular time of 251 min) with 190 ml of contrast used. The procedure did not have complications.
Postoperatively he presented mild renal deterioration reaching the stage “Risk” by RIFLE criteria with a decrease in eGFR to 55 ml/min/1.73 m2. He returned to his baseline renal function before discharge. Postoperative CTA showed significant bilateral kidney infarctions mainly in the right side (Fig. 46.11). Overall he recovered well from the surgery with rapid resume of his regular diet, being discharged at postoperative day 5.
Coronal and axial postoperative CTA images of bilateral kidney infarcts, mainly in the right side (arrows). Note the significant hypotenuse area in middle third of the right kidney which affected up to 30 % of the kidney volume. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
Case 4
A 78-year-old female patient was evaluated for a 7.2-cm type IV TAAA. Medical comorbidities included current smoking, hypertension, stage IV chronic kidney disease, and severe ischemic cardiomyopathy. She was denied treatment of her aneurysm due to extensive atherosclerotic debris in the thoracoabdominal aorta as depicted in Fig. 46.12.
Conclusion
Atherosclerotic aortic wall thrombus is a common finding in the preoperative evaluation of F-BEVAR candidates and 54 % of the patients were classified as moderate and severe AWT in this study. A simple classification is proposed to stratify risk according to the amount of atherosclerotic debris in the aorta (Fig. 46.13). Management of embolization is difficult. For small debris prevention is the only effective treatment. Larger particles may be treated by catheter aspiration devices (Fig. 46.14) with careful attention to avoid vessel perforation (Fig. 46.15) which can further result in end-organ ischemia. Volumetric AWT evaluation is a reliable measurement and correlates with adverse events after F-BEVAR and has excellent correlation with the proposed classification. Therefore, AWT burden correlates with renal function deterioration, longer time to resume enteral diet, and more solid organ infarcts. Assessment of AWT should be part of preoperative planning and therapeutic decision-making in patients with complex aortic aneurysms.
Axial and sagittal CTA sections exemplifying all three aortic wall thrombus graduations by the proposed classification. Mild AWT patients have very slight and regular atheroma plaques without diffuse disease. Moderate AWT patients usually have higher amount of debris with or without finger-like thrombus, whereas severe ones have extremely irregular, large, and diffuse thrombus. By permission of Mayo Foundation for Medical Education and Research. All rights reserved
Side-branch macroembolization s may be treated intraoperatively by suction catheters as depicted here. First, the partially or totally occluded segment has to be crossed by the guidewire (a). Sequentially, using specific catheter aspiration devices, the fresh thrombus can be aspirated as demonstrated (b). By permission of Mayo Foundation for Medical Education and Research. All rights reserved
References
Hayashida N, Murayama H, Pearce Y, Asano S, Ohashi Y, Kohno H, et al. Shaggy aorta syndrome after acute arterial macroembolism: report of a case. Surg Today. 2004;34(4):354–6.
Barbut D, Hinton RB, Szatrowski TP, Hartman GS, Bruefach M, Williams-Russo P, et al. Cerebral emboli detected during bypass surgery are associated with clamp removal. Stroke. 1994;25(12):2398–402.
Fukumoto Y, Tsutsui H, Tsuchihashi M, Masumoto A, Takeshita A. The incidence and risk factors of cholesterol embolization syndrome, a complication of cardiac catheterization: a prospective study. J Am Coll Cardiol. 2003;42(2):211–6.
Dadian N, Ohki T, Veith FJ, Edelman M, Mehta M, Lipsitz EC, et al. Overt colon ischemia after endovascular aneurysm repair: the importance of microembolization as an etiology. J Vasc Surg. 2001;34(6):986–96.
Hoshina K, Hosaka A, Takayama T, Kato M, Ohkubo N, Okamoto H, et al. Outcomes after open surgery and endovascular aneurysm repair for abdominal aortic aneurysm in patients with massive neck atheroma. Eur J Vasc Endovasc Surg. 2012;43(3):257–61.
Mariscalco G, Piffaretti G, Tozzi M, Bacuzzi A, Carrafiello G, Sala A, et al. Predictive factors for cerebrovascular accidents after thoracic endovascular aortic repair. Ann Thorac Surg. 2009;88(6):1877–81.
Van Mieghem NM, El Faquir N, Rahhab Z, Rodríguez-Olivares R, Wilschut J, Ouhlous M, et al. Incidence and predictors of debris embolizing to the brain during transcatheter aortic valve implantation. JACC Cardiovasc Interv. 2015;8(5):718–24.
Patel SD, Constantinou J, Hamilton H, Davis M, Ivancev K. Editor’s choice—a shaggy aorta is associated with mesenteric embolisation in patients undergoing fenestrated endografts to treat paravisceral aortic aneurysms. Eur J Vasc Endovasc Surg. 2014;47(4):374–9.
Abissegue YG, Lyazidi Y, Chtata H, Bakkali T, Taberkant M. Acute systemic embolism due to an idiopathic floating thrombus of the thoracic aorta: success of medical management: a case report. BMC Res Notes. 2015;8:181.
Boufi M, Mameli A, Compes P, Hartung O, Alimi YS. Elective stent-graft treatment for the management of thoracic aorta mural thrombus. Eur J Vasc Endovasc Surg. 2014;47(4):335–41.
Verma H, Meda N, Vora S, George RK, Tripathi RK. Contemporary management of symptomatic primary aortic mural thrombus. J Vasc Surg. 2014;60(6):1524–34.
Eagleton MJ, Follansbee M, Wolski K, Mastracci T, Kuramochi Y. Fenestrated and branched endovascular aneurysm repair outcomes for type II and III thoracoabdominal aortic aneurysms. J Vasc Surg. 2016;63(4):930–42.
Ferrer C, Cao P, De Rango P, Tshomba Y, Verzini F, Melissano G, et al. A propensity-matched comparison for endovascular and open repair of thoracoabdominal aortic aneurysms. J Vasc Surg. 2016;63(5):1201–7.
Hu Z, Li Y, Peng R, Liu J, Zhang T, Guo W. Experience with fenestrated endovascular repair of juxtarenal abdominal aortic aneurysms at a single center. Medicine. 2016;95(10), e2683.
Banno H, Cochennec F, Marzelle J, Becquemin JP. Comparison of fenestrated endovascular aneurysm repair and chimney graft techniques for pararenal aortic aneurysm. J Vasc Surg. 2014;60(1):31–9.
Martin-Gonzalez T, Pincon C, Maurel B, Hertault A, Sobocinski J, Spear R, et al. Renal outcomes following fenestrated and branched endografting. Eur J Vasc Endovasc Surg. 2015;50(4):420–30.
Marzelle J, Presles E, Becquemin JP, WINDOWS trial participants. Results and factors affecting early outcome of fenestrated and/or branched stent grafts for aortic aneurysms: a multicenter prospective study. Ann Surg. 2015;261(1):197–206.
Sailer AM, Nelemans PJ, van Berlo C, Yazar O, de Haan MW, Fleischmann D, et al. Endovascular treatment of complex aortic aneurysms: prevalence of acute kidney injury and effect on long-term renal function. Eur Radiol. 2016;26(6):1613–9.
Shahverdyan R, Majd MP, Thul R, Braun N, Gawenda M, Brunkwall J. F-EVAR does not impair renal function more than open surgery for juxtarenal aortic aneurysms: single centre results. Eur J Vasc Endovasc Surg. 2015;50(4):432–41.
Cochennec F, Kobeiter H, Gohel M, Leopardi M, Raux M, Majewski M, et al. Early results of physician modified fenestrated stent grafts for the treatment of thoraco-abdominal aortic aneurysms. Eur J Vasc Endovasc Surg. 2015;50(5):583–92.
Gallitto E, Gargiulo M, Freyrie A, Mascoli C, Massoni Bianchini C, Ancetti S, et al. The endovascular treatment of juxta-renal abdominal aortic aneurysm using fenestrated endograft: early and mid-term results. J Cardiovasc Surg (Torino). 2015. [Epub ahead of print].
Glebova NO, Selvarajah S, Orion KC, Black 3rd JH, Malas MB, Perler BA, et al. Fenestrated endovascular repair of abdominal aortic aneurysms is associated with increased morbidity but comparable mortality with infrarenal endovascular aneurysm repair. J Vasc Surg. 2015;61(3):604–10.
Sveinsson M, Sobocinski J, Resch T, Sonesson B, Dias N, Haulon S, et al. Early versus late experience in fenestrated endovascular repair for abdominal aortic aneurysm. J Vasc Surg. 2015;61(4):895–901.
Verhoeven EL, Katsargyris A, Bekkema F, Oikonomou K, Zeebregts CJ, Ritter W, et al. Editor’s choice—ten-year experience with endovascular repair of thoracoabdominal aortic aneurysms: results from 166 consecutive patients. Eur J Vasc Endovasc Surg. 2015;49(5):524–31.
Grimme FA, Zeebregts CJ, Verhoeven EL, Bekkema F, Reijnen MM, Tielliu IF. Visceral stent patency in fenestrated stent grafting for abdominal aortic aneurysm repair. J Vasc Surg. 2014;59(2):298–306.
Chisci E, Kristmundsson T, de Donato G, Resch T, Setacci F, Sonesson B, et al. The AAA with a challenging neck: outcome of open versus endovascular repair with standard and fenestrated stent-grafts. J Endovasc Ther. 2009;16(2):137–46.
Kristmundsson T, Sonesson B, Dias N, Tornqvist P, Malina M, Resch T. Outcomes of fenestrated endovascular repair of juxtarenal aortic aneurysm. J Vasc Surg. 2014;59(1):115–20.
Dijkstra ML, Tielliu IF, Meerwaldt R, Pierie M, van Brussel J, Schurink GW, et al. Dutch experience with the fenestrated Anaconda endograft for short-neck infrarenal and juxtarenal abdominal aortic aneurysm repair. J Vasc Surg. 2014;60(2):301–7.
Kasprzak PM, Gallis K, Cucuruz B, Pfister K, Janotta M, Kopp R. Editor’s choice—temporary aneurysm sac perfusion as an adjunct for prevention of spinal cord ischemia after branched endovascular repair of thoracoabdominal aneurysms. Eur J Vasc Endovasc Surg. 2014;48(3):258–65.
Lee JT, Lee GK, Chandra V, Dalman RL. Comparison of fenestrated endografts and the snorkel/chimney technique. J Vasc Surg. 2014;60(4):849–56. discussion 56–7.
Liao TH, Watson JJ, Mansour MA, Cuff RF, Banegas SL, Chambers CM, et al. Preliminary results of Zenith fenestrated abdominal aortic aneurysm endovascular grafts. Am J Surg. 2014;207(3):417–21. discussion 21.
Oderich GS. Commentary: physician-modified vs off-the-shelf fenestrated and branched endografts: is this a fair comparison? J Endovasc Ther. 2016;23(1):110–4.
Vemuri C, Oderich GS, Lee JT, Farber MA, Fajardo A, Woo EY, et al. Postapproval outcomes of juxtarenal aortic aneurysms treated with the Zenith fenestrated endovascular graft. J Vasc Surg. 2014;60(2):295–300.
Canavati R, Millen A, Brennan J, Fisher RK, McWilliams RG, Naik JB, et al. Comparison of fenestrated endovascular and open repair of abdominal aortic aneurysms not suitable for standard endovascular repair. J Vasc Surg. 2013;57(2):362–7.
Kitagawa A, Greenberg RK, Eagleton MJ, Mastracci TM. Zenith p-branch standard fenestrated endovascular graft for juxtarenal abdominal aortic aneurysms. J Vasc Surg. 2013;58(2):291–300.
Perot C, Sobocinski J, Maurel B, Millet G, Guillou M, D’Elia P, et al. Comparison of short- and mid-term follow-up between standard and fenestrated endografts. Ann Vasc Surg. 2013;27(5):562–70.
Suominen V, Pimenoff G, Salenius J. Fenestrated and chimney endografts for juxtarenal aneurysms: early and midterm results. Scand J Surg. 2013;102(3):182–8.
Tsilimparis N, Perez S, Dayama A, Ricotta 2nd JJ. Endovascular repair with fenestrated-branched stent grafts improves 30-day outcomes for complex aortic aneurysms compared with open repair. Ann Vasc Surg. 2013;27(3):267–73.
Donas KP, Eisenack M, Panuccio G, Austermann M, Osada N, Torsello G. The role of open and endovascular treatment with fenestrated and chimney endografts for patients with juxtarenal aortic aneurysms. J Vasc Surg. 2012;56(2):285–90.
British Society for Endovascular Therapy and the Global Collaborators on Advanced Stent-Graft Techniques for Aneurysm Repair (GLOBALSTAR) Registry. Early results of fenestrated endovascular repair of juxtarenal aortic aneurysms in the United Kingdom. Circulation. 2012;125(22):2707–15.
Ferreira M, Lanziotti L, Cunha R, D’Utra G. Endovascular repair of thoracoabdominal aneurysms: results of the first 48 cases. Ann Cardiothorac Surg. 2012;1(3):304–10.
Manning BJ, Agu O, Richards T, Ivancev K, Harris PL. Early outcome following endovascular repair of pararenal aortic aneurysms: triple- versus double- or single-fenestrated stent-grafts. J Endovasc Ther. 2011;18(1):98–105.
Metcalfe MJ, Holt PJ, Hinchliffe RJ, Morgan R, Loftus IM, Thompson MM. Fenestrated endovascular aneurysm repair: graft complexity does not predict outcome. J Endovasc Ther. 2012;19(4):528–35.
Reilly LM, Rapp JH, Grenon SM, Hiramoto JS, Sobel J, Chuter TA. Efficacy and durability of endovascular thoracoabdominal aortic aneurysm repair using the caudally directed cuff technique. J Vasc Surg. 2012;56(1):53–63.
Tambyraja AL, Fishwick NG, Bown MJ, Nasim A, McCarthy MJ, Sayers RD. Fenestrated aortic endografts for juxtarenal aortic aneurysm: medium term outcomes. Eur J Vasc Endovasc Surg. 2011;42(1):54–8.
Troisi N, Donas KP, Austermann M, Tessarek J, Umscheid T, Torsello G. Secondary procedures after aortic aneurysm repair with fenestrated and branched endografts. J Endovasc Ther. 2011;18(2):146–53.
Amiot S, Haulon S, Becquemin JP, Magnan PE, Lermusiaux P, Goueffic Y, et al. Fenestrated endovascular grafting: the French multicentre experience. Eur J Vasc Endovasc Surg. 2010;39(5):537–44.
Verhoeven EL, Vourliotakis G, Bos WT, Tielliu IF, Zeebregts CJ, Prins TR, et al. Fenestrated stent grafting for short-necked and juxtarenal abdominal aortic aneurysm: an 8-year single-centre experience. Eur J Vasc Endovasc Surg. 2010;39(5):529–36.
Greenberg RK, Sternbergh 3rd WC, Makaroun M, Ohki T, Chuter T, Bharadwaj P, et al. Intermediate results of a United States multicenter trial of fenestrated endograft repair for juxtarenal abdominal aortic aneurysms. J Vasc Surg. 2009;50(4):730–7. e1.
Scurr JR, Brennan JA, Gilling-Smith GL, Harris PL, Vallabhaneni SR, McWilliams RG. Fenestrated endovascular repair for juxtarenal aortic aneurysm. Br J Surg. 2008;95(3):326–32.
Ziegler P, Avgerinos ED, Umscheid T, Perdikides T, Stelter WJ. Fenestrated endografting for aortic aneurysm repair: a 7-year experience. J Endovasc Ther. 2007;14(5):609–18.
Roselli EE, Greenberg RK, Pfaff K, Francis C, Svensson LG, Lytle BW. Endovascular treatment of thoracoabdominal aortic aneurysms. J Thorac Cardiovasc Surg. 2007;133(6):1474–82.
Halak M, Goodman MA, Baker SR. The fate of target visceral vessels after fenestrated endovascular aortic repair—general considerations and mid-term results. Eur J Vasc Endovasc Surg. 2006;32(2):124–8.
Muhs BE, Verhoeven EL, Zeebregts CJ, Tielliu IF, Prins TR, Verhagen HJ, et al. Mid-term results of endovascular aneurysm repair with branched and fenestrated endografts. J Vasc Surg. 2006;44(1):9–15.
O’Neill S, Greenberg RK, Haddad F, Resch T, Sereika J, Katz E. A prospective analysis of fenestrated endovascular grafting: intermediate-term outcomes. Eur J Vasc Endovasc Surg. 2006;32(2):115–23.
Semmens JB, Lawrence-Brown MM, Hartley DE, Allen YB, Green R, Nadkarni S. Outcomes of fenestrated endografts in the treatment of abdominal aortic aneurysm in Western Australia (1997–2004). J Endovasc Ther. 2006;13(3):320–9.
Anderson JL, Berce M, Hartley DE. Endoluminal aortic grafting with renal and superior mesenteric artery incorporation by graft fenestration. J Endovasc Ther. 2001;8(1):3–15.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Mayo Foundation for Medical Education and Research
About this chapter
Cite this chapter
Ribeiro, M.S., de Souza, L.R., Oderich, G.S. (2017). Thromboembolic Complications During Endovascular Repair of Complex Aortic Aneurysms. In: Oderich, G. (eds) Endovascular Aortic Repair. Springer, Cham. https://doi.org/10.1007/978-3-319-15192-2_46
Download citation
DOI: https://doi.org/10.1007/978-3-319-15192-2_46
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-15191-5
Online ISBN: 978-3-319-15192-2
eBook Packages: MedicineMedicine (R0)